1 Department of Obstetrics and Gynecology, Union Hospital, Tongji Medical College, Huazhong University of Science and Technology, 430022 Wuhan, Hubei, China
Abstract
Background: The severe acute respiratory syndrome
coronavirus-2 (SARS-CoV-2) virus is continually evolving, and the worldwide
epidemic is still ongoing. There is conflicting evidence regarding how SAS-CoV-2
infection affects the outcomes of assisted reproductive technology (ART). The aim of this study was to investigate whether the outcomes of in
vitro fertilization (IVF) treatment were affected during the acute period of
SARS-CoV-2 infection or immediately after recovery from coronavirus disease 2019
(COVID-19). Methods: In this retrospective cohort study,
SARS-CoV-2-infected couples who underwent IVF treatment at Wuhan Union Hospital
within the first three months following the lifting of the pandemic policy in
mainland China were propensity-score matched (PSM) to uninfected couples who
received IVF during the dynamic COVID-zero policy. Following matching, 358 and
698 patients were assigned to the SARS-CoV-2-infected and uninfected groups,
respectively. The laboratory and clinical outcomes of the two groups were
compared. Results: The blastocyst formation rates were considerably
lower in the infected group than in the uninfected group. Stratification by time
from SARS-CoV-2 infection to oocyte retrieval (
Keywords
- COVID-19
- IVF
- SARS-CoV-2
- infertility
- embryo
- pregnancy
The World Health Organization (WHO) declared that coronavirus disease 2019 (COVID-19) was no longer a public health emergency of international concern (PHEIC) on 5 May 2023. severe acute respiratory syndrome coronavirus-2 (SARS-CoV-2) is still evolving [1], resulting in new cases and reinfections in the population [2, 3, 4]. As SARS-CoV-2 is a new virus, we still need to improve our understanding of it, especially its effects on human reproduction and assisted reproductive technology (ART) [5]. Currently, it is believed that the SARS-CoV-2 virus damages cells or tissues by infecting and replicating in cells, which requires the expression of SARS-CoV-2 receptors, such as angiotensin converting enzyme 2 (ACE2), basigin (BSG), transmembrane serine protease 2 (TMPRSS2) and cathepsin L (CTSL) [6, 7]. It is noteworthy that all the aforementioned viral receptor mRNAs are expressed in most of the human female reproductive tract, including the ovaries (including follicular granulosa cells) [8] and endometrium [9]. A few studies have also shown that ACE2, BSG, and/or TMPRSS2 genes and proteins are expressed in human oocytes, fertilized eggs, and blastocysts [10, 11, 12]. Therefore, the effects of SARS-CoV-2 infection on the pregnancy outcomes of in vitro fertilization/intracytoplasmic sperm injection (IVF/ICSI) have been the focus of attention for ART staff and patients.
A retrospective study from Israel showed that IVF treatment within one year after SARS-CoV-2 infection did not affect the pregnancy outcomes after fresh embryo transfer. It should be noted that this study did not mention whether or not the control group was thoroughly screened for SARS-CoV-2 infection [13]. Several studies, however, have revealed that the rate of high-quality embryos [14] and retrieved oocytes [15] was decreased in patients who underwent IVF treatment after getting infected with SARS-CoV-2 virus. Another study discovered that when only the male partner was infected with SARS-CoV-2, the blastocyst formation rate was reduced, even though the IVF procedure was performed more than 4 months after SARS-CoV-2 infection [16]. It should be noted that all of these studies had small sample sizes and did not conduct stratified analyses of the time from SARS-CoV-2 infection to oocyte retrieval. As a result, the impact of SARS-CoV-2 infection on IVF treatment outcomes remains unclear. The clinical and laboratory results of patients who underwent IVF treatment during the acute infection period, in particular, were mostly from case reports [17, 18].
Due to China’s effective and strict epidemic prevention and control policy, ART services in mainland China were carried out in a nonepidemic state from the beginning of 2020 to November 2022. However, with the attenuated pathogenicity of the omicron subvariants and increasing vaccination coverage, the dynamic zero-COVID policy was terminated in mainland China on 7 December 2022 [19]. A wave of SARS-CoV-2 infections was reported in mainland China from December 2022 to January 2023 [4, 20]. This infection wave was mainly caused by the SARS-CoV-2 omicron variants BF.7 and BA.5.2 [21]. During this time, our center also treated more SARS-CoV-2-infected couples, providing a good observation sample. Thus, in the present study, we collected IVF data from SARS-CoV-2-infected couples who underwent IVF treatment from 7 December 2022 to 7 March 2023 in order to assess the impact of SARS-CoV-2 infection on embryo development and IVF clinical outcomes.
In this retrospective cohort study, all couples who underwent their first or second cycle of IVF or ICSI treatment at Union Hospital, Tongji Medical College, Huazhong University of Science and Technology from 7 December 2022 to 7 March 2023 were enrolled. Couples in which both partners were infected with SARS-CoV-2 on or before the trigger day (based on polymerase chain reaction (PCR) assays for SARS-CoV-2 RNA detection in nasopharyngeal swabs) and the female partner’s age was between 21 and 50 years were included as the SARS-CoV-2-positive group. To avoid the possibility of unknown and asymptomatic incubation periods, the current study also enrolled all couples who underwent their first or second cycle of IVF or ICSI treatment in our center from 1 June 2021 to 30 November 2022 (during which the dynamic zero-COVID policy was implemented in mainland China). Couples with no history of SARS-CoV-2 infection and in which the female partner’s age was 21–50 years were included as the SARS-CoV-2-negative (control) group. Couples in both groups underwent at least two PCR tests to detect SARS-CoV-2 RNA during controlled ovarian stimulation (COS), namely, before COS and on the trigger day. Before COS, the female partner had a pulmonary computed tomography (CT) test to rule out the presence of infectious lesions in the lungs. Moreover, a careful medical history was obtained and a COVID-19 questionnaire survey was performed for all patients before the initiation of COS. Patients who lacked critical information, were lost to follow-up, used donor eggs or sperm, had whole or partial oocyte freezing, or had preimplantation genetic testing cycles were all excluded. To establish groups with comparable characteristics, propensity score matching was performed at a ratio of 1:2 between the infected and uninfected groups. The present study was approved by the Ethical Committee of Union Hospital (no. 2023-S0462), and individual consent for this retrospective analysis was waived.
In this study, most patients underwent the gonadotropin-releasing hormone (GnRH)
agonist protocol or the GnRH antagonist protocol. A few patients underwent the
clomiphene-primed ovarian stimulation (CPOS) protocol and luteal phase stimulation protocol.
For the GnRH agonist protocol, tripreilin acetate was injected at 0.05 mg/d
(Ferring Pharmaceuticals, Kiel, German) at
the middle luteal stage of the previous cycle for pituitary downregulation. When
the downregulation standard was reached (serum luteinizing hormone level
Fertilization was done using IVF or ICSI, depending on the quality of the male
partner’s sperm. For IVF fertilization, approximately 20,000 motile sperm were
added to each oocyte. ICSI was carried out if the percentage of normal sperm was
less than 1% or the total amount of motile sperm was less than 5
Embryo transfer was performed under abdominal ultrasound guidance, with a maximum of 2 cleavage-stage embryos or blastocysts transferred each time. The “freeze-all” strategy was employed for couples in the acute stage of SARS-CoV-2 infection. If the couples met the criteria for fresh embryo transfer, embryo transfer was performed on Day 3, 5 or 6 after oocyte retrieval. The surplus embryos were further cultured in G2-PLUS medium (Vitrolife, Gothenburg, Sweden) up to Day 5–7 until they reached the blastocyst stage, and the available blastocysts were frozen by vitrification. For frozen embryo transfer, most of the enrolled patients underwent hormone replacement cycles to prepare the endometrium. The details of the vitrification procedure and endometrial preparation were described previously [24].
Real-time polymerase chain reaction (RT‒PCR) (Mingde Biotechnology Co., Ltd., Wuhan, Hubei, China) was carried out to detect the presence of SARS-CoV-2 RNA in the specimens collected from nasopharyngeal swabs. The open reading frame 1ab (ORF1ab) and N genes of SARS-CoV-2 were the target genes for RT–PCR. A cycle threshold (Ct) of less than 37 denoted positive SARS-CoV-2 findings.
The important quality control indices during COS and in vitro embryo
culture and pregnancy outcomes in the first trimester were analyzed and compared
between the two groups. The primary outcome measure was the clinical pregnancy
rate after the first embryo transfer cycle. The secondary outcome measures
included the number of oocytes retrieved, the number of mature oocytes, the
number of normal fertilizations, the blastocyst formation rate, the number of
available embryos, and early pregnancy loss. The above measures were calculated
according to our previous report [24]. The high-quality embryo rate was defined
as the number of high-quality embryos on Day 3 divided by the number of normally
fertilized cleavage embryos. The blastocyst formation rate was defined as the
number of blastocysts formed divided by the number of normally fertilized
oocytes. The available blastocyst rate was calculated by dividing the number of
blastocysts available for cryopreservation and transfer by the number of normally
fertilized oocytes. The presence of a gestational sac four weeks after embryo
transfer was recognized as a clinical pregnancy. A biochemical pregnancy was
defined as a serum-hCG level
Kolmogorov–Smirnov or Shapiro–Wilk normality tests were used for all
continuous variables. Variables with a normal distribution are presented as
Standard propensity score matching was conducted using nearest neighbor matching
with a caliper of 0.02. The following baseline characteristics were matched
without replacement at a ratio of 1:2: female age (years), female body mass index
(BMI, kg/m
Among those who underwent IVF/ICSI at our center between 7 December 2022 and 7
March 2023, a total of 386 couples met the inclusion and exclusion criteria, and
both partners were infected with SARS-CoV-2 on or before the trigger day. A total
of 2660 uninfected patients who underwent IVF/ICSI between 1 June 2021 and 30
November 2022 and met the exclusion and inclusion criteria were selected as
controls. Following propensity score matching, 358 patients were assigned to the
infected group and 698 patients to the uninfected group (Fig. 1). Table 1 shows the baseline characteristics of the couples following matching. There were
no significant differences in any baseline characteristics between the two groups
(p
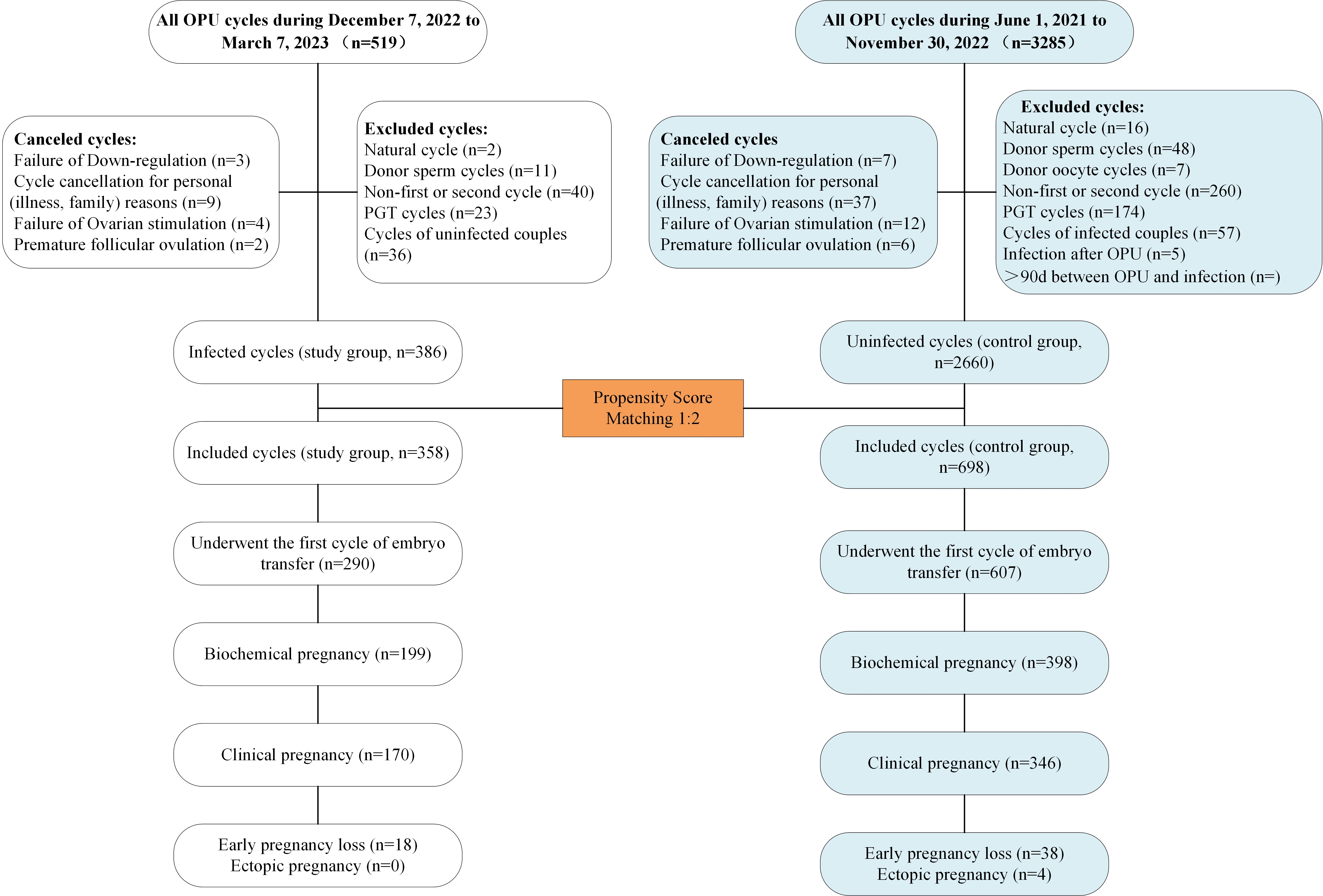 Fig. 1.
Fig. 1.Study flow chart. OPU, oocyte pickup; PGT, preimplantation genetic testing.
| Characteristic | Before propensity score matching | After propensity score matching | |||||
| Uninfected group | Infected group | p value | Uninfected group | Infected group | p value | ||
| (n = 2660) | (n = 386) | (n = 698) | (n = 358) | ||||
| Age of the woman (years) | 32 (29, 35) | 33 (30, 35) | 0.004 | 32 (30, 35) | 33 (30, 35) | 0.631 | |
| Infertility duration (years) | 3 (1.5, 4) | 3 (1.5, 4) | 0.971 | 3 (1.5, 4.13) | 3 (1.5, 4.0) | 0.951 | |
| Primary infertility, n (%) | 1359 (51.09%) | 190 (49.22%) | 0.493 | 350 (50.14%) | 189 (52.79%) | 0.415 | |
| Cycle number, n (%) | 0.221 | 0.158 | |||||
| First cycle | 2106 (79.17%) | 316 (81.87%) | 609 (87.25%) | 301 (84.08%) | |||
| Repeated cycles | 554 (20.83) | 70 (18.13%) | 89 (12.75%) | 57 (15.92%) | |||
| AMH (ng/mL) | 3.07 (1.70, 5.25) | 3.24 (1.92, 5.21) | 0.132 | 3.42 (1.87, 6.17) | 3.23 (1.94, 5.17) | 0.319 | |
| Basal FSH level (IU/L) | 7.19 (5.94, 8.74) | 7.21 (5.77, 8.67) | 0.487 | 7.02 (5.87, 8.47) | 7.10 (5.70, 8.64) | 0.100 | |
| Body mass index (kg/m |
22.50 (20.43, 25.16) | 22.84 (20.99, 24.97) | 0.177 | 22.65 (20.66, 25.23) | 22.83 (20.99, 24.97) | 0.610 | |
| Cause of infertility, n (%) | 0.006 | 0.955 | |||||
| Tubal | 997 (37.48%) | 143 (37.05%) | 260 (37.25%) | 138 (38.55%) | |||
| Male factor | 205 (7.71%) | 32 (8.29%) | 54 (7.74%) | 28 (7.82%) | |||
| Anovulatory | 285 (10.71%) | 33 (8.55%) | 67 (9.60) | 33 (9.22%) | |||
| Unexplained | 640 (24.06%) | 99 (25.65%) | 197 (28.22%) | 96 (26.82%) | |||
| Diminished ovarian reserve | 345 (12.97%) | 44 (11.40%) | 79 (11.32%) | 38 (10.61%) | |||
| Endometriosis | 162 (6.09%) | 22 (5.70%) | 31 (4.44%) | 21 (5.87%) | |||
| Mixed factors | 26 (0.98%) | 13 (3.37%) | 10 (1.43%) | 4 (1.12%) | |||
| OS protocol, n (%) | 0.809 | ||||||
| GnRH-agonist | 1153 (43.35%) | 93 (24.09%) | 175 (25.07%) | 93 (25.98%) | |||
| GnRH-antagonist | 863 (32.44%) | 226 (58.55%) | 393 (56.30%) | 204 (56.98%) | |||
| CPOS | 644 (24.21%) | 67 (17.36%) | 130 (18.62%) | 61 (17.04%) | |||
| Insemination method, n (%) | 0.099 | 0.681 | |||||
| IVF | 1828 (68.72%) | 280 (72.54%) | 499 (71.49%) | 265 (74.02%) | |||
| ICSI | 709 (26.65%) | 84 (21.76%) | 153 (21.92%) | 72 (20.11%) | |||
| IVF+RICSI | 123 (4.62%) | 22 (5.70%) | 46 (6.59%) | 21 (5.87%) | |||
| Gonadotropins dosage (IU) | 2325 (1800, 2925) | 2250 (1819, 2700) | 0.061 | 2300 (1800, 2850) | 2250 (1800, 2700) | 0.415 | |
| Gn duration (days) | 9 (8, 11) | 9 (8, 10) | 9 (8, 10) | 9 (8, 10) | 0.161 | ||
| E2 on trigger day (pg/mL) | 2047 (1188, 3362) | 1720 (1108, 2731) | 1726 (973, 2976) | 1752 (1117, 2760) | 0.864 | ||
| Endometrial thickness (mm) | 10 (8, 12) | 10 (8, 12) | 0.511 | 10 (8, 12) | 10 (8, 12) | 0.509 | |
Note: Data are presented as the median (25th and 75th percentile) or number (%). Mann‒Whitney U statistics were used for continuous variables and chi-square tests were used for categorical variables. There were no significant differences after propensity score matching. AMH, anti-Müllerian hormone; FSH, follicle-stimulating hormone; OS, ovarian stimulation; CPOS, clomiphene-primed ovarian stimulation; ICSI, intracytoplasmic sperm injection; IVF, in vitro fertilization; RICSI, early rescue intracytoplasmic sperm injection; E2, Estradiol; Gn, gonadotropin; GnRH, gonadotropin-releasing hormone.
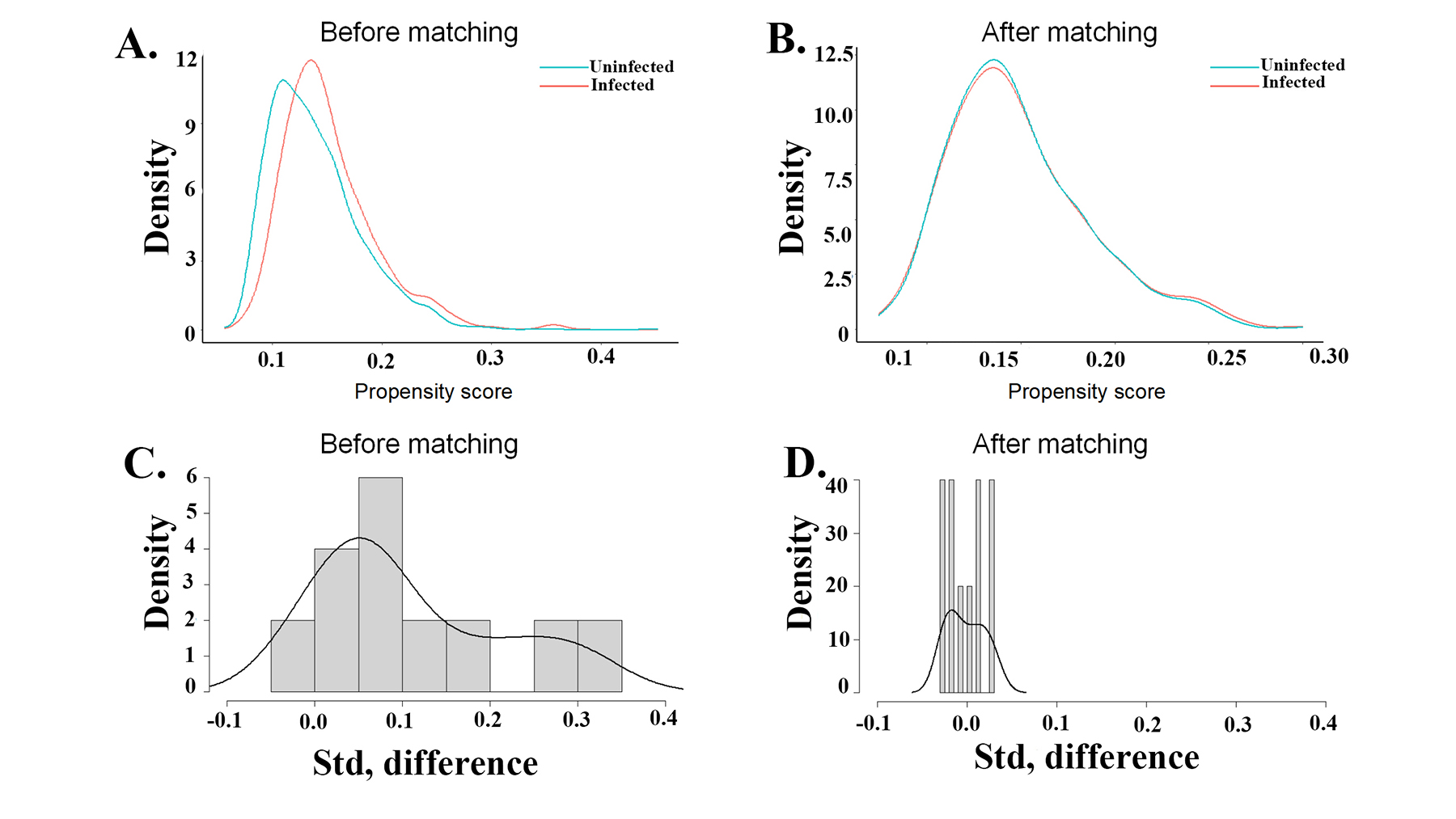 Fig. 2.
Fig. 2.Comparison of the infected and uninfected groups’ propensity scores before and after matching. (A,B) Propensity score distribution before and after matching. (C,D) The standard difference distribution of before and after matching. Std, standard deviation.
For the oocyte and embryo outcomes, there were no significant differences
between the two groups in the average number of oocytes retrieved, the mature
oocyte rates, the normal fertilization rates, the abnormal fertilization rates,
and the cleavage rates. However, compared with the uninfected (control) group,
the blastocyst formation rate in the infected group was significantly decreased
[73.33% (IQR 50.00%–92.31%) vs 66.67% (IQR 50.00%–87.5%);
p
| Uninfected group | Infected group | p value | 95% CI | |
| (n = 698) | (n = 358) | |||
| Average no. of oocytes retrieved | 11 (6, 16) | 11 (6, 17) | 0.646 | –1.00–1.00 |
| Mature oocyte rate, % | 84.81 (71.43, 100) | 82.35 (69.23, 94.12) | 0.138 | –0.03–0.00 |
| Normal fertilization rate, % | 57.14 (40.00, 75.00) | 56.25 (40.00, 71.43) | 0.501 | –0.04–0.02 |
| Abnormal fertilization rate, % | 0.00 (0.00, 12.50) | 0.00 (0.00, 14.29) | 0.840 | 0.00–0.00 |
| Cleavage rate, % | 100 (100, 100) | 100 (100, 100) | 0.659 | 0.00–0.00 |
| High-quality embryo rate, % | 37.50 (11.46, 64.12) | 44.44 (20.00, 66.67) | 0.052 | 0.00–0.08 |
| Blastocyst formation rate, % | 73.33 (50.00, 92.31) | 66.67 (50.00, 87.50) | 0.013 | –0.08–0.00 |
| Available blastocyst rate, % | 62.50 (45.45, 80.00) | 60.00 (40.00, 80.00) | 0.438 | –0.05–0.00 |
Note: 95% CI, 95% confidence interval.
Continuous variables are presented as the median (25th and 75th percentile),
while categorical variables are presented as the % (n); p
High-quality embryo rate = the high quality embryo number on day 3 / normal
fertilization cleavage embryo number
The infected group was further stratified into subgroups by the interval from
SARS-CoV-2 infection to oocyte retrieval (30 days, 31~60 days,
61~90 days, and
| Characteristic | 31 |
61 |
p value | |||
| Age of the woman (years) | 32 (29, 34) | 32 (30, 36) | 33 (30, 35) | 33 (30, 35.5) | 0.710 | |
| Infertility duration (years) | 3.00 (1.00, 3.50) | 2.00 (2.00, 4.00) | 3.00 (1.00, 5.00) | 3.00 (2.00, 5.00) | 0.302 | |
| Primary infertility, n (%) | 31 (44.93) | 34 (49.28) | 56 (47.06) | 56 (55.45) | 0.514 | |
| Cycle number, n (%) | ||||||
| First cycle | 59 (85.51) | 56 (81.16) | 101 (84.87) | 85 (84.16) | 0.896 | |
| Repeated cycles | 10 (14.50) | 13 (18.84) | 18 (15.13) | 16 (15.84) | 0.896 | |
| AMH (ng/mL) | 3.49 (1.79, 6.11) | 3.56 (2.03, 4.97) | 3.31 (1.95, 5.36) | 2.93 (1.65, 4.73) | 0.561 | |
| Basal FSH level (IU/L) | 6.74 (5.33, 8.91) | 6.84 (5.47, 8.41) | 6.97 (5.87, 8.60) | 7.48 (6.21, 8.75) | 0.171 | |
| Body mass index (kg/m |
22.70 (20.83, 24.35) | 23.02 (21.29, 24.83) | 22.84 (21.18, 25.62) | 22.73 (20.78, 24.97) | 0.536 | |
| Cause of infertility, n (%) | ||||||
| Tubal | 31 (44.93) | 26 (37.68) | 39 (32.77) | 43 (42.57) | 0.251 | |
| Male factor | 4 (5.80) | 3 (4.35) | 12 (10.08) | 9 (8.91) | 0.465 | |
| Anovulatory | 8 (11.59) | 7 (10.15) | 13 (10.92) | 5 (4.95) | 0.369 | |
| Unexplained | 15 (21.74) | 23 (33.33) | 28 (23.53) | 29 (28.71) | 0.355 | |
| Diminished ovarian reserve | 8 (11.59) | 5 (7.25) | 15 (12.61) | 9 (8.91) | 0.635 | |
| Endometriosis | 3 (4.35) | 5 (7.25) | 9 (7.56) | 5 (4.95) | 0.635 | |
| Mixed factors | 0.000 | 0.000 | 3 (2.52) | 1 (0.99) | 0.460 | |
| OS protocol, n (%) | ||||||
| GnRH-agonist | 23 (33.33) | 19 (27.54) | 24 (20.17) | 27 (26.73) | ||
| GnRH-antagonist | 30 (43.48) | 32 (46.38) | 73 (61.35) | 69 (68.32) | ||
| CPOS | 16 (23.19) | 18 (26.09) | 22 (18.49) | 5 (4.95) | ||
| Insemination method, n (%) | 0.009 | |||||
| IVF | 44 (63.77) | 42 (60.87) | 94 (80.34) | 83 (83.00) | ||
| ICSI | 19 (27.54) | 20 (28.99) | 18 (15.39) | 14 (14.00) | ||
| IVF+RICSI | 6 (8.70) | 7 (10.15) | 5 (4.27) | 3 (3.00) | ||
| Gonadotropins dosage (IU) | 2175 (1750, 2888) | 2325 (1950, 2663) | 2175 (1800, 2700) | 2250 (1813, 2700) | 0.628 | |
| Gn duration (days) | 9 (8, 10) | 9 (8, 10) | 9 (8, 10) | 9 (8, 10) | 0.576 | |
| E2 on trigger day (pg/mL) | 2037 (1310, 3281) | 1860 (1179, 2705) | 1681 (1087, 2570) | 1622 (984.9, 2683) | 0.075 | |
| Average no. of oocytes retrieved | 10.00 (6.00, 16.50) | 10.00 (6.00, 17.50) | 12.00 (6.00, 17.00) | 11.00 (6.00, 17.00) | 0.986 | |
| Mature oocyte rate, % | 0.81 (0.70, 0.91) | 0.83 (0.67, 0.95) | 0.83 (0.72, 0.95) | 0.82 (0.67, 1.00) | 0.814 | |
| Normal fertilization rate, % | 0.53 (0.37, 0.70) | 0.58 (0.38, 0.73) | 0.60 (0.46, 0.72) | 0.54 (0.39, 0.75) | 0.278 | |
| Abnormal fertilization rate, % | 0 (0, 15.04) | 0 (0, 12.50) | 5.13 (0, 13.33) | 5.28 (0, 15.38) | 0.331 | |
| Cleavage rate, % | 100 (100, 100) | 100 (100, 100) | 100 (100, 100) | 100 (100, 100) | 0.654 | |
| High-quality embryo rate, % | 50.00 (33.33, 65.91) | 33.33 (0, 53.33) | 50.00 (29.64, 66.67) | 45.56 (15.42, 66.67) | 0.011 | |
| Blastocyst formation rate, % | 73.68 (50.00, 100) | 50.00 (31.67, 83.33) | 69.23 (55.56, 87.50) | 66.67 (50.00, 83.33) | 0.012 | |
| Available blastocyst rate, % | 66.67 (50.00, 89.44) | 50.00 (20.00, 71.71) | 66.67 (50.00, 81.82) | 60.00 (40.00, 72.32) | 0.003 | |
| High-quality blastocyst rate, % | 0 (0, 28.57) | 0 (0, 29.67) | 20.00 (0, 40.00) | 3.57 (0, 42.14) | 0.109 | |
| Implantation rate, % | 56.94 (41/72) | 57.63 (34/59) | 56.44 (57/101) | 48.24 (41/85) | 0.593 | |
| Biochemical pregnancy rate, % | 70.97 (44/62) | 75.93 (41/54) | 67.35 (66/98) | 64.47 (49/76) | 0.537 | |
| Clinical pregnancy rate, % | 61.29 (38/62) | 62.96 (34/54) | 58.16 (57/98) | 53.95 (41/76) | 0.730 | |
| Early pregnancy loss rate, % | 13.16 (5/38) | 5.88 (2/34) | 15.79 (9/57) | 7.32 (3/41) | 0.430 | |
Note: Data are presented as the median (25th and 75th percentile) or number (%). Mann‒Whitney U statistics were used for continuous variables and chi-square tests were used for categorical variables. SARS-CoV-2, acute respiratory syndrome coronavirus-2.
To exclude possible confounding factors of the blastocyst formation rate, we
further conducted a linear-regression analysis including patient age, number of
IVF/ICSI cycles, body mass index, ovarian stimulation protocol, fertilization
method, type of infertility, cause of infertility, number of mature oocytes, and
D3 high-quality embryo rate. The results also suggested that SARS-CoV-2
infection, together with female age, number of IVF/ICSI cycles and the D3
high-quality embryo rate, was a significant predictor of the blastocyst formation
rate (Supplementary Table 2). More notably, the linear
regression analysis model for blastocyst formation rate stratified by the
interval from SARS-CoV-2 infection to oocyte retrieval further strengthened the
univariate results, with 31~60 days after SARS-CoV-2 infection
remaining a significant variable (p
| Variable | Unstandardized coefficients | Standardized coefficients | t | p Value | 95% CI | Collinearity statistics | ||||
| Beta | Std Error | Beta | Lower | Upper | Tolerance | VIF | ||||
| Constant | 0.94 | 0.11 | 8.95 | 0.000 | 0.718 | 1.14 | ||||
| Age (years) | –0.01 | 0.002 | –0.11 | –3.10 | 0.002 | –0.01 | –0.002 | 0.75 | 1.34 | |
| The number of IVF cycles | –0.09 | 0.03 | –0.11 | –3.14 | 0.002 | –0.15 | –0.03 | 0.81 | 1.24 | |
| BMI (kg/m |
–0.001 | 0.002 | –0.02 | –0.051 | 0.635 | –0.006 | 0.004 | 0.94 | 1.06 | |
| AMH (ng/mL) | 0.002 | 0.003 | 0.024 | 0.564 | 0.573 | –0.004 | 0.008 | 0.524 | 1.909 | |
| Interval between infection and oocyte retrieval (days) | ||||||||||
| Uninfected (Ref.) | 1 | |||||||||
| 0.003 | 0.04 | 0.003 | 0.08 | 0.939 | –0.07 | 0.07 | 0.94 | 1.06 | ||
| –0.143 | 0.04 | –0.13 | –4.12 | –0.21 | –0.07 | 0.95 | 1.06 | |||
| –0.024 | 0.03 | –0.03 | –0.86 | 0.418 | –0.08 | 0.03 | 0.94 | 1.06 | ||
| –0.059 | 0.03 | –0.06 | –1.95 | 0.056 | –0.12 | 0.002 | 0.94 | 1.07 | ||
| OS protocol | ||||||||||
| GnRH–agonist (Ref.) | 1 | 1 | ||||||||
| GnRH–antagonist | 0.02 | 0.02 | 0.03 | 0.91 | 0.399 | –0.02 | 0.06 | 0.67 | 1.49 | |
| CPOS | 0.05 | 0.03 | 0.07 | 1.59 | 0.104 | –0.01 | 0.11 | 0.54 | 1.85 | |
| Insemination method | ||||||||||
| IVF (Ref.) | 1 | 1 | ||||||||
| ICSI | –0.01 | 0.03 | –0.01 | –0.211 | 0.841 | –0.06 | 0.05 | 0.64 | 1.57 | |
| IVF+RICIS | –0.02 | 0.04 | –0.02 | –0.576 | 0.572 | –0.09 | 0.05 | 0.96 | 1.04 | |
| Type of infertility | ||||||||||
| Primary infertility (Ref.) | 1 | 1 | ||||||||
| Secondary infertility | 0.02 | 0.02 | 0.04 | 1.20 | 0.238 | –0.02 | 0.06 | 0.85 | 1.18 | |
| Cause of infertility | ||||||||||
| Tubal (Ref.) | 1 | |||||||||
| Endometriosis | 0.02 | 0.04 | 0.02 | 0.53 | 0.579 | –0.06 | 0.11 | 0.89 | 1.13 | |
| Male factor | –0.01 | 0.04 | –0.01 | –0.26 | 0.775 | –0.09 | 0.06 | 0.70 | 1.44 | |
| Diminished ovarian reserve | –0.09 | 0.04 | –0.09 | –2.46 | 0.015 | –0.17 | –0.02 | 0.68 | 1.46 | |
| Anovulatory | 0.004 | 0.03 | 0.004 | 0.12 | 0.996 | –0.07 | 0.07 | 0.75 | 1.33 | |
| Unexplained | 0.02 | 0.02 | 0.03 | 0.80 | 0.422 | –0.03 | 0.06 | 0.78 | 1.29 | |
| Mixed factors | –0.10 | 0.08 | –0.04 | –1.21 | 0.228 | –0.27 | 0.06 | 0.90 | 1.12 | |
| Number of mature oocytes | 0.000 | 0.001 | 0.008 | 0.24 | 0.941 | –0.003 | 0.003 | 0.75 | 1.33 | |
| High-quality embryo rate | 0.25 | 0.03 | 0.23 | 8.58 | 0.19 | 0.31 | 0.96 | 1.04 | ||
Note: BMI, body mass index; VIF, variance inflation factor; Ref., reference.
For clinical pregnancy outcomes, 290 couples in the infected group (99 couples underwent fresh embryo transfer) and 607 couples in the matched uninfected group (139 couples underwent fresh embryo transfer) completed the first cycle of embryo transfer. There was no significant difference in embryo implantation rate (54.88% vs 49.54%), biochemical pregnancy rate (68.62% vs 65.56%), clinical pregnancy rate (58.62% vs 57.01%), or early abortion rate (10.59% vs 10.98%) after the first cycle of embryo transfer between the two groups (Table 5).
| Uninfected group | Infected group | Z value | p value | OR (95% CI) | |
| (n = 698) | (n = 358) | ||||
| Single embryo transfer rate, % | 85.67 (520/607) | 88.62 (257/290) | 1.215 | 0.224 | 0.76 (0.50–1.17) |
| Embryo transfer strategies, n (%) | 0.4026 | 0.687 | 0.94 (0.70–1.26) | ||
| Fresh embryo transfer | 199 (32.78) | 99 (34.14) | |||
| Frozen embryo transfer | 408 (67.22) | 191 (65.86) | |||
| Implantation rate, % | 54.32 (377/694) | 53.87 (174/323) | 0.1349 | 0.893 | 1.02 (0.78–1.33) |
| Biochemical pregnancy rate, % | 65.57 (398/607) | 68.62 (199/290) | 0.906 | 0.365 | 0.87 (0.65–1.17) |
| Clinical pregnancy rate, % | 57.00 (346/607) | 58.62 (170/290) | 0.4588 | 0.646 | 0.94 (0.70–1.24) |
| Early pregnancy loss rate, % | 10.98 (38/346) | 10.59 (18/170) | 0.1354 | 0.892 | 1.04 (0.57–1.94) |
| Ectopic pregnancy rate, % | 1.15 (4/346) | 0 | / | 0.307 | 0.00 (0.00–2.04) |
| No available embryo cycle rate | 9.60 (67/698) | 8.04 (32/398) | 0.8657 | 0.387 | 1.21 (0.79–1.88) |
Note: OR, odds ratio.
In the current study, we enrolled SARS-CoV-2-infected couples who underwent IVF treatment during the first three months after the public health control measures were adjusted in mainland China. These infected couples were matched to uninfected couples who underwent IVF treatment during the period of the dynamic zero-COVID-19 policy in mainland China. IVF treatment outcomes were compared between the two groups, and the results showed that the blastocyst formation and available blastocyst rates were significantly decreased in couples who underwent IVF treatment 31~60 days after SARS-CoV-2 infection, implying that there is a potential adverse effect of SARS-CoV-2 on embryo development.
Several pathogens, such as hepatitis virus, human immunodeficiency virus, and Zika virus [27], may have variable impacts on the physiopathology of the reproductive organs, leading to infertility or poor ART outcomes [28]. Therefore, when the new SARS-CoV-2 virus emerged and spread globally, researchers focused on the impact of infection with this virus on human reproduction and ART outcomes [5]. The effects of SARS-CoV-2 infection on the laboratory and clinical outcomes of ART have not yet been consistently documented in the literature [14, 29, 30, 31]. An unclear infection status, the inability to correctly measure the time between SARS-CoV-2 infection and ART treatment, and the absence of a stratification analysis on the time of oocyte retrieval relative to SARS-CoV-2 infection could all be contributing factors. For instance, the pregnancy outcomes of patients who underwent IVF treatment before and during the COVID-19 pandemic were compared in the retrospective studies of Huri et al. [30] and Rageh et al. [32], but the authors failed to clarify whether the cohorts who underwent IVF treatment during the COVID-19 pandemic were infected with SARS-CoV-2. The largest retrospective analysis of IVF outcomes in SARS-CoV-2 patients to date was reported in a 2022 report from Israel [13]. By comparing the IVF data of 121 patients previously infected with COVID-19 and 121 uninfected patients, the researchers discovered that IVF treatment within one year after SARS-CoV-2 infection had no effect on the outcomes of fresh embryo transfer. Nonetheless, it should be highlighted that it was not made clear in this study whether the control group underwent rigorous testing for SARS-CoV-2 infection [13]. Furthermore, in another study, the same group reported that patients with previous SARS-CoV-2 infection who underwent frozen embryo transfer cycles with oocytes retrieved prior to infection had lower pregnancy rates, notably in those who had recovered fewer than 60 days before embryo transfer [33]. More importantly, the clinical outcomes of patients who underwent IVF during the acute period of SARS-CoV-2 infection are mostly described in case reports [17, 18]. As a result, more research on the laboratory and clinical outcomes of ART in patients during and after SARS-CoV-2 infection is needed.
We used propensity score matching in the current study to eliminate the imbalance in the number and distribution of participants between groups. As a result, our findings are far more persuasive and dependable. Notably, the blastocyst formation rates were significantly lower in couples who underwent IVF treatment 31–60 days after SARS-CoV-2 infection than in uninfected couples [50% (31.67%, 0.83.33%) vs 73.33% (50.00%, 92.31%)] and were also significantly lower than the benchmark value recommended by the Vienna consensus, which suggests that the blastocyst formation rate should be above 60% [34]. The rate of blastocyst formation is an essential key performance indicator (KPI) in embryo laboratories. This KPI is influenced by the whole culture system [34], female age [35], oocyte quality [36] and male sperm quality [37, 38]. We thoroughly checked the schedule of embryo laboratory staff and the culture medium used for embryo culture and discovered that the above conditions were constant over the study period. Furthermore, there was no difference in the age of female partners across subgroups and the uninfected group. As a result, we assumed that the lower rate of blastocyst formation in the subgroup who underwent IVF treatment 31~60 days after SARS-CoV-2 infection was due to SARS-CoV-2 infection. Further linear retrospective analysis supported this conclusion. The negative effects of SARS-CoV-2 infection on embryo developmental potential have already been reported in several small-sample retrospective studies. An observational study reported that the proportion of high-quality embryos in patients decreased after SARS-CoV-2 infection, according to a self-controlled analysis of 9 patients [14]. Another study found that couples undergoing IVF treatment in which only the male partner was infected with the SARS-CoV-2 virus also had lower blastocyst formation rates [16]. However, a recent prospective cohort study by Chen et al. [39] included 706 couples who underwent IVF treatment between 1 December 2022 and 11 January 2023, when China’s epidemic control policy was initially relaxed. Surprisingly, they reported that the infected patients had more normally fertilized oocytes than the noninfected patients, but no significant differences were observed between the two groups in oocyte outcomes, such as the number of oocytes retrieved, oocyte maturation rate and normal fertilization rate (these observations were similar to the results obtained in the current study). It is crucial to note, however, that the time of oocyte retrieval relative to the time of SARS-CoV-2 infection was less than 2 weeks in most patients in their study, and they also did not disclose the blastocyst formation rates or clinical pregnancy outcomes of the infected women.
The SARS-CoV-2 host receptors ACE2 and TMPRSS2 have been found in ovarian
tissues [40], oocyte cumulus complexes [41], oocytes [42], and blastocysts [10, 43]. An in vitro study further revealed that fluorescent reporter
virions pseudotyped with SARS-CoV-2 Spike (S) glycoprotein can infect
trophectoderm cells. However, SARS-CoV-2 mRNA has yet to be found in infected
patients’ follicular fluid [44], granulosa cells [18], oocytes [45], or semen
[46]. Therefore, we believe that the decrease in the blastocyst
formation rate in couples 31~60 days after SARS-CoV-2 infection
observed in the current study was more likely due to indirect effects of
SARS-CoV-2 infection. The decreased blastocyst formation rate may be attributed
to several potential causes. First, the SARS-CoV-2 virus can induce an
upregulation of proinflammatory cytokines and systemic oxidative stress in
infected individuals [47, 48], which may damage the human gonads. It has been
reported that the menstrual cycles of women and semen parameters of men
significantly changed approximately 2 months after SARS-CoV-2 infection [49, 50].
Approximately 30 days after SARS-CoV-2 infection, these damaging effects on the
gonads reach their peak [51]. Studies have shown that sperm progressive motility
and morphology are closely connected with the blastocyst formation rate [37, 52].
In the current study, we also found a significant increase in the proportion of
early rescue ICSI in the 31~60 days post-SARS-CoV-2 infection.
Second, during SARS-CoV-2 infection, the body develops neutralizing antibodies,
which peak 3–4 weeks after infection [53, 54]. A previous study showed that
anti-SARS-CoV-2 Immunoglobulin G (IgG) antibodies can be detected in follicular
fluid and in an in vitro experiment, the expression of steroidal acute
regulatory protein (StAR), estrogen receptor
There are some limitations in this study. First, it was a retrospective study, so various confounding factors are likely to affect the study results. The propensity-score matched (PSM) approach was used in the current study, and patients were matched for 9 basic characteristics at a ratio of 1:2 to exclude the influence of confounding factors as much as possible. However, some known or unknown confounding factors may still affect the statistical results. Second, to rule out the possibility of unknown and asymptomatic incubation periods, the current study included patients undergoing IVF treatment at different times as controls, resulting in the proportion of patients completing the first embryo transfer being different between the two groups, which may have an impact on the comparison of the clinical outcomes of the patients in the two groups. Third, due to the short follow-up period in the current study, data on the live birth rate of SARS-CoV-2-infected and uninfected patients undergoing IVF were lacking. In the future, we plan to continue follow up with our study cohort to determine the impact of SARS-CoV-2 infection on the cumulative live birth rate. Finally, there were no severe COVID-19 infected patients included in this study, which means that the results may not accurately represent the overall impact of SARS-CoV-2 infection on IVF treatment.
The results of the current study demonstrated that SARS-CoV-2 infection had no effect on the clinical pregnancy outcomes after the first embryo transfer cycle, but the couples who underwent IVF treatment 31~60 after SARS-CoV-2 infection had significantly lower blastocyst formation and blastocyst availability rates. Prospective studies are needed to confirm these findings. However, until more definitive evidence is available, it is appropriate to postpone IVF beyond 2 months, if possible, in couples with SARS-CoV-2 infection.
ART, assisted reproductive technology; SARS-CoV-2, severe acute respiratory syndrome coronavirus-2; COVID-19, coronavirus disease 2019; IVF, in vitro fertilization; PSM, propensity-score matched; WHO, World Health Organization; PHEIC, public health emergency of international concern; ACE2, angiotensin converting enzyme 2; BSG, basigin; TMPRSS2, transmembrane serine protease 2; CTSL, cathepsin L; IVF/ICSI, in vitro fertilization/intracytoplasmic sperm injection; COS, controlled ovarian stimulation; GnRH, gonadotropin-releasing hormone; CPOS, clomiphene-primed ovarian stimulation; uFSH, urine follicle-stimulating hormone; rFSH, recombinant follicle-stimulating hormone; hCG, human chorionic gonadotropin; RT-PCR, Real-time polymerase chain reaction; IQR, interquartile range; BMI, body mass index; AMH, anti-Müllerian hormone; KPI, key performance indicator.
The datasets used and analyzed during the current study are available from the corresponding author on reasonable request.
YLi, YLiu and HD conceived and designed the study. YLi, XD, DL, TL and HD contributed to acquisition of the data. YLi, YLiu and HD contributed to the analysis. YLi, TL, and HD contributed to the interpretation of the data. All authors contributed to editorial changes in the manuscript. All authors read and approved the final manuscript. All authors have participated sufficiently in the work and agreed to be accountable for all aspects of the work.
This retrospective study was approved by the Medical Ethical Committee of Union Hospital (no. 2023-S0462), and individual consent for this retrospective analysis was waived.
We would like to express our gratitude to Dr. Zhenyuan Chen for his statistical advice. We also would like to thank our colleagues at the Reproductive Medicine Center, Union Hospital, Tongji Medical College, Huazhong University of Science and Technology.
This work was supported by Hubei Provincial Natural Science Foundation of China (No. 2022CFB243).
The authors declare no conflict of interest.
References
Publisher’s Note: IMR Press stays neutral with regard to jurisdictional claims in published maps and institutional affiliations.


