1 Department of Cardiothoracic Surgery, University of Pittsburgh, PA 15213, USA
2 Department of Medicine, University of Milan, 21022 Milano, Italy
3 Department of Neurology, Mahatma Gandhi Mission Hospital, 400703 New Mumbai, India
4 Department of Anesthesiology, Government Medical College, 143001 Amritsar, India
5 Department of Internal Medicine, Medical College of Wisconsin, Milwaukee, WI 53201, USA
6 Department of Internal Medicine, Central Michigan University, Mt Pleasant, MI 48859, USA
7 Department of Anesthesiology, University of Texas Health Center, Houston, TX 77030, USA
8 Division of Cardiothoracic Surgery, University of Kentucky, Lexington, KY 40506, USA
Academic Editor: Peter A. McCullough
Abstract
Sudden cardiac death (SCD) is an unexpected sudden death due to a heart condition, that occurs within one hour of symptoms onset. SCD is a leading cause of death in western countries, and is responsible for the majority of deaths from cardiovascular disease. Moreover, SCD accounts for mortality in approximately half of all coronary heart disease patients. Nevertheless, the recent advancements made in screening, prevention, treatment, and management of the underlying causes has decreased this number. In this article, we sought to review established and new modes of screening patients at risk for SCD, treatment and prevention of SCD, and the role of new technologies in the field. Further, we delineate the current epidemiologic trends and pathogenesis. In particular, we describe the advancement in molecular autopsy and genetic testing, the role of target temperature management, extracorporeal membrane oxygenation (ECMO), cardiopulmonary resuscitation (CPR), and transvenous and subcutaneous implantable cardioverter devices (ICDs).
Keywords
- Sudden cardiac death
- Sudden cardiac arrest
- Cardiopulmonary resuscitation
- Transvenous and subcutaneous implantable cardioverter devices
- Extracorporeal membrane oxygenation
Sudden cardiac death (SCD) is an unexpected sudden death due to a heart condition, which is almost always confirmed upon post-mortem examination. The unexpected death occurs within one hour of symptom onset and is attributed to a cardiac cause [1, 2]. SCD weighs heavily on the health care system and the lives of many families. It is a leading cause of death in western countries (15-20%) and is responsible for the majority of deaths from cardiovascular disease [3]. However, its incidence is decreasing due to the continued advancement in prevention, treatment, and management. The ever growing use of implantable cardioverter devices (ICDs) has been a major factor in seeing these numbers decline recently [4]. Coronary artery disease (CAD) continues to be the main pathology associated with SCD, however deaths from CAD have notably declined over the past decades. Advances in acute treatment strategies and prevention have driven this decline. Consequently, the incidence of SCD and CAD have been declining in parallel. Increasing knowledge and research is improving our understanding of the mechanisms around the disease (Fig. 1) [5].
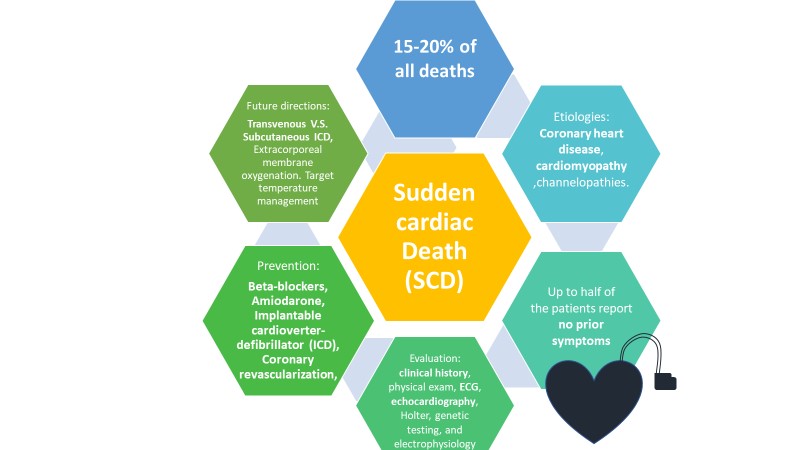 Fig. 1.
Fig. 1.Incidence, Etiology (coronary artery disease, cardiomyopathy, channelopathies, etc.). Prevention (beta-blockers, amiodarone, implantable cardioverter-defibrillator, coronary revascularization) and future directions of treatment for Sudden Cardiac Death.
Each year, approximately 0.1% of the population (in United States and Europe) experience a medical services-assessed, out-of-hospital cardiac arrest [1, 6]. Sudden cardiac arrest (SCA) is more likely to occur in males and between the ages of 66 and 68 [7]. SCD in young athletes is rare but is still a notable cause of death. Early morning and late afternoon show circadian peaks for deaths and Monday is the day of the week with the most deaths [8].
Data from other parts of the worlds is limited, however, it may be fair to predict that the proportion of CAD-related SCD parallels the incidence of CAD mortality as it has been shown in western countries (Fig. 2). This is evidenced in Japan, known for having low incidence and deaths from CAD and hence low SCD rates. Additionally, there is a lot of geographical variation in CAD-related SCD, with possibly high rates in Central Asia, Oceania and Eastern Europe [3].
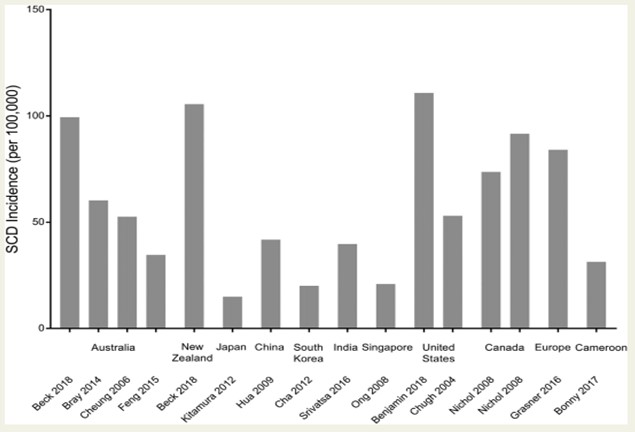 Fig. 2.
Fig. 2.Global incidence of SCD. Incidence demonstrated is from selected studies reporting SCD in all age groups, with the exception of India (Srivatsa 2016; 35 years old) and Cameroon (Bonny 2017; 18 years old). Abbreviation: SCD, sudden cardiac death [3].
Different studies have demonstrated that maximal oxygen uptake (VO2 max), an indicator of cardiorespiratory fitness, is an independent predictor of the risk of SCD [9, 10]. Similarly, exercise-induced ST-segment depression and prolonged QRS duration in resting individuals are predictors of SCD [9, 11]. Other classic independent factors associated with SCD are: smoking, previous myocardial infarction (MI), type 2 diabetes mellitus, body mass index, systolic blood pressure, and C-reactive protein [11]. Interestingly, frequent sauna bathing is associated with a reduced risk of SCD, CVD, and all-cause mortality [10].
Undetected cardiovascular diseases account for the majority of SCD cases [12, 13]. Congenital heart defects causing SCD is more prevalent in younger people [14] whereas, coronary artery disease is the major contributor to SCD cases in individuals over 35 years of age [5]. CAD is involved in 80% cases, making it the most common cause of SCD, while cardiomyopathies and genetic channelopathies are prominent remaining causes [15]. The predominant mechanism of SCD is a form of ventricular arrhythmia (VA). Ventricular arrhythmias are responsible for 84% of SCD. The most common type of ventricular arrhythmias that lead to SCD are VT and VF [16]. Nevertheless, pulseless electrical activity (PEA) and bradyarrhythmia could as well lead to SCD and SCA [17].
At autopsy, coronary artery disease (CAD), hypertrophic cardiomyopathy (HCM) with or without obstruction, and valvular aortic stenosis are the most common causes of SCD. A small percentage of cases, however, show no structural changes (Table 1) [5].
| Age | Primary pathology |
| From birth to 13 years | A congenital abnormality such as Tetraology of Fallot. |
| 14 to 34 years | Hypertrophic cardiomyopathy, arrhythmogenic right ventricular cardiomyopathy, congenital coronary anomalies, genetic channelopathies, myocarditis, Wolff-Parkinson-White syndrome, and Marfan syndrome. |
| Over 35 years | Coronary heart disease. |
SCD accounts for approximately half of all CAD-related deaths, and CAD is thought to be the structural cause of approximately 80% of all SCD. This of course varies for age, gender, race, and ethnicity. In the Oregon SCD Study, CAD was the second most common condition (22%) underlying SCD among subjects aged 5 to 34 years. The spectrum of substrates underlying CAD-related SCD include transient ischaemia, acute coronary syndromes, scar-related pathophysiology, and ischaemic cardiomyopathies [19].
The risk of SCD is greatest in the first month following a myocardial infarction and decreases over time, although those who develop ventricular remodelling and heart failure (HF) have a subsequent increase in risk. However, two-thirds of CAD-related SCD occurs as the first clinical manifestation in supposedly low-risk individuals based on current risk prediction methods, thwarting efforts to reduce the burden of CAD-related SCD [20].
Ischaemic heart disease (IHD) is most commonly due to atherosclerotic CAD. Anomalous coronary arteries with variations in origin or course, are uncommon but are particularly seen in SCDs among athletes. Anomalies with obligate ischaemia (e.g. left main coronary artery arising from pulmonary artery) are rare beyond infancy while those variants without obligate ischaemia but with malignant courses (e.g. between aorta and pulmonary artery) may present in older cohorts [5].
Non-ischaemic cardiomyopathies implicated in SCD include HCM, dilated cardiomyopathy, restrictive cardiomyopathy, arrhythmogenic right ventricular cardiomyopathy (ARVC) and left ventricular non-compaction, a rare cardiomyopathy due to abnormal myocardial formation during early embryogenesis [21, 22]. Approximately 15% of overall SCD occurs in patients with other non-ischaemic structural heart disease in western society. These include dilated cardiomyopathies, HCM, ARVC, infiltrative diseases (sarcoidosis, amyloidosis), myocarditis, and congenital abnormalities. It is clear that SCD caused by non-ischaemic cardiomyopathies is higher in younger populations (15-30% of SCD in under 35’s) [22, 23, 24].
Valvular heart disease causes SCD in two ways; mechanical and arrhythmogenic. New data suggests that severe aortic stenosis poses a risk of 5-7% for SCD. Mitral valve prolapse has long been associated with SCD due to ventricular arrhythmias with an estimated risk of 0.2-1.9% but the incidence is poorly defined [25].
SCD can occur with a structurally normal heart and in these cases, the inherited arrhythmia syndromes are the usual culprits. Genetic mutations in the ion channels of the myocardial cell membrane predispose to malignant arrhythmias and sudden death. The most common cardiac channelopathies are congenitallike long QT syndrome (LQTS), Brugada syndrome, catecholaminergic polymorphic ventricular tachycardia (CPVT), and short QT syndrome (SQTS) [26]. In these cases, the heart is structurally normal, and the pathology is molecular. There are mutations in genes encoding cardiac ion channel proteins. These ion channel diseases increase risk of ventricular fibrillation due to the unstable electrical cardiac activity. In non-structural SCD, clinical screening and genetic testing of family members are important [27].
A detailed post-mortem examination, with molecular biology techniques is essential as the only opportunity for a correct diagnosis according to the guidelines for autopsy investigation of SCD proposed by the Association for European Cardiovascular Pathology [28].
Ventricular fibrillation (VF) is the underlying mechanism in most SCD. The most common cause of VF is acute coronary ischemia whereas increased risk of ventricular tachycardia (VT) commonly occurs in patients with structural heart disease as well as channelopathies [29]. A myocardial scar from a previous infarct is the number one cause of sustained monomorphic VT in patients with structural heart disease. Sudden death in these patients frequently results from VT which eventually leads to VF [29].
Metabolic derangement and oxidative stress particularly during myocardial ischemia may lead to SCD. Impaired myocyte metabolism and increases in reactive oxygen species, lead to malfunction of ionic homeostasis in cardiac myocytes, that in turn cause ventricular tachyarrhythmias and subsequently SCD [30]. Following MI, the major causes of SCD are tachyarrhythmias, re-infarction, and myocardial rupture. Nonetheless, the risk for SCD declines as time passes [31].
Another potential unifying mechanism for SCD is a marked release of catecholamines during the stress response. Massive activation of the sympathetic nervous system leads to alteration in myocyte intracellular calcium handling, which in turn leads to ventricular arrhythmias and subsequent SCD [32]. It has been hypothesized that autonomic nervous system activation during sleep triggers arrhythmias that lead to SCD [18]. In patients with heart failure (HF), in addition to neurohumoral signaling alterations, there is abnormal expression of ion channels, which predisposes patients to ventricular arrhythmias, and consequently to SCD [33]. Animal models have shown downregulation of potassium channels and abnormal regulation of calcium channel in myocytes of a failing heart [34, 35]. It appears that increased sympathetic innervation in failing heart also predisposes patients to arrhythmias [36].
SCD is triggered by a loss of function of one or more of the four vital systems: heart, brain, lungs, and vasculature system. Failure of one of the four causes the cessation in function of the others. For example, in ventricular fibrillation (VF), failure of the heart to circulate blood causes the brain, lungs, and vasculature to fail. In contrast, the collapse of the vascular system may lead to failure of the lungs and brain, as well as to PEA. Similarly, excess anesthesia leading to central nervous system arrest, leads to a pulmonary arrest, followed by vascular and cardiac arrest [37].
SCA often occurs without any warning. SCA and SCD signs and symptoms are immediate and drastic and include loss of consciousness, sudden collapse, pulsesness, and lack of breathing [38]. Reduced cerebral blood flow during SCA causes unconsciousness within seconds. Other symptoms, if present, are nonspecific and include palpitations, chest pains, shortness of breath, and weakness.
Before transportation to a hospital, whenever possible, an automated external defibrillator (AED) should be attached to the patient. Cardiac monitoring using an electrocardiogram (ECG) should begin on arrival of Emergency Medical Services. Once the patient is admitted to hospital, full cardiac assessment should be carried out. A cause should be established while the patient should be further stabilised. Table 2 describe the tests that should be done in survivors of SCA [39].
| Examination | Purpose |
| Electrocardiogram | Diagnosis of ischemic heart disease, Myocardial infarction and inherited channelopathies. |
| Echocardiogram | Can show signs of heart failure, cardiomyopathy, Valvular heart disease and congenital heart disease. |
| Coronary angiography | Evidence of coronary artery disease, congenital abnormalities, and coronary spasms. |
| Exercise test | Can illustrate ischemic heart disease, LQTS and CPVT. |
| Electrophysiology | Detect suspected arrhythmia. Procainamide can provoke Brugada syndrome regardless of the findings on the initial electrocardiogram. |
| Cardiac CMR | To show ARVC, sarcoidosis (fibrotic cardiomyopathy), myocarditis, and myocardial injury from coronary spasms. |
| Genetic testing | If cardiomyopathy, Brugada syndrome, CPVT, or LQTS are found. |
| Cardiac biopsy | Can be considered. |
| ARVC, arrhythmogenic right ventricular cardiomyopathy; CMR, Cardiac magnetic resonance; CPVT, catecholaminergic polymorphic ventricular tachycardia; LQTS, long QT syndrome. | |
Up to half of SCA patients report no symptoms prior to collapse. Some patients report palpitations, dizziness, or near syncope before SCD. Moreover, heart murmurs, heart rate or blood pressure irregularities, or physical stigmata of Marfan syndrome, might be evident [2, 40]. Table 3 summarizes, ceratin findings that might be evident in patients’ medical and family history [2, 40].
| Signs and symptoms in medical history | Common findings in family medical history |
| Exertional symptoms such as dyspnea/fatigue or palpitations. | Premature death or disability before age 50 attributed to heart disease in a relative. |
| Syncope or seizures | Cardiac diseases, such as hypertrophic or dilated cardiomyopathy, channelopathies, Marfan syndrome, or clinically significant arrhythmia. |
| Chest pain/discomfort/tightness/pressure related to exertion related or not related to exertion | Epilepsy or syncope. |
| Intercurrent illnesses and any known cardiac investigations, such as electrocardiogram or cardiac imaging, which must be reviewed where available. | |
| Elevated blood pressure | |
| History of drug use (prescribed or illicit) |
Autopsy in cases of sudden death is essential to determine whether death is caused by cardiac disease or non-cardiac diseases, such as intracranial hemorrhage and pulmonary embolism. Furthermore, an autopsy can determine the mechanism of the SCD: arrhythmic (mostly ventricular fibrillation), or mechanical (i.e. cardiac tamponade, pulmonary thromboembolism, etc.). Therefore, an autopsy is recommended to all cases where SCD is suspected or established [6]. Nonetheless, clinical information, such as gender, age, circumstances of death, past medical history, serum enzymes, and ECG tracing during resuscitation, can also facilitate to determine the cause of death [41].
Standard gross examination of the heart including coronary artery patency assessment and multiple histological samplings are routinely performed. In cases of clinical history or ECG tracing suggestive of an unusual conduction abnormality, it is advised to refer the heart to a specialist center for histological assessment of the conduction system [41].
Toxicology screen, chemistry, and microbiology workup are required to establish a definitive diagnosis, whereas illicit or prescription drug overdose, anaphylaxis, diabetic ketoacidosis, and myocarditis should be excluded as the cause of death (Fig. 3). Genetic testing has an emerging role, particularly in cases of sudden death in children and young adults. Certain genetic diseases causing SCD are associated with structural heart abnormalities, while others could be harder to detect. Many of these genetic conditions are inherited in an autosomal dominant fashion rendering genetic testing an important role in family member risk and screening [18, 41]. Other, non-cardiac causes of death leading to a sudden death include stroke and aortic syndromes - all of which must be considered and ruled out during the post-mortem examination.
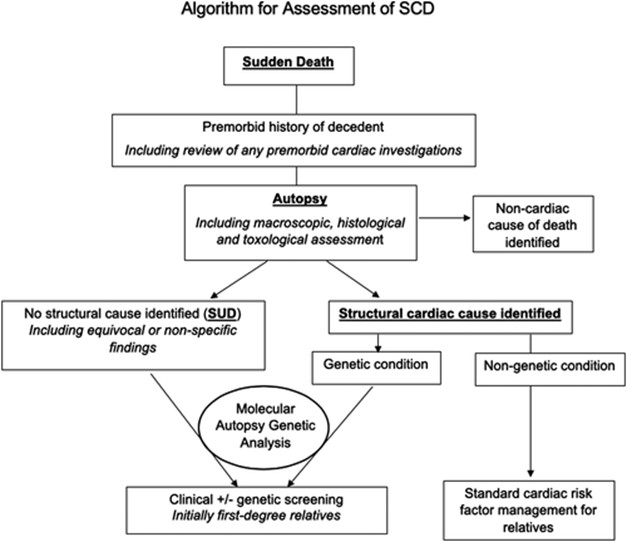 Fig. 3.
Fig. 3.Algorithm for Assessment of SCD [42] includes appropriate Premorbid history of decedent, Autopsy with histological and toxological assessment, molecular and genetic analysis of first-degree relatives as well as identification of structural causes (if any).
The risk of SCD depends on multiple factors and may change markedly over time. Hence, patients have to be monitored continuously with more than one assessment tool. Current guidelines recommend clinical history and physical exam in combination with invasive and non-invasive diagnostic exams to evaluate patients’ risk for SCD. Important factors that should be considered in assessing patients’ clinical history are age, previous documented or symptoms of an adverse cardiac event such as HF, CAD, and sustained or non-sustained ventricular tachycardia. In particular, syncope is an important indicator for further evaluation and management [2, 43]. Risk factors for heart disease, as well as antiarrhythmic medications, medications with potential for QT prolongation, and substance abuse such as cocaine and anabolic steroids should be evaluated. On physical examination, attention should be devoted to heart rate and blood pressure, murmurs, and jugular venous pressure [2, 43].
SCD risk stratification exam can be subdivided into invasive; which mostly consists of electrophysiology (EPS), and noninvasive; 12-leads ECG, image techniques, Holter ECG, high-resolution ECG, and stress test. The EPS utilizes catheters to record the internal cardiac electric activity during induced ventricular arrhythmias. It is mainly used as part of catheter ablation, or if SCA cause is unestablished using other techniques. In the past studies have shown that combining this exam in the screening process might reduce SCD rate in patients with CAD [44, 45]. Nonetheless, EPS reliability in predicting SCD due to ventricular fibrillation or flutter is questionable. Moreover, its negative predictive value is dependent on the ventricular stimulation protocol [45]. In recent guidelines, EPS is not favored over clinical assessment and non-invasive studies, for the risk stratification of SCD [2].
ECG, a widely available exam, can be helpful for the diagnosis of channelopathies and cardiopathies [2]. Moreover, electrocardiogram markers such as microvolt T-wave alternans (MTWA), QRS fragmentation, QRS duration, and signal-averaged ECG, have been demonstrated to correlate with risk for SC [21, 46, 47]. Table 4 summarize ECG markers important for SCD risk stratification. ECG also plays a crucial role in the management of SCA, and MI, hence in the acute prevention of SCD [2].
| Definition | References | |
| Microvolt T-wave alternans (MTWA) | T-wave duration difference between alternate beats at the microvolt level | [21, 46] |
| T-peak–T-end interval | The interval from the peak to the end of the T-wave | [21, 47] |
| QRS fragmentation | Presence of an R’ wave or spikes in the QRS complex. | [21, 47] |
| QRS duration | Duration of the QRS complex | [21, 47] |
Holter or continuous ambulatory electrocardiography are analyzed to detect ventricular extrasystoles, ventricular premature beats, atrial fibrillation, ventricular tachycardia (VT), as well as T wave alternans, heart rate turbulence, or heart rate variability indices, whose alterations can promote ventricular arrhythmias. Ambulatory electrocardiography is recommended for 24 hours for symptomatic patients [2].
Echocardiography enables the assessment of cardiac structures such as cardiac
valves, diagnose cardiomyopathies as well as evaluate left ventricular ejection
fraction (LVEF). A study aimed to evaluate the echocardiography predictor
parameter of SCD found that not only reduced LVEF, but also mitral annular
calcification, mitral E/A
Genetic testing have also found their way into the screening and risk stratification of SCD. It is recommended for patients and family members of patients with channelopathies and cardiomyopathies [2, 6]. The genetic contribution to SCD susceptibility can be divided into genetic variants that are associated with known inherited cardiac disorders, and genetic variants contributing to susceptibility to SCD but are not associated with a known cardiac disorder or ECG pattern. Nonetheless, genetic testing can confirm the diagnosis of the inherited arrhythmic syndrome, which are usually diagnosed with clinical and familiar history.
KCNQ1 and KNCH2 genes encode for the slowly activating delayed rectifier current (IKs) and for rapidly activating delayed rectifier current (IKr), respectively. SCN5A encodes a subunit of the voltage-gated sodium channel Nav 1.5. Mutations in these genes may lead to LQTS and were associated with SCD [50]. Furthermore, different KCNQ1 and KNCH2 may lead to short-QT Syndrome and increased risk for SCD [51]. SCN5A, CACNA1C, and CACNB2B (genes encoding the CaV1.2 L-type calcium channel subunits) mutation are associated also with Brugada syndrome [52].
CPVT (catecholaminergic polymorphic ventricular tachycardia) is a heritable arrhythmia syndrome, in which patients often have normal baseline ECG. But during physical activity or emotional stress, patients might experience, bidirectional or polymorphic VT. Mutation in the ryanodine receptor (RyR2), which is a calcium channel that regulates calcium ion release from the sarcoplasmic reticulum, is founded in 60% of patients with CPVT [53, 54].
Mutations in MYBPC3 or MYH7, that encode sarcoplasmic proteins are one of the genetic causes of the majority of HCM cases, carries risk for SCD [55].
Genome-wide association studies (GWAS) provided new biological insight about the genetic association to SCD. Instead of a specific mutation, GWAS illuminates a haplotype association with SCD. A meta-analysis of GWAS data identified a locus (BAZ2B) that is likely to be involved in gene regulation correlated to SCD risk [56].
A survey from 2015 aimed to assess how screening and risk evaluation of patients with risk of SCD was performed in European centers. This survey indicated that in patients with CAD and low LVEF the vast majority of centers considered the ECG and exercise capacity assessment to be fundamental for SCD risk stratification. For patients with HCM or patients with a family history of HCM-related SCD, history of unexplained syncope or non-sustained VT, low blood pressure during exercise, and extreme left ventricular hypertrophy were the major clinical risk factors [57].
Prevention of SCD is the main goal in management, since the overall survival rate of out of hospital cardiac arrest, and consequently SCD, is estimated to be 10% [58]. Therefore targeting individuals at high risk is the main priority as well as initiating appropriate preventive measures.
Except for quinidine, mexiletine, and flecainide for Brugada syndrome, LQTS, and CPVT sodium channel blockers are not recommended for SCD prevention [59, 60]. CAST I and CAST II are two clinical trials aimed to examine the sodium channel blockers’ anti-arrhythmic ability to prevent SCD. Both studies were prematurely terminated for excess mortality due to arrhythmias [61, 62]. Similarly, non dihydropyridines calcium channel blockers have no role in SCD prevention [6]. On the other hand, beta-blockers, and to a smaller degree amiodarone, are beneficial in the prevention of SCD. Beta-blockers have shown to reduce the mortality, not only of patients with HF and CAD, but also to reduce SCD and ventricular arrhythmias (VA) incidents [63, 64, 65]. Moreover, beta-blockers are also the first-line therapy for previously mentioned channelopathies (e.g. long e.g. QT syndrome) [6]. Intravenous amiodarone is indicated in reducing VA recurrence during resuscitation and hence preventing SCD [2]. However, due to its variety of adverse effects and interactions, it failed to provide strong benefits over a long period of prescription. Even if it reduced SCD risk and cardiovascular death, the overall mortality is not reduced [66]. For this reason, periodical monitoring of thyroid, liver, and lung function are recommended when prescribed for longer periods [2]. Sotalol, which offers beta-blocking activity with amiodarone-like action, has a pro-arrhythmic effect which prevents it from being used in patients’ post-MI or with HF [6, 67]. Hence, its role in the prevention of SCD and SCA is limited.
A combination of antiarrhythmic drugs is recommended in specific cases when other modalities, such as catheter ablation or ICD, have failed [6]. For example, in patients with drug-refractory VT, Ranolazine has been combined with other anti-arrhythmics such as amiodarone or sotalol, with encouraging results [68]. A more frequent approach is prescribing beta-blockers, or less frequently sotalol, to the patient with an ICD to meliorate their control [6, 69].
Another aspect in the prevention of SCD is the treatment of underlying cardiac disease and comorbidities. For instance, in a patient with HF it is important to reduce myocardial oxygen consumption and sympathetic tone to reduce the risk for SCDs. Therefore, beta-blockers, angiotensin-converting enzyme inhibitors or angiotensin-receptor blockers, mineralocorticoid-receptor antagonists, and angiotensin receptor-neprilysin inhibitors are recommended for SCD prevention [70, 71]. Similarly, myocardial infarction patients should receive optimal medication as well (including beta-blockers, dual antiplatelet therapy, and statins) for reducing SCD risk [6]. Furthermore, addressing electrolytes disturbance, especially potassium and magnesium, in patients post-MI and with HF reduces SCD risk [6, 72].
ICDs continuously monitor heart activity and are effective in terminating life-threatening VA. To this date, the mainstay of SCD prevention is ICD. Indication for ICD can be grouped as primary prevention and secondary prevention. Primary SCD prevention, targets patients with no clinical history of ventricular arrhythmias, but are at high risk for SCD. While secondary prevention targets patients who survived SCA. Both groups of patients are evaluated with the tools discussed before, to determine the need for an ICD. A five year followup comparing ICD in patients with primary and secondary indications demonstrated comparable mortality in both groups. Nevertheless, it appears that patients with secondary indications had more incidents of VA that were terminated by ICD [73].
While in most cases ICD is recommended for secondary prevention, primary prevention indications are more complicated. Nevertheless, patients of both groups require more than 1 year of life expectancy and non-reversible VA etiology (such as electrolytes abnormality) to be eligible for ICD [2, 6, 57]. For instance, ICD is recommended only after 40 days post-MI or at least 90 days post revascularization, based upon the belief that left ventricular function can improve following these events, and consequently SCD risk will decrease [74]. In addition, ICD indications are based on LVEF and HF symptoms as classified in NYHA classification (Table 5) [2].
| ICD indication according to LVEF and HF symptoms [2] | |
| LVEF | NYHA classification |
| NYHA class II or III symptoms | |
| NYHA class I | |
| Patients with LVEF | |
| Patients with IHD, unexplained syncope and inducible sustained VT on EPS | |
| EPS, electrophysiological study; HYHA, New York Heart Association classification; LVEF, left ventricle ejaculation fraction; VF, ventricle fibrillation; VT, ventricle tachycardia. | |
Transvenous ICD (T-ICD) is most widely used, and it is beneficial for patients with a life expectancy of more than 1 year, related complications are inappropriate shock and device-related infections [75]. Subcutaneous ICD (S-ICD) is an alternative for T-ICD. It should be considered in patients unfitted to T-ICD, due to inability to access the vascular system when pacing therapy for bradycardia support, cardiac resynchronization, or when anti-tachycardia pacing is not needed [54, 76]. Another alternative is an external ICD (a wearable pads and electrodes). This devices efficiency hasn’t been validated yet, hence it is recommended only as a temporary solution, bridging for cardiac transplant or T-ICD implantation [6].
However, two clinical studies might change the perception that S-ICD is only indicated for the patients who are found to be unfitted for T-ICD. The PRAETORIAN trial that enrolled 876 patients who randomly received either an S-ICD or T-ICD, and were followed up for about 4 years, and UNTOUCHED trial a prospective non-randomized study that followed 1116 patient who received S-ICD, for 18 months. The PRAETORIAN study found that S-ICD was equivalent to the T-ICD with respect to device-related complications and inappropriate shocks rates. Furthermore, the rates of SCD were equal in both S-ICD and T-ICD groups. Similarly, the UNTOUCHED study demonstrated high S-ICD efficacy and safety [77, 78].
While ICD can terminate VA, it cannot prevent VA from reoccurring like catheter ablation can accomplish. Catheter ablation is particularly valuable for patients with scar tissue related to VF or VT [79]. In patients with no structural heart abnormalities, VT is most commonly monomorphic and typically originate from one focal point, commonly at the ventriclar (right or left) outflow tract. On the other hand, in patients with structural heart disease, VT is more commonly due to scar tissue reentry mechanism, and on ECG their VT is also monomorphic (Polymorphic VT is more likely due to acute MI or channelopathies). The procedure is more effective in patients without structural heart abnormalities than patients with structural heart abnormalities. However, 22% of patients without structural heart abnormality and 15% of the patients with structural heart abnormality will require repeated ablation [80]. Common procedural complications are correlated to access sites, such as groin hematoma and pseudoaneuysm [80].
When dealing with acute cardiac arrest, time is key. Survival decreases from 25% after 4-5 minutes to 0% after 10 min [81]. According to the American Heart Associaiton, in patients with ventricular arrhythmias with hemodynamic instability, defibrillation should be performed as quickly as possible, while cardiopulmonary resuscitation (CPR) is used until a perfusing rhythm is restored [2]. In out-of-hospital cardiac arrest, CPR should be performed immediately until the defibrillator is available, unlike in-hospital cases in which defibrillation should occur first [6]. If the patient remains arrhythmic after 3 shocks, amiodarone should be administered [2]. On the other hand, an ECG should be obtained for stable patients, as well as perfusion, and respirations should be assessed [2, 6]. Post-resuscitation care includes, vital-organ support, targeted temperature management and exploring underlying cause.
According to the American Heart Association guidelines, patients with sustained VA and survivors of SCA should be evaluated for ischemic heart disease, and should be revascularized as appropriate [2]. It appears that although revascularization improves survival, there is no difference between coronary artery bypass graft or percutaneous coronary intervention (PCI) in the prevention of SCD [82, 83]. Moreover, it appears that survival and neurological outcomes are better for patients who underwent coronary angiogram in the first 24 hours after regaining spontaneous circulation (ROSC) [84].
However, the Coronary Angiography after Cardiac Arrest Trial (COACT), a randomized clinical trial that included 552 patients, showed there was no significant difference in clinical outcomes at 1 year between patients in the immediate angiography group compared with patients whose angiography was delayed until after neurologic recovery. Survival at 1 year was 61.4% in the immediate group versus 64.0% in the delayed group [85].
Targeted temperature management (TTM), also known as induced hypothermia, is
shown to be beneficial for improving outcomes in patients post-resuscitation. It
can be delivered by several methods: surface cooling ranges from ice packs and
cooling pads to air mattresses, while internal cooling includes specialized
endovascular heat-exchange catheters and intravenous fluids [86]. A large
randomized controlled trial from 2013 aimed at determining the most beneficial
temperature demonstrated no difference in outcomes when using 33
As mentioned previously, coronary angiography is part of the post-cardiac arrest evaluation. A recent retrospective cohort study from Taiwan demonstrated increased survival and neurological outcome in patients who underwent coronary angiography in the first 24 hours, as well as TTM [84].
For survivors of SCA, factors associated with poor neurological outcomes for
out-of hospital cardiac arrrest include advanced age, unwitnessed arrest, no
bystander CPR, time to achievement of ROSC
Hypertrophic cardiomyopathy (HCM) is the most common cardiac abnormality
implicated in SCD in young athletes
As mentioned previously, once a patient is experiencing SCA, CPR should be done to prevent SCD. Nonetheless, CPR efficiency decreases with time, and after 20 minutes of CPR the survival probability decrease by ten times [92]. Therefore, new methods are being explored to improve this aspect in patient care.
As discussed previously, chest compressions as part of CPR are essential in the management of cardiac arrest. Nevertheless, the quality of manual chest compression during CPR may be impaired by CPR provider fatigue and by ambulance movement [93, 94]. To overcome these issues, devices that provide mechanical chest compressions (MCC) have been recently introduced. These devices can be subdivided into three categories: point compression, load distribution compression, and full chest compression. Recent meta-analyses found no advantage of these devices over manual CPR compression, in the reduction of SCD rate, as well as long term mortality and complication of SCA [95, 96]. LUCAS (Lund University Cardiopulmonary Assist) device is commonly used device for this purpose.
In the survival of chain for out-of-hospital cardiac arrest, the goal of CPR is
to establish ROSC so as to provide end-organ perfusion and prevent secondary
brain damage. Recently, insertion of venoarterial extracorporeal membrane
oxygenation (VA-ECMO) during CPR to rapidly provide circulatory support termed
extracorporeal cardiopulmonary resuscitation (eCPR) has been tried especially in
younger patients who do not achieve ROSC after 10-15 minutes of CPR. It is a very
resource-sensitive strategy, performed only by few experienced centers and cannot
be applied to all SCA patients. Napp et al. [97] analyzed 40 patients
with refractory OHCA and potentially favorable circumstances who underwent eCPR.
Overall 30-day survival was 12.5%, with 3 of 5 survivors having a favourable
neurological outcome. No patient selected for eCPR met all pre-defined criteria.
Importantly, time-to-ECMO most often exceeded 60 minutes (mean 102
PCI in patients undergoing CPR after sudden cardiac arrest can be used as a part of the resuscitation effort to address the underlying cause. CPR can be done manually, with mechanical chest compression or utilising ECMO. A retrospective analysis from 2017, showned that MCC provides a better outcome than manual CPR in the catheterization lab [98]. In another study, ECMO when combined with PCI for patients in cardiac arrest was associated with favorable outcomes [99]. Hence, new approaches suggest incorporation of mechanical chest compression, ECMO, TTM, and early reperfusion in the management of SCA [100, 101].
While definitinve treatment of individual underlying cause of SCD are beyond the scope of this review, a few need worth mentioning. Patients with hypertrophied cardiomyopathy should be treated with septal ablation or alcohol injection procedures. Similarly, patients with severe aortic stenosis require relief of outflow tract obstruction with some form procedure including balloon aortic valvotomy, transcatheter aortic valve replacement depending upon their ability to tolerate these procedures. Additonally, survivors of acute pumonary embolism need definitive treatment using procedure like transcatheter guided thrombolysis (EKOS) or pulmonary thromboendarterectomy utilizing cardiopulmonary bypass support [102].
SCD remains a prominent cause of death. Both congenital heart disease and heart failure appear to be the important causes, hence, treatment of these underline conditions and optimizing the cardiac function is essential in the prevention of SCD. Genetic testing and MRI are promising modalities in patients’ screening and risk stratification whereas T-ICDs are widely used in the prevention of SCD. Strategies such as targeted temperature management, mechanical chest compressions, eCPR and PCI during CPR, show promise and will need further validation.
ARVC, arrhythmogenic right ventricular cardiomyopathy; CAD, coronary artery disease; CHD, coronary heart disease; CMR, cardiac magnetic resonance; CPR, cardiopulmonary resuscitation; CPVT, catecholaminergic polymorphic ventricular tachycardia; ECG, electrocardiogram; ECMO, extracorporeal membrane oxygenation; EPS, electrophysiology; GWAS, genome-wide association studies; HCM, hypertrophic cardiomyopathy; HF, heart failure; ICDs, implantable cardioverter devices; IHD, ischaemic heart disease -some font’s are different; LGE, late gadolinium enhancement; LQTS, long QT syndrome; LVEF, left ventricular ejection fraction; MCC, mechanical chest compressors; MI, myocardial infarction; MTWA, microvolt T-wave alternans; PCI, percutaneous coronary intervention; PEA, pulseless electrical activity; SCA, sudden cardiac arrest; SCD, sudden cardiac death; SQTS, short QT syndrome; S-ICD, subcutaneous ICD; TTM, targeted temperature management; T-ICD, transvenous ICD.
AK, NS and SK conceived and designed the paper; RK, AKi and NS did the literature search; AK, DMA, CRJ, JDS and NS wrote the paper; AKi, NS and SK supervised the work and did the critical appraisal.
We would like to acknowledge Dr. Punnoose for her expertise and help in editing the manuscript. Also, we would like to thank Dr. Malke Asaad and Connecting Researchers for their input.
This research received no external funding.
The Authors have nothing to disclose with respect to this submission.



