1 Allergy Department, 2nd Pediatric Clinic, National and Kapodistrian University of Athens, Panagiotis, and Aglaia Kyriakou Children's Hospital, 11527 Athens, Greece
2 Department of Dermatology and Venereology, Faculty of Medicine, National and Kapodistrian University of Athens, Andreas Sygros Hospital, 16121 Athens, Greece
3 Allergy Unit, 2nd Department of Dermatology and Venereology, Medical School, National and Kapodistrian University of Athens, Attikon University Hospital, 12462 Athens, Greece
Abstract
Atopic dermatitis (AD) is a recurrent, chronic, inflammatory, itchy skin
disorder that affects up to 20% of the pediatric population and 10% of the
adult population worldwide. Onset typically occurs early in life, and although
cardinal disease features are similar across all ages, different age groups and
ethnicities present distinct clinical characteristics. The disease imposes a
significant burden in all health-related quality of life domains, both in
children and adults, and a substantial economic cost both at individual and
national levels. The pathophysiology of AD includes a complex and multifaceted
interplay between the impaired dysfunctional epidermal barrier, genetic
predisposition, and environmental contributors, such as chemical and/or
biological pollutants and allergens, in the context of dysregulated T
Keywords
- atopic dermatitis
- atopic eczema
- pathophysiology
- skin barrier disruption
- immunopathogenesis
- skin microbiome
- exposome
- endotypes
Atopic dermatitis (AD) is the most common inflammatory skin disorder, affecting up to 25% of children and 10% of adults, depending on the geographical area [1]. Although almost 85% of AD cases appear before the age of 5 years, the onset of the disease in adults is not uncommon, with almost 25% of the patients reporting symptoms only after adulthood. The characteristic clinical features of the highly pruritic eczematous lesions, consisting of papules and patches and the subsequent exudation and excoriation in the acute phase as well as the chronic lichenified, hyperpigmented lesions are similar across all ages, although distinct clinical characteristics present across different age groups and ethnicities [2]. Even though AD is not associated with mortality and is therefore underreported compared to other fatal diseases, it imposes a significant morbidity burden due to the humanistic and psychosocial effects, both for patients and their families [3].
The two previously main pathogenetic hypotheses, the ‘outside–in’ and the
contrasting ‘inside–out’, which prioritize either the epidermal barrier
dysfunction or the dysregulated immune activation as the primary trigger in the
pathophysiology of AD, are now integrated into a complex and multifaceted model,
including the genetic component and, the effect of environmental pollutants, in
the context of a dysregulated T
The evolution of endotypes in AD and the ongoing research on the determination of non-invasive biomarkers have emerged as an important step toward targeted therapies for personalized treatment in AD patients [9]. This review aims to present state-of-the-art knowledge on the complex, multifactorial, and interactive mechanisms that contribute to the vicious cycle of the pathophysiology of AD and present up-to-date therapeutic interventions.
The dysregulated T cell-mediated immune response, including different patterns
of cytokine release, has a strong and robust role in the pathogenesis of AD. The
disrupted skin barrier enhances exposure to environmental allergens, which can
either activate skin antigen-presenting cells, such as the inflammatory dendritic
epidermal cells (IDECs), resulting in the subsequent “allergic response”, or
induce the chemokine milieu from keratinocytes, such as the thymic stromal
lymphopoietin (TSLP), and interleukins (IL)-23, IL-25, and IL-33, reinforcing the
T2 response and the induction of IL-4 and IL-13, IL-31 cytokines though type 2
human innate lymphoid cells [10]. This, in turn, promotes the class switch of B
cells to plasmacytes toward specific IgE induction. Nevertheless, in chronic AD
cases, a T
IL-4 and IL-13 represent the two main T2-cytokines associated with AD
pathogenesis. In addition to promoting T2 responses and recruiting
eosinophils, they damage the skin barrier by downregulating the expression of
structural proteins such as filaggrin, loricrin, and lipids, while they
concomitantly increase collagen disposition, resulting in skin remodeling and
lichenification. Moreover, they contribute to the neurogenic itch by directly
stimulating pruritogenic sensory neurons, as will be further discussed later
[12]. IL-4 and IL-13 also stimulate the expression of 3
The Janus kinase/signal transducer and activator of transcription (JAK/STAT)
signaling pathway is significant in the pathogenesis of AD and inflammation. The
JAK family consists of four intracellular kinases, JAK1, JAK2, JAK3, and TYK2,
which are activated in pairs when cytokines bind to their respective receptors
[20]. Specifically, JAK1 mediates the IL-4, IL-5, IL-13, IL-22, TSLP, and
IFN-
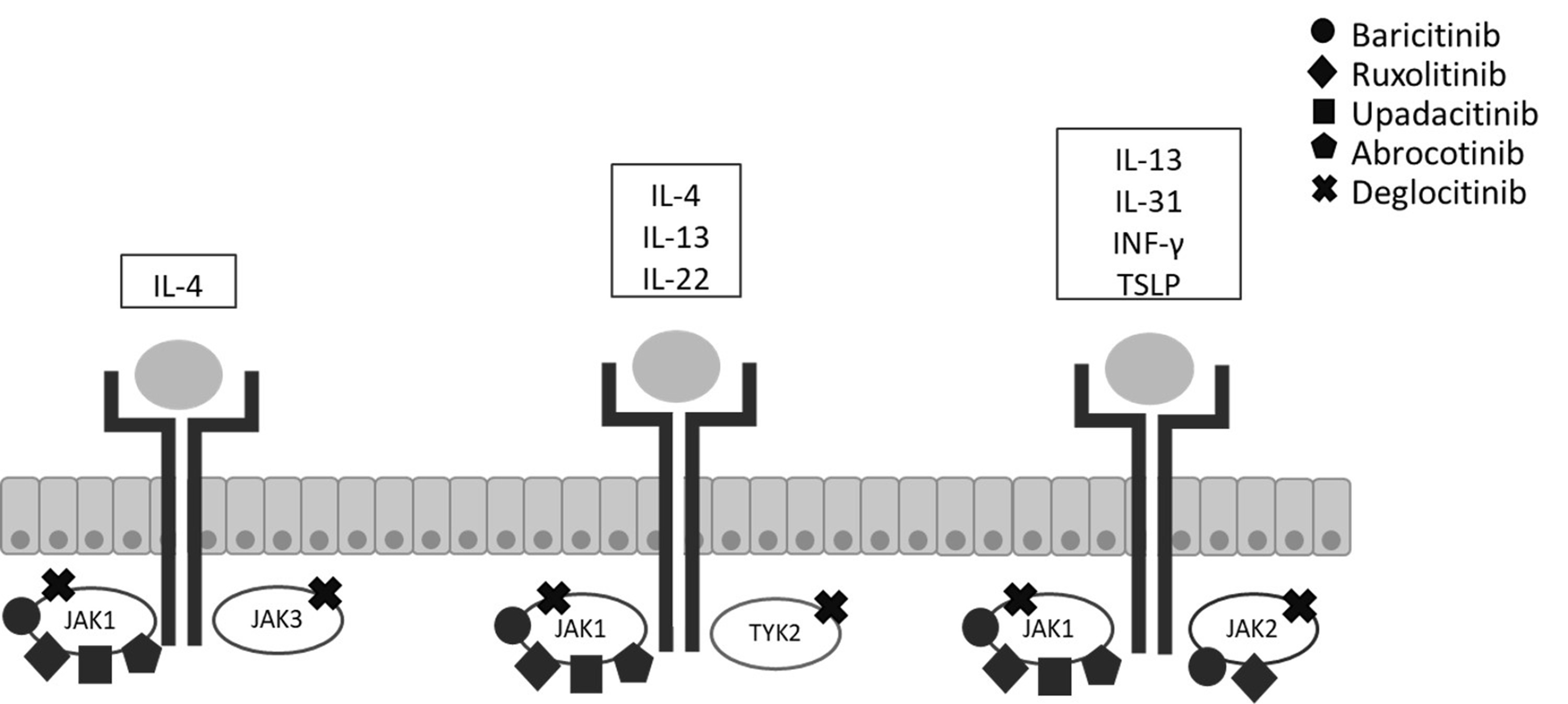 Fig. 1.
Fig. 1.Janus kinase/signal transducer and activator of transcription
(JAK/STAT) inhibitors in atopic dermatitis (AD) inflammatory pathway. IL,
interleukin; IFN-
In addition to epithelial damage and allergen exposure activating the
T
Regarding other mediators involved in the pathogenesis of AD, IL-18, a
proinflammatory cytokine stimulated by epithelial damage and staphylococcal
colonization, promotes T2-mediated inflammation by activating basophils and mast
cells. Elevated IL-18 levels have been associated with increased AD morbidity,
while IL-18 deficiency in murine models ameliorated AD skin lesions by decreasing
IL-4 levels and mast cell infiltration [33, 34]. Nevertheless, its pleiotropic
function in AD has not been fully elucidated. Moreover, high serum IL-21 levels
in AD patients, primarily produced by T
The increased phosphodiesterase 4 (PDE4) activity observed in AD results in the
reduction of intracellular cyclic adenosine monophosphate (cAMP), a negative
regulator of cytokine production, leading to the augmented production of
proinflammatory mediators and cytokines transcription involved in acute and
chronic inflammation. Preventing cAMP breakdown by inhibiting PDE4 suppresses
proinflammatory cytokines, such as tumor necrosis factor-
Innate and adaptive immune cells, such as basophils, eosinophils, and
macrophages, contribute highly to AD pathogenesis. Basophils participate in the
initiation of AD through increased expression of IL-4 and interactions with
keratinocytes and dermal macrophages, resulting in epidermal hyperplasia and skin
barrier dysfunction [42]. Circulated eosinophils in patients with AD express
increased and upregulated histamine receptor 4 (H
The dysregulated immune response in AD is intricate and multidimensional, affecting the antigenic response, the induction of inflammation, the disruption of the cutaneous architectural integrity, and pruritus. Rectifying the imbalanced immune response holds potential advantages in the pathophysiological facet of AD and potentially the progression of an atopic march.
The cardinal role of epidermal barrier dysfunction in the induction and perpetuation of AD is well established. The “leaking epithelial barrier” results in chronic peri-epithelial inflammation in the epithelium-lined human organs, including the skin, the gastrointestinal and respiratory systems, and, consequently, in certain autoimmune, metabolic, and neuropsychiatric diseases [48]. Primarily, the skin acts as a barrier for physical, chemical, and microbial agents; thus, for impairment, a dysbiotic microbiota, impaired remodeling, local immune responses, and increased TEWL facilitate the penetration of allergens and translocation of microbiota to the subepithelial areas, subsequently activating systemic immune responses and prolonging chronic epithelial damage.
The epithelial barrier consists of four cell layers: The stratum basal, the stratum spinosum, the stratum granulosum (SG), and the stratum corneum (SC) within the epidermis. The SC is a semipermeable barrier in the outer part, consisting of corneocytes embedded in a protein-loricrin (LOR) and involucrin- shell, called an envelope, and surrounded by lipids, such as free fatty acids, ceramides, and cholesterol [49]. During the differentiation of keratinocytes, the released keratin (KRT)-1 and KRT-10 in the spinum and the granular layer of the epidermis contribute to the consistency of keratinocytes. In the context of T2 dominance in AD patients, decreased levels of KRTs, desmoglein (DSG)-1 and desmocolline (DSC)-1, and epidermal differentiation-related molecules have been observed [45].
Moreover, alterations in lipid synthesis, lipid content, and structure reduction in AD patients further compromise skin integrity [50]. The lipid chain length of ceramides and free fatty acids and the levels of elongases 3 and 6 (ELOVL3, ELOVL6), which play a significant role in lipid chain elongation, is decreased in both the lesional and non-lesional AD skin [51, 52]. Expression of the elongases is also downregulated by IL-4 and IL-13 under the control of STAT6, suggesting a crosstalk between the inflammatory and the barrier components in AD [51]. Alterations in enzymic expression in AD have also been reported for stearoyl Coa desaturase, SCD, ELOVL1, aSmase, GBA, and CerS3, further enhancing lipid abnormalities [52].
Filaggrin (FLG) is an important structural protein responsible for the keratinocyte shaping and positioning of the cytoskeletal components. During FLG degradation, the newly formed urocanic acid and pyrrolidine carboxylic acid contribute to SC hydration, thus, preserving skin integrity [53]. Loss-of-function FLG gene mutations are the most important genetic risk factors for AD due to alterations in lipid delivery, the decrease in FLG monomers, and natural moisturizing factors produced by FLG metabolites [54, 55], while the resulting altered skin pH leads to impaired lipid construction and cell apoptosis [56]. Furthermore, FLG and LOR, involucrin, and keratins 1,10 are downregulated in the presence of T2 inflammation cytokines, such as IL-4, IL-13, IL-22, and IL-31, in a process mediated by OVO-like 1 (OVOL1), an upstream transcription factor for these proteins [49, 57]. The T2 cytokines and IL-25 downregulate the expression of corneodesmosin, potentially contributing to increased viral penetration [58].
Specifically, OVOL1 activation induces translocation from the cytoplasm to the nucleus and upregulates FLG, while interference by the inflammatory cytokines on OVOL1 decreases FLG expression [59]. IL-13 also inhibits involucrin in an OVOL1-independent way, promoting barrier dysfunction [60], while it reduces the expression of skin barrier proteins and lipids by acting on keratinocytes, regulating the expression of metalloproteinase (MMP)-9 [61]. The IL-4/IL-13 inflammatory pathway blockade with dupilumab has been shown to restore epidermal barrier properties and improve skin hydration [62]. Importantly, the data indicate a restorative effect of dupilumab in AD by progressively ameliorating systemic and cutaneous abnormalities [63].
Granzyme B, an apoptotic protease, also increases skin-barrier permeability through the fracturing of FLG and E-cadherin [64], while upregulated enolase-1 (ENO-1) leads to tight junction defects due to abnormal keratinization [65].
Tight junctions (TJs) form a complex intracellular barrier in the SG, while claudin is the major adhesion structural protein in TJs. Downregulation of claudins and the presence of single nucleotide polymorphisms in the CLDN1 gene lead to TJ defects and increased TEWL in patients with AD [66].
Emerging therapeutic modalities aiming at epidermal barrier functionality restoration by decreasing epidermal hyperplasia, cytokine infiltration, and increasing skin-barrier protein production, such as spirodelapolyrhiza (SPE) and Olea europaea leaf extract (OLE), have been proposed [67]. Glucoseskin application in high concentrations can increase claudin-1 and FLG production [68], while Cimifugin, a bioactive Chinese herb, and the orally administrated PAG (DL-propargylglycine) improve TJs function by suppressing allergic inflammation [69, 70]. In an ex vivo model, the microorganism component Aquaphilus dolomiae induced immunomodulatory and antimicrobial peptides, thus, indirectly restoring skin barrier integrity when applied in cell cultures obtained from patients with AD [71]. Delgocitinib, a JAK kinase inhibitor, in an ointment formulation, ameliorates TJ function without eliminating claudin expression [72], and bortezomib, a proteasome inhibitor, upregulates claudin-1 expression [73].
Aryl hydrocarbon receptor (AHR) is a ligand-dependent transcription factor that controls skin barrier protein activation by regulating the epidermal differentiation complex (EDC) [74]. Several plant-based extracts have shown beneficial effects through binding to AHR and upregulating the expression of barrier protein genes and skin integrity, such as tapinarof, a small molecule produced by bacteria, diosmin, a natural agonist derived from the Rutacae family, and other medical remedies, such as Rhodiola crenulate and Artemisia princeps [60, 75, 76, 77]. It has been postulated that AHR antagonists increase the production of FLG, involucrin, and LOR via the OVOL-1 transcription factor pathway [60].
The epidermal barrier plays a pivotal role in AD by serving as the primary defense mechanism against external irritants and allergens. Thus, agents that restore and maintain an intact barrier are important.
Skin is inhabited by a complex community of bacteria, fungi, and viruses, which constitute the skin microbiota and impose immunomodulatory and protective effects against pathogenetic microbes [78]. The skin microbiome in AD patients is dysbiotic, defined by imbalanced bacterial composition and diversity [57, 79], with reduced commensals, while the increased number of skin pathogens has been positively associated with AD severity [80]. Staphylococcus (S). epidermidis represents the most abundant species in human skin, facilitating the defense against other pathogens and contributing to skin epithelialization, while such responses are also induced by Corynebacterium, Propionibacterium, and Streptococcus sp. [81]. Microbiome dysbiosis in AD impairs immune responses and, in response to the exposome effects, contributes to the “leaking epithelium”, the subepithelial translocation of dysbiotic microbiota and opportunistic pathogens [82]. However, whether skin leakage precedes microbial dysbiosis or vice versa remains controversial.
In infancy, skin colonization with commensal S. epidermidis promotes tolerance mechanisms via the induction of regulatory T cells. On the contrary, in the predominance of S. aureus, which can penetrate via the epidermis more so through a disrupted epithelial barrier, via its superantigen components, a promoted B cell differentiation and induction of T2 cytokines, such as IL-4, IL-13, IL-22, and TSLP, is noted [83]. Furthermore, excessive colonization of S. aureus on the skin leads to biofilm formation and secretion of virulence factors, which further stimulate keratinocytes and Langerhans cells to release T2 inflammatory responses [84, 85]. Biofilm propensity by S. aureus and S. epidermidis has been positively associated with AD severity and epidermal dysfunction [86].
The epidermal fungi, although not considered direct pathogenetic agents, contribute to AD initiation and exacerbation. Specifically, in Candida sp., C. albicans, and C. parapsilosis, colonization is increased in AD patients compared to healthy adults, while Malassezia species, especially M. restricta, M. globose, M. furfur, and M. sympodialis, are frequently detected in AD lesions during disease flares [87]. Ruxolitinib has been shown to reduce Malassezia in an in vitro skin model; however, data on the effect of JAK inhibitors in the microbiome of AD patients is limited [88]. Patients with increased AD morbidity are significantly more often colonized with non-Malassezia species and with an increased diversity of fungi species, including Alternaria, Aureobasidium, Aspergillus, and Cladosporium sp. [89, 90]. Finally, Ascomycota AD skin colonization is related to higher IgE titers and aggravation of AD severity [91]. Of note, colonization with fungi is site-dependent, i.e., Malassezia sp. being more abundant in the scapula; this phenomenon is potentially associated with variations in TEWL [92].
Treatment options might influence both dysbiosis and dysbiosis-associated inflammation. Bleach baths with sodium hypochlorite in bathing water containing oil are still recommended as a treatment option in the most recent European Academy of Dermatology and Venerology (EADV) guidelines [93], although a recent meta-analysis concluded that their beneficial effect through a decrease in S. aureus colonization, per se, is not adequately documented. Thus, they should be used cautiously since adverse effects might be noted [94].
The emollient application can ameliorate AD symptoms by decreasing S. aureus colonization and increasing microbial variety in the skin [95]. In most AD cases, emollient “plus” products combine vehicles and active components using substantial efficacy data. Emollient formulas of 1% colloidal oat or 5% Vitreoscilla filiformis lysate cream decrease the S. aureus population and increase skin microbial richness [96, 97]. However, the long-term effect of emollients on the microbiome and skin pH is still debated [98, 99].
Autologous microbiotherapy is an evolving treatment option with satisfactory
results and only minor adverse effects [100]. S. aureus can be decreased
by other coagulase-negative Staphylococcus sp. (S.
epidermidis, S. hominis, S. warneri, S. capitis) that can grow on the healthy
skin of AD patients [101]. Roseomonas mucosa, a Gram-negative skin
commensal, contributes to tissue repair through sphingolipid production and
stimulating cholinergic signaling and to flagellin expression through the
TNF-mediated signaling pathway, thereby ameliorating AD symptoms [102, 103].
Nitrosomonas eutropha, an ammonia-oxidizing bacteria, suppresses the
T
IL-13 decreases antimicrobial peptides and promotes epidermal dysbiosis [106]. In this respect, the anti-IL4/IL-13 monoclonal antibody, Dupilumab, improves skin dysbiosis by inhibiting S. aureus growth and restoring microbial skin dysbiosis; meanwhile, it also increases S. epidermidis and S. hominis [62, 107].
The key role of skin microbiome dysbiosis in the integrity of the skin barrier and the interplay between microbiome, exposome, skin-barrier leakage, and host immune response highlights the necessity for targeted interventions aiming at rebalancing the skin microbiome.
The role of the exposome in the multidimensional model of AD pathogenesis has recently been explored. The concept of the exposome was introduced in 2005 by Wild et al. [108], highlighting the bidirectional interaction of the external environment and human health and disease, complementing the gene—environmental associations in the pathogenesis of allergic diseases. Exposome refers to the total of the environmental exposures that an individual experiences throughout a lifetime and their effect on their health outcomes (Fig. 2). The recently introduced “metaexposme” includes the complete set of environmental factors that impact halobionts, encompassing a holistic perspective of the policies and practices that shape the environment [109]. Within this concept, distinct exposures include allergens, pollutants, irritants, lifestyle choices, diet, stress, socioeconomic parameters, climate change, microbial agents, etc. [110]. The exposome is further classified, with a high degree of overlap, as the general external: Climate, biodiversity, urbanization, and socioeconomic contexts; the specific external: allergens, pollutants, tobacco smoke, diet, lifestyle factors, and microbes; the internal: Inflammation, metabolism, and oxidative stress exposome [111]. The exposome is the “master regulator” in the interplay between a disrupted and “leaky” epithelium barrier, microbiome, genome, and immune dysregulation in AD [112]. In a simplified model, the exposome contributes to AD pathogenesis by disrupting the epithelium barrier, contributing to the crosstalk with the disturbed skin microbiome, and through epigenetic regulation of the genome of predisposed individuals. The leaky epithelium initiates a vicious cycle of chronic inflammation in AD, which is further supported by microbiome translocation and imbalance under the concept of epithelium barrier hypothesis, as previously described [48].
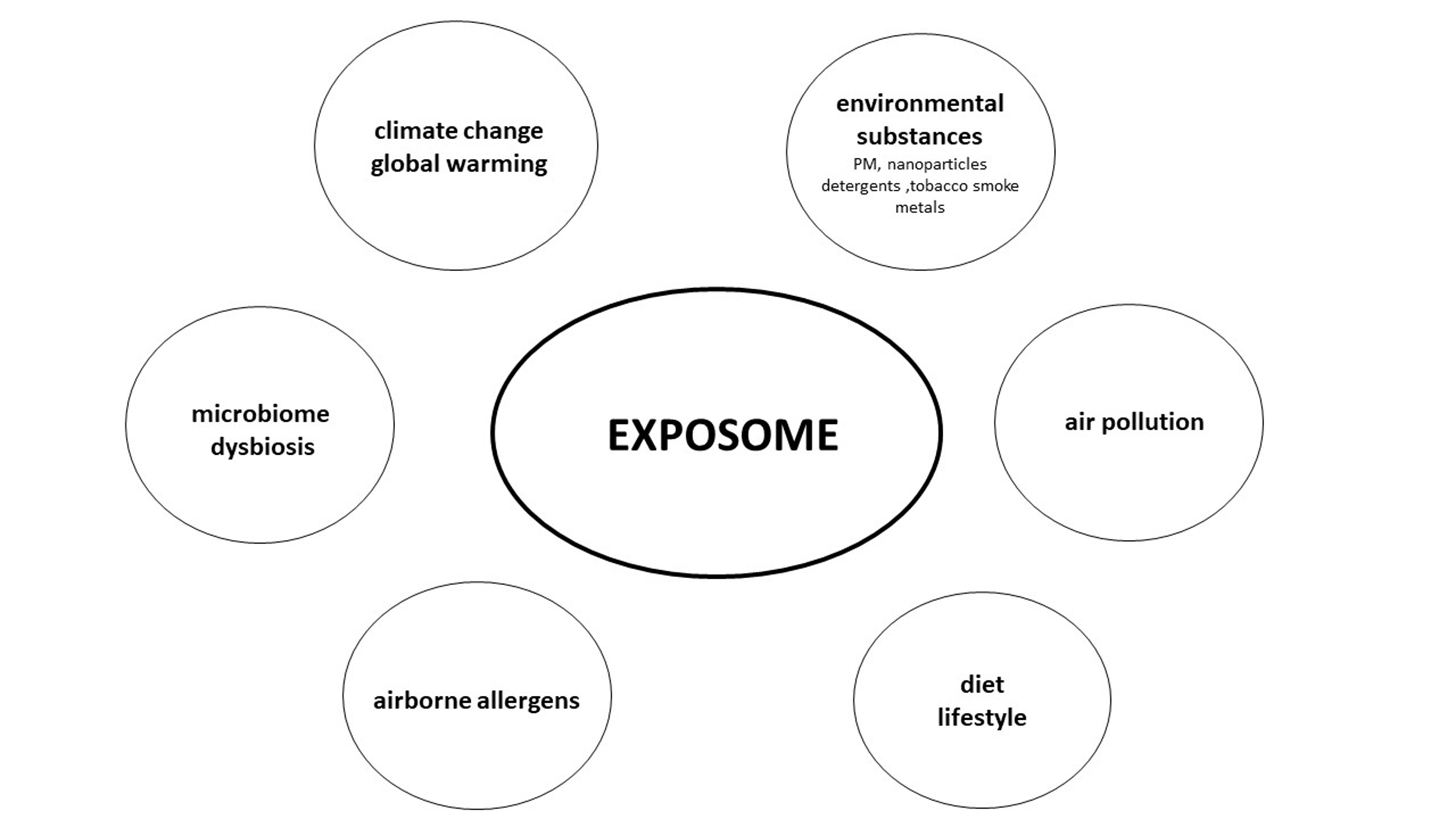 Fig. 2.
Fig. 2.Factors that modulate the exosome and participate in the pathophysiology of AD.
As part of the external exposome, global warming and climate change impact the
development and exacerbation of AD. Floods caused by global warming and polar ice
melting are associated with an increased risk of emergency visits due to
increased morbidity and severity of AD in children. It is plausible that floods
increase humidity, environmental dampness, allergen levels in the environment,
indoor molds, and contaminated water, thereby contributing to AD exacerbation in
sensitized children [113]. Exposure to increased levels of relative humidity
means daily temperatures, precipitation, nitrogen dioxide (NO
It is well established that exposure to synthetic detergents is associated with an increased risk of work-related eczema, e.g., in professional cleaners, potentially through increased TEWL [121]. Noteworthy, during the COVID-19 pandemic, the augmented use of disinfectants resulted in an increased number of AD cases and exacerbations [122].
Tobacco smoke, one of the most toxic substances in the environment, affects not only the epithelium in the airway but also the integrity of the skin barrier. Active or passive exposure to tobacco smoke is associated with an increased prevalence of AD in childhood by directly inhibiting Tregs function and impairing their ability to secrete the anti-inflammatory cytokine IL-10 following exposure to benzene [123].
Most importantly, climate change has altered and prolonged pollen season,
whereas air pollution determinants, such as NO
Westernization in dietary habits has been consistently associated with AD development and severity [127]. Increased consumption of processed foods is correlated with AD severity, while low vitamin C and E intakes are inversely associated with AD [128, 129]. Meanwhile, the relationship between fatty acid intake and AD remains controversial [130, 131].
In summary, the exposome, representing a lifetime of environmental exposures, is a key factor in the complex model of AD pathogenesis. As highlighted by the exposome, the bidirectional interaction between the external environment and human health disrupts epithelial barriers, chronic inflammation, and immune dysregulation in AD. Addressing these diverse exposome components is vital for developing comprehensive strategies to mitigate the risk and progression of atopic dermatitis.
The pathogenetic mechanism in chronic itching, which is a hallmark and the most troublesome symptom in AD, is multifactorial and occasionally individualized [132]. It is well established that the itch in AD is mainly mediated via non-histaminergic pathways; thus, histamine and the respective bioactive amines contribute minimally to the itch pathogenesis, while type 2 cytokines (IL-4, IL-13, IL-31), epithelium alarmins (TSLP, IL-33, IL-25), neuropeptides, neurotrophins, the vicious “itch–scratch cycle”, and microbiome dysbiosis with epithelium leakage, act synergistically in chronic pruritus [45, 133].
The discovery of the IL-4 receptor subunit a (IL-4Ra) on pruritus-sensing nerves has signaled a new era in the chronic itch pathogenesis by demonstrating that type 2 ILs can directly activate sensory nerves via the JAK1–2/STAT pathway [134]. Moreover, IL-4 and IL-13 induce kallikrein (KLK-7) in normal keratinocytes, which mediates the itch pathogenesis via skin–neural mechanisms [135]. IL-4 has an additional role in AD pruritus by enhancing neural responsiveness to pruritogens [134], which by definition include biogenic amines, proteases, and neuropeptides, which in turn activate afferent dorsal ganglion neurons and receptors such as TRPV1 and TRPA1 [136]. Subsequently, new therapeutic targets aiming at inhibiting IL-4R using monoclonal antibodies and JAK inhibitors are developed [137, 138], while the inhibition of IL-13 using monoclonal antibodies attenuates the itch in AD [18, 19].
The T2 cytokines, IL-4, IL-13, and IL-31, act through the TRP channel ankyrin transmembrane protein 1 (TRPA1) and the transient receptor potential (TRP) channel vallinoid 1 (TRPV1) by activating the calcium influx in the sensory fibers [134], while TSLP acts directly on the sensory nerves by binding to its receptor. The release of TSLP by epidermal cells is upregulated by activated T cells and crosstalk with other immune cells [139]. TRP channels, responsive to both intracellular and extracellular signals, chemical compounds, mechanical stimuli, temperature fluctuations, and osmotic stress, contribute to sensory perception and play a role in AD. Furthermore, activation of the TRPV3 and T cells can further augment TSLP production and the itch sensation [140]. The anti-TSLP monoclonal antibody, tezepelumab demonstrated a substantial, yet not statistically significant, improvement in the pruritus rating scale (NRS), Investigator’s Global Assessment (IGA), and also 50% and 75% reductions in the Eczema Area and Severity Index (EASI50 and EASI75, respectively), with 50% and 75% reductions in the SCORing AD index (SCORAD50 and SCORAD75, respectively) [141].
The so-called “itch cytokine” IL-31 is a major pruritogenic component in AD, which binds to its receptor in the peripheral sensory nerve fibers in the epidermis and dermis and enhances the secretion of other pruritogens [142]. Moreover, IL-31 activates STAT3 in astrocytes via lipocalin-2 production, enhancing additional itch signals in the spinal cord [143]. The newly described IL-31 network compromises alternatively activated anti-inflammatory macrophages (M2), TSLP, periostin, and basophils. Specifically, M2 is one of the main sources of IL-31 in human AD skin lesions, while expression of TSLP and periostin promote IL-31 production by macrophages, as was shown in murine models. Direct depletion of macrophages reduces the itch, while the combined blockage of basophils, TSLP, and periostin only attenuates the itch by reducing IL-31-producing macrophages [8]. Furthermore, IL-31 promotes the release of brain-derived natriuretic peptide (BNP) from the dorsal root ganglionic neurons and skin cells, contributing to the itchy sensation [144]. The central role of IL-31 in AD pathogenesis and itch, per se, is supported by phase 3 clinical studies of Nemolizumab, a humanized monoclonal antibody against IL-31 receptor, showing that subcutaneous administration of Nemolizumab in addition to topical agents, effectively improves pruritus compared to the placebo in individuals with AD; thus, it has been granted approval in adults and adolescents for the treatment of itching associated with AD [145, 146].
The cutaneous neurosensory system occupies a central position in pruritus pathogenesis, dispersing throughout skin layers and interacting with multiple mediators and receptors. An increased density of sensory neurons is noted in the skin of AD patients, resulting in exacerbated responses to a variety of pruritogens, such as neurotrophins (nerve growth factor (NGF) and brain-derived neurotrophic factor (BDNF)) [147]. NGF levels are strongly associated with itch severity and AD eruptions [148]. Moreover, neurotransmitters released from nerve fibers can modulate the immune system in the skin and vice versa [149, 150].
More recently, the Mas-related G-protein-coupled receptor X2 (MRGPRX2) on the surface of mast cells, basophils, and eosinophils has been implicated in the itch pathogenesis as an itch receptor [151]. Activation of the receptor via neuropeptides, such as substance P, degranulates mast cells, while their mediators induce an itch by binding to the protease-activating receptor 2 (PAR2) [149]. MRGPRX2 blockade with selective inhibitors holds promise as a potential target in allergic diseases, including AD [152].
Chronic pruritus poses a formidable challenge in clinical practice due to the interplay with skin disruption and inflammation, creating a vicious cycle that complicates AD management while also posing a significant burden on the quality of life of patients. Further knowledge of the underlying mechanisms of a chronic itch in AD is crucial for developing targeted therapies aimed at alleviating the itch and managing AD effectively.
The intricate and multifactorial interplay of well-established and novel pathogenetic mechanisms associated with AD, including dysregulated immune responses, disruption of the epithelial barrier, pruritus, microbiome dysbiosis, and the influence of the exposome is illustrated in Fig. 3. This complexity contributes to the wide range of clinical variations seen in individuals with AD. Comprehending these different pathogenetic elements is crucial to defining effective treatment strategies, as the heterogeneous nature of AD requires an individualized approach to optimize therapeutic outcomes. The novel therapeutic options in association with their corresponding targeted pathogenic mechanisms are presented in Table 1.
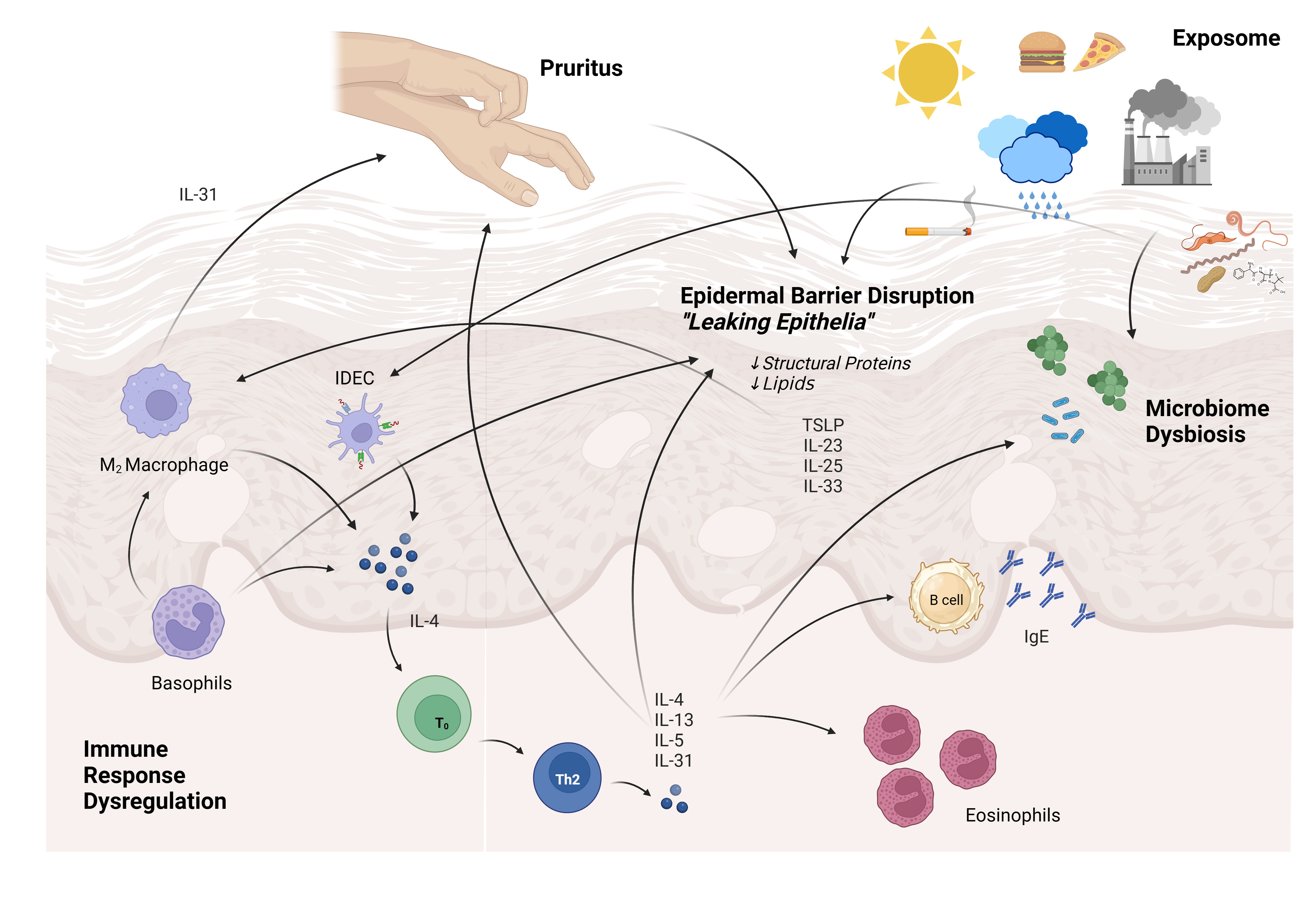 Fig. 3.
Fig. 3.The interplay among different pathogenic factors that contribute to the pathogenesis of atopic dermatitis. IL, interleukin; TSLP, thymic stromal lymphopoietin; IDEC, inflammatory dendritic epidermal cell.
| Pathogenetic mechanism and therapeutic targets | Corresponding treatments | |
| Dysregulated T cell-mediated immune response | ||
| JAK/STAT signaling pathway | - Abrocitinib (JAK1 inhibitor), Baricitinib (JAK1/2 inhibitor) | |
| - Upadacitinib (JAK1 inhibitor) | ||
| - Ruxolitinib (JAK1/2 inhibitor) | ||
| - Delgocitinib (JAK1/2/3, TYK2 inhibitor) | ||
| IL-4/IL-13 | - Dupilumab (IL-4R | |
| - Tralokinumab (IL-13 inhibitor) | ||
| - Lebrikizumab (IL-13 inhibitor) | ||
| IL-31 | - Nemolizumab (IL-31R inhibitor) | |
| IL-21 | - Upadacitinib | |
| IL-22 | - Fezakinumab | |
| PDE4 activity | - Crisaborole (PDE4 inhibitor) | |
| - Difamilast (PDE4 inhibitor) | ||
| Basophils and eosinophils | - Ruxolitinib (¯H4R expression on eosinophils) | |
| - H4R antagonists | ||
| Epidermal Barrier Dysfunction | ||
| Tight junctions (TJs) | - Spirodelapolyrhiza extract | |
| - Olea europaea leaf extract | ||
| - Glucoseskin application | ||
| - Cimifugin | ||
| - DL-Propargylglycine | ||
| Aryl hydrocarbon receptor (AHR) | - Tapinarof (AHR agonist) | |
| - Rhodiola crenulate (AHR agonist) | ||
| - Artemisia princeps (AHR agonist) | ||
| - Diosmin (AHR agonist) | ||
| Skin barrier proteins and lipids | - Crisaborole (PDE4 inhibitor) | |
| - Difamilast (PDE4 inhibitor) | ||
| - Topical formulations with glucoseskin, spirodelapolyrhiza, Olea europaea | ||
| - AHR agonists | ||
| Chronic Itch | ||
| IL-4, IL-13 | - Dupilumab (IL-4R | |
| - Janus Kinase inhibitors | ||
| - Tralokinumab, Lebrikizumab (IL-13 inhibitors) | ||
| - TRP channel modulators (TRPA1, TRPV1) | ||
| IL-31 | - Nemolizumab (IL-31R inhibitor) | |
| Epithelium alarmins (TSLP, IL-33, IL-25) | - Tezepelumab (anti-TSLP) | |
| Neurotransmitters | - NGF and BDNF inhibitors | |
| - MRGPRX2 inhibitor | ||
| Microbiome Dysbiosis | ||
| S. aureus colonization | - Bleach baths | |
| Fungal dysbiosis | - Autologous microbiotherapy | |
| - Emollients enriched with microbiome supportive components | ||
| Exposome | ||
| Environmental allergens and irritants | - Targeted immunotherapy | |
| Air pollution | - Protection from environmental exposure to PM 2.5 | |
| - Avoidance of synthetic detergents | ||
| Climate change and UV-B light | - Monitoring and management of AD during prolonged pollen season | |
| Dietary factors | - Reducing processed food consumption | |
| - Adequate intake of vitamins C and E | ||
AD is remarkably heterogeneous; thus, determining the different endotypes might
offer a comprehensive understanding of the disease’s underlying pathophysiology
and reveal potential treatment targets. Various subtypes of potential AD
biomarkers have been identified and categorized based on their suggested use. For
diagnostic purposes, nitric oxide synthase 2 (NOS2) and cutaneous T
cell-attracting chemokine (CTACK)/CCL27 can differentiate AD from psoriasis in
cases of psoriasiform dermatitis, while T
Blood transcriptome analysis proposed two AD endotypes based on the
eosinophil-related expression signature [154]. The eosinophil-high cluster
exhibited a more pronounced overall dysregulation and a positive correlation
between disease activity and signatures associated with IL-5 signaling, whereas
the eosinophil-low endotype presented minimal dysregulation at the transcriptomic
level and no association between disease activity and gene expression [154]. A
recent study described four serum biomarker-based clusters: One with high levels
of C–C chemokines and IL-1R1 dominance, the second based on the dominance of
T
AD is a complex and heterogeneous condition. Genetic predisposition, epidermal barrier disruption, dysregulated T cell-mediated immune response, skin microbiota dysbiosis, and the exposome effect form the critical components for the development of AD, while the itch is the major and most troublesome symptom that is mainly driven by IL-31 and complex neuro–immune crosstalk. The identification of distinct or even overlapping endotypes raises a translational evolution and leads to an impressive expansion of the therapeutic pipeline; thus, a more personalized treatment approach is now feasible and highly recommended in AD patients.
AD, atopic dermatitis; TEWL, transepidermal water loss; IL, interleukin; JAK/STAT, Janus kinase/Signal transducer and activator of transcription; TJs, tight junctions; FLG, filaggrin; LOR, loricrin.
PX, SG, MM, NGP designed the research study. MS, SK, NP, PX performed the research, interpreted data and wrote the manuscript. SG, MM, NGP, PX edited and reviewed the manuscript, PX supervised. All authors read and approved the final manuscript. All authors have participated sufficiently in the work and agreed to be accountable for all aspects of the work.
Not applicable.
Not applicable.
This research received no external funding.
The authors declare no conflict of interest.
References
Publisher’s Note: IMR Press stays neutral with regard to jurisdictional claims in published maps and institutional affiliations.



