1 Department of Cytopathology, Institute of Pathology, Heinrich Heine University, 40225 Düsseldorf, Nordrhein-Westfalen, Germany
2 Centre for Child and Adolescent Health, HELIOS Klinikum, 47805 Krefeld, Nordrhein-Westfalen, Germany
3 German Fanconi Anemia Support Group, 59427 Unna, Nordrhein-Westfalen, Germany
4 MVZ Pathologie, Zytologie und Dermatologie Viersen, 41747 Viersen, Nordrhein-Westfalen, Germany
Abstract
Fanconi anemia (FA) is an inherited genetic instability syndrome that increases the risk of developing head and neck squamous cell carcinoma, particularly in the oral cavity. These epithelial cancers often arise from visible oral and potentially malignant disorders (OPMD). Research has shown that oral brush biopsies combined with cytology, such as manual DNA cytometry, can facilitate the early detection of OPMDs that require treatment. Thus, this study aimed to evaluate the diagnostic accuracy of a DNA karyometry (DNA-KM) system in the brush biopsy-based diagnostic workup for OPMDs with FA.
Feulgen-stained liquid-based oral smears were included from 327 independent OPMD cases, which had available cytological diagnoses and clinicopathological reference standards. These samples were automatically analyzed using a DNA-KM system (MotiCyte-auto), which employs digital nuclear classifiers based on expert classification of nuclear images and machine learning algorithms.
The detection of (suspected) DNA stemline aneuploidy or single-cell aneuploidy with DNA-KM demonstrated a sensitivity of 69% and a specificity of 96%. In our analysis, when DNA-KM was combined with cytology, we observed a sensitivity of 75% and a specificity of 96%. Meanwhile, additional research using the variation coefficient of a “broad-based” peritetraploid stemline (BPS) as an alternative algorithm further increased the sensitivity to 84%. However, employing this algorithm slightly decreased specificity to 92% at a cut-off of 5.83.
Artificial intelligence (AI)-assisted DNA-KM, with automated slide-scanning and digital classification of nuclei, can serve as a valuable additional method in the brush biopsy-based cytological diagnosis of OPMD in FA. This approach can help identify lesions that require clinical intervention.
Keywords
- image cytometry
- Fanconi anemia
- mouth neoplasms
- early detection of cancer
Oral cancer is one of the most common types of cancer worldwide, with 377,713 new cases and 177,757 deaths reported in 2020 [1]. While smoking, alcohol consumption, and Human papilloma virus (HPV) infection are the primary risk factors, certain genetic disorders can increase the likelihood of developing oral cancer [2]. One such disorder, Fanconi anemia (FA), is an inherited cancer susceptibility syndrome caused by a bi-allelic mutation in one of the 23 genes that are a part of the FA DNA repair pathway [3, 4]. Physiologically, the FA gene products work to remove interstrand crosslinks in DNA [5]. However, in individuals with FA, unrepaired interstrand crosslinks contribute to genomic instability and tumorigenesis [3, 6].
Compared with the non-FA population, FA patients face a 500–700-fold higher risk of developing head and neck squamous cell carcinoma (HNSCC), with most of these lesions located in the oral cavity [7, 8]. Similar to other cancers, oral cancers have a better prognosis if diagnosed early [8, 9, 10]. Compared to the general population, FA patients are often diagnosed at a later stage leading to a significantly poor prognosis [8]. Standard chemoradiation treatments are not applicable for FA due to their hypersensitivity to DNA-cross-linking agents, which can also harm normal cells [11]. Therefore, early detection of cancer or its immediate precursor lesions, such as high-grade oral epithelial dysplasia is crucial for successful treatment [8].
In a study involving 713 FA patients, Velleuer et al. [12] demonstrated that brush biopsy-based cytology, including DNA ploidy analysis, is a highly accurate first-level diagnostic tool for detecting visible (pre) malignant oral lesions in FA patients. Moreover, patients diagnosed in the early stages show excellent survival, proving that early detection improves quantity and quality of life. The detection of DNA aneuploidy using interactive DNA image cytometry is strongly associated with malignant transformation and is detectable in oral cancers and oral potentially malignant disorders (OPMDs), that show malignant progression [13]. Nonetheless, the interactive (i.e., manual) DNA image cytometry analysis is time-consuming and demands up to 60 minutes for a complete DNA ploidy analysis.
This problem may be overcome with the introduction of DNA ploidy analysis via Artificial intelligence (AI)-assisted DNA-KM, which enables a semi-automated or automated analysis of liquid-based cytological samples [14]. Similar to interactive DNA image cytometry, DNA-KM enables precise quantification of the nuclear DNA content. However, it further incorporates digital nuclear classifiers, which are developed through expert-based classification of nuclear images and machine learning algorithms [15]. The complete process of slide scanning in different focal planes, segmentation of nuclei, and measurement of the DNA content is performed autonomously, reducing the investigator’s workload. DNA-KM automatically classifies various cell types, including normal squamous cells, granulocytes, lymphocytes, abnormal cells, or defocused nuclei and artifacts, and presents them in an image gallery [16]. The workload for cytotechnicians or cytopathologists is reduced by verifying the accuracy of the automated classifications, and when necessary, reclassifying the nuclei or artifacts. This approach allows for the analysis of a greater number of cells across the entire cytological slide, compared to interactive DNA image cytometry.
The present study aims to evaluate the diagnostic accuracy of DNA ploidy analysis using DNA-KM for the detection of (pre) malignant oral lesions in patients with FA. In addition, a combined statistical analysis was conducted, integrating the results from DNA-KM with those from liquid-based oral cytology.
All samples were provided by FA individuals who participated in our ongoing oral cancer surveillance study, as described by Velleuer et al. [12]. The participants gave informed consent for additional DNA ploidy analysis, and the study adhered to the principles outlined in the 1964 Helsinki Declaration and its subsequent amendments. The study received approval from the Western Institutional Review Board® (WIRB - Puyallup, WA, USA) before its initiation (number of studies: 1139633).
In summary, after standardized inspection of the oral cavities of FA individuals, visible lesions (e.g., leukoplakia, erythroplakia, erythroleukoplakia, ulcer, erosion) were documented through digital photographs and anatomically on a mouth map (https://www.fanconi.de/scc_en). These lesions were sampled using Orcellex® Brushes (Rovers Medical Devices, Oss, The Netherlands). The exfoliated cells were processed in a vial for liquid-based cytology (Safeprep®, Medite, Burgdorf, Germany or BD SurePath®, BD, Heidelberg, Germany). After following the routine Papanicolaou staining, a cytological diagnosis was made at the Department of Cytopathology of the Heinrich Heine University Düsseldorf. The diagnostic cytological category (“negative”, “atypical”, “suspicious”, “positive”, and “not sufficient”) was provided as previously described [12].
Archived Papanicolaou-stained liquid-based cytospin preparations from February 2016 to February 2020 were utilized for automated DNA ploidy analysis using DNA-KM. The slides were deparaffinized in xylene and re-stained using the method described by Feulgen in a temperature-controlled staining machine (Cellstain, Tharmac GmbH, Limburg, Germany) [17].
In total, 743 consecutive brush biopsy-based samples from various oral lesions were available for the study. Samples containing almost anuclear keratinocytes, fewer than 100 reference cells (normal epithelial cells), or those without an available reference standard were excluded from the evaluation.
Samples were analyzed with the MotiCyte-auto system (Motic Group Co., Ltd.,
Xiamen, China) consisting of a motorized Motic BA610 microscope with a
40
The screening process took between 60 and 150 minutes per 2.5
DNA ploidy measurements, including internal calibration of nuclear DNA values on
normal oral squamous nuclei, were conducted following the recommendations of the
European Society for Analytical Cellular Pathology (ESACP) [19, 20, 21, 22].
Euploid-diploid, euploid-polyploid, and aneuploid DNA stemlines were
automatically identified in histograms by the MotiCyte-auto algorithm as distinct
peaks with additional values at their doubling position according to Haroske
et al. [22]. A DNA stemline was classified as euploid-diploid if the
modal value in c-units was within the range of 1.8c to 2.2c (2c
Euploid-polyploid DNA stemlines display modal values within 1.8c and 2.2c (2c
• A DNA stemline was classified as aneuploid if the modal value of
the DNA stemline was outside the above-mentioned limits of 2c, 4c, and 8c
• Single-cell DNA aneuploidy was identified when one or more nuclei
with a DNA content
The morphology of these nuclei was carefully assessed by re-localization and manual microscopic evaluation with the MotiCyte-auto system.
Fig. 1 shows examples of Feulgen-stained cells and the respective DNA histograms. DNA stemline aneuploidy and in addition, DNA single-cell aneuploidy was considered as specific indicators of malignant cells [12, 22, 23].
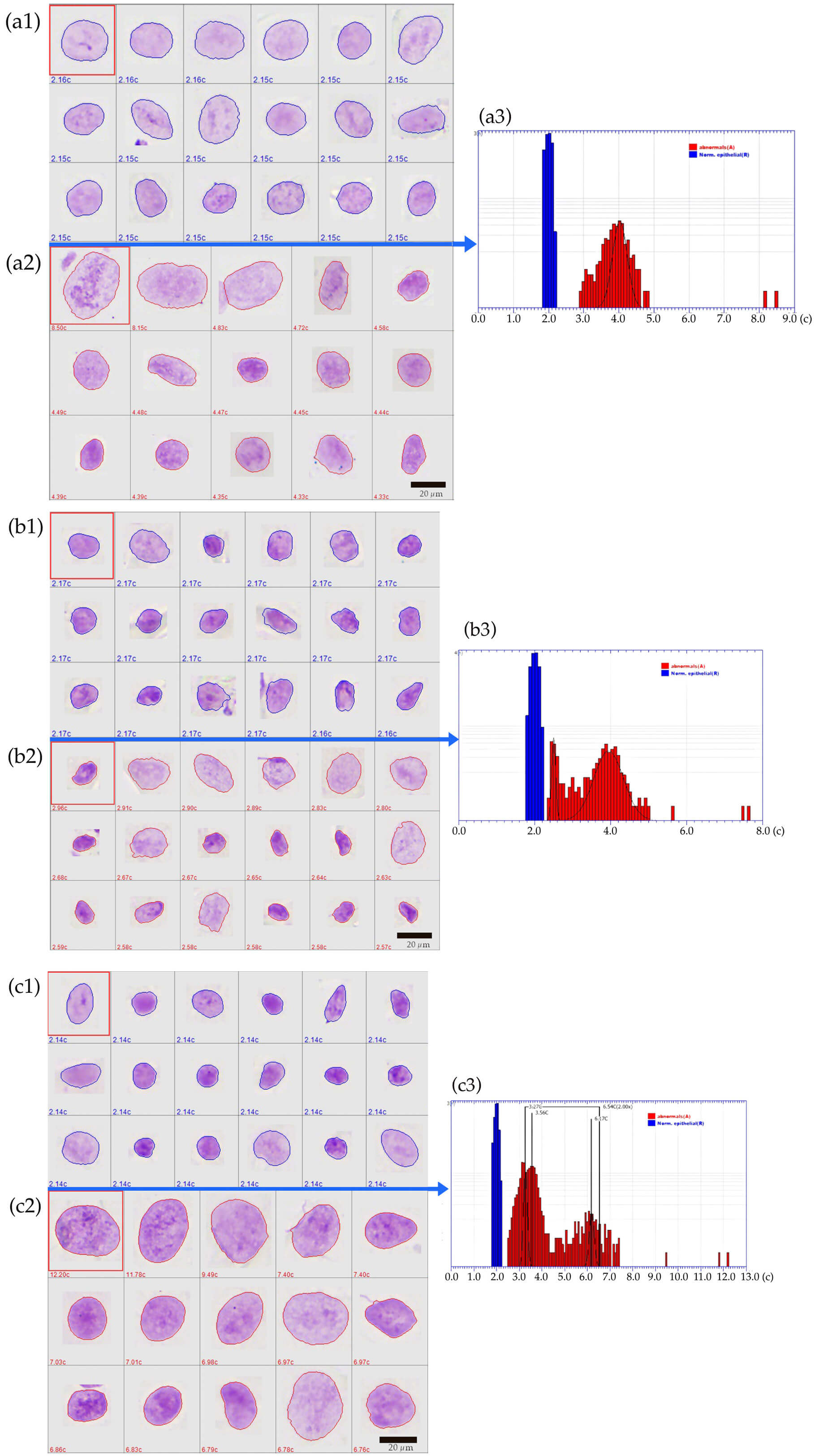 Fig. 1.
Fig. 1.
Representative images of classified Feulgen-stained cells in the image gallery and DNA histograms of positive cases (y-axis: numbers of nuclei, logarithmic scaling. x-axis: DNA content in c-units). (a1–a3) case classified as DNA euploid-polyploid showing a broad peritetraploid stemline (BPS). Follow-up: positive. Histology: high grade oral epithelial dysplasia (HG OED); (a1) image gallery of reference cells (normal epithelial cells); (a2) image gallery of analysis cells (abnormal cells), cytologically not atypical (a3) DNA histogram. (b1–b3) case classified as suspected DNA aneuploidy with a broad peritetraploid stemline at 3.94c and an additional small aneuploid stemline at 2.49c. Follow-up: positive. Histology: OSCC stage T1; (b1) reference cells; (b2) abnormal cells of the aneuploid stemline, hyperchromatic nuclei with irregular nuclear outline; (b3) DNA histogram. (c1–c3) case classified as DNA stemline aneuploidy plus single-cell aneuploidy with abnormal stemlines at 3.27c and 3.56c and three 9c exceeding events. Follow-up: positive. Histology: HG OED; (c1) reference cells; (c2) abnormal nuclei, cytologically hyperchromatic and enlarged; (c3) DNA histogram. (c) represents the relative nuclear DNA amount per cell. Scale bars in image galleries a1, a2, b1, b2, and c1, c2 = 20 μm (black bars indicate the approximate size of Feulgen-stained cells).
In addition to the above-mentioned well-defined and published criteria, a
measurement was defined as “suspected DNA aneuploidy” if an aneuploid DNA
stemline consisted of only a few cells (
For each of the oral lesions, a follow-up clinicopathological reference standard was applied. This reference standard refers to the location and the time of the respective brush biopsies from the visible oral lesions and was defined according to Velleuer et al. (2020) [12]:
• Positive: a histological diagnosis of oral squamous cell carcinoma (OSCC) or high-grade oral epithelial dysplasia (OED) (including moderate and severe OED) [24] within six months of oral examination.
• Positive: a positive cytological diagnosis or DNA aneuploidy with a consistent clinical course within six months (i.e., OSCC therapy, palliative care, or definite imaging).
• Negative: a negative (benign) or low-grade OED histological diagnosis within six months of oral examination or a two-year negative clinical follow-up.
The evaluation of DNA-KM and liquid-based oral cytology was performed by calculating sensitivity, specificity, positive predictive value (PPV), negative predictive value (NPV), receiver operating characteristic (ROC) curve analysis, and their respective 95% confidence intervals. Inconclusive test results such as atypical cytology, suspicious cytology, or suspected DNA aneuploidy were classified as either positive or negative for the different statistical evaluations. For the comparison of the variation coefficients of the nuclear DNA contents of the cells within “broad” peritetraploid stemlines (BPS) between samples with a positive or a negative follow-up reference standard (Supplementary Material Table 1), the Gaussian distribution of the data was checked using the Shapiro-Wilk test. The Mann-Whitney test was applied in conjunction with the visualization of the data distribution in the histogram.
All statistical analyses were performed with R language and environment for
statistical computing version 4.2.2 (R Foundation for Statistical Computing,
Vienna, Austria). The following packages were used: epiR, RVAideMemoire, static,
and Rcmdr-Plugin.ROC. The threshold level of significance was set to p
Between February 2016 and February 2020, DNA ploidy analysis was performed using
DNA-KM on 743 liquid-based Feulgen-stained brush biopsy-based cytological
specimens (Fig. 2). Sixty-six samples were excluded from statistics due to
insufficient number of reference cells (
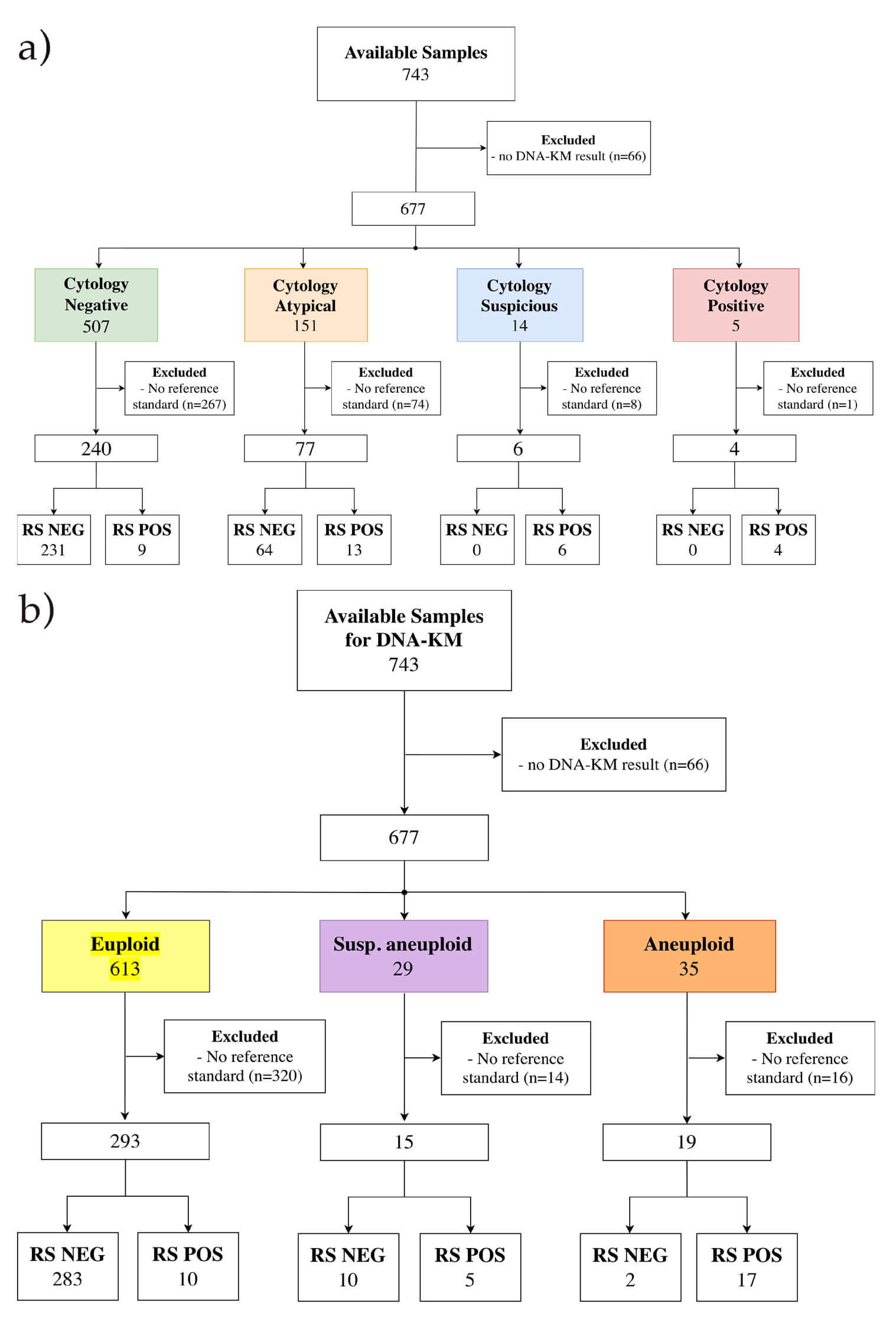 Fig. 2.
Fig. 2.
Flow diagram displaying sample inclusion and dropouts as well as the reference standard. (a) displays the cytological diagnosis and (b) the DNA ploidy analysis using DNA karyometry. Abbreviations: No DNA-KM results, cases where DNA ploidy analysis could not be completed or yielded no interpretable results; No reference standard, cases that had successful DNA-KM analysis but no available histological follow-up or clinical reference standard for validation. RS NEG, negative clinicopathological follow-up reference standard; RS POS, positive clinicopathological follow-up reference standard.
Table 1 presents some demographic characteristics of the patients. All results and information presented in the tables refer to the location and the time of the respective brush biopsies from the visible oral lesions. The share of patients with a positive follow-up is similar between those who underwent a hematopoietic stem cell transplant and those who did not (8.7% and 9.1%, respectively). The prevalence of positive lesions is slightly lower compared to 11.7% determined by Velleuer et al. (2020) [12].
| Characteristics | All | No HSCT | HSCT | No information on HSCT | ||||
| Negative FUP | Positive FUP | Negative FUP | Positive FUP | Negative FUP | Positive FUP | Negative FUP | Positive FUP | |
| Total No. | 295 | 32 | 69 | 6 | 219 | 20 | 7 | 6 |
| Sex, F/M | 146/149 | 14/18 | 42/27 | 0/6 | 99 /120 | 9/11 | 5/2 | 5/1 |
| Median age at sample collection (Range), Y | 28 (8/48) | 30 (13/44) | 28 (11/46) | 29 (24/35) | 27 (8/48) | 30 (13/44) | 30 (30/34) | 30 (30/31) |
Abbreviations: FUP, follow-up; HSCT, hematopoietic stem cell transplantation; No., number; M, male; F, female; Y, years.
Table 2 displays the results of DNA-KM, liquid-based cytology, and the combination of DNA-KM with cytology. Furthermore, inconclusive results like suspected DNA aneuploidy, and atypical or suspicious cytology are classified as either statistically negative or positive and compared to the reference standard for the respective calculations to analyze the influence on the diagnostic accuracy. In the combined evaluation of DNA ploidy analysis with cytology, some cytological results are replaced by the results of DNA ploidy analysis as described in Table 2. In these evaluations, suspected DNA aneuploidy is always considered as a positive test result.
| DNA karyometry | ||||
| Sensitivity | Specificity | PPV | NPV | |
| Suspected DNA aneuploidy = positive | 69% (22/32)a [0.50, 0.84]b | 96% (283/295) [0.93, 0.98] | 65% (22/34) [0.46, 0.80] | 97% (283/293) [0.94, 0.98] |
| Suspected DNA aneuploidy = negative | 53% (17/32) [0.35, 0.71] | 99% (293/295) [0.98, 1.00] | 89% (17/19) [0.67, 0.99] | 95% (293/308) [0.92, 0.97] |
| Liquid-based cytology | ||||
| Atypical and suspicious = statistically positive | 72% (23/32) [0.53, 0.86] | 78% (231/295) [0.73, 0.83] | 26% (23/87) [0.18, 0.37] | 96% (231/240) [0.93, 0.98] |
| Atypical = statistically negative | 31% (10/32) [0.16, 0.50] | 100% (295/295) [0.99, 1.00] | 100% (10/10) [0.69, 1.00] | 93% (295/317) [0.90, 0.96] |
| Suspicious = statistically positive | ||||
| DNA karyometry + Cytology | ||||
| The result of ploidy analysis replaces atypical cytology | 63% (20/32) [0.44, 0.79] | 98% (288/295) [0.95, 0.99] | 74% (20/27) [0.54, 0.89] | 96% (288/300) [0.93, 0.98] |
| The result of ploidy analysis replaces negative and atypical cytology | 75% (24/32) [0.57, 0.89] | 96% (283/295) [0.93, 0.98] | 67% (24/36) [0.49, 0.81] | 97% (283/291) [0.95, 0.99] |
| The result of ploidy analysis replaces negative, atypical, and suspicious cytology | 69% (22/32) [0.50, 0.84] | 96% (283/295) [0.93, 0.98] | 65% (22/34) [0.46, 0.80] | 97% (283/293) [0.94, 0.96] |
Abbreviation: PPV, positive predictive value; NPV, negative predictive value.
a In parentheses: number of samples used in the respective analyses.
b In box brackets: 95% confidence intervals.
DNA ploidy analysis with a DNA aneuploidy (DNA stemline aneuploidy and/or single cell aneuploidy) result shows a nearly perfect specificity of 99%, but the corresponding sensitivity was relatively low at 53%. Including suspected DNA aneuploidy in the category of statistically positive test results rather than negative, improves sensitivity by about 16% without significantly compromising the specificity.
All oral brush biopsy samples that exhibit suspicious and positive cytology are considered true positives. When evaluating liquid-based cytology without additional DNA karyometry, the specificity is only 31% if only suspicious and positive cytology are deemed test-positive. Since negative cytology indicates a low probability for a positive follow-up (3.75%) compared to 16.9% for atypical cytology, atypical cytology results are inconclusive for further clinical action. Therefore, we classify atypical cytology as a positive test result, in addition to suspicious and positive cytology to ensure that a few (pre) cancers as possibly missed. This classification increases sensitivity to 72%, although specificity decreases to 78%.
We also explored a combined evaluation of both, cytological diagnosis and DNA karyometry. It is important to mention that the cytological diagnosis and the DNA ploidy analysis are done on the same cells of a cytological slide using different staining techniques. The best result of the combined evaluation is observed if both negative and atypical cytological results are replaced by the results of DNA-KM. In this evaluation, the sensitivity is 75%, representing the highest of all analyses (Table 2) with a corresponding specificity of 96%. Out of the nine samples with (false) negative cytology but a positive follow-up outcome (Fig. 2), four showed positive DNA-KM results (three cases of DNA aneuploidy and one of suspected DNA aneuploidy), indicating a cytological screening error. Out of the 13 samples with atypical cytology and positive follow-up, 10 yielded a positive DNA-KM result, including eight cases of DNA aneuploidy and two of suspected DNA aneuploidy.
Some analyses present a “broad-based” peritetraploid DNA stemline (BPS) but with a non-aneuploid modal value. Table 3 compares the means of the variation coefficient obtained from the DNA content of the cells contributing to broad peritetraploid stemlines of samples with a negative and positive follow-up. The Mann-Whitney test showed that the variation coefficient (CV) distribution of the negative group is different from the CV distribution of the positive group (W = 125; p = 0.01164).
| Follow-up | DNA aneuploidy (Stemline or 9cEE) | Number of samples | Median | Mean | IQR | W | Significance level |
| Negative | 0 | 51 | 5.22 | 5.51 | 2.15 | 125 | 0.01164a |
| Positive | 1 | 10 | 6.37 | 7.14 | 3.28 |
The Mann-Whitney test is used to analyze the difference between the medians.
Abbreviations: IQR, interquartile range; W, Wilcoxon statistic. a Level of
significance p
The ROC curve (Supplementary Fig. 1) analyzes different thresholds to define the best CV value to separate a negative or a positive follow-up. The ROC curve and the table with all its results generated by the ROC curve are presented in supporting information. Using a CV value of 5.83 or higher to define a BPS, a positive reference standard is predicted best with a sensitivity of 80% and a specificity of 66.7%.
Based on these results, we analyzed the diagnostic accuracy of the additional application of the BPSs on the DNA-KM results of all 327 evaluable samples. In this analysis, the results of the DNA euploid and suspected DNA aneuploid samples are substituted by the BPS result. Thus, DNA euploid and suspected DNA aneuploid cases with a BPS are considered as test-positive but without a BPS as test-negative. In samples without statistical data of peritetraploid stemlines for the determination of a BPS, the euploid cases are classified as negative, and suspected DNA aneuploid cases are classified as positive. Clear-cut DNA aneuploid samples are not affected by the calculation of a BPS. The results of this analysis are summarized in Table 4.
| DNA karyometry | ||||
| Sensitivity | Specificity | PPV | NPV | |
| DNA | 84% (27/32)a [0.67, 0.95]b | 92% (271/295) [0.88, 0.95] | 53% (27/51) [0.38, 0.67] | 98% (271/276) [0.96, 0.99] |
| Aneuploidy + BPS = positive | ||||
| BPS = positive | 80% (8/10)a [0.44, 0.97]b | 66.7% (34/51) [0.52, 0.79] | 32% (8/25) [0.15, 0.54] | 94% (34/36) [0.81, 0.99] |
Abbreviation: CV, variation coefficient; BPS, “broad” peritetraploid stemline; PPV, positive predictive value; NPV, negative predictive value.
a In parentheses: number of samples used in the respective analyses.
b In box brackets: 95% confidence intervals.
Comparing the results of the isolated BPS analysis using a CV value of 5.83 (Table 4) with DNA aneuploidy results (DNA stemline aneuploidy and/or single cell aneuploidy, while suspected DNA aneuploidy was considered negative, Table 2), we observed improved sensitivity and lower specificity. The comparison was performed to evaluate the performance of the novel approach (BPS) against a validated method (DNA aneuploidy). Otherwise, Fig. 3 shows that the best results from our study were achieved when DNA karyometry analysis classified cases as statistically positive based on suspected DNA aneuploidy and ‘broad’ peritetraploid stemline cases with a coefficient of variation exceeding 5.83.
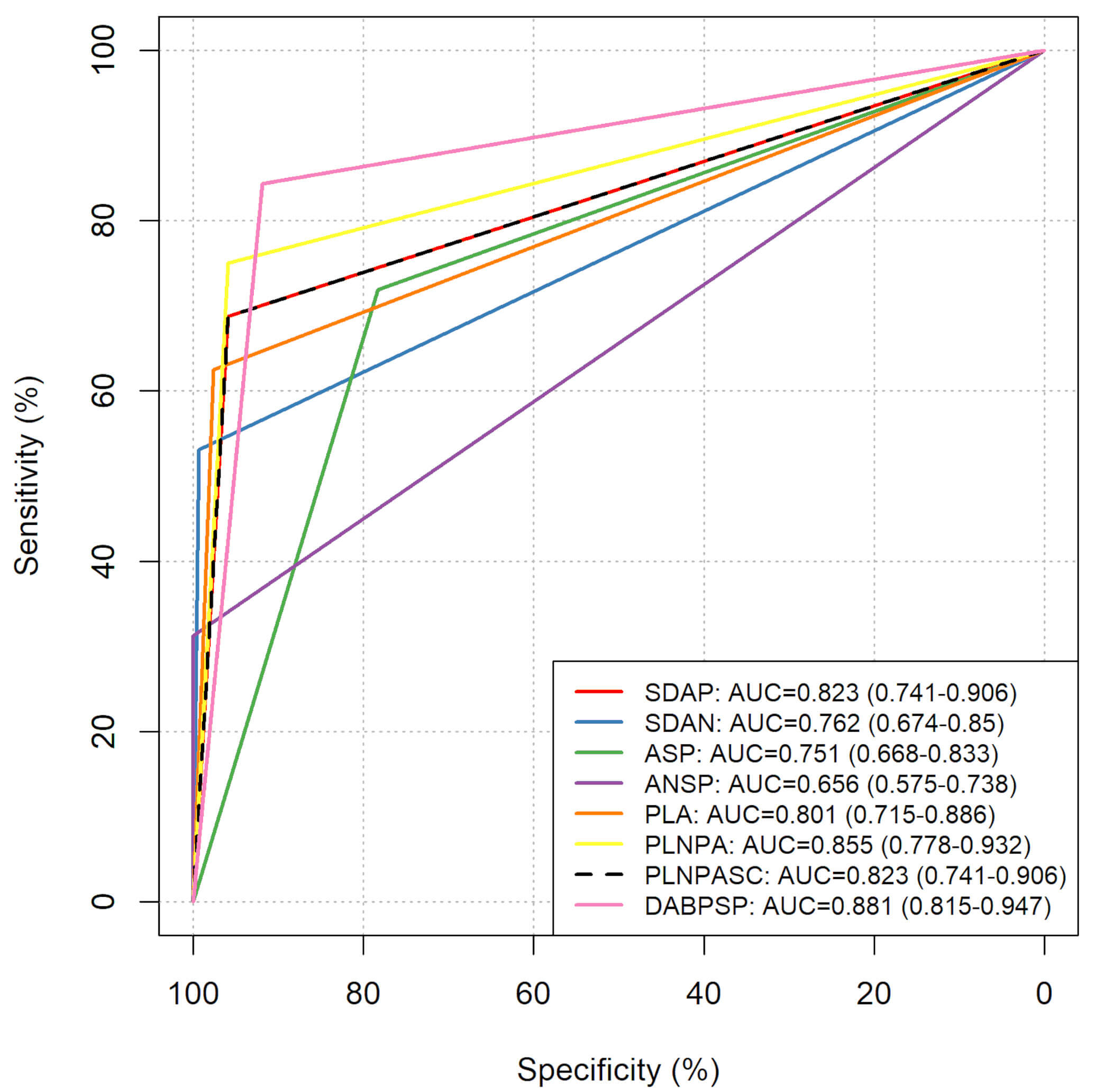 Fig. 3.
Fig. 3.
Comparative receiver operating characteristic (ROC) curves of all tested approaches for the prediction of a positive reference standard. Abbreviations: SDAP, ROC curve of the DNA karyometry analysis considering suspected DNA aneuploidy cases as statistically positive; SDAN, ROC curve of the DNA karyometry analysis considering suspected DNA aneuploidy cases as statistically negative; ASP, ROC curve of the cytological analysis considering atypical and suspicious cases as statistically positive; ANSP, ROC curve of the cytological analysis considering atypical and suspicious cases as statistically negative; PLA, ROC curve of the cytological and DNA karyometry analysis replacing atypical cytology results with ploidy analysis; PLNPA, ROC curve of the cytological and DNA karyometry analysis replacing negative and atypical cytology results with ploidy analysis; PLNPASC, ROC curve of the cytological and DNA karyometry analysis replacing negative, atypical and suspicious cytology results with ploidy analysis; DABPSP, ROC curve of the DNA karyometry analysis considering suspected DNA aneuploidy and “broad” peritetraploid stemline cases with a coefficient of variation higher than 5.83 as statistically positive.
The early and non-invasive diagnosis of oral (pre) cancer is essential for increasing the chances of survival and avoiding overdiagnosis for patients with FA. Velleuer et al. [12] demonstrated the high accuracy of brush biopsy-based cytology and DNA ploidy analysis using manual DNA image cytometry to detect OPMDs in FA patients who are at high risk for malignant transformation, and therefore, warrant treatment. However, manual DNA image cytometry is time-consuming and needs specialized personnel (cytopathologists or cytotechnicians), which may not be available in every country. Consequently, its practical application is limited to those cytological samples with inconclusive results, i.e., those diagnosed as “atypical” or “suspicious”, as also applied by Velleuer et al. [12]. Additionally, the production of existing manual DNA image cytometry devices has ceased, and the development of new ones has not progressed. Implementing an automated, AI-assisted alternative to manual DNA image cytometry could help to overcome these issues. The automated scanning process and detection of different types of cells using expert-trained classifiers and machine learning algorithms enable the evaluation of the entire slide. Moreover, it enables the evaluation of more samples, including those with a negative cytological result. This may help to reduce the occurrence of false-negative cytology. In this study, out of the nine liquid-based samples with false negative cytology, four showed a positive DNA-KM result. Our study on oral liquid-based cytological specimens aimed to validate the DNA-KM with the MotiCyte-auto for identifying OPMDs in a high-risk population, warrants further clinical intervention. As already shown for manual DNA ploidy analysis with DNA image cytometry [25] DNA-KM may also be useful in early detection of oral cancer in the common population.
Our study achieved a sensitivity and a specificity of 69% and 96%, respectively (Table 2) for the diagnosis of OPMDs that show at least a high-grade oral epithelial dysplasia but more often an OSCC in the follow-up. In comparison with the cytological diagnosis, the specificity is 18% higher and sensitivity is only 3% lower. This result is only surpassed by the combined application of cytology and DNA-KM (when DNA-KM results replace negative and atypical cytology), which shows the same specificity (96%) but a 6% higher sensitivity (75%). Accordingly, based on our data, the additional application of DNA-KM is most valuable in negative and atypical cytology. In comparison, its application subsequent atypical cytology only has a lower sensitivity of 63% but a slightly higher specificity of 98%. Because all suspicious and positive cytological specimens have a positive follow-up, an additional DNA-KM would have no beneficial effect in these cases.
Other automated DNA cytometry systems have already been tested in the diagnosis of OPMDs.
In a study using the automated iClearCyte® system, Parfenova
et al. [26] found a sensitivity of 100% and a specificity of 86.7% for
the screening of high-grade oral lesions. This study, however, had a lower number
of test samples (30 controls and 35 abnormal samples) and excluded samples with
histopathologically confirmed mild to moderate oral epithelial dysplasia. In
measurements with the iClearCyte, the mean DNA amount is adopted as the DNA Index
(DI) of a diploid cell population to calibrate the DI of other cells. The cells
were categorized according to the DI into diploid (0.85
Most recently, a successor of the MotiCyte auto system, the EasyScan-AI (Motic
China Group, Ltd., Xiamen, PR China) was tested with 92 liquid-based oral brush
biopsy samples from FA individuals by Böcking et al. (2022) [15].
Notably, the specimens analyzed overlapped with those included in the present
study. Similar to the Moticyte auto system, the nuclear classification is based
on random forest classifiers and supervised machine learning techniques. Under
stringent criteria for defining DNA aneuploidy, they report a sensitivity of 35%
and a specificity of 94.4%. With defining
Using exfoliative cytology with cytobrushes for the collection of cells from OPMD, Ma et al. [27] found a sensitivity of 86.36% and a specificity of 90% for the detection of histologically proven severe dysplasia or neoplasia with an automated DNA image cytometer (Wuhan Landing Medical High-tech Co., Ltd., China). This study used the same stemline DNA ploidy interpretation as adopted in our study, but 5c exceeding events are applied to indicate DNA single-cell aneuploidy.
Earlier results from our group, published by Velleuer et al. [12] applying a manual DNA image cytometer reported a sensitivity of 89.5% and a specificity of 93.4% when suspected DNA aneuploidy was considered as a negative test result in the combined evaluation with cytology. If suspected DNA aneuploidy was considered a positive test result, the sensitivity was 100% and the specificity 92.2%. As indicated above, the manual DNA ploidy analysis was applied almost exclusively to samples, that had “atypical” or “suspicious” cytological diagnoses. In comparison, our study has 75% and 96% sensitivity and specificity in the combined analysis of DNA-KM and cytology, respectively, including the analysis of all cytologically negative samples. The lower sensitivity in our present study is not expected because some of the brush biopsy-based samples analyzed are shared in both studies. However, in our previous study, reported by Velleuer et al. [12], often a conventional smear and several cytospins of liquid-based cytological preparations were available from a single lesion. The highest-grade cytological diagnosis of all these slides was always correlated with the follow-up findings. This procedure was labor-intensive but may have led to improved cytological results compared to the sole utilization of one liquid-based cytospin slide as in our present study. Besides that bias, others are conceivable like incorrect classification by the machine classifier that has been overlooked during the “safety net” validation process of the cytopathologist. Several thousands of automatically classified nuclear images must be checked during this procedure with a focus on relevant contents in the regions of the 9c exceeding events and aneuploid stemlines. Another bias may be a possible inconsistency of the Feulgen stain of different cytological preparations and different points in time of the Feulgen stain or the DNA ploidy analysis. Effects of an inconsistent Feulgen stain during manual and automated DNA ploidy analysis can be overcome by adherence to the reported guidelines for quality assurance [21]. A significant problem in our hands is the decline of the Feulgen stain in archived materials as observed in more than 30 years of DNA-ploidy analysis in our institution. Although we often use the same slides for manual and automated DNA ploidy analysis as mentioned above, the time points differ and thus an irregular attenuated Feulgen stain may have affected the automated analyses. In addition, it is known that storage may result in different intensities of the Feulgen stain of simultaneously stained specimens, that warrant the correct application of internal reference cells [28].
DNA image cytometry, whether performed using a manual cytometer or with
automated devices aids in differentiating reactive lesions (inflamed or
regenerating tissues) from (pre) malignant lesions in cytology. Both methods
require a minimum of atypical cells to detect malignant clones. However,
liquid-based or conventional cytological preparations from oral brushings often
contain many normal squamous epithelial cells and white blood cells along with a
few atypical cells. This scarcity may make it difficult to identify a stemline of
cells with similar DNA content. To address this issue, we propose less stringent
criteria for the detection of DNA aneuploidy referred to as “suspected DNA
aneuploidy”. In our study, we use this category if an aneuploid DNA stemline
consists of only a few cells (
To establish an objective parameter that can distinguish samples with a positive
or negative reference standard for those that do not meet the standard criteria
of DNA aneuploidy, we analyze the variation coefficient to define a “broad
peritetraploid stemline” (BPS). We found a significant difference (p =
0.01164) between the mean CVs of samples with negative and positive reference
standards (Table 3). Using the ROC curve, we determined that a CV
In summary, the calculation of the CV of peritetraploid stemlines and establishing a cutoff for positive and negative test results enhances the diagnostic accuracy of DNA-KM compared to the traditional criteria for DNA aneuploidy (Table 3). This could also serve as an additional objective criterion in measurements with suspected single-cell DNA aneuploidy.
While our study focuses on the utility of automated DNA ploidy analysis for
routine diagnostics, it does not allow us to define the biological significance
of BPSs. However, in certain samples, a considerable number of cells within a
peritetraploid stemline, but outside the limits of 3.6c and 4.4c (4c
In short, there is evidence suggesting that tetraploidy can promote chromosomal instability. Tetraploid cells often possess supernumerary centrosomes and may be halted in the cell cycle by tetraploidy checkpoint under normal conditions [33]. In instances of mutated TP53, these cells progress through the cell cycle, leading to catastrophic mitotic failures that result in the loss of genomic material and subsequent aneuploidy. TP53 alterations are present in most FA-associated head and neck cancers [34]. A tetraploid state poses challenges for cell survival as tetraploid cells are likely to lose chromosomal material due to replication stress and chromosome missegregation during mitosis. This process can lead to a near tetraploid state, which carries a higher risk of chromosomal instability and malignant transformation [35]. Furthermore, subtetraploid cell populations have been linked to increased metastatic prevalence in colorectal cancer [36], primary renal cell carcinomas [37], and lung cancer [38]. Research by Wangsa et al. [39] indicated that despite their proliferative disadvantages due to replication stress-induced S-phase delays, subtetraploid clones exhibit increased migratory and invasive capacities. Our BPS concept captures this dynamic instability by identifying cell populations ranging from 3c to 5c, predominantly tetraploid—reflecting the expected patterns of ongoing chromosomal missegregation in unstable subtetraploid cells. Consequently, a BPS may reflect chromosomal instability and genomic alterations such as amplifications or deletions, as opposed to reactive tetraploidy caused by inflammation or tissue repair.
Some limitations of this study should be acknowledged. Selection bias may be introduced due to the retrospective design’s reliance on archived cytological samples. Additionally, variations in sample processing over time could impact the accuracy of DNA ploidy measurements.
Since images of normal and abnormal nuclei, along with artifacts, were looked to identify misclassified cells, the diagnostic reliability of AI-classified nuclear images may have been affected by the involvement of multiple observers performing manual corrections.
Although the same slides are used for manual and automated DNA ploidy analysis, the timing of these analyses differs, which may lead to irregular attenuation of Feulgen stain and potentially affect the accuracy of automated measurements.
In conclusion, this study demonstrates that DNA-KM with automated slide-scanning and AI-assisted classification of nuclei, can significantly enhance the accuracy of brush biopsy-based cytological diagnosis of OPMD in patients with FA. The implementation of cutoffs based on CVs of broad peritetraploid stemlines significantly improves diagnostic precision. However, future prospective studies are needed to validate these findings.
The original contributions presented in the study are included in the article/Supplementary Material, further inquiries can be directed to the corresponding author.
MS conceptualized and designed the research study. BESA and LH performed the DNA ploidy analysis. BESA, MS and IKSAA analyzed the data. MS and NP did the cytopathological diagnosis. BESA and MS wrote the manuscript. MS, RD and EVC administrated the project and acquired the funds. RD and EVC were responsible for providing the samples and patient data, and also contributed critical clinical insights and played a key role in data analysis, substantially shaping the study’s interpretation. All authors contributed to editorial changes in the manuscript. All authors read and approved the final manuscript. All authors have participated sufficiently in the work and agreed to be accountable for all aspects of the work.
The study was conducted in accordance with the 1964 Declaration of Helsinki and later amendments and approved by the Western Institutional Review Board® (WIRB - Puyallup, WA, USA) prior to its initiation (number of study: 1139633). The participants gave informed consent for additional DNA ploidy analysis.
The authors express their gratitude to all individuals with Fanconi Anemia who contributed to this research. Significant contributions were provided by Christine Krieg and Marleen Schmitt from the German Fanconi Anemia Support Group. The authors extend their sincere appreciation to Dr. Leonid Berynskyy for his sustained project support, extensive expertise with the MotiCyte system, and numerous DNA-ploidy analyses, as well as to Irene Esposito from the Institute of Pathology, Heinrich Heine University of Düsseldorf for her comprehensive assistance.
This research was funded by the Fanconi Cancer Foundation, previously known as the Fanconi Anemia Research Fund (FARF), and the German Fanconi Anemia Support Group. Author Bruno Eduardo Silva de Araujo received authorization from the CAPES Foundation under the Brazilian Ministry of Education to extend his residency at Heinrich Heine University Düsseldorf and conduct this investigation following a 4-year scholarship award (2014–2018) (BEX: 99999.0013111/2013-01).
Bruno Eduardo Silva de Araujo, Isabela Karoline de Santana Almeida Araujo and Martin Schramm report grants from German Fanconi Anemia Support Group during the conduct of the study. Eunike Velleuer-Carlberg reports grants from German Fanconi Anemia Support Group and grants from Fanconi Anemia Research Fund during the conduct of the study. Until July 2019, Ralf Dietrich was managing director of the German Fanconi Anemia Support Group and reports grants from Fanconi Anemia Research Fund during the conduct of the study. Natalia Pomjanski and Leonie Hirner have nothing to disclose.
Supplementary material associated with this article can be found, in the online version, at https://doi.org/10.31083/FBE38747.
References
Publisher’s Note: IMR Press stays neutral with regard to jurisdictional claims in published maps and institutional affiliations.



