Objective: To evaluate the effectiveness of uterine artery embolization
(UAE) with gelatin sponge particles for symptomatic focal and diffuse
adenomyosis. Materials and Methods: This was a retrospective study
conducted between January 2014 and December 2019. All women underwent UAE for
symptomatic adenomyosis without leiomyomas. Gelatin sponge particles were used in
all cases. Patients were assessed for effectiveness of symptom control, changes
in uterine volume, and degree of tumor necrosis on magnetic resonance (MR)
imaging. Results: One hundred and sixty-three patients underwent UAE.
There were statistically significant differences in bleeding score, pain score,
and uterine volume at three months after UAE (P
Adenomyosis is described as the ectopic growth of endometrial tissues into the myometrium with adjacent smooth muscle hyperplasia [1]. The prevalence of adenomyosis is 20.9% [2], and the two most common presenting symptoms are menorrhagia and dysmenorrhea [3]. Surgical hysterectomy is considered to be the only definitive treatment for patients with symptomatic adenomyosis [4]. Although conservative therapies such as hormone therapy (oral contraceptive pills, selective estrogen/progesterone receptor modulators, a levonorgestrel releasing intrauterine device, danazol, aromatase inhibitors) and minimally invasive therapy are also widely used in treating adenomyosis, hormone therapies are unable to achieve mass resorption, and symptom recurrence will occur when therapy is discontinued [5]. Other methods such as high intensity focused ultrasound (HIFU) have limited availability, relative high cost, unknown fertility outcomes, and strict indications [6].
Uterine artery embolization (UAE) on the other hand is minimally invasive, relatively low cost, allows preservation of uterus, and has fewer complications a low complication rate [7]. Therefore, UAE is more favourable compared with many hormone therapies and HIFU. Therefore, UAE is considered an alternative therapeutic method compared to many hormone therapies and HIFU.
UAE has emerged as a possible treatment option for patients with symptomatic adenomyosis [8, 9, 10]. Traditionally, UAE studies have used non spherical polyvinyl alcohol particles, with subsequent introduction of other embolic agents. These include tris-acryl gelatin microspheres (EmbosphereR), acrylamido polyvinyl alcohol microsphere, Bead Block, and spherical PVA microspheres (PVA; Contour SE) for symptomatic adenomyosis [8, 9, 10, 11, 12]. The disadvantages of non-spherical PVA particles were variation in the size of the particles and the tendency for them to aggregate resulting in obstruction of microcatheter and proximal vessel occlusion or unpredictable level of occlusion [13, 14]. Gelatin sponge particles have been used since 2001 as the primary embolic material in intervention radiology, and blood vessels occluded by gelatin sponge can be recanalized within several weeks [15]. Therefore, gelatin sponge particles are advantageous in that they are low-cost, temporary embolic agents that enable reintervention [15, 16].
There are few reports of UAE using gelatin sponge particles in the treatment of symptomatic adenomyosis [17].
Therefore, we aimed to investigate the effectiveness and safety of UAE with gelatin sponge particles for patients with symptomatic adenomyosis.
This retrospective study was approved by our Institutional Review Board
(approval number 2020-SCMC-02-012) and informed consent was waived. We reviewed
the medical records of patients who underwent UAE for symptomatic uterine
adenomyosis between January 2014 and December 2019. Their ages ranged from 30 to
53 years (median age, 42 years). Their body mass index ranged from 19 to 32.8
kg/m
Exclusion criteria were acute pelvic infection, pregnancy, gynecologic malignancy, endometriosis and contraindications or allergy to iodinated contrast medium. There were no cases of concomitant leiomyomas. Patients desiring future pregnancy were not excluded, and they were provided with information regarding potential benefits and risks associated with UAE. The follow-up period ranged from eight to 15 months (mean, 12. 3 months).
All patients underwent unenhanced and enhanced pelvic MR imaging with a 3.0-T
Ingenia unit (Philips Healthcare, Eindhoven, the Netherlands). Axial and sagittal
MR imaging were obtained before the procedure and at the 3-month follow-up. The
T1-weighted images were obtained using the following parameters: repetition time
(TR) msec/echo time (TE) msec, 570/10; field of view, 23 cm; matrix, 400
Adenomyosis was considered when diffuse (
 Fig. 1.
Fig. 1.MR images from a 30-year-old woman with focal adenomyosis. (1A) T2-weighted sagittal image shows asymmetrical thickening of uterine posterior wall (white arrow) with multifocal high signal spots. (1B) Gadolinium-enhanced T1-weighted sagittal image corresponding to (1A). (2A) T2-weighted sagittal image 3 months after embolization shows area of very low SI (white arrow). (2B) Gadolinium-enhanced T1-weighted sagittal image 3 months after embolization show no enhancement at the adenomyotic region (white arrow) suggesting complete necrosis.
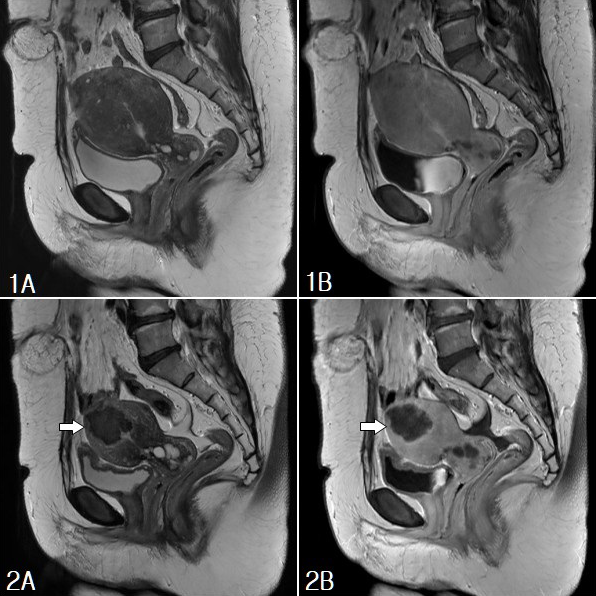 Fig. 2.
Fig. 2.MR images from a 44-year-old woman with diffuse adenomyosis. (1A) T2-weighted sagittal image shows diffuse enlargement of uterus with multifocal bright spots. (1B) Gadolinium-enhanced T1-weighted sagittal image shows diffuse enhancement of adenomyosis. (2A) T2-weighted sagittal image 3 months after embolization shows area of very low SI (white arrow) and marked decrease in uterine size. (2B) On gadolinium-enhanced T1-weighted image 3 months after embolization, non-enhancing portions (white arrow) are seen in uterus, suggesting partial necrosis.
A unilateral femoral artery approach was performed in all cases under local
anesthesia. A 5.0-F RUC catheter (Cook, Bloomington, IN, USA) was placed in the
internal iliac artery and a coaxial 3-F microcatheter (Stride Hi-flow; Asahi
Intecc, Osaka, Japan) was advanced distally into the uterine artery. Because of
the possible need for reintervention, embolization was performed only using
gelatin sponge particles (SPONGOSTAN; Johnson & Johnson, Skipton, UK) for
symptomaticadenomyosis. Before the embolization procedure, the gelatin sponge
particles were mixed with 40 mL of 1 : 1 saline solution-contrast agent mixture
(Iomeron {Iomeperol}; Bracco, Milano, Italy). A 40-mL mixture with 150-350
Pain within 24 hours of the procedure was primarily managed through an intravenous patient-controlled analgesia pump containing 1,500 mg fentanyl sulfate and 150 mg ketorolac tromethamine. Use of patient-controlled analgesia pump was started after the procedure in the angiography suite. Nonsteroidal anti-inflammatory drugs were additionally administered by intravenous injection if needed and oral analgesic agents were prescribed simultaneously.
Clinical response was assessed by questionnaire including symptomatic changes in
menorrhagia and dysmenorrhea before UAE, and at the 3-month and 12-month
follow-up visits. Number of used pads was used to quantify bleeding. Points were
assigned for bleeding based on the number of pads used and were categorized into:
0 points (no pad was used), one point (1-3 pads), two points (4-6 pads), three
points (7-9 pads), four points (10-12 pads), five points (13-15 pads), six points
(16-18 pads), seven points (19-21 pads), eight points (22-24 pads), nine points
(25-27 pads), 10 points (
Statistical analysis was performed with SPSS version 21.0 software (IBM
Institute, Chicago, IL, USA). Continuous variables were expressed as mean and SD.
Analyses were performed with Wilcoxon signed rank test for continuous variables
and Pearson’s chi-square tests or Fisher’s exact test for categorical variables.
A P-value
UAE was successfully performed in all 163 patients. The symptom outcomes and
changes in uterine volume are shown in Table 1. The median scores of menorrhagia
and pelvic pain at 12 months were reduced from 8 (6-9) to 2 (1-6) and from 7
(5-9) to 2 (1-6), respectively (P
| Pre procedure | 3-month follow-up | 12-month follow-up | |||
| (n = 163) | (n = 163) | (n = 102) | |||
| P value | P value | ||||
| Age (years) | 42 (30-53) | ||||
| Body mass index (kg/m |
23.71 (18.97-32.77) | ||||
| Parity (no.) | 1 (0-3) | ||||
| Hb (g/dL) | 8.25 (3.80-10.00) | 12.7 (9.20-14.70) | 12.1 (10.7-14.2) | ||
| WBC (10 |
5.37 (2.12-9.75) | 5.48 (2.93-11.52) |
0.425 | ||
| CA125 (U/mL) | 74.56 | 45.87 | 30.25 | ||
| (6.37-653.00) | (6.21-450.10) | (6.01-78.39) | |||
| Bleeding score | |||||
| Focal type (n = 46) | 7 (6-9) | 2 (2-6) | 0.004 | 2 (2-5) | 0.004 |
| Diffuse type (n = 56) | 8 (6-9) | 2 (1-6) | 0.007 | 2 (1-6) | 0.007 |
| Overall (102) | 8 (6-9) | 2(1-6) | 2 (1-6) | ||
| Pain score | |||||
| Focal type (n = 45) | 7 (5-9) | 2 (1-6) | 0.007 | 2 (1-5) | 0.006 |
| Diffuse type (n = 50) | 7 (5-9) | 2 (1-6) | 0.026 | 2 (1-6) | 0.02 |
| Overall (n = 95) | 7 (5-9) | 2 (1-6) | 2 (1-6) | ||
| Uterine volume (cm |
|||||
| Focal type (n = 78) | 242.8 (100.3-610) | 130.6 (58.9-460) | 0.001 | ||
| Diffuse type (n = 85) | 310.4 (180.8-688.8) | 173.3 (100-652.1) | 0.012 | ||
| Overall (n = 163) | 274.9 | 138.05 | |||
| (100.3-688.8) | (58.9-652.1) | ||||
Of the 163 patients, 78 patients had focal adenomyosis and 85 had diffuse adenomyosis. Complete necrosis of adenomyosis after UAE was seen in 109 patients (66.9%), partial necrosis was seen in 45 patients (27.6%), and no necrosis was seen in nine patients (5.5%) (Table 2). Statistically significant differences were found in the occurrence of complete necrosis between focal adenomyosis and diffuse adenomyosis (P = 0.023).
| Necrosis | ||||
| n | Complete | Partial | None | |
| Focal adenomyosis | 74 | |||
| Recurrent dysmenorrhea | 4 | 0/74 (0%) | 2/74 (2.7%) | 2/74 (2.7%) |
| Recurrent menorrhagia | 2 | 0/74 (0%) | 1/74 (1.4%) | 1/74 (1.4%) |
| Diffuse adenomyosis | 81 | |||
| Recurrent dysmenorrhea | 8 | 2/81 (2.5%) | 3/81 (3.7%) | 3/81 (3.7%) |
| Recurrent menorrhagia | 7 | 0/81 (0%) | 3/81 (3.7%) | 4/81 (4.9%) |
Symptom recurrence occurred in 20.6% of patients at 12 months’ follow-up after UAE (Table 2). Three patients had a hysterectomy. Patients who had focal adenomyosis with complete necrosis had no recurrent menorrhagia and dysmenorrhea. Of the nine patients with no necrosis after UAE, three patients exhibited no improvement in clinical symptoms after UAE and four patients had recurrent symptoms.
Ten patients with complete and partial necrosis of adenomyosis experienced transient amenorrhea. However, most patients resumed menstruation within seven months. Two patients aged 47 years and 50 years did not resume menstruation until 12 months after UAE. There were 98 women of childbearing age before the procedure, and twelve of them Twelve women attempted natural pregnancy and three women attempted artificial reproduction after procedure. Three women succeeded in becoming pregnant, one of whom underwent a natural pregnancy and the other two underwent artificial reproduction. One woman who conceived naturally, delivered a full-term baby. Two women who became pregnant with artificial reproduction had one miscarriage and the other had follow-up loss. Three women succeeded in becoming pregnant. One woman conceived naturally and delivered a full-term baby. Two women became pregnant after artificial reproduction, one had a miscarriage at 6 weeks, the other was lost to follow up.
There was no procedure related complications. Four patients complained of allergic reaction or rash, a minor complication, and they recovered with appropriate medications. Three other patients who reported symptoms of urinary tract infection after discharge were also recovered with medication. Two patients complained of urinary retention, and they recovered with conservative managements. There were no major complications that required readmissions.
Gelatin sponge is inexpensive and has been used as a safe and effective embolic agent for more than 30 years in UAE for some uterine disorders [22, 23]. Despite their merits, gelatin sponge particles have recently become available as an approved embolic agent in Korea.
It has been reported that UAE offers significant short- and long-term
improvements in symptoms for both pure or combined adenomyosis [11]. In our
study, there were significant symptom improvements or uterine volume reduction,
(P
While we found complete necrosis of adenomyosis in 66.9% of patients in the current study, the corresponding estimates reported by Kim et al. [24] with nonspherical polyvinyl alcohol particles and Lohle et al. [25] with calibrated tris-acryl gelatin microspheres were 82.5% and 44.1%, respectively. Our findings of statistically significant differences in complete necrosis between focal adenomyosis and diffuse adenomyosis (P = 0.023) is inconsistent with estimates reported by Kim et al. [24] who found no significant differences in the occurrence of complete necrosis between focal adenomyosis and diffuse adenomyosis. We believe that these differences may be related to differences in embolic material characteristics, sample size, and utero-ovarian anastomoses [26]. Unlike leiomyomas, previous studies with pathologic examination of specimens showed that embolic materials are randomly distributed in the myometrium in adenomyosis, and blood vessels feeding adenomyosis are not clearly defined [27, 28].
Pelage et al. [29] performed embolization with PVA particles or
tris-acryl gelatin microspheres and reported that eight (53%) of 15 women had
complete resolution at 1-year follow-up. In our study, 20.6% of patients had
symptom recurrence at 12 months’ follow-up. We assume that the discrepancy
between these studies may be related to differences in embolic material used.
Pelage et al. [29] and Kim et al. [24] used permanent embolic
materials, such as PVA particles or tris-acryl gelatin microspheres, with
variable diameters of 150-250
Occurrence of complete necrosis of adenomyosis is thought to be positively associated with embolization [30, 31]. When adenomyosis had complete necrosis after UAE, there was no recurrence of menorrhagia. Only two out of 38 patients (5.7%) with diffuse type adenomyosis had recurrent dysmenorrhea in our study. This result was consistent with those reported by Kim et al. [24]. Therefore, we believe that achievement of complete necrosis of adenomyosis is the target in UAE for symptomatic adenomyosis.
A previous study by Kim et al. [32] using gelatin sponge particles, which assessed ovarian reserve using AMH after UAE for symptomatic uterine fibroids, also reported that UAE influenced ovarian function, but younger ovaries had greater capacity for recovery after ovarian damage. Therefore, we speculate that a variety of factors, including utero-ovarian anastomosis, embolic agent size, embolic agent type, extent of embolization, and the endpoint of embolization, may be associated with ovarian damage [12, 33].
In our study, one patient with complete necrosis of focal adenomyosis, a 30-year-old woman who desired future pregnancy, succeeded in becoming pregnant. Twenty-four months after UAE, this woman delivered a full-term baby. However, Liang et al. [34] reported pregnancy following UAE for adenomyosis is likely to be complicated and cannot be recommended at this time. So, larger studies should be performed for more conclusive results for patients wishing to preserve fertility.
In the present study, eight patients developed transient amenorrhea. Two patients over 47 years of age did not resume menstruation until 12 months after UAE. The frequency of minor complications was comparable with that of other studies. There were no major complications after UAE with gelatin sponge particles.
Our study has some limitations. Firstly, a significant number of patients were lost to follow up. This may have induced a potential bias. Secondly, we only included patients with adenomyosis without myoma. However, adenomyosis and myoma often coexist. Therefore, the results are not necessarily valid for all women with adenomyosis. Thirdly, the current study was conducted at a single institution with a relatively short follow-up period. So, multicenter study should be conducted to confirm these findings. Finally, this study was not a comparison study, therefore, further randomized controlled trials to compare the effects of UAE with non-spherical polyvinyl alcohol particles on imaging and clinical outcomes with those of UAE with gelatin sponge particles among patients with symptomatic adenomyosis are needed.
Despite its limitations, UAE using gelatin sponge particles is an effective and safe treatment for symptomatic adenomyosis without leiomyomas. Patients with focal adenomyosis with complete necrosis after UAE had no symptom recurrence at midterm follow-up.
YG and MO designed the research study. JY and C-W performed the research. YG and JY analyzed the data. YG, MO and JY wrote the manuscript. All authors contributed to editorial changes in the manuscript. All authors read and approved the final manuscript.
This retrospective study was approved by Samsung Changwon hospital Institutional Review Board (SCMC 2020-02-012) and informed consent was waived.
We would like to acknowledge Mi Hyeon Jin’s (Department of Biostatistics, Samsung Changwon Hospital, Sungkyunkwan University School of Medicine) assistance with statistical analysis.
We certify that there is no conflict of interest with any financial or other potential conflict of interest.
