1 Serviço de Imagem Médica, Centro Hospitalar e Universitário de Coimbra (CHUC), 3000-075 Coimbra, Portugal
2 Univ Coimbra, Coimbra Institute for Clinical and Biomedical Research (iCBR), Area of Environment Genetics and Oncobiology (CIMAGO), Instituteof Biophysics, Faculty of Medicine, Coimbra, Portugal, 3000-548 Coimbra, Portugal
3 Univ Coimbra, Institute of Experimental Pathology, Faculty of Medicine, 3000-548 Coimbra, Portugal
4 Univ Coimbra, Institute of Integrated Clinical Practice and Laboratory for Evidence-Based Sciences and Precision Dentistry, Faculty of Medicine, 3000-548 Coimbra, Portugal
5 Univ Coimbra, Centre for Innovative Biomedicine and Biotechnology (CIBB), 3000-548 Coimbra, Portugal
6 Clinical Academic Center of Coimbra (CACC), 3000-075 Coimbra, Portugal
7 Univ Coimbra, Clínica Universitária de Radiologia, Faculty of Medicine, 3000-548 Coimbra, Portugal
8 Univ Coimbra, Coimbra Institute for Biomedical Imaging and Translational Research (CIBIT), 3000-548 Coimbra, Portugal
†These authors contributed equally.
Abstract
Prostate cancer ranks as the second most frequently diagnosed cancer globally among men and stands as the fifth leading cause of cancer-related death in males. Hence, an early and precise diagnosis and staging are critical. Traditional staging is based on clinical nomograms but presents a lower performance than prostate multiparametric magnetic resonance imaging (mpMRI). Since tumor staging serves as the basis for risk stratification, prognosis, and treatment decision-making, the primary objective of mpMRI is to distinguish between organ-confined and locally advanced diseases. Therefore, this imaging modality has emerged as the optimal selection for the local staging of prostate cancer, offering incremental value in evaluating pelvic nodal disease and bone involvement, and supplying supplementary insights regarding the precise location and disease extension. As per the Prostate Imaging Reporting & Data System v2.1 guideline, a comprehensive and accurate mpMRI requires several key sequences, which include T1-weighted imaging (T1WI) and T2-weighted imaging (T2WI) for morphological assessment, with T2WI serving as the cornerstone for local staging. Additionally, diffusion-weighted imaging (DWI) and dynamic sequences acquired with intravenous administration of paramagnetic contrast medium (DCE) are crucial components. It is worth noting that while MRI exhibits high specificity, its sensitivity in diagnosing extracapsular extension, seminal vesicle invasion, and lymph node metastases is limited. Moreover, mpMRI has its own constraints and is not as effective in detecting distant metastases or evaluating lymph nodes, for which extended pelvic lymph node dissection remains the gold standard. This review aims to highlight the significance of mpMRI in prostate cancer staging and provide a practical approach to assessing extracapsular extension, seminal vesicle invasions, and the involvement of adjacent organs and lymph nodes.
Keywords
- prostatic neoplasms
- tumour, node and metastasis (TNM) staging
- local staging
- multiparametric MRI
- extraprostatic disease
Prostate cancer (PC) stands as the second most prevalent cancer among men worldwide and ranks as the fifth leading cause of cancer-related mortality in this population. In 2020 alone, an estimated 1,414,000 new prostate cancer cases were diagnosed, which resulted in 375,304 deaths globally [1].
The aggressiveness of PC exhibits considerable variability, underscoring the critical importance of precise diagnoses, staging, and risk assessment for informed therapeutic decision-making. To guide prognostic and therapeutic decisions, the primary goal is to differentiate between organ-confined diseases and locally advanced stages, as differentiation carries significant implications.
According to the guidelines provided by the European Association of Urology
(EAU), local staging investigations are recommended specifically for intermediate
and high-risk patient groups who present with some criteria, such as
prostate-specific antigen (PSA) levels
Moreover, in specific scenarios, such as when considering a repeated biopsy, the utilization of mpMRI offers notable advantages. Indeed, employing mpMRI to identify suitable candidates for a repeated biopsy both enhances the detection rate of any form of PC and clinically significant PC (csPC), when compared to relying solely on transrectal ultrasound biopsy and also holds the potential to significantly curtail the required number of biopsies (by a substantial 73%) [8]. This reduction in biopsy frequency leads to cost savings per detection as opposed to the expenses associated with transrectal ultrasound procedures. Furthermore, the ability to identify suspicious areas during the mpMRI presents an additional advantage when conducting systematic or targeted biopsies consecutively. This allows us to extract tissue cores from the specific prostate regions that have been flagged by mpMRI [9].
In PC, the presence of an extracapsular extension (ECE), staged as T3a, and seminal vesicle invasion (SVI), staged as T3b, are associated with poorer prognoses. An extracapsular disease increases the risk of positive surgical margins, leading to a higher likelihood of biochemical recurrence [10, 11]. In contrast, SVI is linked to an elevated risk of lymph node (LN) metastasis [12]. Therefore, knowing the exact tumor extension becomes crucial to making the correct treatment decisions, such as selecting between external beam radiation therapy, brachytherapy, or surgery. Additionally, the accurate knowledge of tumor extension allows for more precise definitions of surgical resection margins, thereby reducing the risk of positive resection margins. It can even influence the decision to perform nerve-sparing surgery, with the aim of minimizing postoperative morbidity [10, 13, 14].
Nodal disease in PC carries an increased risk of progression to metastatic disease, leading to higher cancer-specific mortality rates [15, 16, 17]. While MRI currently lacks sufficient diagnostic performance for nodal staging, extended pelvic lymph node dissection (ePLND) remains the gold standard [2]. However, ePLND is an invasive method with disadvantages associated with it. For this reason, additional studies have been developed to find an imaging technique that allows a more efficient and less invasive evaluation of patients with metastatic LN(s) [18].
This review focuses on the role of mpMRI in PC staging and presents a practical approach to assessing ECE, SVI, and/or other adjacent organs, and LN involvement.
Image quality in medical imaging is influenced by many factors, with one crucial factor being the strength of the magnetic field of the scanner. The 3T scanners offer a fundamental advantage over 1.5T scanners due to their higher signal-to-noise ratio (SNR). The SNR is a parameter that theoretically increases linearly with the static magnetic field [19]. Consequently, 3T scanners can potentially provide enhanced image quality compared to their 1.5T counterparts.
It is worth noting that both 1.5T and 3T scanners can yield satisfactory and reliable diagnostic results when the acquisition parameters are optimized and state-of-the-art technology is employed [7]. According to the PI-RADS v2.1 guideline, both 1.5T and 3T scanners are considered suitable for performing prostate MRI; however, most experts prefer and recommend 3T [20]. In a study conducted by Ullrich et al. [21], a comparison was made between the 1.5T and 3T MRI systems, revealing that the SNR and the “contrast-to-noise ratio” (CNR) for T2-weighted images (T2WI) exhibit similar performance across both field strengths. However, when it comes to diffusion-weighted images (DWI), the SNR and CNR notably diminish at 1.5T. Given the particular significance of DWI in identifying csPC within the peripheral zone (PZ), the preference lies with the utilization of 3T scanning. Exceptions exist, and there are some situations in which it is preferable to perform the examination on a 1.5T scanner, namely:
- When patients have implanted devices, it may not be safe to perform the exam in 3T.
- While patients can undergo MRI safely using 3T scanners, it is important to consider the presence of implanted devices, such as bilateral metallic hip prostheses. In some cases, the proximity of these devices to the area being imaged can lead to artifacts that negatively affect image quality. Therefore, caution should be exercised when imaging patients with such implants, to ensure optimal image interpretation.
It is essential to emphasize that conducting prostate MRI at lower magnetic field intensities, particularly, those that are below 1.5T, is not advisable and is currently not being practiced [20].
The limitations inherent to mpMRI can be classified into two categories: factors affecting image acquisition quality and those influencing accurate interpretation [22].
To align with PI-RADS 2.1 recommendations, mpMRI testing requires a minimum system field strength of 1.5T [20].
Crucial sequences within mpMRI, such as DWI and dynamic sequences acquired with intravenous administration of paramagnetic contrast medium (DCE) imaging, extend beyond morphological assessment. These sequences are notably sensitive to motion artifacts induced by prostate spasms, muscle movements, and even intestinal motility. To counter this, implementing strategies to limit intestinal motion is suggested (check section 2.5).
Inherent patient attributes can impose additional constraints on prostate MRI [22]. The strength of organ signals, a crucial determinant of image quality, depends on their proximity to the MRI receiver coil. In cases of severe obesity, where increased adipose tissue thickness creates a greater distance between the coil and the prostate, image quality may suffer a significant decline. Furthermore, the presence of metallic foreign objects, especially hip endo-prostheses, which tend to become more common with age, can introduce substantial limitations. Metal endo-prostheses can induce field distortions, potentially compromising the reliability of mpMRI assessments [22].
To achieve the best outcomes, it is imperative that mpMRI studies be reviewed by experienced radiologists [23]. These studies are most effectively conducted within specialized reference centers, thereby augmenting quality through the input of multiple experienced professionals. The proficient interpretation of morphological data demands a thorough patient profile, ideally provided in a comprehensive manner by urologists. This collaborative effort between radiologists and urologists cultivates mutual expertise, ensuring that radiologists furnish essential information for urologists, who, in turn, adeptly decipher radiological descriptions [23].
Prior to undergoing an MRI, thorough contraindication screening is imperative to ensure patient safety. Essential checks encompass implants, metallic foreign bodies, contrast allergies, and renal function. In cases of potential contraindications, consultation with a radiologist is prudent. Guidelines for contrast agent contraindications and renal function are outlined in the European Society of Urogenital Radiology (ESUR) contrast media guidelines [24].
Post-biopsy hemorrhage, contrary to earlier assumptions, does not hinder mpMRI. A study by Rosenkrantz et al. [25] demonstrated that substantial hemorrhage and a brief post-biopsy interval do not compromise the accuracy of csPC detection via mpMRI. Despite this finding, the latest European Association of Urology (EAU) guidelines recommend prioritizing MRI before biopsy [26].
In patients with contraindications to mpMRI, alternatives for local staging encompass transrectal ultrasound and abdominopelvic CT [26]. However, both methods have limited accuracy for local staging [27]. In cases of locally advanced cancers, abdominopelvic ultrasound or CT might reveal rectal or bladder invasion, along with upper collecting system dilatation [27].
The utilization of mpMRI has revolutionized the diagnostic approach to PC. It serves not only as an imaging technique for identifying suspicious lesions but also as an intraprocedural guide for targeted biopsies (MRI-TBx), thereby effectively closing the diagnostic gap [28].
Multiple randomized trials conducted at both single and multicenter levels, including studies, such as PROMIS [29], MRI-first [30], PRECISION [31], and the investigation by van der Leest et al. [32], have consistently demonstrated a superiority by the “MRI pathway”. This approach involves employing mpMRI and MRI-TBx on suspicious lesions, outperforming the conventional “standard pathway” of the standard biopsy for all patients with elevated PSA levels and/or positive digital rectal exploration results. MRI-TBx offers the advantage of reducing the overall number of biopsies performed while also diminishing the diagnosis of clinically insignificant diseases. Simultaneously, it either maintains or enhances the diagnosis of csPC [28].
Recent studies have revealed that using an endorectal coil (ERC) in prostate imaging does not necessarily lead to increased tumor detection rates. However, employing an ERC can offer the advantage of obtaining higher-resolution images and, as a result, may improve local staging. However, although the ERC enhances image quality, it is also associated with several drawbacks. These include deformation of the gland contour, enlargement of the near-field coil, increased cost and examination time, and greater patient discomfort [33, 34]. Currently, with the continuous improvements in hardware and software, it is possible to obtain adequate and accurate images without it [19]. Consequently, the use of ERC is no longer recommended as routine [34].
The PI-RADS v2.1 guideline does not provide a definitive consensus on patient preparation for prostate MRI. In cases where an ERC is not utilized, the presence of air and/or stool in the rectum can cause artifactual distortion, potentially compromising the quality of the diffusion-weighted imaging (DWI). To mitigate this issue, a minimal preparation enema, administered by the patient prior to the examination, may prove beneficial, especially when an ERC is not used. However, it is important to note that an enema can stimulate bowel peristalsis, leading to increased motion-related artifacts in certain instances [20].
In some patients, the use of an antispasmodic agent may help reduce these motion artifacts from the bowel peristalsis. However, it is not always necessary, and factors such as potential adverse drug reactions and the additional cost should be carefully considered before administering [20].
A point of general agreement is that patients should, whenever feasible, empty their rectum just before undergoing an MRI examination. This is because rectal distension caused by a stool or gas has been proven to markedly amplify the extent of geometric distortion within the prostate gland [20].
A comprehensive prostate mpMRI protocol should incorporate a combination of morphological sequences, including T1-weighted imaging (T1WI) and T2-weighted imaging (T2WI) with two functional sequences: DWI and DCE [35]. Each sequence serves a specific purpose in evaluating prostate pathology.
T2-weighted sequences play a pivotal role in prostate MRI, serving as the cornerstone of the imaging protocol. It is crucial to acquire T2WI in the axial plane, and in at least one orthogonal plane, such as sagittal or coronal, to facilitate the morphologic assessment of lesions [20]. These images provide optimal visualization of the zonal anatomy of the prostate, enable the assessment of abnormalities within the gland, and aid in determining the presence of ECE, SVI, and LN spread [19].
Conversely, T1-weighted images are primarily utilized to identify the presence of a hemorrhage within the prostate and seminal vesicles, to delineate the gland’s contour, and as a potentially valuable tool in detecting skeletal and nodal metastasis, particularly following the intravenous administration of paramagnetic contrast medium [20].
An essential component of mpMRI is DWI, a sequence that reflects the random Brownian motion of water molecules within tissues. This functional sequence should include both high b-value images and the apparent diffusion coefficient (ADC) map [20].
The degree of cellularity in PC correlates with GS, which reflects the aggressiveness of the cancer. As the GS increases, there is a greater reduction in the water diffusion capacity. In simpler terms, PC demonstrates restricted diffusion of water molecules, with higher GS presenting more significant restrictions [36, 37].
Dynamic contrast enhancement involves acquiring T1WI before and after the intravenous administration of a gadolinium-based contrast agent (GBCA). It is recommended to apply fat suppression and/or subtraction techniques to improve image evaluation [20].
Similar to other types of tumors, PC typically exhibits early enhancement in the dynamic study compared to normal tissue. A positive finding on DCE is characterized by focal enhancement that occurs earlier or simultaneously, in relation to the enhancement of adjacent normal prostatic tissues. This enhancement pattern typically correlates with suspicious findings by T2WI and/or DWI [20].
During the dynamic study of mpMRI, it is crucial to conduct a thorough evaluation, specifically focusing on the identification of early focal enhancement. If such enhancement is detected, it is essential to carefully examine the corresponding T2WI and DWI to assess the associated abnormality [20].
Currently, the additional value of DCE in PC is not definitively established. Most published data indicate that the incremental benefit of DCE, when added to the combination of T2WI and DWI, is modest. Therefore, while DCE remains an integral component of mpMRI, its role in determining the PI-RADS v2.1 assessment category is considered secondary to T2WI and DWI [20].
Technical specifications in the prostate mpMRI protocol, according to the PI-RADS v2.1 guideline, and some considerations regarding the protocol for the use of a 3T scanner at the authors’ institution are detailed in Table 1.
| Imaging sequence | Technical parameters |
| Isotropic T2-weighted imaging (T2WI) | Use high-resolution small FOV in two planes: one axial (straight/oblique) and one orthogonal (sagittal/coronal). |
| Slice thickness: 3 mm with no inter-slice gap. | |
| FOV should be adjusted up to 20 cm to include the margins of the gland and seminal vesicles. | |
| Diffusion-weighted imaging (DWI) and appar-ent diffusion coefficient (ADC) map calculation should be performed using the following: | Use low b-values (0–100 s/mm |
| A high b-value ( | |
| T1-weighted imaging (T1WI) pre-contrast acquisition | |
| Dynamic contrast-enhanced (DCE) imaging | Prefer 3D DCE acquisitions for improved signal-to-noise ratio. Choose the axial plane. |
| A temporal resolution of no more than 15 s is recommended rather than 10 s or less since it mitigates the potential trade-off in image quality (e.g., lower spatial resolution) associated with excessively high temporal resolutions. | |
| Inject at 2–3 mL/s, beginning with continuous acquisition. The total observation rate must be greater than 2 min. |
Considerations of the protocol made by the authors are indicated by the symbol †.
FOV, field of view.
The establishment of a classification and staging system is essential for grouping patients with similar outcomes and enabling the development of universal recommendations for the therapeutic management of various patient populations [2].
The American Joint Committee on Cancer TNM system, which comprises the T component (extent of primary tumor), N component (LN involvement), and M component (presence of distant metastases), alongside serum PSA levels at the time of diagnosis and histological GS, is the prevailing system used for staging prostate cancer [7]. The most recent version (8th edition) was introduced in January 2018, which incorporated grade groups and simplified organ-confined diseases to pathological stage pT2, while omitting pT2a–pT2c; nevertheless, these subclassifications were maintained for clinical staging purposes [38].
Table 2 provides a comprehensive overview of the specific characteristics of PC, classified according to the TNM staging.
| TNM staging categories | ||
| Category | Definition | |
| T—Primary Tumor | ||
| Tx | Primary tumors cannot be assessed | |
| T0 | No evidence of a primary tumor | |
| T1 | Clinically inapparent tumor that is not palpable | |
| T1a–T1b—tumor incidental histologic finding | ||
| T1c—tumor identified by needle biopsy (e.g., because of elevated prostate-specific antigen (PSA)), although not visible by imaging | ||
| T2 | Tumor that is palpable and confined within the prostate | |
| T2a—tumor involves half of one lobe or less (Fig. 1) | ||
| T2b—tumor involves more than half of one lobe but not both lobes (Fig. 2) | ||
| T2c—tumor involves both lobes (Fig. 3) | ||
| T3 | Tumor extends through the prostatic capsule | |
| T3a—extraprostatic extension (unilateral or bilateral) or microscopic invasion of the bladder neck (Fig. 4) | ||
| T3b—tumor invades Seminal vesicle(s) (SV(s)) | ||
| T4 | Tumor invades adjacent structures other than SV(s): external sphincter, rectum, bladder, levator muscles, and/or pelvic wall | |
| N—Regional (pelvic) lymph nodes | ||
| Nx | Regional lymph nodes cannot be assessed | |
| N0 | No regional lymph node metastasis | |
| N1 | Regional lymph node metastasis | |
| M—Distant metastasis | ||
| Mx | M staging cannot be assessed (e.g., only prostate MRI was performed) | |
| M0 | No distant metastasis | |
| M1 | Distant metastasis | |
| M1a—nonregional lymph node(s) | ||
| M1b—bones | ||
| M1c—other site(s) with or without bone disease | ||
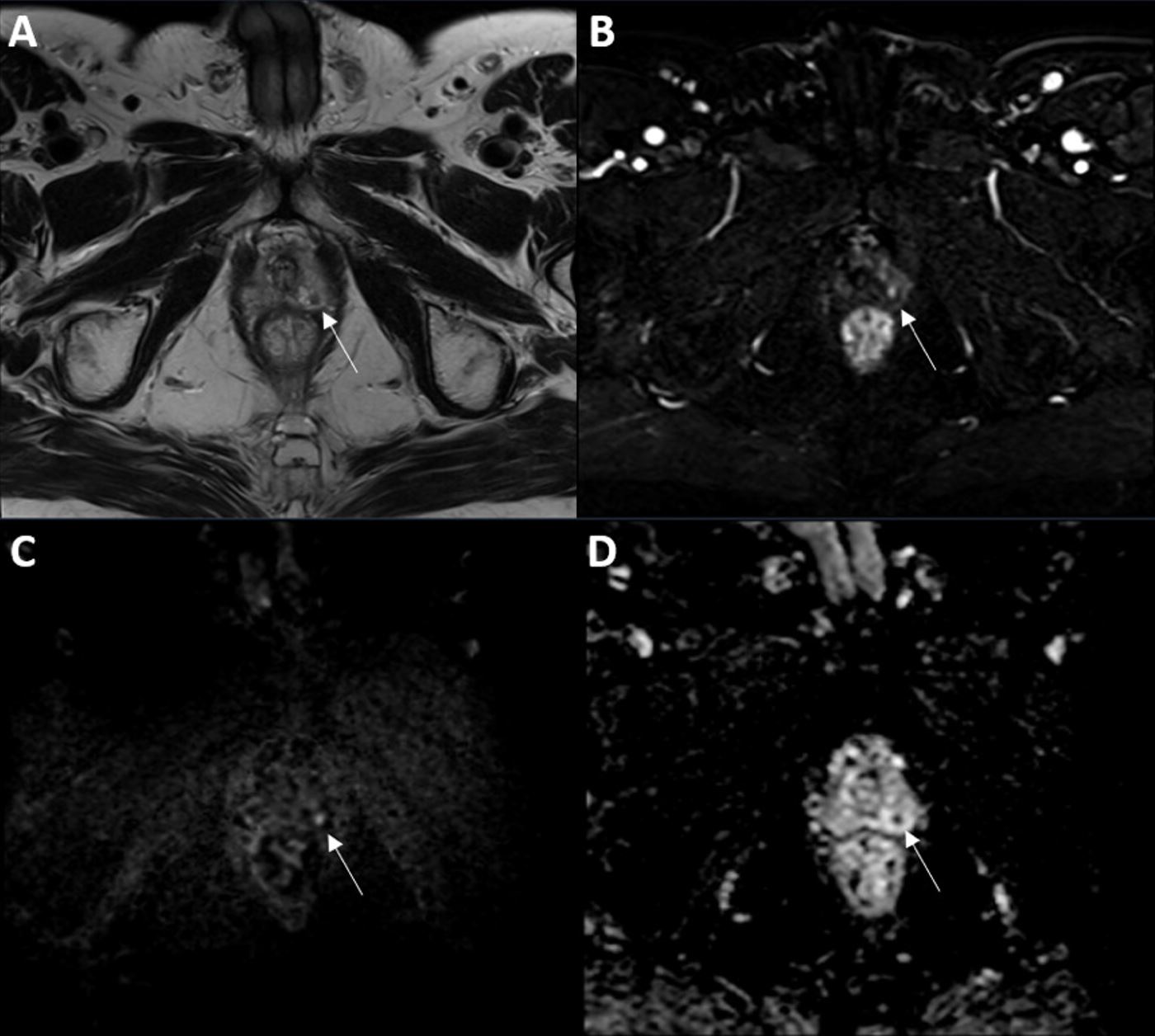 Fig. 1.
Fig. 1.T2a prostate cancer. (A) Axial T2-weighted imaging (T2WI), (B) dynamic contrast-enhanced imaging (DCE), (C) diffusion-weighted imaging (DWI), and (D) apparent diffusion coefficient (ADC) map of a T2a prostate cancer (white arrows), located in the peripheral zone at the left posterolateral sector of the apex.
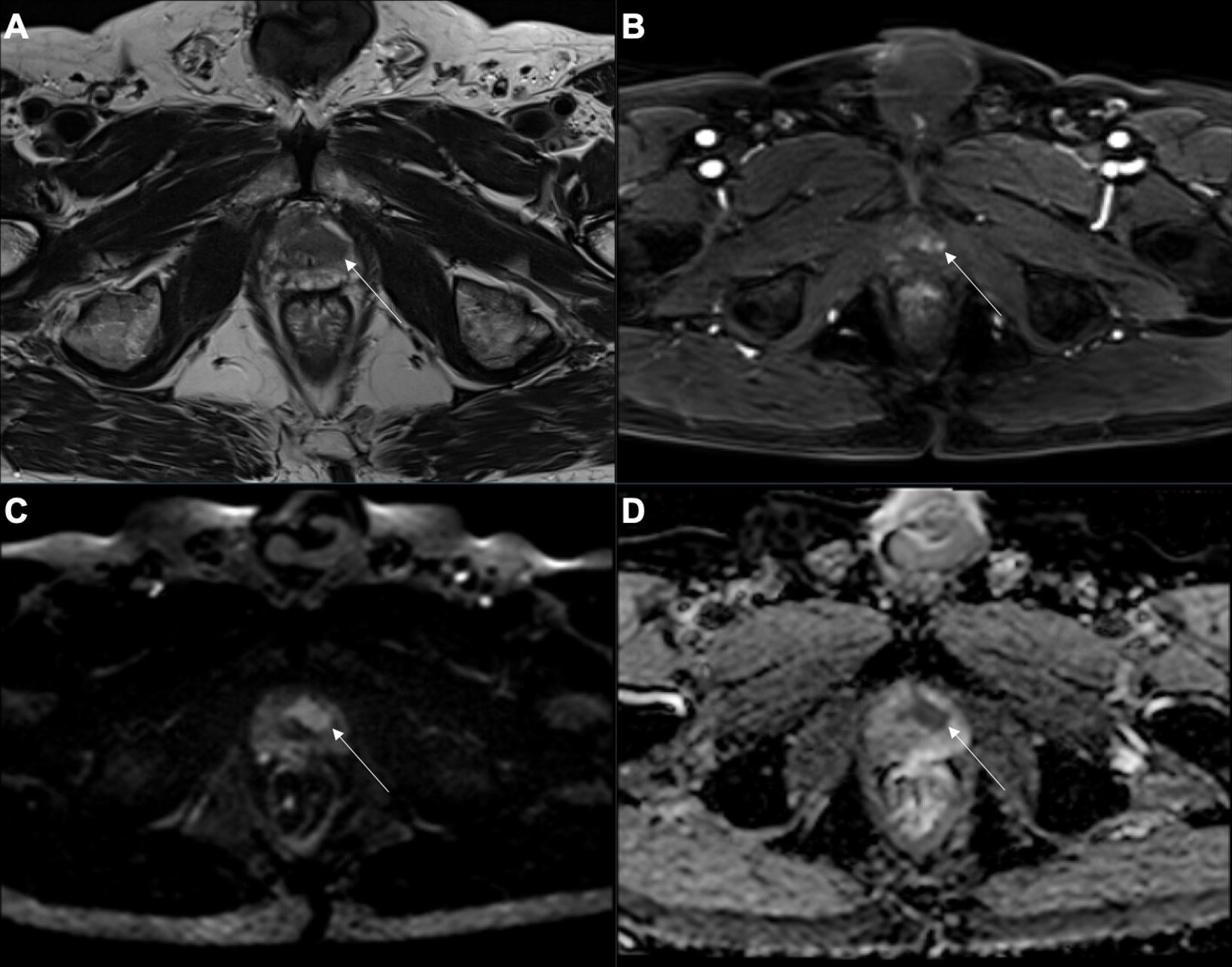 Fig. 2.
Fig. 2.T2b prostate cancer. (A) Axial T2-weighted imaging (T2WI), (B) dynamic contrast-enhanced imaging (DCE), (C) diffusion-weighted imaging (DWI), and (D) apparent diffusion coefficient (ADC) map of a T2b prostate cancer (white arrows), located at the apex and affecting the entire left transition zone.
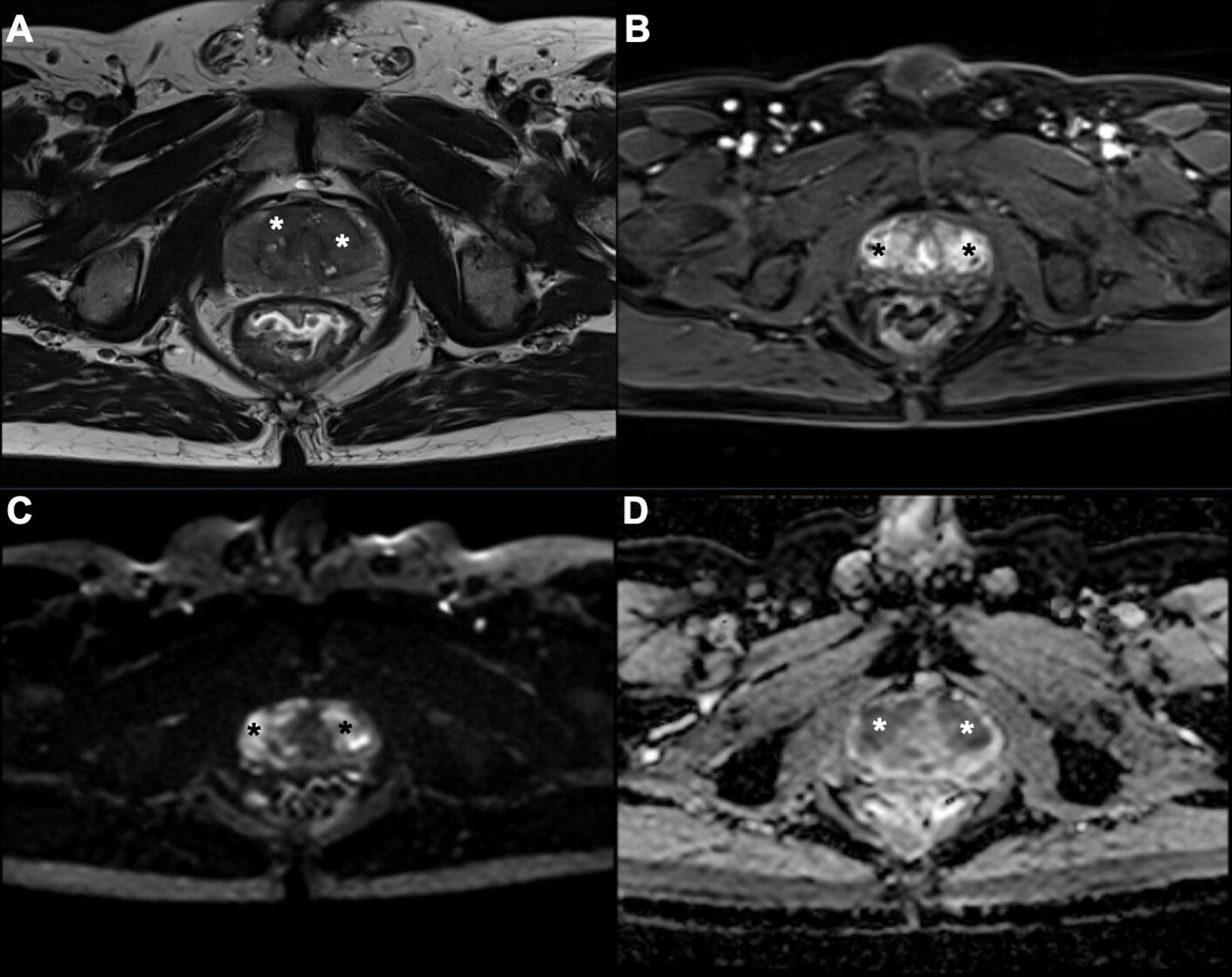 Fig. 3.
Fig. 3.T2c prostate cancer. Extensive lesion (asterisks) located at the mid-gland, affecting all sectors of the transition zone bilaterally, hypointense on T2-weighted imaging (T2WI) (A), with significant restriction of diffusion in diffusion-weighted imaging (DWI) and apparent diffusion coefficient (ADC) map (C,D), and early and focal enhancement on dynamic contrast-enhanced imaging (DCE) (B), compatible with a final PI-RADS v2.1 category 5. Histopathological analysis of the surgical specimen revealed prostate cancer (pT2c N0 Mx). *: an extensive lesion that affects practically the entire prostate gland.
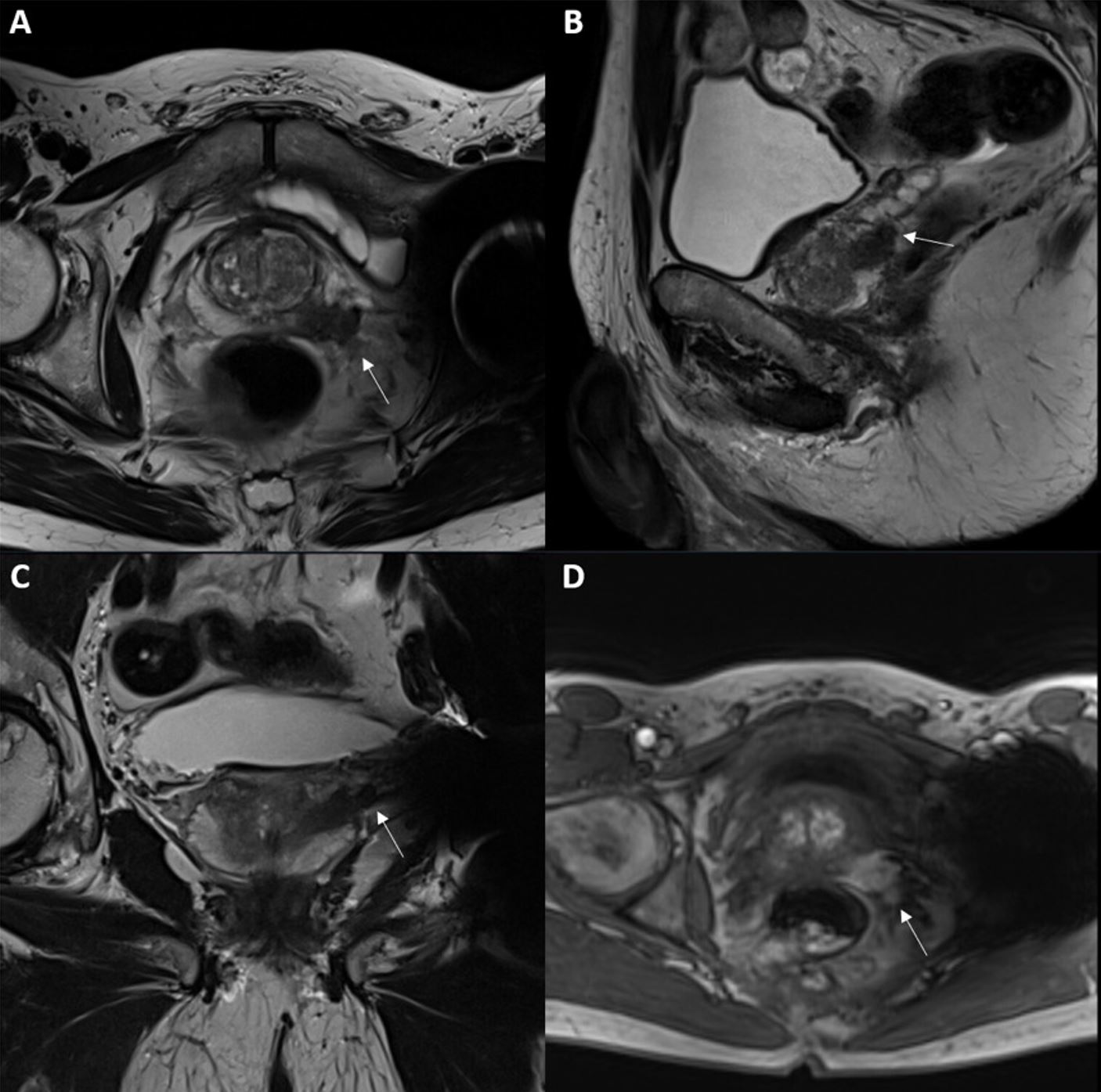 Fig. 4.
Fig. 4.T3a prostate cancer. Extensive lesion located in the peripheral zone, at the base/mid-gland, left posterolateral sector, hypointense on T2-weighted imaging (T2WI) (A–C), with early and focal enhancement on dynamic contrast-enhanced imaging (DCE) (D), compatible with a final PI-RADS v2.1 category 5. There is a high probability of extracapsular extension (ECE) (European Society of Urogenital Radiology (ESUR) Score of 5, high risk of ECE) and invasion of the periprostatic neurovascular bundle, as indicated by the white arrows. These findings were confirmed in the histological analysis of the surgical specimen (pT3a N0 Mx).
According to the latest EAU guidelines [2], PC confined to the prostate gland is classified into groups T1 and T2. Within these groups, there are cases of asymptomatic neoplasia that are not clinically visible and are incidentally detected during transurethral resection (T1a—T1b). For an organ-confined disease, the T1c and T2 stages are particularly relevant from a radiological perspective, as both stages histologically represent a carcinoma that has been proven by a biopsy. However, an important distinction exists between them: by definition, T1c cancer is not visualized by MRI [7]. This differentiation is significant in the context of cohorts in active surveillance studies, as non-visible lesions (T1c) exhibit a significantly higher progression-free survival compared to visible lesions (T2) [39].
Locally advanced prostate cancer (T3—T4) is associated with a poorer prognosis and an increased likelihood of positive surgical margins and biochemical recurrence after primary therapy than the organ-confined disease (T1—T2). In T3a diseases, there is ECE, which indicates the spread of the cancer beyond the prostate capsule. T3b denotes SVI, where cancer has reached and infiltrated the seminal vesicles. T4 means direct invasion of adjacent organs or structures, excluding the seminal vesicles [7].
Multiparametric MRI plays a crucial role in distinguishing between the T2 disease (tumor confined to the prostate) and T3 or higher diseases (tumor extending beyond the prostate). However, the ability of mpMRI to discriminate between the different subcategories (a–c) within the T2 stages is limited. While mpMRI exhibits high sensitivity in detecting the index lesion (the largest and usually most aggressive lesion), its sensitivity for detecting multifocal lesions, smaller, and/or non-aggressive tumors is relatively low [40, 41].
A recent meta-analysis has demonstrated that mpMRI exhibits high specificity ranging from 88 to 96% for detecting ECE, SVI, and the overall staging of T3 diseases [42].
In addition to its role in local staging, mpMRI can also provide valuable information for evaluating pelvic LN involvement and bone metastases. However, due to the limited field of view (FOV), other cross-sectional imaging modalities, such as nuclear medicine techniques and computed tomography (CT), are better at N and M staging.
According to EAU guidelines, local staging is recommended specifically for
intermediate and high-risk groups of patients (PSA
T3a is characterized not only by the presence of ECE but also by the neurovascular bundle involvement, as well as microscopic invasion of the bladder, neck, and internal bladder sphincter [2]. Histopathologically, ECE is further subclassified into focal and established subtypes [43]. Focal ECE is identified when there are only some foci outside the prostate, and this subtype generally carries a better prognosis compared to established ECE. However, the detection of focal ECE using mpMRI has certain limitations. When there are multiple foci present, it is considered an established ECE, which is associated with a worse prognosis, particularly if there is a positive surgical margin. In such cases, the accuracy of mpMRI is higher [44].
Expert readers are required to evaluate the possibility of ECE [45]. The European Society of Urogenital Radiology (ESUR) has suggested a scoring system to predict ECE, known as the ESUR score, which provides qualitative descriptors designed to assess ECE (Table 3) [46].
| Criteria | Tumor characteristics | Score |
| Extracapsular extension | Capsular abutment | 1 (low risk of ECE)—Fig. 5 |
| Capsular irregularity, retraction, or thickening | 3 (moderate risk of ECE)—Fig. 6 | |
| Neurovascular bundle thickening | 4 (high risk of ECE)—Fig. 7 | |
| Bulge or loss of capsule | 4 (high risk of ECE)—Fig. 8 | |
| Measurable extracapsular disease | 5 (high risk of ECE)—Fig. 9 |
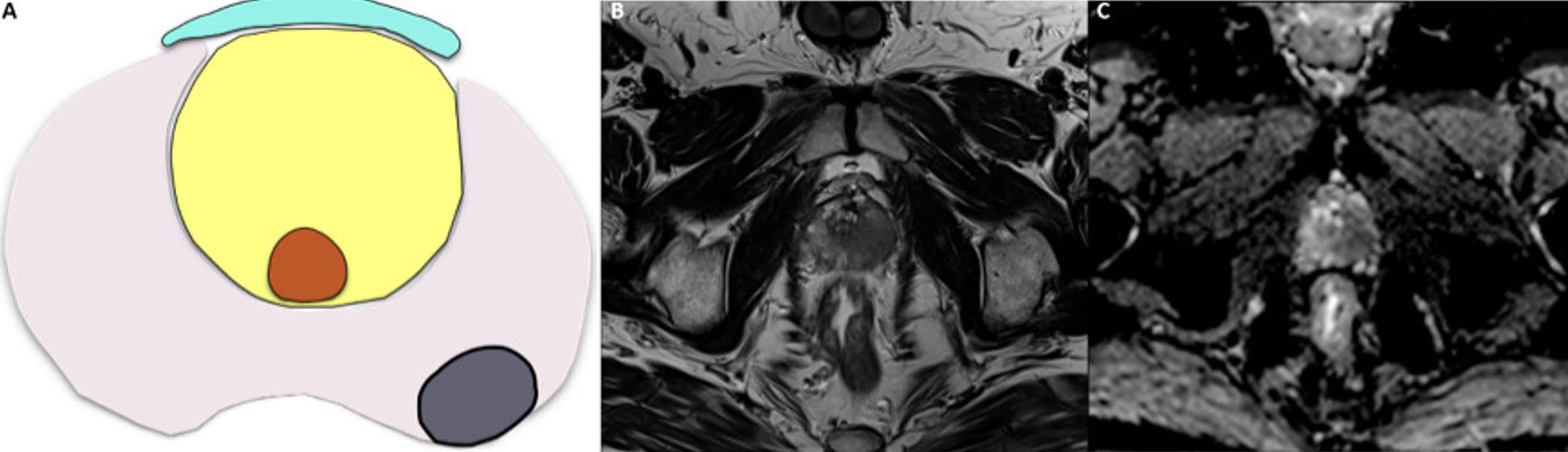 Fig. 5.
Fig. 5.Capsular abutment in a 65-year-old patient with a PSA of 8 ng/mL. (A) Visual depiction of the capsular abutment. (B) Axial T2-weighted imaging (T2WI) of the prostate at the apex shows an ill-defined and hypointense area in the left peripheral zone, which also shows a hypointense signal on the apparent diffusion coefficient (ADC) map (C), compatible with a final PI-RADS v2.1 category 5. There is contact between the suspicious lesion and the posterior margin of the prostatic capsule, indicating capsular abutment and suggesting a low risk of extracapsular extension (ECE), according to the European Society of Urogenital Radiology (ESUR) score (capsular abutment—ESUR Score 1).
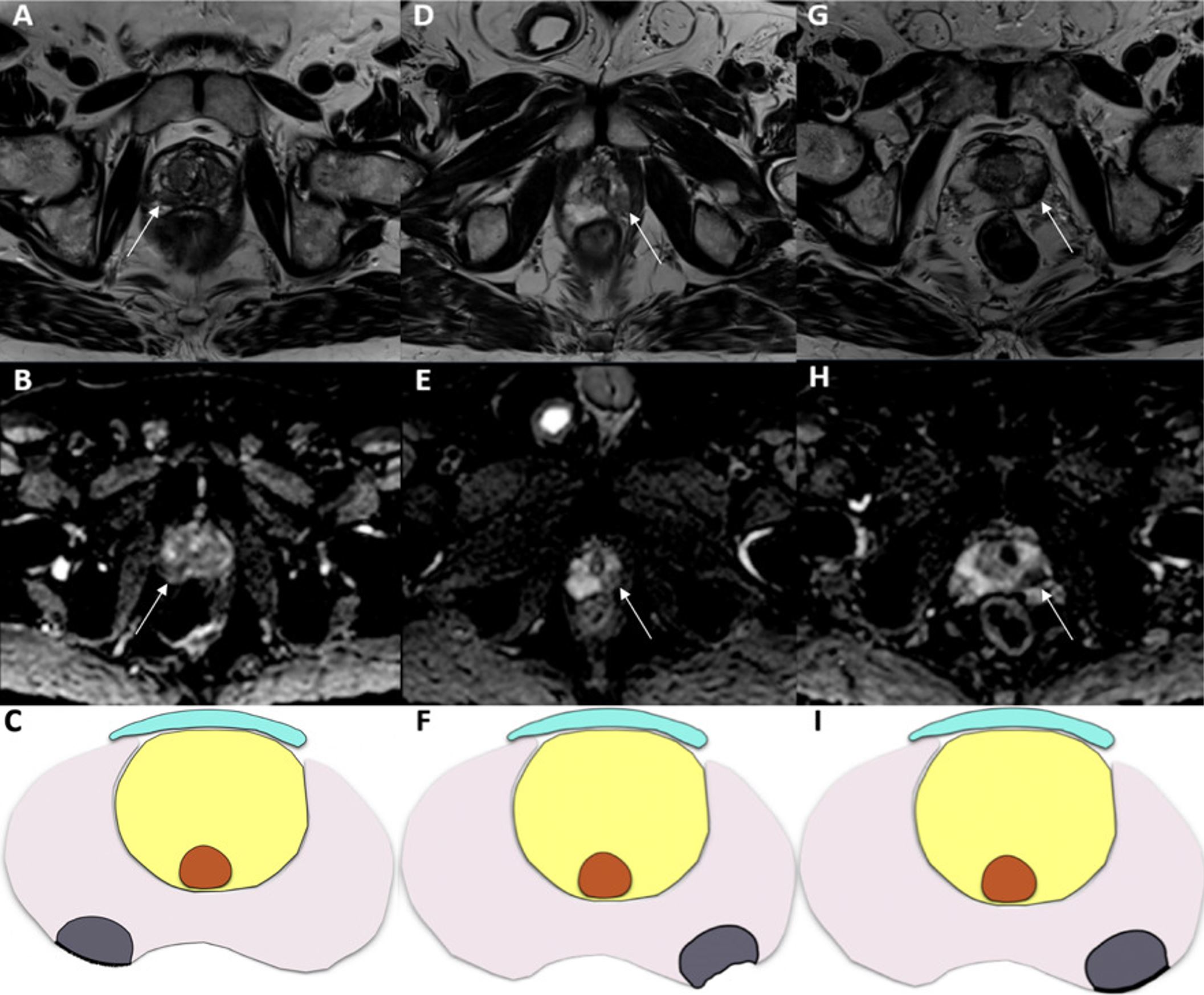 Fig. 6.
Fig. 6.Three examples of prostate cancer patients with moderate risks of extracapsular extension (ECE)—European Society of Urogenital Radiology (ESUR) Score 3. Capsular irregularity as a sign of ECE in a 73-year-old patient with a 5.8 ng/mL prostate-specific antigen (PSA). (A) Axial T2-weighted imaging (T2WI) and (B) apparent diffusion coefficient (ADC) map of the prostate show visible irregularity in the prostate capsule in the right peripheral zone (as indicated by the white arrows). This irregularity has been reported as a possible indication of ECE and graded as an ESUR Score of 3, corresponding to a moderate risk of ECE. (C) Visual depiction of capsular irregularity. Capsular retraction as a sign of ECE in a 71-year-old patient with a PSA of 8 ng/mL. (D) Axial T2WI of the prostate at the apex shows a nodular hypointensity in the left peripheral zone with a hypointense signal on the apparent diffusion coefficient (ADC) map (E), compatible with a final PI-RADS v2.1 category 4. There is a visible asymmetry in the margins of the peripheral zone of both lobes, with notable retraction of the left capsule, leading to an alteration in the contour of the left peripheral zone (as indicated by the white arrows). This finding should be reported as a sign of ECE (ESUR Score 3, moderate risk of ECE). (F) Visual depiction of capsular retraction. Thickening of the capsule in ECE in a 59-year-old patient with a PSA of 4.8 ng/mL. Note a focal thickening of the capsule (as indicated by the white arrows) in the left lobe (G,H), which can be compared to the normal capsule surrounding the right peripheral zone (ESUR Score 3, moderate risk of ECE). (I) Visual depiction of capsular thickening.
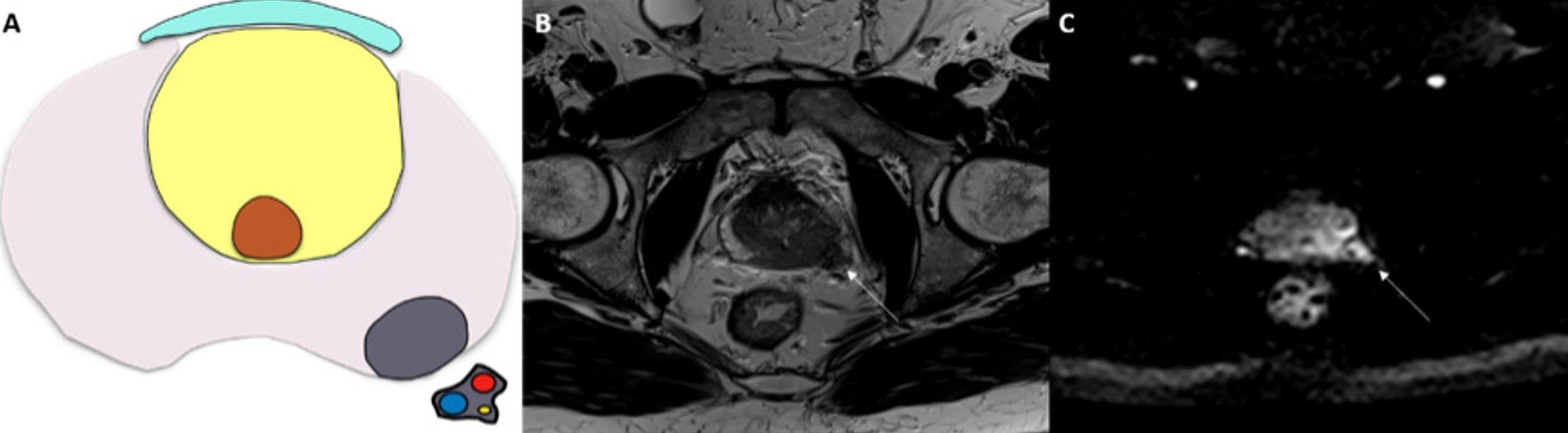 Fig. 7.
Fig. 7.Neurovascular bundle thickening as a sign of extracapsular extension (ECE) in a 69-year-old patient with a prostate-specific antigen (PSA) of 6.5 ng/mL. (A) Visual depiction of neurovascular bundle thickening. (B) Axial T2-weighted imaging (T2WI) and (C) diffusion-weighted imaging (DWI) of the prostate at the mid-gland show an ill-defined and hypointense area in the left peripheral zone, with a significant DWI restriction, which is compatible with a final PI-RADS v2.1 category 5. The thickening of the capsule extends to the left neurovascular bundle, which also seems enlarged compared to the contralateral bundle (as indicated by the white arrows) (European Society of Urogenital Radiology (ESUR) Score 4, high risk of ECE).
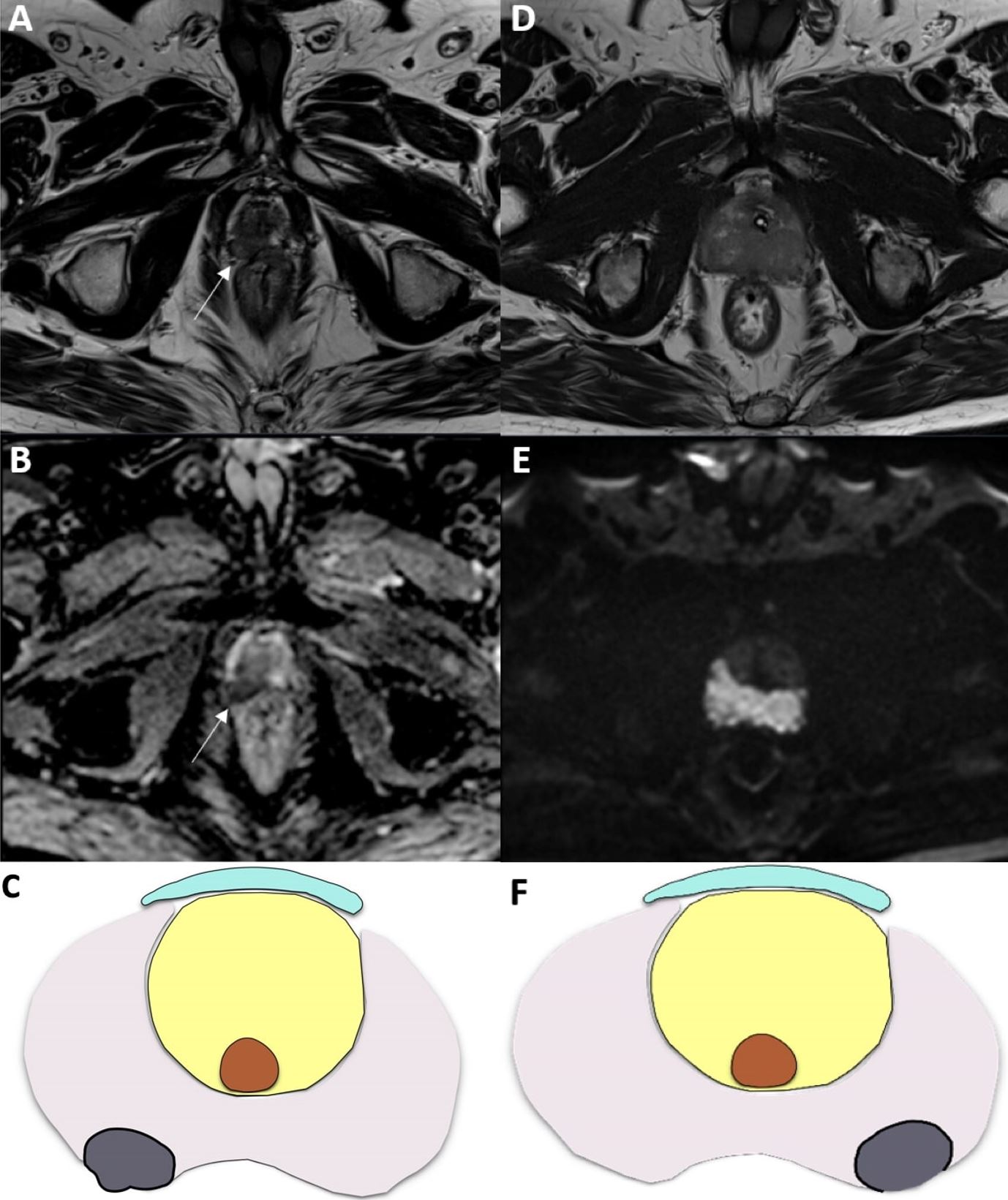 Fig. 8.
Fig. 8.Two examples of prostate cancer patients with high risks for extracapsular extension (ECE)—European Society of Urogenital Radiology (ESUR) Score 4. Capsular bulging in a 72-year-old patient with a prostate-specific antigen (PSA) of 9.3 ng/mL. (A) Axial T2-weighted imaging (T2WI) and (B) apparent diffusion coefficient (ADC) map of the prostate at the mid-gland-apex level, a PIRADS 4 lesion is identified in the right peripheral zone. Additionally, there is a noticeable asymmetry between the two lobes, with the right lobe enlarged due to the presence of the lesion and a corresponding bulging of the capsule (as indicated by the white arrows). This finding suggests ECE (ESUR Score 4, high risk of ECE). (C) Visual depiction of capsular bulging. Capsule loss in a 77-year-old patient with a PSA of 11 ng/mL. (D) Axial T2WI and (E) diffusion-weighted imaging (DWI) of the prostate at the mid-gland reveals a PIRADS 5 lesion in both the right and left peripheral zones. Notably, there is a loss of the capsule in the left lobe, which can be compared to the normal capsule observed around the right peripheral zone. This finding suggests the possibility of ECE (ESUR Score 4, high risk of ECE). (F) Visual depiction of capsular loss.
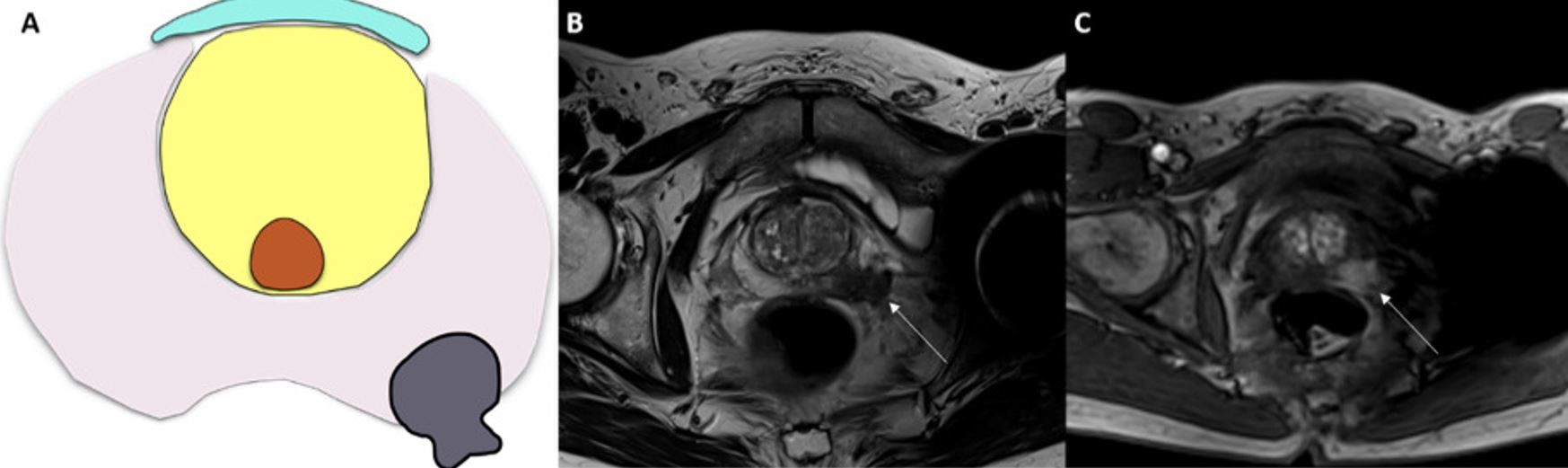 Fig. 9.
Fig. 9.Measurable extracapsular extension in a 71-year-old patient with a prostate-specific antigen (PSA) of 14 ng/mL. (A) Visual depiction of measurable extracapsular extension. (B) Axial T2-weighted imaging (T2WI) and (C) dynamic contrast-enhanced imaging (DCE) of the prostate at the mid-gland show an ill-defined and hypointense area in the left peripheral zone. In the DCE image, focal and early enhancement is observed, compatible with a final PI-RADS v2.1 category 5. However, in (B,C), the suspicious lesion extends beyond the capsule, infiltrating into the periprostatic fat (as indicated by the white arrows). This measurable ECE is highly suggestive of ECE (European Society of Urogenital Radiology (ESUR) Score 5, high risk of ECE).
The probability of an extracapsular extension (ECE) is evaluated using a five-point scoring system that assigns an ordinal risk score to signify the likelihood of an ECE. It is crucial to highlight that this scale does not incorporate a score of two.
In a study conducted by Boesen et al. [47], in 2015, the authors
scrutinized this scoring model and identified that a cutoff threshold of
Furthermore, the length of the tumor contact with the capsule, as observed by MRI, has been shown to be a strong predictor of ECE, by demonstrating good to excellent agreement among different readers [48, 49, 50]. Nonetheless, it is important to acknowledge the considerable diversity in the threshold values documented in various studies, spanning from 6 to 20 mm. In response to this incongruity, the PI-RADS v2.1 guidelines have incorporated an arbitrary reference point, setting the cutoff at a length of 10 mm [49].
A recent development in this field is the introduction of a novel grading system by Mehralivand et al. [51], known as the extraprostatic extension (EPE) grade, which utilizes MRI features to predict the likelihood of an ECE. The grading system defines the following categories:
- Grade 0: No suspicion for EPE.
- Grade 1: Either tumor contact length
- Grade 2: Both features defined for grade 1 are present.
- Grade 3: Visible ECE is detected by MRI [51].
In 2022, Caglic et al. [52] evaluated the capsular enhancement signal (CES) role in DCE imaging to detect ECE. Their findings demonstrated that CES is a highly predictive indicator of ECE presence and is closely associated with increased tumor aggressiveness [52]. Moreover, they conclude that the presence of CES may offer significant clinical utility in predicting ECE, particularly in the small but significant percentage of patients where this signal is found. This observation can be visually appreciated in Fig. 10, which illustrates the distinctive CES characteristic on MRI scans (Fig. 10).
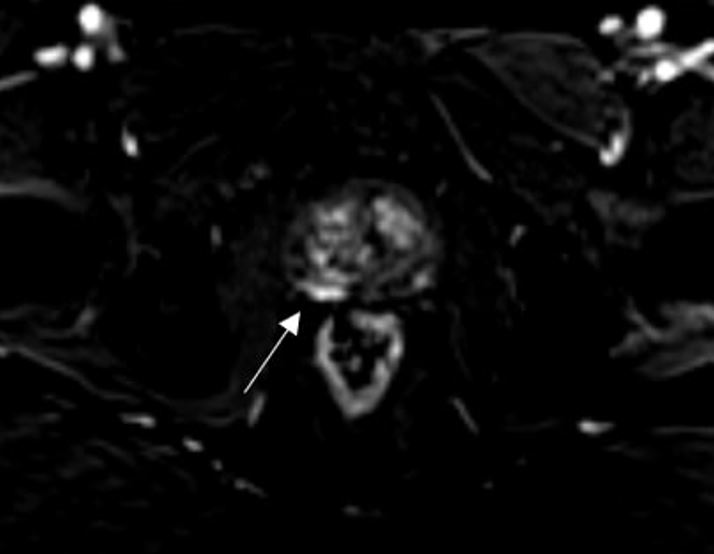 Fig. 10.
Fig. 10.Capsular enhancement sign (CES). Subtraction image after the intravenous administration of a low molecular weight gadolinium-based contrast agent demonstrates capsular enhancement sign (CES), as indicated by the arrow in the right peripheral prostate, and predicts T3a disease. The surgical specimen confirmed a pT3a Gleason 4 + 3 prostate cancer with extracapsular extension.
To evaluate the seminal vesicles effectively, a combination of T2WI and functional imaging is recommended. Recent studies have proven that incorporating functional sequences, particularly DWI, enhances the accuracy of seminal vesicle assessment more significantly than DCE [55, 56]. In addition, acquisition/reconstructions in the sagittal and coronal planes play a vital role in characterizing the pattern of tumor dissemination, whether it is through the ejaculatory ducts (type I) or by ECE (type II) [7].
Hypointensity on T2WI, DWI restriction, or DCE enhancement in the seminal vesicle region indicates SVI (Figs. 11,12). Therefore, it is essential to always evaluate the three orthogonal planes and look for asymmetries.
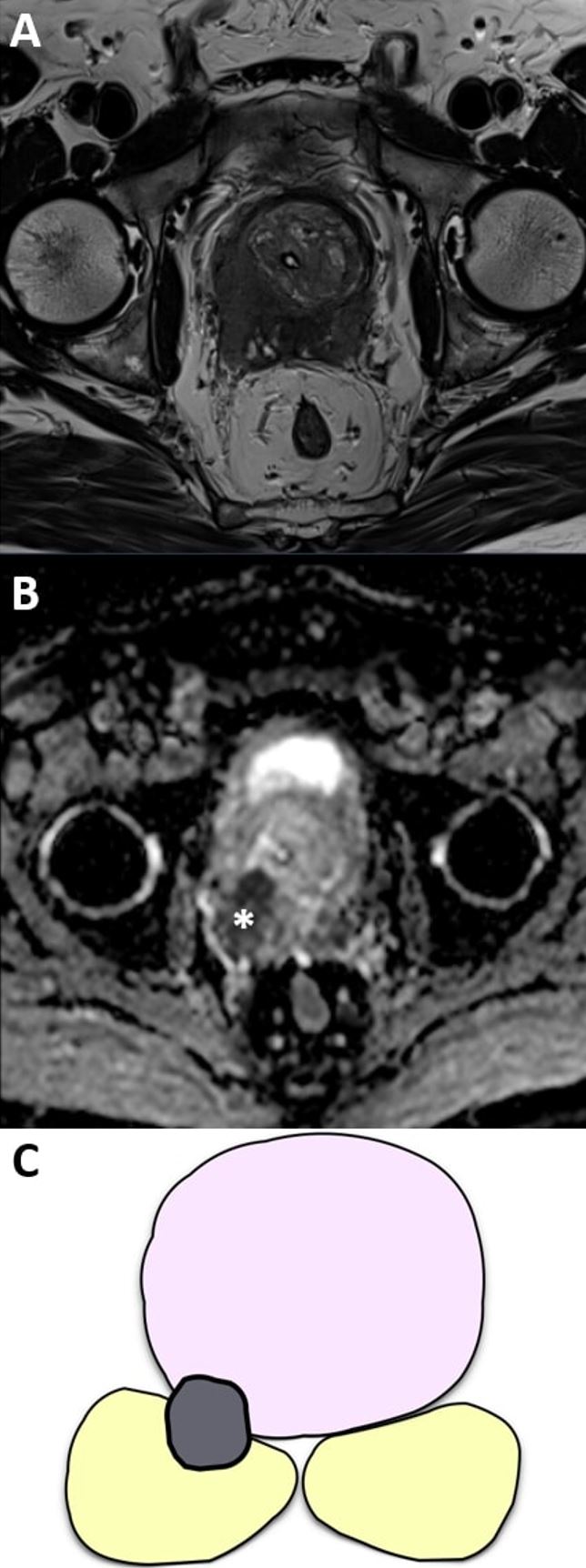 Fig. 11.
Fig. 11.Invasion of the right seminal vesicle (T3b disease) in a 74-year-old patient with a prostate-specific antigen (PSA) of 13 ng/mL. (A) Axial T2-weighted imaging (T2WI) and (B) apparent diffusion coefficient (ADC) map show tumoral invasion of the right seminal vesicle, originating from a prostate cancer located in the right prostatic base (partially depicted as a hypointense lesion in (A)). The most caudal segment of the right seminal vesicle demonstrates an ill-defined abnormal hypointensity, which is also apparent as a hypointense signal on the ADC map (as represented by the asterisk). (C) Visual depiction of seminal vesicle invasion.
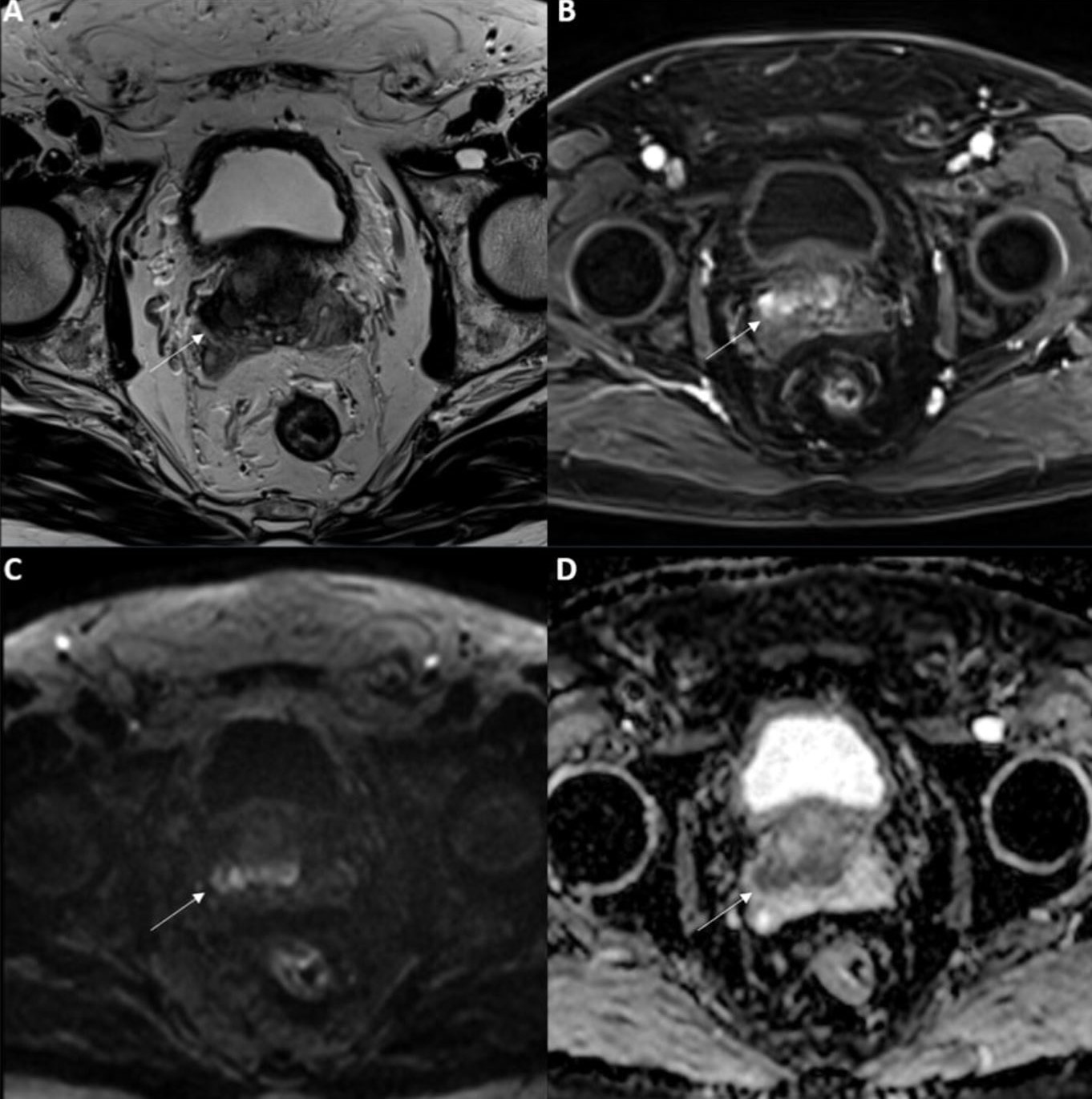 Fig. 12.
Fig. 12.Invasion of both seminal vesicles (T3b disease) in a 66-year-old patient with a prostate-specific antigen (PSA) of 15 ng/mL. (A) Axial T2-weighted imaging (T2WI), (B) dynamic contrast-enhanced imaging (DCE), (C) diffusion-weighted imaging (DWI), and (D) apparent diffusion coefficient (ADC) map of the lower segment of the seminal vesicles in a patient with a known prostate cancer reveal an abnormal hypointensity of both seminal vesicles. Additionally, there is a significant restriction observed on DWI, along with focal and early enhancement (as indicated by the arrows), which strongly suggests seminal vesicle invasion (SVI). The subsequent surgical specimen confirmed a pT3b Gleason 4 + 4 prostate cancer with infiltration of both seminal vesicles.
Finally, T4 PC involves the invasion of adjacent structures beyond the seminal vesicles, including the bladder (Fig. 13), external urethral sphincter, levator ani muscles, pelvic wall, and/or rectum (Fig. 14).
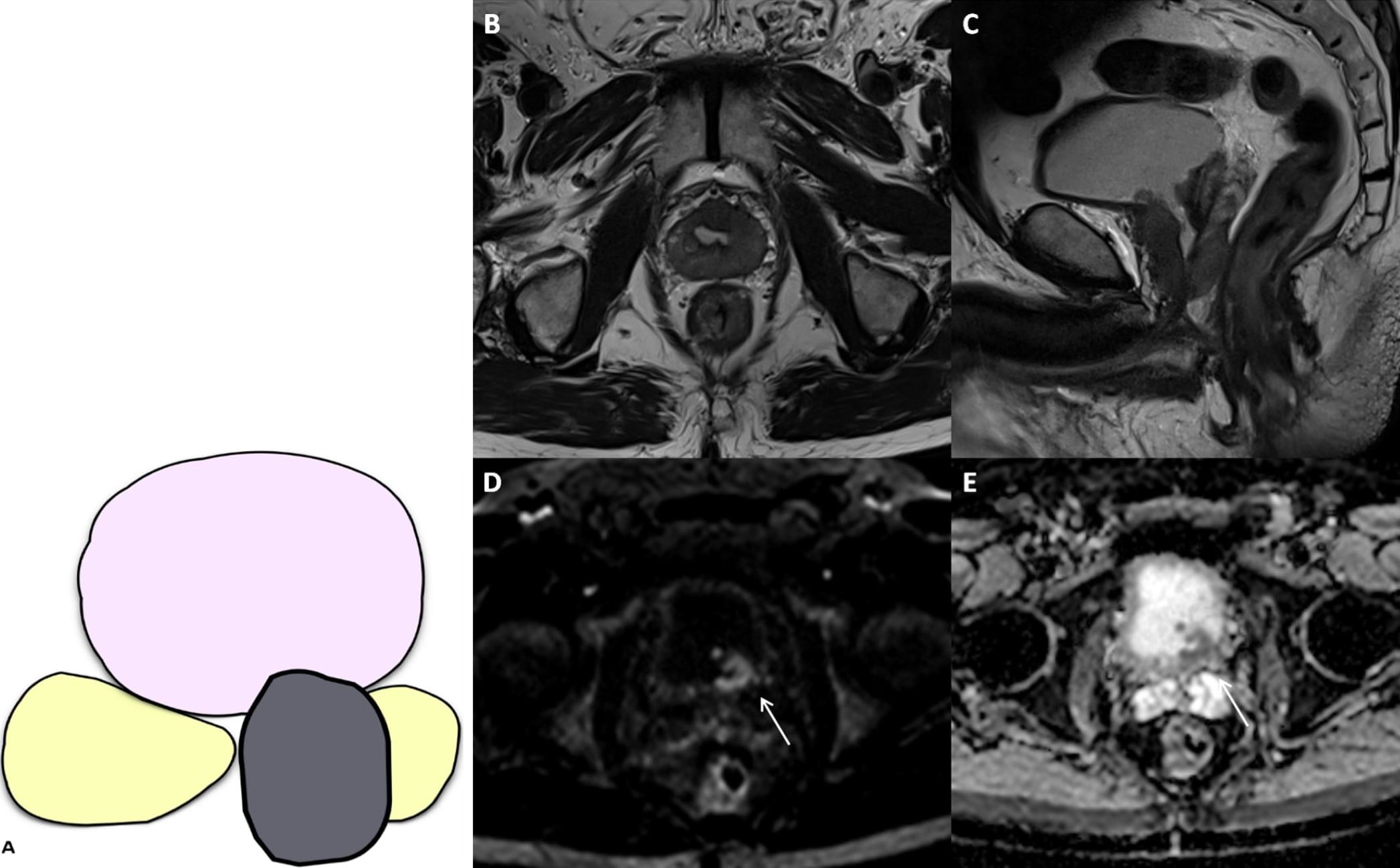 Fig. 13.
Fig. 13.T4 prostate cancer. (A) Visual depiction of T4 disease (tumor invades adjacent structures other than seminal vesicles). Previous transurethral resection of the prostate. An extensive lesion located on both lobes of the transition and peripheral zones is observed, hypointense on T2-weighted imaging (T2WI) (B,C), with significant restriction on diffusion-weighted imaging (DWI) (D) and with the hypointense signal on apparent diffusion coefficient (ADC) map (E), compatible with a final PI-RADS v2.1 category 5. There is an invasion of the left seminal vesicle and bladder (as indicated by the white arrows). The findings were confirmed in the histological analysis of the surgical specimen (pT4 N0 Mx).
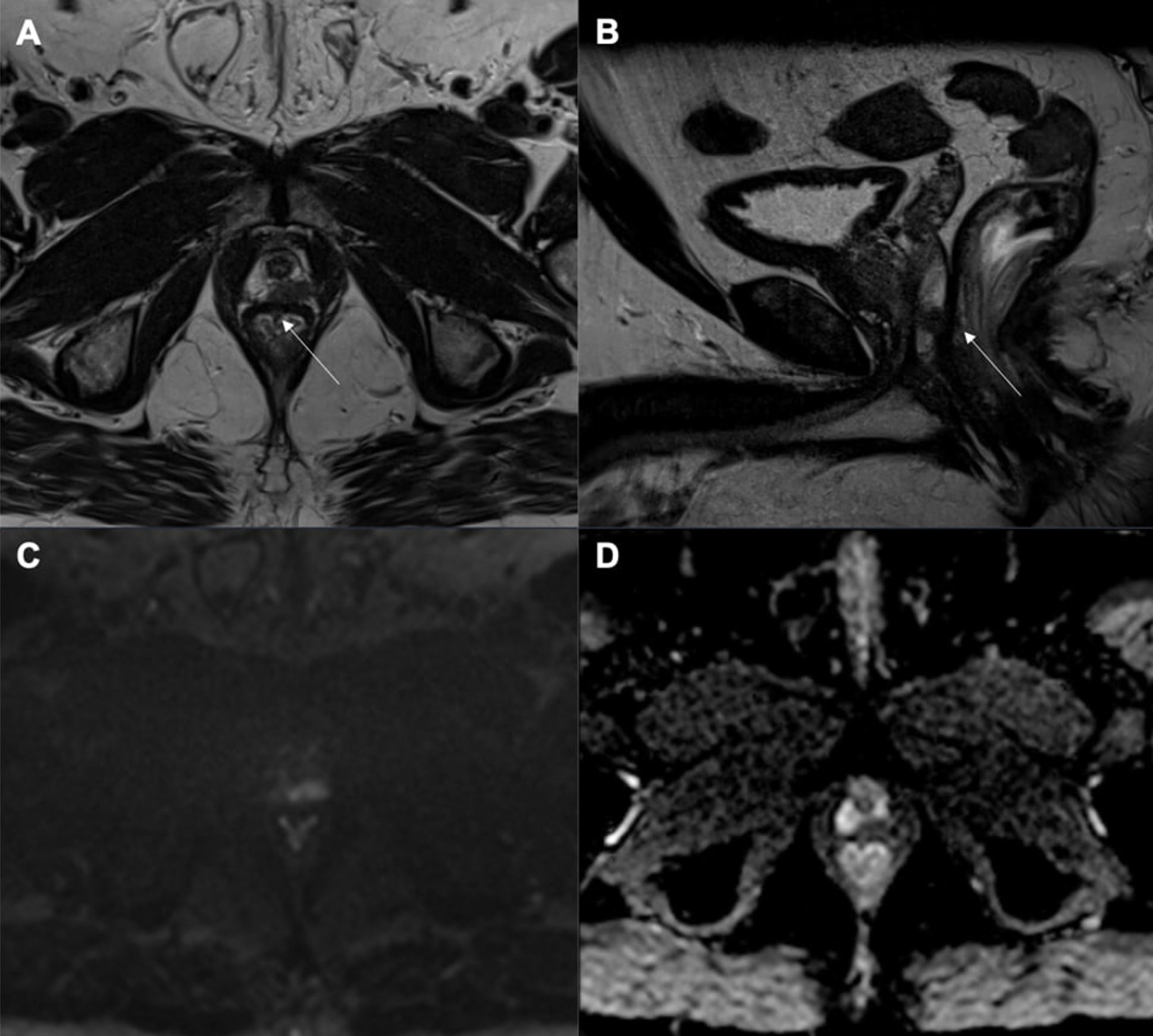 Fig. 14.
Fig. 14.T4 prostate cancer. An ill-defined and hypointense area on T2-weighted imaging (T2WI) (A,B) located in the left peripheral zone, at the apex, with significant restriction on diffusion-weighted imaging (DWI) (C) and with hypointense signal on apparent diffusion coefficient (ADC) map (D), compatible with a final PI-RADS v2.1 category 5. The lesion is in contact with the anterior wall of the lower rectum, with an evident interruption of the hypointense serosal line at this level (as indicated by the white arrows), suggesting an invasion of this organ. The findings were confirmed by histological analysis of the surgical specimen (pT4 N0 Mx).
Given its poor prognosis and elevated risk of biochemical recurrence, most guidelines recommend a combination of androgen deprivation therapy and radiation to manage T4 PCs [58]. Consequently, the accurate detection of a T4 disease before surgery is of paramount importance to ensure appropriate treatment planning.
Nodal spread is seen in 5–10% of PCs at the time of radical prostatectomy [59]. Prostate cancer primarily metastasizes to four specific nodal stations in the pelvis, freferred to as regional nodes: the obturator chain, internal and external iliac chains, and presacral chain [60]. The involvement of any regional node is classified as stage N1. Conversely, the involvement of non-regional stations (e.g., paraaortic, paracaval, deep inguinal, femoral, and common iliac lymph nodes) represents the M1a disease (Fig. 15) [61, 62].
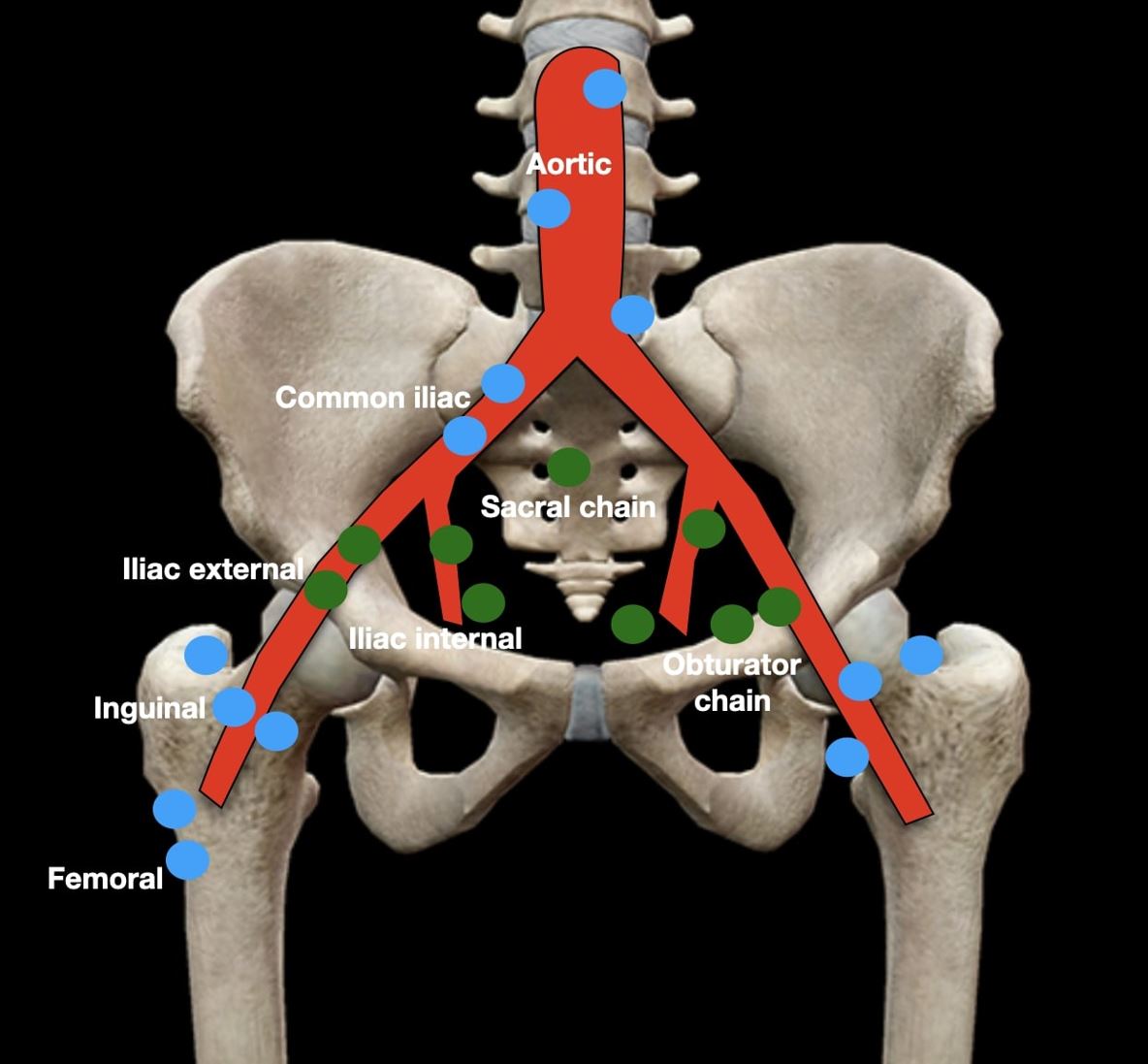 Fig. 15.
Fig. 15.Visual depiction of lymph node dissemination of prostate cancer. Regional lymph nodes (green) are below the common iliac junction level and are staged as N1. These include four chains: iliac (internal and external), sacral, and obturator. Distant lymph nodes (blue) are outside these regions and are staged as M1a metastatic diseases. They include, among others, the aortic, common iliac, femoral, and inguinal chains.
A retrospective study conducted by Asfuroğlu et al. [53], in 2022, sought to determine the most effective MRI-based method for predicting EPE. They compared the performance of the ESUR score, Likert scale (a score based on a subjective overall assessment of a combination of mpMRI criteria by an experienced radiologist), tumor contact length, and EPE grade. The study concluded that all four methods exhibited good diagnostic performance in predicting EPE. However, the study specifically highlighted the EPE grade as a promising approach due to its utilization of both qualitative and quantitative parameters. Moreover, the EPE grade was found to be less dependent on the reader’s experience, further enhancing its reliability as a predictive tool for EPE [53].
Considering the lack of a definitive consensus on ECE-related signs for PC, further studies are needed to establish the most effective methods for predicting ECE when utilizing mpMRI.
In addition to detecting ECE, pinpointing the specific location of T3a is vital since clear surgical margins become harder to achieve in the apex. Conversely, tumors situated away from the neurovascular bundle, e.g., anteriorly, allow for nerve-sparing surgery, thereby reducing postoperative complications, such as incontinence and erectile dysfunction [54].
T3b disease involves neoplastic growth in one or both seminal vesicles. This occurs through PC cell penetration via ejaculatory ducts or direct contact with the prostatic capsule. SVI prevalence ranges from 4% to 23% [55, 56].
Ejaculation abstinence aids SV distension; however, the PI-RADS v2.1 benefits are uncertain [20].
Additionally, T3b patients face heightened risks of LN involvement, local recurrence, and distant metastasis. Identifying SVI preoperatively becomes crucial for prognosis and treatment planning [57].
Differentiating between T3a and T3b stages is of utmost importance when determining the appropriate therapeutic approach. Thus, patients with T3b tumors are more likely to benefit from external beam radiotherapy or androgen deprivation therapy instead of radical prostatectomy or brachytherapy [7].
Studies mapping the distribution of nodal metastases demonstrated that around 75% of pelvic nodal metastases are located within the obturator chain and the internal and external iliac chains, while the remaining 25% are found in the aortic bifurcation, common iliac chain, and presacral chain [60].
The PI-RADS v2.1 guideline, in alignment with the EAU recommendations, emphasizes the importance of performing N staging using mpMRI in all patients, irrespective of their risk classification, and even prior to the biopsy. This approach entails not only the employment of standardized sequences, to distinguish confined neoplasia from locally advanced neoplasia (T staging), but also the utilization of an appropriate FOV that extends up to the aortic bifurcation. This expanded FOV allows for the evaluation of common iliac lymph nodes and bifurcations (M1a), to facilitate the partial staging of the bony pelvis (M1b) [35].
Currently, the identification of abnormal LN(s) by MRI, primarily, relies on assessing their size, morphology, shape, and enhancement pattern [20]. Some of the suggested evaluation criteria include a size exceeding 8 mm, a round shape, the loss of the fatty hilum, a low T2WI signal relative to the primary tumor, and an irregular border (Fig. 16) [7].
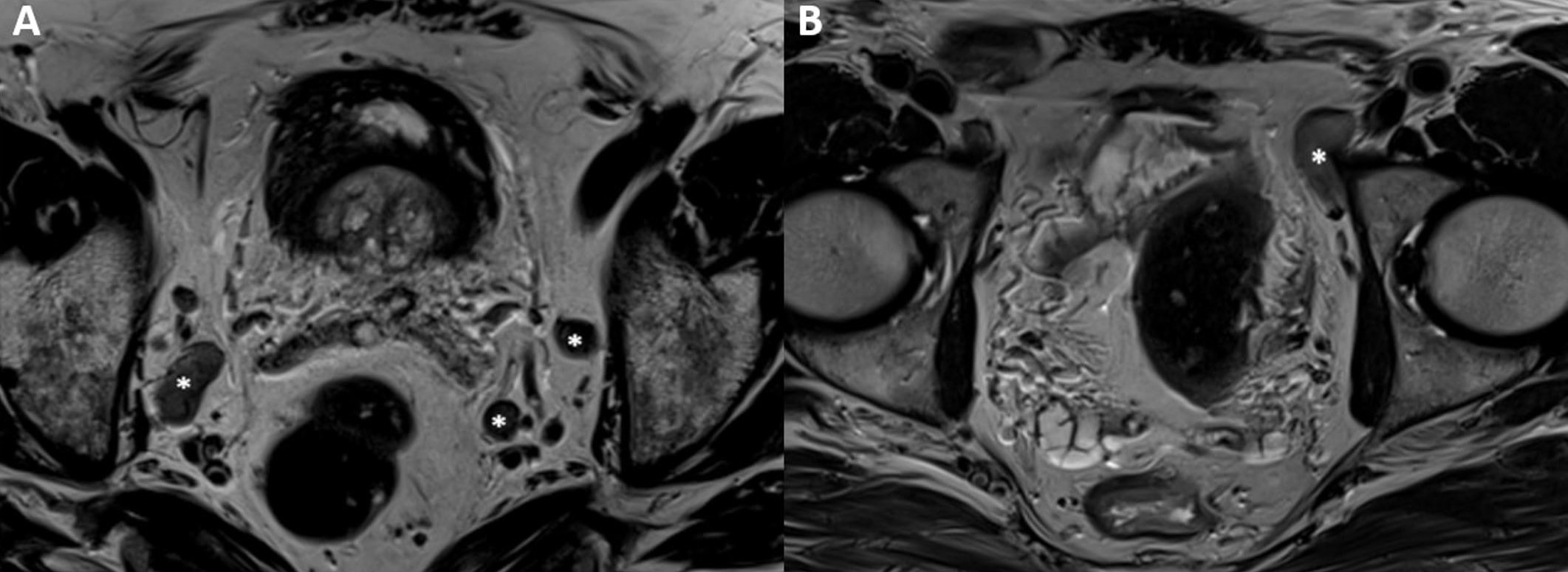 Fig. 16.
Fig. 16.Two patients with prostate cancer with metastatic lymph node (LN) involvement. (A) A 77-year-old patient with a prostate-specific antigen (PSA) of 25 ng/mL. Enlarged LN bilaterally (as represented by the asterisks) consistent with metastatic involvement by T2-weighted imaging (T2WI). (B) A 66-year-old patient with a PSA of 21.2 ng/mL. Enlarged left external iliac LN (asterisk), consistent with metastatic involvement by T2WI.
Size alone is a useless criterion for evaluating a positive LN disease. Not only is there significant dimensional overlap between positive and negative LN(s) but certain reactive inflammatory changes can also produce false positive results. In addition, smaller LN(s) may harbor micrometastases that do not affect the LN size, thus, leading to incorrect staging [63].
Recent studies have revealed that a significant proportion of positive lymph nodes dissected during ePLND, after MRI, have a short axis smaller than 5 mm, below the conventional cutoff point of 8 mm [64].
Despite advancements in MRI, the current diagnostic performance for nodal staging remains suboptimal. Consequently, ePLND remains the gold standard procedure for the accurate detection of LN metastases in PC [26].
More work and development are needed to identify an imaging technique that
allows for a more efficient and less invasive assessment of patients with
metastatic LN(s). Indeed, initial clinical trials of a prostate-specific membrane
antigen
According to the EUA guidelines [26], patients categorized as intermediate- and high-risk should undergo CT imaging of the abdomen and pelvis to evaluate non-regional LN (M1a disease) and assess visceral metastasis (M1c disease). Additionally, bone scintigraphy is recommended for evaluating bone metastasis (M1b disease).
In recent years, whole-body MRI (WB-MRI) has gained attention due to its ability to detect bone marrow infiltration by malignant cells before visible bone remodeling occurs (which can be detected by bone scintigraphy) [67]. For this reason, WB-MRI is particularly useful in M staging, especially in M1b cancers.
The METastasis Reporting and Data System for Prostate Cancer (MET-RADS-P) provides practical guidance for the acquisition, interpretation, and reporting of WB-MRI in advanced PC [68]. The PI-RADS guidelines for the evaluation of metastasis in WB-MRI recommend a protocol consisting of a combination of anatomical (T1WI, short tau inversion recovery [STIR] or T2WI with fat suppression) and functional (DWI) sequences [68].
Despite the diagnostic potential of WB-MRI, several limitations hinder its widespread use for PC staging. The main challenges include high costs and long scanning times [7].
Magnetic resonance imaging has held a central role in PC management, encompassing screening, diagnosis, surveillance, biopsy, and treatment strategies [69, 70, 71]. Yet, the escalating cost-effectiveness concerns associated with MRI, particularly mpMRI, have spurred exploration into more economical alternatives. Additionally, the adverse reactions triggered by gadolinium-based contrast agents have raised critical safety considerations [72], particularly given the complex health profiles of many PC patients. Renal complications, such as end-stage renal disease, acute kidney injury, and chronic kidney disease have been linked to contrast agents [73, 74], with nephrogenic systemic fibrosis being a major concern [74].
In response to these challenges, there is growing interest in using biparametric MRI (bpMRI) as a potential substitute for mpMRI. Indeed, the advantages of bpMRI lie in its contrast-agent-free nature, thereby providing benefits in terms of cost-effectiveness, safety, and efficiency [75, 76]. Eliminating the need for contrast agents significantly reduces the expenses associated with imaging studies. Given these advantages, the call to prioritize bpMRI over mpMRI is becoming increasingly prevalent.
It is important to note that certain contraindications related to MRI scans, such as cardiac implantable electronic devices, metallic intraocular foreign bodies, and other medical implants, apply regardless of the contrast agent. Similarly, issues such as claustrophobia and extreme obesity can still pose challenges during bpMRI [77].
In the context of active surveillance for PC, recent research suggests that while MRI scans reduce the need for repeated biopsies, biopsies are not yet dispensable in the absence of MRI progression [78]. For patients eligible for active surveillance, mpMRI scans to aid in monitoring, while similar efforts are being directed toward understanding the role of bpMRI in active surveillance [79, 80].
Literature consistently underscores the potential for bpMRI to replace mpMRI in diagnosing csPC, thus, offering comparable accuracy in detecting suspicious lesions. An exception lies in lesions graded PI-RADS categories three and four, which may necessitate DCE sequences. PI-RADS category three indicates an equivocal lesion with a significant risk of progressing to clinically significant cancer, while PI-RADS category four indicates a high likelihood of such cancer [81]. Incorporating DCE for PI-RADS category three lesions could upgrade their grading to PI-RADS four if enhancement is focal [82]. Moreover, for extracapsular extension assessment, as indicated by Caglic et al. [52], DCE sequences remain necessary [83].
For future applications, there are several promising avenues for exploration in the realm of bpMRI utilization. These include investigating its applicability in active surveillance, its potential as a biopsy guide, its effectiveness in local staging of PC, and its role in guiding treatment decisions. Additionally, there is a crucial need for the formulation of standardized protocols to incorporate bpMRI whenever feasible, particularly when its accuracy aligns with that of mpMRI.
Fig. 17 briefly illustrates the role of mpMRI in the local staging of PC.
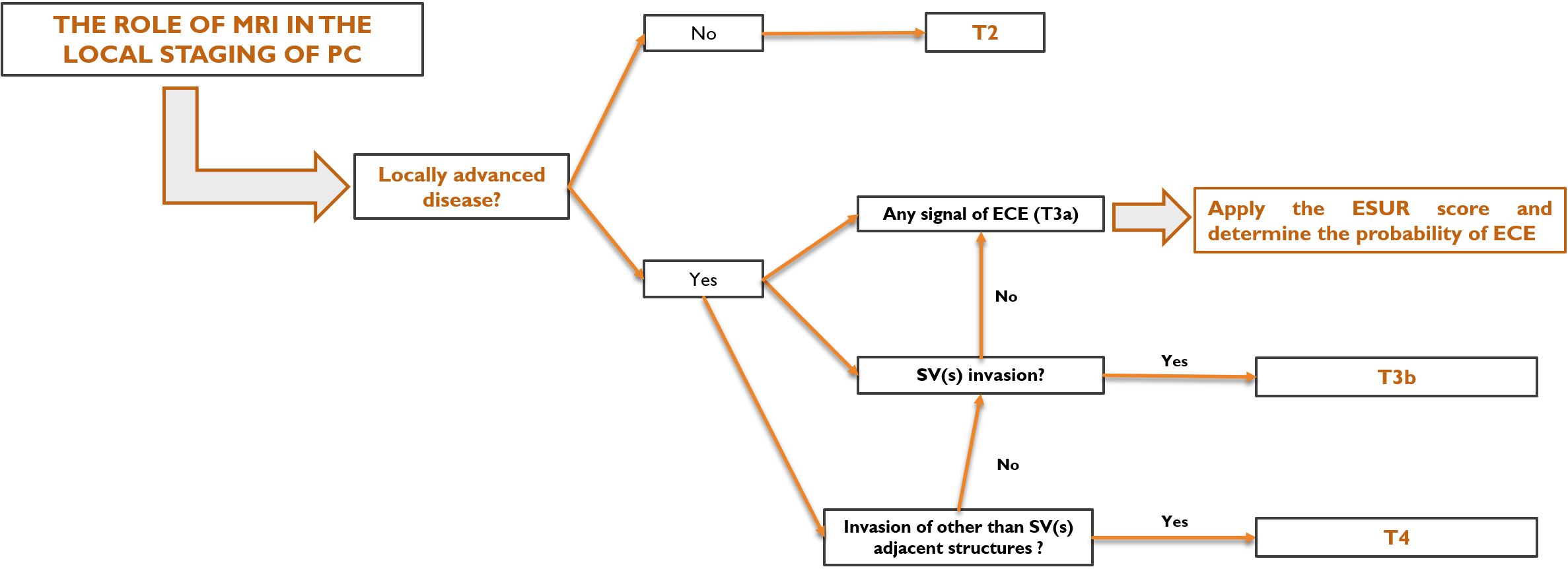 Fig. 17.
Fig. 17.Summary of the role of magnetic resonance imaging in the local staging of prostate cancer.
Prostate mpMRI is the recommended technique for the local staging of PC. It has demonstrated superior performance compared to traditional staging based on clinical nomograms. This non-invasive imaging approach provides comprehensive information regarding the location and extent of the disease, aiding in accurate risk stratification, and playing a crucial role in therapeutic planning.
The standardized protocols suggested by PI-RADS v2.1 yield valuable prognostic
information for patients with intermediate- and high-risk PC, even before biopsy.
T2-weighted imaging continues to be the cornerstone for assessing ECE and SVI;
however, the incorporation of functional sequences, such as DWI and DCE, and the
preference for scanning using 3T, improves staging accuracy. While the current
role of prostate MRI in nodal and bone staging is limited, emerging
“next-generation” imaging modalities, such as
TO and LAF performed the research, analyzed the data, and wrote the original draft. CO and CMM conceptualized the study and reviewed and edited the initial draft. CM and PD provided scientific support and knowledge. CM and PD provided supervision and a critical review of the manuscript. All authors contributed to editorial changes in the manuscript. All authors read and approved the final manuscript. All authors have participated sufficiently in the work and agreed to be accountable for all aspects of the work.
Not applicable.
We acknowledge our hospital colleagues for their help and discussion.
This research received no external funding.
The authors declare no conflict of interest.
References
Publisher’s Note: IMR Press stays neutral with regard to jurisdictional claims in published maps and institutional affiliations.

















