1 Department of Child, Adolescent Health and Maternal Care, School of Public Health, Capital Medical University, 100069 Beijing, China
2 Department of Hematology, Beijing Friendship Hospital, Capital Medical University, 100032 Beijing, China
3 UNESCO Chair on Global Health and Education, Peking University, 100083 Beijing, China
4 Beijing Key Laboratory of Environment and Aging, Capital Medical University, 100069 Beijing, China
†These authors contributed equally.
Abstract
Suboptimal hydration status has increasingly been recognized as a risk factor for the progression of chronic diseases. A nationwide survey conducted in China found that 82% of children aged 6 to 17 years failed to meet the recommended daily total water intake of 1600–2500 mL. On average, boys consumed 1603 ± 731 mL per day, while girls consumed 1487 ± 661 mL per day, placing them at a higher risk of dehydration. Worldwide studies have suggested associations between dehydration and chronic kidney disease, steatotic liver disease, and cardiovascular diseases in adults. However, there is a lack of evidence concerning hydration status and target organ damage in the pediatric population. Only a limited number of studies have suggested that suboptimal hydration status is associated with transient renal impairment, an increased risk of metabolic dysfunction-associated steatotic liver disease (MASLD), and decreased ventricular structure and function in children. This article reviews the association between hydration status and target organ damage in both adult and pediatric populations and summarizes tailored water intake recommendations for Chinese children. We aim to advance research on hydration status and kidney, liver, and cardiovascular health, especially in the pediatric population.
Keywords
- hydration status
- dehydration
- target organ damage
- kidney
- liver
- cardiovascular
- healthy drinking recommendations
Water is a vital nutrient required in large quantities and plays a critical role in human physiology, essential for growth, development, and overall health maintenance [1]. Body water percentage decreases with age, constituting approximately 80% of body weight in newborns, 70% in infants and toddlers, and gradually declining to 60–70% by the age of 12 [2]. Adequate water intake is essential for maintaining the osmotic pressure and electrolyte balance in the body, especially in regulating sodium (Na+) and potassium (K+) levels [3]. Additionally, water facilitates crucial biochemical processes (such as glycolysis, the citric acid cycle, and oxidative phosphorylation) in intracellular and extracellular environments, and helps preserve the structural integrity and functional efficiency of various tissues, organs, and systems [3]. Age- and sex-specific recommendations for adequate water intake have been developed by the World Health Organization (WHO), China, the United States, and the European Food Safety Authority [4]. Specifically, the daily total water intake (TWI) for boys aged 4–17 years ranged from 1.6 L to 3.3 L, while for girls it ranged from 1.6 L to 2.3 L [4]. Disruption in water balance, such as dehydration, can lead to organ dysfunction and even target organ damage due to oxidative stress and inflammatory responses triggered by the activation of the renin-angiotensin-aldosterone system (RAAS), arginine vasopressin (AVP), and the aldose reductase-fructokinase (AR-F) pathway [5, 6, 7, 8]. Emerging evidence underscores the role of healthy lifestyles, including a balanced diet, sufficient physical activity, and adequate sleep, in preventing chronic non-communicable diseases and adverse health outcomes [9, 10]. As an important component of healthy lifestyles, adequate water intake and optimal hydration status have garnered increasing attention regarding their impact on health [7, 8].
This narrative review is conducted to summarize the studies on the association between hydration and various target organ damage in adults and children, and the tailored water intake recommendations for Chinese children. We aim to offer empirical evidence and practical guidance on the role of hydration status in promoting health and preventing chronic diseases. Current studies consistently identify suboptimal hydration status as a significant risk factor for target organ damage [11, 12, 13], as briefly summarized in Table 1 (Ref. [14, 15, 16, 17, 18, 19, 20, 21, 22, 23, 24, 25, 26, 27, 28, 29, 30, 31, 32, 33, 34, 35, 36, 37]) and Fig. 1. However, studies on hydration status and health remain limited, particularly in the pediatric population. Large-sample population studies are needed utilizing adequate water intake interventions and accurate measurements of hydration status and adverse health outcomes to inform causal inferences.
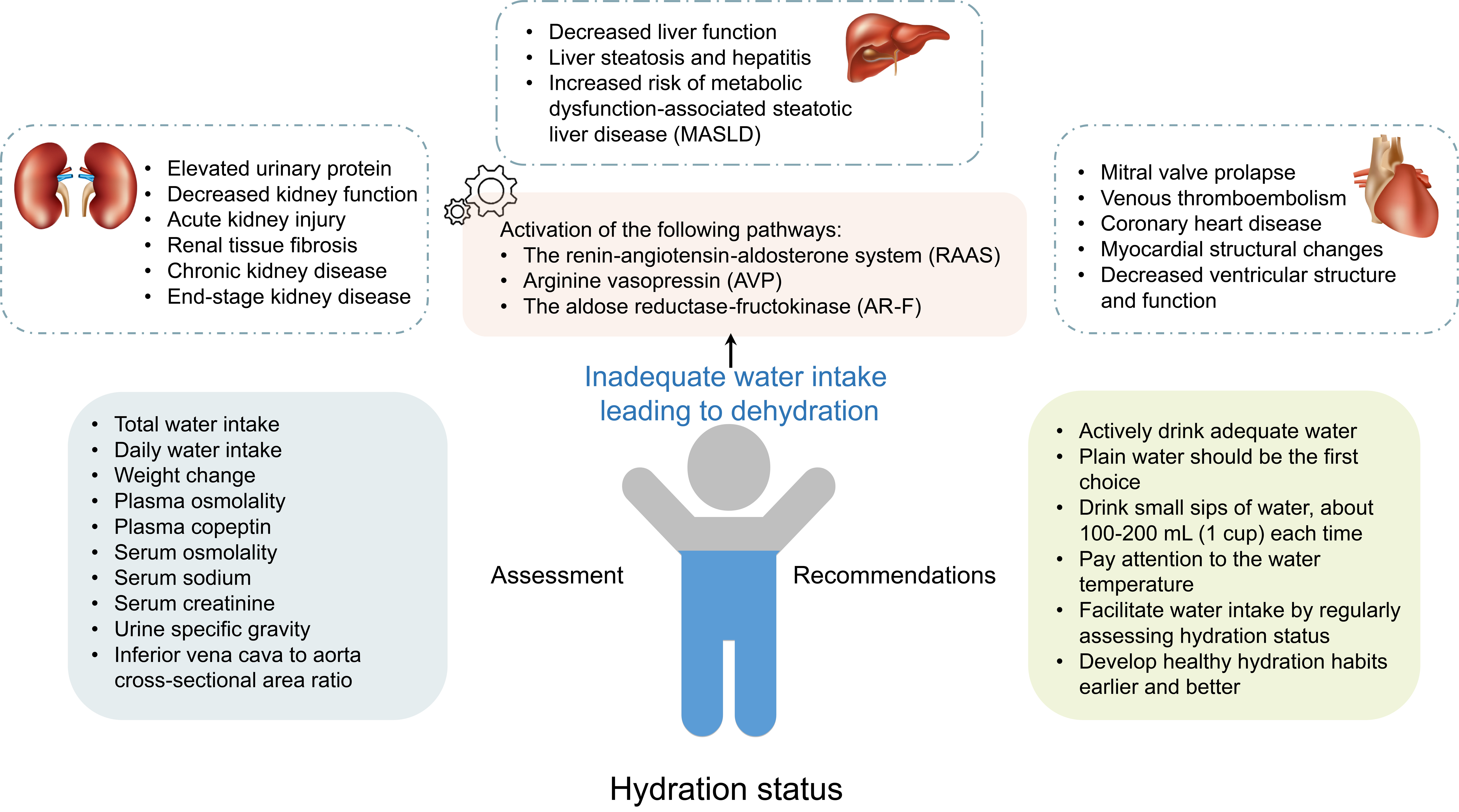 Fig. 1.
Fig. 1.
Hydration status assessment, risks and mechanisms of dehydration-associated kidney, liver, and cardiovascular damage, and water intake recommendations.
| Population | Study type | Hydration status assessment | Adverse health effects | Publication year |
| Kidney | ||||
| Adult | Cross-sectional study | Total water intake | Decreased kidney function/chronic kidney disease [14] | 2013 |
| Adult | Cross-sectional study | Weight change | Decreased kidney function [15] | 2015 |
| Adult | Cohort study | Serum sodium | Decreased kidney function/chronic kidney disease [16] | 2017 |
| Adult | Experimental study | Weight change | Decreased kidney function/kidney injury [17] | 2018 |
| Adult | Cohort study | Dehydration/weight change | Acute kidney injury [18] | 2019 |
| Adult | Cross-sectional study | Plasma osmolality | Urinary protein level/renal tissue fibrosis and sclerosis/end-stage kidney disease [19] | 2020 |
| Adult | Experimental study | Weight change | Kidney injury [20] | 2021 |
| Adult | Cohort study | Serum creatinine | Incident kidney injury [21] | 2022 |
| Pediatric | Cohort study | Urine specific gravity | Elevated urinary protein/transient renal impairment [22, 23, 24] | 2022, 2024 |
| Liver | ||||
| Adult | Crossover study | Weight change | Decreased liver function [25] | 2001 |
| Adult | Cross-sectional study | Plasma copeptin | Liver steatosis and hepatitis [26] | 2019 |
| Adult | Experimental study | Inferior vena cava to aorta cross-sectional area ratio (IVC/Ao) | Liver tissue changes [27] | 2021 |
| Pediatric | Cohort study | Urine specific gravity | Increased risk of incident MASLD [28] | 2023 |
| Cardiovascular | ||||
| Adult | Observational study | Dehydration/weight change | Mitral valve prolapse [29, 30] | 1992, 1995 |
| Adult | Cohort study | Daily water intake | Increased coronary heart disease risk [31] | 2002 |
| Adult | Observational study | Serum osmolality | Increased risk of venous thromboembolism [32] | 2004 |
| Adult | Cohort study | Serum sodium | Increased coronary heart disease risk [33] | 2015 |
| Adult | Observational study | Weight change | Reduced stroke volume/cardiac output [34] | 2020 |
| Adult | Experimental study | Weight change | Myocardial structural changes [35] | 2020 |
| Adult | Meta-analysis | Total water intake | Decreased cardiovascular performance [36] | 2023 |
| Pediatric | Observational study | Weight change | Decreased ventricular structure and function [37] | 2011 |
Abbreviations: MASLD, metabolic dysfunction-associated steatotic liver disease.
Recent studies underscored the importance of hydration status on kidney function
and health. In the adult population, data from the 2005–2006 National Health and
Nutrition Examination Survey (NHANES) indicated an association between low water
intake and chronic kidney disease (CKD), suggesting a protective role of adequate
water intake in maintaining kidney health [14]. A cross-sectional study conducted
in Central America among 189 sugarcane workers found that repeated dehydration
can lead to kidney damage, as indicated by 14% of participants exhibiting
decreased kidney function (estimated glomerular filtration rate [eGFR]
Several population studies examined the impact of hydration status on liver and metabolic health. In the adult population, a crossover study conducted in Denmark on the acute effects of moderate dehydration in healthy adult males found that dehydration led to a 25% reduction in functional hepatic nitrogen clearance and impaired urea synthesis [25]. In Italy, a cross-sectional study compared plasma copeptin levels among obese individuals with and without non-alcoholic fatty liver disease (NAFLD) and healthy non-obese individuals, reporting that obese NAFLD patients had significantly higher plasma copeptin levels, which positively correlated with the severity of hepatic steatosis, lobular inflammation, and non-alcoholic steatohepatitis [26]. In the United Kingdom, an experimental study involving twelve healthy adults observed that suboptimal hydration status (assessed by the inferior vena cava to aorta cross-sectional area ratio) shortened liver T1 relaxation time measured via liver tissue imaging [27]. In the pediatric population, the PROC study suggested that suboptimal hydration status may increase the risk of incident metabolic dysfunction-associated steatotic liver disease (MASLD, updated definition of NAFLD in 2023). The study observed that children transitioning from euhydration to dehydration or consistent with dehydration presented higher incidence rates of MASLD over a 4.5-year follow-up period [28]. In summary, these studies underscore the importance of maintaining optimal hydration status for liver health and highlight the risks associated with dehydration, including impaired urea synthesis, and the development and progression of liver diseases such as MASLD.
Extensive research conducted over decades has consistently demonstrated the significant impact of hydration status on cardiovascular health. In the adult population, two early studies observed that mild dehydration induced by furosemide led to mitral valve prolapse, and prolapse-associated murmurs or echocardiographic changes improved upon rehydration, highlighting the impact of dehydration on cardiac structure [29, 30]. Another large-scale prospective cohort study in the United States involving 20,297 participants without pre-existing heart disease, stroke, or diabetes found that higher water intake (5 glasses or more, 240 mL/glass) was associated with a decreased risk of fatal coronary heart disease [31]. In the United Kingdom, a prospective observational study involving 102 patients with acute ischemic stroke found that elevated serum osmolality, urea levels, and the urea-to-creatinine ratio after stroke were associated with an increased risk of venous thromboembolism [32]. A community-based prospective cohort study in the United States, involving 12,779 participants, found a positive association between serum sodium concentration and the ten-year risk of coronary heart disease [33]. Furthermore, an interventional trial involving 12 healthy adult males reported no significant changes in cardiovascular function indicators after exercise under various hydration conditions, indicating limited impact of exercise or dehydration on myocardial contractility or function [38]. However, a similar study in the United Kingdom observed that dehydration reduced stroke volume and cardiac output during exercise due to impaired cardiac filling and venous return, rather than affecting left ventricular function [34]. In Germany, an observational study among healthy adults found that dehydration significantly reduced myocardial T1 and T2 relaxation times, suggesting that hydration status affects myocardial structure [35]. A meta-analysis on hydration status in relation to heart rate, heart rate variability, and blood pressure during exercise found that optimal hydration reduced exercise-induced heart rate increases and improved heart rate variability after exercise [36]. In the pediatric population, a study involving Iranian adolescent wrestlers showed that a 3.4% weight loss due to dehydration affected cardiac structure and function, evidenced by changes in electrocardiogram and echocardiogram parameters [37]. In summary, these studies emphasize the association between dehydration and cardiovascular structural changes, and the increased risk of cardiovascular diseases.
Optimal hydration status is crucial for maintaining physiological functions and
health, and adequate water intake recommendations have been established by the
WHO, the United States, and the European Union [4]. In China, water intake
recommendations for adult and pediatric populations have been outlined in the
Chinese Dietary Reference Intakes, both in 2013 and the
updated version in 2023 [39, 40]. Despite these guidelines, inadequate water intake
remains common among children and adolescents. A national survey on Chinese
children’s drinking behavior reported that the average TWI for boys aged 6 to 17
years was 1603
According to China’s dietary guidelines, the adequate intake (AI) of total water, including water from beverages and water from food, varies by age and sex: for children aged 6–11 years, it is 1800 mL/day (with 1000 mL drinking water from beverages); for adolescents aged 12–14 years, the AI is 2300 mL/day for males and 2000 mL/day for females, with drinking water contributing 1300 mL/day and 1100 mL/day, respectively; and for those aged 15–17 years, the AI increases to 2500 mL/day for males and 2200 mL/day for females, with 1400 mL/day and 1200 mL/day from drinking water, respectively.
Plain water refers to various types of drinking water, including tap water, filtered and purified water, boiled water, bottled water, packaged drinking water, natural mineral water, and spring water. Unlike sugar-sweetened beverages, plain water contains no calories or artificial additives such as colorants, flavorings, or preservatives. It is affordable and easily absorbed by the body, ensuring efficient hydration without the need for complex metabolic processing. In contrast, sugar-sweetened beverages and caffeinated drinks contain complex components that may slow absorption and even promote fluid loss, potentially worsening dehydration. Thus, children were not recommended to drink sugar-sweetened, caffeinated (especially those under 12) and non-caloric sweetened beverages.
Drinking small sips of water or drinking slowly allows the body to gradually absorb water. This approach helps to prevent the rapid intake of large amounts of fluid, which could lead to increased urine output, rapid fluid loss, electrolyte imbalances, and gastrointestinal stress.
Drinking beverages above 65 °C can damage the esophageal mucosa. Additionally, drinking cold water, particularly ice-cold water, can cause sudden constriction of gastrointestinal blood vessels, which may lead to stomach spasms, abdominal pain, or even diarrhea.
Hydration status can be assessed by thirst level, urination frequency, urine volume, and urine color, allowing for timely water replenishment.
For the development of healthy drinking habits in children, parents should provide healthy drinking choices, set reminders for drinking water, and demonstrate proper drinking behavior. Schools should enhance water supply facilities, incorporate health education into the curriculum, and organize water-related activities. Effective communication between families and schools is essential for monitoring the hydration status of children.
Dehydration adversely impacts kidney, liver, and cardiovascular health in both adult and pediatric populations. Further research is needed for adequate water intake interventions, especially in children and adolescents. Targeted recommendations for children, including active and adequate water intake, healthy drinking habits, and hydration status monitoring, may contribute to preventing dehydration-related target organ damage and improve long-term health consequences.
Not applicable.
YH, ML, and DH designed the study. ML, BW, MG, HH, and JL performed the review. ML and BW drafted the first version of the manuscript. All authors contributed to interpreting and editing the manuscript. All authors read and approved the final manuscript. All authors have participated sufficiently in the work and agreed to be accountable for all aspects of the work.
Not applicable.
Not applicable.
This research was funded by the Capital’s Funds for Health Improvement and Research, grant number 2022-1G-4262 to YH and the National Natural Science Foundation of China, grant number 82073574 to YH.
The authors declare no conflict of interest.
References
Publisher’s Note: IMR Press stays neutral with regard to jurisdictional claims in published maps and institutional affiliations.

