1 Department of Obstetrics & Gynecology, Boonshoft School of Medicine, Wright State University, OH 45409 Dayton, USA
Abstract
Background: The optimal management of patients diagnosed in the
mid-gestation with a low-lying placenta (LLP) is controversial. We sought to
determine the rate of adverse pregnancy outcomes with an initial diagnosis of
LLP, and whether this was dependent on a follow up sonographic diagnosis of
resolution or the initial placenta-to-internal os distance (P-IOD).
Methods: A retrospective cross-sectional study of singleton pregnancies
with a sonographically diagnosed LLP between 18–24 weeks’ gestation (12/2010 to
7/2018) was conducted at a tertiary referral center in the U.S. Follow-up
ultrasound examinations from the late second or early third trimester were
reviewed. Maternal morbidity associated with blood loss, regardless of resolution
of LLP was recorded and stratified by P-IOD at
diagnosis. The LLP was considered resolved if the P-IOD was
Keywords
- low lying placenta
- hemorrhage
- resolution
- morbidity
Placental related pregnancy complications such as obstetrical hemorrhage are common etiologies of global maternal and neonatal morbidity, mortality, and near misses. The reported incidence of a low-lying placenta (LLP) at 18–20 weeks’ gestation is 1–9% in developed nations where second trimester ultrasound is routinely practiced [1, 2]. Despite the high incidence, data regarding clinical implications of LLP in mid-gestation have been scarce and conflicting. Additionally, the term “low-lying placenta” has historically been used interchangeably with “marginal placenta previa”, which has further complicated management guidelines [3, 4, 5]. The dearth of generalizable and reproducible evidence has led to controversy in the optimal approach to management of LLP.
Vintzileos in an expert opinion in 2015 proposed guidelines for management
of LLPs diagnosed in mid gestation [3]. A repeat transvaginal
ultrasound was recommended at 28–32 weeks’ gestation. If the placental-internal
os distance (P-IOD) was
Several studies have demonstrated that the vast majority, 95–99.5%, of
strictly defined LLPs (distal placental edge
There also continues to be concern regarding morbidity and adverse outcomes associated with LLP. There have been few studies looking at the finding of a mid-gestation LLP as an independent risk factor for adverse outcomes, which have shown that the most significant concern is increased blood loss or postpartum hemorrhage [9, 10, 13, 14, 15]. Interestingly, even in the setting of a persistent LLP, the mode of delivery does not appear to affect the rate of postpartum hemorrhage or blood loss [6, 13, 16]. The objective of this study was to determine if an initial diagnosis of LLP affected the rate of adverse pregnancy outcomes and to determine the rate of LLP resolution.
This is a retrospective cross sectional study of patients with singleton pregnancies with a sonographically diagnosed LLP between 18 w 0 d and 24 w 0 d gestation from an American Institute of Ultrasound in Medicine (AIUM) accredited single institution, from December 2010 through July 2018. The hospital is a tertiary referral center located in the Midwest United States, with approximately 4500 annual deliveries during the study period. Obstetrical care is provided by private attending obstetricians, midwifes, faculty attending physicians and resident physicians. All ultrasounds were performed by sonographers with American Registry for Diagnostic Medical Sonography (ADRMS) registration in obstetrical ultrasound and read by one of six board-certified Maternal-Fetal Medicine specialists. The ultrasound equipment consisted of General Electric Voluson E8 (GE Healthcare, Chicago, IL, USA) and Siemens S2000 (Siemens Healthcare, Erlangen, Germany). Inclusion criteria were all singleton pregnancies with a diagnosed LLP between 18–24 weeks’ gestation. Exclusion criteria consisted of multiple gestations, major congenital anomalies, placenta previa, vasa previa, suspected morbidly adherent placenta, known maternal coagulopathy, intrauterine fetal death, inability to clearly image the inferior placental edge or internal cervical os on transabdominal ultrasound and declined transvaginal ultrasound, and women who did not deliver at our institution.
In accordance with AIUM and ACOG guidelines, the placental location, appearance, and relationship to the internal cervical os were recorded on digital media [17]. The placental location was determined by transabdominal ultrasound (TAUS) in the absence of a lower uterine segment contraction defined as a transient focal thickening of the myometrium. The cervix was identified in the mid-sagittal plane by locating the echolucent or echodense endocervical canal and the proximal internal cervical os. If the inferior edge of the placenta was unable to be clearly visualized, or if the internal cervical os could not be identified, transvaginal ultrasound (TVUS) was then performed with an empty bladder. The P-IOD was measured from the inferior placental edge to the internal cervical os. LLP was diagnosed when the inferior placental edge was less than 2.0 cm from the internal cervical os, but not overlying the cervical os. The cervical length was measured in all cases.
Patients with the diagnosis of LLP had a follow-up ultrasound scheduled at 28–32 weeks. The placental location and LLP were assessed earlier if a repeat ultrasound was performed for an alternative indication, or later if one was not performed at the recommended gestational age.
The stored digital images from all ultrasounds were reviewed by a single author (BLC). The patients were divided into three groups based upon the resolution outcome at the follow-up ultrasound (Fig. 1).
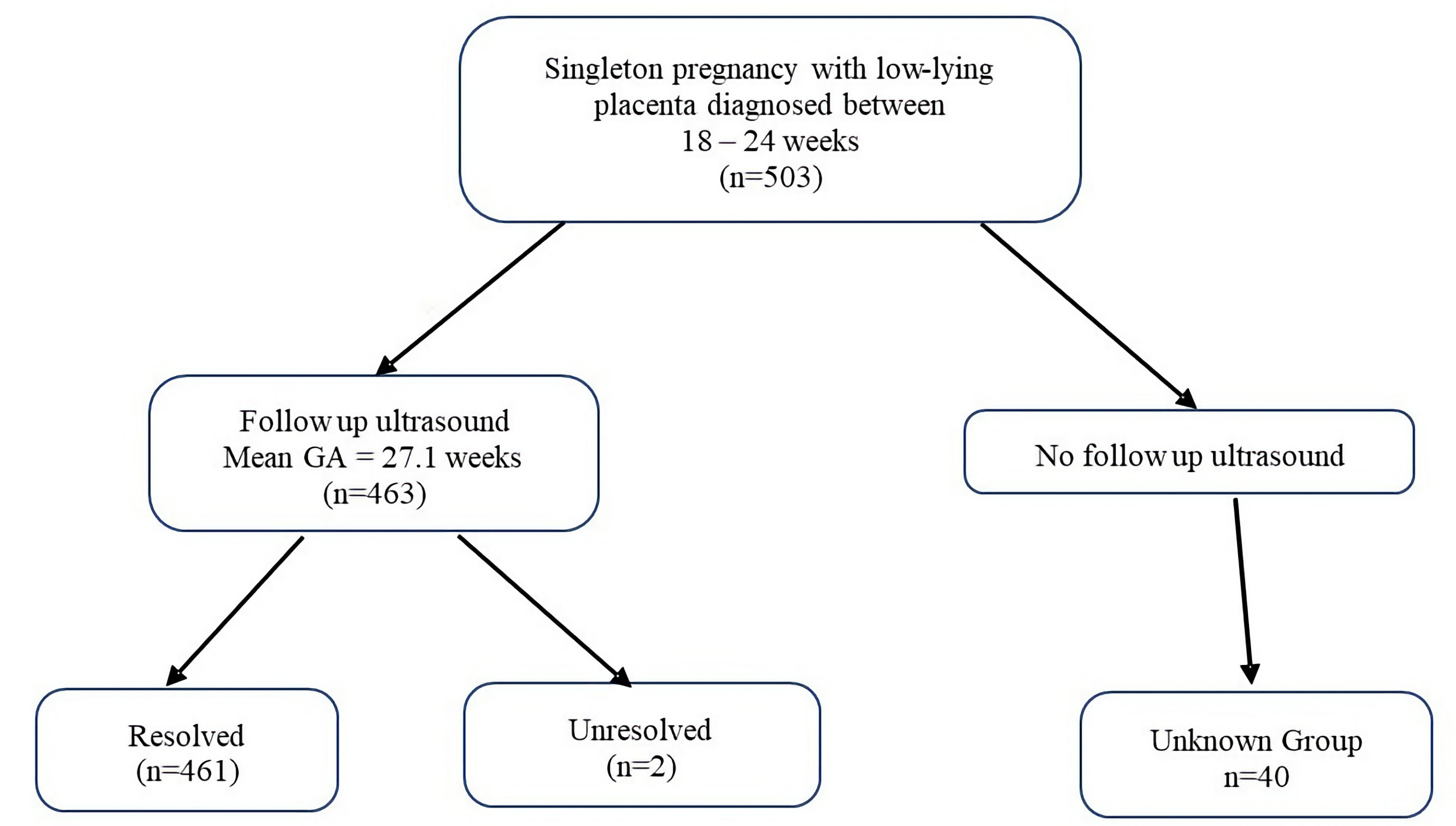 Fig. 1.
Fig. 1.Groupings based upon resolution outcome at follow-up ultrasound. If the placenta-to-internal os distance (P-IOD) was 2.0 cm or greater on any subsequent ultrasound, the low-lying placenta (LLP) was considered resolved (n = 461) and no further investigation was recommended. The second group, “unknown resolution” (n = 40), was when the P-IOD was less than 2.0 cm at the initial ultrasound and did not have a follow up ultrasound. The third group, “unresolved” (n = 2), was when the P-IOD was less than 2.0 cm at 34 weeks’ or later. Patients with unknown resolution were excluded from the analysis of the resolution rate, though were included in overall outcome analyses. GA, gestational age.
All deliveries were performed at a single institution in Dayton, OH, USA, a regional
perinatal tertiary referral center. The ultrasound data base and electronic
medical record were used to collect demographic, placental and delivery data.
Parity was counted for deliveries that occurred at
Morbidity from blood loss was described by the following characteristics:
postpartum hemorrhage (PPH) defined as estimated blood loss (EBL)
Statistical analyses consisted of comparing categorical variables via
Chi-squared test, and continuous variables using Student t-test and
analysis of variance (ANOVA). A p value of
Five hundred three patients meeting the inclusion criteria were found to have an
LLP between 18–24 weeks’ gestation. For the entire sample, the mean maternal age was
29.4
| Initial P-IOD measurement | LLP resolution status | |||||||
| 0–0.49 cm | 0.5–0.99 cm | 1.0–2.0 cm | p value | Resolved | Unresolved | Unknown | p value | |
| (n = 40) | (n = 77) | (n = 386) | (n = 461) | (n = 2) | (n = 40) | |||
| Age (years) | 31.1 ( |
29.1 ( |
29.2 ( |
0.585 | 29.3 ( |
32.8 ( |
31.0 ( |
0.406 |
| BMI (kg/m |
29.6 ( |
29.7 ( |
30.3 ( |
0.762 | 30.2 ( |
24.0 ( |
29.7 ( |
0.167 |
| Caucasian | 29 (72.5) | 62 (80.5) | 301 (78.0) | 0.698 | 355 (77.0) | 2 (100) | 34 (85) | 0.436 |
| Posterior placenta | 23 (57.5) | 53 (68.8) | 255 (66.1) | 0.708 | 301 (65.3) | 1 (50) | 29 (72.5) | 0.996 |
| Tobacco use | 11 (27.5) | 13 (16.9) | 107 (27.7) | 0.144 | 125 (27.1) | 1 (50) | 14 (35) | 0.285 |
| Prior uterine surgery | 9 (22.5) | 16 (20.8) | 68 (17.6) | 0.619 | 80 (17.4) | 1 (50) | 11 (27.5) | 0.225 |
| Parity | 2.18 ( |
1.94 ( |
2.11 ( |
0.502 | 2.06 ( |
3.00 ( |
2.50 ( |
0.574 |
| GA at diagnosis (weeks) | 19.9 ( |
20.1 ( |
19.9 ( |
0.375 | 19.9 ( |
19.9 ( |
20.2 ( |
0.559 |
| Cervical length (cm) | 3.73 ( |
3.80 ( |
3.83 ( |
0.659 | 3.83 ( |
4.63 ( |
3.82 ( |
0.176 |
Values are mean of group (
Follow up ultrasounds were performed in 463/503 (92.0%) patients, of which 461/463 (99.6%) resolved. The average gestational age at the time of the follow up ultrasound was 27.1 weeks, which did not differ between P-IOD measurements. Given that there were only 2 unresolved patients, analysis of the unresolved group was not practical.
Out of the 503 patients evaluated, 21 (4.2%) experienced a PPH, 59 (11.7%) had
UPPH, and 13 (2.6%) required a blood transfusion. The overall mean blood loss
was 430
| Initial P-IOD measurement | LLP resolution status | |||||
| 0–0.49 cm | 0.5–0.99 cm | 1.0–2.0 cm | Resolved | Unresolved | Unknown | |
| (n = 40) | (n = 77) | (n = 386) | (n = 461) | (n = 2) | (n = 40) | |
| GA at delivery (weeks) | 38.7 ( |
38.8 ( |
38.7 ( |
38.7 ( |
39.2 ( |
38.4 ( |
| PPH | 3 (7.5) | 2 (2.6) | 16 (4.1) | 20 (4.3) | 0 | 1 (2.5) |
| UPPH | 7 (17.5) | 8 (10.3) | 44 (11.3) | 56 (12.1) | 1 (50.0) | 2 (5.0) |
| Blood transfusion | 2 (5.0) | 1 (1.3) | 10 (2.6) | 12 (2.6) | 0 | 1 (2.5) |
| Manual removal of the placenta | 2 (5.0) | 1 (1.3) | 0 | 3 (0.7) | 0 | 0 |
Values are mean of group (
There were 24/503 (4.8%) antepartum admissions for vaginal bleeding. There was
a statistically significant difference in the number of admissions for antepartum
bleeding based in the initial P-IOD, Table 3. The odds of being admitted for
antepartum bleeding was significantly greater if the P-IOD was
| Initial P-IOD measurement | LLP resolution status | |||||
| 0–0.49 cm | 0.5–0.99 cm | 1.0–2.0 cm | Resolved | Unresolved | Unknown | |
| (n = 40) | (n = 77) | (n = 386) | (n = 461) | (n = 2) | (n = 40) | |
| Antepartum admissions for bleeding | 7/40 (17.5)* | 3/77 (4.0) | 14/386 (3.6) | 22/461 (4.8) | 0/2 | 2/40 (5.0) |
| Vaginal delivery | 25/40 (62.5) | 53/77 (68.8) | 267/386 (69.2) | 319/461 (69.2) | 1/2 (50.0) | 25/40 (62.5) |
| Cesarean delivery | 15/40 (37.5) | 24/77 (31.2) | 119/386 (30.8) | 142/461 (30.8) | 1/2 (50.0) | 15/40 (37.5) |
| UA pH |
8/27 (29.6)* | 3/43 (7.0) | 21/207 (10.1) | 32/268 (11.9) | 0/2 | 0/9 |
| Neonatal Hgb |
0/6 | 1/13 (7.7) | 3/53 (5.7) | 1/71 (1.4) | 0/2 | 0/1 |
| Preterm birth | 6/40 (15.0) | 12/77 (15.6) | 40/386 (10.4) | 54/461 (11.7) | 0/2 | 4/40 (10.0) |
Values are n (%). UA pH, umbilical arterial cord pH at delivery; Hgb,
hemoglobin.
Almost all (99.6%) LLPs diagnosed at mid-gestation resolve by 34 weeks’
gestation. Regardless of resolution or the P-IOD, patients with a mid-gestation
diagnosis of LLP had higher rates of maternal morbidity related to bleeding than
what is seen in the general population (4.2% PPH, 11.7% UPPH, and 2.6% blood
transfusion). Also, when the P-IOD was
The rate of resolution is consistent with previous literature, documenting
between 95–99% [1, 2, 10, 11, 14, 18]. The rate of PPH was higher than what has
been reported based on data from the Nationwide Inpatient Sample (NIS), the
largest publicly available inpatient database in the U.S. (4.2% vs
2.9%) [19, 20, 21, 22, 23]. The postpartum transfusion rate was 2.6% which appears to be
almost two-fold the documented range of national postpartum transfusion rate (0.3%
to 1.7%) [20, 24, 25, 26]. UPPH, defined here as a change in hemoglobin from
antepartum to postpartum of
We speculate the observed higher rate of obstetrical hemorrhage and blood
transfusion, antepartum hemorrhage, and umbilical cord acidosis may have a common
etiology due to defective placental implantation and function. The lower uterine
segment is thinner, with less blood flow compared to the contractile portion of
the uterine corpus. This may be confounded when the placenta lies closer to the
internal cervical os (e.g.,
The strengths of this study include the large sample size obtained in a setting where evaluation of the placental location with respect to the cervix was the routine. As such, it was pragmatic compared to a study specifically focusing on evaluation of the placental location. For the study, all ultrasounds were reviewed by a single observer, decreasing inter-observer variability. Blood loss was quantified objectively with pre- and post-partum hemoglobin assessment, in addition to the subjective EBL documented by providers. Limitations of this study include the retrospective study design which is a lower level of evidence compared to a prospective study. Furthermore, the diagnosis of LLP and P-IOD was not universally confirmed with transvaginal ultrasound if able to be clearly visualized with transabdominal ultrasound, which may increase or decrease the diagnosis of LLP. Lastly, the ultrasounds were performed by one of several available sonographers, though all American Registry for Diagnostic Medical Sonographers (ARDMS) registered, and read by one of six Maternal-Fetal Medicine specialists, providing the opportunity for interobserver variation.
This research suggests that the presence of an LLP results in an inherent increase in maternal morbidity, which does not change despite P-IOD or resolution. In cases where both vasa previa and morbidly adherent placenta are confidently ruled out at the initial ultrasound, a follow-up ultrasound evaluation solely for LLP may be redundant. Providers may safely choose to forgo a follow up ultrasound, simply note the increased risk for maternal morbidity, and provide patients with precautions.
The datasets used and/or analyzed during the current study are available from the corresponding author on reasonable request.
BLC contributed to the conception, design, acquisition, analysis, and interpretation of data, and was involved in drafting and critically reviewing the manuscript. DSM contributed to the conception, design, interpretation of data, and was involved in drafting and critically reviewing the manuscript. RAM contributed to the design, analysis, and interpretation of data, and was involved in drafting and critically reviewing the manuscript. Each author has participated sufficiently in the work and takes responsibility for appropriate portions of the content; and agrees to be accountable for all aspects of the work in ensuring that questions related to the accuracy or integrity of any part of the work are appropriately investigated and resolved. All authors read and approved the final manuscript.
An exemption for informed consent was obtained from the institutional review board for this study since it was retrospective and only de-identified data were utilized. The Wright State University Institutional Review Board reviewed and determined this study was exempt from IRB review (WSU IRB #06611, February 18, 2019).
We would like to express our gratitude to all those who helped us during the writing of this manuscript. Thanks to all the peer reviewers for their opinions and suggestions.
This research received no external funding.
The authors declare no conflict of interest.
References
Publisher’s Note: IMR Press stays neutral with regard to jurisdictional claims in published maps and institutional affiliations.

