Background: Diabetes mellitus type 2 is a risk factor for developing
heart failure and myocardial fibrosis, but there is no specific therapy for
diabetic heart disease. 1-[2-(4-methoxyphenyl)]-2-[3-(4-methoxyphenyl)
propoxy]ethyl-1H-imidazole (SKF96365) is regarded as an inhibitor of
receptor-mediated calcium ion (Ca) entry. This study aimed to explore the
effects of SKF96365 on diabetic myocardial fibrosis. Methods: A type 2
diabetic rat model induced by a high-sugar and high-fat diet combined with
streptozotocin was established. Thirty specific pathogen-free male Wistar rats
were divided randomly into three groups: group A (the blank control group), group
B (the diabetes group) and group C (the diabetes + transient receptor potential
canonical channel [TRPC] blocker intervention group). Group C was given
0.74-µmol/kg SKF96365 by intraperitoneal injection, and groups A and B were
given the same amount of normal saline by intraperitoneal injection. The weight
and blood sugar of the rats were monitored. After 12 weeks, the weight of the
whole heart and the left ventricle was measured, and the heart and the left
ventricular weight ratios were calculated. Haematoxylin–eosin (HE) staining was
used to observe pathological changes in the myocardial tissue and the
distribution of nuclei. Masson staining was used to identify collagen and muscle
fibres, and the myocardial collagen volume fraction (CVF) was calculated.
Semi-quantitative reverse transcription–polymerase chain reaction was used to
detect the messenger ribonucleic acid (mRNA) expression of SKF96365 target genes.
A value of p 0.05 indicated that the difference between the groups
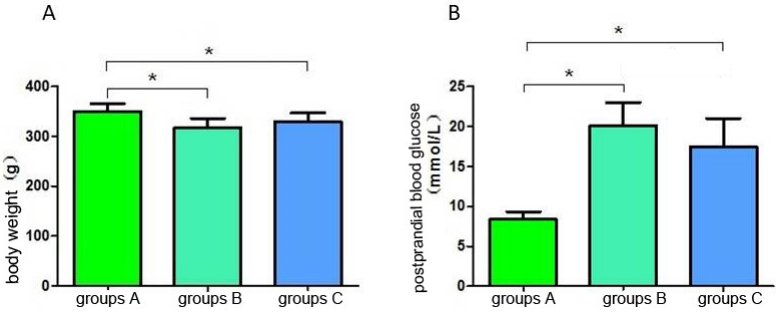
was statistically significant. Results: Compared with the weight of the
rats in group A, the weight of those in groups B and C decreased, while blood
sugar, whole heart weight and left ventricular weight increased (p
0.05). There was no significant difference in body weight between the rats in
groups B and C (p 0.05). The HE staining results showed that the
arrangement of cardiomyocytes in groups B and C was irregular, and focal necrosis
was seen in severe cases. The degree of diabetic cardiomyopathy (DCM) in group C
was less severe than that in group B. Masson staining showed that the CVF
increased in groups B and C, with group B group C (p 0.05); the
mRNA expressions of TRPC3 and TRPC6 were upregulated in groups A, B and C, and
the mRNA expressions of TRPC3 and TRPC6 in group C were downregulated compared
with those in group B (p 0.05). Compared with the expression levels
of SKF96365 target genes (STIM1, Orai1 and Homer1) in
group A, those in group B were lower, while the administration of SKF96365 in
group C did not affect the expression levels of those genes.
Conclusions: SKF96365 can effectively improve myocardial fibrosis in
type-II diabetic rats.