1 Department of Cardiology, Tan Tock Seng Hospital, 308433 Singapore, Singapore
Academic Editors: Brian Tomlinson and Takatoshi Kasai
Abstract
Treatment for acute coronary syndrome (ACS) in women during pregnancy is challenging. Current standard treatment for ACS includes coronary angioplasty with guideline-directed medical therapy including aspirin, P2Y12 inhibitors, beta-blockers, angiotensin converting enzyme inhibitors, which may portend adverse effects to the fetus. ACS increases ischemic and obstetric complications during pregnancy and the postpartum period. Management of these patients necessitates balancing the potential risks and benefits to both maternal and fetal health. We present a case of a 37-year-old female with a background of hypertension and hyperlipidemia who presented with Non-ST segment elevation myocardial infarction (NSTEMI). The urine pregnancy test that was performed turned positive with an estimated gestational age of four weeks. After counselling on the potential risks and benefits, a diagnostic angiogram was performed which revealed triple vessel disease with critical stenosis in all three vessels. Percutaneous coronary intervention (PCI) was performed successfully with precautions taken to minimize radiation exposure to the fetus. In such cases, there is a fundamental trade-off between maternal and fetal health in the treatment of NSTEMI. Medications used for the treatment of acute coronary syndrome will need to be balanced against the potential risks to the fetus. Invasive coronary angiogram results in exposure to potentially teratogenic ionizing radiation and hence all efforts must be made to minimize exposure. Thus, risks and benefits of treatment ought to be discussed with patients and measures need to be taken to minimize potential harm to both the mother and fetus.
Keywords
- NSTEMI
- Acute coronary syndrome
- Pregnancy
- Radiation safety
Acute coronary syndrome (ACS) in women during pregnancy remains a relatively rare occurrence with an estimated incidence rate of 6.2 per 100,000 deliveries [1]. Yet maternal mortality with ACS is reported to be as high as 20% [2]. These numbers are expected to be rise with increasing maternal age and associated risk factors of obesity, hypertension, hyperlipidemia, and maternal diabetes — all of which are well documented to increase the risk of atherosclerosis [2, 3]. According to the published guidelines in 2018 from the European Society of Cardiology (ESC) for cardiovascular diseases in pregnancy, the standard of care for patients with Non-ST elevation myocardial infarction (NSTEMI) and high-risk features, entails invasive coronary angiography with angioplasty [4]. Medical therapy including dual antiplatelet agents, beta-blockers, and angiotensin converting enzymes (ACE) inhibitors is also recommended but these can be potentially harmful to the developing fetus. We present a case illustrating the tradeoffs in ACS treatment between maternal and fetal health.
A 37-year-old Chinese female presented to the emergency department with a one-day history of recurrent angina at rest and on exertion. Her past medical history includes that of hypertriglyceridemia and hypertension, for which she is on fenofibrate and atenolol. There were no other significant cardiovascular risk factors, smoking history, or family history of premature coronary artery disease. Obstetric history includes two previous uncomplicated pregnancies. A 12-lead electrocardiogram was performed and revealed normal sinus rhythm with T-wave inversions in the anterolateral leads (leads V1–V5) (Fig. 1). Laboratory tests showed elevated high sensitivity Troponin I at 1418 ng/L, which subsequently rose to 2352 ng/L after 6 hours. Her low-density lipoprotein was 127.6 mg/dL, with a normal HbA1c of 5.6%. Other results were unremarkable. A diagnosis of NSTEMI was established and she was started on dual antiplatelet agent therapy with loading doses of aspirin and clopidogrel, and subcutaneous Enoxaparin 1 mg/kg twice daily. She was transferred to the ward with continuous cardiac monitoring and plans for discussion for an early invasive coronary angiogram. A transthoracic echocardiogram was also obtained showing a left ventricular ejection fraction of 55% and no regional wall motion abnormality.
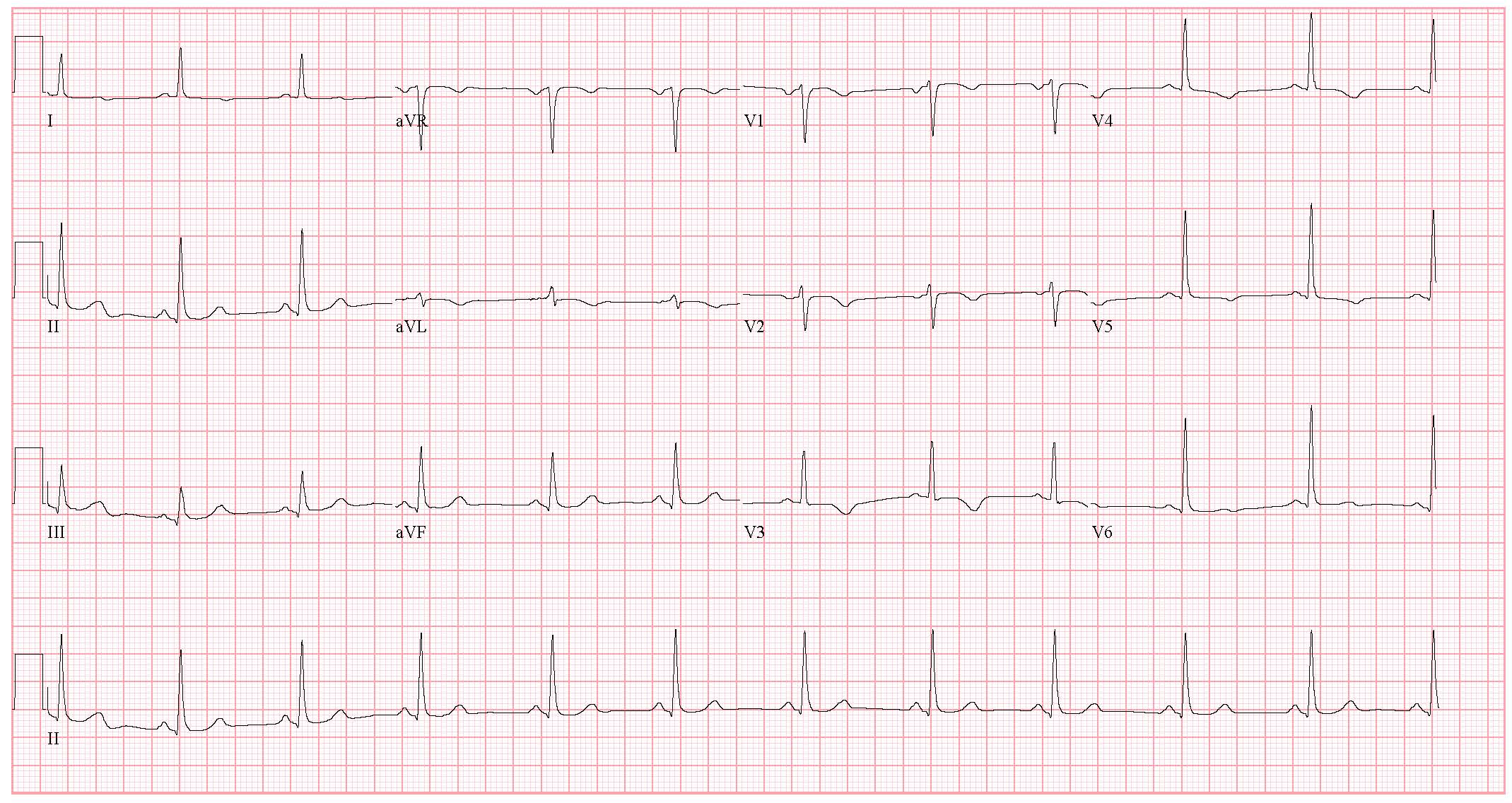 Fig. 1.
Fig. 1.12-lead electrocardiogram obtained on admission revealing normal sinus rhythm with T-wave inversions in anterolateral leads (leads V1–V5).
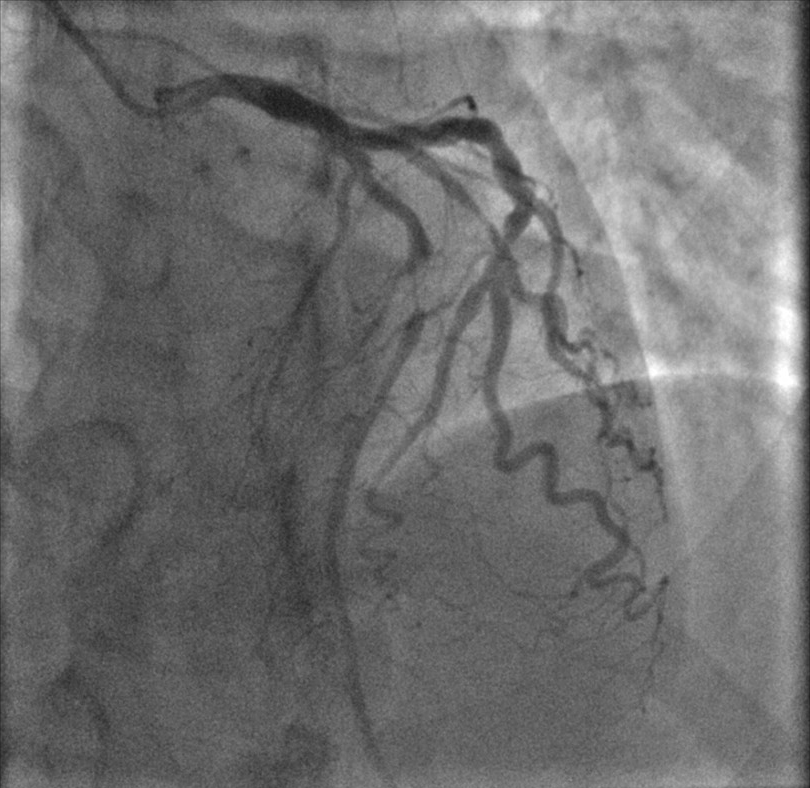
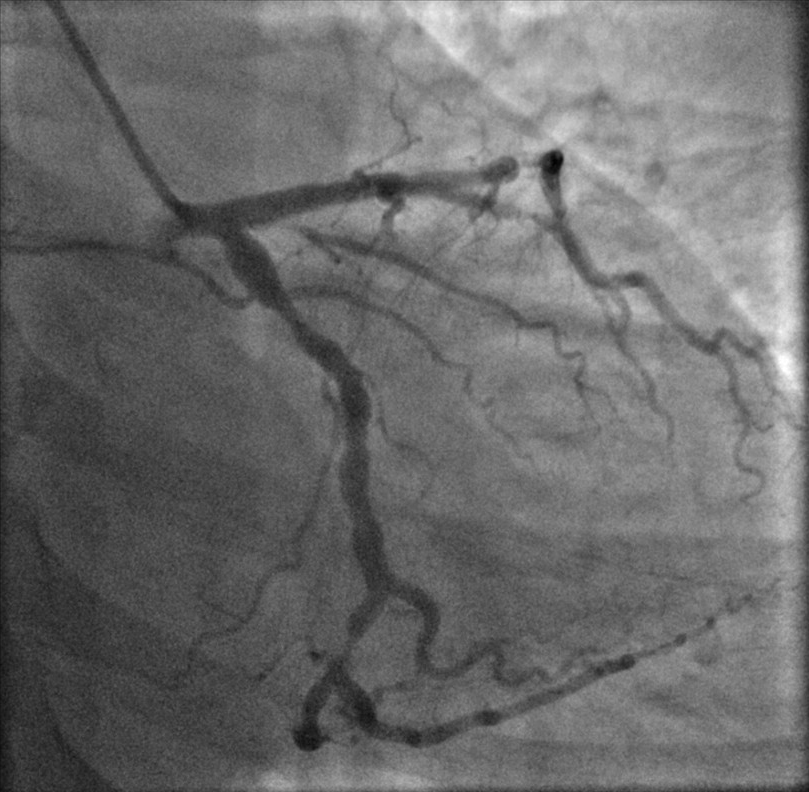
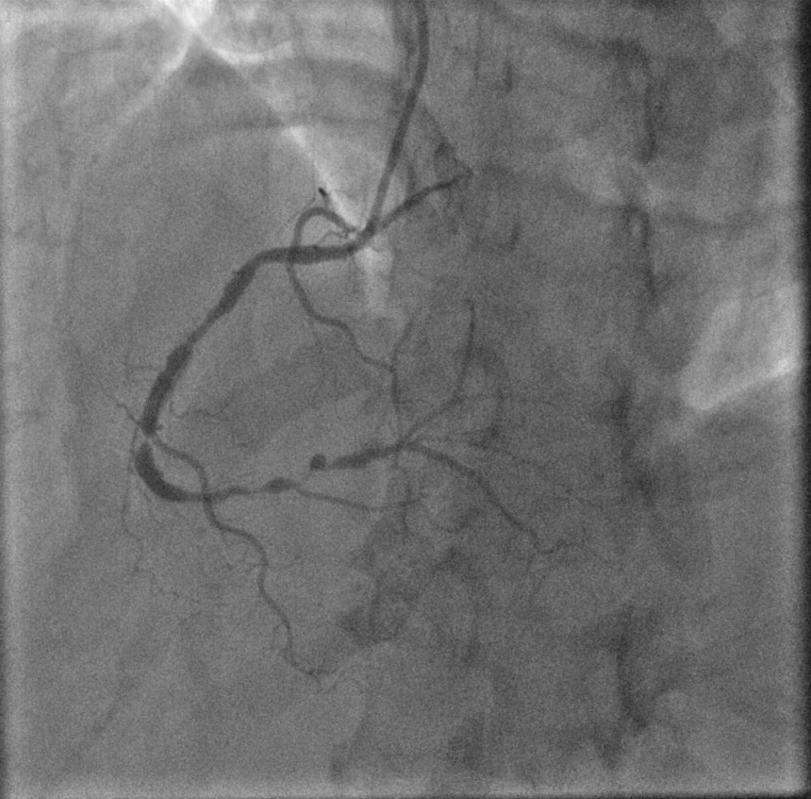
Upon further history taking, her last menstrual period was found to be 32 days ago and a positive beta-human Chorionic Gonadotropin (beta-hCG) confirmed pregnancy with an estimated gestational age of four weeks. After an extensive discussion with the patient, the decision was made to proceed with an invasive coronary angiogram due to an intermediate TIMI risk score of 2 and the presence of recurring rest angina, accepting the risk of exposure to ionizing radiation in the first trimester. Invasive coronary angiogram revealed critical triple vessel disease with 99% stenosis in the mid Left Anterior Descending (LAD) artery (Fig. 2), 95% stenosis in distal Left Circumflex (LCx) artery (Fig. 3), and tandem lesions of 95% in distal Right Coronary Artery (RCA) (Fig. 4).
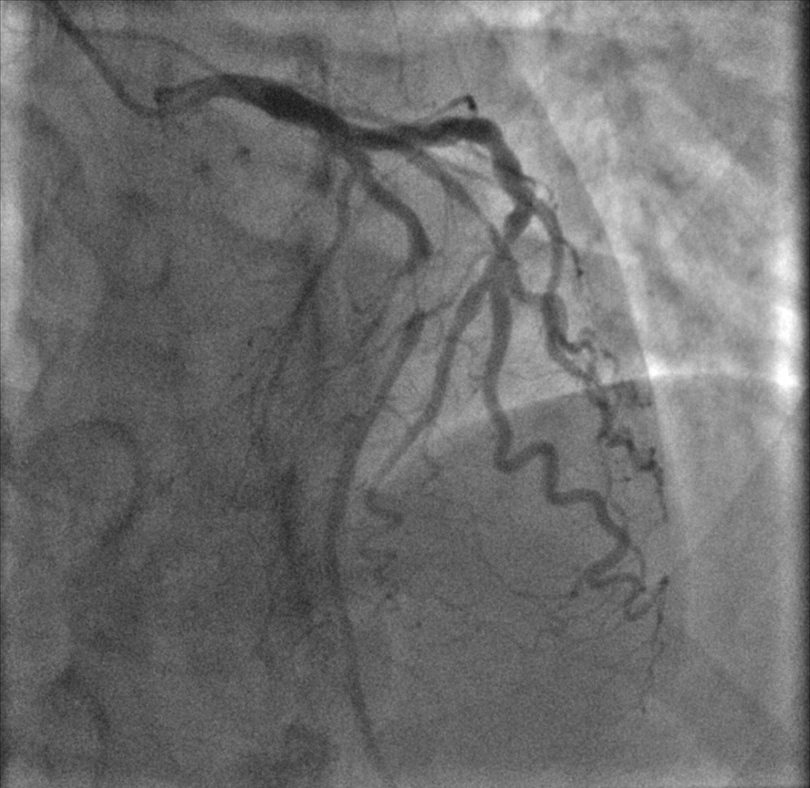 Fig. 2.
Fig. 2.Left anterior descending artery: critical lesion in mid lad.
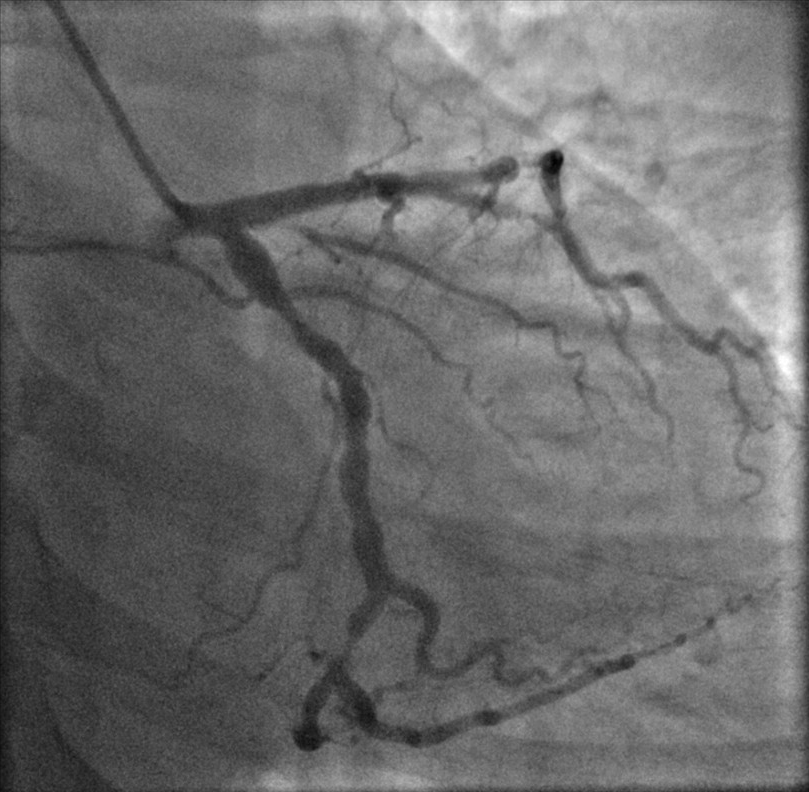 Fig. 3.
Fig. 3.Left circumflex artery: severe stenosis in distal LCx.
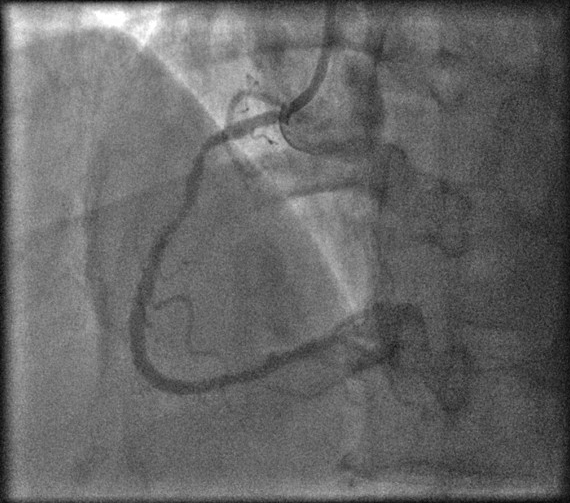
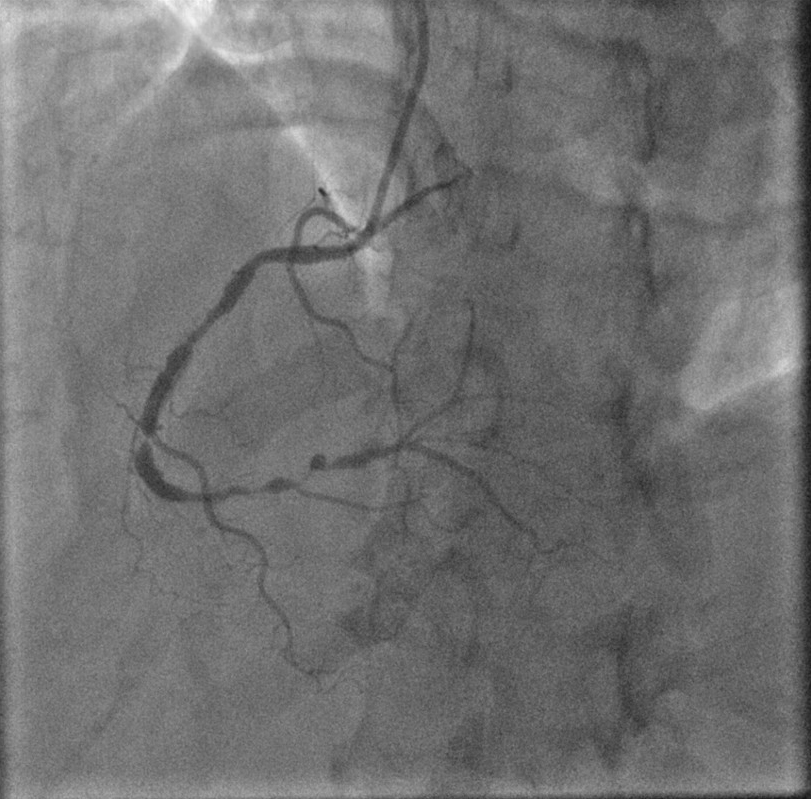 Fig. 4.
Fig. 4.Right coronary artery: critical lesion in mid RCA with critical tandem lesions in distal RCA.
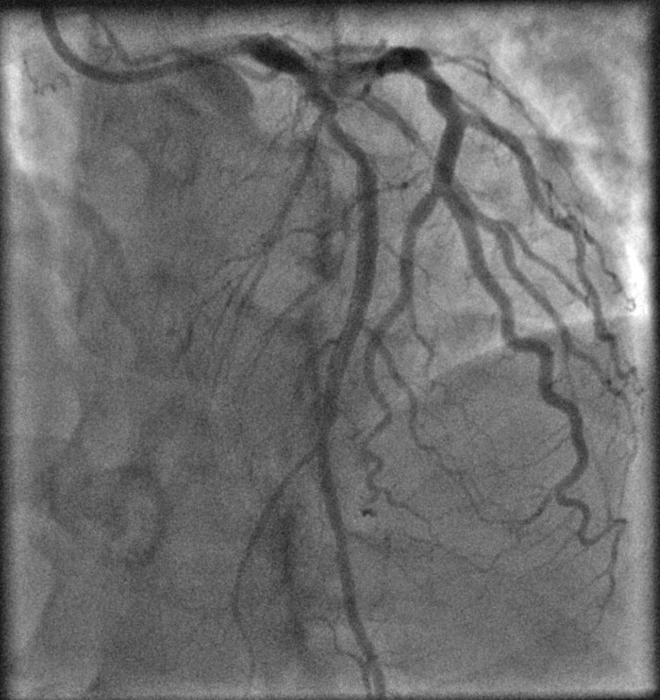
The medical conundrum we now face is that of balancing the risks of maternal and fetal mortality from untreated coronary artery disease against the risks of teratogenicity and miscarriage as a result of radiation exposure during complex multivessel PCI. Surgical coronary artery bypass was also discussed but deemed to be less favorable as SYNTAX Score is low at 14.0 and there were increased surgical risks in view of pregnancy. Thus, a shared decision was eventually made for PCI. We proceeded with PCI with one drug-eluting stent each in the mid LAD and distal LCx (Fig. 5), followed by a staged procedure two days later to mid-distal RCA with implantation of another two drug-eluting stents (Fig. 6). Total radiation used in both procedures was 0.424 Gy, with a combined contrast dose of 190 mL. Precautions were taken during the intervention to minimize radiation exposure to the fetus.
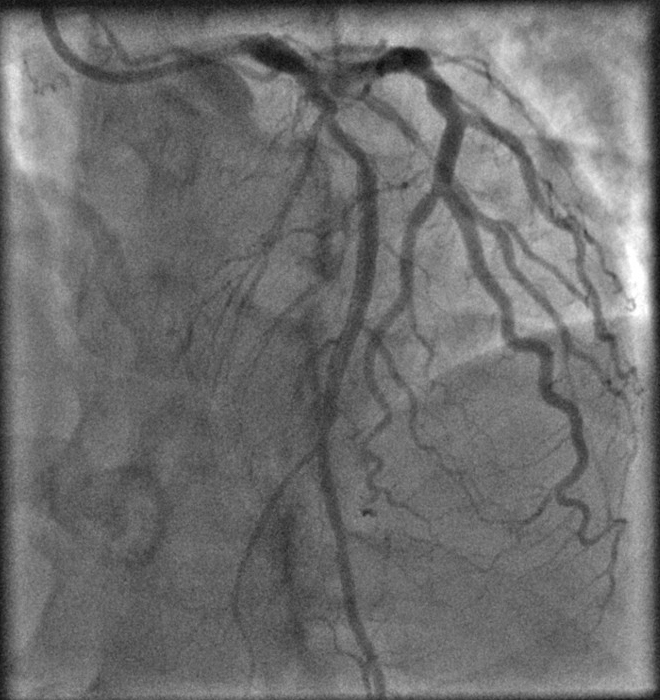 Fig. 5.
Fig. 5.Post PCI to mid LAD and distal LCX.
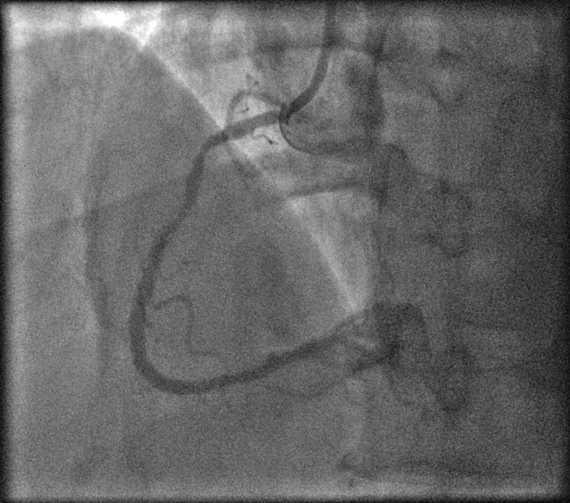 Fig. 6.
Fig. 6.Post PCI to mid-distal RCA.
Medical therapy was optimized with aspirin, clopidogrel and folic acid. ACE inhibitors and beta-blockers were withheld in view of potential harm to the fetus. She was eventually discharged well with early obstetric follow up.
This high mortality rate in ACS during pregnancy can be attributed to physiological changes during pregnancy which includes increased cardiac output, blood pressure, and heart rate with reduced systemic vascular resistance, contributing to an increase in maternal cardiac workload and stress [5]. These are coupled with increased risks of obstetric complications, as high as 58%, including hypertensive disorders, intrauterine growth retardation (IUGR), and prematurity [6]. Both ESC and the American Heart Association (AHA) recommends an early invasive coronary angiogram in patients presenting with NSTEMI with high-risk features such as elevated cardiac markers, recurrent rest angina, cardiogenic shock, and heart failure [4, 7]. This applies in pregnancy as well. However, ionizing radiation has detrimental and irreversible effects on the fetus. During early organogenesis in the first trimester, as in this case report, there is an increased risk of IUGR, teratogenicity, and radiation induced abortion [8]. The American College of Radiology guidelines for imaging women during pregnancy with ionizing radiation [9] stated that in radiation doses beyond 100 mGy in the 5th to 10th week of estimated gestation age, there exists a dose-dependent risk of possible malformation. Thus, there are two main challenges in the management of our patient that we wish to further discuss — (i) Minimization of radiation exposure to the fetus and (ii) considerations for post-PCI pharmacological therapy during pregnancy.
The AHA describes three ways to minimize radiation in the cardiac catheterization laboratory [10]: Justification, optimization, and dose limitation. We applied the same principles in the management of our patient. Rest angina and elevated troponin levels are indicators of high risk NSTEMI, suggesting an elevated risk of new or recurrent myocardial infarction, ischemia or mortality. Considering the above, an invasive coronary angiogram was unarguably beneficial for maternal health, thus justifying the medical decision after discussion with the patient. During the procedure, we sought to reduce radiation exposure through the application of a lead shield on the patient’s abdomen and pelvis. A radiation tag was placed inside the lead apron to monitor exposure radiation. In addition, the procedure was performed by a senior interventionist, with limited angiographic shots in predominantly anteroposterior projection and strict beam collimation for dose limitation. The cinegraphic frame rate was set low at 7.5 frames per second, no magnification and low dose fluoroscopic acquisition was done for the majority of the procedure. Intravascular ultrasound was utilized to study the coronary vessels to aid in the choice of stent and post stent implantation with minimal fluoroscopy time. These measures have demonstrated a significant reduction in total air kerma during PCI [10] so as to minimize potential fetal harm during multivessel PCI.
The benefits of dual antiplatelet agent therapy (DAPT) with aspirin and a P2Y12 inhibitor after PCI for ACS for at least 12 months have been well established in the prevention of ischemic complications and stent thrombosis [7, 11]. Although traditional recommendations state that aspirin should be avoided in the third trimester due to concerns of premature closure of ductus arteriosus and inhibition of uterine contractions via inhibition of prostacyclin, low dose aspirin (60 to 150 mg) has been proven to be safe [12, 13]. Evidence for P2Y12 inhibitors is less robust, and clopidogrel use is controversial as there have been no human studies to suggest the absence of side effects and it is not known whether clopidogrel crosses the placenta. The use of short-acting glycoprotein IIa/IIIb inhibitors is not well studied in pregnancy [4], but has been suggested as a bridge should there be a need for DAPT interruption during the peripartum period for neural anesthesia [2]. Evidence for ticagrelor and prasugrel are also limited and use is not recommended [4]. Thus, the general consensus is for clopidogrel to be used only when strictly indicated and for the shortest duration possible [4].
The morbidity and mortality benefits of beta-blockers and high-intensity statins in ACS treatment have also been well-established [7]. However, these are potentially harmful to the fetus. Both bisoprolol and metoprolol cross the placenta and can cause increased risks of fetal bradycardia and hypoglycemia. Atenolol is not recommended due to increased risks of IUGR, low birth weight, congenital birth defects on top of fetal bradycardia and hypoglycemia [4, 12]. In situations that necessitate the use of a beta-blocker, labetalol has been recommended as the choice of drug in this class based on available data [4, 5]. HMG-CoA reductase inhibitors are contraindicated in pregnancy as they inhibit the synthesis of mevalonic acid, which is essential in DNA replication and hence fetal development [12, 13]. With these concerns, published guidelines have recommended the withdrawal of statins in pregnancy [4].
Considering the limitations above, we started DAPT with aspirin and clopidogrel to decrease the risk of ischemic complications, while withholding beta-blockers and statin therapy for our patient. Oral folate supplementation was started to reduce the risks of neural tube defects [14]. Obstetrics services were consulted throughout the management of this lady.
Management of ACS in women during pregnancy is challenging due to the high incidence of mortality and obstetric complications, on top of the fundamental tradeoffs between maternal and fetal health. There remain many uncertainties on the long-term effects of radiation exposure to the fetus and a holistic management plan needs to consider maternal cardiac health during pregnancy, postpartum period and future family planning. We believe that effective communication with the patient and a multi-disciplinary team including the cardiologist, experienced cardiac interventionist and obstetricians is sine qua non in this process. Enhanced measures should be adopted in the invasive cardiac laboratory to minimize radiation exposure in line with the three principles of justification, optimization and dose limitation.
PJO designed the case report. KXJN, KFCL, CKT performed the literature review and worked on the manuscript. All authors contributed to the editorial changes in the manuscript. All authors read and approved the final manuscript.
All subjects gave their informed consent for inclusion before they participated in the study.
We would like to express our gratitude to all those who have contributed to the care of our patient and helped us in the writing of this manuscript. Thanks to all the peer reviewers for their insightful opinion and suggestions.
This research received no external funding.
The authors declare no conflict of interest.