1 Department of Cardiovascular Sciences, Katholieke Universiteit Leuven, 3000 Leuven, Belgium
2 Department of Cardiovascular Medicine, University Hospitals Leuven (UZLeuven), 3000 Leuven, Belgium
Abstract
Severe aortic valve stenosis is the most frequent valve pathology in the western
world and approximately 50% of these patients have concomitant coronary artery
disease (CAD). Revascularization of proximal obstructive CAD in patients
undergoing surgical aortic valve replacement (SAVR) is common practice considered
appropriate. However, the management of patients with CAD undergoing
transcatheter aortic valve implantation (TAVI) is more controversial.
Nevertheless, performing percutaneous coronary intervention (PCI) of significant
(
Keywords
- coronary artery disease
- aortic valve stenosis
- percutaneous coronary intervention
- transcatheter aortic valve implantation
Coronary artery disease (CAD) and aortic valve stenosis (AS) have common risk
factors and a shared pathogenesis, and therefore frequently co-exist in clinical
practice [1]. In patients receiving surgical aortic valve replacement (SAVR),
40–65% of patients undergo concomitant coronary artery bypass grafting (CABG)
and this percentage increases with age [2, 3]. In patients considered for
transcatheter aortic valve implantation (TAVI), approximately 50% have
obstructive CAD and half of these have multivessel disease with a reported mean
Syntax score (SS) of 14 [4, 5, 6]. Both CAD and AS can present with dyspnea and
angina, and their relative contribution to the complaints of the patient is often
unclear [7]. Finally, AS can cause myocardial ischemia on its own, further
complicating the assessment of CAD and the need for revascularization [8].
Significant CAD has been defined in the American guidelines as a minimal 70%
reduction in diameter in a major coronary artery (50% in the left main coronary
artery) and/or physiologically significance [9]. This guideline considers it is
reasonable to revascularize these significant lesions both in patients undergoing
SAVR (with concomitant CABG) or TAVI (with percutaneous coronary intervention
(PCI) before TAVI) irrespective of anginal complaints, although only with a level
C evidence. According to the latest European guidelines, in patients undergoing
SAVR, CABG of lesions
Current evidence suggests that patients with CAD and AS have worse clinical outcomes after AVR. A large systematic review showed that patients with CAD had a higher risk of early mortality after valve replacement [13]. Another retrospective analysis showed that omitting revascularization in these patients is an independent predictor for early mortality [14]. Moreover, Cox regression analysis identified CAD as a determinant of late mortality after hospital discharge.
In contrast with SAVR, observational studies assessing the association of CAD
and outcomes post-TAVI have provided heterogenic results. These studies show CAD
to have either no, a partial (only severe/complex lesions) or a systematic
negative prognostic effect on short term outcomes after TAVI. Even two large
meta-analyses on this topic revealed conflicting results [6, 15]. One showed that
the presence of CAD did not affect 30-day outcomes after TAVI, but demonstrated a
significant negative effect of CAD on survival one year after the procedure [15].
The other suggested that the presence of CAD did not impact on 30-day or one year
mortality after TAVI [6]. However, the presence of severe CAD (defined by a SS
There are multiple non-invasive methods for the assessment of the functional
severity of CAD, by investigating the perfusion of the heart during stress.
Stress testing is not routinely advised in current guidelines for valvular heart
disease [9, 10], mainly due to difficulties in interpreting the cause of
hypoperfusion if it is seen, due to severe changes in coronary hemodynamics in
AS, and due to some concerns about safety in this population. Nevertheless, a
number of smaller studies have shown promising results. Perfusion cardiac
magnetic resonance imaging (MRI) and positron emission tomographic (PET) have
shown to be safe in AS patients, however their ability to identify flow limiting
coronary lesions needs still to be validated [17, 18, 19]. Stress transthoracic
echocardiography (TTE) in AS patients showed good specificity and moderate
sensitivity to detect
From an anatomical perspective, cardiac computed angiography (CTA) has successfully been used as an alternative to invasive coronary angiography (CA) during the pre-TAVI work-up [27]. Supporting this approach are numerous studies showing a very high sensitivity (89–99%) and negative predictive value (90–96%) compared with CA in this setting for the detection of significant coronary stenosis [28, 29, 30, 31, 32, 33, 34]. The disadvantage is a relative low specificity (37–91%) and positive predictive value (59–87%), although a broad range in values has been reported. Overall, CTA has a similar sensitivity but a lower specificity in severe AS patients when compared to patients without AS, probably in part due to the higher burden of coronary calcium in AS [35, 36]. Combining coronary CTA analysis with valve sizing and assessment of vascular access during work-up might decrease the number of CA performed by up to 37%, and this percentage may further decrease as younger patients with a lower risk profile are being selected for TAVI [36]. Moreover, CTA may offer evaluation of the functional severity of lesions on top of anatomical information, with promising modalities such as CT-derived FFR. A study in AS patients showed that this tool was safe and feasible in this population, however with a moderate sensitivity (74%) and specificity (78%) and with a diagnostic accuracy of 77% compared to invasive FFR [37]. It is the view of the authors that CTA can be used during the pre-SAVR/TAVI workup in severe AS patients without angina, mainly to avoid unnecessary CA in relatively young low-risk patients with a low pre-probability of CAD. In patients with a very high coronary risk profile, history of CAD or active angina the performance of CA would remain standard practice.
Studies assessing CAD in patients with severe AS have used a luminal narrowing
of
Building further on QCA imaging, quantitative flow ratio (QFR) is a technique
integrating functional relevance of a coronary stenosis without the use of
Adenosine or a pressure wire. During angiography the flow of contrast is analyzed
and 3D QCA information is computed to estimate a pressure loss over a given
lesion. In a recent study in patients with AS, QFR had a better diagnostic
performance than angiography alone to assess FFR-based significance of a lesion
[47]. However, diagnostic accuracy decreased considerably when the aortic valve
area (AVA) was smaller than 0.80 cm
Alternatively, intravascular imaging using ultrasonography (IVUS) or optical
coherence tomography, while providing more detailed anatomical information, has a
limited role in the decision to revascularize in daily practice, and no studies
are available in the AS population. However, for the treatment of left main
coronary artery (LMCA) stenoses, a cut-off of
Finally, from a more global perspective, anatomical scoring systems can be used to further describe the extent and complexity of CAD in the individual patient. Studies in AS patients have used the Duke Myocardial Jeopardy score [53] or the synergy between percutaneous coronary intervention with taxus and cardiac surgery – score (SYNTAX-score, SS) [54]. Some studies showed that patients with a high baseline SS or high residual SS had worse outcomes after TAVI in comparison with patients with less complex disease [16, 44, 55], indicating that these scores can potentially be used for risk stratification in patients with AS.
Angiographic assessment of luminal narrowing is a poor predictor of coronary
hemodynamic physiological indices, such as coronary flow reserve (CFR), FFR, iFR
and resting flow ratio (RFR). The blood flow through a coronary artery and its
fractional decrease over a lesion are also dependent on other physiological and
anatomical factors besides luminal narrowing, such as the length of the lesion
and microvascular function [56]. There is data supporting the use of these
indices in stable CAD and the FAME-2 trial supports performing PCI in lesions
with FFR
Although patients who undergo combined AVR with CABG have higher unadjusted
mortality, this difference is no longer present after propensity matching [63, 64]. Two retrospective studies showed that patients with significant AS and CAD
undergoing SAVR with CABG had a significantly reduced early and late mortality
when compared with SAVR alone [14, 65]. Therefore concomitant revascularization
of coronary lesions
Treatment of stable CAD with PCI in non-AS patients is controversial, and should
potentially be viewed as mainly a symptomatic treatment, as several prospective
randomized studies have not showed a clear prognostic benefit [68, 69, 70]. This
becomes even more complex in the AS population, especially those who are elderly
and frail. Revascularization with PCI pre-TAVI of every proximal coronary lesion
with
| Study | Design | Population | Follow-up time | Outcome | Result |
|---|---|---|---|---|---|
| Wenaweser et al. 2011 [73] | Single-centre prospective registry | 197 TAVI | 2 years | All-cause Mortality | No difference (p = 0.96) |
| vs 59 TAVR + PCI | |||||
| Abdel-Wahab et al. 2012 [41] | Single-centre retrospective registry | 70 TAVI | 3 years | All-cause Mortality | No difference (p = 0.36) |
| vs 55 TAVI + PCI | |||||
| Codner et al. 2013 [74] | Single-centre prospective registry | 117 TAVI | 2 years | All-cause Mortality | No difference (p = 0.67) |
| vs 36 TAVI + PCI | |||||
| Abramowitz et al. 2014 [43] | Single-centre prospective registry | 105 TAVI (without CAD) | 3 years | All-cause Mortality | No difference (p = 0.68) |
| vs 83 TAVI (with CAD) | |||||
| vs 61 TAVI + PCI | |||||
| Khawaja et al. 2015 [44] | Single-centre retrospective registry | 68 TAVI (with CAD) | 1 year | All-cause Mortality | No difference (p = 0.918) |
| vs 25 TAVI + PCI | |||||
| Snow et al. 2015 [75] | Multicentre prospective registry | 2005 TAVI without historical PCI | 5 years | All-cause Mortality | No difference (p = 0.81) |
| vs 363 TAVI with historical PCI | |||||
| vs 169 TAVI + hybrid PCI | |||||
| vs 169 TAVI + PCI | |||||
| Huczek et al. 2016 [76] | Multicentre retrospective registry | 434 isolated TAVI (without CAD) | 30 days | All-cause Mortality | No difference (p = 0.098) |
| vs 293 isolated TAVI (with CAD) | |||||
| Chakravarty et al. 2016 [77] | Multicentre retrospective registry | 128 isolated TAVI | 1 year | All-cause Mortality | No difference (HR: 1.09; 95% CI: 0.50–2.39; p = 0.83) |
| vs 128 TAVR + LM PCI | |||||
| (1:1 case-control matched) | |||||
| Millan-Iturbe et al. 2017 [78] | Single-centre prospective registry | 720 isolated TAVI (without CAD) | 9 years | All-cause Mortality | No difference (p = 0.229) |
| vs 88 TAVI (with CAD) | |||||
| vs 136 TAVI + PCI | |||||
| Minten et al. 2022 [16] | Single-centre prospective study | 239 isolated TAVI | 5 years | All-cause Mortality | No difference (p = 0.162) |
| vs 107 TAVI + PCI |
CAD, coronary artery disease; 95% CI, 95% confidence interval; CR, complete revascularization; HR, hazard ratio; IR, incomplete revascularization; LM, left mainstem coronary artery; MACCE, major adverse cardiac and cerebrovascular events; PCI, Percutaneous coronary intervention; rSS, residual Syntax score; SS, Syntax-score; TAVI, Transcutaneous aortic valve implantation.
In patients with stable CAD and ischemia without significant valvular disease, the ISCHEMIA trial confers limited to no influence on early invasive revascularization strategy on outcomes [70]. Nevertheless, AS patients with a very high burden or very complex CAD (represented by a high SS-score) may have better outcomes when revascularized. Data to support this comes from observational studies that analyzed completeness of revascularization. Several studies have shown a correlation between incomplete revascularization (high residual SS) and worse clinical outcomes such as increased mortality or major adverse cardiac or cerebrovascular events (MACCE) supporting PCI in the peri-TAVI period [83, 84, 85, 86, 87, 88]. However, other studies could not find an association between incomplete revascularization and clinical events [38, 89, 90, 91, 92, 93]. Recently, two important papers regarding this topic were published. One prospective study with 5-year follow-up showed there was no benefit of (complete) revascularization for stable CAD in TAVI patients [16]. A large retrospective registry among TAVI patients with significant stable CAD showed no benefit of complete myocardial revascularization to reduce the risk of all cause death at 2 years [94]. Limitations in combining the results of these studies lie in differences in the definition of incomplete revascularization, follow-up times and comorbidities, and overall small patients numbers in the cohorts studied (Table 2, Ref. [16, 38, 83, 84, 85, 86, 87, 88, 89, 90, 91, 92, 93, 94]).
| Study | Design | Population | Follow-up time | Outcome | Result |
|---|---|---|---|---|---|
| Ussia et al. 2013 [89] | Multicentre prospective registry | 92 TAVI + no PCI | 1 year | All-cause mortality | No difference (p = 0.807) |
| 88 TAVI + IR | MACCE | No difference (p = 0.594) | |||
| 95 TAVI + CR | |||||
| Van Mieghem et al. 2013 [38] | Single-centre prospective study | 124 TAVI + IR | 1 year | All-cause mortality | No difference (p = 0.85) |
| 139 TAVI + CR | |||||
| Stefanini et al. 2014 [83] | Single-centre prospective registry | TAVI + PCI both groups: | 1 year | MACCE | High residual SS = higher risk (RR: 1.92; 95% CI: 1.02–3.61; p = 0.042) |
| - 192 low residual SS (0–14) | |||||
| - 95 high residual SS ( |
|||||
| Kleczynski et al. 2016 [84] | Single-centre prospective registry | 16 TAVI + IR | 1 year | All-cause mortality | IR = higher mortality (HR: 10.86; 95% CI: 3.72–31.73; p |
| 85 TAVI + CR | |||||
| Paradis et al. 2017 [90] | Multicentre retrospective registry | TAVI all groups: | 1 year | MACCE | No difference (p = 0.16) |
| - 82 No CAD | |||||
| - 17 low residual SS (0–7) | |||||
| - 37 high rSS ( |
|||||
| Shamekhi et al. 2017 [85] | Single-centre prospective study | TAVI all groups: | 3 years | All-cause mortality | Univariate analysis: higher residual SS = increased mortality (p = 0.01) |
| - 229 no CAD | Multivariate analysis: no significant effect of rSS | ||||
| - 140 low residual SS (0–3) | |||||
| - 205 high residual SS ( |
|||||
| Witberg et al. 2017 [86] | Multicentre retrospective registry | TAVI all groups: | 5 years | All-cause mortality | High rSS = higher mortality (HR: 1.72; 95% CI: 1.051–2.814; p = 0.031) |
| - 817 no CAD | |||||
| - 331 low residual SS (0–8) | |||||
| - 122 high residual SS ( |
|||||
| Li et al. 2019 [91] | Single-centre retrospective registry | TAVI + PCI in all groups: | 3 years | All-cause mortality | No difference (p = 0.40) |
| - 144 CR | MACCE | No difference (p = 0.18) | |||
| - 151 major IR | |||||
| - 29 minor IR | |||||
| López Otero et al. 2019 [92] | Single-centre retrospective registry | TAVI + PCI in all groups: | 3 years | All-cause mortality | No difference (p = 0.605) |
| - 56 CR (rSS = 0) | MACCE | No difference (p = 0.866) | |||
| - 85 RCR (rSS = 1–7) | |||||
| - 46 IR (rSS |
|||||
| Saia et al. 2019 [93] | Single-centre retrospective registry | TAVI + PCI in both groups: | 5 years | Cardiovascular mortality | No difference (p = 0.25) |
| - 138 CR | |||||
| - 153 IR | |||||
| Landt et al. 2019 [87] | Single-centre retrospective registry | TAVI + PCI in both groups: | 1 year | All-cause mortality | CR = lower mortality (HR: 0.450; 95% CI: 0.218–0.926, p = 0.030) |
| - 129 CR (rSS = 0) | |||||
| - 78 IR (rSS |
|||||
| Faroux et al. 2020 [88], | Multicentre retrospective registry | TAVI + PCI in both groups: | 2 years | MACCE | CR = lower MACCE (HR: 0.77; 95% CI: 0.63–0.95, p = 0.014) |
| - 889 CR | |||||
| - 308 IR | |||||
| Minten et al. 2022 [16] | Single centre prospective study | TAVI + PCI in all groups: | 5 years | All-cause mortality | No difference (p = 0.678) |
| - 66 RCR (rSS = 1–7) | Cardiovascular mortality | No difference (p = 0.361) | |||
| - 41 IR (rSS |
|||||
| Costa et al. 2022 [94] | Multi-centre retrospective registry | Stable CAD in TAVI: | 2 years | Cardiovascular death | No difference (p = 0.63) |
| - 657 CR | MACCE | No difference (p = 0.94) | |||
| - 287 IR | |||||
| - 370 no revascularisation |
CAD, coronary artery disease; 95% CI, 95% confidence interval; CR, complete revascularization; HR, hazard ratio; IR, incomplete revascularization; LM, left mainstem coronary artery; MACCE, major adverse cardiac and cerebrovascular events; PCI, Percutaneous coronary intervention; rSS, residual Syntax score; SS, Syntax-score; TAVI, Transcutaneous aortic valve implantation.
To date, only one randomized clinical trial comparing TAVI with medical therapy
vs TAVI with PCI in patients with severe AS and CAD has been performed [95]. CAD
was defined as stenosis severity of
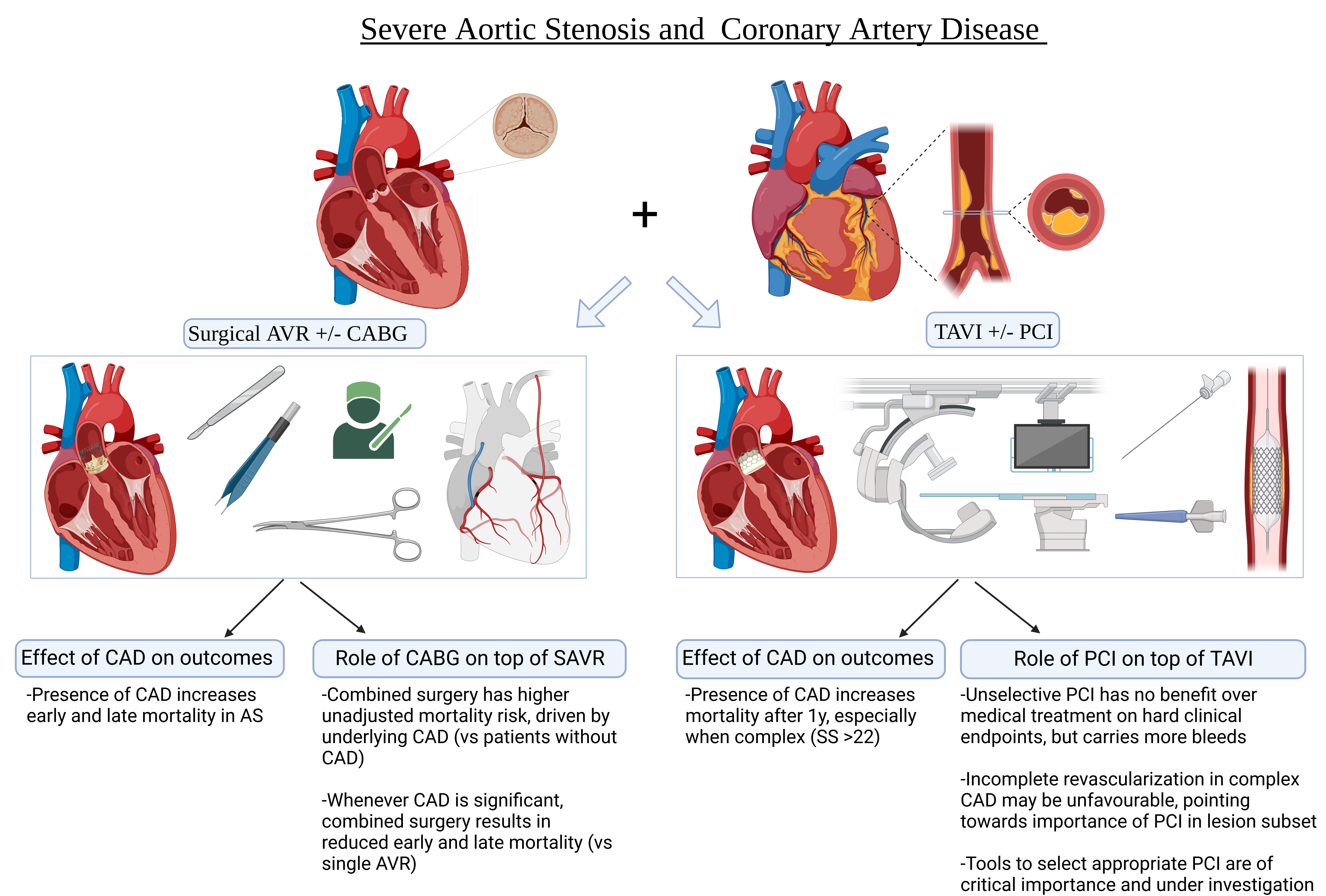 Fig. 1.
Fig. 1.Central Figure with overview.
Ideally, additional tools are needed to select patients benefiting most from PCI at the time of TAVI. Unfortunately, the invasive assessment of coronary hemodynamics by using indices such as FFR, iFR, and RFR cannot simply be extrapolated from patients with stand-alone stable CAD to a population with AS [48]. Severe AS induces dramatic changes in coronary physiology that are still incompletely understood. Moreover, it is unclear which index to use since it is expected that severe AS and valve replacement impact differently on these indices [96]. When looking at outcomes, one observational study compared patients who underwent angiography versus physiology-guided PCI before TAVR [61]. In this study, patients in whom the decision was based on physiological assessment had better survival free from MACCE at two years follow-up (HR: 0.40; 95% CI: 0.20–1.00, p = 0.035). More studies to investigate the role of coronary physiological in AS are currently underway [62].
In case of acute cardiac symptoms (such as chest pain and dyspnea), raised troponin levels and ECG changes, the difficult differential between an acute coronary syndrome and acute decompensated AS should lead to the predominate cause of decompensation being treated first [97]. However, most decisions in this population are made in an elective setting.
For patients going to SAVR, CABG should be performed during the same procedure for obvious reasons. In contrast, patients receiving TAVI can undergo revascularization before, during or after valve implantation, and several considerations can be made in this respect.
Performing PCI before TAVI has the theoretical disadvantage of inflicting multiple hospital admissions and invasive cardiovascular procedures to the patient with repeated risk for contrast induced kidney injury, while increasing dual antiplatelet-related bleeding risk following TAVI. The benefits of this strategy include the potential reduction of ischemia during TAVI, in case of severe lesions with high-risk features or left main stem disease, especially when rapid pacing is required [98]. Moreover, the PCI-first strategy will maintain optimal coronary access, allowing optimal guide catheter support for more complex revascularization. It remains unclear, however, how long the time interval between PCI and TAVI should be. One study showed that there was no significant difference in mortality at 2 year follow-up between PCI within one month or more than one month prior to TAVI [99]. Nevertheless, the group with the PCI closer to the valve procedure had significantly more bleeding and minor vascular complications, suggesting a potential benefit of leaving enough time between both procedures.
Performing PCI and TAVI in one procedure is feasible and limits the number of hospital admissions and invasive cardiovascular procedures [100, 101]. However, the higher volume of contrast medium administered in these combined interventions carries an increased risk for acute kidney injury, especially when considering complex CAD interventions in frail patients. Furthermore, the results of a large registry suggest that patients undergoing PCI during the same admission as TAVI had a higher rate of complications and mortality [102].
There is general agreement that overall, in patients with severe AS and CAD, the severity of the valve disorder is driving the symptoms and risk, and PCI should only be considered for severe proximal lesions in vessels supplying a large myocardial territory [9]. Deferring PCI until after TAVI, to observe how symptoms (and coronary indices such as FFR and RFR) evolve, seems like a valid strategy, especially in equivocal lesions [103]. This is supported by previously mentioned studies showing no short-term outcome benefit of PCI. Moreover, although patients with complex (CAD) had worse outcomes in a recent study, this difference only started to appear after a few years [16]. TAVI operators should however take into account the impact of the valve procedure on future coronary access as in some cases access may become technically challenging depending on the anatomy of the aortic root and the valve type used [104]. While it has been reported that PCI after TAVI has a high success rate for all available transcatheter valves [105, 106], modifications in PCI and TAVI technique are sometimes necessary [107, 108]. In this respect, the use of the Evolut R/PRO valve, the interaction of the valve with the sinus of Valsalva and the mean valve implantation depth have been identified as independent predictors for difficult coronary access post-TAVI [109].
The challenge remains to identify which patients and coronary lesions may benefit from myocardial revascularization at the time of AVR in the setting of severe AS. While non-invasive functional imaging, such as CT-based FFR looks promising, its potential role, even in a context without AS, needs to be finetuned. However, invasive assessment of coronary physiology by means of FFR and non-hyperemic pressure ratios (NHPRs) has become standard practice in cathlabs, and decision algorithms for revascularization should now be validated or adapted in the context of AS. Currently, several smaller or larger scale studies are recruiting patients in this field, focusing on either mechanistic understanding of physiologic variables impacted by AS, or rather pure clinical outcomes (Table 3, Ref. [62, 110, 111, 112, 113, 114, 115]). Ultimately, randomized controlled trials, will be needed to answer remaining questions. As a matter of fact, the COMPLETE TAVR trial (NCT04634240) is comparing medical therapy versus complete revascularization in patients undergoing TAVI. The TAVI-PCI (NCT04310046) study is trying to determine the ideal timing for physiology-guided revascularization relative to the TAVI. Further studies regarding gender differences in regard to CAD in patients undergoing TAVI will also be important [116].
| Study | Design | Population | Recruitment target | Description | Primary outcome | Completion date |
|---|---|---|---|---|---|---|
| FORTUNA [110] (NCT03665389) | Single centre, prospective open-label study | TAVI patients with moderate- severe CAD | 25 | CT-based FFR, FFR and iFR pre-TAVR and FFR and iFR post-TAVR | Comparison between CT based FFR and iFR/FFR | 2023 |
| FAVOR IV-QVAS [111] (NCT03977129) | Multicentre, randomized control trial | AS patients undergoing valve surgery + moderate to severe CAD | 792 | Angiography guides vs QFR guided revascularization | Composite endpoint: all-cause mortality, MI, stroke, unplanned revascularization, kidney injury requiring dialysis at 30 days | 2026 |
| COMIC-AS [62] (NCT04420325) | Multicentre, prospective cohort study | AS patients undergoing TAVI or SAVR + moderate to severe CAD | 100 | FFR, RFR, CFR and IMR with SPECT myocardial perfusion imaging pre-(T)AVR and FFR, RFR, CFR and IMR immediately and 6 months after TAVI | Change in FFR and RFR, correlation between indices and non-invasive imaging at 6 months | 2024 |
| TCW [112] (NCT03424941) | Multicentre, open-label, non-inferiority randomized controlled trial | AS patients undergoing SAVR/TAVI with multivessel CAD | 328 | CABG + SAVR vs FFR-guided PCI +TAVI | Composite endpoint: mortality, MI, disabling stroke, major bleeding, valve re-intervention or need for target lesion revascularization at 1 year | 2024 |
| FAITAVI [113] (NCT03360591) | Single centre, open-label, randomized controlled trial | AS patients undergoing TAVI with moderate to severe CAD | 320 | Angiography guided versus physiology guided PCI | Composite endpoint: all-cause mortality, MI, stroke, major bleeding and target lesions revascularization at 1 year | 2024 |
| NOTION-3 [114] (NCT03058627) | Multicentre, open-label, randomized controlled trial | AS patients undergoing TAVI, with one significant coronary lesion (FFR |
452 | TAVI + FFR-guided complete revascularization vs TAVI + medical management of CAD | Composite endpoint: all cause death, myocardial infarction, or urgent revascularization at 1 year | 2027 |
| TAVI-PCI [115] (NCT04310046) | Open-label, randomized controlled trial | AS patients undergoing TAVI and PCI for CAD | 986 | iFR-guided revascularization: performed 1–45 days before versus 1–45 days after TAVI | Composite endpoint: All-cause mortality, MI; ischemia driven revascularization, rehospitalization, major bleeding at 1 year | 2028 |
CABG, Coronary Artery Bypass Grafting; CAD, coronary artery disease; CFR, coronary flow reserve; CT, computed tomography; FFR, fractional flow reserve; iFR, instantaneous wave-free ratio; IMR, index of microvascular resistance; MI, myocardial infarction; QFR, Quantitative flow ratio; RFR, resting full-cycle ratio; SAVR, surgical aortic valve replacement; SPECT, Single photon-emission computed tomography; TAVI, transcutaneous aortic valve implantation.
Patients with CAD and severe AS represent a frequently-encountered clinical entity in daily practice. It appears that (complex) CAD independently negatively influences the outcomes after AVR and so deserves particular attention. Although important, the ideal methods to assess and treat CAD in this population remain unclear. Some data suggest complete revascularization might benefit these patients but many studies fail to show a beneficial effect of angiography-guided PCI in this population. Severe AS induces severe coronary hemodynamic changes that make the physiological assessment of lesions severity challenging. Nevertheless, this field is advancing rapidly and several large clinical trials are actively recruiting and will significantly improve our understanding of CAD in the setting of severe AS.
LM, JB, KM and CD participated in conceptualization and methodology of the review article. LM performed the data gathering, analysis and wrote the first draft. CD, JB, KM reviewed and edited the first draft. LM Finalized the final draft and made the figures and tables. CD and JB supervised the review article. All authors contributed to editorial changes in the manuscript. All authors read and approved the final manuscript.
Not applicable.
Not applicable.
L. Minten is supported by the Research Foundation Flanders Grant 1194521 N and Belgian Fund For Heart surgery Grant 489686.
The authors declare no conflict of interest.
References
Publisher’s Note: IMR Press stays neutral with regard to jurisdictional claims in published maps and institutional affiliations.

