1 Department of Breast Surgery, Luoyang Central Hospital Affiliated to Zhengzhou University, 471000 Luoyang, Henan, China
Abstract
Background: Compared with other subtypes, triple-negative breast cancer
(TNBC) is more aggressive and has a lower survival rate with chemotherapy being
the only acknowledged systemic treatment option. Recently, PD-1/PD-L1 (programmed
cell death-1 and programmed death-ligand 1) inhibitors have demonstrated survival
benefits in locally advanced or metastatic TNBC patients. However, the effects of
PD-1/PD-L1 inhibitors in neoadjuvant chemotherapy remain controversial.
Methods: Extensive literature searches were conducted in the PubMed,
Embase and Cochrane databases. A pooled odds ratio (OR) with 95% confidence
intervals (CI) was analyzed. Results: Seven randomized controlled trials
(N = 1707) were included. PD-1/PD-L1 inhibitor chemotherapy group showed
pathological complete response (pCR) benefit of 59.0% vs. 40.4% (OR 1.98, 95%
CI 1.38–2.82, p
Keywords
- PD-1/PD-L1 inhibitors
- neoadjuvant therapy
- pathological complete remission
- triple negative breast cancer
Breast cancer remains one of the most common malignant tumors worldwide. Triple-negative breast cancer (TNBC) is a special subtype characterized by non-expression of estrogen receptor (ER), progesterone receptor (PR) and human epidermal growth factor receptor 2 (HER-2). At present, owing to the absence of approved therapeutic regimens, chemotherapy is the only accepted systemic treatment option for TNBC. In contrast with other subtypes, TNBC is associated with more aggressive tumors, higher mortality rate and lower survival rate. Accordingly, it is crucial to develop treatment plans that can alter this outcome.
Patients with breast cancer, especially TNBC, who attain pathological complete response (pCR) have greatly improved survival [1]. Therefore, seeking a higher pCR rate has become an important purpose of neoadjuvant therapy for TNBC. Recently, PD-1/PD-L1 (programmed cell death-1 and programmed death-ligand 1) inhibitors have demonstrated survival benefits in locally advanced or metastatic TNBC patients [2, 3]. As for early TNBC patients, several studies have been conducted to evaluate the impact of PD-1/PD-L1 inhibitors in addition to neoadjuvant chemotherapy. However, the results are contradictory [4, 5, 6, 7, 8, 9, 10].
We performed a systematic review and meta-analysis to clarify the effects of PD-1/PD-L1 inhibitors in the neoadjuvant setting for patients with TNBC.
An extensive literature search was performed in the PubMed, Embase and Cochrane databases from inception to November 14, 2022 without restriction to language. The following key words were used for the search: “PD 1”, “PD-1”, “PD-L1”, “PD L1”, “PD-1 Inhibitors”, “PD-L1 Inhibitors”, “Programmed Death-Ligand 1 Inhibitors”, “Programmed Cell Death Protein 1 Inhibitor”, “pembrolizumab”, “atezolizumab”, “durvalumab”, “Triple-negative Breast Cancer”, “ER Negative PR Negative HER2 Negative Breast Cancer”, and “Triple Negative Breast Neoplasms” When repeated studies were determined, the most detailed and recent articles were included.
Only those randomized controlled trials (RCTs) that compared the effects of PD-1/PD-L1 inhibitors during neoadjuvant chemotherapy including PD-1/PD-L1 inhibitors (the experimental group) with neoadjuvant chemotherapy alone (the control group) were considered qualified.
Eligible studies had to meet the following criteria: (1) RCTs included at least two treatment groups (PD-1/PD-L1 inhibitors plus chemotherapy and chemotherapy alone); (2) subjects were adult TNBC patients; and (3) pCR was reported as an outcome. Exclusion criteria were: (1) RCTs with incomplete data; (2) non-RCTs; and (3) metastatic or inflammatory breast cancer.
Two authors carried out the citation searches independently and identified eligible trials based on the aforementioned criteria. Cases of discrepancies were resolved through discussion with a third reviewer.
Two investigators independently extracted the following variables from each trial: (1) study information (author and year of publication); (2) trial design, including PD-1/PD-L1 inhibitor intervention, therapy regimens, number of patients in each arm and adverse events.
We evaluated the bias risk of eligible studies based on the guidelines in the Cochrane Reviewers’ Handbook. We assessed selection bias, performance bias, detection bias, attrition bias, reporting bias, and other biases. The risk of bias was divided into three levels: high, low, and unclear.
We used a funnel plot to evaluate publication bias, which was created using the
Egger and Begg tests in Stata 15.1 software (Stata, College Station, TX, USA). In
addition, we conducted a t-test to determine the significance of the
intercept, where a p-value of
Review Manager (version 5.3.5; Cochrane Collaboration, Oxford, UK) was used for
our meta-analysis. We used pooled odds ratios (ORs) with 95% confidence
intervals (CIs) to calculate the binary variable. In addition, a Q statistical
test based on chi square was conducted to evaluate the heterogeneity between
studies. When the p-value in the Q-test was less than 0.10, a random
effects model was used. For all other cases, a fixed effects model was performed.
We used the classic forest map to present the results of the meta-analysis, with
a statistical significance setting of p
We first identified 4804 records in the three databases for evaluation. Based on the inclusion and exclusion criteria utilized, 7 studies and 1707 patients were eligible for meta-analysis by examining the title, abstract, and full text of the records. The reference flow is shown in Fig. 1. The characteristics of these 7 studies are summarized in Table 1 (Ref. [4, 5, 6, 7, 8, 9, 10]).
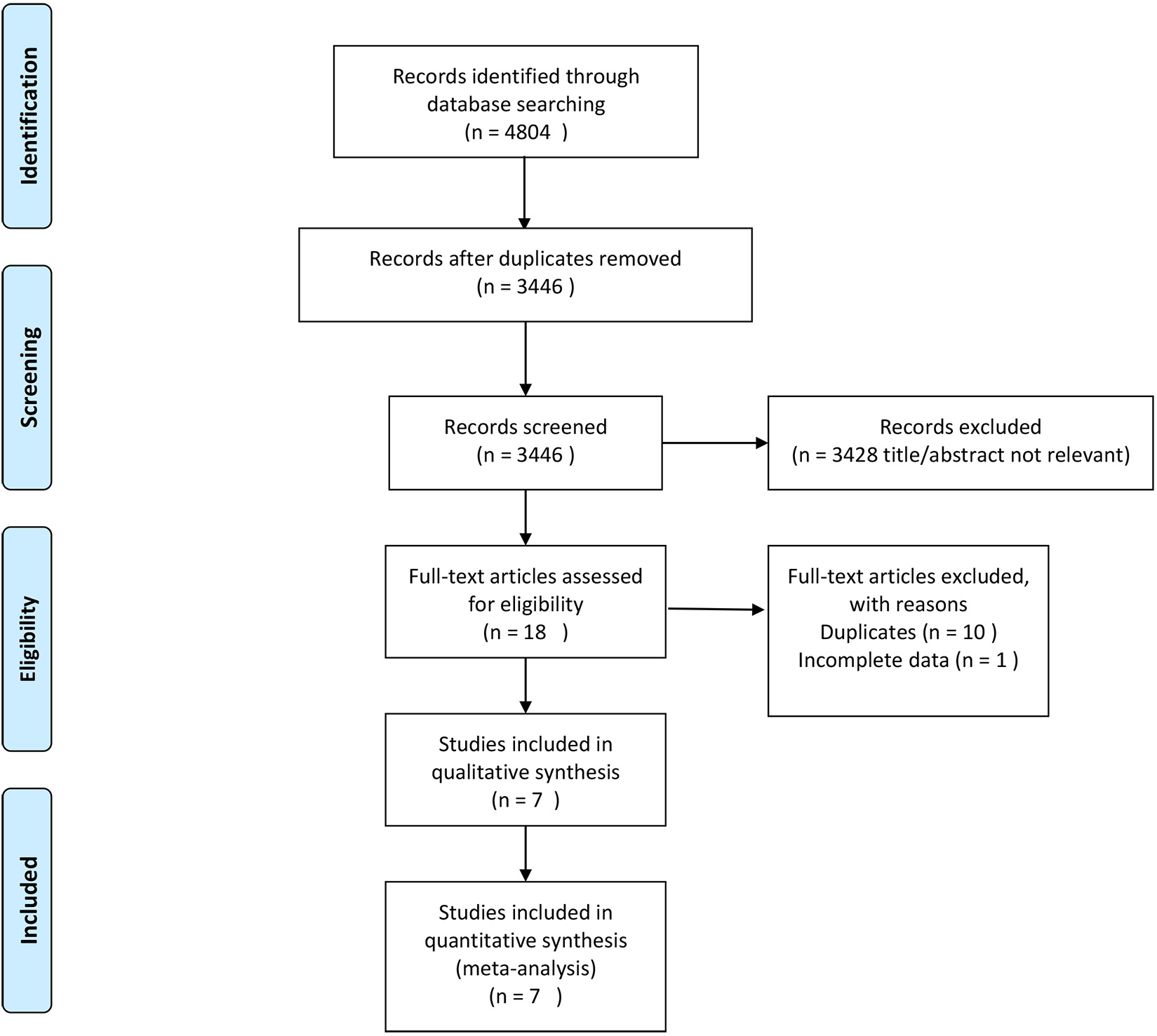 Fig. 1.
Fig. 1.Flow chart of the literature identify.
| Study | Year | Country | PD-1/PD-L1 inhibitors | Treatment arms | Anemia | Neutropenia | Number of participants | |||
| Experimental | Control | Experimental | Control | Experimental | Control | |||||
| Ademuyiwa, Foluso O et al. [10] | 2022 | USA | atezolizumab | Carboplatin + paclitaxel vs. carboplatin + paclitaxel + atezolizumab | NA | NA | NA | NA | 45 | 16 |
| Gianni, L. et al. [9] | 2022 | Italy | atezolizumab | Carboplatin + nab-paclitaxel vs. carboplatin + nab-paclitaxel + atezolizumab | 5 | 4 | 68 | 76 | 138 | 142 |
| Loibl, S. et al. [8] | 2019 | Germany | durvalumab | Epirubicin + cyclophosphamide + nab-paclitaxel + placebo vs. nab-paclitaxel + epirubicin + cyclophosphamide + durvalumab | 2 | 2 | 34 | 34 | 88 | 86 |
| Mittendorf, E. A. et al. [7] | 2020 | USA | atezolizumab | Doxorubicin + cyclophosphamide + nab-paclitaxel + placebo vs. doxorubicin + cyclophosphamide + nab-paclitaxel + atezolizumab | 14 | 12 | 38 | 36 | 165 | 168 |
| Nanda, R. et al. [6] | 2020 | USA | pembrolizumab | Paclitaxel + doxorubicin + cyclophosphamide vs. pembrolizumab + paclitaxel | NA | NA | NA | NA | 28 | 79 |
| Pusztai, L. et al. [5] | 2021 | USA | durvalumab | Paclitaxel vs. durvalumab + olaparib + paclitaxel | NA | NA | NA | NA | 20 | 130 |
| Schmid, P. et al. [4] | 2020 | USA | pembrolizumab | Carboplatin + paclitaxel + placebo vs. carboplatin + paclitaxel + pembrolizumab | 142 | 58 | 270 | 129 | 401 | 201 |
In total, 1707 patients were included in the final selected studies, of whom 885 were in the experimental group and 822 in the control group. Four studies reported hematological adverse events (anemia and neutropenia).
The bias risk of seven of the included studies was appraised using the Cochrane risk of bias tool. As shown in Fig. 2 (Ref. [4, 5, 6, 7, 8, 9, 10]), our results demonstrated that all studies randomly allocated patients to the appropriate treatment arms. All studies had registration information. Overall, these characteristics indicated a lower risk of design bias in the study (Fig. 3).
 Fig. 2.
Fig. 2.Quality assessment for risk of bias.
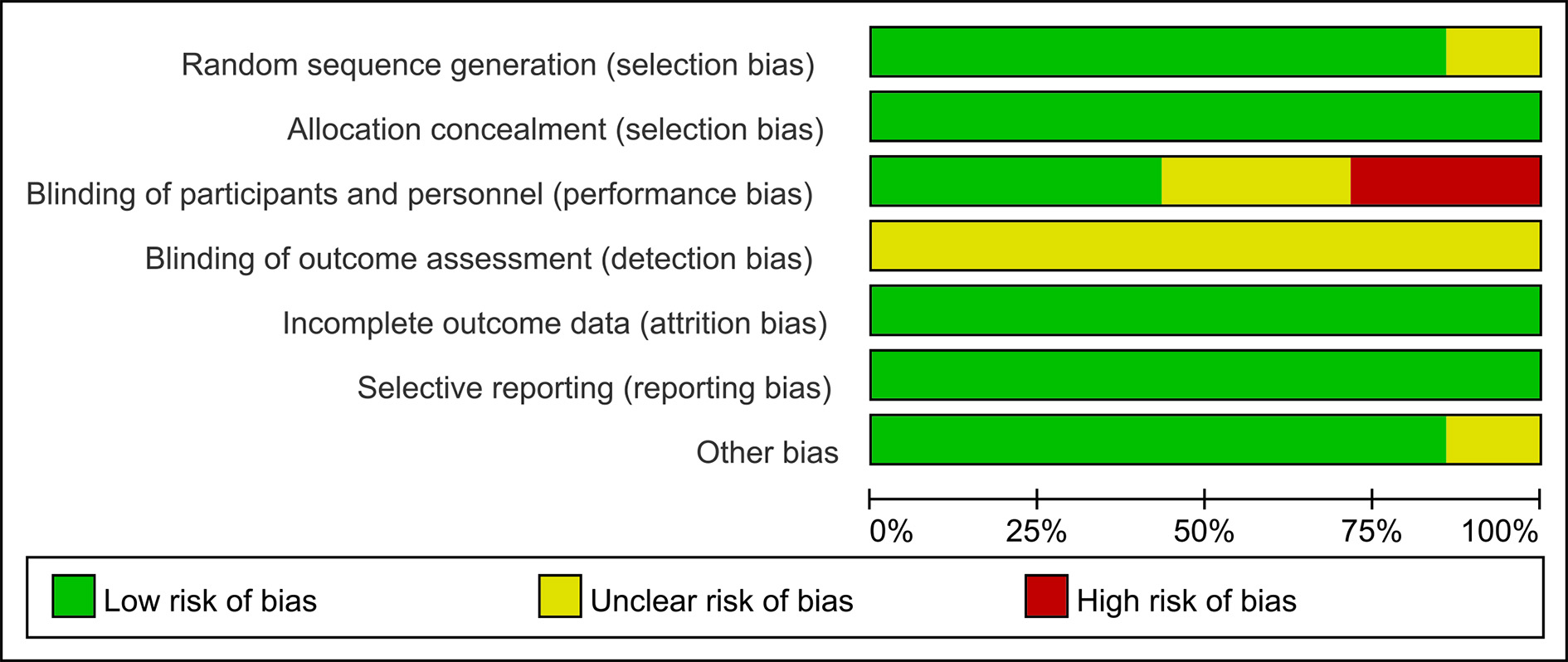 Fig. 3.
Fig. 3.Graphs of risk of bias.
Overall, including all the seven studies, 854 of 1707 (50.0%) patients achieved
a pCR after neoadjuvant treatment, 522 of 885 (59.0%) patients in the PD-1/PD-L1
inhibitor chemotherapy group and 332 of 822 (40.4%) patients in the control
group. As shown in Fig. 4 (Ref. [4, 5, 6, 7, 8, 9, 10]), a significant statistical difference was observed (OR
1.98, 95% CI 1.38–2.82, p
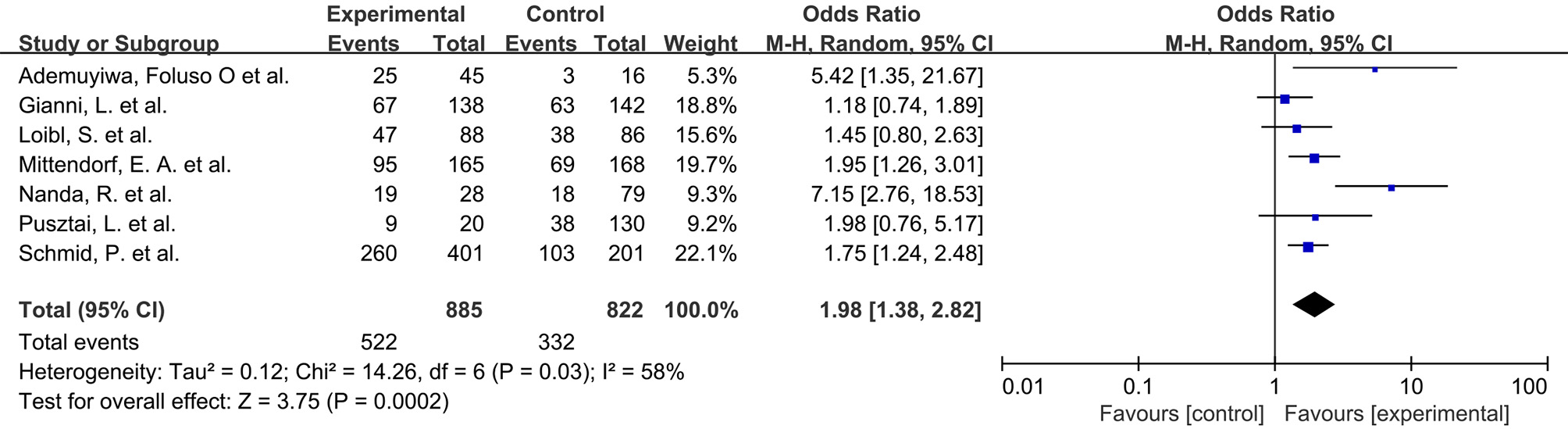 Fig. 4.
Fig. 4.Odds ratio for pathological complete response of experimental versus control.
Anemia. As shown in Fig. 5 (Ref. [4, 7, 8, 9]), four RCTs reported the incidence of grade
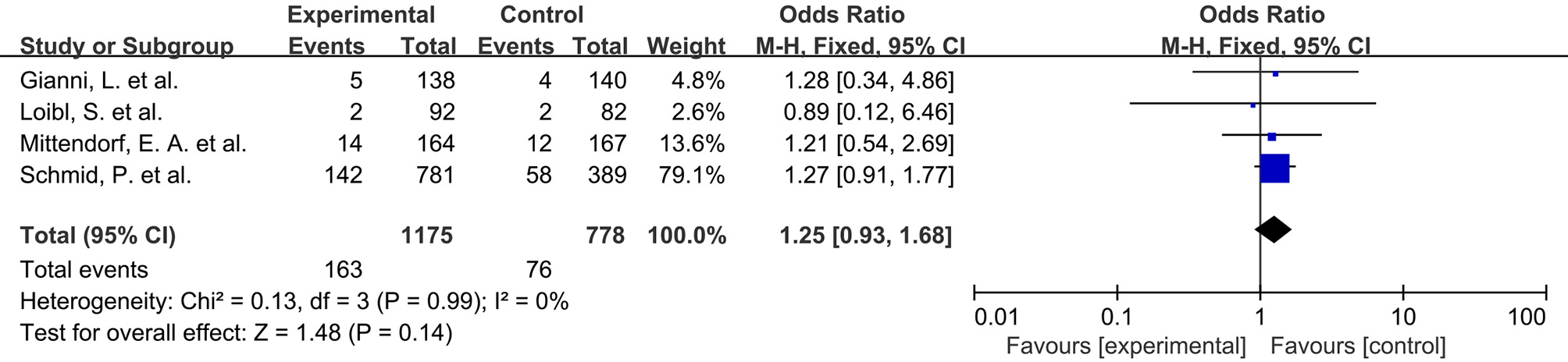 Fig. 5.
Fig. 5.
Odds ratio for grade
Neutropenia. As shown in Fig. 6 (Ref. [4, 7, 8, 9]), four RCTs reported the incidence of grade
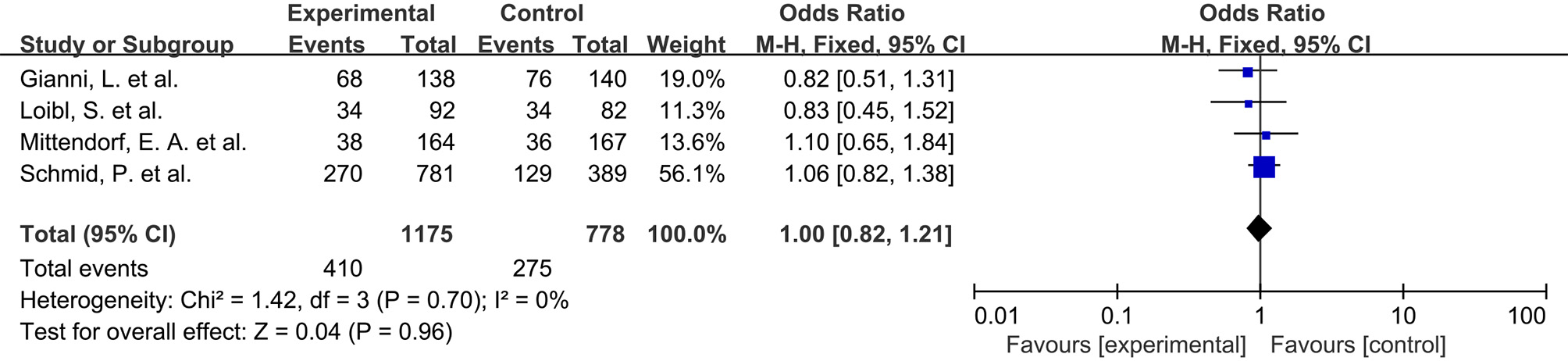 Fig. 6.
Fig. 6.
Odds ratio for grade
The sensitivity analysis was conducted by excluding each study one by one. The result showed the stability of pooled OR estimates (Fig. 7, Ref. [4, 5, 6, 7, 8, 9, 10]).
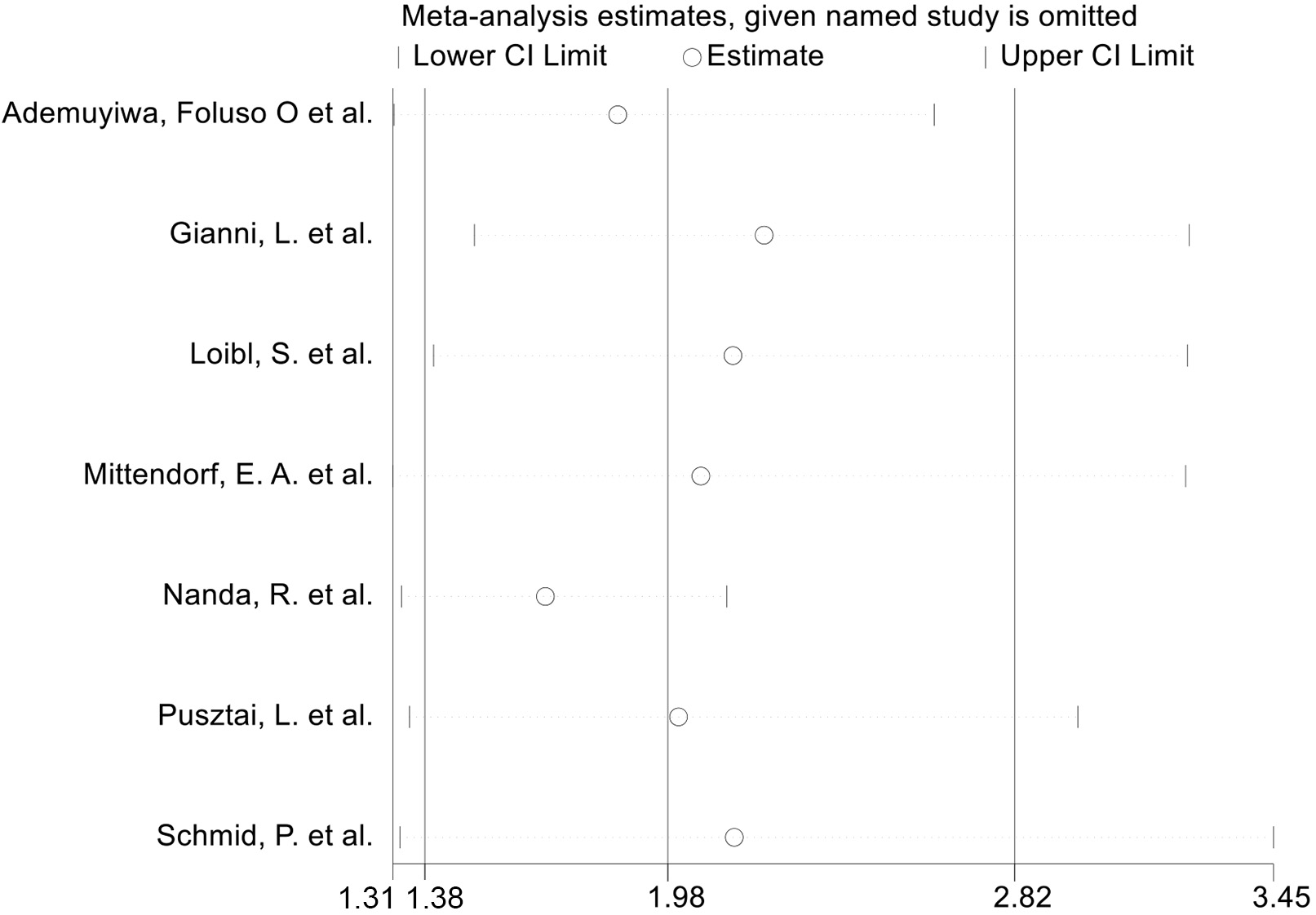 Fig. 7.
Fig. 7.Forest plot for sensitivity analysis (random effects model with 95% confidence interval).
As shown in Fig. 8, we did not detect any publication bias in the funnel plot (Begg’s test, p = 0.293).
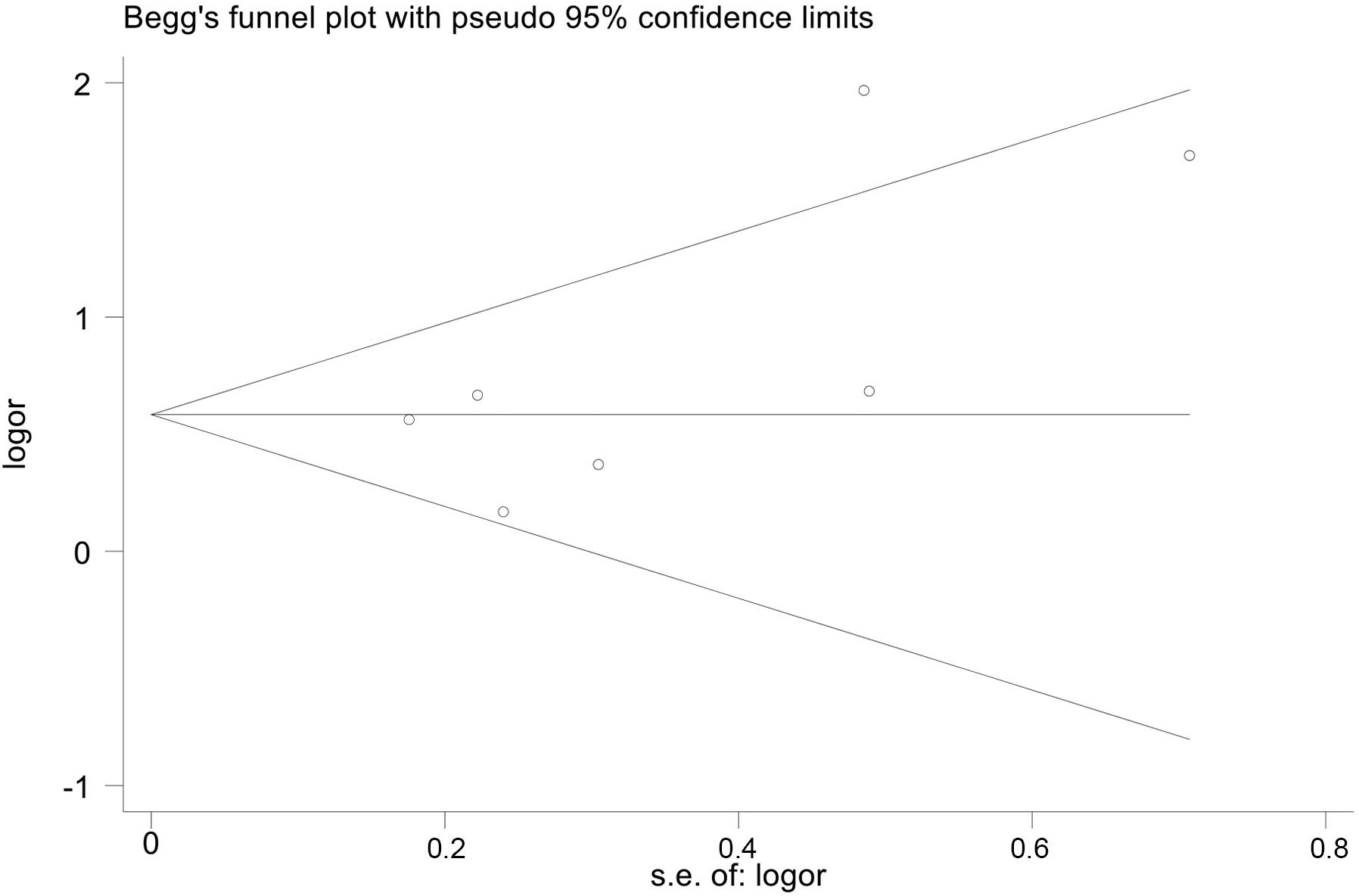 Fig. 8.
Fig. 8.Funnel plots for publication bias.
To assess the role of PD-1/PD-L1 inhibitors in the neoadjuvant setting for patients with TNBC, we conducted a systematic review and meta-analysis of PD-1/PD-L1 inhibitor co-treatment during chemotherapy. Our meta-analysis revealed that the inclusion of PD-1/PD-L1 inhibitors to neoadjuvant chemotherapy regimens significantly increased the pCR rate without raising hematological toxicities.
Chemotherapy elicits cancer cell death and generates signals to prompt dendritic
cells to stimulate the presentation of tumor antigens to T cells, which is a
pathway to activate the immune system against cancer [11]. PD-L1 expression on
tumor cells and its binding to PD-1 on activated T cells inhibits T cell
proliferation, survival, cytokine production, and other effector functions,
ultimately inhibiting anti-tumor immune responses [12, 13]. These considerations
have led to the hypothesis that TNBC may be particularly susceptible to
PD-1/PD-L1 inhibitors. The results of several studies in related fields support
this opinion [14, 15, 16]. Similarly, the current meta-analysis showed that TNBC
patients would benefit from the addition of PD-1/PD-L1 inhibitors. A significant
absolute 18.6% increased pCR rate was observed with the use of PD-1/PD-L1
inhibitors-based neoadjuvant chemotherapy (OR 1.98, 95% CI 1.38–2.82, p
Chemotherapy is plagued with a series of hematological side effects, such as
anemia and neutropenia. Hematological adverse events, especially those graded
Several limitations in our meta-analysis exist. First, non-hematologic adverse reactions to the lungs, endocrine system, and nervous system are important factors that influence treatment decisions and have not been evaluated in our study. Second, due to the lack of long-term follow-up in these studies, whether the increased pCR rates with the addition of PD-1/PD-L1 inhibitors would improve long-term outcomes, such as disease-free survival (DFS) and overall survival (OS), remains unknown. Third, the number of included patients was not very large. Fourth, the detection bias (blinding of outcome assessment) of the included studies was unclear. Fifth, different chemotherapy regimens in the study may affect the interpretation of the results. Hence, future research should focus more on the design of RCTs, such as sufficient sample size and strict blinding to guarantee counterbalance between intervention groups, as well as evaluating other side effects and long-term efficacy.
Our results demonstrated that adding PD-1/PD-L1 inhibitors to neoadjuvant chemotherapy could improve pCR rates in TNBC patients without increasing hematological toxicities. Nevertheless, further high-quality RCTs are needed to support any definitive recommendations for the routine use of PD-1/PD-L1 inhibitors in clinical practice.
All data generated or analyzed during this study are included in this published article.
ZYL designed the study. YF and XZC conducted the selection of relevant studies and data extraction separately. ZZ evaluated the quality of each study independently. SSR and XZC performed the statistical analysis. ZZ and SSR drafted the manuscript. ZYL contributed to the interpretation of the results and critically checked the manuscript. All authors contributed to editorial changes in the manuscript. All authors read and approved the final manuscript. All authors have participated sufficiently in the work and agreed to be accountable for all aspects of the work.
Not applicable.
We would like to express our gratitude to all those who helped us during the writing of this manuscript. Thanks to all the peer reviewers for their opinions and suggestions.
This research received no external funding.
The authors declare no conflict of interest.
References
Publisher’s Note: IMR Press stays neutral with regard to jurisdictional claims in published maps and institutional affiliations.








