1 Department of Surgery, Lahey Clinic, Burlington, MA 01805, USA
2 Divison of Cardiothoracic Surgery, Department of Surgery, Johns Hopkins University School of Medicine, Baltimore, MD 21287, USA
3 Department of Cardiovascular Medicine, Brigham and Women’s Hospital Heart and Vascular Center, Harvard Medical School, Boston, MA 02115, USA
4 Division of Cardiology, Montefiore Medical Center, Albert Einstein College of Medicine, Bronx, NY 10467, USA
5 Division of Cardiovascular Medicine, Section of Heart Failure and Transplantation, University of Iowa, Iowa City, IA 52242, USA
Abstract
Postpartum cardiomyopathy is defined as an incident of acute heart failure in the postpartum period in the absence of any other cause. Up to 10% of postpartum cardiomyopathy may need to undergo heart transplantation later in life. This study aimed to provide a present-day perspective on all-cause mortality and transplant-related complications after heart transplantation for postpartum cardiomyopathy.
A retrospective analysis of the United Network for Organ Sharing (UNOS) registry was performed for adult patients undergoing heart transplants (01/2001–01/2023) for postpartum cardiomyopathy.
A total of 677 patients were identified, with a mean age of 35 years. The mean body mass index (BMI) was 27.2 kg/m2; the most common comorbidity was type 2 diabetes (T2D) (n = 589; 87%). Older age was associated with lower overall mortality (hazard ratio (HR): 0.97; 95% CI: 0.95, 0.98; p < 0.01), while diabetes (HR: 1.01; 95% CI: 1.01, 1.01; p < 0.01), dialysis (HR: 1.01; 95% CI: 1.01, 1.01; p < 0.01), days on Status 1 on the UNOS registry (HR: 1.06; 95% CI: 1.03, 10.9; p < 0.01), creatinine (HR: 1.29; 95% CI: 1.02, 1.64; p = 0.034), and length of stay (HR: 1.01; 95% CI: 1.01, 1.02; p = 0.02) were associated with a higher risk of overall mortality. Moreover, 30-day mortality was 2.8%, and 1-year mortality was 11.1%. The era effect was prominent in cases of 1-year mortality (odds ratio (OR): 0.95; 95% CI: 0.91, 0.99, p = 0.006).
Our results suggest that younger age, diabetes, pretransplant dialysis, days on Status 1, and creatinine are associated with higher mortality, while an era effect was observed for 1-year mortality after heart transplantation (HTx) in patients with postpartum cardiomyopathy.
Keywords
- UNOS
- heart transplantation
- postpartum cardiomyopathy
Postpartum cardiomyopathy is defined as an incident of acute heart failure (HF)
associated with systolic dysfunction (ejection fraction
This is a retrospective United Network for Organ Sharing (UNOS) registry
analysis. Deidentified patient-level variables for postpartum cardiomyopathy were
collected from all adult patients (
The primary outcomes of the study were 30-day and all-cause mortalities. Secondary outcomes included the need for pacemaker placement, dialysis, stroke, length of stay, and treatment for rejection within the first year after transplant.
All continuous variables are expressed as the mean
A total of 677 patients were identified. The average age was 35 years, and most
of the women were black (n = 345; 51%). The mean BMI was 27.2 kg/m2; the
most common comorbidity was type 2 diabetes (T2D) (n = 589; 87%). More than half
of the patients had an implantable cardiac defibrillator (ICD) (n = 371; 55%),
while approximately one out of ten patients had either a left ventricular assist
device (LVAD) (n = 72; 11%) or a total artificial heart (TAH) (n = 68; 11%).
Intra-aortic balloon pump (IABP) was used in 67 (10%) patients when wait-listed,
while this number increased to 95 (14%) at the time of transplantation. A total
of 135 patients (20%) had a previous cardiac surgery operation, and 95 (14%)
were intravenous drug users (IVDUs). Average creatinine, calculated panel
reactive antibody (CPRA), pulmonary capillary wedge pressure (PCWP), and mean
pulmonary arterial pressure (mPAP) were 1.08
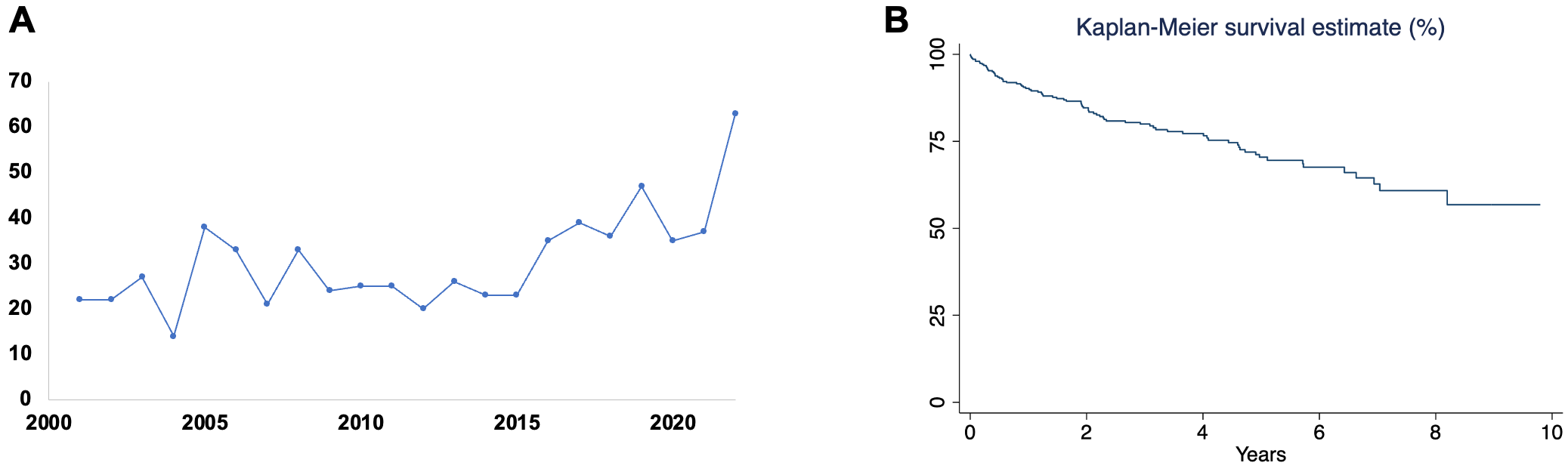 Fig. 1.
Fig. 1.
Incidence and survival outcomes of postpartum cardiomyopathy requiring heart transplantation. (A) The dot plot depicts the number of patients undergoing heart transplants for postpartum cardiomyopathy over time; (B) Kaplan–Meier curve shows the survival rate of patients undergoing heart transplants for postpartum cardiomyopathy over 10 years.
| Variable | n (%) or mean (SEM) | ||
| Recipient characteristics | |||
| Age, years | 34.9 | ||
| Race | |||
| White | 241 (36) | ||
| Black | 345 (51) | ||
| Other | 91 (13) | ||
| BMI, kg/m2 | 27.2 | ||
| T2D | 589 (87) | ||
| CVD | 32 (5) | ||
| Smoking | 155 (23) | ||
| Malignancy | 27 (4) | ||
| ICD | 371 (55) | ||
| Dialysis | 15 (2) | ||
| IVDU | 95 (14) | ||
| Days on Status 1 | 0.4 | ||
| Days on Status 2 | 2.4 | ||
| Days on Status 3 | 5.2 | ||
| Days on Status 4 | 19.4 | ||
| Days on Status 1A | 20.4 | ||
| Days on Status 1B | 60.3 | ||
| LVAD at listing | 72 (11) | ||
| RVAD at listing | 10 (2) | ||
| TAH at listing | 68 (11) | ||
| On ventilator at listing | 26 (4) | ||
| Inotropes at listing | 287 (42) | ||
| Prior cardiac surgery | 135 (20) | ||
| Creatinine, mg/dL | 1.08 | ||
| CPRA value | 29.2 | ||
| Cardiac output, L/min | 4.1 | ||
| PCWP, mmHg | 20.1 | ||
| mPAP, mmHg | 27.9 | ||
| IABP at listing | 67 (10) | ||
| IABP at Tx | 95 (14) | ||
| ECMO at listing | 13 (2) | ||
| ECMO at Tx | 20 (3) | ||
| Donor characteristics | |||
| Age, years | 30.5 | ||
| Race | |||
| White | 419 (62) | ||
| Black | 123 (18) | ||
| Other | 135 (20) | ||
| Female gender | 325 (48) | ||
| BMI | 26.2 | ||
| Creatinine, mg/dL | 1.45 | ||
| T2D | 20 (3) | ||
| LVEF, % | 61 | ||
| Ischemic time, hours | 3.3 | ||
| Distance (miles) | 222 | ||
SEM, standard error of the mean; BMI, body mass index; T2D, type 2 diabetes; CVD, cardiovascular disease; ICD, implantable cardiac defibrillator; IVDU, intravenous drug user; LVAD, left ventricular assist device; RVAD, right ventricular assist device; TAH, total artificial heart; CPRA, calculated panel reactive antibody; PCWP, pulmonary capillary wedge pressure; mPAP, mean pulmonary arterial pressure; IABP, intra-aortic balloon pump; Tx, transplant; ECMO, extracorporeal membrane oxygenator; LVEF, left ventricular injection fraction.
Regarding donor characteristics, the mean donor age was 30.5
Older age was associated with lower overall mortality (hazard ratio (HR): 0.97; 95% CI: 0.95,
0.98; p
The most common postoperative complication was renal failure requiring dialysis
(n = 59; 9%), followed by stroke (n = 17; 3%) and permanent pacemaker
implantation (n = 8; 1%). A total of 202 patients (30%) required treatment for
graft rejection within one year of the transplant. The mean length of hospital
stay was 19.9
No significant differences in mortality or secondary outcomes were observed when comparing the old with the new allocation systems.
When comparing females who underwent HTx for postpartum cardiomyopathy to all
the other females in the UNOS databases who underwent HTx for different reasons,
an increased association with postoperative mortality (HR: 1.42; 95% CI: 1.25,
1.61; p
This study offers a comprehensive insight into the outcomes of patients with postpartum cardiomyopathy after HTx based on nationwide data from the USA over the past two decades. The average age of the recipients was 35 years, and half were black, while nine out of ten had T2D. Younger age, diabetes, pretransplant dialysis, days on Status 1, and creatinine were associated with higher mortality, while an era effect was observed for 1-year mortality.
A population-based study from the late 90s utilizing the National Hospital
Discharge Survey showed that the incidence of postpartum cardiomyopathy is
approximately 0.03% and is associated with 1.4% and 2% inpatient and one-year
mortality, respectively [2]. A prospective multicenter study (Investigations of
Pregnancy Associated Cardiomyopathy; IPAC study) of 100 women with postpartum
cardiomyopathy showed that 3% had experienced major events or had persistent
severe cardiomyopathy (ejection fraction
We also observed an increased risk for mortality and rejection associated with postpartum cardiomyopathy as the etiology of heart failure requiring HTx, which agrees with a previous UNOS study [5]. The observed era effect can be attributed to better peripartum management of these patients and optimized general medical management of heart failure.
Interpretation and extrapolation of our study’s results should be performed cautiously, given certain limitations associated with its design. This is a retrospective cohort utilizing the UNOS database; thus, these data provide a snapshot of the reported evidence over the past two decades and do not include information derived from a prospective randomized study designed to address our primary and secondary objectives. Furthermore, these are nationwide derived data specific only to the USA population and may not apply to other populations.
In conclusion, our results show that younger age, diabetes, pretransplant dialysis, days on Status 1, and creatinine are associated with higher mortality, while an era effect was observed for 1-year mortality in patients with postpartum cardiomyopathy after HTx. Further studies are required to investigate the role of heart transplants in postpartum cardiomyopathy refractory to medical management.
The datasets used and/or analyzed during the current study are available from the corresponding author on reasonable request.
IPD, AT, AK, TK and AB have made substantial contributions to the conception, analysis, and interpretation of data. They have all contributed to the drafting and revision of the manuscript and they approved the final version. Moreover, they are in agreement to be accountable for all aspects of the work per International Committee of Medical Journal Editors (ICMJE) Guidelines.
Ethics approval was not necessary since this is a retrospective study of the UNOS database. Patient’s informed consent was not required.
Not applicable.
This research received no external funding.
The authors declare no conflict of interest. Alexandros Briasoulis is serving as Guest Editor of this journal. We declare that Alexandros Briasoulis had no involvement in the peer review of this article and has no access to information regarding its peer review. Full responsibility for the editorial process for this article was delegated to Michael Dandel.
References
Publisher’s Note: IMR Press stays neutral with regard to jurisdictional claims in published maps and institutional affiliations.

