1 College of Science and Sustainability, School of Health, Medical and Applied Sciences, Central Queensland University, 4702 Rockhampton North, Queensland, Australia
2 Coastal Marine Ecosystems Research Centre, Central Queensland University, 4680 Gladstone, Queensland, Australia
Abstract
The COVID-19 pandemic has affected several facets of human existence globally. To counter the spread of the virus, several vaccines have been developed and administered worldwide, using various technologies. Due to the need for the mRNA to be safely ‘protected’ until it can reach the host’s cells, innovative transport, casing, stabilization and attachment mechanisms need to be harnessed to accompany the mRNA. Nanotechnology has featured in several such capacities. Therefore, our short review explores the role of nanomaterials in COVID vaccines, with a core focus on those based on mRNA. Often, the chemistry of these nanomaterials is critical to their success in these, and such important aspects are highlighted in our review. Towards the end, we have also discussed the various vaccine types.
Keywords
- COVID
- micro RNA
- lipids
- nanotechnology
- vaccines
The COVID-19 pandemic is believed to have originated in Wuhan China and for over two years, affected several facets of human existence globally [1]. The statistics on mortality and hospitalizations from the pandemic are still being updated at the time of writing, however by the end of 2021, 690.37 persons per million had succumbed to the virus globally [2]. Against a global population of 7.87 billion in 2021 [3], this number is a conservative representation of about 5.4 million deaths from the pandemic. In contrast, the Spanish Flu had claimed 100 million lives between 1918–1920 [4]. Despite the lower statistic for COVID-19, contextualized against the technological advancements in science (including medicine and health) within a hundred years, the death toll from COVID-19 is simply astonishing.
There are several vaccines on the market [5]. Among these, the Pfizer-BioNTech (Comirnaty®) vaccine [6] and the Moderna COVID-19 (Spikevax®) vaccines were fully licensed for use on December 16, 2021 and January 31, 2022, respectively [7]. Both are notably based on mRNA technology. The effectiveness of such mRNA vaccines is dependent on the mRNA being protected until it reaches the appropriate cell regions where the payload is to be released. There are several advantages with using mRNA vaccines. The non-infectious mRNA cannot be integrated in the genome of the host, the mRNA is processed directly in the cytosol, it has a short half-life which can easily be regulated and it is immunogenic [8].
The protection of the mRNA is therefore critical to its success as a vaccine. This is where nanomaterials are often used as the choice of nanocarrier. The use of nanoparticles as drug delivery vehicle is a relatively new development in medicine, with the first examples appearing in the early 1970’s [9, 10]. However, the use of the ‘nano’ term did not come about until 1974 when Norio Taniguchi coined ‘nanotechnology’, which is the observation, measurement, manipulation, assembly, control, and manufacture of matter at the nanometer scale [11]. Nanomaterials (including those carrying pharmaceutical drug payloads) have at least one critical dimension of up to 100 nm and generally adopt 3-dimensional stable particle forms [10, 12].
This paper has been prepared with a view to explaining the role of lipid nanoparticles in the Pfizer-BioNTech® and Moderna® COVID-19 vaccines. It begins with a detailed review of the constituents and structure of mRNA/lipid nanoparticles (MLNPs) in the vaccines, as well as a comparison of these to other vaccines used for COVID-19 and similar respiratory viruses, such as influenza. The benefits, limitations, and efficacy of the MLNPs will then be explored, addressing concerns raised from their use with the goal of showing that vaccine hesitancy related to this technique is, for the most part, unfounded.
Vaccines help increase the body’s ability to produce antigens against biological threats. A vaccine against a virus contains weakened or inactive fragments of the virus. By being weakened or inactive, the actual threat of harm from the viral fragment remains low. However, it is still sufficient to act as a blueprint for the body to produce the appropriate antigens against the virus [13].
To be successful, a vaccine may require to be delivered to specific tissue sites for maximal action. To ensure this, vaccines may require controlled or delayed release once administered [14]. This is where protection of the payload in the vaccine is critical to its success.
Therefore, more specifically, the vaccine payload may be coated with protecting casing and the assembly is implanted (often via injection) into an individual. As soon as this occurs, the assembly meets the cells of the human body, causing the cells to immediately react to this ‘foreign intrusion’ and capture it. The assembly then makes its way to the nucleus where the cell’s own DNA is stored. There, the payload is released into the nucleus where its DNA information is read and copied onto a messenger RNA molecule.
The mRNA then leaves the cell with the genome information that it was ‘given’ by its cell and starts to assemble spike proteins as directed by the genome. Because the spike proteins that the mRNA produces are foreign to the human body, they trigger an immunological response which is the body’s defense against future intrusions by the same virus.
The important constituent of these vaccines is the liposome, a self-assembling, spherical-shaped vesicle consisting of lipid bilayers. The term “liposome” was coined in the 1960s following the discovery of closed bilayer lipid vesicles spontaneously forming in water. However, it was not until the early 1990s that the term “lipid nanoparticle” came into use, and it is due in large part to the emergence of the nanotechnology era. In fact, because of their lipid composition and having at least one critical dimension of up to 100 nm, liposomes are also considered as the earliest generation of lipid nanoparticles [15]. The first lipid nanoparticle application to carry RNA was approved in 2018, although it was in theranostic applications [16, 17]. Hou et al. have already and excellently captured the historical developments in mRNA and lipid nanoparticles technologies, which is why it is not re-examined in this discussion [17].
Fig. 1 (Ref. [18]) depicts the historical development of liposomes, especially illustrating the flourish of applications in the last two decades.
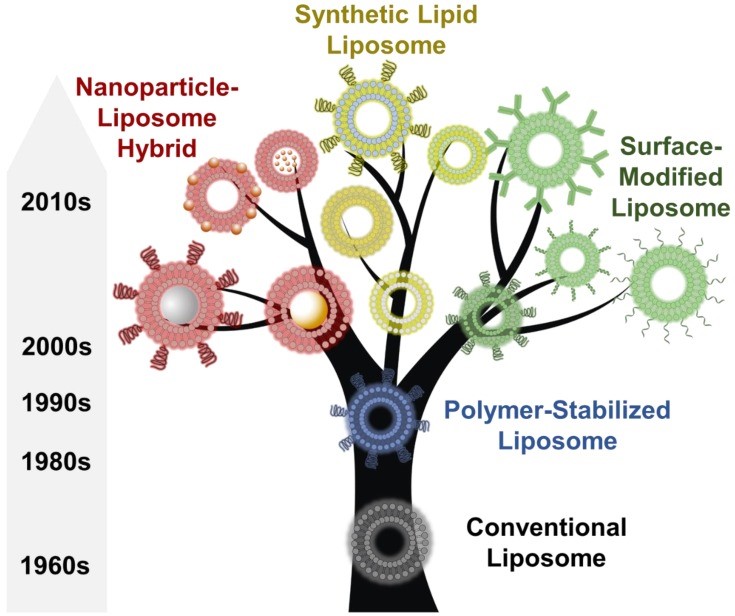 Fig. 1.
Fig. 1.An overview of the discovery, development, and evolution of liposomes since their first report in 1965. Reproduced under Creative Commons License [18].
While the first lipids were entirely natural, synthetic liposomes have emerged in recent applications. The reason for their popularity as drug carriers stems from their morphological similarity to that of cellular membranes as well as their ability to incorporate various substances [19].
Lipids play an extremely important role in the mRNA vaccines. When in the sub-100 nm sizes that they are used in, lipid molecules are stable, low-cost, biocompatible and well endured by natural biochemicals in the body such as fatty acids, triglycerides, waxes and steroids [20, 21].
It is within the enclosing liposomes that aqueous cores bearing the biomolecule payload is transported [17, 22]. In the case of the mRNA vaccines, such as those from Pfizer-BioNTech and Moderna®, this biomolecule is a section of mRNA (hence the term mRNA vaccine).
A lipid molecule can be assigned a head and tail end, and the way each end of one lipid interacts with those of others around it within the same nanoparticle unit has direct influence on the shape of the overall nanoparticle. The amount of water contained both within and externally to the nanoparticle is also believed to play a role in its structure [23], although the mechanism remains unclear [24]. The arrangement of lipids also facilitates variations in the water channels formed by the liposome. These channels may be stacked throughout the liposome in a so-called honeycomb structure, or they may be found as continuous nonintersecting channels that run through the liposome [25]. Furthermore, the incorporation of artificial water channels made from carbon nanotubes into the surface of the lipid layer can also replicate the function of aquaporins in biological membranes [25, 26]. External factors including temperature, pressure, light, and magnetic fields also contribute to the final structure of the liposome [27]. Temperature affects the chemical stability of the molecule, which is why low temperatures are used for lipid storage or nanoparticle lypholization [28]. Hydrostatic pressure helps in the colloidal stabilization of lipid nanoparticles [29]. Light accelerates lipid oxidation, thus degrading its structure [30]. Similarly, the presence of a magnetic field is known to influence lipid peroxidation [31]. Thus, different combinations of lipids, water content, and external factors give rise to several phases for the lipid nanoparticle, the most common of which are shown in Fig. 2 (Ref. [27]).
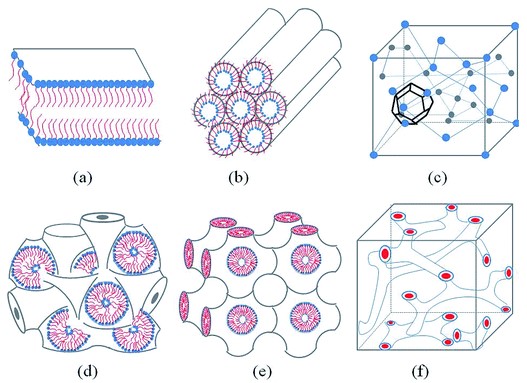 Fig. 2.
Fig. 2.Schematic representation of the phases most common to neutral lipid/water systems. (a) Lamellar phase. (b) Reverse hexagonal phase. (c) Reversed micellar cubic. (d) Reversed bicontinuous cubic (lm3m). (e) Reversed bicontinuous cubic (Pn3m). (f) reversed bicontinuous cubic (Ia3d). Reproduced under Creative Commons License [27].
The differing positions inside these structures affects the route and rate of payload diffusion [32]. In the case of mRNA, which is a hydrophilic payload, it is most likely to take up position in the large water channels which form upon entering the hexagonal phase, which gives it a superior release rate compared to the bicontinuous cubic and lamellar phases [32, 33].
The major lipid components in liposomes are ionizable (hence bearing the name
ionizable lipids). Due to this ability and their pK
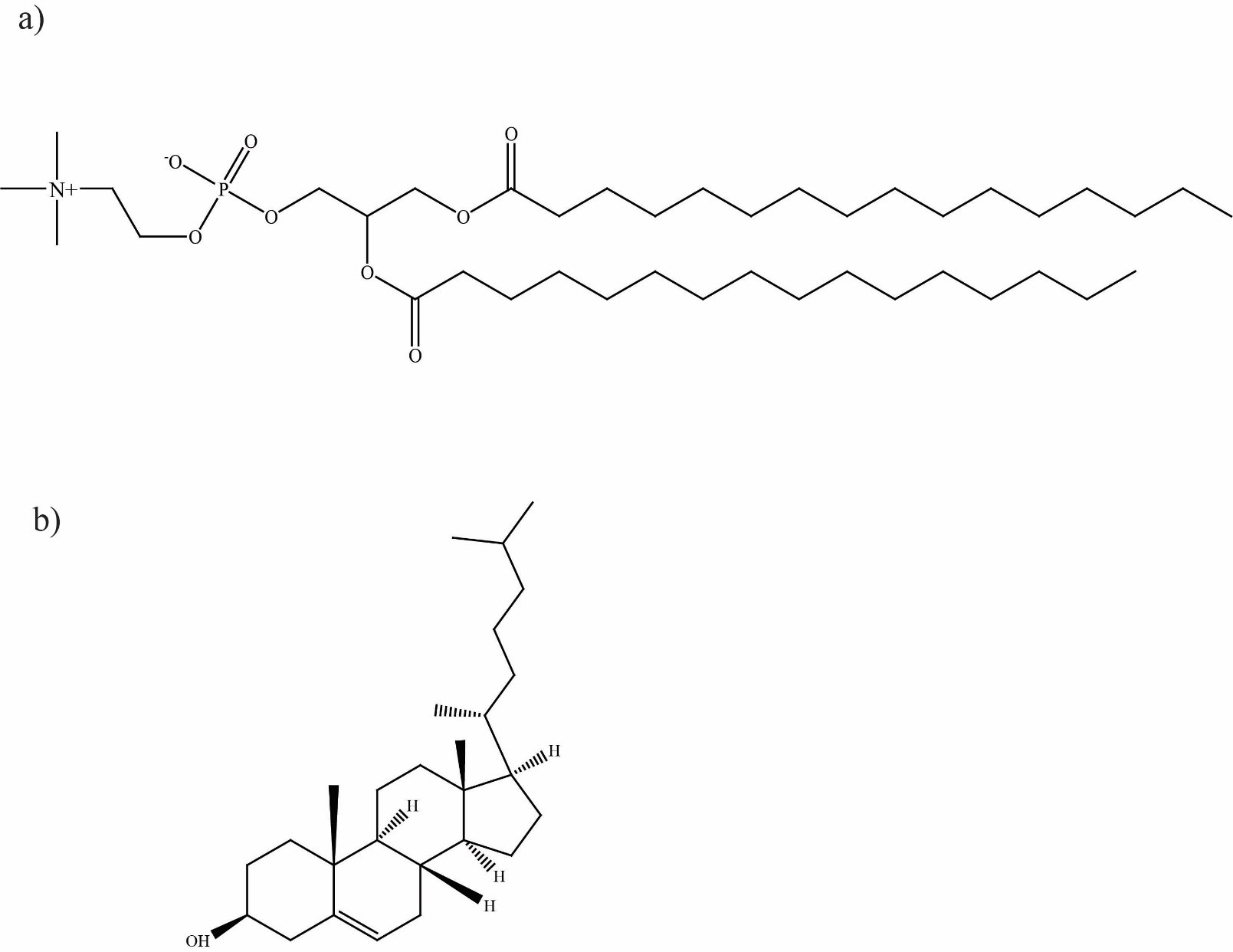 Fig. 3.
Fig. 3.Structures of (a) distearoylphosphatidylcholine (DSPC) and (b) cholesterol.
In the lipid nanoparticle, cholesterol aids in phase changes of the lipid bilayer which enhances stability and also allows it to alter shape at physiological temperatures, enhancing the release rate of the mRNA payload when in the cell cytosol [16, 17]. As cholesterol is also naturally found in cell membranes, its presence is less likely to provoke an immune response from the body [34]. This is achieved by lowering the transition temperature of the lipid nanoparticle, which in turn allows it to easily move from the lamellar phase to the hexagonal phase [16].
In fact, cholesterol plays such a vital role in this phase change that future
versions of MLNP vaccines may introduce naturally-occurring cholesterol analogues
such as
The use of another type of lipid, polyethylene glycol (PEG) achieves some useful outcomes in mRNA vaccine delivery. The particular PEG lipid varieties used in the Pfizer-BioNTech® and Moderna® vaccines are ALC-0159 and PEG-DMG, respectively [33]. PEG-lipids have several vital roles in the lipid nanoparticle. Their capacity to increase both compression of the lipid bilayer and repulsive forces between particles also makes PEG-lipids crucial for decreasing nanoparticle aggregation and controlling the size of the final nanoparticle [16]. By compacting the size of the nanoparticle bearing the mRNA, opsonization (the immune system’s method of tagging foreign pathogens for destruction) is minimized, enabling increased circulation time for the carriers in the body [16, 17].
In a similar manner to mRNA vaccines, viral vector vaccines aim to deliver a section of genetic material to the cell where it can be processed to produce a protein that elicits an immune response [23, 36]. The difference in this technique comes from the carrier, which in the case of viral vectors is a modified version of a different virus, most commonly retrovirus, adenovirus, lentivirus, or herpes simplex virus [36]. Two of the other common COVID-19 vaccines produced by the manufacturers Oxford/AstraZeneca® and Janssen/Johnson & Johnson® utilize the viral vector method. This takes the form of a modified adenovirus containing genetic material for the SARS-CoV-2 spike protein [23, 36].
Whole-inactivated and live-attenuated vaccines contain version of the target virus which has been artificially weakened through heat, chemical treatment, or a gene sequence change that retards their reproductive rate [36]. These types of vaccines are very common for preventing seasonal influenza, and there are several versions still under development for COVID-19 [36, 37]. As may be inferred, the structure of these vaccines is the same as the wild-type virus. Other, subunit protein vaccines contain the specific fragments of a virus that elicit the immune response, which is stimulated such that an immunity to the target virus is developed [37, 38]. Vaccines that utilize this structure have been used to prevent Middle Eastern Respiratory Syndrome (MERS-CoV), and other vaccines addressing SARS-CoV-2 are still under development [38]. In the case of COVID-19 vaccines, the subunit is the spike protein.
A key attribute of MLNP vaccines is their rapid development cycle: once the applicable section of mRNA has been identified, it can readily be incorporated into the nanoparticle delivery vehicle and deployed [33]. Their comparative advantages over other vaccines include good patient tolerance, a flexible and wide choice of coding molecules, the ability to engineer these vaccines to full-length antigens containing multiple epitopes without significant major histocompatibility complex (MHC) restriction and are easy to mass produce [39]. The latter two features are of particular note. Epitopes represent the section of an antigen which is recognizable to the body’s immune system, so synthesis of vaccines can be more targeted and versatile [38]. The MHC produces major histocompatibility complex molecules, which are the portions of cells which present antigen peptides to the cell surface to be combated by T-cells, but this immune response can only be successful with specific MHC molecules. MHC restriction materializes through the inability of T-cell receptors to bind to certain MHC molecules and therefore be rendered ineffective at developing the desired immune response [40]. Vaccines with lower MHC restriction are therefore likely to provide greater treatment efficacy.
As our article has demonstrated, the ability to incorporate cholesterol and PEG-lipids improves circulation times and integration of vaccine payloads with host cells. In addition, and potentially most importantly, these types of vaccines are considered very safe due to a reduced likelihood of infection and endotoxin exposure or potential for genomic integration which are associated with whole-inactivated and live-attenuated vaccines [41].
As with any technology, there are downsides to the use of mRNA/lipid nanoparticle vaccines which relate primarily to their stability. For instance, the susceptibility of mRNA to enzymatic degradation by the body’s natural enzymes remains a constant concern [42]. In addition, the long chains of nucleotides that comprise mRNA are critical to be retained to full length for active translation. Such long chains often increase the risk of degradation [43].
In addition, the concerns around nanoparticles intruding in human tissues/organs extend to nanocarrier systems such as in vaccines. Similarly, shedding of the antigen and/or related peptide fragments is a likely occurrence [44].
Concerns around long-term effects of mRNA vaccines may prevail until more scientific information becomes available. Reports from the clinical trials of both the Pfizer-BioNTech® and Moderna® products reveal that instances of serious short-term adverse effects were rare, and when they did occur, the manifestation was similar in both the treatment and placebo groups [45, 46, 47].
In this commentary, we have examined the nanotechnology associated with the vaccines developed against the SARS-Cov-2 virus. Our coverage included all the various types of vaccines that are in the market. However, evidently, it is the mRNA vaccines that extensively rely on the use of nanomaterials, and these nanomaterials include liposomes and lipids. As a result, our focus has been largely on mRNA vaccines. We have examined the roles of both liposomes and lipids which include carriage of the mRNA entity, its stabilization, protection from the body’s phagocytic system and eventual, controlled release. We have also extended the discussion to cholesterol and its effect on affording greater protection to the nanocarrier. It is hoped that our detailed analysis of the structure of MLNPs in the Pfizer-BioNTech® and Moderna® vaccines, as well as showing some of their benefits and limitations would be useful in highlighting the role of nano-sized components in vaccines against the SARS-Cov-2 virus.
RJB wrote the original manuscript and SC revised and rewrote it for submission. After review, both authors contributed to the revision.
Not applicable.
Not applicable.
This research received no external funding.
The authors declare no conflict of interest.
References
Publisher’s Note: IMR Press stays neutral with regard to jurisdictional claims in published maps and institutional affiliations.



