1 Cardiology Department, Beijing AnZhen Hospital: Capital Medical University Affiliated Anzhen Hospital, 100089 Beijing, China
Academic Editor: Brian Tomlinson
Abstract
Background: As an alternative method to evaluate insulin resistance
(IR), triglyceride-glucose index (TyG) was shown to be related to the severity
and prognosis of cardiovascular diseases. The main aim of this
study was to explore the association between TyG and in-hospital mortality in
critically ill patients with heart disease. Method: The calculation
method of TyG has been confirmed in previous report: Ln [fasting TGs (mg/dL)
Keywords
- insulin resistance
- TyG index
- critically ill
- heart disease
- in-hospital mortality
In contemporary society, cardiovascular disease (CVD) is still the leading cause of morbidity and mortality worldwide. Especially, in patients with severe CVD, the mortality was greatly increased [1, 2]. In order to reduce the mortality of serious CVD patients, coronary artery care unit (CCU) and cardiac intensive care unit (CICU) came into being. After decades of development, CCU and CICU eventually focused on the management of patients with severe CVD which needed meticulous care and targeted treatment [3, 4]. Nowadays, the status of CCU and CICU are increasingly important and a variety of studies were performed to explore how to predict and improve prognosis of patients. As for clinicians, easily accessible and reliable prognostic indicators for critically ill patients with heart disease are always welcomed, especially, in patients with severe CVD, the mortality was greatly increased.
Type 2 diabetes mellitus (T2DM) has been widely proven to be one of the most significant risk factors for CVD [5]. The key mechanism of T2DM is insulin resistance (IR), which has been shown to be closely associated with the development of CVD and atherosclerosis [6, 7, 8, 9]. However, as the gold standard test for IR, the hyperinsulinaemic-euglycaemic clamp is time-consuming, expensive and complex [10], the triglyceride-glucose index (TyG index) is an alternative method, which evaluates IR by using the levels of glycemia (mg/dL) and fasting triglycerides (TG) (mg/dL) [11]. Studies have indicated that TyG index was associated positively with T2DM risk [12, 13, 14, 15]. Notably, previous studies have manifested that TyG index was related to the increased risk of worse outcomes in patients with CVD. Zhao et al. [16] recently demonstrated that TyG index had a prognostic role in patients with T2DM and non‑ST‑segment elevation acute coronary syndrome (NSTE-ACS) undergoing percutaneous coronary intervention (PCI). In addition, high TyG index was also proved to be associated with increased incidence of CVD events in healthy Caucasian and China participants [17, 18, 19]. Nevertheless, to the best of our knowledge, no research has demonstrated the effect of TyG index in patients with severe CVD. Thus, our main objective in this study was to investigate the relationship between TyG index and in-hospital mortality of critically ill patients with heart disease.
The research objects were selected from CCU and CICU patients in eICU
Collaborative Research Database [20]. Adult patients (
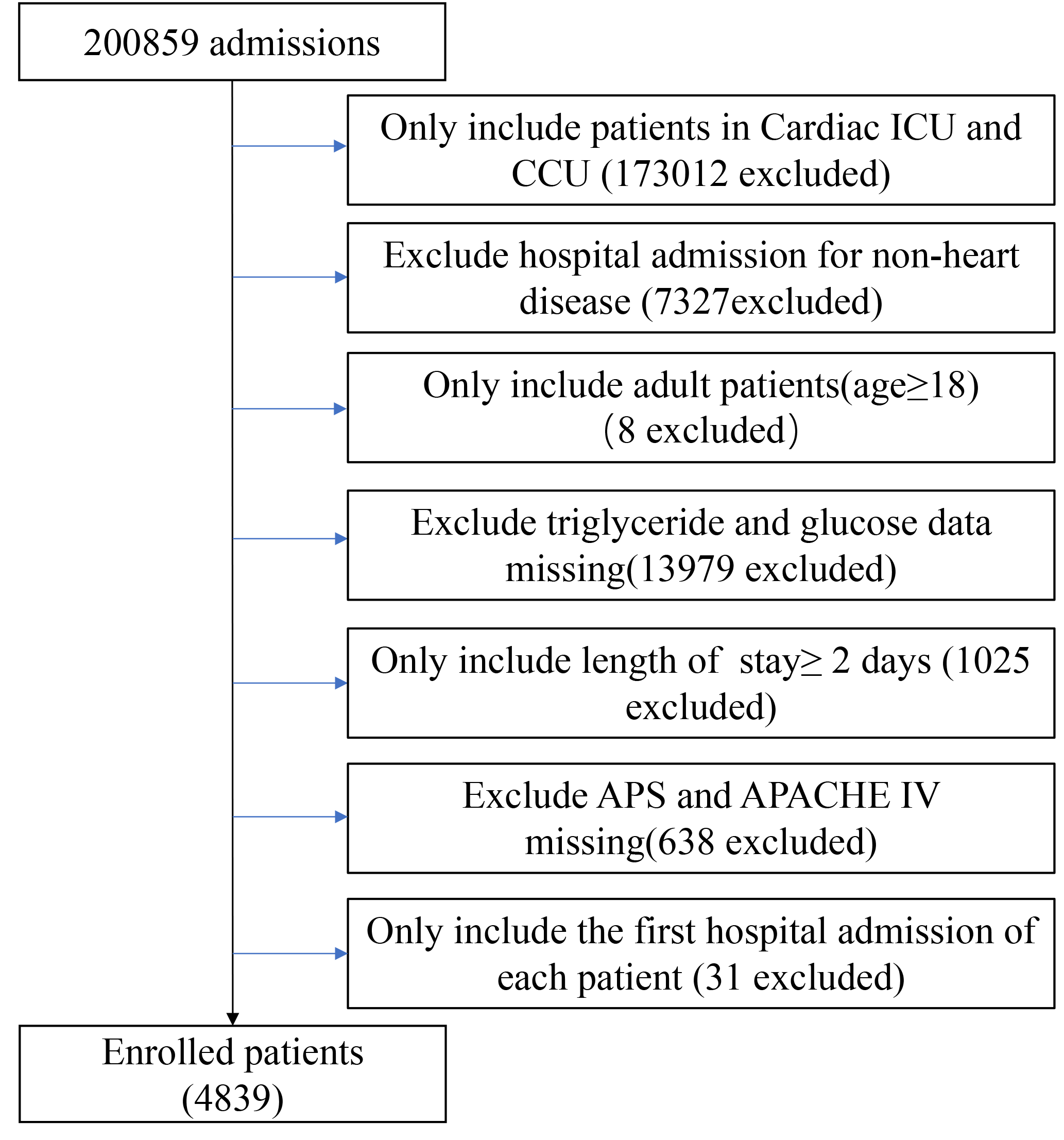
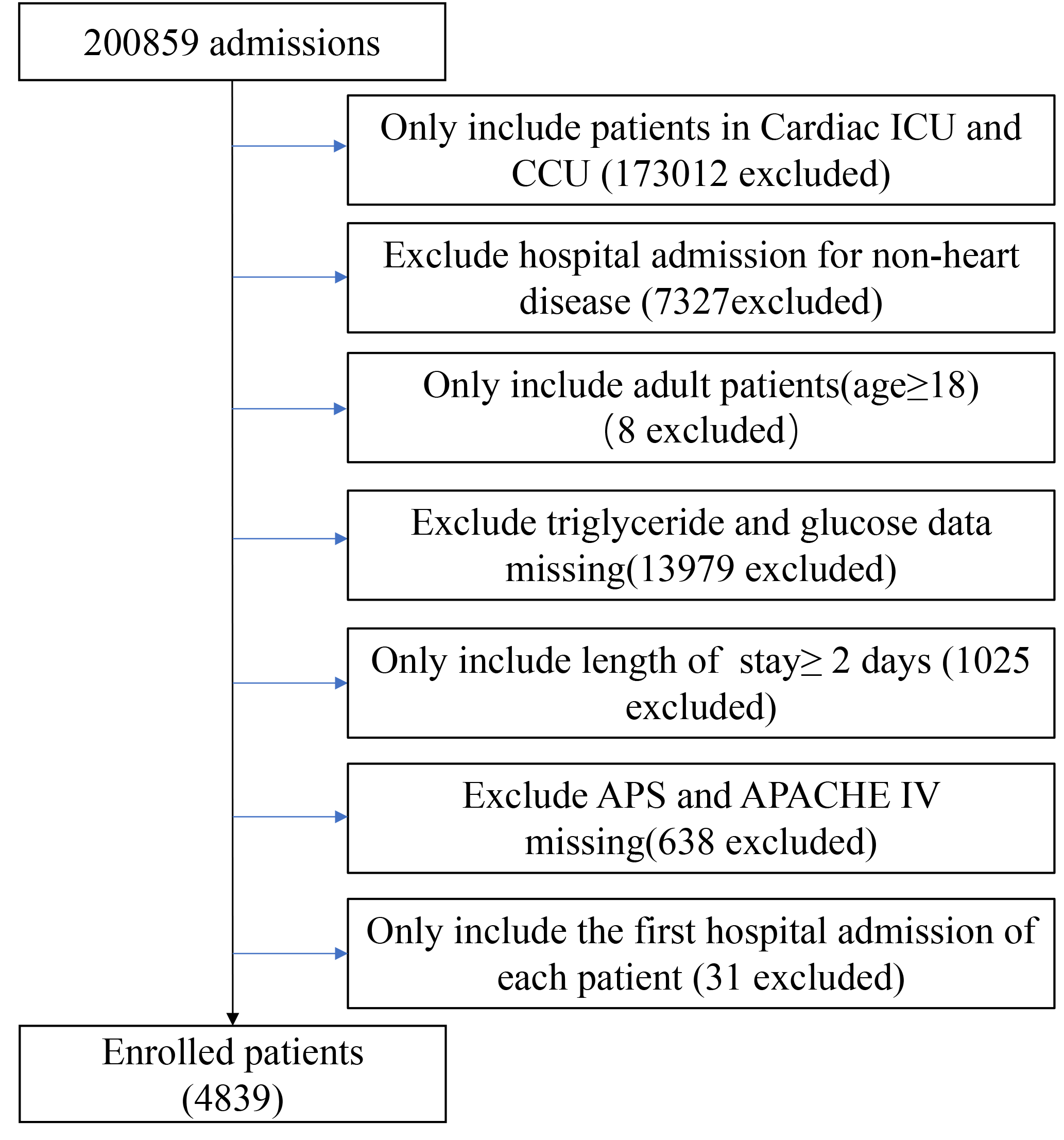 Fig. 1.
Fig. 1.Flow chart of study population. Abbreviation: CCU, coronary artery care unit; CICU, cardiac intensive care unit.
The original data for this study was from eICU Collaborative Research Database (https://doi.org/10.13026/C2WM1R) [20]. We passed the Protecting Human Research Participants exam to get access to the database (certificate number: 9728458).
Following data were collected: demographics, vital signs, body mass index, diagnoses and comorbidities, laboratory parameters, medication use, acute physiology score (APS) and Acute Physiology and Chronic Health Evaluation IV (APACHE IV) [21]. All data were extracted using Structured Query Language. Details was available in the Supplementary Material named “Data extraction”.
TyG index was obtained by the formula Ln [fasting triglycerides (mg/dL)
Depending on the TyG quartiles, all enrolled patients were divided into four different categories. The primary outcome was in-hospital mortality. Secondary outcomes were length of intensive care unit (ICU) stay and length of hospital stay.
Normally distributed continuous variables were expressed as mean
Binary logistic regression analysis was used to identify the independent
relationship between TyG and in-hospital mortality and the results were expressed
as odds ratio (OR) and 95% confidence interval (CI). P for trend was calculated.
Covariates were selected by statistical analysis and clinical doubt to modulate
the outcome. Local weighted regression (Lowess) was used to plot the curve in
line with overall trend, which described the probability of mortality predictded
by TyG in raw calculations without adjustment for other covariates.
Receiver-operating characteristic (ROC) curve was applied to evaluate the
sensitivity and specificity of TyG. DeLong test was applied to compare the area
under the curve (AUC) of different parameters. Subgroup analysis was used to
determine the correlation between TyG and in-hospital mortality in different
subgroups, P for interaction was calculated. A two-tailed p value
4839 patients were analyzed (Fig. 1). According to TyG quartiles, all patients
were divided into four groups: TyG
| Characteristics | Total (n = 4839) | Quartiles of TyG | p value | ||||
| Quartile 1 | Quartile 2 | Quartile 3 | Quartile 4 | ||||
| (n = 1201) | (n = 1221) | (n = 1214) | (n = 1203) | ||||
| TyG |
8.51 |
8.92 |
TyG | ||||
| Age (years) | 65.2 |
67.8 |
67.0 |
64.5 |
61.5 |
||
| Gender, n (%) | 0.626 | ||||||
| Male | 2993 (61.9) | 756 (63.0) | 743 (60.9) | 741 (61.0) | 753 (62.6) | ||
| Female | 1846 (38.1) | 445 (37.0) | 478 (39.1) | 473 (39.0) | 450 (37.4) | ||
| Ethnicity, n (%) | 0.001 | ||||||
| Caucasian | 3668 (75.8) | 887 (73.9) | 929 (76.1) | 934 (76.9) | 918 (76.3) | ||
| African American | 663 (13.7) | 198 (16.5) | 176 (14.4) | 155 (12.8) | 134 (11.1) | ||
| Other | 508 (10.5) | 116 (9.7) | 116 (9.5) | 125 (10.3) | 151 (12.6) | ||
| Vital signs | |||||||
| Systolic blood pressure (mmHg) | 122.3 |
120.7 |
121.6 |
122.7 |
124.5 |
||
| Diastolic blood pressure (mmHg) | 66.5 |
65.8 |
66.4 |
66.8 |
67.2 |
0.011 | |
| Mean blood pressure (mmHg) | 82.4 |
81.2 |
82.0 |
82.7 |
83.5 |
||
| Heart rate (beats/min) | 85.0 |
83.0 |
85.0 |
85.3 |
86.9 |
||
| Respiration rate (beats/min) | 20.0 |
20.0 |
20.1 |
19.9 |
20.1 |
0.694 | |
| Oxygen saturation (%) | 98 (95, 100) | 98 (95, 99) | 98 (95, 100) | 98 (95, 100) | 98 (95, 99) | 0.535 | |
| Body mass index (kg/m |
29.5 |
27.3 |
28.9 |
30.0 |
31.8 |
||
| Diagnoses and comorbidities, n (%) | |||||||
| Congestive heart failure | 793 (16.4) | 242 (20.2) | 210 (17.2) | 180 (14.8) | 161 (13.4) | ||
| Coronary artery disease | 3043 (62.9) | 691 (57.5) | 776 (63.6) | 802 (66.1) | 774 (64.3) | ||
| Acute coronary syndrome | 2295 (47.4) | 511 (42.6) | 608 (49.8) | 601 (49.5) | 575 (47.8) | 0.001 | |
| STEMI | 1035 (21.4) | 223 (18.6) | 267 (21.9) | 275 (22.7) | 270 (22.4) | 0.050 | |
| NSTEMI | 563 (11.6) | 122 (10.2) | 168 (13.8) | 131 (10.8) | 142 (11.8) | 0.032 | |
| Arrhythmias | 1234 (25.5) | 358 (29.8) | 354 (29.0) | 280 (23.1) | 242 (20.1) | ||
| Cardiac arrest | 430 (8.9) | 75 (6.2) | 98 (8.0) | 126 (10.4) | 131 (10.9) | ||
| Bradycardia | 178 (3.7) | 59 (4.9) | 47 (3.9) | 38 (3.1) | 34 (2.8) | 0.033 | |
| Atrial fibrillation | 675 (14.0) | 194 (16.2) | 199 (16.3) | 154 (12.7) | 128 (10.6) | ||
| Ventricular arrhythmias | 344 (7.1) | 87 (7.2) | 99 (8.1) | 82 (6.8) | 76 (6.3) | 0.355 | |
| Atrioventricular block | 127 (2.6) | 35 (2.9) | 36 (3.0) | 30 (2.5) | 26 (2.2) | 0.569 | |
| Cardiomyopathy | 297 (6.1) | 85 (7.1) | 103 (8.4) | 54 (4.5) | 55 (4.6) | ||
| Valve disease | 182 (3.8) | 53 (4.4) | 54 (4.4) | 48 (4.0) | 27 (2.2) | 0.014 | |
| Shock | 975 (20.2) | 220 (18.3) | 225 (18.4) | 251 (20.7) | 279 (23.2) | 0.008 | |
| Pulmonary embolism | 58 (1.2) | 15 (1.3) | 16 (1.3) | 14 (1.2) | 13 (1.1) | 0.957 | |
| Pulmonary hypertension | 49 (1.0) | 18 (1.5) | 13 (1.1) | 11 (0.9) | 7 (0.6) | 0.156 | |
| Hypertension | 1133 (23.4) | 291 (24.2) | 284 (23.3) | 264 (21.8) | 294 (24.4) | 0.384 | |
| Diabetes | 770 (15.9) | 97 (8.1) | 162 (13.3) | 197 (16.2) | 314 (26.1) | ||
| Hypercholesterolemia | 452 (9.3) | 94 (7.8) | 117 (9.6) | 110 (9.1) | 131 (10.9) | 0.077 | |
| COPD | 352 (7.3) | 105 (8.7) | 98 (8.3) | 75 (6.2) | 74 (6.2) | 0.026 | |
| Respiratory failure | 1038 (21.5) | 202 (16.8) | 248 (20.3) | 287 (23.6) | 301 (25.0) | ||
| Chronic kidney disease | 546 (11.3) | 149 (12.4) | 106 (8.7) | 144 (11.9) | 147 (12.2) | 0.011 | |
| Acute kidney injury | 659 (13.6) | 128 (10.7) | 128 (10.5) | 184 (15.2) | 219 (18.2) | ||
| Malignancy | 121 (2.5) | 22 (1.8) | 35 (2.9) | 38 (3.1) | 26 (2.2) | 0.144 | |
| Stroke | 233 (4.8) | 65 (5.4) | 62 (5.1) | 49 (4.0) | 57 (4.7) | 0.433 | |
| Sepsis | 519 (10.7) | 105 (8.7) | 103 (8.4) | 140 (11.5) | 171 (14.2) | ||
| Laboratory parameters | |||||||
| White blood cell (10 |
11.3 |
10.3 |
11.1 |
11.9 |
12.1 |
||
| Lymphocyte percentage (%) | 17.8 |
17.1 |
17.6 |
17.5 |
18.8 |
||
| Monocyte percentage (%) | 7.6 |
8.0 |
7.7 |
7.4 |
7.3 |
||
| Neutrophil percentage (%) | 71.9 |
72.4 |
72.1 |
72.3 |
70.9 |
0.003 | |
| Red blood cell (10 |
4.3 |
4.2 |
4.2 |
4.3 |
4.4 |
||
| Platelet (10 |
227 |
219 |
227 |
231 |
233 |
||
| Hemoglobin (g/dL) | 12.8 |
12.6 |
12.6 |
12.8 |
13.2 |
||
| Hematocrit (%) | 38.5 |
38.0 |
38.0 |
38.5 |
39.4 |
||
| Glucose (mg/dL) | 139.6 |
116.6 |
129.8 |
142.1 |
170.1 |
||
| Triglyceride (mg/dL) | 140.6 |
65.3 |
98.9 |
136.9 |
261.7 |
||
| Creatinine (mg/dL) | 1.44 |
1.34 |
1.38 |
1.49 |
1.54 |
||
| Blood nitrogen urea (mg/dL) | 24.6 |
23.3 |
24.5 |
24.4 |
25.9 |
0.002 | |
| Sodium (mmol/L) | 137.3 |
137.3 |
137.5 |
137.6 |
136.9 |
||
| Potassium (mmol/L) | 4.2 |
4.1 |
4.1 |
4.2 |
4.2 |
||
| TyG | 8.91 |
8.26 |
8.73 |
9.12 |
9.73 |
||
| Medication use, n (%) | |||||||
| Antiplatelet | 2611 (54.0) | 629 (52.4) | 662 (54.2) | 661 (54.5) | 659 (54.8) | 0.639 | |
| Oral anticoagulants | 375 (7.8) | 107 (8.9) | 96 (7.9) | 94 (7.7) | 78 (6.5) | 0.173 | |
| Beta-blockers | 1877 (38.8) | 430 (35.8) | 476 (39.0) | 481 (39.6) | 490 (40.7) | 0.079 | |
| ACEI/ARB | 1054 (21.8) | 270 (22.5) | 266 (21.8) | 247 (20.4) | 271 (22.5) | 0.531 | |
| Statin | 1680 (34.7) | 386 (32.1) | 443 (36.3) | 421 (34.7) | 430 (35.7) | 0.145 | |
| APS | 35 (25, 50) | 33 (24, 46) | 35 (25, 48) | 36 (25, 53) | 38 (26, 56) | ||
| APACHE IV | 49 (36, 64) | 48 (36, 61) | 49 (36, 64) | 49 (35, 67) | 49 (35, 68) | 0.146 | |
| Continuous variables were presented as mean | |||||||
Overall, in-hospital mortality rate was 8.5%. As TyG quartiles increased,
in-hospital mortality increased significantly (Quartile 4 vs Quartile 1: 12.1 vs
5.3, p
| Outcomes | Total (n = 4839) | Quartiles of TyG | p value | |||
| Quartile 1 | Quartile 2 | Quartile 3 | Quartile 4 | |||
| (n = 1201) | (n = 1221) | (n = 1214) | (n = 1203) | |||
| TyG |
8.51 |
8.92 |
TyG | |||
| In-hospital mortality, n (%) | 413 (8.5) | 64 (5.3) | 87 (7.1) | 117 (9.6) | 145 (12.1) | |
| Length of ICU stay (days) | 2.2 (1.3 4.3) | 2.1 (1.3, 3.8) | 2.2 (1.3, 4.2) | 2.4 (1.3, 4.7) | 2.3 (1.3, 4.9) | 0.007 |
| Length of hospital stay (days) | 5.9 (3.3, 11.1) | 5.7 (3.2, 9.8) | 6.0 (3.5, 11.5) | 6.2 (3.3, 11.7) | 5.9 (3.1, 11.5) | 0.100 |
| Continuous variables were presented as median (IQR). Categorical variables were presented as number (percentage). p values were calculated using Kruskal–Wallis test or Chi-square test to compare differences in outcomes between different TyG quartiles. Abbreviation: TyG, triglyceride-glucose index; ICU, intensive care unit. | ||||||
| OR (95% CI) | p value | P for trend | ||
| Model 1 | ||||
| Quartile 1: TyG |
Reference | |||
| Quartile 2: 8.51 |
1.36 (0.98, 1.90) | 0.068 | ||
| Quartile 3: 8.92 |
1.89 (1.38, 2.60) | |||
| Quartile 4: TyG |
2.43 (1.79, 3.31) | |||
| Continuous | 1.35 (1.23, 1.48) | |||
| Model 2 | ||||
| Quartile 1: TyG |
Reference | |||
| Quartile 2: 8.51 |
1.40 (1.00, 1.95) | 0.051 | ||
| Quartile 3: 8.92 |
2.07 (1.50, 2.85) | |||
| Quartile 4: TyG |
2.90 (2.12, 3.96) | |||
| Continuous | 1.43 (1.30, 1.58) | |||
| Model 3 | ||||
| Quartile 1: TyG |
Reference | |||
| Quartile 2: 8.51 |
1.15 (0.80, 1.68) | 0.448 | ||
| Quartile 3: 8.92 |
1.47 (1.03, 2.11) | 0.035 | ||
| Quartile 4: TyG |
1.83 (1.27, 2.64) | 0.001 | ||
| Continuous | 1.23 (1.10, 1.38) | |||
| Models were derived from binary logistic regression analysis. P for trend was calculated using binary logistic analysis to determine whether there was a trend when TyG was included as a grouping variable in the model (Quartile 1–4). When TyG was included as a grouping variable in the model, p values were calculated using binary logistic analysis to determine whether there was a relationship between TyG quartiles and in-hospital mortality with Quartile1 serving as the reference group. When TyG was included as a continuous variable in the model, p values were calculated using binary logistic analysis to determine whether there was a relationship between TyG and in-hospital mortality. Model 1: unadjusted. Model 2: adjusted for age, gender, ethnicity. Model 3: adjusted for age, gender, ethnicity, systolic blood pressure, diastolic blood pressure, respiration, congestive heart failure, STEMI, cardiac arrest, acute kidney injury, respiratory failure, stroke, malignancy, white blood cell, neutrophil percentage, oral anticoagulants, ACEI/ARB, APACHE IV, length of ICU stay and length of hospital stay. Abbreviation: TyG, triglyceride-glucose index; STEMI, ST-elevation myocardial infarction; ACEI, angiotensin-converting enzyme inhibitor; ARB, angiotensin receptor blocker; APACHE IV, Acute Physiology and Chronic Health Evaluation IV; ICU, intensive care unit; OR, odds ratio; CI, confidence interval. | ||||
| DM | OR (95% CI) | p value | P for trend | No-DM | OR (95% CI) | p value | P for trend | ||
| Model 1 | 0.291 | Model 1 | |||||||
| Quartile 1: TyG |
Reference | Quartile 1: TyG |
Reference | ||||||
| Quartile 2: 8.51 |
1.14 (0.46, 2.79) | 0.782 | Quartile 2: 8.51 |
1.37 (0.95, 1.96) | 0.090 | ||||
| Quartile 3: 8.92 |
1.33 (0.57, 3.12) | 0.515 | Quartile 3: 8.92 |
1.95 (1.39, 2.74) | |||||
| Quartile 4: TyG |
1.44 (0.65, 3.21) | 0.373 | Quartile 4: TyG |
2.62 (1.87, 3.66) | |||||
| Continuous | 1.13 (0.90, 1.41) | 0.297 | Continuous | 1.38 (1.25, 1.53) | |||||
| Model 2 | 0.009 | Model 2 | |||||||
| Quartile 1: TyG |
Reference | Quartile 1: TyG |
Reference | ||||||
| Quartile 2: 8.51 |
1.14 (0.46, 2.81) | 0.781 | Quartile 2: 8.51 |
1.41 (0.98, 2.02) | 0.062 | ||||
| Quartile 3: 8.92 |
1.37 (0.58, 3.24) | 0.477 | Quartile 3: 8.92 |
2.15 (1.52, 3.03) | |||||
| Quartile 4: TyG |
1.58 (0.69, 3.60) | 0.280 | Quartile 4: TyG |
3.16 (2.24, 4.46) | |||||
| Continuous | 1.17 (0.92, 1.48) | 0.196 | Continuous | 1.48 (1.33, 1.64) | |||||
| Model 3 | Model 3 | ||||||||
| Quartile 1: TyG |
Reference | Quartile 1: TyG |
Reference | ||||||
| Quartile 2: 8.51 |
1.38 (0.47, 4.04) | 0.554 | Quartile 2: 8.51 |
1.25 (0.83, 1.89) | 0.283 | ||||
| Quartile 3: 8.92 |
1.79 (0.63, 5.04) | 0.273 | Quartile 3: 8.92 |
1.57 (1.05, 2.36) | 0.028 | ||||
| Quartile 4: TyG |
2.37 (0.87, 6.46) | 0.091 | Quartile 4: TyG |
2.08 (1.38, 3.16) | 0.001 | ||||
| Continuous | 1.32 (0.99, 1.77) | 0.057 | Continuous | 1.28 (1.12, 1.46) | |||||
| Models were derived from binary logistic regression analysis. P for trend was calculated using binary logistic analysis to determine whether there was a trend when TyG was included as a grouping variable in the model (Quartile 1–4). When TyG was included as a grouping variable in the model, p values were calculated using binary logistic analysis to determine whether there was a relationship between TyG quartiles and in-hospital mortality with Quartile1 serving as the reference group. When TyG was included as a continuous variable in the model, p values were calculated using binary logistic analysis to determine whether there was a relationship between TyG and in-hospital mortality. In DM group: Model 1: unadjusted. Model 2: adjusted for age, gender, ethnicity. Model 3: adjusted for age, gender, ethnicity, systolic blood pressure, respiratory failure, stroke, pulmonary embolism, hemoglobin, hematocrit, APACHE IV. In No-DM group: Model 1: unadjusted. Model 2: adjusted for age, gender, ethnicity. Model 3: adjusted for age, gender, ethnicity, systolic blood pressure, diastolic blood pressure, congestive heart failure, STEMI, cardiac arrest, malignancy, respiratory failure, shock, stroke, acute kidney injury, white blood cell, neutrophil percentage, sodium, oral anticoagulants, ACEI/ARB, APS, APACHE IV, length of ICU stay and length of hospital stay. Abbreviation: TyG, triglyceride-glucose index; DM, diabetes; STEMI, ST-elevation myocardial infarction; ACEI, angiotensin-converting enzyme inhibitor; ARB, angiotensin receptor blocker; APS, acute physiology score; APACHE IV, Acute Physiology and Chronic Health Evaluation IV; ICU, intensive care unit; OR, odds ratio; CI, confidence interval. | |||||||||
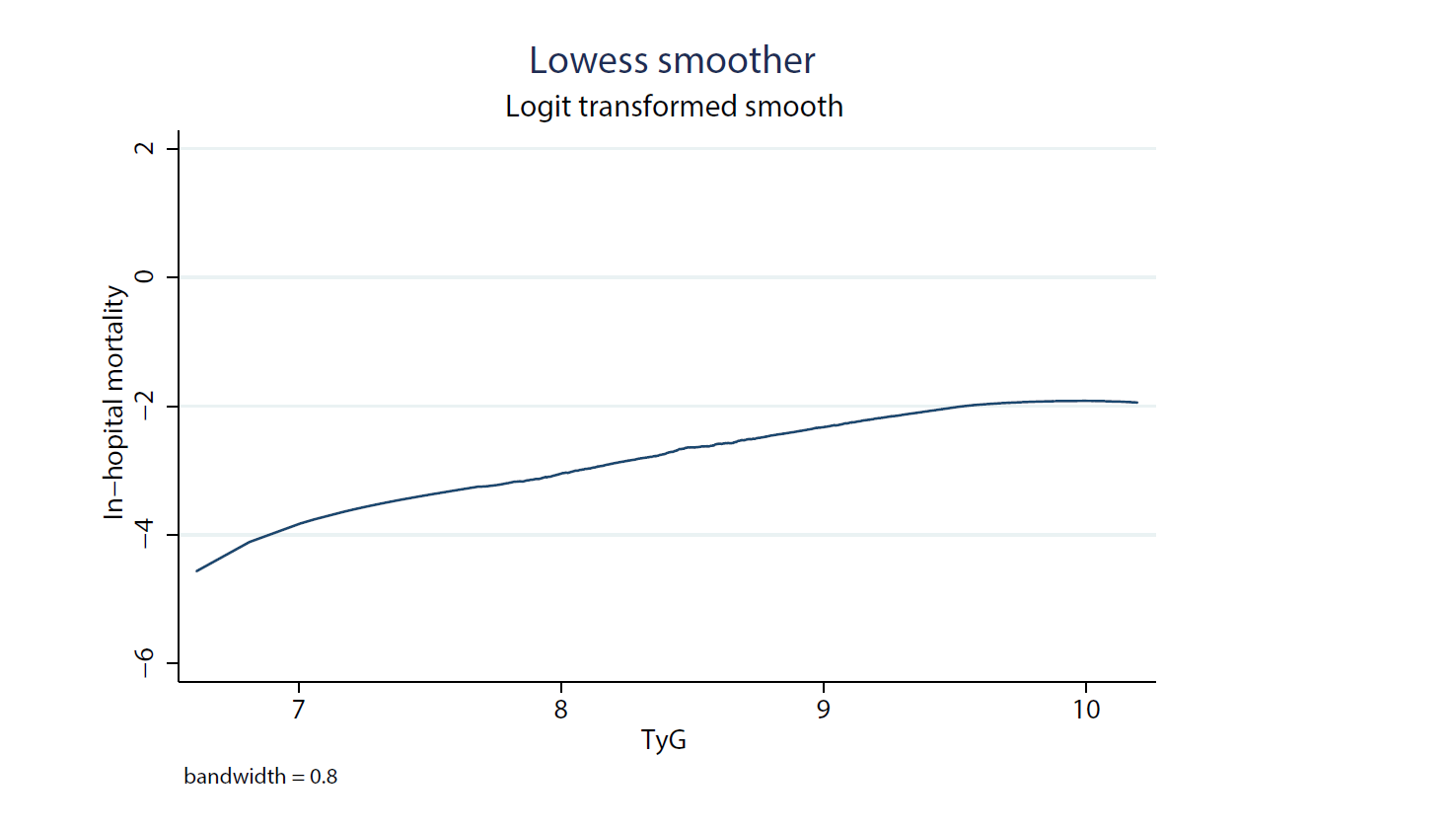
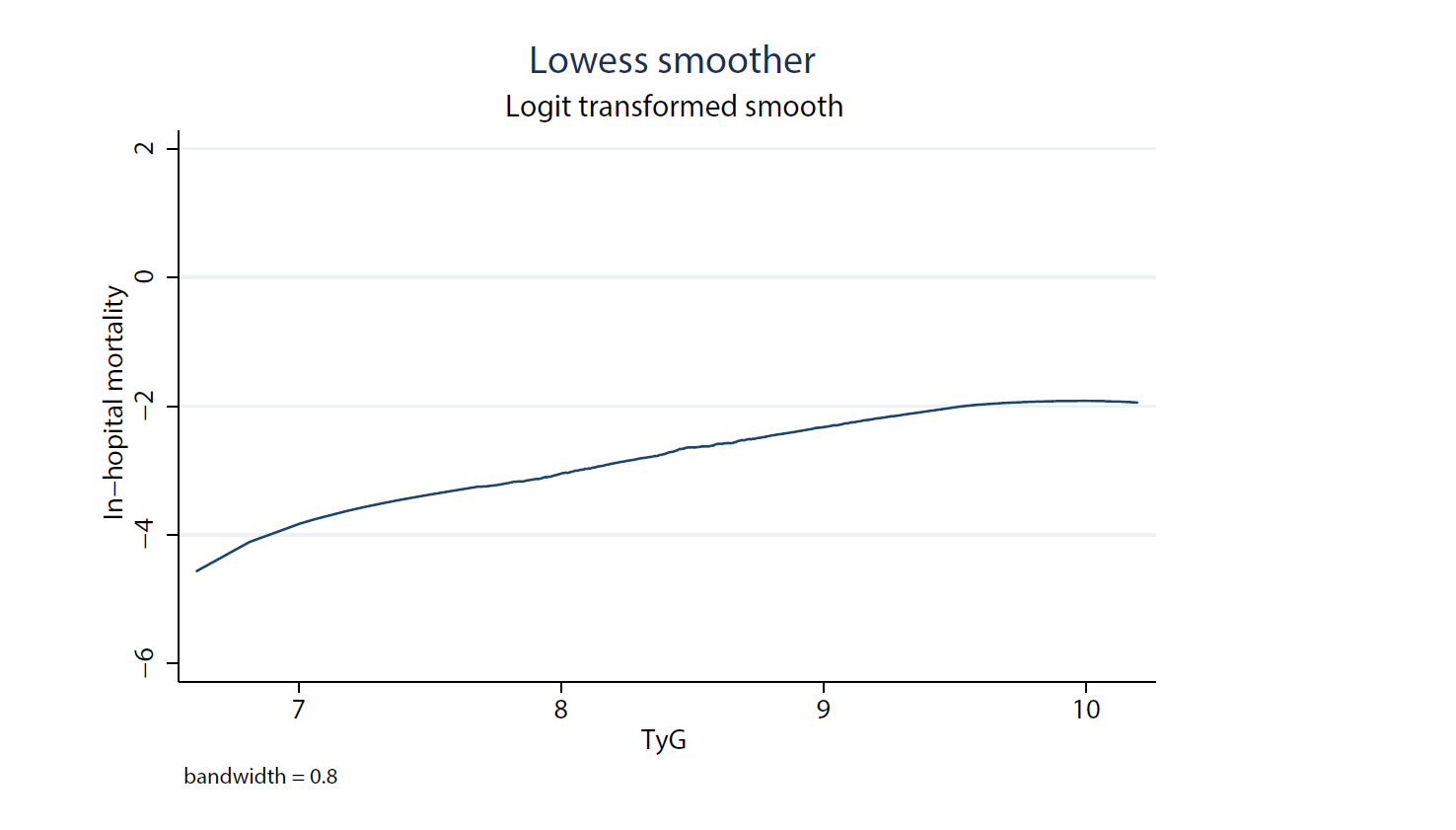 Fig. 2.
Fig. 2.Local weighted regression was used to plot the curve in line with overall trend, which described the probability of mortality predictded by TyG in raw calculations without adjustment for other covariates.
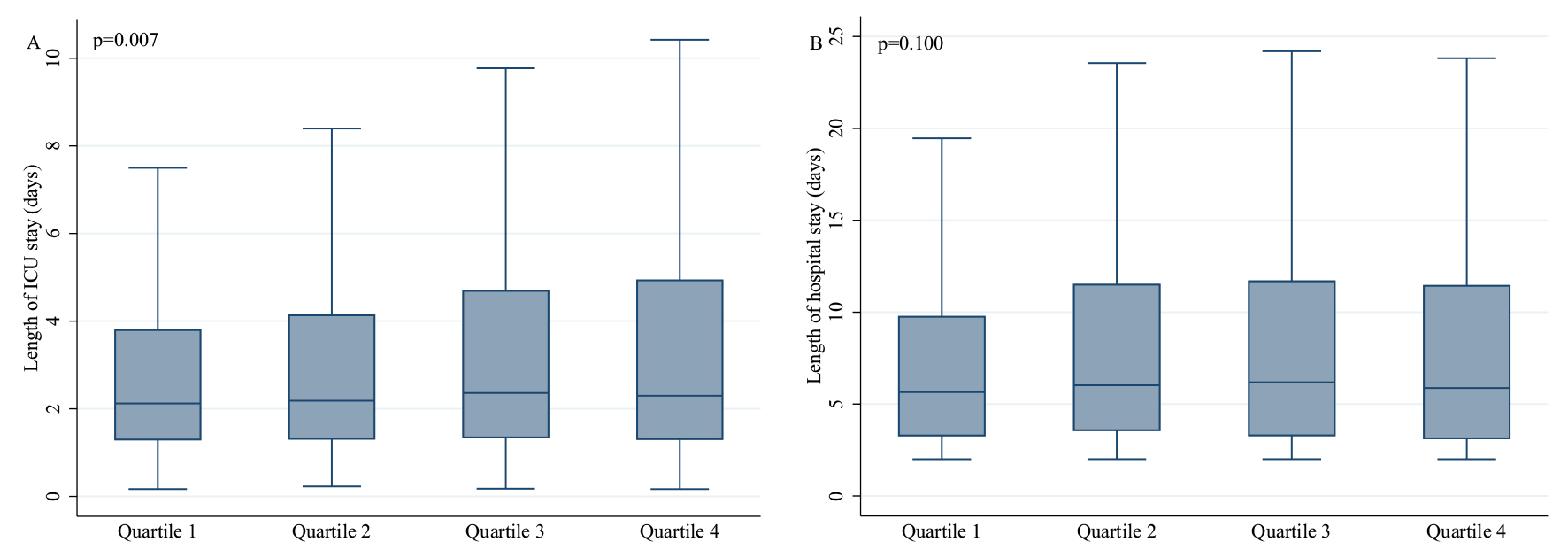
Besides, increased TyG quartiles were associated with prolonged length of ICU stay (Quartile 4 vs Quartile 1: 2.3 (1.3, 4.9) vs 2.1 (1.3, 3.8), p = 0.007), while with the growth of the TyG index, the length of hospital stay failed to increase significantly (Quartile 4 vs Quartile 1: 5.9 (3.1, 11.5) vs 5.7 (3.2, 9.8), p = 0.100) (Table 2). Moreover, we drew the box plot to reflect the relationship between TyG and length of ICU and hospital stay more intuitively. The obvious association between TyG and length of ICU stay was indicated (Fig. 3).
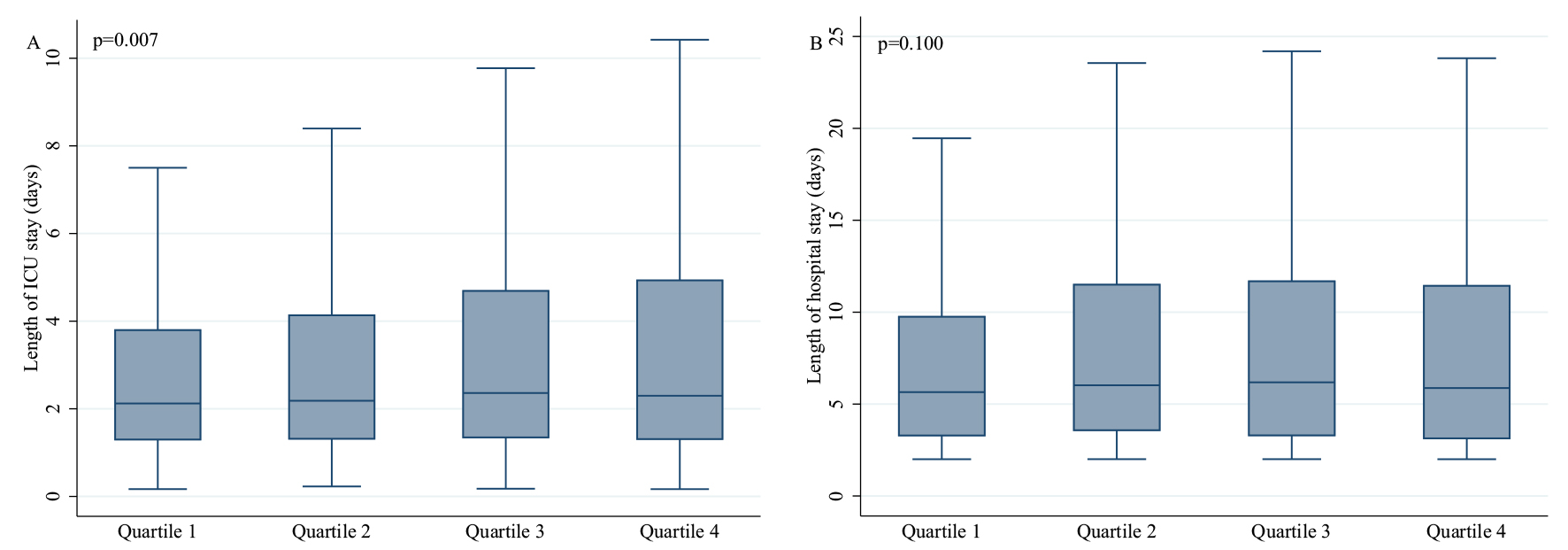 Fig. 3.
Fig. 3.Association between the triglyceride-glucose index and the length of ICU and hospital stay through box plot. Abbreviation: ICU, intensive care unit.
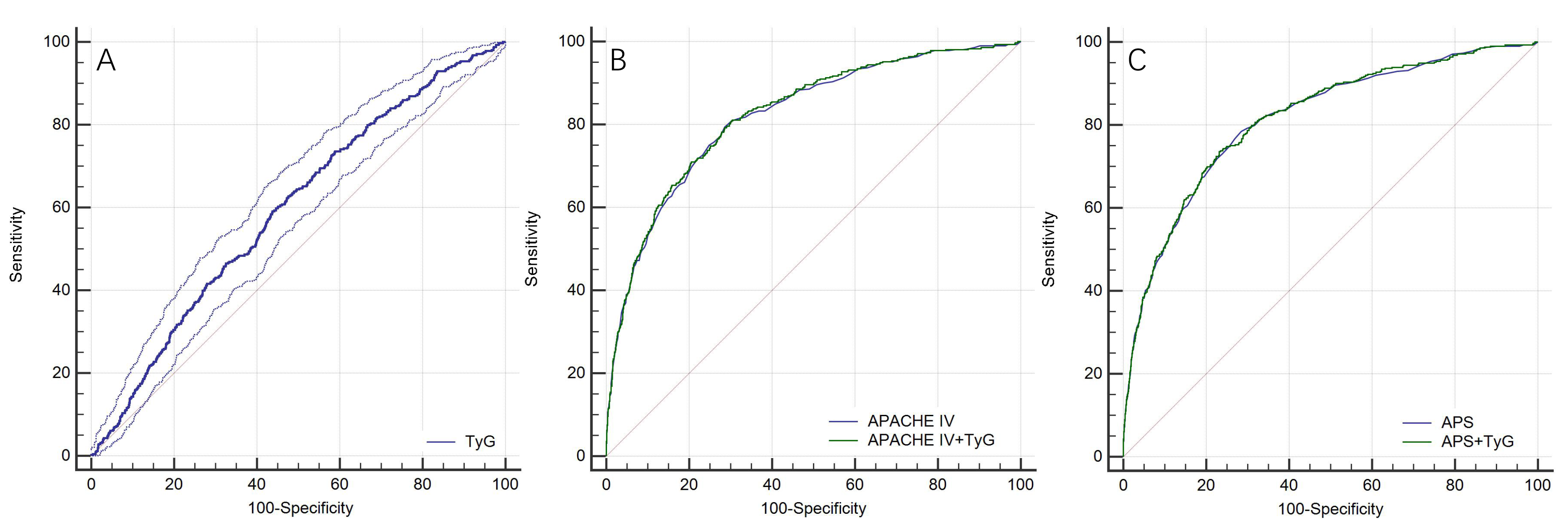
The ROC curve revealed a moderate ability of TyG to predict in-hospital mortality (AUC = 0.594 (0.580, 0.608)), the optimal cutoff value was 8.99, the sensitivity was 59.08%, and the specificity was 56.17%. The AUC of APACHE IV was 0.821 (0.810, 0.832), when combined with TyG, the AUC increased to 0.824 (0.813, 0.835), but there was no statistically significant difference (p = 0.069). The AUC of APS was 0.813 (0.802, 0.824), when combined with TyG, the AUC increased to 0.815 (0.804, 0.826), there was still no statistically significant difference (p = 0.254) (Fig. 4).
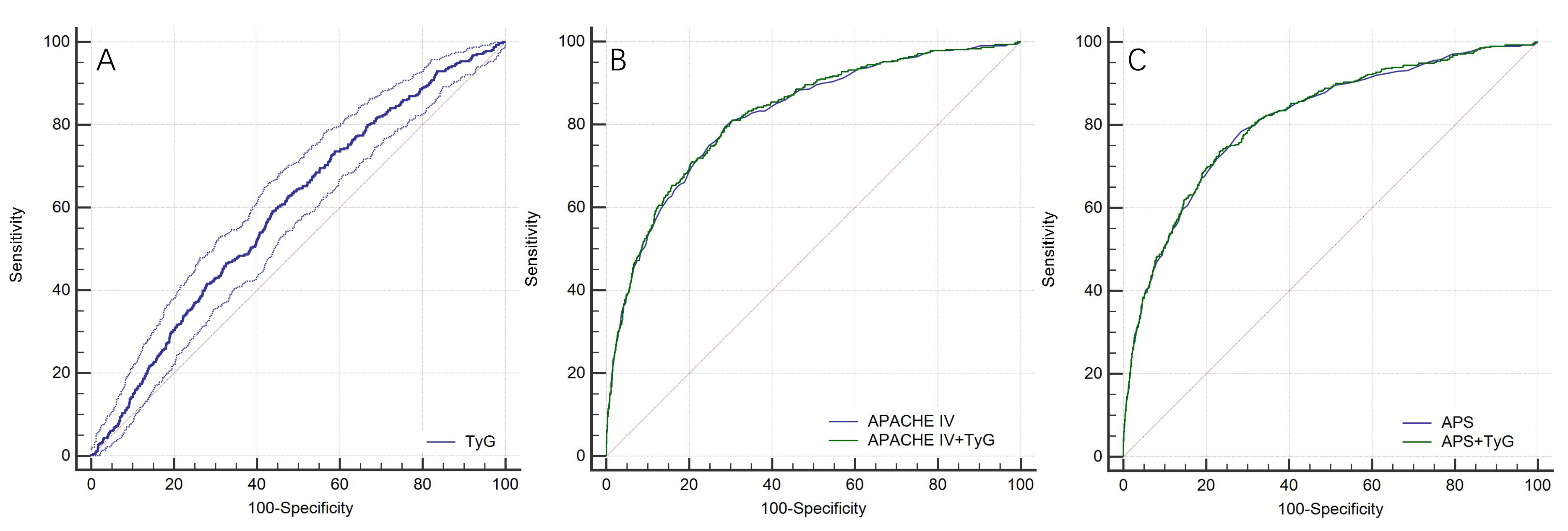 Fig. 4.
Fig. 4.ROC curves for the prediction of in-hospital mortality. (A) ROC curve for the prediction of in-hospital mortality of Tyg. (B) ROC curves for the prediction of in-hospital mortality of APACHE IV and APACHE IV+TyG. (C) ROC curves for the prediction of in-hospital mortality of APS and APS+TyG. Abbreviation: ROC, receiver-operating characteristic; TyG, triglyceride-glucose index; APACHE IV, Acute Physiology and Chronic Health Evaluation IV; APS, acute physiology score.
Patients complicated by arrhythmias or atrial fibrillation had higher risk of in-hospital mortality for TyG while patients with sepsis had lower risk of in-hospital mortality for TyG (Table 5).
| Subgroups | N | Quartile 1 | Quartile 2 | Quartile 3 | Quartile 4 | P for interaction | |
| Age (years) | 0.259 | ||||||
| 2376 | Reference | 1.44 (0.80, 2.60) | 1.70 (0.97, 2.98) | 2.40 (1.42, 4.05) | |||
| 2463 | Reference | 1.35 (0.90, 2.02) | 2.20 (1.50, 3.24) | 3.12 (2.12, 4.60) | |||
| Gender | 0.659 | ||||||
| Male | 2993 | Reference | 1.52 (0.99, 2.34) | 1.84 (1.21, 2.79) | 2.44 (1.63, 3.64) | ||
| Female | 1846 | Reference | 1.15 (0.68, 1.94) | 1.95 (1.21, 3.17) | 2.43 (1.51, 3.90) | ||
| Ethnicity | 0.722 | ||||||
| Caucasian | 3668 | Reference | 1.45 (0.99, 2.11) | 1.89 (1.31, 2.71) | 2.38 (1.67, 3.39) | ||
| African American | 663 | Reference | 1.58 (0.62, 4.03) | 3.52 (1.51, 8.22) | 5.45 (2.37, 12.50) | ||
| Other | 508 | Reference | 0.61 (0.19, 1.92) | 0.68 (0.23, 2.02) | 0.96 (0.37, 2.51) | ||
| Body mass index (kg/m |
0.707 | ||||||
| 2679 | Reference | 1.56 (1.03, 2.35) | 2.47 (1.67, 3.65) | 2.62 (1.74, 3.96) | |||
| 2160 | Reference | 1.07 (0.60, 1.89) | 1.27 (0.74, 2.18) | 2.15 (1.31, 3.52) | |||
| Systolic blood pressure (mmHg) | 0.239 | ||||||
| 2592 | Reference | 1.49 (1.00, 2.23) | 1.85 (1.25, 2.73) | 2.66 (1.82, 3.90) | |||
| 2247 | Reference | 1.17 (0.64, 2.13) | 2.09 (1.21, 3.59) | 2.46 (1.46, 4.14) | |||
| Diastolic blood pressure (mmHg) | 0.159 | ||||||
| 2647 | Reference | 1.37 (0.93, 2.00) | 1.72 (1.19, 2.49) | 2.62 (1.84, 3.72) | |||
| 2790 | Reference | 1.52 (0.75, 3.07) | 2.72 (1.42, 5.18) | 2.48 (1.30, 4.76) | |||
| Mean blood pressure (mmHg) | 0.078 | ||||||
| 2552 | Reference | 1.36 (0.91, 2.04) | 1.92 (1.31, 2.83) | 2.86 (1.97, 4.15) | |||
| 2287 | Reference | 1.44 (0.80, 2.60) | 1.99 (1.34, 3.48) | 2.17 (1.25, 3.74) | |||
| Heart rate (beats/min) | 0.449 | ||||||
| 1781 | Reference | 1.35 (0.81, 2.25) | 1.85 (1.14, 3.00) | 2.43 (1.52, 3.88) | |||
| 2226 | Reference | 1.51 (0.98, 2.35) | 1.88 (1.23, 2.87) | 2.37 (1.57, 3.57) | |||
| Respiration rate (beats/min) | 0.063 | ||||||
| 2444 | Reference | 1.27 (0.75, 2.15) | 1.54 (0.93, 2.55) | 1.94 (1.18, 3.17) | |||
| 2395 | Reference | 1.43 (0.93, 2.20) | 2.21 (1.47, 3.33) | 2.81 (1.90, 4.17) | |||
| Oxygen saturation (%) | 0.695 | ||||||
| 2814 | Reference | 1.21 (0.80, 1.81) | 1.71 (1.18, 2.48) | 2.41 (1.69, 3.44) | |||
| 3058 | Reference | 1.39 (0.89, 2.15) | 1.94 (1.28, 2.94) | 2.45 (1.64, 3.68) | |||
| Congestive heart failure | 0.150 | ||||||
| Yes | 793 | Reference | 2.05 (1.05, 3.99) | 2.91 (1.51, 5.60) | 4.05 (2.13, 7.72) | ||
| No | 4046 | Reference | 1.21 (0.83, 1.78) | 1.73 (1.20, 2.48) | 2.21 (1.56, 3.14) | ||
| Coronary artery disease | 0.095 | ||||||
| Yes | 3043 | Reference | 1.10 (0.67, 1.83) | 1.42 (0.88, 2.28) | 1.92 (1.22, 3.03) | ||
| No | 1796 | Reference | 1.76 (1.12, 2.76) | 2.78 (1.81, 4.27) | 3.35 (2.21, 5.09) | ||
| Acute coronary syndrome | 0.940 | ||||||
| Yes | 2295 | Reference | 1.02 (0.55, 1.89) | 1.55 (0.87, 2.76) | 2.31 (1.33, 3.98) | ||
| No | 2544 | Reference | 1.67 (1.12, 2.49) | 2.24 (1.53, 3.28) | 2.65 (1.83, 3.84) | ||
| STEMI | 0.223 | ||||||
| Yes | 1035 | Reference | 1.17 (0.37, 3.75) | 1.65 (0.55, 4.89) | 3.68 (1.36, 9.92) | ||
| No | 3804 | Reference | 1.43 (1.01, 2.02) | 2.00 (1.44, 2.79) | 2.39 (1.73, 3.30) | ||
| NSTEMI | 0.755 | ||||||
| Yes | 563 | Reference | 1.80 (0.62, 5.25) | 1.52 (0.48, 4.79) | 2.56 (0.89, 7.32) | ||
| No | 4276 | Reference | 1.33 (0.93, 1.89) | 1.93 (1.39, 2.69) | 2.44 (1.77, 3.35) | ||
| Arrhythmias | 0.006 | ||||||
| Yes | 1234 | Reference | 1.37 (0.73, 2.58) | 3.33 (1.87, 5.93) | 4.20 (2.36, 7.46) | ||
| No | 3605 | Reference | 1.36 (0.92, 2.01) | 1.51 (1.04, 2.21) | 2.03 (1.42, 2.92) | ||
| Cardiac arrest | 0.694 | ||||||
| Yes | 430 | Reference | 0.90 (0.45, 1.82) | 1.32 (0.69, 2.51) | 2.13 (1.14, 3.99) | ||
| No | 4409 | Reference | 1.45 (0.98, 2.15) | 1.86 (1.27, 2.70) | 2.20 (1.52, 3.18) | ||
| Bradycardia | 0.444 | ||||||
| Yes | 178 | Reference | 0.94 (0.20, 4.41) | 1.18 (0.25, 5.58) | 1.33 (0.28, 6.33) | ||
| No | 4661 | Reference | 1.39 (0.99, 1.96) | 1.94 (1.40, 2.68) | 2.49 (1.82, 3.41) | ||
| Atrial fibrillation | 0.018 | ||||||
| Yes | 675 | Reference | 1.76 (0.81, 3.79) | 3.54 (1.69, 7.39) | 5.09 (2.45, 10.60) | ||
| No | 4164 | Reference | 1.28 (0.89, 1.86) | 1.67 (1.18, 2.37) | 2.16 (1.54, 3.02) | ||
| Ventricular arrhythmias | 0.111 | ||||||
| Yes | 237 | Reference | 0.69 (0.26, 1.82) | 1.22 (0.50, 2.96) | 2.06 (0.86, 4.92) | ||
| No | 4495 | Reference | 1.35 (0.96, 1.92) | 1.83 (1.31, 2.54) | 2.29 (1.66, 3.16) | ||
| Atrioventricular block | 0.821 | ||||||
| Yes | 127 | Reference | 0.47 (0.04, 5.45) | 1.83 (0.29, 11.78) | 2.15 (0.33, 13.92) | ||
| No | 4712 | Reference | 1.39 (0.99, 1.95) | 1.90 (1.38, 2.61) | 2.44 (1.79, 3.33) | ||
| Cardiomyopathy | 0.554 | ||||||
| Yes | 297 | Reference | 1.48 (0.42, 5.22) | 2.07 (0.53, 8.07) | 3.45 (0.98, 12.07) | ||
| No | 4542 | Reference | 1.36 (0.96, 1.92) | 1.88 (1.36, 2.60) | 2.38 (1.74, 3.27) | ||
| Valve disease | 0.952 | ||||||
| Yes | 182 | Reference | 3.33 (0.85, 13.08) | 1.94 (0.44, 8.58) | 3.79 (0.83, 17.26) | ||
| No | 4657 | Reference | 1.28 (0.90, 1.80) | 1.89 (1.37, 2.62) | 2.41 (1.76, 3.29) | ||
| Shock | 0.067 | ||||||
| Yes | 975 | Reference | 1.08 (0.65, 1.79) | 1.36 (0.84, 2.20) | 1.63 (1.03, 2.58) | ||
| No | 3864 | Reference | 1.68 (1.06, 2.66) | 2.37 (1.53, 3.68) | 3.05 (1.98, 4.68) | ||
| Pulmonary embolism | 0.006 | ||||||
| Yes | 43 | , | 0.89 (0.01, 0.57) | 0.47 (0.10, 2.18) | , | ||
| No | 4781 | Reference | 1.33 (0.95, 1.86) | 1.79 (1.30, 2.46) | 2.28 (1.68, 3.10) | ||
| Pulmonary hypertension | 0.249 | ||||||
| Yes | 49 | Reference | 0.91 (0.13, 6.40) | 0.50 (0.05, 5.51) | 0.83 (0.07, 9.69) | ||
| No | 4790 | Reference | 1.39 (0.99, 1.95) | 1.96 (1.42, 2.71) | 2.52 (1.84, 3.44) | ||
| Hypertension | 0.814 | ||||||
| Yes | 1133 | Reference | 1.28 (0.60, 2.70) | 1.75 (0.85, 3.60) | 2.25 (1.14, 4.44) | ||
| No | 3706 | Reference | 1.38 (0.95, 2.00) | 1.92 (1.35, 2.72) | 2.49 (1.77, 3.51) | ||
| Diabetes | 0.109 | ||||||
| Yes | 770 | Reference | 1.14 (0.46, 2.79) | 1.33 (0.57, 3.12) | 1.44 (0.65, 3.21) | ||
| No | 4069 | Reference | 1.37 (0.95, 1.96) | 1.95 (1.39, 2.74) | 2.62 (1.87, 3.66) | ||
| Hypercholesterolemia | 0.199 | ||||||
| Yes | 452 | Reference | 1.65 (0.48, 5.66) | 1.53 (0.43, 5.39) | 1.46 (0.43, 5.01) | ||
| No | 4387 | Reference | 1.34 (0.95, 1.90) | 1.93 (1.39, 2.68) | 2.56 (1.86, 3.51) | ||
| COPD | 0.833 | ||||||
| Yes | 352 | Reference | 1.35 (0.53, 3.41) | 1.83 (0.72, 4.67) | 2.71 (1.12, 6.59) | ||
| No | 4487 | Reference | 1.37 (0.96, 1.96) | 1.94 (1.39, 2.72) | 2.46 (1.78, 3.42) | ||
| Respiratory failure | 0.419 | ||||||
| Yes | 1038 | Reference | 1.27 (0.77, 2.11) | 1.58 (0.98, 2.55) | 2.41 (1.52, 3.81) | ||
| No | 3801 | Reference | 1.28 (0.81, 2.03) | 1.79 (1.16, 2.77) | 1.88 (1.21, 2.91) | ||
| Chronic kidney disease | 0.388 | ||||||
| Yes | 546 | Reference | 0.54 (0.20, 1.43) | 1.79 (0.90, 3.56) | 2.49 (1.28, 4.82) | ||
| No | 4293 | Reference | 1.60 (1.11, 2.31) | 1.95 (1.36, 2.78) | 2.45 (1.73, 3.47) | ||
| Acute kidney injury | 0.574 | ||||||
| Yes | 659 | Reference | 1.29 (0.69, 2.41) | 1.80 (1.02, 3.16) | 1.86 (1.08, 3.21) | ||
| No | 4180 | Reference | 1.43 (0.95, 2.13) | 1.71 (1.15, 2.54) | 2.29 (1.57, 3.35) | ||
| Malignancy | 0.426 | ||||||
| Yes | 121 | Reference | 0.70 (0.19, 2.66) | 1.06 (0.30, 3.67) | 1.25 (0.33, 4.69) | ||
| No | 4718 | Reference | 1.39 (0.98, 1.97) | 1.92 (1.38, 2.67) | 2.52 (1.84, 3.46) | ||
| Sepsis | |||||||
| Yes | 519 | Reference | 1.27 (0.67, 2.43) | 1.07 (0.58, 1.99) | 0.94 (0.51, 1.71) | ||
| No | 4320 | Reference | 1.45 (0.97, 2.17) | 2.18 (1.50, 3.19) | 3.02 (2.10, 4.36) | ||
| Stroke | 0.754 | ||||||
| Yes | 233 | Reference | 1.25 (0.40, 3.96) | 2.52 (0.85, 7.50) | 2.62 (0.91, 7.52) | ||
| No | 4606 | Reference | 1.38 (0.97, 1.95) | 1.88 (1.35, 2.62) | 2.44 (1.77, 3.36) | ||
| Antiplatelet | 0.793 | ||||||
| Yes | 2611 | Reference | 2.01 (1.18, 3.43) | 2.32 (1.37, 3.91) | 2.79 (1.67, 4.66) | ||
| No | 2228 | Reference | 1.05 (0.68, 1.63) | 1.72 (1.15, 2.58) | 2.34 (1.59, 3.45) | ||
| Oral anticoagulants | 0.765 | ||||||
| Yes | 375 | Reference | 2.88 (0.55, 15.23) | 4.22 (0.86, 20.86) | 2.10 (0.34, 12.88) | ||
| No | 4464 | Reference | 1.31 (0.93, 1.84) | 1.81 (1.31, 2.50) | 2.40 (1.76, 3.28) | ||
| Beta, blockers | 0.242 | ||||||
| Yes | 1877 | Reference | 2.51 (1.28, 4.94) | 2.23 (1.13, 4.44) | 4.22 (2.23, 8.02) | ||
| No | 2962 | Reference | 1.10 (0.74, 1.63) | 1.89 (1.32, 2.70) | 2.05 (1.43, 2.93) | ||
| ACEI/ARB | 0.221 | ||||||
| Yes | 1054 | Reference | 3.42 (1.10, 10.62) | 1.94 (0.56, 6.71) | 2.28 (0.69, 7.51) | ||
| No | 3785 | Reference | 1.22 (0.86, 1.74) | 1.86 (1.34, 2.59) | 2.48 (1.80, 3.41) | ||
| Statin | 0.348 | ||||||
| Yes | 1680 | Reference | 2.23 (0.97, 5.13) | 3.37 (1.52, 7.48) | 3.93 (1.79, 8.61) | ||
| No | 3159 | Reference | 1.28 (0.88, 1.85) | 1.71 (1.21, 2.43) | 2.30 (1.64, 3.22) | ||
| White blood cell (10 |
0.763 | ||||||
| 2849 | Reference | 1.63 (1.00, 2.66) | 1.60 (0.97, 2.65) | 2.21 (1.37, 3.57) | |||
| 1990 | Reference | 1.06 (0.67, 1.67) | 1.72 (1.13, 2.60) | 2.13 (1.42, 3.21) | |||
| Lymphocyte percentage (%) | 0.428 | ||||||
| 3159 | Reference | 1.60 (1.09, 2.33) | 2.18 (1.52, 3.13) | 2.68 (1.87, 3.84) | |||
| 1680 | Reference | 0.80 (0.38, 1.66) | 1.30 (0.68, 2.50) | 2.15 (1.18, 3.89) | |||
| Monocyte percentage (%) | 0.542 | ||||||
| 2972 | Reference | 1.20 (0.79, 1.83) | 1.74 (1.17, 2.58) | 2.43 (1.67, 3.53) | |||
| 1876 | Reference | 1.65 (0.96, 2.84) | 2.12 (1.25, 3.61) | 2.22 (1.30, 3.79) | |||
| Neutrophil percentage (%) | 0.122 | ||||||
| 1548 | Reference | 0.74 (0.33, 1.64) | 0.91 (0.42, 1.96) | 2.06 (1.08, 3.93) | |||
| 3291 | Reference | 1.57 (1.09, 2.28) | 2.22 (1.56, 3.15) | 2.66 (1.87, 3.76) | |||
| Red blood cell (10 |
0.320 | ||||||
| 2270 | Reference | 1.38 (0.90, 2.12) | 2.20 (1.47, 3.28) | 3.17 (2.14, 4.69) | |||
| 2569 | Reference | 1.40 (0.82, 2.41) | 1.69 (1.01, 2.83) | 2.06 (1.25, 3.38) | |||
| Platelet (10 |
0.683 | ||||||
| 2688 | Reference | 1.39 (0.91, 2.12) | 1.84 (1.22, 2.78) | 2.42 (1.63, 3.60) | |||
| 2151 | Reference | 1.34 (0.79, 2.29) | 1.99 (1.21, 3.27) | 2.49 (1.54, 4.04) | |||
| Hemoglobin (g/dL) | 0.691 | ||||||
| 2175 | Reference | 1.41 (0.94, 2.13) | 1.82 (1.22, 2.71) | 2.83 (1.91, 4.18) | |||
| 2664 | Reference | 1.33 (0.75, 2.36) | 2.20 (1.30, 3.71) | 2.55 (1.53, 4.23) | |||
| Hematocrit (%) | 0.810 | ||||||
| 2201 | Reference | 1.37 (0.89, 2.11) | 1.94 (1.28, 2.94) | 2.82 (1.88, 4.24) | |||
| 2638 | Reference | 1.39 (0.82, 2.34) | 1.93 (1.18, 3.16) | 2.36 (1.47, 3.78) | |||
| Creatinine (mg/dL) | 0.670 | ||||||
| 3525 | Reference | 1.22 (0.78, 1.89) | 1.68 (1.10, 2.56) | 2.15 (1.43, 3.23) | |||
| 1314 | Reference | 1.57 (0.93, 2.64) | 1.96 (1.20, 3.20) | 2.44 (1.51, 3.92) | |||
| Blood nitrogen urea (mg/dL) | 0.356 | ||||||
| 3236 | Reference | 1.45 (0.91, 2.33) | 1.93 (1.23, 3.02) | 2.46 (1.59, 3.80) | |||
| 1603 | Reference | 1.24 (0.77, 2.01) | 1.84 (1.17, 2.89) | 2.29 (1.49, 3.54) | |||
| Sodium (mmol/L) | 0.722 | ||||||
| 1802 | Reference | 1.72 (1.02, 2.90) | 2.26 (1.37, 3.75) | 2.12 (1.30, 3.48) | |||
| 3037 | Reference | 1.15 (0.74, 1.78) | 1.68 (1.12, 2.52) | 2.66 (1.80, 3.92) | |||
| Potassium (mmol/L) | 0.255 | ||||||
| 2638 | Reference | 0.99 (0.63, 1.58) | 1.25 (0.81, 1.95) | 1.94 (1.28, 2.95) | |||
| 2201 | Reference | 1.93 (1.18, 3.17) | 2.91 (1.82, 4.65) | 3.09 (1.95, 4.88) | |||
| APS | 0.086 | ||||||
| 2937 | Reference | 1.77 (0.86, 3.65) | 2.03 (0.99, 4.16) | 1.95 (0.94, 4.05) | |||
| 1902 | Reference | 1.14 (0.77, 1.69) | 1.53 (1.06, 2.21) | 2.01 (1.41, 2.86) | |||
| APACHE IV | 0.155 | ||||||
| 2799 | Reference | 1.92 (0.91, 4.03) | 1.65 (0.77, 3.56) | 2.08 (0.99, 4.34) | |||
| 2040 | Reference | 1.17 (0.80, 1.72) | 1.86 (1.30, 2.66) | 2.46 (1.74, 3.49) | |||
| Binary logistic regression analysis was used and results were presented as OR (odds ratio) and 95% CI (confidence interval). P for interaction was calculated using binary logistic analysis to determine whether there is interaction between different subgroups and TyG quartiles. Abbreviation: STEMI, ST-elevation myocardial infarction; NSTEMI, non-ST-elevation myocardial infarction; COPD, chronic obstructive pulmonary disease; triglyceride-glucose index; ACEI, angiotensin-converting enzyme inhibitor; ARB, angiotensin receptor blocker; APS, acute physiology score; APACHE IV, Acute Physiology and Chronic Health Evaluation IV. | |||||||
This study affirmed the relationship between TyG and in-hospital mortality in critically ill patients with heart disease. The highlights of this study are as follows: (1) TyG index was a strong indicator of in-hospital mortality in critically ill patients with heart disease, even after adjusting for possible confounding variables. Whereas, we failed to reveal a significant association between the TyG index and in-hospital mortality in patients with diabetes. (2) The Lowess curve presented a positive relationship between TyG and in-hospital mortality. (3) Significant interactions were not observed in most subgroups. (4) Length of ICU was prolonged as TyG increased.
Previous studies have indicated that IR was strongly associated with the development and prognosis of CVD [22, 23, 24]. As an alternative method for evaluating, IR is a well-recognized risk factor for cardiovascular disease that induces an imbalance in glucose metabolism, leading to hyperglycemia, triggering inflammation and oxidative stress, systemic lipid disorders, which may contribute to the development of atherosclerosis [25]. In addition, studies have shown that IR can induce an increase in glycosylation products and free radicals, leading to inactivation of nitric oxide (NO), activation of the mitochondrial electron transport chain, and overproduction of reactive oxidative stress (ROS), which damage blood vessels endothelium [26, 27]. Moreover, IR can increase the expression of adhesion-inducing and thromboxane A2 (TxA2)-dependent tissue factor in platelets. These are associated with thrombosis and inflammation [28]. Furthermore, IR can induce excessive glycosylation, promote smooth muscle cell proliferation, collagen cross-linking, and collagen deposition, leading to increased left ventricular stiffness, cardiac fibrosis, and ultimately heart failure [29]. In addition, IR-induced activation of the renin-angiotensin system [30] and impaired cardiac calcium processing [31] may also contribute to the development of cardiovascular disease. As we know, the euglycemic-hyperinsulinemic clamp is the gold standard method for the diagnosis of IR [32]. However, due to the high cost and complex operation of this method, it is relatively difficult to carry out in practical clinical application. The homeostasis model assessment of insulin resistance (HOMA-IR) is a substitutive method for IR evaluation [33]. While it requires insulin concentration which is not routine clinical examination item. In this respect, TyG index which is calculated by fasting TGs and glucose is more readily available in clinical practice. And it has been proven to have a good predictive ability on IR compared with the above-mentioned two methods [34, 35]. Therefore, as a good substitute indicator for IR, TyG index may be a risk factor which associated with prognosis of CVD.
TyG has been extensively demonstrated to be significantly related to the development of a variety of diseases in former studies. A recent meta-analysis which included 13 cohort studies confirmed that TyG index was strongly related to the incidence of diabetes [36]. Furthermore, higher TyG index has been indicated to be associated with the increased risk of ischemic stroke [37]. Similarly, a large number of studies have also confirmed the relationship between TyG and CVD. A previous prospective cohort study proved that higher TyG index was related to the increased complexity of coronary lesions and the risk of worse outcomes in patients with NSTE-ACS [38]. Zhao et al. [16] enrolled 798 patients with T2DM and NSTEACS who underwent PCI and revealed that the level of TyG index was strongly associated with the incidence of adverse cardiovascular event during a 36-month follow-up. Luo et al. [38] reached the same conclusion in STEMI patients who were treated with PCI. Besides, TyG index was also proved to be an independent predictor of major cardiovascular events in patients with T2DM complicated by ACS undergoing PCI [39]. Even among patients with stable CAD, higher TyG index was still associated with the increased risk of mortality [40, 41]. Thus, paying attention to TyG in clinical practice and improving the level of nursing, monitoring may improve the prognosis and reduce mortality.
This study drawn a similar conclusion that increased TyG was independently related to the in-hospital mortality in critically ill patients with heart disease, providing evidence for the use of TyG in patients with severe CVD. While, when conducting multiple logistic regression analysis, there was no significant association between TyG and in-hospital mortality among patients with diabetes in model 1–3. The discrepancy might be explained by the small number of patients with diabetes in the cohort.
Interestingly, gender differences appeared to have an impact on the prediction
of adverse outcomes of TyG. The previous study has shown that the ability of TyG
to predict adverse cardiovascular events was better in women than men when TyG
Through the Lowess curve, we found that in-hospital mortality increased as the increase of TyG value. This was consistent with the conclusion that TyG was an independent predictor when considered as a continuous variable in multivariate logistic regression, which reconfirmed the reliability of TyG application in critically ill patients with heart disease.
In addition, higher TyG quartiles were associated with the increased length of ICU stay, which brought the psychological, physical, and financial burden on patients. Most of critically ill patients with heart disease have limited mobility so that complex clinical examination cannot be performed. In this circumstance, some of complex predictive scores can’t be calculated. Therefore, easily accessible indicators like TyG are more cost-effective and important for ICU patients.
This study is a single-center retrospective cohort study. Due to the limitations of the retrospective study, selection bias and recall bias cannot be avoided, and the causal relationship cannot be determined. Moreover, the severity for each kind of heart disease can not be stratified and the cause-of-death data was unavailable due to the limitation of our database. Furthermore, in patients with diabetes, the accuracy of the model is reduced because of the small sample size. And we are not able to demonstrate whether the appropriate treatment which aimed to reduce the TyG value related to the lower incidence of adverse clinical outcomes.
To summarize, the results indicated that TyG was an independent predictor of in-hospital mortality in critically ill patients with heart disease. And through multivariate logistic regression, the in-hospital mortality increased significantly as TyG quartiles increased. When considered as a continuous variable, TyG has been proven to significantly related to adverse events. In subgroup analysis, no significant interactions were observed in most subgroups. Furthermore, high TyG was associated with prolonged ICU stay length.
All methods were carried out in accordance with relevant guidelines and regulations.
The data used in this study was from eICU Collaborative Research Database [24], which is available at: https://doi.org/10.13026/C2WM1R. The author was approved to access to the database through Protecting Human Research Participants exam (certificate number: 9728458).
GZ and YZ contributed to the study design, data collection, data analysis and article writing. JW and YL contributed to the data analysis and article writing.
This study was exempted from institutional review Board approval for the following reasons: (1) retrospective design, which was lack of direct patient intervention; (2) Privacert certification of reidentification risk conforming to safe harbor standards for security protocols (Cambridge, MA) (HIPAA Certification no. 1031219-2). Data collection was in accordance with the ethical standards of the institutional review board of the Massachusetts Institute of Technology (no. 0403000206) and with the 1964 Declaration of Helsinki and its later amendments.
Thanks to Biyang Zhang for contributing to the first edition of this article.
Beijing Municipal Health Commission (Grant No. PXM2020_026272_000002; PXM2020_026272_000014); Natural Science Foundation of Beijing, China (Grant No. 7212027) to Yujie Zhou.
The authors declare no conflict of interest.
Supplementary material associated with this article can be found, in the online version, at https://doi.org/10.31083/j.rcm2308263.
References
Publisher’s Note: IMR Press stays neutral with regard to jurisdictional claims in published maps and institutional affiliations.