1 Emergency Center, Fuwai Hospital, National Center for Cardiovascular Diseases, Chinese Academy of Medical Sciences and Peking Union Medical College, 100037 Beijing, China
2 National Clinical Research Center of Cardiovascular Diseases, Fuwai Hospital, National Center for Cardiovascular Diseases, Chinese Academy of Medical Sciences and Peking Union Medical College, 100037 Beijing, China
Academic Editors: Giuseppe Nasso, Giuseppe Santarpino and Boyoung Joung
Abstract
Background: Early risk stratification of patients with atrial
fibrillation (AF) and acute coronary syndrome (ACS) or undergoing percutaneous
coronary intervention (PCI) has relevant implication for individualized
management strategies. The CHA
Keywords
- atrial fibrillation
- acute coronary syndrome
- percutaneous coronary intervention
- GRACE
- CHA2DS2-VASc score
Atrial fibrillation (AF) is the most common sustained cardiac arrhythmia, occurring in 2%–4% of the general population with increasing prevalence among the elderly [1]. It is predicted that 10%–15% AF patients will require percutaneous coronary intervention (PCI) for coronary artery disease (CAD) during their life, while patients with AF and acute coronary syndrome (ACS) will be more likely to experience adverse outcomes than ACS patients without AF [2, 3]. Concomitant risks of subsequent ischemic events, in-stent thrombosis and treatment-related bleeding need to be carefully considered before initiating appropriate antithrombotic therapy.
Several risk clinical scores have been proven to enhance the assessment of
thrombo-embolic risk in AF. CHA
Early risk stratification is also important for ACS patients to help clinicians to determine prognosis and therefore guide management strategies. A number of prognostic models have been developed including Global Registry of Acute Coronary Events (GRACE) [9], thrombolysis in myocardial infarction (TIMI) [10], and platelet glycoprotein IIb/IIIa in unstable angina: receptor suppression using Integrilin therapy (PRUSUIT) [11]. Among these, the GRACE risk score has been externally validated and proved to display the best discriminative performance [12]. The GRACE score at admission [age, systolic blood pressure (SBP), heart rate, serum creatinine, cardiac arrest at admission, elevated cardiac biomarkers, ST-segment deviation and Killip class at presentation] is established and widely accepted for assessing death or myocardial infarction from admission to six months after discharge [13]. Meanwhile, another prediction model, the GRACE score at discharge [age, history of CHF, history of myocardial infarction (MI), heart rate, SBP, ST-segment depression, serum creatinine, elevated cardiac enzymes and no in-hospital PCI] also derived by the implemented GRACE registry, has been established a robust tool for predicting 6-month post-discharge mortality in patients with ACS [14].
For patients with AF and ACS, it still remains unclear whether
CHA
This is an observational, prospective, single-center registry. From January 2017
to December 2018, a total of 1408 patients with AF (new-onset, paroxysmal,
persistent, long-standing or permanent) who were diagnosed with ACS or referred
for PCI were consecutively enrolled in the present study. All participants aged
Patients were categorized into three risk groups according to the GRACE score at
admission (low:
Cardiovascular (CV) death was adjudicated as any death with a demonstrable
cardiovascular cause or any death that was not clearly attributable to a
noncardiovascular cause. MI (myocardial infarction)was defined according to the
third universal definition of MI [15]. Ischemic stroke was adjudicated as an
episode of neurological dysfunction caused by focal cerebral, spinal, or retinal
infraction and transient ischemic attack (TIA) was defined as focal cerebral
ischemic event with symptoms lasting
The primary outcome of interest was MACCEs defined as cardiovascular (CV) mortality, myocardial infarction (MI), ischemic stroke or TIA, systemic embolism and ischemia-driven revascularization in follow-up and these events were analyzed individually. All-cause mortality was analyzed as a secondary end-point. The primary safety objective was a composite of major bleeding according to the Thrombolysis in Myocardial Infarction (TIMI) criteria [16] or bleeding in need of medical attention.
Follow-up by telephone interviews or clinic visits were scheduled every 6 months lasting for 36 months. Every adverse event or bleeding was carefully reviewed by an independent clinical event adjudication committee. The study was approved by the ethics committee of Fuwai Hospital and was conducted in accordance with the Declaration of Helsinki. All subjects provided written consent form before participation.
For baseline characteristics, categorical variables were displayed as
frequencies (percentages), and continuous variables were expressed as means
Receiver-operating curves (ROC) and c-statistics were constructed for MACCE and all-cause mortality to compare the discrimination performance of the three models. The statistical difference of c-statistics was evaluated through the Delong method and the net classification improvement (NRI) was further calculated.
The software package SPSS version 25.0 (IBM Corporation, New York, NY, USA) and
R version 4.1.2 (R Core Team, Vienna, Austria) were utilized for statistical
analysis. All statistical tests were 2-tailed, with a p value
A total of 1408 patients were included and their baseline characteristics
categorized by outcomes were displayed in Table 1. The mean age was 67.3
| Variable | Total (n = 1408) | MACCE | p value | All-cause death | p value | ||
| No (n = 1188) | Yes (n = 220) | No (n = 1267) | Yes (n = 141) | ||||
| Age (years) | 67.3 |
67.0 |
69.3 |
0.001 | 66.7 |
73.1 |
|
| Male , n (%) | 1027 (72.9) | 890 (74.9) | 137 (62.3) | 935 (73.8) | 92 (62.5) | 0.036 | |
| Emergency presentation, n (%) | 471 (33.5) | 370 (31.1) | 101 (45.9) | 381 (30.1) | 90 (63.8) | ||
| Vital signs | |||||||
| BMI (kg/m |
25.17 |
25.26 |
24.70 |
0.131 | 25.39 |
23.20 |
|
| SBP (mmHg) | 130.4 |
130.7 |
128.8 |
0.209 | 130.9 |
126.2 |
0.025 |
| DBP (mmHg) | 77.1 |
77.1 |
76.8 |
0.738 | 77.2 |
75.7 |
0.178 |
| Resting heart rate (bpm) | 78 (64–82) | 70 (64–80) | 75 (66–91) | 70 (64–80) | 78 (67–95) | ||
| Medical history, n (%) | |||||||
| Myocardial infarction | 397 (28.2) | 310 (26.1) | 87 (39.5) | 324 (25.6) | 73 (51.8) | ||
| PCI | 419 (29.8) | 351 (29.5) | 68 (30.9) | 0.689 | 370 (29.2) | 49 (34.8) | 0.175 |
| Heart failure | 302 (21.4) | 209 (17.6) | 93 (42.3) | 230 (18.2) | 72 (51.1) | ||
| Hypertension | 1088 (77.3) | 909 (76.5) | 179 (81.4) | 0.136 | 977 (77.1) | 111(78.7) | 0.751 |
| Hyperlipidemia | 1037 (73.7) | 872 (73.4) | 165 (75.0) | 0.677 | 930 (73.4) | 107 (75.9) | 0.614 |
| Diabetes | 600 (42.6) | 490 (41.2) | 110 (50.0) | 0.018 | 527 (41.6) | 73 (51.8) | 0.025 |
| Stroke/TIA | 355 (25.2) | 278 (23.4) | 77 (35.0) | 305 (24.1) | 50 (35.5) | 0.004 | |
| Chronic kidney disease | 187 (13.3) | 133 (11.2) | 54 (24.5) | 131 (10.3) | 56 (39.7) | ||
| AF pattern, n (%) | 0.330 | ||||||
| First diagnosed | 106 (7.5) | 87 (7.3) | 19 (8.6) | 96 (7.6) | 10 (7.1) | ||
| Paroxysmal | 795 (56.5) | 701 (59.0) | 94 (42.7) | 725 (57.2) | 70 (49.6) | ||
| Persistent | 462 (32.8) | 364 (30.6) | 98 (44.5) | 406 (32.0) | 56 (39.7) | ||
| Long-standing persistent | 41 (2.9) | 33 (2.8) | 8 (3.6) | 37 (2.9) | 4 (2.8) | ||
| Permanent | 4 (0.3) | 3 (0.3) | 1 (0.5) | 3 (0.2) | 1 (0.7) | ||
| Diagnosis for CAD, n (%) | 0.001 | ||||||
| SCAD | 433 (30.8) | 379 (31.9) | 54 (24.5) | 414 (32.7) | 18 (13.5) | ||
| Unstable angina | 471 (33.5) | 402 (33.8) | 69 (31.4) | 436 (34.4) | 35 (24.8) | ||
| STEMI | 204 (14.5) | 176 (14.8) | 28 (12.7) | 171 (13.5) | 33 (23.4) | ||
| NSTEMI | 300 (21.3) | 231 (19.4) | 69 (31.4) | 246 (19.4) | 54 (38.3) | ||
| Laboratory test | |||||||
| Hemoglobin (g/dL) | 14.25 |
14.33 |
13.82 |
14.38 |
13.14 |
||
| Serum potassium (mmol/L) | 4.18 |
4.17 |
4.23 |
0.096 | 4.18 |
4.21 |
0.363 |
| Creatinine (mg/dL) | 1.07 |
1.05 |
1.16 |
1.04 |
1.30 |
||
| eGFR (mL/min/1.73 m |
77.96 |
79.38 |
70.31 |
79.74 |
61.93 |
||
| cTNI elevation | 0.3 (0.0–3.6) | 0.3 (0.0–3.2) | 1.1 (0.0–7.4) | 0.052 | 0.3 (0.0–3.0) | 2.0 (0.3–23.3) | |
| NT-proBNP (pg/mL) | 766.95 (234.78–2122.95) | 619.05 (205.03–1691.88) | 1920.5 (704.28–5004.38) | 630.40 (210.90–1692.0) | 3334.4 (1550.20–9368.80) | ||
| LDL-C (mg/dL) | 89.71 |
89.71 |
90.87 |
0.620 | 89.71 |
88.94 |
0.766 |
| INR | 1.15 |
1.12 |
1.28 |
0.008 | 1.12 |
1.34 |
0.011 |
| HbA1c (%) | 6.63 |
6.59 |
6.86 |
0.005 | 6.62 |
6.78 |
0.159 |
| LVEF (%) | 56.3 |
57.2 |
51.5 |
57.4 |
46.6 |
||
| Medications, n (%) | |||||||
| Aspirin | 1147 (81.5) | 996 (83.8) | 151 (68.6) | 1053 (83.1) | 94 (66.7) | ||
| Clopidogrel | 1257 (89.3) | 1054 (88.7) | 203 (92.3) | 0.124 | 1132 (89.3) | 125 (88.7) | 0.801 |
| Ticagrelor | 118 (8.4) | 111 (9.3) | 7 (3.2) | 0.001 | 114 (9.0) | 4 (2.8) | 0.010 |
| Anticoagulant therapy | 682 (48.4) | 528 (44.4) | 154 (70.0) | 612 (48.3) | 70 (49.6) | 0.790 | |
| Statin | 1375 (97.7) | 167 (98.2) | 208 (94.5) | 0.003 | 1247 (98.4) | 128 (90.8) | |
| ACEi or ARB | 898 (63.8) | 770 (64.8) | 128 (58.2) | 0.067 | 828 (65.4) | 70 (49.6) | |
| Diuretics | 550 (39.1) | 425 (35.8) | 125 (56.8) | 447 (35.3) | 103 (73.0) | ||
| 1210 (85.9) | 1017 (85.6) | 193 (87.7) | 0.460 | 1090 (86.0) | 120 (85.1) | 0.798 | |
| CHA |
3.7 |
3.6 |
4.6 |
3.6 |
5.1 |
||
| GRACE at admission | 126 |
123 |
142 |
122 |
161 |
||
| GRACE at discharge | 108 |
105 |
126 |
104 |
144 |
||
| MACCE, major adverse cardiovascular and cerebrovascular events; BMI, body mass index; SBP, systolic blood pressure; DBP, diastolic blood pressure; PCI, percutaneous coronary intervention; TIA, transient ischemic attack; AF, atrial fibrillation; CAD, coronary artery disease; SCAD, stable coronary artery diseases; eGFR, estimated glomerular filtration fraction; NT-proBNP, N-terminal pro-B-type natriuretic peptide; LDL-C, low-density lipoprotein cholesterol; INR, international normalized ratio; LVEF, left ventricular ejection fraction. | |||||||
The mean value of CHA
The clinical outcomes classified by GRACE and CHA
| Endpoints | CHA |
GRACE score at admission | GRACE score at discharge | |||||||
| Total (n = 1408) | 1, 2 (n = 380) | 3, 4 (n = 584) | 109–140 (n = 517) | 89–118 (n = 536) | ||||||
| MACCE | 220 (15.6) | 29 (7.6) | 79 (13.5) | 112 (25.2) | 57 (11.1) | 69 (13.3) | 94 (25.0) | 36 (8.8) | 69 (12.9) | 115 (24.8) |
| Cardiovascular mortality | 99 (7.0) | 7 (1.8) | 29 (5.0) | 63 (14.2) | 9 (1.7) | 26 (5.0) | 64 (17.0) | 3 (0.7) | 18 (3.4) | 78 (16.8) |
| Myocardial infarction | 39 (2.8) | 2 (0.5) | 11 (1.9) | 26 (5.9) | 7 (1.4) | 11 (2.1) | 21 (5.7) | 2 (0.5) | 14 (2.6) | 23 (5.0) |
| Stroke/TIA | 57 (4.0) | 6 (1.6) | 25 (4.3) | 26 (5.9) | 20 (3.9) | 21 (4.1) | 16 (4.3) | 16 (3.9) | 19 (3.5) | 22 (4.7) |
| Ischemia-driven revascularization | 56 (4.0) | 14 (3.7) | 23 (4.0) | 19 (4.3) | 27 (5.2) | 21 (4.1) | 8 (2.2) | 17 (4.2) | 29 (5.4) | 10 (2.2) |
| Systemic embolism | 6 (0.4) | 0 (0.0) | 5 (0.9) | 1 (0.2) | 2 (0.4) | 3 (0.6) | 1 (0.3) | 2 (0.5) | 1 (0.2) | 3 (0.7) |
| All-cause mortality | 136 (9.7) | 8 (2.1) | 43 (7.4) | 85 (19.1) | 11 (2.1) | 38 (7.4) | 89 (23.7) | 4 (1.0) | 27 (5.0) | 105 (22.6) |
| Major bleeding | 24 (1.7) | 5 (1.3) | 10 (1.7) | 9 (2.1) | 6 (1.2) | 13 (2.5) | 5 (1.4) | 5 (1.2) | 13 (2.4) | 6 (1.3) |
| Minor bleeding | 24 (1.7) | 2 (0.5) | 10 (1.7) | 12 (2.7) | 3 (0.6) | 9 (1.7) | 12 (3.2) | 1 (0.2) | 9 (1.7) | 14 (3.1) |
| Data presented as number of events and 36-month Kaplan-Meier estimates: n (%). Abbreviations: MACCE, major adverse cardiovascular and cerebrovascular events; TIA, transient ischemic attack. | ||||||||||
Kaplan-Meier curves for MACCE and all-cause mortality in patients at low,
intermediate and high risk based on different scores were plotted in Fig. 1.
Higher CHA
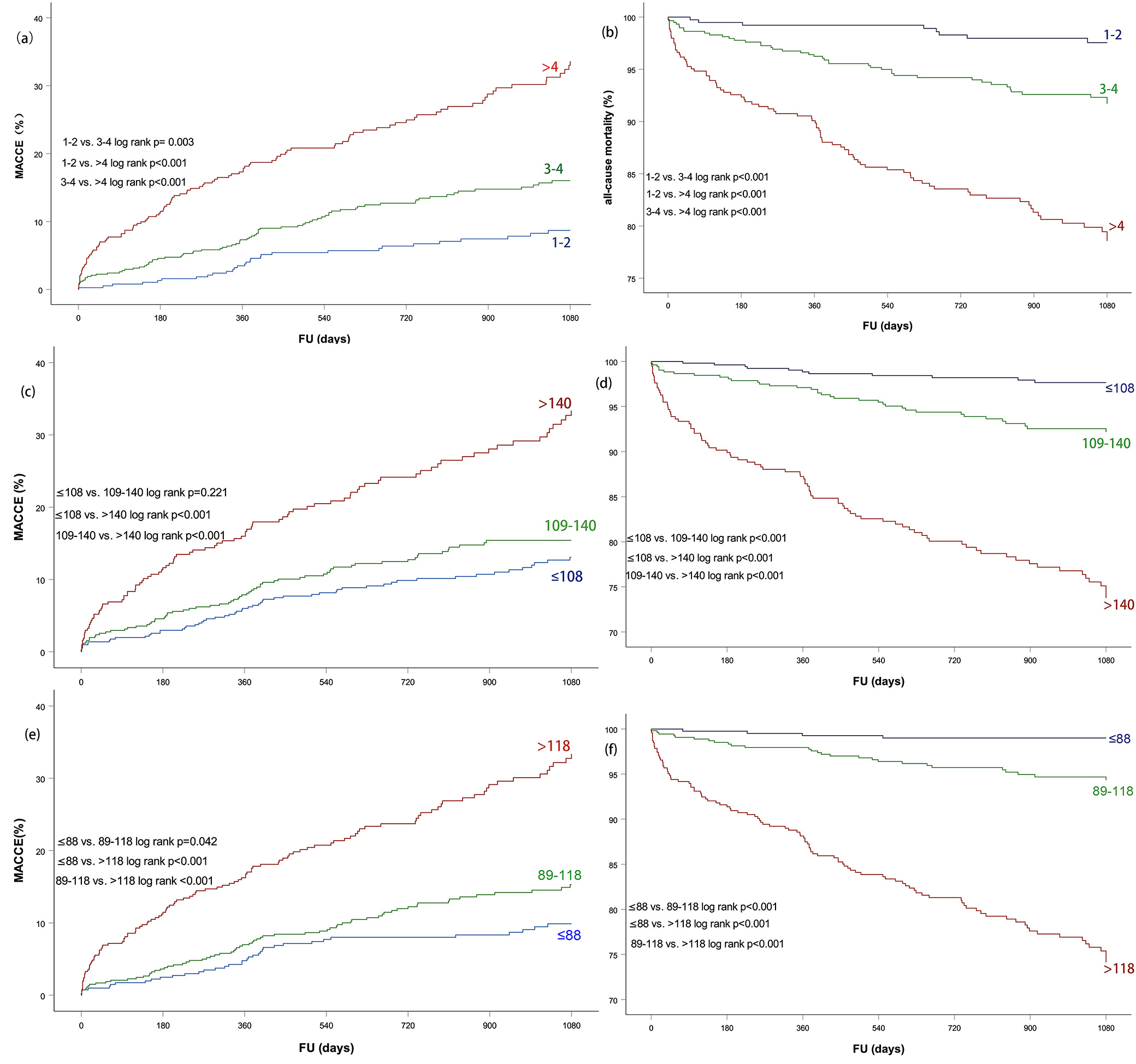 Fig. 1.
Fig. 1.Kaplan-Meier curves for 36-month adverse events in patients at
low, intermediate and high risk based on three risk scores. (a)
CHA
| MACCE | All-cause mortality | Major bleeding | |||||
| HR (95% CI) | p | HR (95% CI) | p | HR (95% CI) | p | ||
| CHA |
1.184 (1.091–1.284) | 1.348 (1.216–1.494) | 0.995 (0.770–1.286) | 0.972 | |||
| 1–2 | Reference | Reference | Reference | ||||
| 3–4 | 1.449 (0.935–2.244) | 0.097 | 2.878 (1.285–6.446) | 0.010 | 0.933 (0.304–2.860) | 0.903 | |
| 2.226 (1.436–3.453) | 5.457 (2.469–12.061) | 1.082 (0.335–3.497) | 0.895 | ||||
| GRACE at admission (continuous) | 1.004 (1.000–1.008) | 0.061 | 1.013 (1.008–1.018) | 0.992 (0.978–1.006) | 0.275 | ||
| Reference | Reference | Reference | |||||
| 109–140 | 1.089 (0.755–1.571) | 0.648 | 2.863 (1.450–5.653) | 0.002 | 3.148 (1.000–9.518) | 0.050 | |
| 1.32 (0.786–2.229) | 0.292 | 5.309 (2.727–10.336) | 0.966 (0.207–4.510) | 0.966 | |||
| GRACE at discharge (continuous) | 1.009 (1.004–1.014) | 1.026 (1.020–1.032) | 0.992 (0.977–1.007) | 0.300 | |||
| Reference | Reference | Reference | |||||
| 89–118 | 1.268 (0.839–1.917) | 0.260 | 4.219 (1.471–12.101) | 0.007 | 1.573 (0.550–4.498) | 0.399 | |
| 1.631 (1.066–2.498) | 0.024 | 11.666 (4.177–32.585) | 0.638 (0.171–2.383) | 0.504 | |||
| Adjusted for emergency presentation, atrial fibrillation patterns, subtypes of coronary artery disease, hemoglobin, NT-proBNP at admission, LVEF, INR, anticoagulant therapy, use of aspirin, use of ticagrelor. | |||||||
ROC curves of CHA
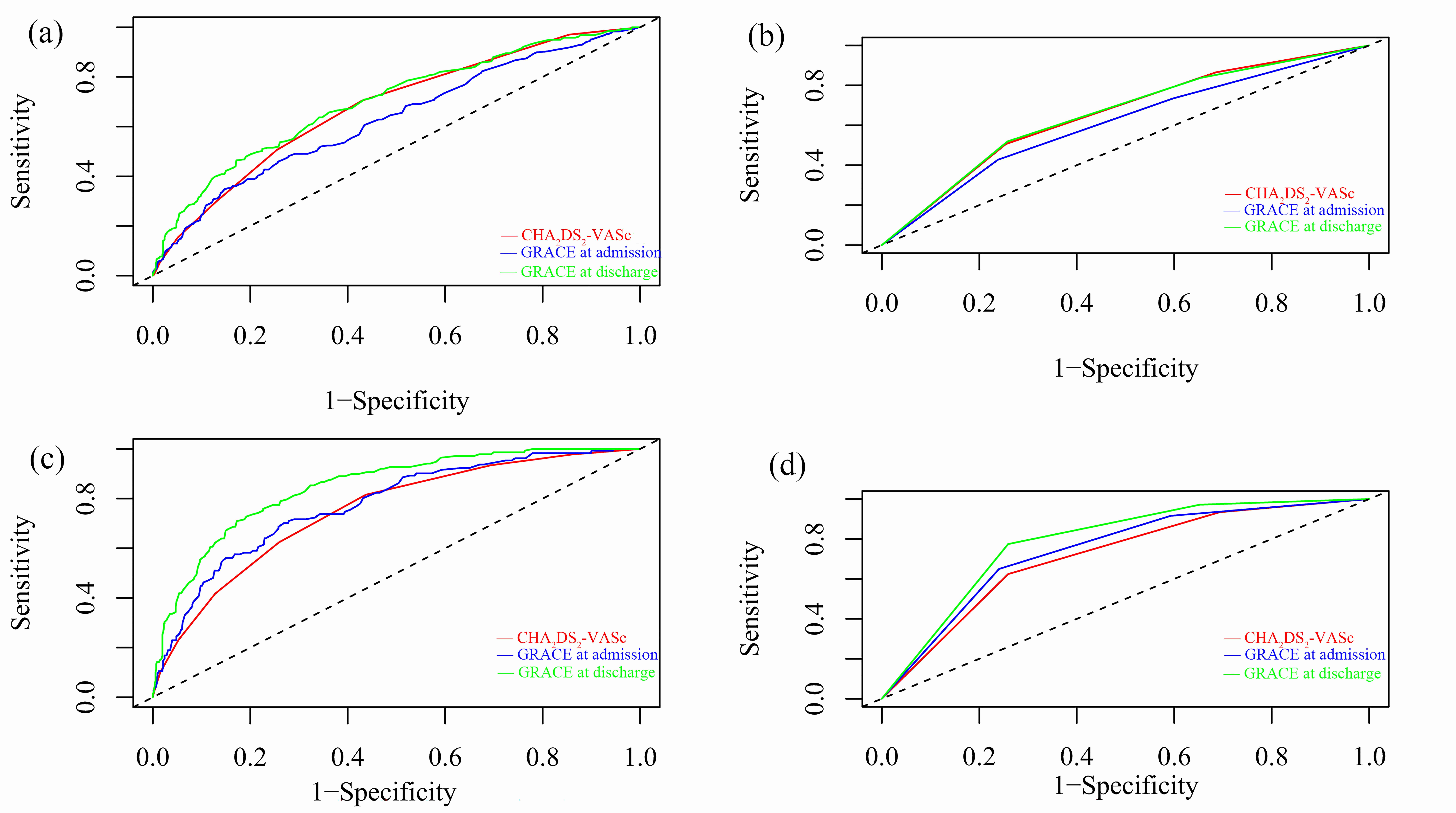 Fig. 2.
Fig. 2.ROC curves for predicting MACCEs or all-cause mortality during follow-up. Three scores were treated (a) as continuous variables for MACCEs. (b) as categorical variables for MACCEs. (c) as continuous variables for all-cause mortality. (d) as categorical variables for all-cause mortality.
To assess whether predictive performance differed depending on sex, primary
outcome was also analyzed comparing CHA
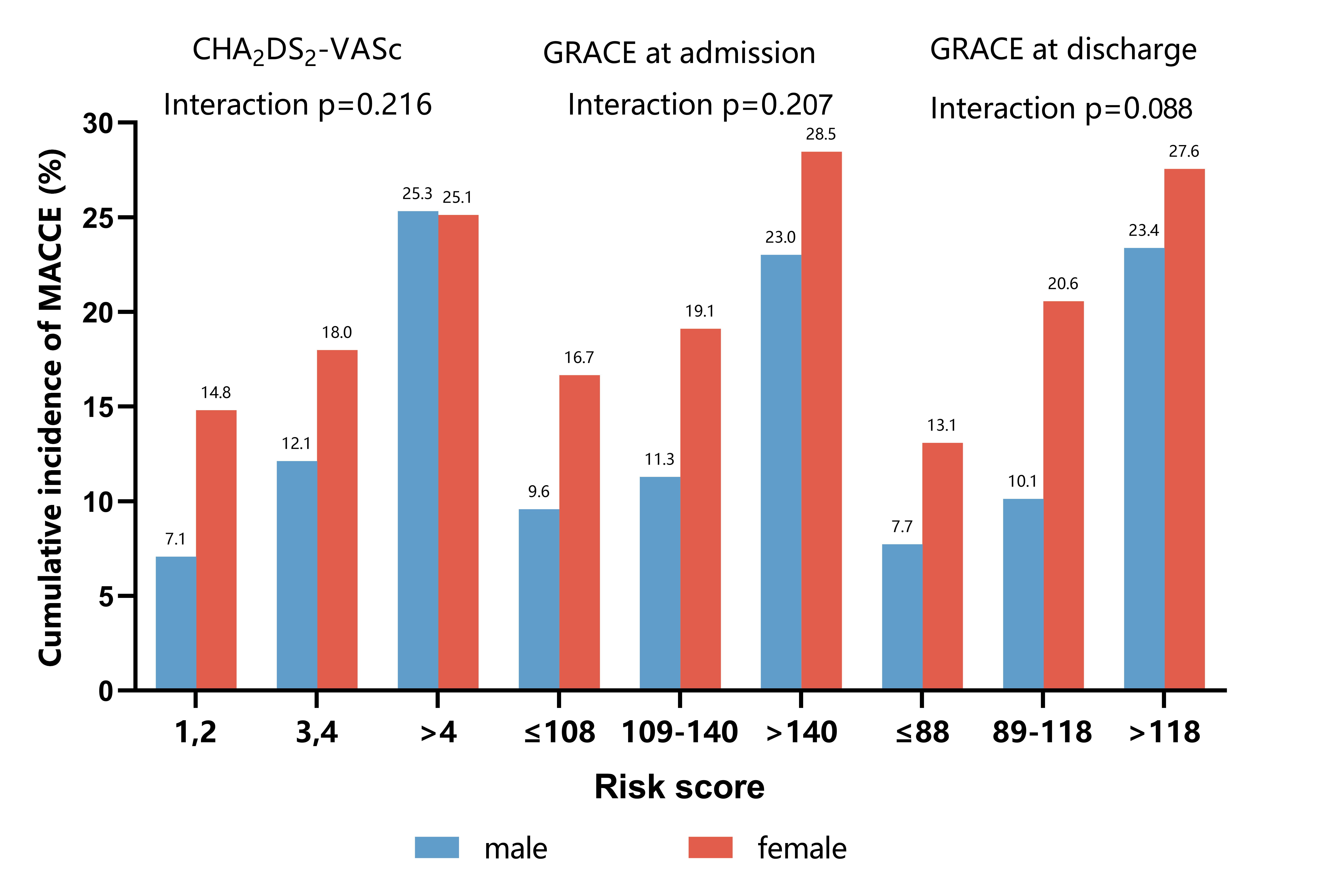 Fig. 3.
Fig. 3.Cumulative incidence of MACCEs according to sex during 36 months
follow-up. The predictive performance of CHA
In the present study, we assessed prognostic values of the
CHA
The co-existence of AF and the need for PCI is a much more complicated situation compared to suffering from AF or CAD alone. Existing evidence reports the incidence of ACS with concomitant AF between 6% to 22%, with an increased incidence in elderly and female patients [17, 18]. AF is a well-established marker of poor short- and long-term prognosis in patients with ACS and is associated with an increased risk of overall mortality. An analysis derived from 1558205 ACS patients observed that patients with AF had significantly longer and more complicated hospital stays with nearly double adjusted in-hospital mortality [19]. Pilgrim et al. [20] showed that among patients with CAD undergoing revascularization with drug-eluting stents (DES), AF conferred a rising risk of both all-cause mortality and ischemic stroke during four-year follow-up. Similar results were obtained from sub analysis of the Global Registry of Acute Coronary Events (GRACE) study where ACS patients with concomitant AF were more likely to have a complicated in-hospital course than those without AF [21]. Meanwhile, in a large-scale, prospective registry including 29,679 consecutive patients presenting with AF, a prior ACS conferred higher adjusted risks of stroke, systemic embolism, all-cause mortality and CV mortality [22]. In the present study, we reported that the 3-year incidences of composite MACCEs, all-cause mortality, CV mortality reached 15.6%, 9.7% and 7.0% respectively. In the EPICOR (long-tErm follow-uP of antithrombotic management patterns In acute CORonary syndrome patients) Asia study, 6.2% patients experienced the composite endpoint of death, MI and ischemic stroke and 3.6% suffered all-cause death (including 1.3% cardiovascular-related) within 2 years. Although our analysis was from a different group of patients in EPICOR Asia, it could be predicted that ACS combined with AF had a numerically higher relative risk in long-term adverse events compared to ACS alone. Whether AF contributes to the onset of ACS or if ACS leads to AF is beyond the scope of this paper as we lack the precise information about the time of appearance of these diseases. However, previous studies observed that AF could promote inflammation that could cause a prothrombotic state and eventually coronary artery occlusion [23]. In addition, AF with high heart ventricular rates might yield symptoms of myocardial ischemia characterized by an imbalance between demand and blood supply [24]. Conversely, CAD affecting the atrial branches could result atrial scarring and remodeling to form a substrate conducive for consequent persistent AF [25]. In the past three decades, catheter ablation has evolved to a well-established treatment option for AF patients to obtain rhythm control. The safety and effectiveness of ablation in increasing freedom from recurrences and lowering AF burden during one year follow-up has been documented in multiple clinical trials [26, 27]. While the study lacked information on catheter ablation, there is no randomized controlled trial sufficiently large to properly evaluate a reduction in thromboembolic events compared with antiarrhythmic dugs [5].
The CHA
The GRACE ACS score was derived from an international registry of ACS patients
and has been a well-recognized risk system to stratify patients according to
their estimated risk of future death or ischemic events. Several studies have
also tried to evaluate and compare the predictive performance of
CHA
The following were several limitations in the present study. First, this is an observational, prospective, single-center registry and has its inherent residual confounding bias. Our findings should be carefully interpreted when applied to external validation cohorts. However, we analyzed a total of 1408 AF patients with ACS or undergoing PCI and the sample size was comparable to those of similar researches. Second, we did not assess the prognostic values of the three models according to the subtypes of AF for we were unable to determine the accurate order of the presence of AF and ACS. Previous evidence suggested that only permanent AF was an independent predictor for death in AMI patients treated invasively [36]. Third, the post-discharge antithrombotic regimens were collected and treated as a covariate in our study. During 3-year follow-up, the medication adherence of participants and the possible transitions in dual-antiplatelet therapy after coronary stenting were unable to be obtained. The changes in anticoagulant or antiplatelet therapies might have significantly affected the incidence of ischemic or bleeding events. Further well-designed clinical trials are needed to compare and validate the prediction performance of several risk stratification systems for AF patients with ACS or undergoing stent implantation.
In the setting of coexistence of AF and ACS or coronary stenting, higher
CHA
RM acquired the data, performed statistical analysis and drafted the manuscript. YMY designed the research and revised the manuscript. HZ and NS collected data and provided help in interpreting. JYW and SQL collected the data and helped in endpoints adjudication. All authors contributed to editorial changes in the manuscript. All authors read and approved the final manuscript.
The study was approved by the ethics committee of Fuwai Hospital and was conducted in accordance with the Declaration of Helsinki (No. 2017-922).
We wish to thank all individuals who agreed to participate in this study. The authors also thank the staff in Emergency Department in Fuwai Hospital for patients’ recruitment.
This research was funded by Capital’s Funds for Research and Application of Clinical Diagnosis and Treatment Technology, grant number Z171100001017193.
The authors declare no conflict of interest.
Supplementary material associated with this article can be found, in the online version, at https://doi.org/10.31083/j.rcm2305168.



