1 Breast Unit, Academic Hospital of Udine, 33100 Udine, Italy
2 Ennergi Research, 33050 Lestizza, Italy
3 Department of Neuroscience, Rehabilitation, Ophthalmology, Genetics, Maternal and Infant Health, University of Genoa, 16132 Genova, Italy
4 Obstetrics and Gynecology Unit, IRCCS Istituto Giannina Gaslini, 16147 Genova, Italy
5 Institute of Pathologic Anatomy, DAME, Academic Hospital of Udine, 33100 Udine, Italy
6 Clinic of Plastic Surgery, DAME, Academic Hospital of Udine, 33100 Udine, Italy
7 Clinic of Surgery, DAME, University of Udine, 33100 Udine, Italy
Abstract
Background: The introduction of skin-sparing mastectomy (SSM) and
nipple-sparing mastectomy (NSM) with immediate reconstruction allowed a
noticeable improvement in reconstructive surgery aesthetic results and patients’
psychophysical well-being. In any case, there are still concerns about the
long-term oncological safety of these two procedures. This study aims to assess
the oncological outcomes of women who underwent SSM and NSM and to compare them
with traditional modified total mastectomy (MTM). The secondary outcome was to
compare mastectomy with breast-conserving surgery (BCS) outcome.
Methods: We performed a retrospective chart review study concerning all
patients who had experienced SSM and NSM in our Clinic between January 2004 and
July 2013. The main outcomes were overall survival (OS), disease-free survival
(DFS), and recurrences cumulative rate. Results: Among this study’s 1836
invasive breast carcinomas, we found NSM (86.7, 95% confidence interval (CI),
76.7–98.0%) to have a significantly shorter 5-year DFS than MTM (90.4%, 95%
CI, 87.9–93.0%). Furthermore, low body mass index (odds ratio (OR) 0.733,
p = 0.056), basal-like molecular subtype (OR 28.932, p
Keywords
- breast cancer
- nipple-sparing mastectomy
- skin-sparing mastectomy
- disease-free survival
- breast-conserving surgery
- modified total mastectomy
- overall survival
- local recurrence
Skin-sparing mastectomy (SSM) and nipple-sparing mastectomy (NSM) allowed for a noticeable improvement in reconstructive surgery aesthetic results [1]. SSM, in particular, is defined as the removal of the mammary gland and the nipple-areola complex (NAC) with breast skin sparing, whereas NSM saves both the NAC and the breast skin [1, 2, 3]. Both of these procedures aim to reduce the sense of mutilation after breast cancer surgery, particularly NSM, by avoiding NAC loss, which patients will not fully perceive until several weeks after surgery [2, 4, 5, 6, 7].
Candidates for SSM and NSM are generally subjected to an immediate reconstruction, which can be prosthetic or non-prosthetic, as well as in a single stage or two stages in the case of expander placement. Consequently, a further fundamental aspect to be taken into consideration when speaking of skin- or nipple-sparing mastectomy is that of perioperative complications, generally associated with reconstructive procedures, which can also significantly impact the patient’s well-being [8].
Women’s psychophysical wellness, which results strongly related to their individual perception of the aesthetic result, represents a critical target of breast reconstruction [2]. And actually, it is demonstrated by the current literature that psychophysical stress may correlate with bad oncological outcomes [9]. Therefore, it is imperative to achieve an optimal balance between oncological safety and aesthetic results [10].
Comparing SSM and NSM with the traditional modified total mastectomy (MTM), the current literature supports the oncological safety of these two procedures followed by immediate reconstruction, recognizes their evident improvement of cosmetic results to a high degree, and excludes any evidence of impairment of disease local control nor any increase of local or distant recurrence rates [11, 12, 13, 14], especially when combined with the use of radiation therapy and adjuvant chemotherapy, as indicated [15]. However, controversies still exist about the long-term oncological safety of these two procedures, and the data in the literature are not conclusive [16, 17, 18].
Our study aims to evaluate the oncological outcomes of women who underwent SSM and NSM in terms of overall survival (OS) and disease-free survival (DFS) and to analyze eventual risk factors for recurrence in patients treated by NSM, comparing them to MTM. The secondary aim was to compare the outcome of mastectomy to breast-conserving surgery (BCS).
In this retrospective chart review study, we collected data on all consecutive women who had invasive breast carcinoma surgery in our Clinic between January 2004 and December 2013. The data was collected up until December 2018. Furthermore, the study was carried out following the Helsinki Declaration and was approved by the Internal Review Board (IRB). Furthermore, with regard to the consent for processing data used in this retrospective analysis, we followed the guidelines of the Italian Data Protection Authority’s general authorization to process personal data for scientific research purposes.
In this study, we retained all women affected by invasive breast carcinoma with complete information about the type of intervention performed, either mastectomy or BCS. We excluded all subjects with tumor-node-metastasis (TNM) stage IV at the time of diagnosis. The data for selection and analysis was gathered from our Clinic’s operative theater register and clinical files.
This study’s primary outcomes were overall survival (OS), disease-free survival (DFS), and local or distant recurrences. Additional information about patient characteristics, tumor characteristics, and non-surgical treatments was gathered. Body mass index (BMI), age at diagnosis, fertility status, familial history of breast or ovarian cancer, and eventual use of estrogen/progesterone therapies were all factors considered. TNM tumor size, histological type, stage at diagnosis, Mib1/Ki-67 proliferation index, tumor grading, hormone receptor status (Estrogen Receptor (ER), Progesteron Receptor (PR), and Her2/neu expression), and other microscopic features such as peritumoral inflammation (PTI), multicentricity/multifocality, peritumoral vascular invasion (PVI), or extensive intraductal component (EIC) were all evaluated [19, 20]. TNM nodal status, eventual involvement of loco-regional extra-axillary lymph nodes (internal mammary chain or subclavian), lymph node extracapsular invasion (ExCp), and bunched lymph nodes were all taken into account. We also looked into therapeutic management, which included neoadjuvant therapies, breast and axillary surgery, and adjuvant treatment (breast irradiation, endocrine therapy, and chemotherapy).
As previously stated, pathological tumor stage (pTNM) was defined using the VII edition of the TNM classification (AJCC/UICC), tumor histology was classified using World Health Organization criteria modified by Rosen and Oberman, and tumor grade was determined using Elston and Ellis’ recommendations [19, 21]. We assessed the presence of PVI using the previously stated Rosen and Oberman criteria [19, 21]. Furthermore, as previously described, the expression and quantification of ER, PR, Her-2/Neu, and the proliferative tumor fraction (Mib1/Ki67) were assessed [19, 21]. Furthermore, we defined lymph node ExCp as extracapsular tumor cell growth, invasion of perinodal fat, or extranodal tumor cell location [19, 21].
For the purpose of the study, we divided our population into four groups according to the type of breast surgery performed: women treated only by BCS, NSM group, SSM group, and MTM group.
The included group of patients was treated by the same multidisciplinary surgical team, including a breast surgeon and, when required, a reconstructive surgeon. The surgical techniques used were BCS or mastectomy.
BCS consisted of the removal of a limited portion of the breast, including the neoplastic lesion, starting from the skin up to the pectoralis major muscle fascia. Clips are usually left at the level of the resection bed in order to guide any subsequent complementary radiotherapy. The macroscopic intraoperative pathological evaluation of the piece allows to exclude of a gross involvement of the margins, which obviously is evaluated microscopically later, and in the case of non-palpable lesions, the radiological evaluation of the piece allows to verify the inclusion in the same of microcalcifications and metal clips where necessary. In the case of non-palpable breast lesions, BCS was performed according to wire-localized breast biopsy (WLBB) or radio-guided occult lesion localization (ROLL) [10, 22].
Mastectomy was performed according to three different techniques: MTM, SSM, and NSM. MTM was performed by removing the breast (including the breast skin, breast parenchyma, and NAC), and the lining over the pectoralis major was also removed but spearing the pectoralis major muscle itself. The SSM was performed as MTM, but the skin incision was periareolar, the breast skin was conserved, and the biopsy scar was removed [2]. The NSM was performed as SSM, but the NAC was conserved, and the skin incision was inframammary [2]. In particular, the subcutaneous dissection under the areola was aimed at removing the glandular and ductal tissue without compromising the vascularization of the NAC. The ducts beneath the areola were analyzed by frozen section, and the NAC was removed in case of positive histology. Also, in case of poor supply and a high risk of NAC necrosis, the breast surgeon could decide to remove the NAC before radiotherapy. Surgical resection of the needle biopsy tract, including the dermal entry site, was always performed at the time of mastectomy, based on the evidence of displacement of tumor cells and the potential non-resection of such tumor seeding at the time of skin-sparing mastectomy [23].
Patient preference was noteworthy in determining whether to use MTM, SSM, or NSM. SSM was typically used to treat extensive, multicentric, or recurrent lesions and early-stage breast cancer for which breast-conserving therapy was ineffective. In this population, the only absolute contraindication considered was tumor skin involvement. Cases with invasive carcinoma located peripherally in the breast parenchyma (any of the four quadrants with a distance from the NAC equal or greater than 2 cm) and clinically negative axilla were additional selection criteria in the case of NSM. As a result, preoperative imaging (mammography, ultrasound, and/or breast magnetic resonance imaging) and an intraoperative retro-areolar biopsy of ductal tissue were used to assess NAC involvement.
Every patient’s reconstructive strategy after mastectomy was evaluated individually, considering tumor characteristics, planned non-surgical treatments, breast volume and shape, and the patient’s personal desires. Depending on the contraindications, the size of the breast, and the patient’s wishes, immediate breast reconstruction (IBR) techniques included the insertion of an expander, a definitive prosthetic implant, or autogenous tissue [24].
Axillary surgery was performed as previously described by sentinel lymph node biopsy (SLNB) followed as necessary by complete axillary lymph node dissection (CALND) [19, 20]. In the case of SLNB, patients underwent subdermal, periareolar, or perilesional injection of 2.5 mL of human serum albumin macroaggregate labeled with 74 mBq 99 m-technetium 3 to 24 hours before surgery. All hot nodes are intra-operatively identified by a gamma finder and then sent to intra-operative examination (one-step nucleic acid amplification or frozen section) [19], whereas, in the case of identification lack, an axillary lymph node sampling is performed. Breast radiotherapy was indicated after BCS except for some selective cases in which age and comorbidities contraindicated it. Chest wall radiotherapy was delivered when indicated in patients with locally advanced tumors. Regional lymph nodes have been irradiated in all cases involving more than 3 lymph nodes, except for individual contraindications.
Data were analyzed using R (version 4.2.2, Vienna, Austria,
https://www.R-project.org/, accessed on 10 November 2022) and considering significant p
Potentially eligible women treated because of invasive breast carcinoma during the study period were in 2036. Among these, we excluded 104 cases of TNM stage IV at diagnosis and 96 patients from the analysis because of incomplete data about axilla or breast surgery or follow-up. Finally, 1739 women were considered eligible for the present study, treated for 1836 invasive breast carcinomas.
In Table 1, we present the population characteristics. The 49% (899/1836) of the considered cancers were treated by BCS, 4.7% (87/1836) by NSM, 10.7% (196/1836) by SSM, and 35.6% (654/1836) by MTM. CALND was required in 49.6% (911/1836) of women, including cases of primary CALND and those of CALND secondary to a positive intraoperative SLNB. The median follow-up was 66 months (34–98), and the maximum follow-up was 120 months.
| Variables | All (1836) | BCS (49%; 899/1836) | NSM (4.7%; 87/1836) | SSM (10.7%; 196/1836) | MTM (35.6%; 654/1836) | p(*) | |
|---|---|---|---|---|---|---|---|
| Woman age at surgery (years) | 59.14 ( |
59.36 ( |
51.17 ( |
52.95 ( |
61.77 ( |
1,2,3,5,6 | |
| BMI (kg/m |
25.71 ( |
25.89 ( |
24.18 ( |
24.36 ( |
26.05 ( |
1,2,5,6 | |
| Follow up time (months) | 66 (34–98) | 67.89 ( |
29.10 ( |
75.34 ( |
75.43 ( |
1,2,3,4,5 | |
| Tobacco smoke | 6.4% (118/1836) | 6.85% (49/715) | 1.82% (1/55) | 11.04% (18/163) | 9.43% (50/530) | 4 | |
| Familial history of cancer | 12.8% (235/1836) | 34.86% (114/327) | 40.43% (19/47) | 44.62% (29/65) | 38.62% (73/189) | NS | |
| Use of estrogen/progesteron pills | 6% (111/1836) | 33.33% (60/180) | 42.86% (6/14) | 34.88% (15/43) | 24.39% (30/123) | NS | |
| Post-menopausal status | 77.8% (1429/1836) | 82.76% (744/899) | 50.57% (44/87) | 60.20% (118/196) | 80.21% (523/652) | 1,2,5,6 | |
| Definitive axilla surgrery | |||||||
| CALND | 49.6% (911/1836) | 30.92% (278/899) | 33.33% (29/87) | 49.49% (97/196) | 77.52% (507/654) | 2,3,4,5,6 | |
| SLNB | 50.4% (925/1836) | 69.08% (621/899) | 66.67% (58/87) | 50.51% (99/196) | 22.48% (147/654) | 2,3,4,5,6 | |
| Non surgical therapy | |||||||
| Neoadjuvant chemotherapy | 5.6% (102/1836) | 3.34% (30/899) | 0.00% (0/87) | 5.10% (10/196) | 9.48% (62/654) | 3,4,5 | |
| Adjuvant radiotherapy | 54.5% (1000/1836) | 92.40% (814/881) | 11.90% (10/84) | 16.49% (31/188) | 22.52% (145/644) | 1,2,3,5 | |
| Adjuvant chemotherapy | 41.1% (755/1836) | 31.78% (280/881) | 54.76% (46/84) | 58.51% (110/188) | 49.53% (319/644) | 1,2,3,6 | |
| Adjuvant hormonal therapy | 78.4% (1439/1836) | 84.11% (741/881) | 76.19% (64/84) | 77.13% (145/188) | 75.93% (489/644) | 2,3 | |
(*) Significant differences with a p-value
BMI, body mass index; CALND, Complete Axillary Lymph Node Dissection; SLNB, Sentinel Lymph Node Biopsy; BCS, Breast-Conserving Surgery; NSM, Nipple-Sparing Mastectomy; SSM, Skin-Sparing Mastectomy; MTM, Modified Total Mastectomy.
The mean age of the whole population was 59.14 years (
Tables 2,3 show, respectively, tumor characteristics and TNM staging. The prevalence of Luminal A, Luminal Her, Her enriched, and Basal-like subtypes was similar in patients treated by BCS and NSM. Furthermore, women who underwent mastectomy (NSM, SSM, or MTM) had a higher prevalence of comedo-like necrosis, multifocality/multicentricity, extended intraductal component, and lymphovascular invasion than BCS. The prevalence of extra-capsular invasion of lymph node metastasis was similar between NSM and BCS. BCS had a significantly smaller tumor size and a more favorable nodal status than mastectomies (NSM, SSM, and MTM). However, the NSM group had a non-significant higher prevalence of N1, N2, N3, and G3 than the BCS group.
| All (1836) | BCS (899) | NSM (87) | SSM (196) | MTM (654) | p(*) | ||
|---|---|---|---|---|---|---|---|
| Histological type | |||||||
| Invasive carcinoma non-special type | 78.3% (1437/1836) | 81.42% (732/899) | 80.46% (70/87) | 80.61% (158/196) | 72.94% (477/654) | 3,6 | |
| Lobular invasive carcinoma | 12.9% (236/1836) | 10.68% (96/899) | 10.34% (9/87) | 14.80% (29/196) | 15.60% (102/654) | 3 | |
| Ductal and lobular invasive carcinoma | 5.4% (100/1836) | 4.56% (41/899) | 2.30% (2/87) | 2.04% (4/196) | 8.10% (53/654) | 3,6 | |
| Other invasive carcinoma | 3.4% (63/1836) | 3.34% (30/899) | 6.90% (6/87) | 2.55% (5/196) | 3.36% (22/654) | NS | |
| Tumor characteristics | |||||||
| ER positivity | 84.3% (1516/1799) | 87.54% (773/883) | 82.35% (70/85) | 80.41% (156/194) | 81.16% (517/637) | 2,3 | |
| PR positivity | 70.2% (1263/1799) | 73.05% (645/883) | 67.06% (57/85) | 68.04% (132/194) | 67.35% (429/637) | 3 | |
| Ki-67/Mib-1 |
31.8% (433/1362) | 24.32% (169/695) | 35.00% (28/80) | 45.68% (74/162) | 38.12% (162/425) | 1,2,3 | |
| Molecular Subtype | |||||||
| Luminal A | 37.9% (695/1836) | 46.83% (421/899) | 41.38% (36/87) | 27.55% (54/196) | 28.13% (184/654) | 2,3,4,5 | |
| Luminal B | 20.6% (378/1836) | 18.13% (163/899) | 29.89% (26/87) | 29.59% (58/196) | 20.03% (131/654) | 1,2,5,6 | |
| Luminal Her | 5.8% (107/1836) | 4.67% (42/899) | 6.90% (6/87) | 9.18% (18/196) | 6.27% (41/654) | 2 | |
| Her enriched | 4.7% (86/1836) | 2.22% (20/899) | 3.45% (3/87) | 9.18% (18/196) | 6.88% (45/654) | 2,3 | |
| Basal-like | 8.5% (156/1836) | 8.57% (77/899) | 10.34% (9/87) | 8.67% (17/196) | 8.10% (53/654) | NS | |
| Non descript | 22.5% (414/1836) | 19.58% (176/899) | 8.05% (7/87) | 15.82% (31/196) | 30.58% (200/654) | 1,3,5,6 | |
| Comedo-like necrosis | 10.3% (189/1836) | 8.01% (72/899) | 11.49% (10/87) | 17.86% (35/196) | 11.01% (72/654) | 2,3,6 | |
| Multifocality/multicentricity | 17.5% (322/1836) | 8.34% (75/899) | 28.74% (25/87) | 33.16% (65/196) | 26.61% (174/654) | 1,2,3 | |
| Extended intraductal component | 27.7% (509/1836) | 21.02% (189/899) | 39.08% (34/87) | 40.82% (80/196) | 31.50% (206/654) | 1,2,3,6 | |
| Lymphovascular invasion | 24.2% (445/1836) | 17.13% (154/899) | 26.44% (23/87) | 24.49% (48/196) | 33.64% (220/654) | 1,2,3,6 | |
| Peritumoral inflammation | 1.1% (20/1836) | 0.78% (7/899) | 0.00% (0/87) | 1.02% (2/196) | 1.68% (11/654) | NS | |
| Lymph nodes characteristics | |||||||
| Non axillary loco-regional lymph nodes | 1.5% (27/1836) | 1.67% (15/899) | 0.00% (0/87) | 1.53% (3/196) | 1.38% (9/654) | NS | |
| Isolated tumor cells | 1% (19/1836) | 1.00% (9/899) | 2.30% (2/87) | 2.04% (4/196) | 0.61% (4/654) | NS | |
| Micrometastases | 5.8% (106/1836) | 5.45% (49/899) | 11.49% (10/87) | 8.67% (17/196) | 4.59% (30/654) | 1,5,6 | |
| Extracapsular invasion of lymph node metastasis | 9.3% (170/1836) | 4.34% (39/899) | 5.75% (5/87) | 11.22% (22/196) | 15.90% (104/654) | 2,3,5 | |
| Bunched axillary lymph nodes | 1.8% (33/1836) | 0.33% (3/899) | 0.00% (0/87) | 1.53% (3/196) | 4.13% (27/654) | 2,3 | |
(*) Significant differences with a p-value
ER, Estrogen Receptor; PR, Progesteron Receptor; BCS, Breast-Conserving Surgery; NSM, Nipple-Sparing Mastectomy; SSM, Skin-Sparing Mastectomy; MTM, Modified Total Mastectomy.
| All (1836) | BCS (899) | NSM (87) | SSM (196) | MTM (654) | p(*) | ||
|---|---|---|---|---|---|---|---|
| Tumor size | |||||||
| T1 | 75.2% (1381/1836) | 89.99% (809/899) | 81.61% (71/87) | 73.47% (144/196) | 54.59% (357/654) | 1,2,3,5,6 | |
| T2 | 21.6% (396/1836) | 10.01% (90/899) | 17.24% (15/87) | 24.49% (48/196) | 37.16% (243/654) | 1,2,3,5,6 | |
| T3 | 2.3% (43/1836) | 0.00% (0/899) | 1.15% (1/87) | 2.04% (4/196) | 5.81% (38/654) | 1,2,3,6 | |
| T4 | 0.9% (16/1836) | 0.00% (0/899) | 0.00% (0/87) | 0.00% (0/196) | 2.45% (16/654) | 3,6 | |
| Nodal status | |||||||
| N0 | 66.2% (1215/1836) | 76.86% (691/899) | 65.52% (57/87) | 66.33% (130/196) | 51.53% (337/654) | 1,2,3,5,6 | |
| N1 | 23% (422/1836) | 18.24% (164/899) | 26.44% (23/87) | 20.92% (41/196) | 29.66% (194/654) | 3,6 | |
| N2 | 6.7% (123/1836) | 3.11% (28/899) | 5.75% (5/87) | 8.16% (16/196) | 11.31% (74/654) | 2,3 | |
| N3 | 4.1% (76/1836) | 1.78% (16/899) | 2.30% (2/87) | 4.59% (9/196) | 7.49% (49/654) | 2,3 | |
| pTNM stage | |||||||
| I | 54.4% (999/1836) | 69.19% (622/899) | 56.32% (49/87) | 51.53% (101/196) | 34.71% (227/654) | 1,2,3,5,6 | |
| II | 32.8% (603/1836) | 26.14% (235/899) | 34.48% (30/87) | 33.16% (65/196) | 41.74% (273/654) | 2,3,6 | |
| III | 12.7% (234/1836) | 4.67% (42/899) | 9.20% (8/87) | 15.31% (30/196) | 23.55% (154/654) | 2,3,5,6 | |
| Tumor grading | |||||||
| G 1 | 21% (386/1836) | 28.25% (254/899) | 22.99% (20/87) | 10.20% (20/196) | 14.07% (92/654) | 2,3,4,5 | |
| G 2 | 53.8% (988/1836) | 52.84% (475/899) | 50.57% (44/87) | 53.57% (105/196) | 55.66% (364/654) | NS | |
| G 3 | 25.2% (462/1836) | 18.91% (170/899) | 26.44% (23/87) | 36.22% (71/196) | 30.28% (198/654) | 2,3 | |
(*) Significant differences with a p-value
pTNM, pathological tumor stage; BCS, Breast-Conserving Surgery; NSM, Nipple-Sparing Mastectomy; SSM, Skin-Sparing Mastectomy; MTM, Modified Total Mastectomy.
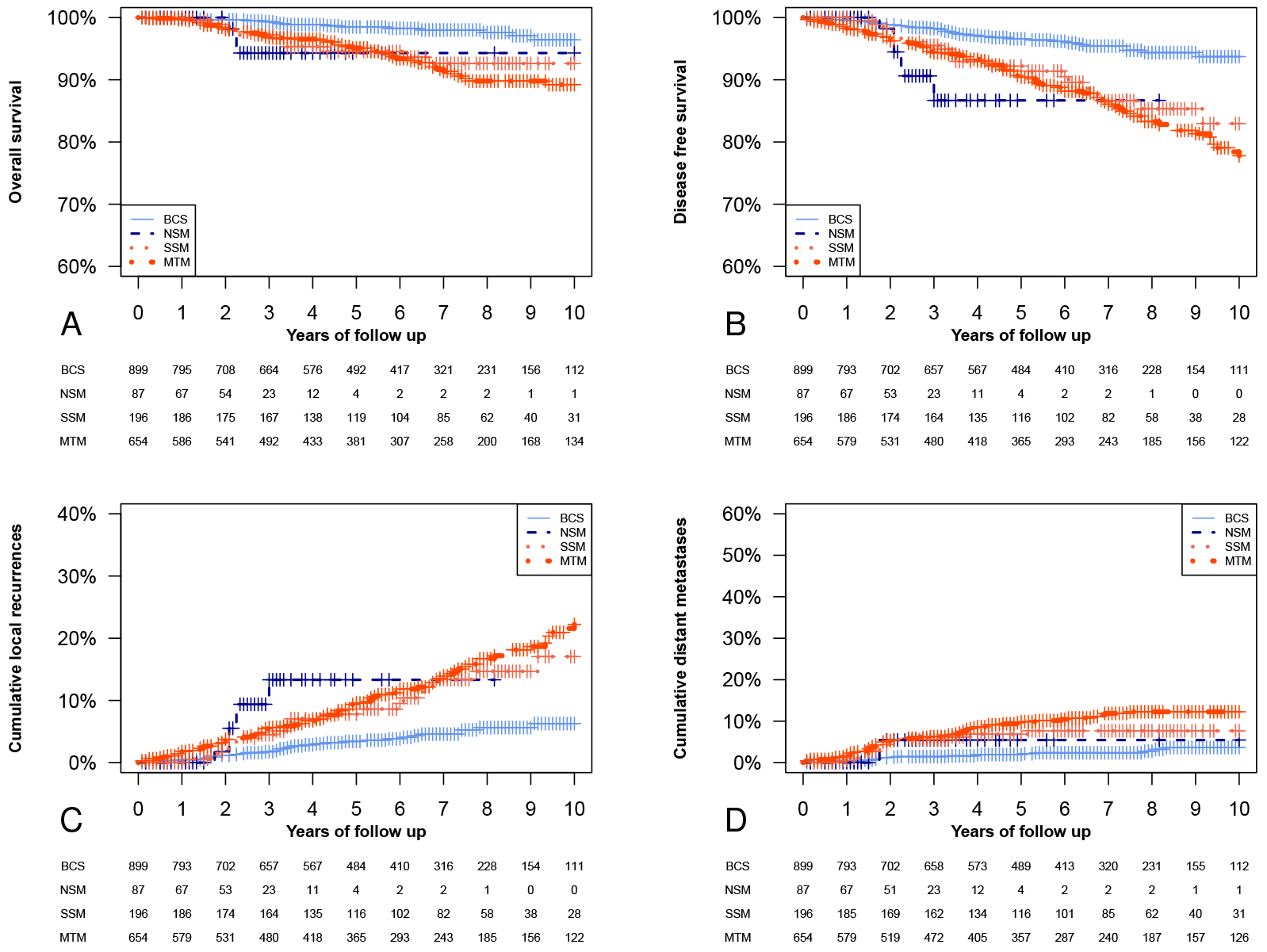
We analyzed in this population OS and DFS among the four groups of different
breast surgery types (Figs. 1,2). The 5-year OS was 98.5% (95% confidence
interval (CI), 97.6–99.4%) in the BCS group, 94.3% (95% CI, 88.2–100.0%) in
NSM, 94.6% (95% CI, 91.1–98.1%) in SSM, and 95.1% (95% CI, 93.2–97.0%) in
MTM. The 5-year DFS was 96.6% (95% CI, 95.2–98.0%) in BCS, 86.7 (95% CI,
76.7–98.0%) in NSM, 92.2% (95% CI, 88.2–96.4%) in SSM, and 90.4% (95% CI,
87.9–93.0%) in MTM. We found no significant differences in OS and DFS between
SSM and MTM. At the same time, we found a significantly shorter DFS in NSM than
MTM among TNM stage I cancers (p
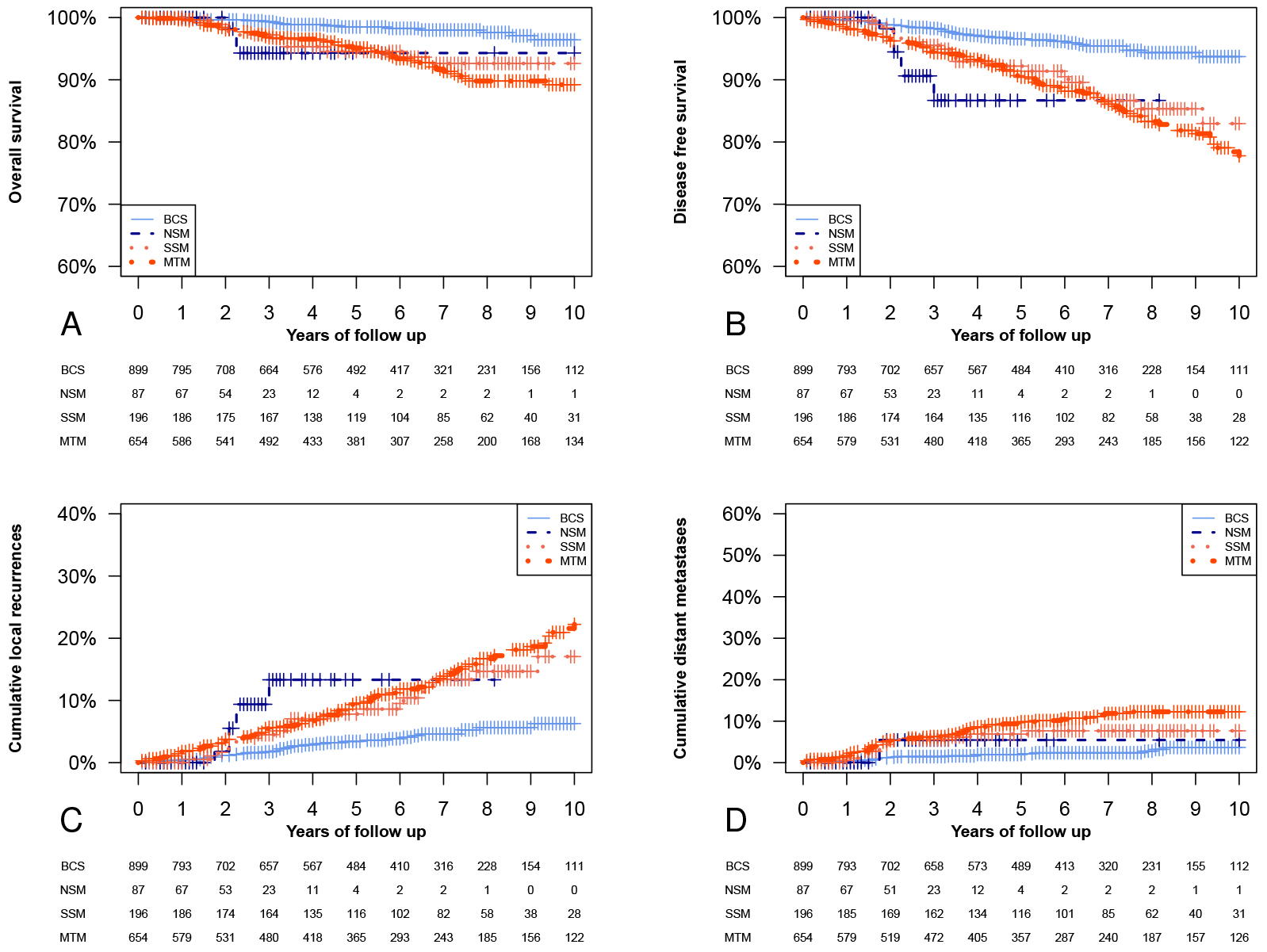 Fig. 1.
Fig. 1.Kaplan-Meier analysis of the entire population. Kaplan-Meier
curves and cumulative events curves of the whole considered population
(p-values in this figure refer to the Log-rank test). (A) Overall
survival (OS) analyses (BCS had a significantly longer OS than NSM, SSM, or MTM
p
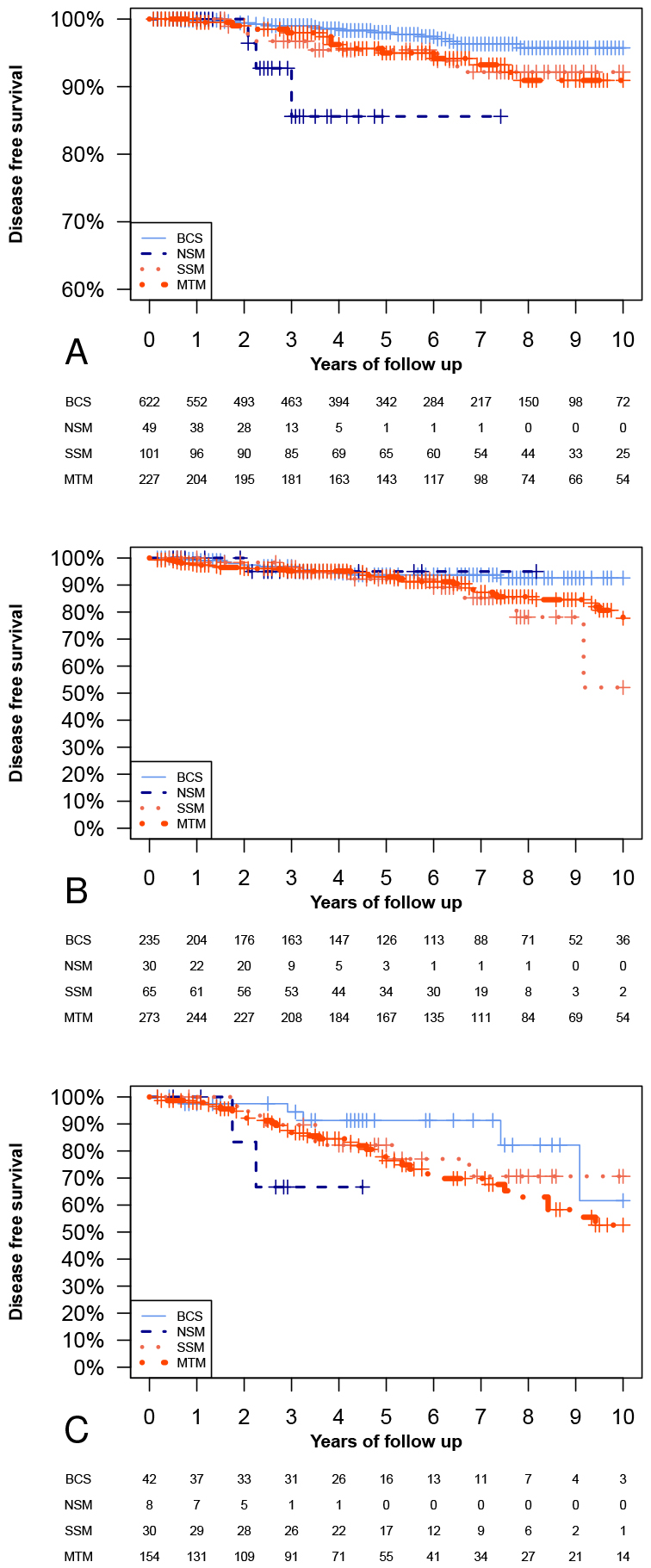
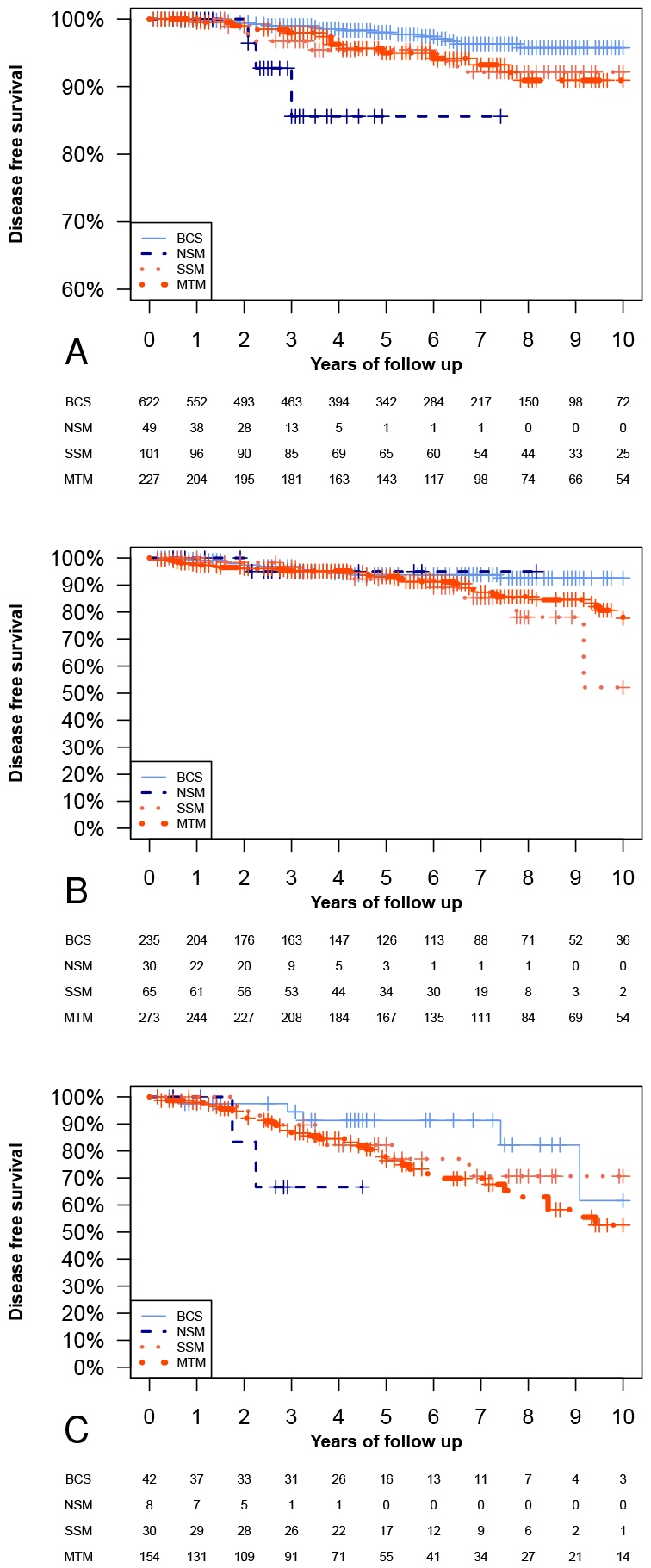 Fig. 2.
Fig. 2.Kaplan-Meier analysis according to TNM stage. Kaplan-Meier
curves of disease-free survival (DFS) analyses are subdivided by TNM stage
(p-values in this figure refer to Log-rank test). (A) DFS analyses in
TNM stage I. In this analysis, we found NSM to have a shorter DFS than MTM and
BCS (p
Table 4 also shows an analysis using univariate and multivariate Cox
proportional hazards regression models. In particular, in the multivariate
analyses, we adjusted for the following factors: menopausal status, type of
axilla surgery, neoadjuvant or adjuvant therapies, histological type, molecular
sub-type, comedo-like necrosis, perivascular invasion, peritumoral inflammation,
extra-capsular invasion of lymph node metastasis, bunched lymph nodes, TNM stage,
and grading. After adjusting the multivariate analysis for these factors, we
found BCS to influence DFS compared to MTM positively and NSM to have a
significantly shorter DFS than MTM (p
| HR (95% CI) | p | HR (95% CI) (*) | p | ||
|---|---|---|---|---|---|
| Overall survival | |||||
| Type of breast surgery | |||||
| Modified total mastectomy | Reference | 1 | Reference | 1 | |
| Skin sparing mastectomy | 0.82 (0.42–1.59) | 0.549 | 0.87 (0.42–1.8) | 0.705 | |
| Nipple sparing mastectomy | 1.49 (0.45–4.88) | 0.513 | 3.22 (0.88–11.76) | 0.077 | |
| Breast conservative surgery | 0.27 (0.15–0.5) | 0.65 (0.31–1.36) | 0.249 | ||
| Disease free survival | |||||
| Type of breast surgery | |||||
| Modified total mastectomy | Reference | 1 | Reference | 1 | |
| Skin sparing mastectomy | 0.82 (0.51–1.33) | 0.418 | 0.76 (0.45–1.28) | 0.303 | |
| Nipple sparing mastectomy | 1.86 (0.84–4.09) | 0.123 | 2.57 (1.09–6.07) | ||
| Breast conservative surgery | 0.3 (0.2–0.46) | 0.36 (0.21–0.63) | |||
| Local disease free survival | |||||
| Type of breast surgery | |||||
| Modified total mastectomy | Reference | 1 | Reference | 1 | |
| Skin sparing mastectomy | 0.81 (0.4–1.62) | 0.544 | 0.63 (0.29–1.35) | 0.233 | |
| Nipple sparing mastectomy | 1.89 (0.66–5.4) | 0.236 | 1.68 (0.53–5.34) | 0.379 | |
| Breast conservative surgery | 0.35 (0.2–0.62) | 0.16 (0.07–0.34) | |||
| Distant metastases disease free survival | |||||
| Type of breast surgery | |||||
| Modified total mastectomy | Reference | 1 | Reference | 1 | |
| Skin sparing mastectomy | 0.67 (0.37–1.23) | 0.197 | 0.75 (0.39–1.45) | 0.388 | |
| Nipple sparing mastectomy | 0.67 (0.21–2.15) | 0.500 | 1.58 (0.45–5.5) | 0.474 | |
| Breast conservative surgery | 0.24 (0.14–0.4) | 0.75 (0.38–1.5) | 0.420 | ||
(*) Multivariate analysis correction for menopausal status, type of axilla surgery, neoadjuvant therapy, adjuvant therapies, histological type, molecular type, comedo like necrosis, perivalscilar invasion, peritumoral inflammation, ExCp, blanching, TNM stage, and grading.
HR, hazard ratio; CI, confidence interval.
In particular, among the 87 cancers treated by NSM, we registered six local
breast recurrences and, in three of these cases, also distant metastases. Among
women experiencing any recurrence, we found a significantly lower BMI, higher
prevalence of basal-like sub-type, extra-capsular invasion of lymph node
metastasis, N2 status, and TNM stage III than the cases without recurrence. We
also performed a univariate and multivariate logistic regression model analysis
to define the most predictive factor for disease recurrence in women treated by
NSM. In the initial logistic regression multivariate model, we included all
factors showing in univariate analysis a p-value
In this study, we found NSM to have a significantly shorter DFS than MTM. Furthermore, low BMI, basal-like molecular sub-type, extended intraductal component, and extracapsular invasion of lymph node metastasis resulted in the most significant predictive factors for recurrence in women treated with NSM. We found no significant differences between SSM and MTM, while breast cancers treated by BCS had better OS and DFS than those who underwent a mastectomy.
The 5-year recurrence rate among women who underwent SSM and NSM in our population was respectively 7.8% and 13.3%. Despite the high variability in median follow-up lengths, in the literature recurrence rate of SSM and NSM range respectively from 0% to 14.3% [15, 25, 26, 27, 28, 29, 30, 31, 32, 33, 34, 35, 36] and from 0% to 10.3% [25, 32, 34, 35, 37, 38, 39].
Some risk factors for recurrence among women who underwent NSM, such as basal-like subtype or extended intraductal component, are recognized risk factors for an unfavorable prognosis independently by surgical strategy [40, 41, 42]. By sparing the skin and, in some selected cases, the NAC, the risk of leaving some occult residual neoplastic foci and the recurrence rate increases [17]. Although NSM should be offered to women without any ascertained skin or NAC tumoral involvement, it is impossible to completely exclude the likelihood of the misdiagnosed presence of tumoral cells on the residual skin or NAC. For example, Mallon and colleagues [43] described an overall rate of occult nipple malignancy of 11.5%. Moreover, they saw the following primary tumor characteristics impacting occult nipple malignancy: tumor-nipple distance less than 2 cm, grade, lymph node metastasis, lymphovascular invasion, Her2/Neu overexpression, hormonal receptors negativity, tumor size greater than 5 cm, retro-areolar/central location, and multicentric tumors [43]. Among these factors, our receiver operating characteristic (ROC) curve confirmed the strong predictivity only of hormonal receptors negativity, as in our population, basal-like tumors treated by NSM were significantly more likely to experience local recurrence. However, the other risk factors for occult nipple involvement include many factors recognized nowadays as generally predictive of an unfavorable prognosis. Huang and coworkers [17] recently also found an overall rate of occult nipple malignancy of 12.6%. They also discovered that nipple signs, tumor location, tumor size, tumor-nipple distance, lymph node metastasis, and HER2 over-expression were all predictive of occult nipple malignancy [17]. Furthermore, other authors observed an increased probability of retro-areola positive histology directly correlated with the tumor size but not related to the nodal status [44]. However, these factors did not significantly predict recurrences after NSM in our study population.
For what concerns BMI, although a high BMI is recognized to be a risk factor for surgical complications after SSM and NSM [45, 46], the literature lacks its eventual role in the oncological outcomes. A confounding factor may be that low BMI has a probable direct correlation with small-volume breasts, which are more likely to undergo NSM in case of an unfavorable rate between tumor size and breast volume.
In agreement with the literature, non-surgical treatments had no significant influence on OS or DFS in our population of women who underwent SSM and NSM. In particular, many studies demonstrated that SSM with immediate reconstruction could be offered to patients who have been down-staged with neoadjuvant chemotherapy [14]. Moreover, even the performance of SSM and NSM did not significantly influence non-surgical treatment success. In particular, some authors remarked that SSM with immediate reconstruction prolonged overall cancer treatment time but did not impair oncological outcomes [33, 47].
In summary, we could explain the higher recurrence rate among women undergoing NSM through a possible occult nipple neoplastic involvement by negative intraoperative histological examination of subareolar tissue, as well as an occult skin involvement. NSM has often been offered to women with the multicentric disease, who were probably more likely to have occult neoplastic foci involving the NAC or residual skin. In this perspective, more attention should be paid to those patients who present one or more risk factors for recurrence after NSM, including basal-like molecular sub-type, extended intraductal component, and extracapsular invasion of lymph node metastasis. These patients should be cautiously counseled about the possibility of undergoing NSM and be made aware of their possible recurrence risk by the presence of one or more of the risk factors observed in this study to plan a more frequent better follow-up and promptly recognize any possible recurrence.
AJCC/UICC, American Joint Committee on Cancer/International Union Against Cancer; BCS, Breast-Conserving Surgery; BMI, Body Mass Index; CALND, Complete Axillary Lymph Node Dissection; DFS, Disease-Free Survival; EIC, Extensive Intraductal Component; ER, Estrogen Receptor; ExCp, Extracapsular Invasion; IBR, Immediate Breast Reconstruction; IRB, Internal Review Board; MTM, Modified Total Mastectomy; NAC, Nipple-Areola Complex; NSM, Nipple-Sparing Mastectomy; OS, Overall Survival; PR, Progesteron Receptor; PTI, Peritumoral Inflammation; PVI, Peritumoral Vascular Invasion; ROLL, Radio-Guided Occult Lesion Localization; SLNB, Sentinel Lymph Node Biopsy; SSM, Skin-Sparing Mastectomy; TNM, Tumor-Node-Metastasis; WLBB, Wire-Localized Breast Biopsy.
The datasets used and/or analyzed during the current study are available from the corresponding author on reasonable request.
Substantial contributions to conception and design (SB, APL, LM, PCP, AR, CC). Significant contributions to data acquisition (SB, LS, FP, SM, VM, MA, MO) or analysis and interpretation of data (SB, APL, CC). Drafting or revising the article critically for important intellectual content (SB, APL, LS, FP, SM, VM, MA, MO, LM, PCP, AR, CC). All authors have read and approved the final manuscript.
The present study was approved by the internal review board of the Department of Medical Area (University of Udine, approval number: #34/14), it was conducted in accordance with Helsinki Declaration, and it followed the dictates of the general authorization to process personal data for scientific research purposes by the Italian Data Protection Authority. According to national legislation, the need for informed consent was waived by the IRB listed above because this was a retrospective cohort study.
We would like to thank the whole staff for collaborating in article collection, selection, reading, and in paper writing and reviewing.
This research received no external funding.
The authors declare no conflict of interest. Serena Bertozzi is serving as one of the Guest editors of this journal. Ambrogio Pietro Londero is serving as one of the Editorial Board members and Guest editors of this journal. We declare that Serena Bertozzi and Ambrogio Pietro Londero had no involvement in the peer review of this article and has no access to information regarding its peer review. Full responsibility for the editorial process for this article was delegated to Felix Wong.
References
Publisher’s Note: IMR Press stays neutral with regard to jurisdictional claims in published maps and institutional affiliations.