1 Department of Biological Sciences, College of Science, University of Jeddah, 21959 Jeddah, Saudi Arabia
2 Department of Food Science and Nutrition, College of Sciences, Taif University, 21944 Taif, Saudi Arabia
3 Department of Biology, College of Sciences, Taif University, 21944 Taif, Saudi Arabia
4 Department of Food Science and Human Nutrition, College of Agriculture and Food, Qassim University, 51452 Buraydah, Saudi Arabia
5 Program of Food Sciences and Nutrition, Turabah University College, Taif University, 21944 Taif, Saudi Arabia
6 Molecular Diagnostic Unit, Alhada Armed Forces Hospital, 26792 Taif, Saudi Arabia
7 Department of Biology, College of Sciences, Umm Al-Qura University, 21955 Makkah, Saudi Arabia
8 Department of Biology, Al-Jumum University College, Umm Al-Qura University, 21955 Makkah, Saudi Arabia
Abstract
Aloe vera gel is well-known as a beauty product, nutrient and herbal medicine due to its therapeutic properties. The current research aimed to make a comparative study of natural Aloe vera gel (AG), sitagliptin (SIAG) and glibenclamide (GLIB) as diabetes medications on streptozotocin (STZ)-induced albino Wistar male rat models.
Rat models (60) were grouped equally into control, diabetic, normal+AG, STZ+AG, STZ+GLIB and STZ+SIAG. After 3 weeks of treatments, body weights, fasting blood glucose levels, blood analyses, fat profile and biochemical and antioxidant enzymes were evaluated. Data were analyzed in SPSS and all values are reported as Mean ± SD. The post hoc multiple comparison tests revealed significant differences among rat groups at p ≤ 0.05.
The oral administration of Aloe vera gel was efficient in the STZ+AG group compared to STZ+GLIB and STZ+SIAG. Treatments of the STZ+AG group caused a remarkable reduction of fasting blood glucose level 100.01 mg/dL. The STZ+AG group and STZ+GLIB group detected the same hemoglobin and glycosylated hemoglobin values. The STZ+GLIB group reported the lowest values for Homeostatic Model Assessment of Insulin Resistance (HOMA IR and β cell) 46.73 and 474.02, respectively.
The effect of Aloe vera gel was more pronounced for the biochemical and antioxidant enzymes. These results involved that, when compared to sitagliptin and glibenclamide as diabetes medications, Aloe vera gel ingestion significantly enhanced the diabetic rat' antioxidant defense system.
Keywords
- Aloe vera
- streptozotocin-induced diabetes
- antidiabetic activity
- diabetes medications
- antioxidant enzymes
The diverse condition known as diabetes is typified by hyperglycemia, which has been accomplished by epidemic proportions in the current century [1]. It is one of the major healthcare problems of mortality worldwide [2]. Numerous complications, such as diabetic retinopathy, sorbitol pathway metabolic disorders, autoxidation of glycosylated proteins and glycation of body proteins, can occur from hyperglycemia [3]. These complications can lead to secondary problems that affect membrane damage and oxidation of cellular lipids in the kidneys, nerves and arteries [4]. Several medications such as biguanides, sulfonylureas sitagliptin and glibenclamide are well-known to lower hyperglycemia in diabetic patients [5]. Some of these drugs are expensive with poor availability for numerous countryside populations and developing countries [6]. However, such medications can have some side effects [7]. There is an essential need in the medical system for the identification of antidiabetic plants, herbal medicines, natural compounds and alternative medications which shall have the therapeutic potential to overcome and reduce those side effects [8]. Numerous plant products and herbs have been demonstrated to have hypoglycemic effects [9]. Aloe vera (L.) plant has many medical benefits against stomach ailments, influenza, constipation, psoriasis, burns, lichen planus, healing wounds, plaque increase, gingivitis, gastrointestinal, ulcer and intestinal problems [10]. At present, it is utilized in nutraceuticals, skin care products and cosmetics [11]. It is considered an oral hypoglycaemic compound to reduce blood sugar levels and regulate plasma lipid levels [12]. Ghannam et al. [13] reported the positive effects of Aloe gel to lower blood glucose levels in the streptozotocin (STZ) induced type-II diabetic animal model. The STZ may cause diabetes by selectively degenerating pancreatic B-cells [14]. In diabetic rat models, Noor et al. [15] reported that Aloe vera restored the bulk and function of pancreatic islet cells, demonstrating the protective benefits of the plant on the organ. Additionally, from Aloe vera extracts, a water-soluble compound with Dipeptidyl Peptidase-IV inhibitory action was extracted and some of their constituents can alter the expression of Glucose Transporter Type 4 [16, 17, 18].
Nevertheless, more thorough research is required to determine the safety and effectiveness of plant extracts. In the current investigation, natural Aloe vera gel, sitagliptin and glibenclamide as diabetes medications on streptozotocin-induced male rat models’ comparison with healthy and diabetic groups were studied.
Specimens Aloe vera (L.) plant, commonly known as Aloe vera, was cultivated and purchased in June, 2024 from a garden in Taif, Kingdom of Saudi Arabia. In this investigation, fresh leaves from this cultivated plant were used. The Aloe vera powder was prepared according to the protocol mentioned by Can et al. [9]. In brief, approximately 70 cm length of mature, healthy and fresh green leaves were cut transversely into several parts and then washed thoroughly with clean tap water and air-dried after the thick epidermis removal. The fleshy, colorless, semi-solid mucilaginous gel in the center of the leaves was extracted with the help of a sterilized knife and cut into small parts. The homogenate, which was thick and straw in color, was lyophilized, which was extracted with ethanol (95%) and water, filtrated, collected and freeze-dried by (ALPHA 1-4 LSC, Germany) to dryness. A non-metallic electric grinder (JH-E01, China) was used to crush the dried gel into powder and it was sieved through 300 µm. The gel powder was stored in dry sterilized vacuumed tubes and kept at 4 °C until further use.
Approximately 3 month old male albino 150–200 g Wistar strain rats were employed. Rats were obtained from the Animal House in Jeddah, Kingdom of Saudi Arabia and selected as the animal models. Rats were maintained under the optimal laboratory conditions at 25 °C, 12 hrs light/dark cycle and had unlimited access to rat chow and tap water. The Gulf Countries Association of Sciences in Animal Experimentation granted Ethics Committee Number (8901/3151) approval for the 30 days animal study. Streptozotocin (STZ) a glucose analogue (2-deoxy-2-(3-methyl-3-nitrosouredio)-D-glucopyranose), sitagliptin and glibenclamide was obtained from Sigma, USA. All other chemicals, reagents and kits used were of analytical grade.
Fig. 1 shows the design of the protocol and the treatment schedule. After acclimatization for a week for any observation of untoward symptoms, the rat models were randomly distributed into six main groups of ten rats each in separate cages as follows:
• Vehicle group: Healthy rat models.
• Diabetic group: Diabetic rat models Type 1 (induced with 30 mg/kg of STZ).
• Normal+Aloe vera gel (AG) group: Healthy rat models were given Aloe vera gel extract (300 mg/kg) daily by using gavage needles for 21 days.
• STZ+AG group: Diabetic rat models were given Aloe vera gel extract (300 mg/kg b.wt.) daily by using gavage needles for 21 days.
• STZ+glibenclamide (GLIB) group: Diabetic rat models were given glibenclamide (600 µg/kg) daily by using gavage needles for 21 days.
• STZ+sitagliptin (SIAG) group: Diabetic rat models were given sitagliptin (10 mg/kg) daily by using gavage needles for 21 days.
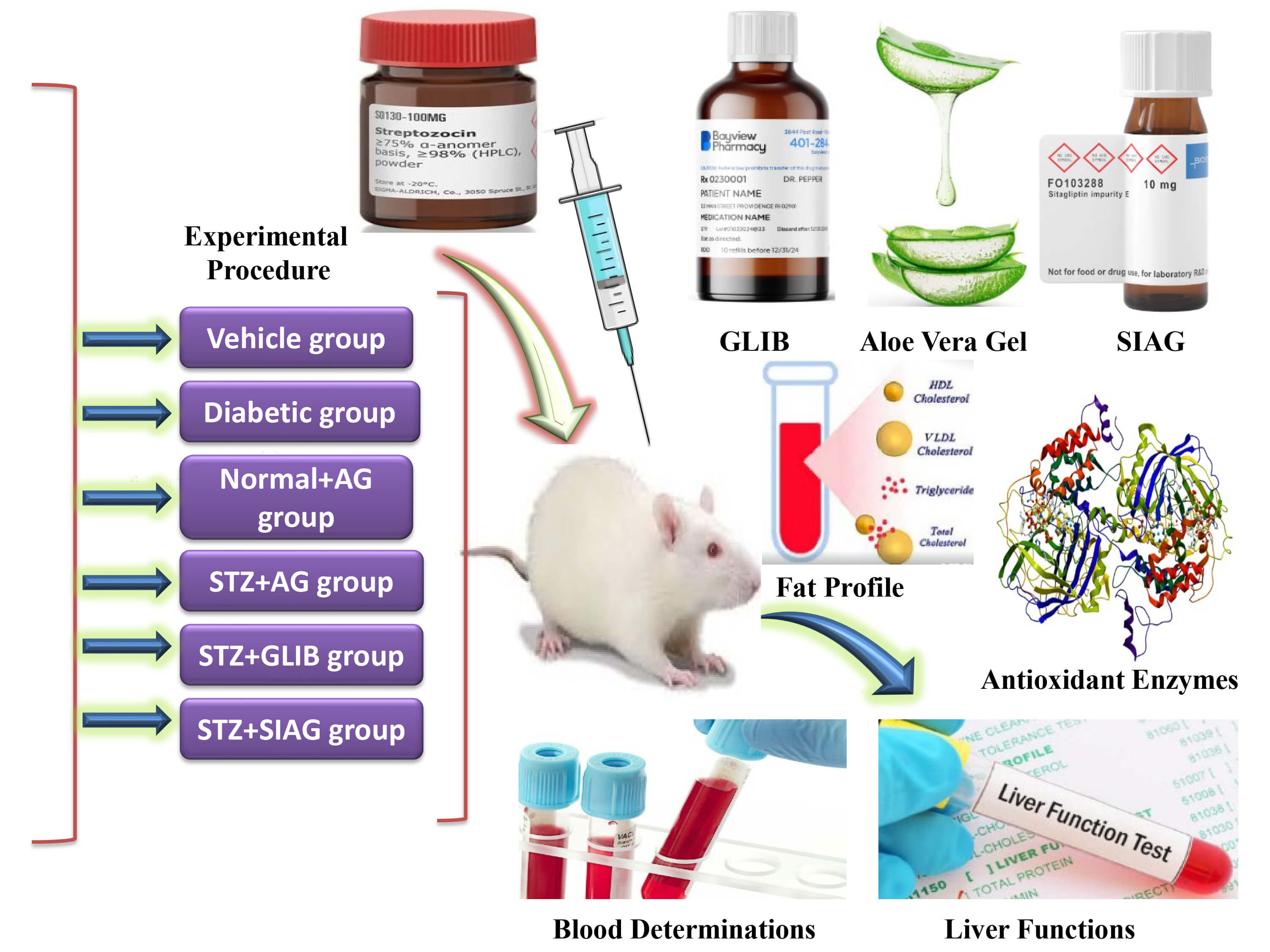 Fig. 1.
Fig. 1.
Design of the protocol and the treatment schedule. AG, Aloe vera gel; STZ, streptozotocin; GLIB, glibenclamide; SIAG, sitagliptin.
After the first seven days of the examination of rat models, the weight of rats was recorded after overnight fasting. Consequently, approximately 30 mg/kg of STZ in citrate buffer (0.1 M) with acidity (pH 4.5) was managed by a single intraperitoneal injection. The vehicle group of healthy rat models received an equal intraperitoneal dose of citrate buffer [19]. Blood glucose was assessed following a 16 hrs fast with free access to tap water. Overnight, the rats were given a 5% glucose solution to help them overcome the hypoglycemia caused by the medication. A glucometer (Bionime®, Switzerland) was used to measure fasting blood glucose levels and confirm the hyperglycemia before and 24 hrs following injection for diabetes approval and 7 days following injection for diabetes consolidation from the tails of the rat models. Fasting blood glucose levels were detected at weekly intervals on the 7th and 14th day with the tail prick assay. The body weight of each rat was then recorded every on the (1st, 7th, 14th and 21st) day by an electronic balance. The current study included STZ-treated animals that were diagnosed with diabetes if their fasting plasma levels were greater than 200 mg/dL with glucosuria. In order to prepare the Aloe vera gel extract, 300 mg of powdered Aloe vera gel was combined with 5 mL of water to create a solution. After the standardizing of the STZ dose, the experiments were conducted on animal groups to see the effect of natural Aloe vera gel and other diabetes medications, such as sitagliptin and glibenclamide, on rat models. Rat models in all groups were treated orally by using gavage needles every day in a single dose for 21 days.
After a continuous three-week treatment period, the animals were fasted overnight to reduce experimental variability and normalize any possible changes in feeding behavior. The purpose of this fasting period was to improve the consistency of experimental outcomes by preventing recent food intake from influencing metabolic and physiological parameters. Necropsy was carried out right after euthanasia of thiopental sodium (40 mg/kg) in order to gather the organs and tissues required for further examination [20].
Blood samples were drawn from the tail vein following 24 hrs fasting with
unrestricted access to water. A sharp, sterilized blade was used to cut the tail
tip in a single stroke. Heparinized tubes were used to collect blood, the plasma
was separated from the blood to detect the essential measurements by centrifuging
it for 15 min at 2500 rpm. Approximately, 40 µL was taken to measure
glucose concentration according to the glucose oxidase assay (Reflotron 1,
Boehringer, Germany). While hemoglobin and glycosylated hemoglobin were detected
[21]. Homeostatic Model Assessment of Insulin Resistance (HOMA IR and
The fat profile of blood, such as triglycerides (TG) and total cholesterol, was determined by the enzymatic colorimetric assays. The High-Density Lipoprotein (HDL) and Very Low-Density Lipoprotein (VLDL) of cholesterols were detected [24].
The biochemical and antioxidant enzyme evaluations for plasma and liver samples were detected [20]. Kits for blood and liver markers were purchased from Sigma, Darmstadt, Germany. Alkaline phosphatase (ALP) and Alanine Transaminase (ALT) were expressed as (U/L); Glutathione (GSH) and malondialdehyde (MDA) were expressed as (nmol/mg); Thiobarbituric Acid Reactive Substances (TBARS) and hydroperoxides were expressed as (mM/100 g); while antioxidant enzyme activities as glutathione peroxidase (GPx), superoxide dismutase (SOD), catalase (CAT) and glutathione-S-transferase (GST) were expressed as (U/mg).
ANOVA test was used as the primary statistical analysis to compare differences
between groups, followed by post-hoc test (Bonferroni) to identify specific group
differences, with significance set at p
Body weights were severely decreased in the diabetic group and STZ+SIAG group compared to the vehicle group on the 21st day (149.48, 161.84 and 179.89 g), respectively. Increases in body weights were improved by STZ+AG group or STZ+GLIB group treatments (189.33 g and 195.22 g) (Fig. 2).
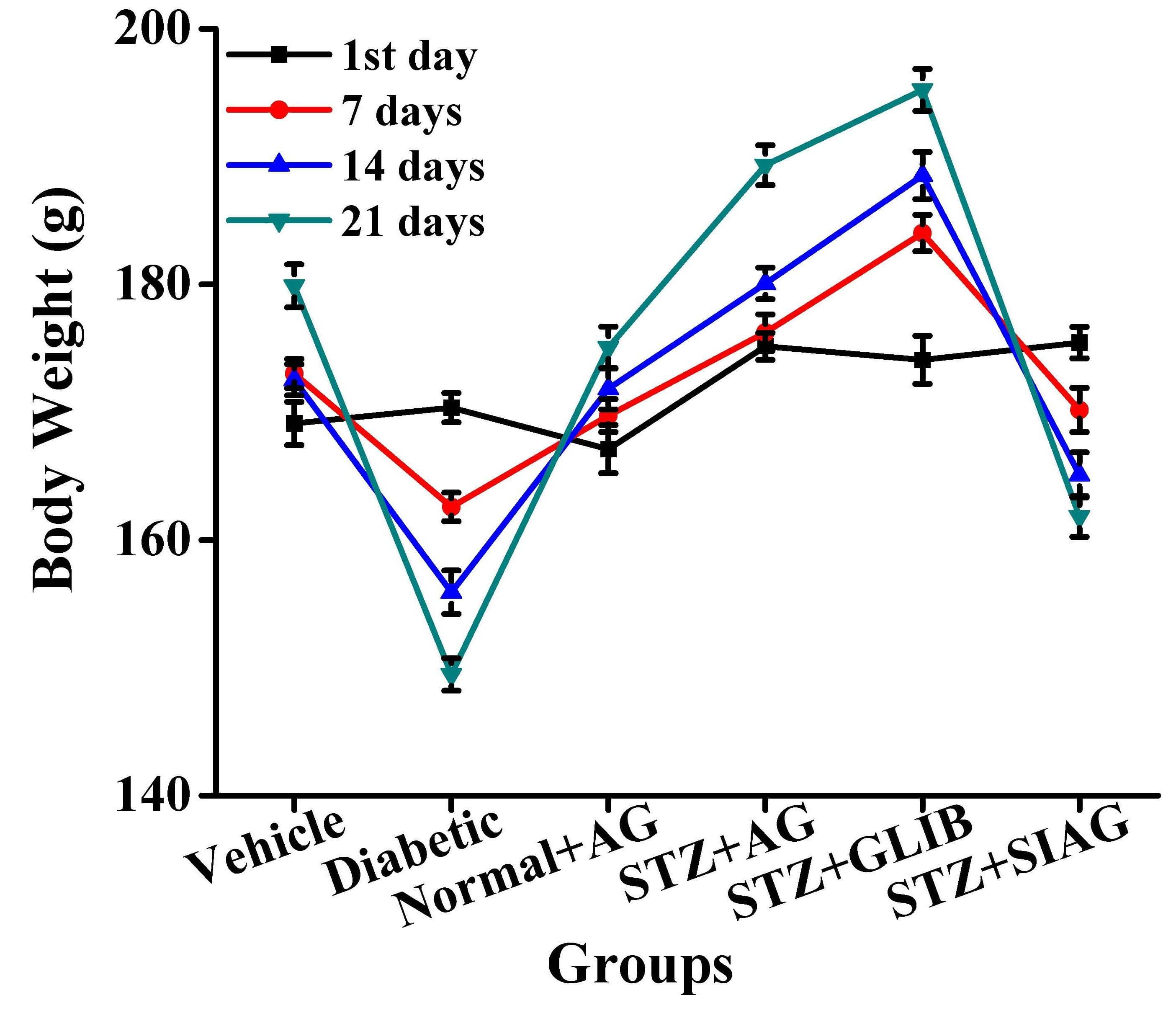 Fig. 2.
Fig. 2.
Effects of various medications on body weights in rat models. n = 60; each group n = 10.
Fasting blood glucose levels were increased during the 21 days of post-diabetic inductions after the injection of the STZ dose. The level of the STZ+AG group consequently dropped down to reach 128.14 mg/dL on the 7th day, which further decreased to normal levels on the 14th and 21st day. Treatments of the STZ+AG group caused a remarkable reduction level of 100.01 mg/dL compared to the diabetic group 277.13 mg/dL (Fig. 3). On the other hand, the other two diabetes medications sitagliptin and glibenclamide as did not show the ability to decrease the fasting blood glucose levels 201.42 and 115.14 mg/dL after 3 weeks compared with the vehicle group, respectively.
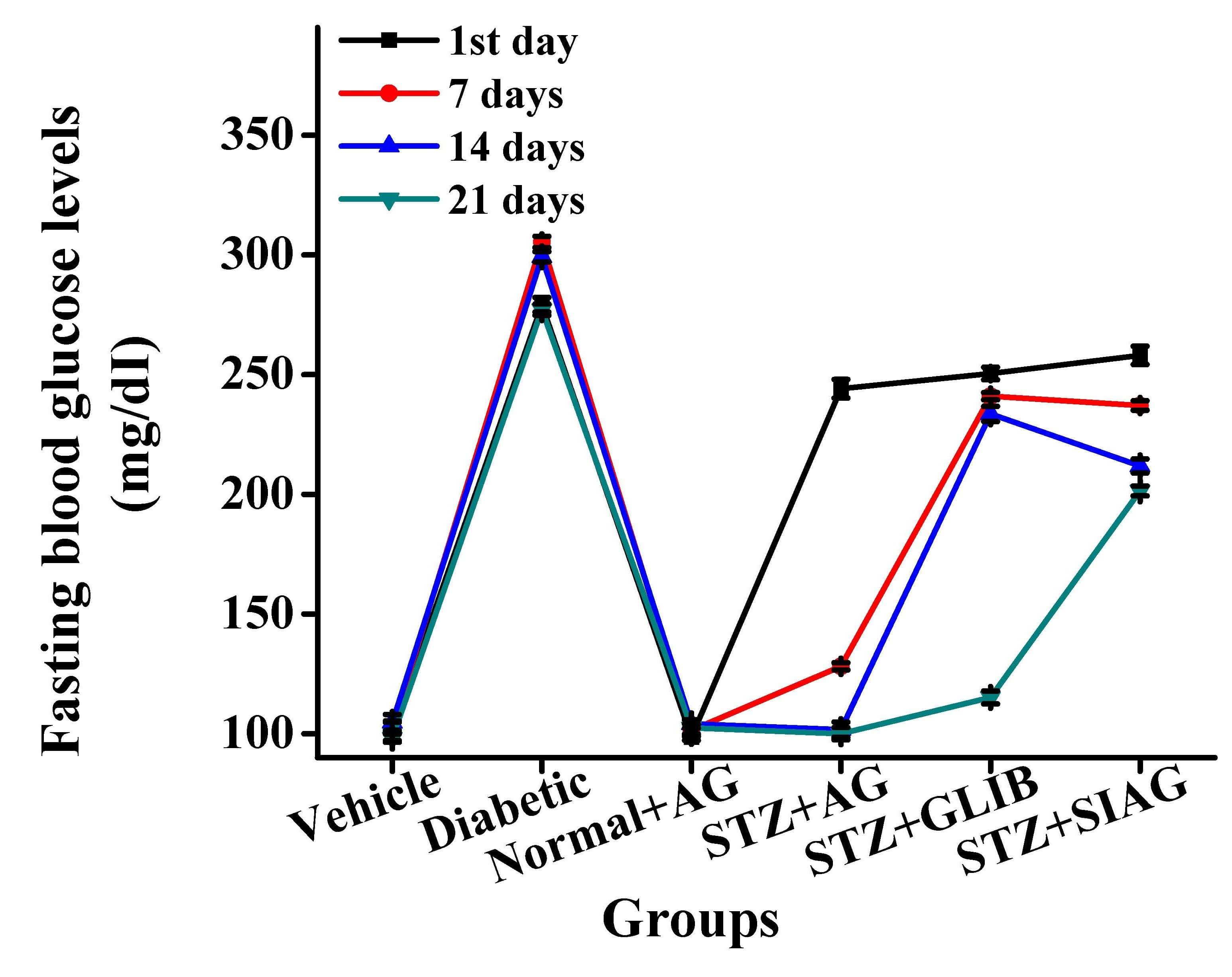 Fig. 3.
Fig. 3.
Effects of various medications on fasting blood glucose levels in rat models. n = 60; each group n = 10.
Hemoglobin levels rise in a glucose level-dependent manner in response to the
severity of hyperglycemia. After 21 days, the administration of natural
Aloe vera gel and other diabetes medications such as sitagliptin and
glibenclamide (STZ+SIAG group) caused a reduction in hemoglobin level (12.04
g/dL), while STZ+AG group and STZ+GLIB group detected the same value and tended
to reach the vehicle group (12.3 g/dL) compared to the diabetic group (11.25
g/dL) (Fig. 4). On the same trend, STZ+AG group and STZ+GLIB group detected the
same value of glycosylated hemoglobin and tended to reach the vehicle group
(7.05% Hb) compared to the diabetic group (12.41% Hb), while STZ+SIAG group had
higher values (8.14% Hb) at the end of the experimental period (Table 1). The
DPP IV enzyme activity demonstrated an increase in diabetic rat models from 4.85
U/min/mL in the STZ+SIAG group to 10.11 U/min/mL in the diabetic group compared
to the vehicle group recorded 2.56 U/min/mL. While administration of
glibenclamide decreased the DPP IV enzyme activity to reach 5.01 U/min/mL
followed by the STZ+AG group (6.23 U/min/mL). The increases in (HOMA IR and
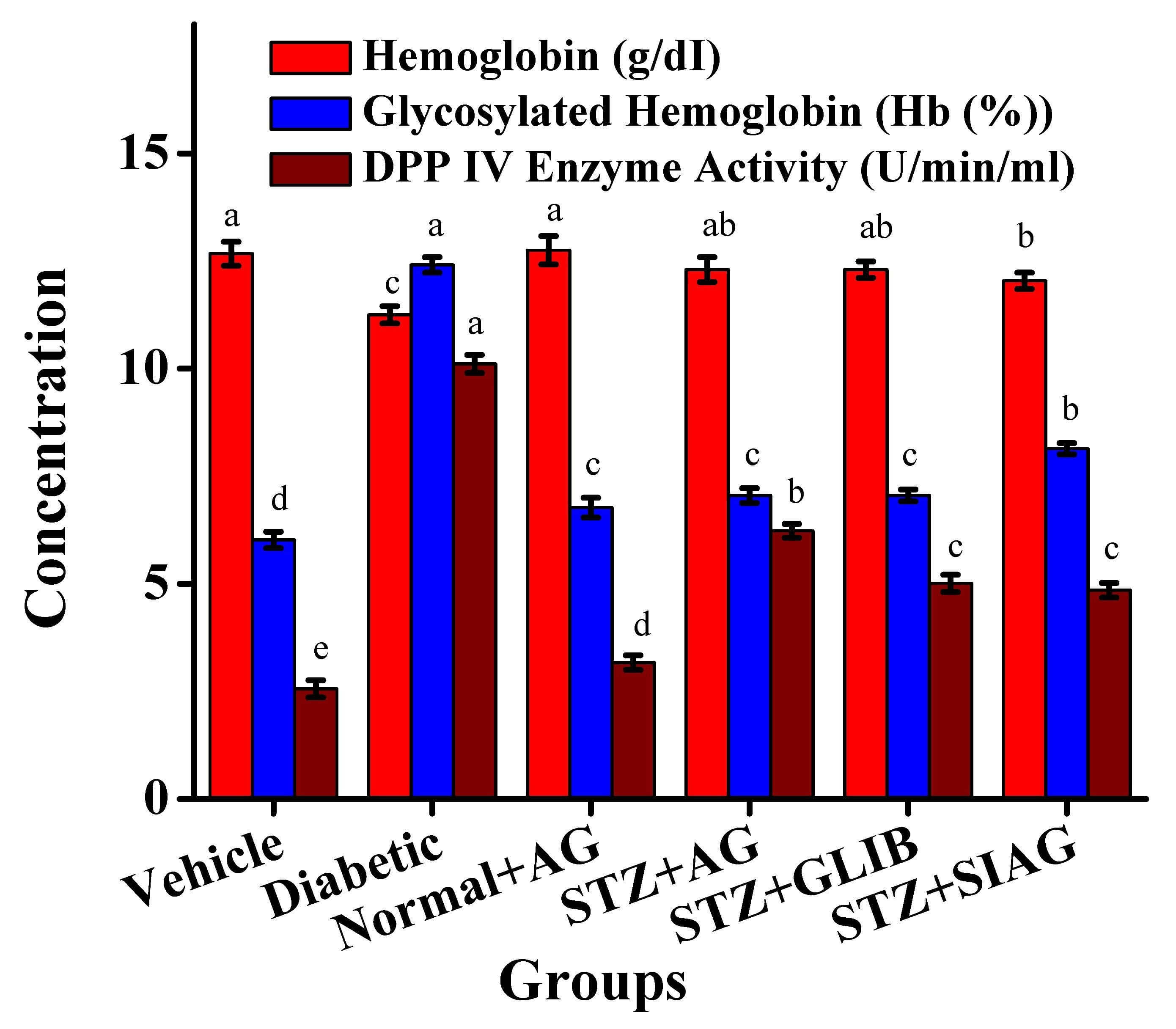 Fig. 4.
Fig. 4.
Effects of various medications on blood analysis in rat models. Different letters mean significant differences among rat models group. Dipeptidyl Peptidase-4 (DDP IV), n = 60; each group n = 10.
| Group | HOMA IR | HOMA |
| Vehicle | 74.44 |
1010.02 |
| Diabetic | 58.76 |
955.32 |
| Normal+AG | 53.12 |
889.08 |
| STZ+AG | 49.03 |
600.07 |
| STZ+GLIB | 46.73 |
474.02 |
| STZ+SIAG | 48.46 |
488.76 |
Different letters mean significant differences among rat models group. HOMA IR, Homeostatic Model Assessment of Insulin Resistance.
The fat profile values among all rat models are presented in Table 2. An increase in TG and VLDL values in the diabetic group (802.00–115.41 mg/dL) compared with that in the vehicle group (568.32–82.34 mg/dL), respectively. The STZ+AG group maintained TG and VLDL values (420.51–59.12 mg/dL) than the STZ+GLIB group (289.40–50.02 mg/dL) and STZ+SIAG group (245.42–56.32 mg/dL), respectively. The STZ+AG group preserved HDL value to reach 27.03 mg/dL compared with the vehicle group’s 28.14 mg/dL. The STZ+SIAG group normal+AG group reported higher values of total cholesterol at 83.30 mg/dL followed by the normal+AG group, which reached 81.04 mg/dL. In the current work, supplementation of Aloe vera decreased the TG and VLDL levels; however, no obvious changes occurred in total cholesterol and HDL levels, indicating that lipid metabolism may be improved by gel. The highest values for TG and VLDL were noticed in the normal+AG group, which fed on Aloe vera only at 510.75 and 78.03 mg/dL, respectively (Table 2).
| Group | Triglycerides (mg/dL) | Total cholesterol (mg/dL) | HDL (mg/dL) | VLDL (mg/dL) |
| Vehicle | 568.32 |
76.13 |
28.14 |
82.34 |
| Diabetic | 802.00 |
74.22 |
27.13 |
115.41 |
| Normal+AG | 510.75 |
81.04 |
29.62 |
78.03 |
| STZ+AG | 420.51 |
76.96 |
27.03 |
59.12 |
| STZ+GLIB | 289.40 |
75.87 |
21.45 |
50.02 |
| STZ+SIAG | 245.42 |
83.30 |
22.54 |
56.32 |
Different letters mean significant differences among rat models group. HDL, High-Density Lipoprotein; VLDL, Very Low-Density Lipoprotein.
Some biochemical parameters for the liver functions were determined such as ALP and ALT activities (Fig. 5). The ALP activity was increased in the diabetic group, compared to the vehicle group. The ALT activity was reduced in the diabetic rat models given Aloe vera gel to reach 59.10 U/L. It was noticed that the STZ+AG group got protective effects comparable to STZ+GLIB and STZ+SIAG groups against hepatotoxicity. Fig. 6 presents liver tissue GSH and MDA values in the liver for all rat models. There was a great reduction in GSH values among diabetes rats compared to the vehicle group. The Treatments with Aloe vera and glibenclamide medication raised the GSH values to reach 32.57 and 29.03 nmol/mg, respectively. As shown in Fig. 6, the diabetic group detected an increase in MDA level 13.23 nmol/mg compared to the vehicle group 7.16 nmol/mg. It is known that higher levels of MDA are an indicator of increased oxidative stress. The administration of natural Aloe vera gel, sitagliptin and glibenclamide as diabetes medications to the diabetic rat models resulted in a great reduction of MDA levels as 9.11, 10.12 and 11.44 nmol/mg, respectively. Fig. 7a,b presents TBARS and hydroperoxides values in the liver of rat models. There were great elevations in tissue TBARS and hydroperoxides for diabetic rats (1.82 and 95.47 mM/100 g) compared to the vehicle group (0.90 and 70.05 mM/100 g), respectively. The administration of natural Aloe vera gel, glibenclamide and sitagliptin as diabetes medications to the diabetic rat models resulted in great reductions as 0.95, 1.51, 1.49, 75.21, 82.04 and 87.92 mM/100 g, respectively.
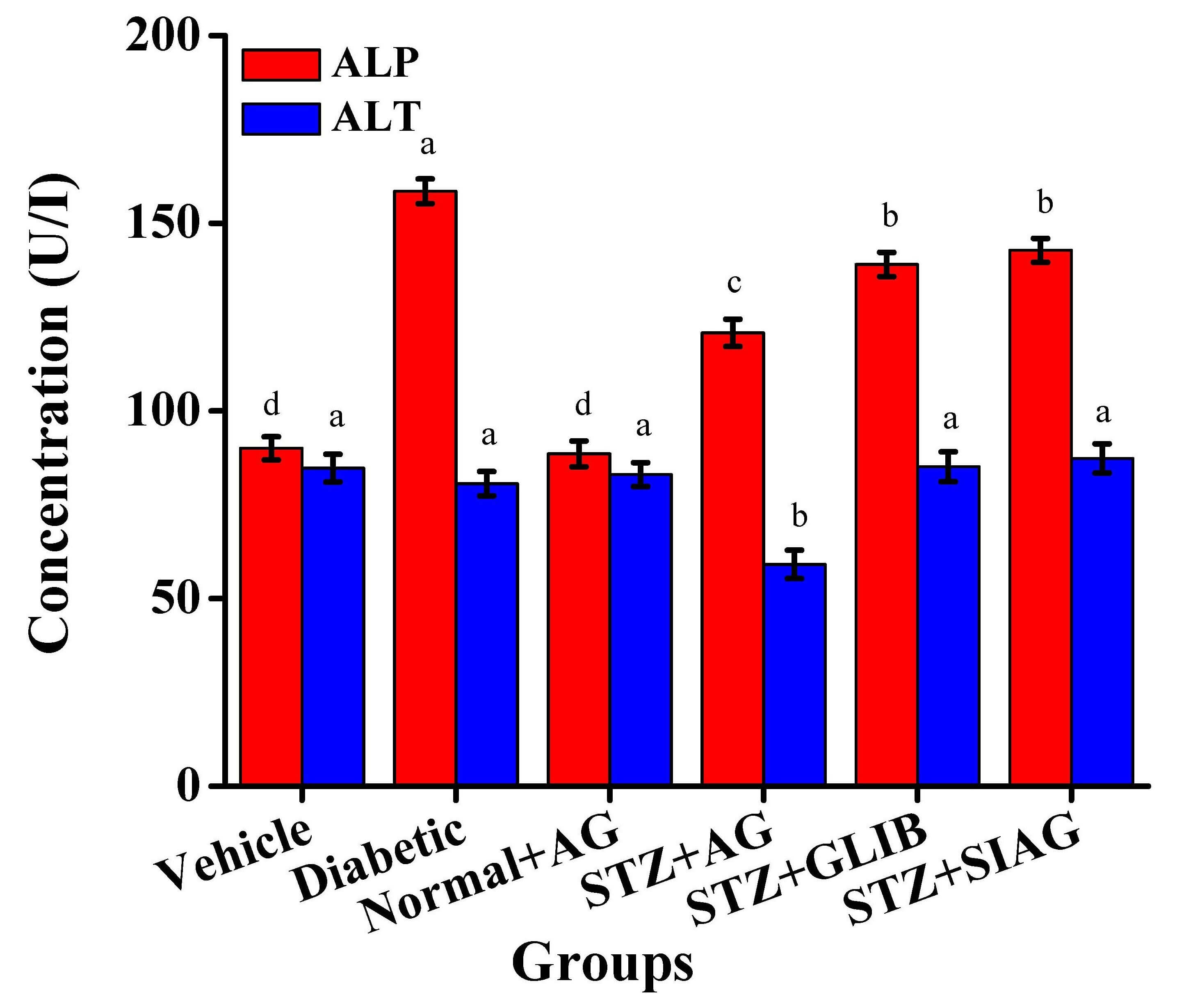 Fig. 5.
Fig. 5.
Effects of various medications on liver tissue as Alkaline phosphatase (ALP) and Alanine Transaminase (ALT) activities in rat models. Different letters mean significant differences among rat models group, n = 60; each group n = 10.
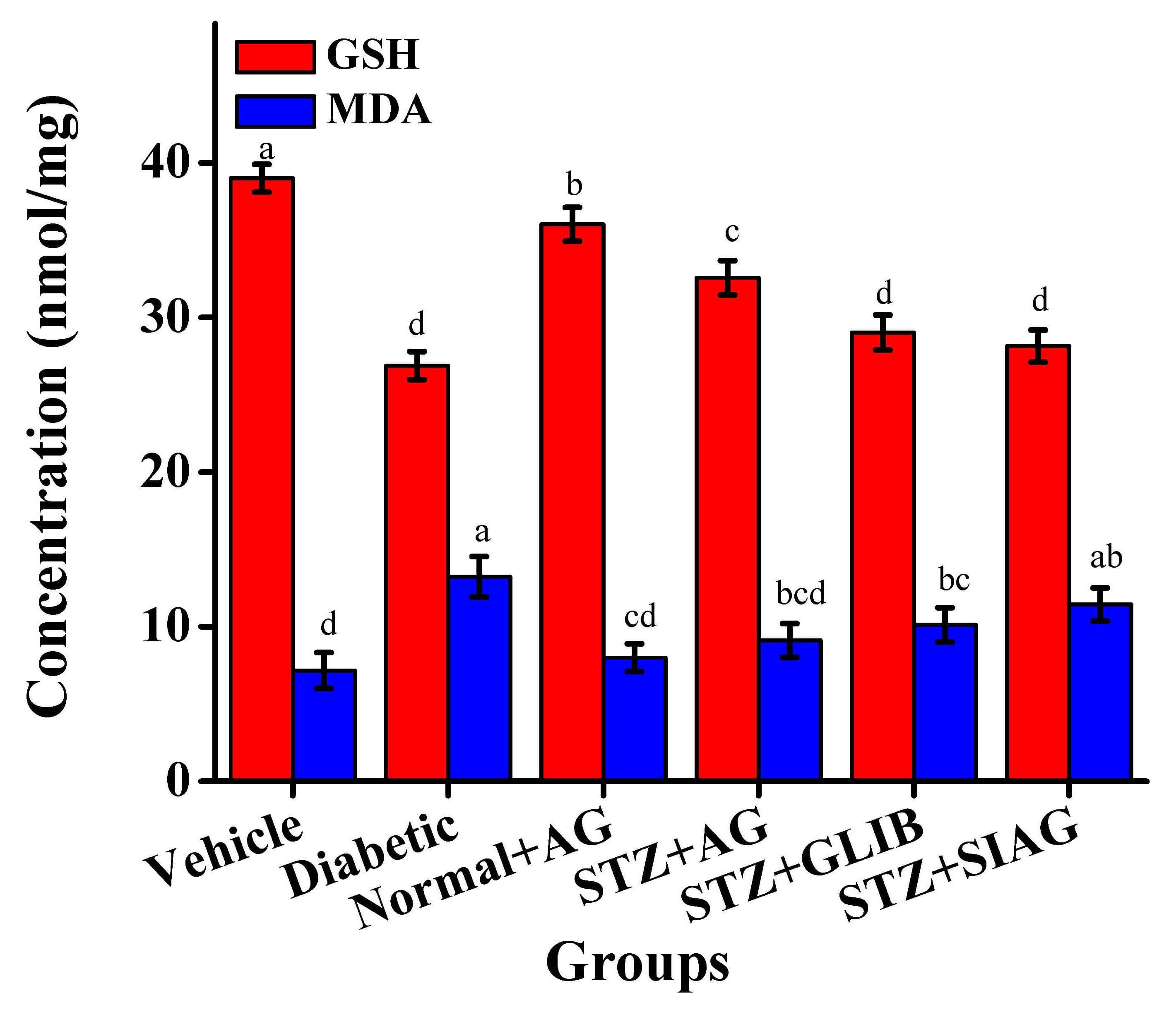 Fig. 6.
Fig. 6.
Effects of various medications on liver tissue as Glutathione (GSH) and malondialdehyde (MDA) in rat models. Different letters mean significant differences among rat models group, n = 60; each group n = 10.
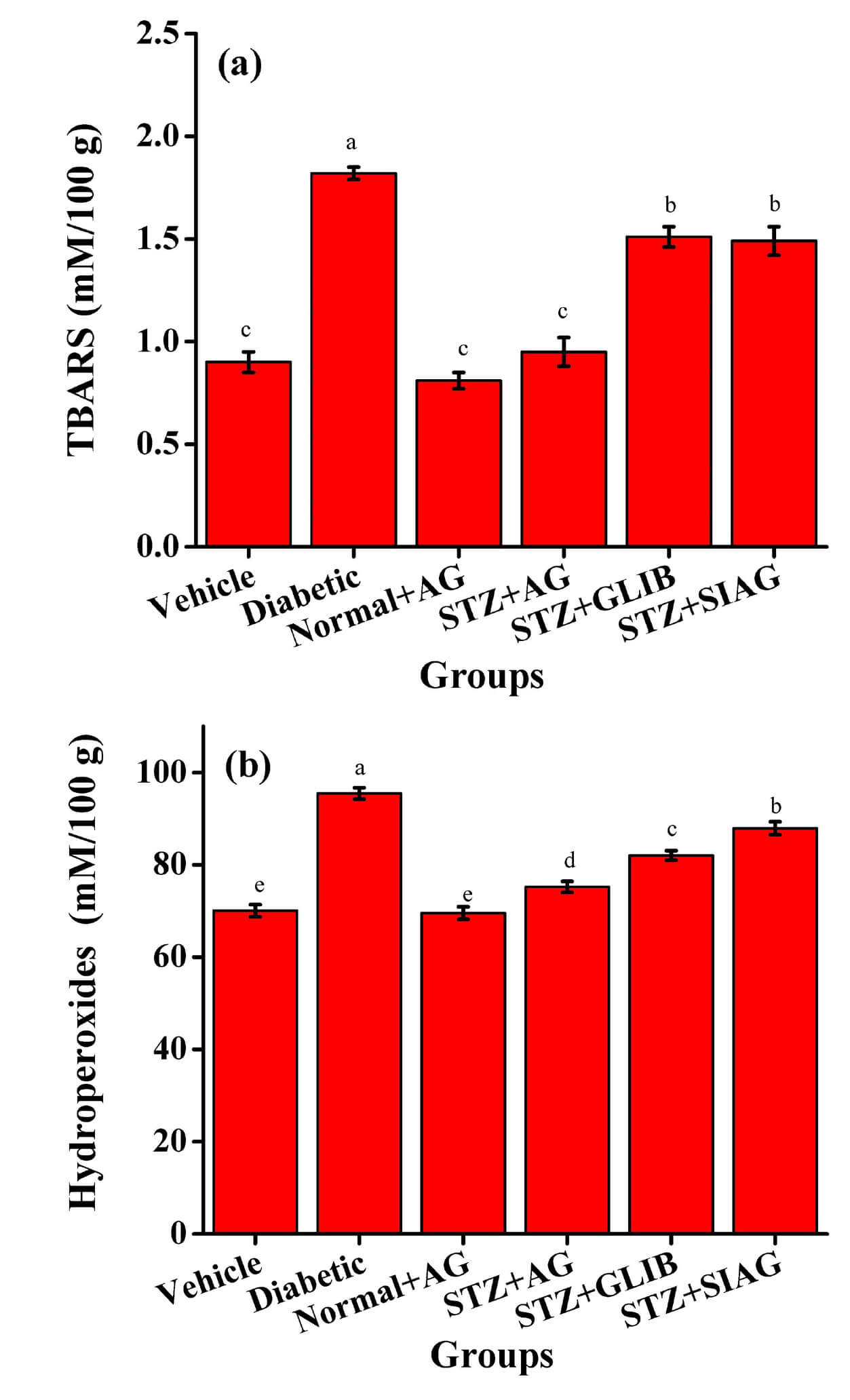 Fig. 7.
Fig. 7.
Effects of various medications on liver tissue in rat models. (a) Thiobarbituric Acid Reactive Substances (TBARS) and (b) Hydroperoxides, n = 60; each group n = 10.
Table 3 presents the enzyme activities of GPx, SOD, CAT and GST in the liver tissues of rat models. The GPx activity recorded a considerable reduction from 1.74 U/mg in the diabetic group to 1.01, 1.17 and 1.20 U/mg for STZ+AG, STZ+GLIB and STZ+SIAG groups, respectively. The effect of Aloe vera gel was more pronounced which reached 6.17, 0.67 and 4.04 U/mg compared with the diabetic group that recorded (3.88, 0.48 and 1.23 U/mg) for SOD, CAT and GST activities, respectively.
| Group | Gpx activity (U/mg) | SOD activity (U/mg) | CAT activity (U/mg) | GST activity (U/mg) |
| Vehicle | 1.22 |
5.33 |
0.53 |
2.11 |
| Diabetic | 1.74 |
3.88 |
0.48 |
1.23 |
| Normal+AG | 1.03 |
6.12 |
0.61 |
2.23 |
| STZ+AG | 1.01 |
6.17 |
0.67 |
4.04 |
| STZ+GLIB | 1.17 |
4.77 |
0.63 |
3.56 |
| STZ+SIAG | 1.20 |
5.03 |
0.62 |
3.72 |
Different letters mean significant differences among rat models group. GPx, glutathione peroxidase; SOD, superoxide dismutase; CAT, catalase; GST, glutathione-S-transferase, n = 60; each group n = 10.
The diabetic rat models in STZ-induced diabetes may display the majority of problems, including oxidative stress-induced neurological, vas deferens, kidney and urine bladder dysfunctions [6, 7].
These positive effects of body weight can be due to the prevention of
Aloe vera sterols are plentiful and structurally comparable to cholesterol, including stigmasterol, campesterol and b-sitosterol [25]. Furthermore, it regulates the enzymes that break down carbohydrates to preserve glucose homeostasis [27]. Another study compared oral medication of Aloe vera gel (200–400 mg/kg) with metformin (50 mg/kg) in rat models. All therapies decreased the high blood glucose levels in all diabetic-induced rats and there were no significant differences between them [28]. Another study on the alloxan-induced mice that used oral natural Aloe vera gel in a dose of 500 mg/kg twice a day reported a reduction in blood glucose levels from 30.7 to 37.7% on the 5th day [29].
Mohamed [25] isolated phytosterol and fraction components from Aloe vera gel for studying the anti-hyperglycemic activities. Glycosylated hemoglobin is created when hemoglobin and excess blood glucose combine in diabetes [30]. Glycosylated hemoglobin is increased over a long period in diabetes.
The reduction of glycosylated hemoglobin might be due to the enhancement in the
glycemic status. This implies that the natural Aloe vera gel treatment
will reduce oxidative stress. The DPP IV enzyme activity is known as an
attractive anti-diabetic medication target [16]. The current date for the DPP IV
enzyme activity was in agreement with Nayak and Pattabiraman [26], who
demonstrated that Aloe vera gel may inhibit that enzyme and the
dipyrrole derivative in vitro study. Those results referred to the
protective roles of Aloe vera gel on the pancreatic IR and
As well-known cholesterol, elevated TG levels may contribute to the development
of type 2 diabetes by pathologically impairing
Increased blood activity of certain enzymes, such as ALT and ALP, are common biochemical indicators of liver damage [33]. According to the current results, although ALP is a critical marker for various metabolic functions that might be impaired by diabetes, healthy compounds in Aloe vera gel may decrease ALP activity, considered a result of the toxic metabolites produced by the streptozotocin. The GSH is primarily involved in metabolism and detoxification. As an antioxidant, it shields tissues from oxidative stress and is, therefore, frequently used as a gauge of free radical damage [34]. Reduced GSH levels in the liver with diabetes due to STZ injection indicate tissue damage and the increased oxidative stress-induced GSH consumption [35]. The usage of more “SH” in proteins to protect them from lipid peroxide may be the cause of the decrease in GSH values [36]. This suggests that the natural Aloe vera plant may either promote GSH biosynthesis, lessen oxidative stress, which prevents GSH from degrading or have both benefits. The MDA, a biomarker of oxidative stress, is produced when reactive oxygen species break down polyunsaturated fatty acids [19]. The reduction in MDA formation values in the liver was in agreement with Tanaka et al. [37], indicating the plant’s function in preventing oxidative damage caused by cellular damage. Aloe vera gel can reduce MDA values by raising the production of nitric oxide, which strengthens the antioxidant capacity as a way to regulate blood glucose levels [38]. The TBARS is the most widely used lipid peroxidation indicator [39]. The notable rise in TBARS and hydroperoxide values in the liver of diabetic rat models may be due to the elevated lipid peroxidation in the tissues [40].
Antioxidant enzymes play very essential roles in the defense system, while CAT is a hemeprotein that catalyzes the reduction of hydrogen peroxide and shields the tissue from extremely dangerous hydroxyl radicals, SOD can scavenge superoxide radicals by converting them to H2O2 and molecular oxygen [20, 24]. The GPx and GST enzymes can break down H2O2 and other organic hydroperoxides into non-toxic byproducts at the GSH’s expense, while any inactivation and glycation of the enzyme caused by radicals may lead to decreased GPx activity [40]. These results involved that, when compared to sitagliptin and glibenclamide as diabetes medications, Aloe vera gel ingestion significantly enhanced the diabetic rats’ antioxidant defense system.
The results of the current work indicated that the oral administration of Aloe vera gel was sufficient and might have beneficial effects on body weight, blood analyses, fat profile and biochemical and antioxidant enzymes for the liver comparable to sitagliptin and glibenclamide against hepatotoxicity produced by streptozotocin for diabetic rat models. Extra research on the application of Aloe vera gel is needed in the treatment and/or prevention of diabetes complications.
Glibenclamide, sitagliptin and natural Aloe vera gel have been used as diabetes medications in streptozotocin-induced male rat models. The present study concluded that the oral administration of Aloe vera gel was adequate and could potentially have positive effects on body weight, blood analysis, fat profile, liver biochemical and antioxidant enzymes similar to sitagliptin and glibenclamide against streptozotocin-induced hepatotoxicity in diabetic rat models. In order to cure and/or prevent problems from diabetes, more research is required on the use of Aloe vera gel.
All relevant data are within the paper and its supporting information files.
Conception or design: AAH, RS, RAA, SHQ, AGA, SAA. Acquisition, analysis, or interpretation of data: RMA, HFA, SHA, SBA. Drafting the work or revising: SHQ, AGA, SAA, RMA, HFA, SHA, SBA. Final approval of the manuscript: AAH, RS, RAA. All authors contributed to editorial changes in the manuscript. All authors read and approved the final manuscript. All authors have participated sufficiently in the work and agreed to be accountable for all aspects of the work in the end.
The Gulf Countries Association of Sciences in Animal Experimentation granted Ethics Committee Number (8901/3151) approval for the 30 days animal study. Every animal procedure was carried out in compliance with the 3R principles (replacement, reduction, and refinement) and the ethical standards of the institution’s guidelines. Additionally, the work followed the ARRIVE criteria for reporting research using animals.
The authors extend their appreciation to Taif University, Saudi Arabia, for supporting this work through project number (TU-DSPP-2024-10).
This research was funded by Taif University, Saudi Arabia, Project No. (TU-DSPP-2024-10).
The authors declare no conflict of interest.
References
Publisher’s Note: IMR Press stays neutral with regard to jurisdictional claims in published maps and institutional affiliations.







