1 Department of Anesthesiology, The First Affiliated Hospital of Shaoyang University, 422000 Shaoyang, Hunan, China
2 Department of Anesthesiology, Hunan Want Want Hospital, 410000 Changsha, Hunan, China
Abstract
Background: This study aims to investigate the effect of ropivacaine
combined with sufentanil on hemodynamics and expression levels of serum tumor
necrosis factor-
Keywords
- ropivacaine
- sufentanil
- cesarean section
- hemodynamics
- inflammatory reaction
- tumor necrosis factor-α
- interleukin-6
- anesthesia
Cesarean section provides an effective solution for dystocia and serious
obstetric complications. Women during pregnancy have different anatomy and higher
sensitivity to anesthetics. Reasonable anesthesia method is a key factor to
ensure successful completion of cesarean section as well as good maternal and
infant outcomes [1]. Clinical operation of cesarean section may cause abnormal
stimulation of the sympathetic nerves of pregnancy body, rapid increase in the
levels of norepinephrine and blood glucose, leading to higher heart beat and more
violent contraction of the systemic blood vessels, and various complications.
Moreover, cesarean section affects the uterine contraction, incision pain and
postpartum recovery of the women [2]. At the same time, surgical wounds can
stimulate the body to release tumor necrosis factor-
The clinical data of 135 women who received cesarean section in our hospital
from March 2021 to June 2022 were retrospectively collected (the case screening
process is shown in Fig. 1), and all of them were single pregnancy. Inclusion
criteria: ① Full-term pregnancies; ② No contraindications to
intravertebral anesthesia. Exclusion criteria: ① Complicated with severe
gestational hypertension and diabetes; ② Twin or multiple pregnancies;
③ Allergy to anesthetic drugs; ④ Complicated with mental
diseases. Through anesthesia, 135 parturients were divided into observation group
and control group. In the observation group, there were 68 patients (41 cases of
primiparum and 27 cases of multiparum) aged 21~36 (28.64
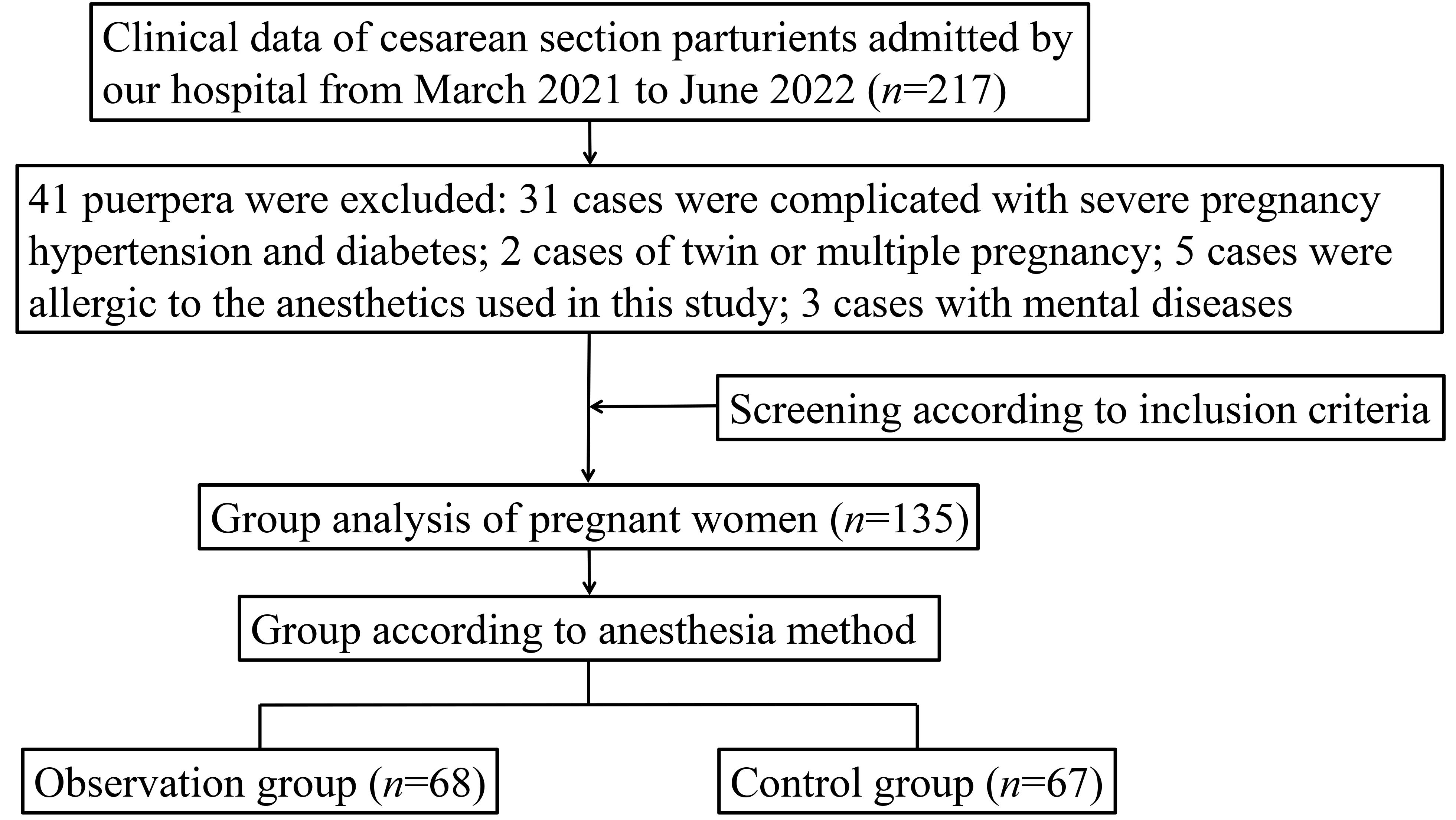 Fig. 1.
Fig. 1.Case screening flow chart.
The two groups were given elective cesarean section, with all examinations
completed before the surgery. The parturients were instructed to abstain from
drinking and fasting, taking the left lateral position. The control group was
given ropivacaine for lumbar anesthesia, the puncture site was
L
① The time for anesthesia to reach the highest block level and
analgesic maintenance time were recorded in both groups. Visual analog scale
(VAS) was used to evaluate the degree of pain in parturients at the 6th hour
after delivery. ② The mean arterial pressure (MAP), heart rate (HR),
cardiac output (CO), stroke volume (SV) and systemic circulation resistance (SVR)
of the two groups were recorded before anesthesia (T
SPSS 22.0 software (IBM Corp., Armonk, NY, USA) was used for statistical
processing. The measurement data were expressed as
Table 1 shows the time for anesthesia to reach the highest block level,
analgesic maintenance time and the VAS score at the 6th hour after delivery of
the two groups. Compared with the control group, the observation group had a
shorter time to reach the highest block level, longer analgesic maintenance time
and lower VAS score at the 6th hour after delivery (all p
| Group | Time to reach the maximum block plane (min) | Time to maintain analgesia (h) | VAS score at 6 h postpartum (score) |
|---|---|---|---|
| Observation group | 9.79 |
6.48 |
4.06 |
| Control group | 13.26 |
5.24 |
4.75 |
| t | 7.666 | 4.296 | 3.095 |
| p | 0.000 | 0.000 | 0.002 |
VAS, visual analog scale.
Table 2 shows the MAP, HR, CO, SV and SVR levels of the two groups at different
time. Compared with the control group, observation group had higher MAP and HR at
T
| Group | MAP (mmHg) | HR (times/min) | CO (L/min) | SV (mL/times) | SVR (dyne/(s·cm | |
|---|---|---|---|---|---|---|
| Observation group | ||||||
| T |
92.78 |
76.34 |
6.20 |
76.46 |
1235.84 | |
| T |
89.65 |
75.07 |
5.53 |
71.32 |
1092.63 | |
| T |
93.83 |
77.92 |
4.87 |
63.59 |
1018.53 | |
| Control group | ||||||
| T |
93.14 |
75.86 |
6.16 |
75.48 |
1249.36 | |
| T |
81.47 |
66.58 |
5.13 |
67.31 |
1002.54 | |
| T |
95.83 |
79.15 |
4.52 |
59.27 |
943.48 | |
| F | F |
F |
F |
F |
F | |
| p | p |
p |
p |
p |
p | |
MAP, mean arterial pressure; HR, heart rate; CO, cardiac output; SV, stroke volume; SVR, systemic circulation resistance; F, analysis of variance.
Table 3 shows the PaCO
| Group | PaCO |
PaO | |
|---|---|---|---|
| Observation group | |||
| T |
50.21 |
32.75 | |
| T |
48.87 |
32.61 | |
| T |
49.28 |
32.03 | |
| Control group | |||
| T |
49.89 |
32.68 | |
| T |
57.41 |
28.82 | |
| T |
55.63 |
28.36 | |
| F | F |
F | |
| p | p |
p | |
PaCO
Table 4 shows serum TNF-
| Time | TNF- |
IL-6 (ng/mL) | |
|---|---|---|---|
| Observation group | |||
| 1 d before delivery | 1.65 |
0.17 | |
| The 12th hour after delivery | 2.17 |
0.26 | |
| The 24th hour after delivery | 2.76 |
0.33 | |
| Control group | |||
| 1 d before delivery | 1.68 |
0.18 | |
| The 12th hour after delivery | 3.13 |
0.34 | |
| The 24th hour after delivery | 3.65 |
0.41 | |
| F | F |
F | |
| p | p |
p | |
TNF-
The Apgar scores of neonates were (9.24
The cesarean section rate has been climbing in recent years [7, 8]. Cesarean section means the fetus is taken out via abdominal incision without vaginal delivery, which is an important way to save the life of pregnant women and perinatal infants in obstetrics. Cesarean section as invasive midwifery practice can stimulate maternal abdominal organs, causing pain. The body released a large amount of catecholamines within 48 h after cesarean section, which could cause pain peaks, reduced secretion of oxytocin and decreased uterine contraction ability, resulting in affected maternal hemodynamics [9]. Appropriate anesthetics and anesthesia method can guarantee the smooth operation of cesarean section, and reasonable and effective anesthetic drugs can help reduce postpartum inflammatory reaction and stress reaction [10]. In cesarean section, anesthetic drugs enter the fetus through the placental barrier, producing certain effects on the fetus. Therefore, it is of great clinical significance to select appropriate anesthetics for cesarean section.
Ropivacaine, as long-acting amide local anesthetic, plays an anesthetic role in inhibiting the flow of sodium ions in nerve cells, blocking ion exchange and blocking nerve conduction. This drug is less toxic to the central nervous system and cardiovascular system of the parturients, which is commonly used for local anesthesia during cesarean section [11]. Compared with other anesthetic drugs, ropivacaine has higher sensitivity and longer anesthetic duration, but the blocking effect needs to be improved. Opioids are powerful analgesics. Sufentanil is an opioid receptor agonist with high lipophilic properties. Sufentanil acts on opioid receptors and binds to blood proteins via the blood-brain barrier, and it is eliminated quickly and has a short half-life after infusion. At the same time, it can directly reach the subarachnoid space through the lipid dura mater, exerting rapid anesthesia block effect, without causing respiratory depression or affecting postoperative recovery [12]. Clinical studies [13, 14, 15] have confirmed that local anesthetics combined with opioids can play a synergistic role in analgesia, reduce the dosage of anesthetic drugs, stabilize hemodynamics, and reduce the adverse reactions caused by anesthetic drugs. In this study, women who underwent cesarean section received anesthesia using ropivacaine combined with sufentanil before surgery. Compared with the control group, the time for anesthesia to reach the highest block level was shorter, the analgesic maintenance time was longer and the VAS score at the 6th hour after delivery was lower in the observation group. It suggests that ropivacaine combined with sufentanil can accelerate the onset time of anesthesia, extend the analgesia duration and reduce postoperative pain, showing better anesthetic effect than using ropivacaine alone.
Wang et al. [16] reported that spinal epidural anesthesia after combined use of ropivacaine and sufentanil has shorter onset time, shorter labor process, more obvious analgesic effect and lower incidence of adverse reactions than continuous epidural anesthesia. Miao et al. [17] found that combined administration of epidural ropivacaine and sufentanil could relieve pain after cesarean section. However, the effect of ropivacaine combined with sufentanil on the hemodynamics of cesarean section parturients remains to be verified. The changes of hemodynamic indexes (MAP, HR, CO, SV, SVR, etc.) are the focus of monitoring in clinical anesthesia during gynecological surgery. The results of this study showed that the hemodynamic stability was better in the observation group than in the control group. The reason may be that anesthesia can be stopped quickly after withdrawal regardless of how long sufentanil is administered. Moreover, sufentanil has good hemodynamic stability to effectively guarantee myocardial oxygen supply. The results of this study also showed that the change of arterial blood gas indexes was less significant in the observation group than in the control group, suggesting that ropivacaine combined with sufentanil could better stabilize blood gas indexes.
TNF-
To conclude, ropivacaine combined with sufentanil has a good anesthetic effect on cesarean section, which can effectively stabilize maternal hemodynamic indexes and induce body inflammatory response without causing any adverse effects on the fetus, demonstrating certain clinical application value.
The datasets used during the present study are available from the corresponding author upon reasonable request.
ML—Manuscript writing, Project development, Data Collection. DM—Designed the research, revised the paper, Data analysis. BL and JZ—Data collection. All authors contributed to editorial changes in the manuscript. All authors have participated sufficiently in the work and agreed to be accountable for all aspects of the work. All authors read and approved the final manuscript.
All subjects gave their informed consent for inclusion before they participated in the study. This retrospective study involving human participants was conducted in accordance with the ethical standards of the institutional research committee and the 1964 Helsinki Declaration and its later amendments. The protocol was approved by the Ethics Committee of The First Affiliated Hospital of Shaoyang University (approval number: SYFY2021008).
Not applicable.
This research received no external funding.
The authors declare no conflict of interest.
References
Publisher’s Note: IMR Press stays neutral with regard to jurisdictional claims in published maps and institutional affiliations.

