- Academic Editor
-
-
-
†These authors contributed equally.
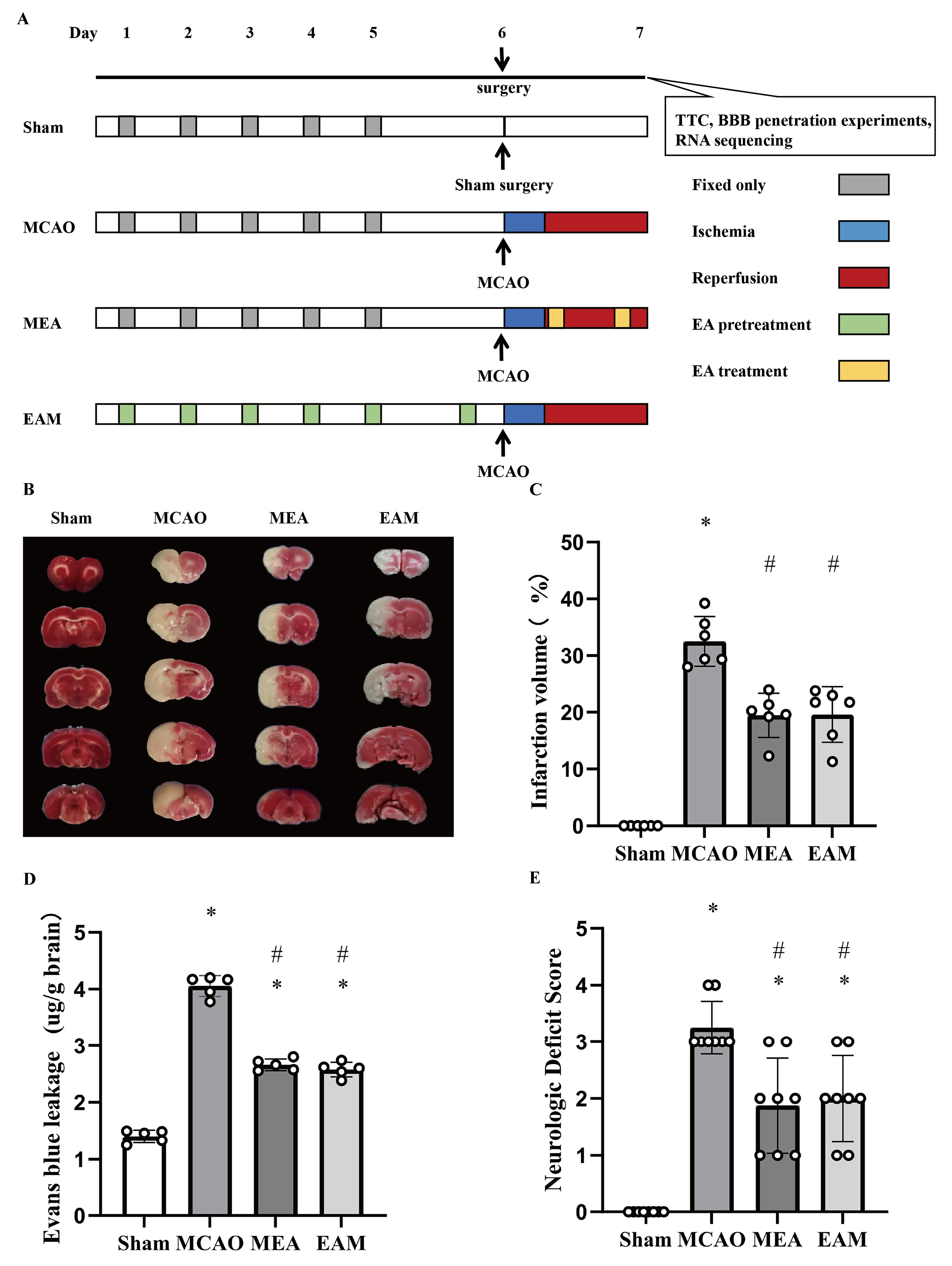
Background: Accumulating evidence suggests that acupuncture may serve as a potent strategy to mitigate the deleterious effects of ischemic stroke on neural tissue. The present investigation delineated the neuroprotective potential of electroacupuncture (EA) administered pre-and post-stroke, with a focus on determining the commonalities and disparities between these two therapeutic approaches in ameliorating ischemic stroke-induced brain injury. The ultimate objective is to inform optimal timing for acupuncture intervention in the clinical management and prevention of stroke. Methods: The extent of cerebral infarction was quantified with 2,3,5-triphenyltetrazolium chloride staining. The integrity of the blood–brain barrier was assessed by evaluating the extravasation of Evans blue (EB) dye, while neurological function was appraised using the Longa neurological scoring system. RNA sequencing was employed to examine the transcriptomic landscape of ischemic brain tissue, with subsequent bioinformatics annotation of the sequencing data facilitated by Metascape. Results: (1) A notable decrease in the ischemic infarct volume was observed in both the EA-preconditioned plus middle cerebral artery occlusion (MCAO), EA-preconditioned plus middle cerebral artery occlusion (EAM) and MCAO plus EA-treated (MEA) groups, compared to the MCAO group. Furthermore, the decreased leakage of EB and reduction in neurological function impairment scores were evident in the EAM and MEA groups compared with the MCAO group. (2) Relative to the Sham group, the MCAO group exhibited a total of 4798 differentially expressed genes (DEGs), with 67.84% demonstrating an expression fold change (FC) greater than 1.5, and 34.16% exceeding a FC of 2. The EAM and MEA groups displayed 4020 and 1956 DEGs, respectively, compared to the MCAO group. In both groups, more than 55% of DEGs showed an expression FC surpassing 1.5, whereas only approximately 10% exhibited a change greater than 2-fold. Remarkably, EA preconditioning and EA treatment resulted in the reversal of 18.72% and 28.91% of DEGs, respectively, in the MCAO group. (3) The DEGs upregulated in response to ischemic stroke were predominantly implicated in immune inflammatory processes and cellular apoptosis, whereas the downregulated DEGs were associated with neurogenesis and neuronal signal transduction. The MEA-induced upregulated DEGs were primarily involved in neural transmission and metabolic processes, whereas the downregulated DEGs were linked to excessive inflammatory responses to physical and chemical stimuli, as well as cell matrix adhesion chemotaxis. In the context of EAM, the upregulated DEGs were chiefly related to protein biosynthesis, and energy and metabolic processes, whereas the downregulated genes were connected to gene transcriptional activity, synaptic function, and neuronal architecture. Conclusions: Both preconditioning and post-event treatment with acupuncture demonstrated efficacy in mitigating pathological damage to brain tissue in a rat model of ischemic stroke, albeit with some divergences in their gene targets. The integration of EA preconditioning and treatment may potentially confer enhanced neuroprotection in the clinical management of stroke patients.