1 Department of Obstetrics and Gynecology, Shimane University Faculty of Medicine, 6938501 Izumo, Shimane, Japan
2 Department of Obstetrics and Gynecology, Nagoya City University East Medical Center, 4648547 Nagoya, Aichi, Japan
3 Department of Legal Medicine, Shimane University Faculty of Medicine, 6938501 Izumo, Shimane, Japan
Abstract
Background: This study aimed to compare the oncologic and surgical
outcomes of patients treated with robot-assisted modified radical hysterectomy
(RAMRH) and total laparoscopic modified radical hysterectomy (TLMRH) for
endometrial cancer (EC) with those of patients treated with abdominal modified
radical hysterectomy (AMRH). Methods: We performed a retrospective
analysis of 133 patients with early-stage EC who underwent different surgical
approaches (RAMRH, n = 14; TLMRH, n = 94; AMRH, n = 25) between 2018 and 2021 at
Shimane University Hospital. The data on clinical outcomes, including estimated
blood loss, duration of surgery, duration of hospital stay, and number of
dissected lymph nodes were collected from the patients’ electronic medical
records. Kaplan–Meier curves were used to plot survival data, and log-rank tests
were used to determine the statistical significance of differences in survival
rates. Results: RAMRH showed the lowest bleeding volume (RAMRH: 95
Keywords
- robotic surgery
- hysterectomy
- endometrial cancer
- laparoscopic surgery
Endometrial cancer (EC) is the fifth most common gynecological cancer in developed countries with an estimated global incidence of 417,367 [1, 2]. The number of patients with EC in Japan has increased, according to a report from the Japan Society of Obstetrics and Gynecology [2]. Most patients with EC are diagnosed at an early-stage; therefore, their prognosis is generally favorable. A Danish nationwide survey of EC patients with stage-I tumors reported 5-year and 10-year disease-specific survival rates of 99% and 98%, respectively [3]. However, recurrent EC is generally incurable.
The standard treatment for EC involves total abdominal hysterectomy and bilateral salpingo-oophorectomy (TAH + BSO) with or without lymphadenectomy [4]. Technological advances continue to revolutionize the surgical treatment of gynecological conditions. The utilization of minimally invasive surgery (MIS) for EC have increased from 9.3% in 2006 to 61.7% in 2011 worldwide [5]. Total laparoscopic hysterectomy (TLH) was first reported as an MIS for EC in the 1990s [6]. Multiple randomized trials and meta-analyses have shown that the laparoscopic approach has advantages over traditional open hysterectomy, including fewer complications, shorter hospital stays, accelerated recovery, improved quality of life, similar survival rates, and lower cost [7, 8, 9, 10, 11, 12, 13]. However, the laparoscopic approach can be challenging in the highest strata of obese patients due to limited exposure and cardiopulmonary compromise while in Trendelenburg position [14, 15].
Robot-assisted surgery (RAS) is an alternative to increase access to MIS. The use of robotic surgery has increased substantially since its approval by the Federal Drug Administration in 2005 [16]. Despite concerns regarding increased costs, RAS has the potential to overcome the challenges associated with laparoscopy. In morbidly obese patients, who present a significant challenge to laparoscopic and open surgeries, RAS has the potential to decrease postoperative complications [17]. In addition, it may be beneficial in elderly patients with EC who may not be able to tolerate the steep Trendelenburg position because of their comorbidities. These demands are lower in RAS [18, 19, 20]. This is encouraging as, till date, no clear difference in survival has been observed on comparison of RAS and TLH in EC patients [21].
The advantages of RAS over TLH are attributed to the engineering of the robotic system that allows for higher wrist mobility, thus allowing the surgeon to execute more complex tasks, such as delicate tissue dissection and intracorporeal knot tying [22, 23]. Previous studies have found that MIS and open hysterectomy do not differ in terms of intraoperative and postoperative complications [24]. Treatment of EC using a MIS approach provides benefits to the patient; however, there are currently few studies comparing RAS with TLH or TAH in Japan.
The aim of our study was to investigate the surgical outcomes of robot-assisted modified radical hysterectomy (RAMRH) in terms of duration of surgery, bleeding volume, intraoperative complications, number of removed lymph nodes, and postoperative hospital stay, and to compare them retrospectively with those of total laparoscopic modified radical hysterectomy (TLMRH) and abdominal modified radical hysterectomy (AMRH) in patients with EC. The usefulness of robotic surgery was also examined.
This study included 133 patients diagnosed with International Federation of Gynecology and Obstetrics stage-I EC at the Obstetrics and Gynecology Department of Shimane University Hospital. This study was approved by the Institutional Ethics and Research Review Board of Shimane University (IRB No. 20191120-1). This study was a retrospective review and the patients could opt out at any time from the study using the opt-out option on the hospital’s website.
All enrolled women underwent preoperative radiological assessment (pelvic magnetic resonance imaging or abdominopelvic computed tomography) and endometrial biopsy. Between January 2014 and August 2021, a total of 133 patients who underwent surgery for EC were included in this study, including 94 who underwent TLMRH, 14 RAMRH, and 25 AMRH. The clinicopathological characteristics of each surgical group are summarized in Table 1. In this experiment, all patients were enrolled, and there were no exclusion criteria. Ninety-nine patients (60%–78.7% in each surgical group) underwent pelvic lymphadenectomy (Table 2). In both RAMRH and TLMRH groups, a uterine manipulator for hysterectomy was used in almost 80% of the patients.
| AMRH | TLMRH | RAMRH | p (AMRH/TLMRH) | p (AMRH/RAMRH) | p (TLMRH/RAMRH) | ||
| n = 25 | n = 94 | n = 14 | |||||
| Age, years | 58.50 |
61.48 |
60.86 |
0.611 | 0.660 | 0.916 | |
| BMI, kg/m |
27.52 |
25.25 |
25.08 |
0.141 | 0.308 | 0.928 | |
| FIGO stage, n (%) | |||||||
| IA | 21 (84.0) | 81 (86.2) | 12 (85.7) | ||||
| IB | 4 (16.0) | 13 (13.8) | 2 (14.3) | ||||
| Histology, n (%) | |||||||
| Endometrioid carcinoma | 18 (72.0) | 78 (83.0) | 12 (85.7) | ||||
| Mucinous carcinoma | 2 (8.0) | 0 (0.0) | 1 (7.1) | ||||
| Serous carcinoma | 3(12.0) | 11 (11.7) | 0 (0.0) | ||||
| Clear cell carcinoma | 1 (4.0) | 2 (2.1) | 0 (0.0) | ||||
| Carcinosarcoma | 1 (4.0) | 1 (1.1) | 1 (7.1) | ||||
| Dedifferentiated carcinoma | 0 (0.0) | 2 (2.1) | 0 (0.0) | ||||
| Metastasis, n (%) | |||||||
| Pelvic lymphnode, n (%) | 1 (4.0) | 1 (1.1) | 0 (0.0) | ||||
| Lymphovascular space invasion, n (%) | 6 (24.0) | 34 (36.2) | 1 (7.1) | ||||
RAMRH, robot-assisted modified radical hysterectomy; TLMRH, total laparoscopic modified radical hysterectomy; AMRH, abdominal modified radical hysterectomy; BMI, body mass index; FIGO, International Federation of Gynecology and Obstetrics.
| AMRH | TLMRH | RAMRH | p (AMRH/TLMRH) | p (AMRH/RAMRH) | p (TLMRH/RAMRH) | ||
| n = 25 | n = 94 | n = 14 | |||||
| Operative time, min | 250.64 |
245.81 |
264.00 |
0.777 | 0.618 | 0.412 | |
| Estimated blood loss, mL | 482.60 |
140.74 |
95.0 |
0.001 | 0.002 | 0.342 | |
| Hospitalization, days | 9.88 |
7.32 |
6.43 |
0.333 | |||
| Blood transfusion, n (%) | 2 (8.0) | 0 | 1 (7.1) | ||||
| Lymph nodes disection, n (%) | 15 (60.0) | 74 (78.7) | 10 (71.4) | ||||
| Lymph nodes counted, n | 29.80 |
37.38 |
34.10 |
0.027 | 0.303 | 0.575 | |
| Conversion to laparotomy, n (%) | 0 | 0 | |||||
| Follow-up visit result | |||||||
| No relapse | 24 (96.0) | 92 (97.9) | 14 | ||||
| Relapse | 1 (4.0) | 2 (2.1) | 0 | ||||
| Death | 0 | 2 (2.1) | 0 | ||||
| Complications injury | 1 (4.0) | 3 (3.2) | 0 | ||||
RAMRH, robot-assisted modified radical hysterectomy; TLMRH, total laparoscopic modified radical hysterectomy; AMRH, abdominal modified radical hysterectomy.
All procedures were performed by two experienced gynecological oncologists who were appropriately trained and mentored in robotic surgery and were supported by a trained robotic surgery team. Data on age, body mass index (BMI), advanced stage, myometrium infiltration, lymph node metastasis, lymphovascular space invasion, surgery type and timing, blood loss, hospital status, and postoperative complications were collected and compared between TLMRH (94 cases) and AMRH (25 cases) performed by the same team. The data were collected retrospectively from the electronic databases of our hospital. Operative time was defined as the time from incision to skin closure. Operative time in RAS was defined as the console time. Hospital stay was calculated in hours from admission to discharge and subsequently converted to days. Intraoperative complications were defined as bowel, bladder, ureter, nerve, or vascular injuries.
The data were compared among the three groups using student’s t-test
and Mann-Whitney U test for parametric and non-parametric variables,
respectively. Differences between proportions were compared using Fisher’s exact
test or
A comparison of three consecutive case series is presented in Table 1. The mean
age and BMI of the AMRH, TLMRH, and RAMRH groups were 58.5, 61.4, and 60.8 years
and 27.5, 25.2, and 25.0 kg/m
The surgical outcomes of RAMRH, TLMRH, and AMRH are summarized in Table 2.
Although no significant difference was observed in the duration of surgery
between the three groups (RAMRH: 264
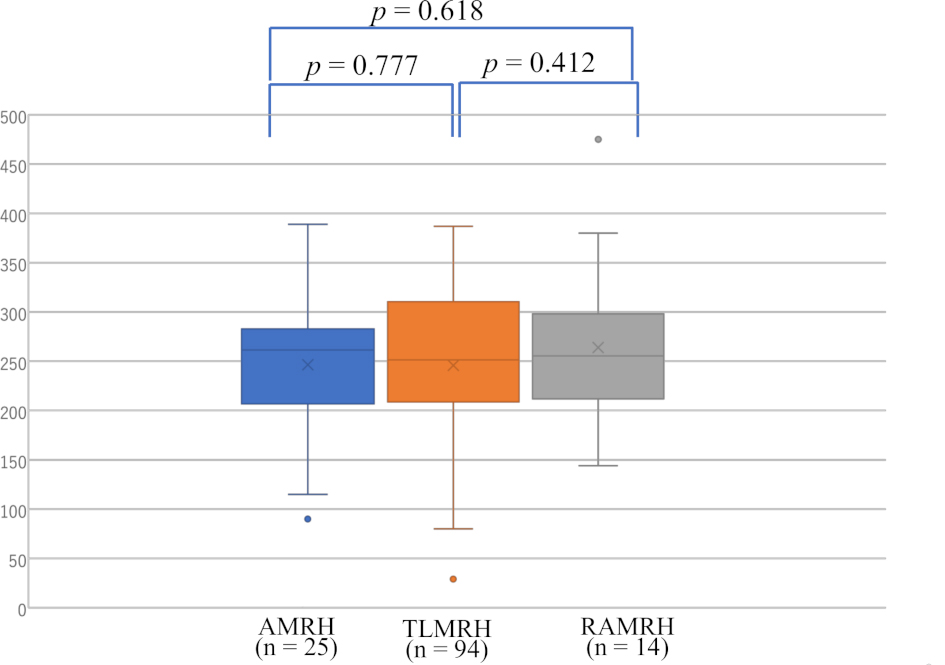 Fig. 1.
Fig. 1.Duration of surgery in patients with endometrial cancer operated by RAMRH, TLMRH, and AMRH.
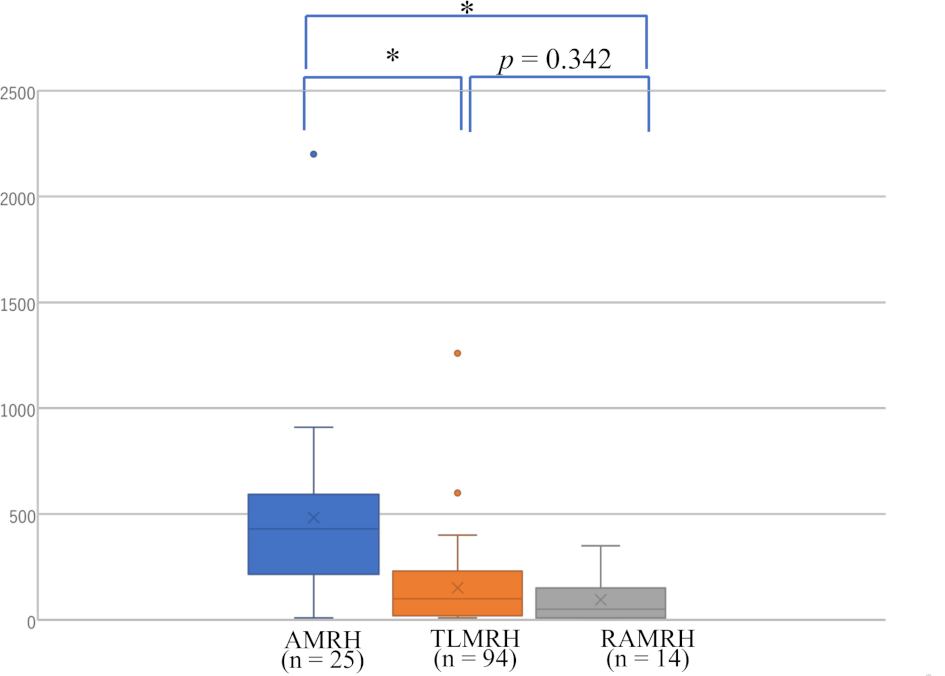 Fig. 2.
Fig. 2.Bleeding volume in patients with endometrial cancer operated by
RAMRH, TLMRH, and AMRH. * p
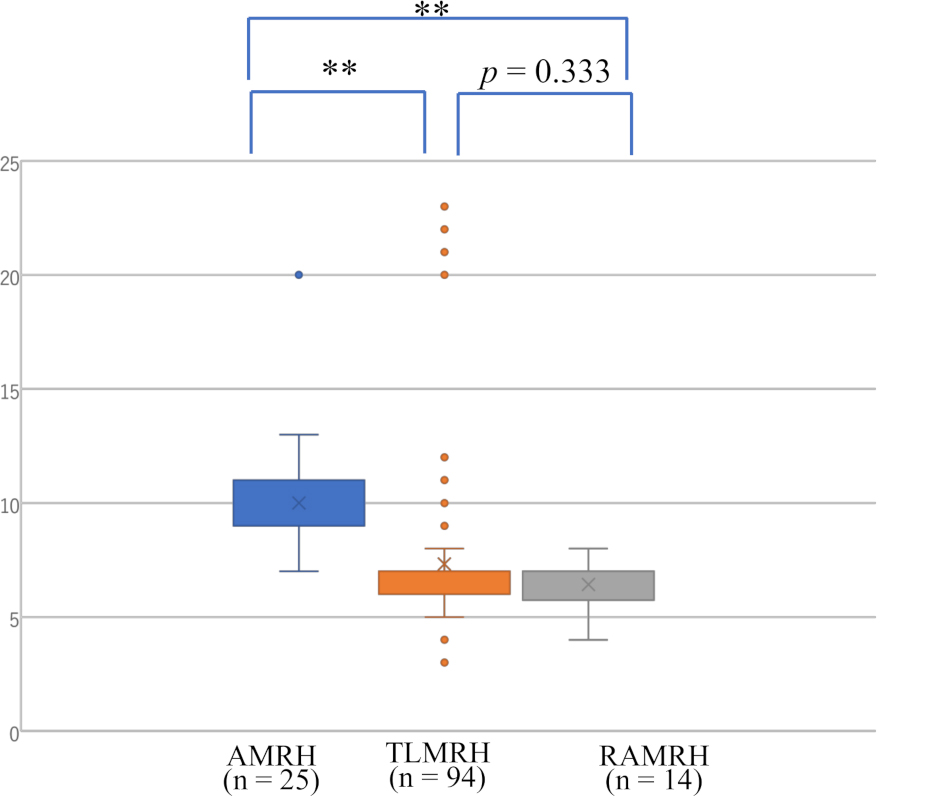 Fig. 3.
Fig. 3.Postoperative duration of hospital stays in patients with
endometrial cancer operated by RAMRH, TLMRH, and AMRH. ** p
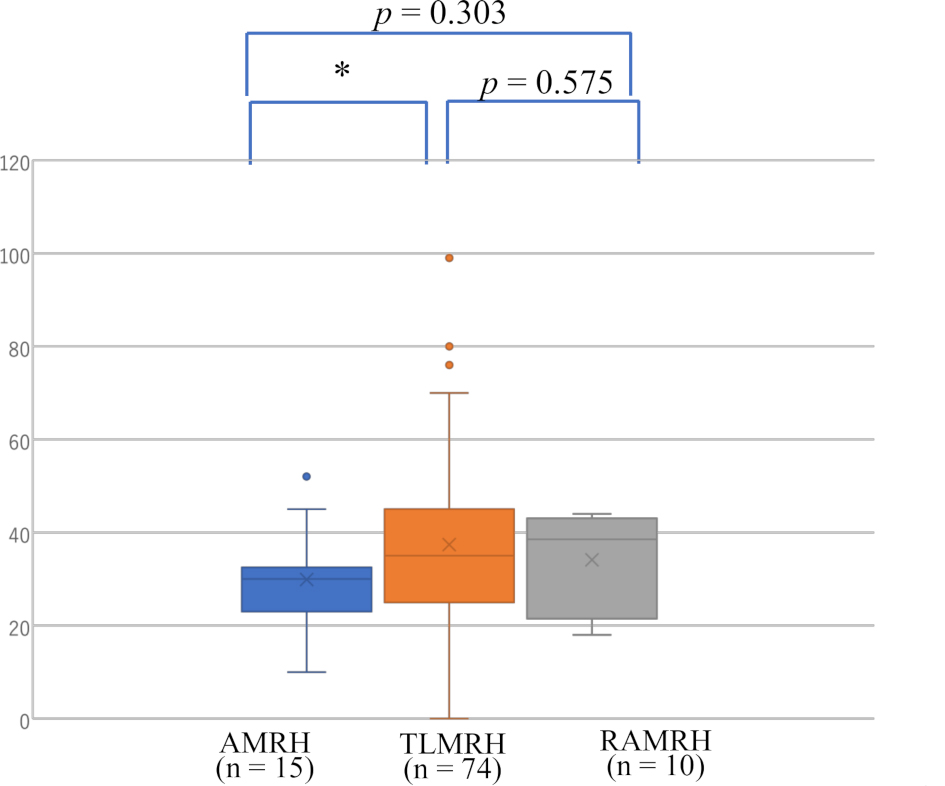 Fig. 4.
Fig. 4.Number of removed lymph nodes in patients with endometrial
cancer operated by RAMRH, TLMRH, and AMRH. * p
We examined the prognostic outcomes of each surgical procedure. There was no significant difference between the different surgical procedures in terms of PFS (AMRH vs. TLMRH, p = 0.609; AMRH vs. RAMRH, p = 0.454; TLMRH vs. RAMRH, p = 0.598) or OS (AMRH vs. TLMRH, p = 0.451; AMRH vs. RAMRH, p = not significant (NS); TLMRH vs. RAMRH, p = 0.585) (Fig. 5).
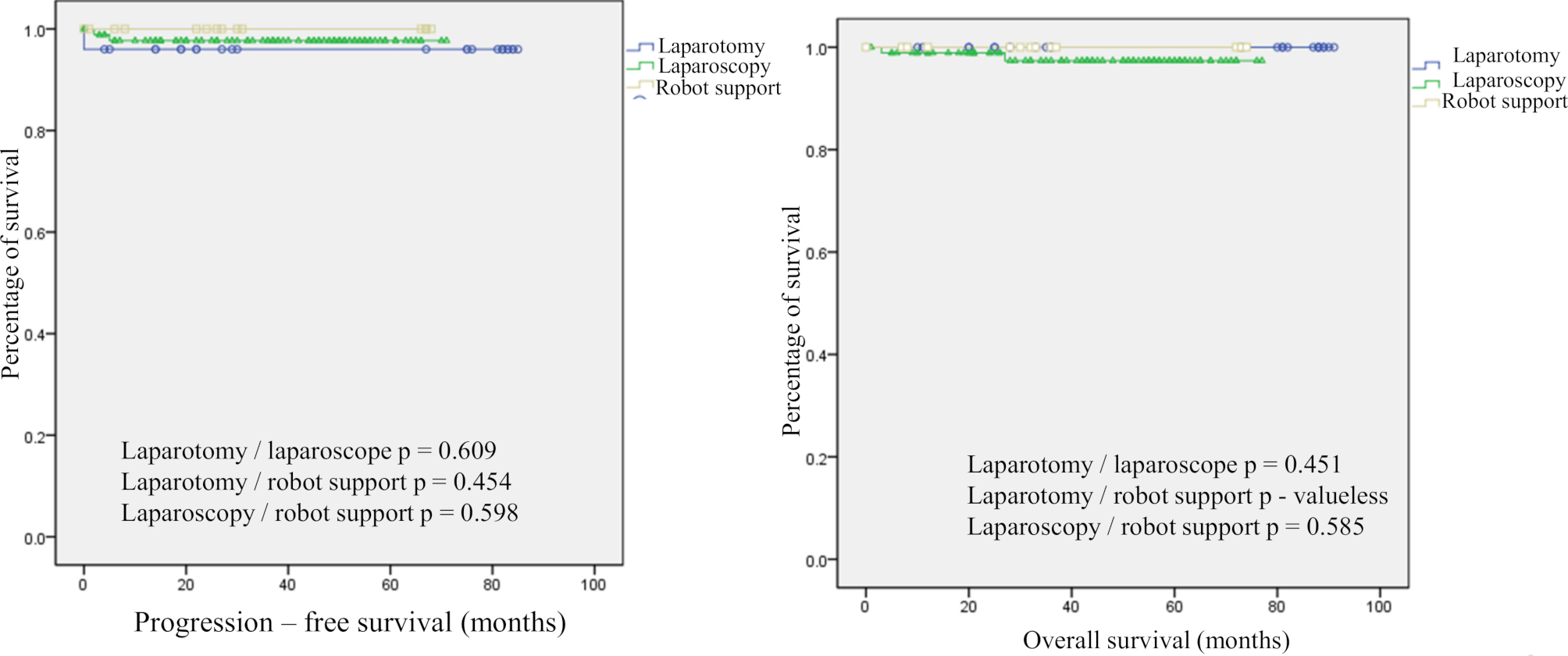 Fig. 5.
Fig. 5.Prognostic outcome of patients with endometrial cancer operated by RAMRH, TLMRH, and AMRH.
EC is diagnosed in its early stages in most of the patients, and the demand for minimally invasive approaches has recently been increasing worldwide due to its benefits to the patients. Many studies have shown that MIS has a favorable prognosis for early-stage EC [25]; however, some of them have faced challenges and been restricted by some limitations [26]. In Japan, RAS was developed to overcome the limitations of TLH and has been used in gynecological surgery for malignancies since 2009 as clinical trial. Furthermore, RAS for uterine corpus carcinomas has been covered by insurance since April 2018. Additionally, a few randomized controlled trials have assessed the clinical outcomes of robotic surgery for gynecological malignancies [27]. Our study assessed the surgical outcomes and comprehensive results of RAMRH, evaluated its usefulness and safety in patients diagnosed with early-stage EC, and compared it with TLMRH and AMRH retrospectively. This study provides a basis for the selection of an optimal surgical method, together with the actual role of RAS as an MIS in early-stage EC.
In the current study, both RAMRH and TLMRH showed patient outcomes similar to those of AMRH, without an increase in intraoperative complications. In detail, both MIS groups (RAMRH and TLMRH) were associated with the least estimated blood loss and shorter hospital stays than those of the AMRH group. In the MIS group, estimated blood loss and duration of hospital stay did not differ significantly between the RAMRH and TLMRH groups. Our results for estimated blood loss of the RAMRH group were within the range reported in previous studies (43.6–166.0 mL) [24, 28], although our hospital stays were longer compared to those stated in previous studies (1–2.5 days) [25, 26, 29]. Previous reports have shown that MIS (RAMRH, TMRAH) have less blood loss and shorter hospital stay duration compared with treatment comprising an AMRH [30]. Our findings were similar to this cited study. MIS (RAMRH, TMRAH) involve making smaller incision compared to the large incision required in AMRH. This results in less tissue trauma and reduced blood vessel disruption, leading to decreased blood loss. Furthermore, MIS (RAMRH, TMRAH) provide surgeons with high-definition imaging systems that offer magnified and clear views of the surgical site. This enhanced visualization allows for precise and meticulous surgery, reducing the risk of unintentional damage to blood vessels and surrounding tissues. This helps minimize blood loss during the procedure. Smaller incisions and reduced tissue trauma contribute to faster healing and recovery. Patients undergoing minimally invasive surgery typically experience less postoperative pain and can resume normal activities sooner than those undergoing open surgery. The combination of smaller incisions, reduced blood loss, and faster recovery allows patients to leave the hospital sooner [31, 32].
The mean duration of surgery did not differ significantly among the three
groups. These findings are similar to those of recently published meta-analysis
[33] and systematic review [34]. No statistically significant differences were
found in the number of dissected lymph nodes for any surgical procedure. Besides,
the mean number of dissected lymph nodes was 34
The knowledge on quality of life during the postoperative recovery period is important for healthcare providers to provide adequate preventive measures, information, and follow-ups. Previous studies compared the quality of life of patients with different surgical techniques and found that the type of surgery affected the quality of life by multivariate linear regression analysis; for example, patients who underwent robotic surgery had better physical and mental quality of life due to lower pain levels and early ambulation after surgery than patients who underwent laparoscopic surgery or laparotomy for both benign and malignant diseases [16]. Sarlos et al. [39] also reported a better quality of life in patients who underwent robotic surgery for benign gynecologic disorders than that in those who underwent laparoscopic surgery. In this study, we examined the relationship between different surgical approaches and prognosis. Although the number of cases was small, the different surgical approaches did not correlate with PFS and OS. As PFS and OS do not depend on surgical approaches, the above discussion, including our prognostic results, may suggest that RAS procedures could be the recommended treatment for patients with EC.
Robot-assisted surgery is designed to be safe with fewer complications. Robotic systems provide surgeons with enhanced precision and accuracy [40]. The robotic arms can make smaller and more controlled movements than the human hand. This can be particularly advantageous in delicate procedures or when working in confined spaces [22, 23]. The robot helps surgeons see better and makes their movements steady, reducing the chances of mistakes. The advanced technology also lets surgeons work with smaller cuts, causing less harm to the body. This kind of surgery is usually quicker to recover from, increased patient quality of life and decreased surgical complication [41]. Moreover, the learning curve for RAS is shorter than that of other approaches, and the surgeon is likely to perceive less fatigue because of the ergonomic design of the surgical system. Owing to its accuracy and reduced fatigue, RAS may continue to expand the field of gynecological malignancies, including uterine cancer.
Robotic surgery has been used in the past with good results, especially in obese patients, but the high cost is a problem. Recently, v-notes (vaginal natural orifice transluminal endoscopic surgery), which is more accessible in obese patients, has begun to be reported. The present study compared the results of abdominal robotic-assisted total hysterectomy with those of other surgical methods. It is recommended that v-notes surgery also be compared with other surgical methods for its usefulness, especially in obese patients [42].
The present study has several limitations. First, it was conducted at a single institution; therefore, the number of cases was small. Second, the estimated blood loss and duration of hospitalization have been shown to be significantly better in MIS than those in open surgery, although the outcome measurement of patients after robotic surgery has been explored in only a limited number of studies. Therefore, concrete conclusions could not be drawn. Hence, further investigation with larger study populations is required.
Our findings suggest that RAMRH could serve as a viable treatment alternative to both TLMRH and AMRH for individuals diagnosed with EC. Notably, the surgical outcomes of RAMRH, including factors such as bleeding volume, duration of hospital stay, and the extent of lymph node dissection, demonstrate favorable results. The current study also indicated that MIS including RAMRH may be safe, feasible, innovative, and an alternative to AMRH for patients with EC, although the evaluation of MIS is controversial for previous studies [43].
Our results indicate that RAMRH could be an alternative treatment option to TLMRH and AMRH for patients with EC. In this context, the surgical outcomes of RAMRH, in terms of bleeding volume, duration of hospital stay, and lymph node dissection, were favorable. Furthermore, there was no significant difference in prognosis between the three surgical procedures. In the future, it might be necessary to determine the group of patients with most benefits of MIS.
The data presented in this study are available upon request from the corresponding author (KN).
MI, SR, and KN drafted the manuscript. SR, HY, MI, TI, KK, and SS collected data and performed statistical analysis. KN, SK were involved design, planning, conduct, revising critically the manuscript for important. All authors contributed to editorial changes in the manuscript. All authors read and approved the final manuscript. All authors have participated sufficiently in the work and agreed to be accountable for all aspects of the work.
This study protocol was approved by the institutional ethics and research review boards at Shimane University (IRB No.20191120-1). The requirement for individual consent for this retrospective analysis was waived. Patients could opt out at any moment from the study using the opt out option on the hospital’s website.
We thank all the peer reviewers for their opinions and suggestions.
This research received no external funding.
The authors declare no conflict of interest. Kentaro Nakayama is serving as one of the Guest editors of this journal. We declare that Kentaro Nakayama had no involvement in the peer review of this article and has no access to information regarding its peer review. Full responsibility for the editorial process for this article was delegated to Michael H. Dahan.
References
Publisher’s Note: IMR Press stays neutral with regard to jurisdictional claims in published maps and institutional affiliations.





