- Academic Editor
*Correspondence: lars.saemann@uk-halle.de (Lars Saemann)
Background: Off-pump coronary artery bypass grafting (OPCAB) is an
alternative to on-pump coronary artery bypass grafting (CABG) with
cardiopulmonary bypass (CPB). During OPCAB, the temporary use of an intracoronary
shunt and inotropic medication or catecholamines should keep the central
hemodynamics constant. Nevertheless, the need for conversion to on-pump CABG
often occurs unexpectedly, most likely due to circulation instability.
Circulation instability can appear first in peripheral body parts; therefore,
peripheral microcirculation might serve as a predictor for the upcoming
conversion to on-pump CABG. We investigated the impact of coronary artery
ligation and shunt insertion during OPCAB on cutaneous microcirculation (cLDP)
with Laser Doppler Perfusion Technology and transcutaneous oxygen partial
pressure (tcpO
Coronary artery bypass grafting (CABG) is the method of choice for the surgical treatment of coronary heart disease. CABG can either be performed on the cardioplegic heart while cardiopulmonary bypass (CPB) maintains the circulation of the body, known as on-pump CABG, or on the beating heart without CPB, known as off-pump CABG (OPCAB). OPCAB is applied to avoid potential adverse effects from the cardioplegic heart and CPB, such as ischemia/reperfusion injury, coagulation activation, systemic inflammation, endothelial dysfunction, and oxidative stress [1]. Although OPCAB rarely needs to be converted to on-pump CABG, a low rate of conversions still exists. The most common reason for conversion to on-pump is hemodynamic instability. Surgery-associated reasons for conversion, such as difficult anastomozation because of small vessels or inadequate visualization, are less frequent [2]. However, small vessels make anastomozation very complicated.
During OPCAB, inserting an intracoronary shunt instead of ligating the coronary artery during anastomozation reduces myocardial dysfunction [3]. Nevertheless, administering inotropic medication according to the typical dynamic hemodynamic demands during OPCAB remains necessary. Despite the use of intracoronary shunts, inotropes, or catecholamines, the necessity to convert OPCAB to on-pump CABG often occurs spontaneously.
The circulation is only monitored by central, macrovascular hemodynamics. Nevertheless, the global circulation of the body might behave inconsistently. Thus, we hypothesize that even under consistent hemodynamics due to coronary shunts and inotropes or catecholamines, tissue perfusion is not stable in the whole body during OPCAB.
Circulation instability can often be observed first in peripheral body parts before central hemodynamics change. It might, therefore, be of high interest as a measure for early prediction for conversion to on-pump. Considering all aspects, this work investigates the course of central hemodynamics and peripheral microcirculation to evaluate circulation instability during OPCAB.
In an experimental model of CABG surgery, healthy pigs with a body weight between 45 and 55 kg underwent OPCAB surgery. The local Ethical Committee for Animal Experimentation (Regierungspräsendium Karlsruhe) reviewed and approved the investigations. Anesthesia was induced with Ketamine and Midazolam. After intubation was performed, anesthesia was maintained intravenously with Propofol 2% (B. Braun, Melsungen, Germany). During the surgical procedure on the beating heart, norepinephrine (Arterenol, Sanofi-Aventis Deutschland GmbH, Frankfurt am Main, Germany) was infused to keep arterial blood pressure stable if necessary.
A median sternotomy followed by pericardiotomy was performed. Internal thoracic arteries were harvested, and heparin was administered to avoid coagulation in the bypass vessels. The left anterior descending coronary artery (LAD) was exposed and ligated so that bleeding could have been avoided during the insertion of an intracoronary shunt (Fig. 1). While the shunt re-established the blood flow through the LAD, the graft was anastomosed.
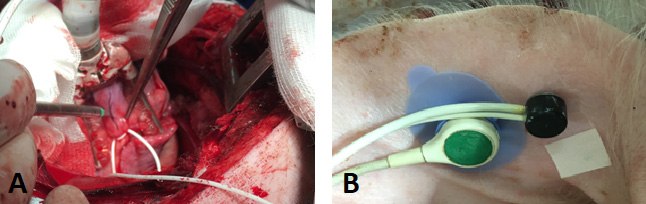 Fig. 1.
Fig. 1.Animal operation. (A) Ligating the left anterior descending coronary artery. (B) Probes. Black probe: Measurement of Laser Doppler Perfusion. Green probe: Measurement of transcutaneous oxygen partial pressure.
We have already shown that Laser Doppler Perfusion Monitoring (LDPM) is a very
sensitive method for observingffective tissue perfusion on the microcirculatory
level in cardiac surgical patients [4]. In LDPM, the measured data is
proportional to microcirculation and expressed in relative units, compared to a
baseline measurement [5]. We applied two monitoring methods for peripheral
perfusion: LDPM to measure cutaneous microcirculation (cLDP) in 17 subjects and
measurement of transcutaneous oxygen partial pressure (tcpO
Statistical analysis was performed using IBM SPSS Statistics for Windows
(Version 20.0, IBM Corp., Armonk, NY, USA). All measurement values are presented
as mean
Peripheral microcirculation was monitored before LAD ligation, after LAD
ligation, and after inserting an intracoronary shunt (Fig. 2). Both cLDP and
tcpO
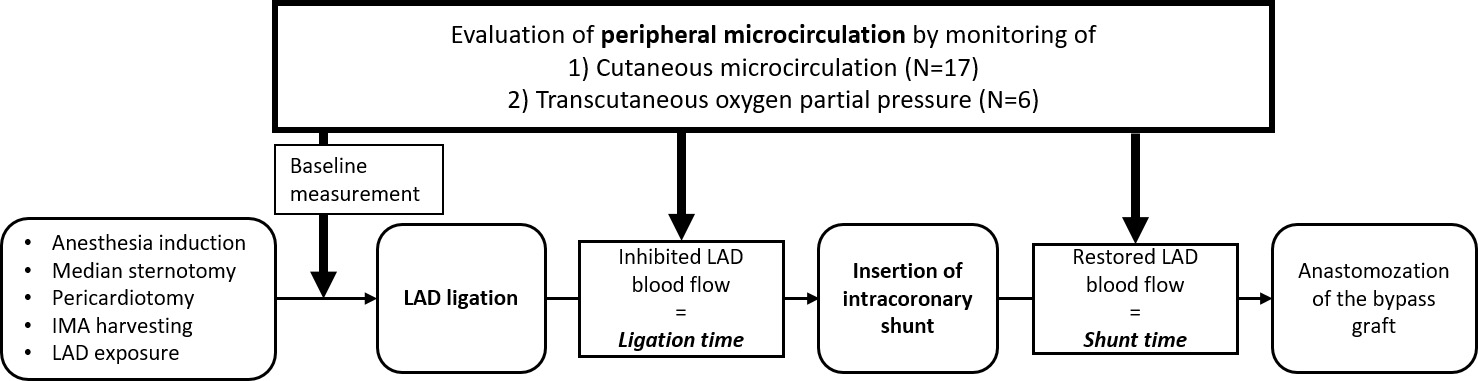 Fig. 2.
Fig. 2.Flow chart of the measurement sequence. IMA, internal mammary artery; LAD, left anterior descending coronary artery.
LAD blood flow was inhibited by ligation for 101
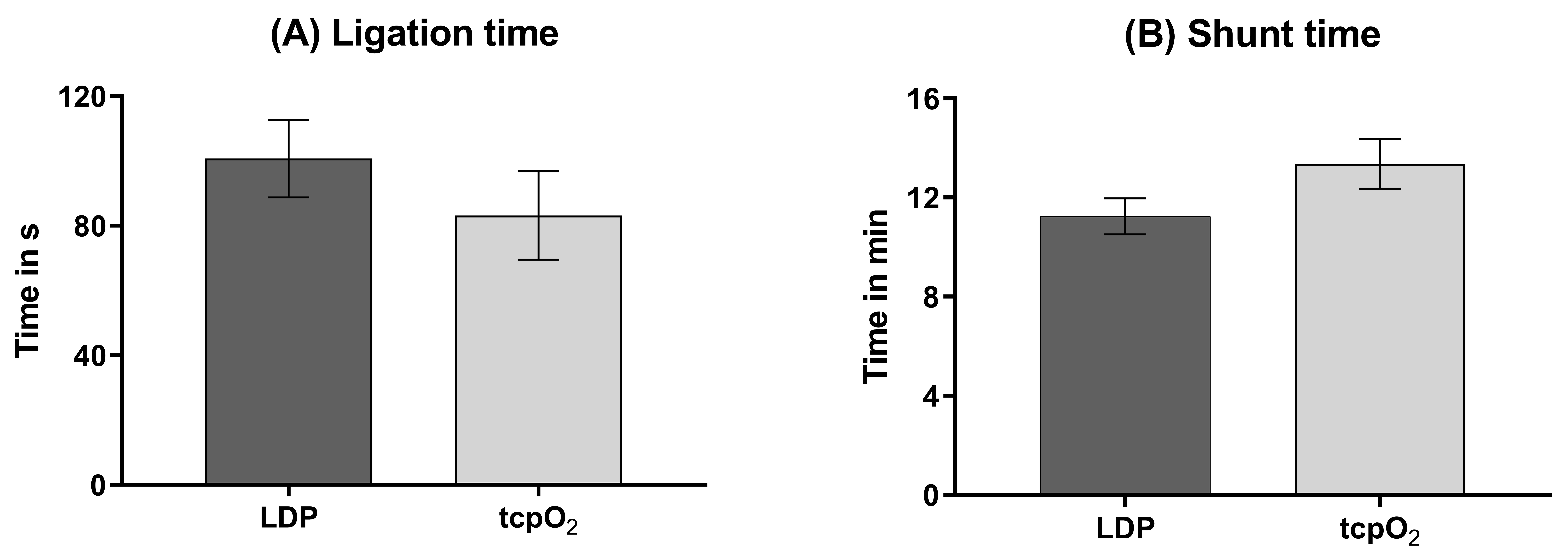 Fig. 3.
Fig. 3.Critical periods. (A) Ligation time. (B) Shunt time. N (LDP) = 17. N (tcpO
 Fig. 4.
Fig. 4.Peripheral microcirculation during OPCAB. (A) Cutaneous LDP. (B) Transcutaneous pO
In one pig, hemodynamics (Fig. 4) could not have been monitored during cLDP
measurement due to technical failure of the monitoring system. Systolic,
diastolic, and mean arterial blood pressure did not significantly change
throughout the evaluation period of peripheral perfusion by both cLDP (Fig. 5)
and tcpO
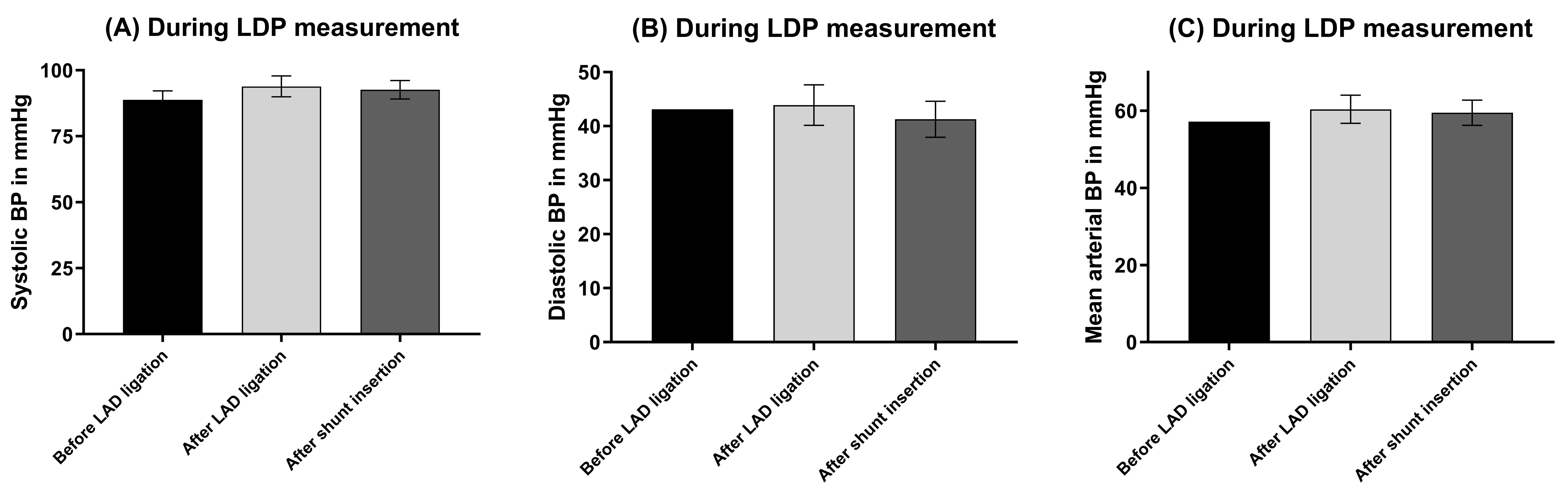 Fig. 5.
Fig. 5.Hemodynamics during LDP measurement. (A) Systolic blood pressure. (B) Diastolic blood pressure. (C) Mean arterial blood pressure. No significant differences between groups. N = 16. BP, blood pressure; LDP, Laser Doppler Perfusion; LAD, left anterior descending coronary artery; N, number of animals.
 Fig. 6.
Fig. 6.Hemodynamics during tcpO
In the LDP group in N = 17 pigs (100%), no catecholamines were administered
during the observation of peripheral perfusion. During tcpO
Both measurement technologies indicated a significantly improved peripheral microcirculation by inserting a temporary shunt into the LAD. Total ligation of the LAD leads to temporal ischemia of the myocardium, as shown in a study based on surrogate parameters by Takami et al. [6]. Myocardial ischemia leads to myocardial dysfunction [3] and consequently to a decreased perfusion of the whole body. Arterial blood pressure was kept constant during LAD ligation by vasoconstrictive medication. This indicates that responsive and vigilant anesthesia management can keep hemodynamics constant during OPCAB.
Nevertheless, this does not prevent peripheral circulation instability and thus
confirms our hypothesis that global circulation is not stable during OPCAB even
under stable arterial blood pressure. In the present work, peripheral perfusion
seems downregulated to maintain circulation in central body parts and the heart,
resulting in partial peripheral malperfusion. As the insertion of an
intracoronary shunt can at least partially re-establish the myocardial blood flow
[6], circulation in the periphery was also re-established analogously. The
reduced circulation led to an oxygen debt in peripheral body parts, as shown by
tcpO
Except for one pig, no catecholamine administration was necessary to keep blood
pressure constant during ligation and shunt insertion. The propofol infusion was
also not changed during the procedure. Therefore, we conclude that external
catecholamine administration did not overlay the actual effects in the peripheral
microcirculation, leading to an artificially reduced LDP and tcpO
Another important factor that might impact the results is the surgeon and the respective duration to finish the anastomoses. However, the same experienced cardiac surgeon performed all anastomosis during this project.
Another method to monitor microvascular circulation, tested in cardiac surgical
patients, is camera-based photoplethysmography [7]. This technology is less well
established in a clinical setting, by far more space-consuming than LDP or
tcpO
An alternative to the continuous observation of LDP is moderate local heating of the skin by special thermostatic LDP probes to verify the thermal reactivity of cutaneous microvasculature [9]. A third but rarely applied method is investigating the local effect of acetylcholine or sodium nitroprusside on cutaneous microcirculation [10]. Both heat and pharmacological activation demand a more extended period to build up an effect or subside than the ligation time or shunt time. Consequently, they are inapplicable to evaluating cutaneous perfusion during OPCAB.
A permanent monitoring of LDP and tcpO
As known from a clinical setting of LDPM on patients, cutaneous microcirculation is measured on the finger [4], forearm [9], forehead [9, 11], or foot [12]. These areas of the skin appear different and tougher in a pig already by macroscopic inspection compared to human skin. Therefore, we decided to choose the inside of the left ear to place probes. All medication was administered through a vein of the other ear to prevent the immediate effect on local microvascular circulation, which could have occurred from anesthetics, analgesics, or vasoconstrictive agents.
Monitoring cLDP and tcpO
A larger series on tcpO
Evaluation of peripheral microcirculation by cLDP and tcpO
AUC, area under the curve; CABG, coronary artery bypass grafting; cLDP,
cutaneous microcirculation; CPB, cardiopulmonary bypass; LAD, left anterior
descending coronary artery; LDPM, Laser Doppler Perfusion Monitoring; OPCAB,
off-pump coronary artery bypass grafting; r-cLDP, relative cutaneous Laser
Doppler Perfusion; r-tcpO
The datasets used and/or analyzed during the current study are available from the corresponding author on reasonable request.
LS and GV designed the study. LS, AZ, JS and GV performed the study. LS performed the statistical analysis and wrote the manuscript. FH, AZ, JS, SKI, MK, FW, AS and GS were involved in conceptualization and performed critical review of the manuscript. GV supervised the project and critically reviewed the manuscript. SKI and MK provided facilities. All authors read and approved the final manuscript. All authors have participated sufficiently in the work and agreed to be accountable for all aspects of the work.
The local Ethical Committee for Animal Experimentation (Regierungspräsendium Karlsruhe) reviewed and approved the investigations. The ethics number is G-20718.
We kindly thank Patrizia Kraft for sharing her broad experience and technical assistance.
This research received no external funding.
The authors declare no conflict of interest.
Publisher’s Note: IMR Press stays neutral with regard to jurisdictional claims in published maps and institutional affiliations.
