1 Academic Centre for Materials and Nanotechnology, AGH University of Krakow, 30-059 Krakow, Poland
2 Department of Biomaterials and Composites, Faculty of Materials Science and Ceramics, AGH University of Krakow, 30-059 Krakow, Poland
Abstract
Diabetic wounds are one of the most common and challenging complications of diabetes. Similar to chronic wounds, diabetic wounds are difficult to treat due to prolonged inflammation, a lack of angiogenesis, abnormal differentiation of new scar tissue, and the occurrence of numerous bacterial infections. Moreover, elevated sugar levels in tissues disrupt the healing process by enhancing inflammatory reactions, disrupting signaling pathways, and leading to the production of abnormal biological structures, which contribute to improper cell differentiation. Traditional dressings, such as bandages, gauze, and semi-occlusive foams, are inadequate for diabetic wounds with high exudation; moreover, frequently changing the dressing can cause secondary irritation. Hence, innovative hydrogel dressings are being developed, which, thanks to their soft polymer matrix, provide an ideal substrate for regenerating tissue. Hydrogels also allow for the introduction and controlled release of growth factors, making them a promising solution for treating diabetic wounds. Recently, researchers have focused on insulin, a hormone secreted by the human body to lower blood sugar levels, due to its interesting characteristics, such as supporting anti-inflammatory and proangiogenic processes and stimulating cell migration and proper proliferation. This review discusses the most important aspects of diabetes and diabetic wounds and traditional and innovative treatment methods, particularly hydrogel dressings used as systems for insulin delivery in response to glucose concentration.
Keywords
- diabetic wounds
- insulin
- hydrogel dressings
- stimuli-controlled release
- drug delivery systems
Diabetes mellitus is defined as a complex metabolic disorder characterized by
the presence of hyperglycemia in the body, resulting from abnormalities in
insulin secretion and action. Hyperglycemia occurs due to insufficient insulin
production or an abnormal cellular response to insulin, leading to a chronic
disorder of carbohydrate, fat, and protein metabolism. Long-term hyperglycemia is
associated with the development of diabetes and can result in serious health
complications, such as damage to the nervous system and dysfunction of the eyes
and kidneys [1]. Currently, diabetes is classified into several types, with type
1 diabetes (T1DM) and type 2 diabetes (T2DM) being the most commonly diagnosed.
Type 1 diabetes is primarily diagnosed in young individuals and accounts for
approximately 5–10% of diagnosed diabetes cases [2]. It is characterized by the
autoimmune destruction of
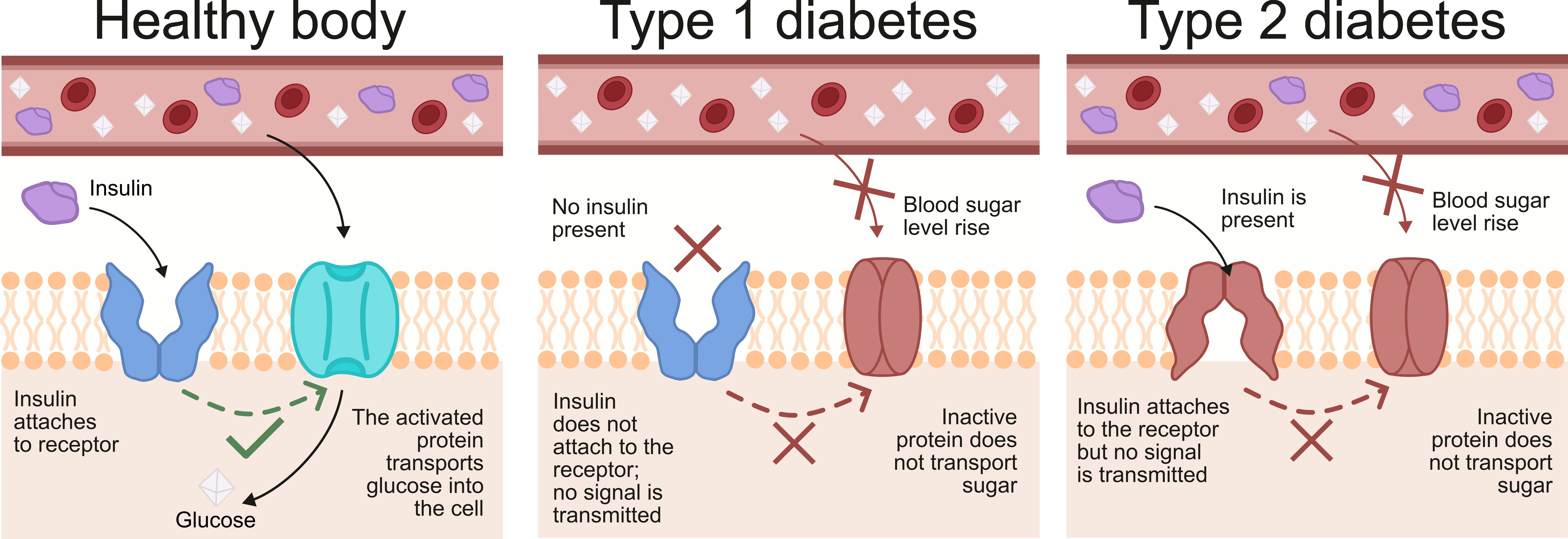 Fig. 1.
Fig. 1.
Basic differences between healthy organism, type I, and type II diabetes. In a healthy individual, the body produces insulin efficiently, and cells respond to its presence, allowing blood glucose levels to be maintained within a normal range. Type 1 diabetes is an autoimmune condition resulting in little to no insulin production, while in type 2 diabetes, which is predominantly linked to lifestyle and genetic factors, insulin is produced but the body cells develop resistance, not responding effectively to its presence; in both cases blood sugar levels are too high. The image was created with Inkscape v1.4, retrieved from https://inkscape.org.
Diabetic Foot Syndrome is a condition that affects individuals with diabetes, characterized by ulcers and wounds on the lower limbs [5]. These ulcers result from repeated compressive and shear stresses on the foot, typically occuring in patients with diagnosed peripheral neuropathy. Factors that increase the likelihood of a wound include the presence of foot deformities, the application of abnormal loads during walking, joint mobility disorders, and the occurrence of minor injuries. In diabetic patients, persistent hyperglycemia compromises overall immunity and prolongs inflammation in wounds, as well as the wound healing process. Coexisting ischemia and infections are significant impediments to wound healing in these patients. The disease’s progression is linked to the development of peripheral artery diseases and osteomyelitis; in severe cases, complications can lead to tissue necrosis and the need for lower limb amputation [6]. Among patients with advanced diabetic wounds, 17% require amputation of a small part of the limb, while 5% require a major amputation within one year of diagnosis [7]. In the most severe cases, amputation is performed. The risk of death within five years is 2.5 times higher for individuals with diabetic foot ulcers (DFUs) than for those with diabetes alone, and the five-year mortality rate following diabetes-related amputations exceeds 70%, which is worse than in many common cancers [8]. Given these considerations, there is a critical need to develop an integrated system that combines the use of wound dressings, bioactive substances, and antibiotics, as well as the to implement changes in treatment strategies concerning wound dressing design and quantitative diagnostics, to enhance patient treatment and comfort [9].
Due to the rapid development of nanobiotechnology in regenerative medicine, this article aims to present current trends in the pursuit of improved solutions for future researchers. This work provides a concise overview of the challenges associated with treating diabetic wounds, taking into account the primary pathophysiological factors that influence the progression of this disease, such as prolonged inflammation, local hyperglycemia, the presence of reactive oxygen species, insufficient angiogenesis, and bacterial infections. The article discusses currently developed methods for treating these wounds, which utilize hydrogel matrix dressings containing polymer micro- and nanocarriers with insulin that acts as a growth factor. Recent research on micro- and nanoparticles made from both natural and synthetic polymers incorporated into hydrogel matrices is analyzed, highlighting the potential of this system for the therapy of diabetic wounds. The methods for synthesizing these carriers and the results of in vitro and in vivo tests published in selected articles over the last ten years are briefly summarized.
In the case of normal skin wound healing, this process consists of a series of complex and orderly events that can be divided into four main phases: hemostasis, inflammation, proliferation, and remodelling. During the hemostasis phase, coagulation factors promote clotting, which reduces bleeding and provides mechanical support for the damaged tissue. Subsequently, in the inflammatory phase, inflammatory cells—such as lymphocytes, monocytes, and macrophages—eliminate damaged tissue and pathogens. In the proliferation phase that follows, epithelial cells and fibroblasts fill the space left by the lost tissue, leading to a gradual decrease in the size of the open wound. Once the wound bed is filled with granulation tissue, it undergoes remodeling in the scarring phase, transforming into connective tissue that forms a supportive layer for the newly formed epithelium [10]. In summary, diabetic wounds exhibit deregulated angiogenesis, a chronically sustained suboptimal inflammatory response, increased levels of reactive oxygen species, and persistent bacterial colonization that often develops into a difficult-to-treat biofilm [11].
Diabetic wound healing is disrupted by several factors. Diabetes impairs the inflammatory, proliferative, and scarring phases, negatively affecting wound healing and resulting in scarring. In diabetic wound healing, the inflammatory phase is prolonged due to the failure of the transition between M1 and M2 macrophages, causing an abnormal accumulation of inflammatory cells in the wound and an exaggerated inflammatory response. The excessive number of inflammatory cells increases the levels of proteases, which damage the extracellular matrix (ECM) and degrade growth factors and their receptors. This proteolytic damage to the ECM attracts even more inflammatory cells, leading to increased production of reactive oxygen species in the hypoxic conditions present in the wound. Additionally, reactive oxygen species can activate proteases and inhibit their inhibitors, resulting in increased proteolysis and further damage to the ECM, ultimately causing significant cellular damage.
In addition, similar to chronic wounds, diabetic wounds are particularly susceptible to re-injury. The constant reopening of these wounds result in an excessive accumulation of neutrophils and phagocytes around the damaged tissue. This leads to the extension of what is known as NETosis, a physiological response in the body aimed at producing neutrophil extracellular traps (NETs) capable of trapping pathogens and cleansing the wound through their engulfment by neutrophils. However, an imbalanced response in the case of NETosis within the wound can also cause direct damage to the epithelium and endothelium, thereby delaying the wound healing process [12].
In the case of diabetic wounds, elevated blood glucose levels adversely affect the regulation of growth factors, subsequently impairing cell proliferation and differentiation. This results in phenotypic abnormalities within the structures of the dermis and epidermis. Fibroblasts in diabetic wounds exhibit resistance to proliferation, and this, coupled with their accelerated aging process, contributes to poor wound healing. High glucose levels promote accelerated cell growth and the accumulation of oxidized protein forms in fibroblasts, which ultimately leads to skin atrophy and dermatosis due to the accumulation of advanced glycation end products (AGE) [13].
AGEs are a group of compounds formed under conditions of excessively high blood glucose levels, resulting from the condensation reaction between glucose and proteins or from the action of reducing sugars on lipids and nucleic acids [14]. AGEs are responsible for the glycosylation of collagen and the formation of cross-linked, difficult-to-degrade protein products, which ultimately leads to delayed angiogenesis and tissue remodeling. Aging processes reduce cell proliferation and blood flow in tissues, contributing to the degradation of extracellular matrix components and cell apoptosis [15].
In patients with diabetic wounds, a low density of blood vessels results in hypoxia and nutritional deficiency at the wound site. Moreover, a significant reduction in the density of growth factor receptors on the wound hinders their normal regulatory function, slowing the rate of skin regeneration [16]. The insufficient angiogenesis observed in diabetic wounds is due to the elevated concentrations of antiangiogenic factors present in the circulatory system of patients with diabetic foot ulcers. These factors weaken proangiogenic stimuli and induce changes in capillary maturation factors, leading to a slower maturation of these vessels in the reconstructed tissues. Additionally, the diabetic condition causes a deficit in the number of endothelial progenitor cells (EPCs) derived from the bone marrow, further contributing to reduced tissue vascularization of the tissue. In diabetic patients, EPCs show a reduced ability to produce functional angiogenic structures in ischemia models, which adversely affects the formation of granulation tissue, capillary growth, and collagen deposition in the wound [17].
Diabetic wounds are also particularly prone to bacterial colonization due to
elevated glucose levels in the blood, which serves as an energy source for
bacterial growth and reproduction. Pathogenic bacteria adhere to the wound
surface and subsequently form multicellular aggregates, leading to biofilm
formation. The presence of a biofilm in a wound significantly reduces the
effectiveness of antimicrobial agents due to several factors: their inability to
penetrate the biofilm matrix, the lack of intracellular accumulation of
antibiotics, the presence of metabolically inactive bacteria, and the development
of antibiotic resistance. Furthermore, biofilms increase the likelihood of
transferring virulence and antibiotic-resistant genes between bacteria, and the
rate of genetic mutations in biofilms is higher than in free-living cells.
Additionally, bacterial cells within biofilms can develop an intracellular
communication mechanism known as quorum sensing (QS), which helps protect them
from immune cells attack and antibiotic action. Cells from the biofilm can detach
and spread throughout the wound, forming multimicrobial biofilms that facilitate
mutual growth. In the context of diabetic foot disease, the best-studied
interaction is between Staphylococcus aureus and Pseudomonas
aeruginosa, where substances produced by P. aeruginosa protect
S. aureus, complicating the treatment of infections caused by these
bacteria [18]. An interaction between P. aeruginosa and S.
aureus contributes to increased antibiotic tolerance, the ability to form
biofilms, and the secretion of virulence factors. In the case of P.
aeruginosa, these factors include hydrogen cyanide, exoenzyme S, exotoxin A, and
pyocyanin, while for S. aureus, they include Panton-Valentine leukocidin
(PVL) and
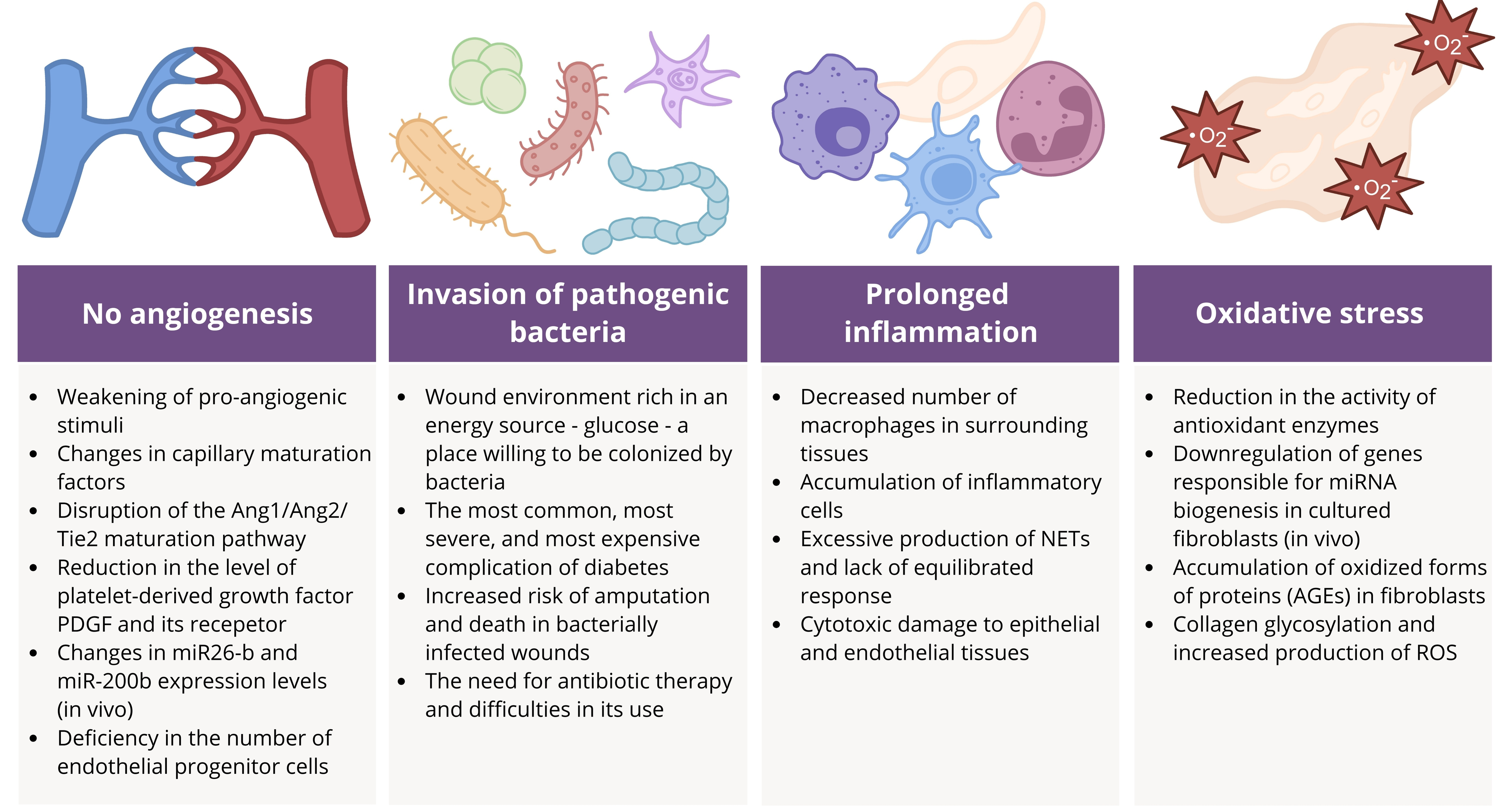 Fig. 2.
Fig. 2.
A summary of the most important factors determining the prolonged healing of diabetic wounds. Under diabetic foot ulcer (DFU) conditions, there is an unbalanced accumulation of immune cells, as well as an increase in the M1/M2 macrophage ratio, reactive oxygen species (ROS), and pro-inflammatory cytokines. Furthermore, reepithelialization and angiogenesis occur rarely, unlike in bacterial infections, ultimately leading to chronic, non-healing wounds that remain in a state of low inflammation: angiopoietin-1 (Ang1), angiopoietin-2 (Ang2), tyrosine kinase (Tie2), micro-ribonucleid acids (miRNA: miR26-b and miR-200b), neutrophil extracellular traps (NETs). The image was created with Inkscape v1.4, retrieved from https://inkscape.org.
Dressings are selected based on various wound characteristics, including type, depth, location, extent, amount of exudation, presence of infection, and tissue adhesion. Standard dressings such as gauze, fibers, plasters, bandages, and cotton wool have been used for years on wounds with either normal or abnormal healing processes. Gauze and bandages, typically applied to dry and well-cleaned wounds, are primarily used for mechanical tissue protection. Gauze dressings absorb secretions from open wounds, while natural cotton bandages are mainly used to treat dry venous and arterial ulcers. However, wounds with a large amount of exudate necessitate frequent changes, which can result in discomfort and pain for the patient, as well as additional irritation of the wound [23, 24].
In the treatment of diabetic wounds, semipermeable porous polyurethane dressings are often utilized, as they allow gases and water vapor to pass through while blocking fluids and bacteria. Their thinness, flexibility, and ease of conformation make them ideal for epithelial and superficial wounds with low exudate, as well as for lacerated or shallow wounds. However, due to their lack of absorbency, they are not suitable for wounds with high exudation, as this can lead to excessive secretion and maceration of the wound edges, necessitating frequent dressing changes, sometimes several times a week [24, 25]. Alternatively, foam dressings are used, which consist of a polyurethane or silicone core surrounded by a semi-occlusive outer layer. Foams can remain on the wound for several days without risking tissue maceration. The hydrophobic outer layer protects against fluids and bacteria while facilitating gas exchange. The foam structure allows it to conform to the shape of the wound, and its absorbent and autolytic properties make it appropriate for moderately to heavily exuding wounds, leg ulcers, and granulating wounds [23, 24]. Another type of dressing is hydrocolloids, which comprises an inner layer of hydrophilic colloidal particles and an outer layer of polyurethane. Hydrocolloids prevent the penetration of water and bacteria but they are impermeable to oxygen, which limits their use in deeper, heavily exuding, or infected wounds. Additionally, they are less transparent, making it challenging to inspect the wound, and the gel formed during use can be mistaken for an infection. Hydrocolloids are primarily used in the treatment of superficial wounds, postoperative wounds, and shallow pressure ulcers [26].
Dressings are selected based on various wound characteristics, such as type, depth, location, extent, amount of exudation, presence of infection, and tissue adhesion. Although traditional dressings fulfil basic functions, they do not provide adequate wound drainage. As a result, they are being replaced by modern solutions that actively support the healing process by accelerating the formation of granulation tissue and facilitating the migration of epithelial cells from the edges of the wound to its center [24, 27].
The most fundamental aspect that must be achieved by a hydrogel in its application as a medical device is biocompatibility. Biocompatibility is defined as the ability of a biomaterial to perform specific functions while eliciting an acceptable tissue response from the body. For a biomaterial to be considered biocompatible, it must meet the criteria specified in the International Standards Organization (ISO) 10993 standard. These requirements include not only the lack of cytotoxicity but also the exclusion of potential carcinogenic and mutagenic properties of the material. Moreover, the biomaterial should not cause allergic reactions, and in the case of materials that come into contact with blood, it is essential to ensure their athrombogenicity [28]. Additionally, in the design and production of products made from biomaterials, it is necessary to consider all aspects that determine their suitability for a specific purpose and function. For hydrogel materials, these aspects primarily include chemical, physical, mechanical, and rheological properties, as well as those related to morphology and biological activity [29].
The ideal wound dressing system should maintain high humidity, which provides nutrients and protection while facilitating cell growth and migration. Moist treatment prevents scar formation, allowing epithelial cells to close the wound more quickly. The dressing should be easy to remove without irritating the wound or causing pain; it should offer mechanical protection, proper gas and vapor exchange, and be non-toxic and non-allergenic. Additionally, it should be impermeable to bacteria and support tissue regeneration, enabling the delivery of therapeutic substances. Furthermore, it should be affordable, easy to produce, and readily available. All of these features can be achieved by using carefully designed hydrogel dressings [30, 31].
Hydrogel dressings are highly regarded for their superior properties compared to traditional bandages and gauze, which do not maintain a moist environment and can cause irritation to wounds. Due to their elasticity and softness, hydrogels easily adapt to soft tissues and are particularly effective in treating deep wounds with irregular shapes. They provide a moist environment, absorb exudate, and support tissue homeostasis. Their three-dimensional, porous structure mimics the natural extracellular matrix, promoting fibroblast proliferation, epithelialization, neovascularization, and new tissue remodeling. Hydrogels can be modified through the addition of antibacterial, antiviral, and antifungal agents, growth factors, biomolecules, or cells. Currently, functional hydrogel dressings are being developed with antimicrobial, anti-inflammatory, and antioxidant properties, as well as the capability for controlled delivery of substances in response to stimuli [32, 33].
Insulin is a peptide hormone composed of 51 amino acids, with a total mass of
5808 Da. The synthesis of insulin is carried out by the
The general anti-inflammatory properties of insulin are derived from metabolic
synthesis pathways that regulate cell proliferation, survival, migration,
anti-inflammatory activity, and angiogenesis. Insulin receptors—specifically
insulin receptor substrates (IRS-1 and IRS-2), extracellular signal-regulated
kinase (ERK), and protein kinase B (Akt)—located in keratinocytes and epidermal
fibroblasts, are upregulated in wounded skin compared to intact skin, indicating
a potential role of the insulin signaling pathway in wound healing. The effects
of insulin on wound healing include an increased expression of laminin
(alpha3beta1) integrin receptors in keratinocytes and increased levels of Laminin
332 (LN332). Local administration of insulin to skin wounds has been shown to
stimulate the migration and proliferation of fibroblasts and endothelial cells,
as well as the production of extracellular matrix proteins. Additionally, insulin
supports keratinocyte migration in a dose-dependent manner by activating the
nuclear transcription factor kappa B (NF-
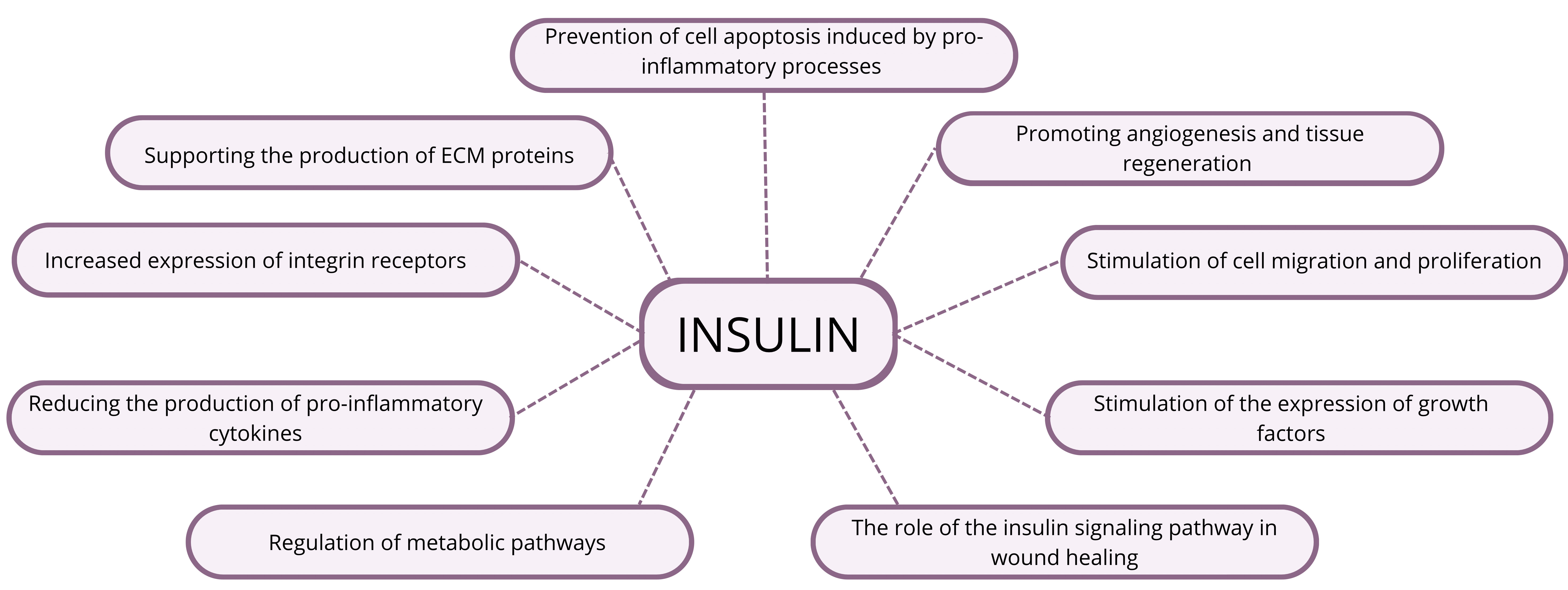 Fig. 3.
Fig. 3.
The effect of insulin in wound treatment. There are many ways in which insulin affects the treatment of diabetic wounds from supporting Extracellular Matrix (ECM) protein production, through regulation of metabolic pathways and stimulation of cell migration and proliferation, to promoting angiogenesis and tissue regeneration. The image was created with Inkscape v1.4, retrieved from https://inkscape.org.
The positive effect of insulin on the processes occurring during the inflammatory and proliferative phases has been recognized by researchers looking for its potential use in the treatment of chronic wounds. However, the local administration of insulin in an aggressive wound environment is a major challenge due to the presence of degrading proteases, the need to control or self-regulate insulin delivery, the need to overcome natural barriers and the selection of the appropriate formulation. The main issue in delivering insulin to diabetic wounds is the impact of proteases present in the wound, which perform insulin proteolysis upon contact, disturbing the tertiary conformation of the protein and leading to a loss of its bioactivity. The primary requirements and difficulties associated with insulin delivery to diabetic wounds are summarized in Fig. 4. Therefore, methods that protect against the proteolytic degradation of insulin in tissues are highly desirable. Currently developed solutions in the form of injectable hydrogel systems and the use of micro- and nanocarriers provide opportunities for the effective delivery of insulin to diabetic wounds [37].
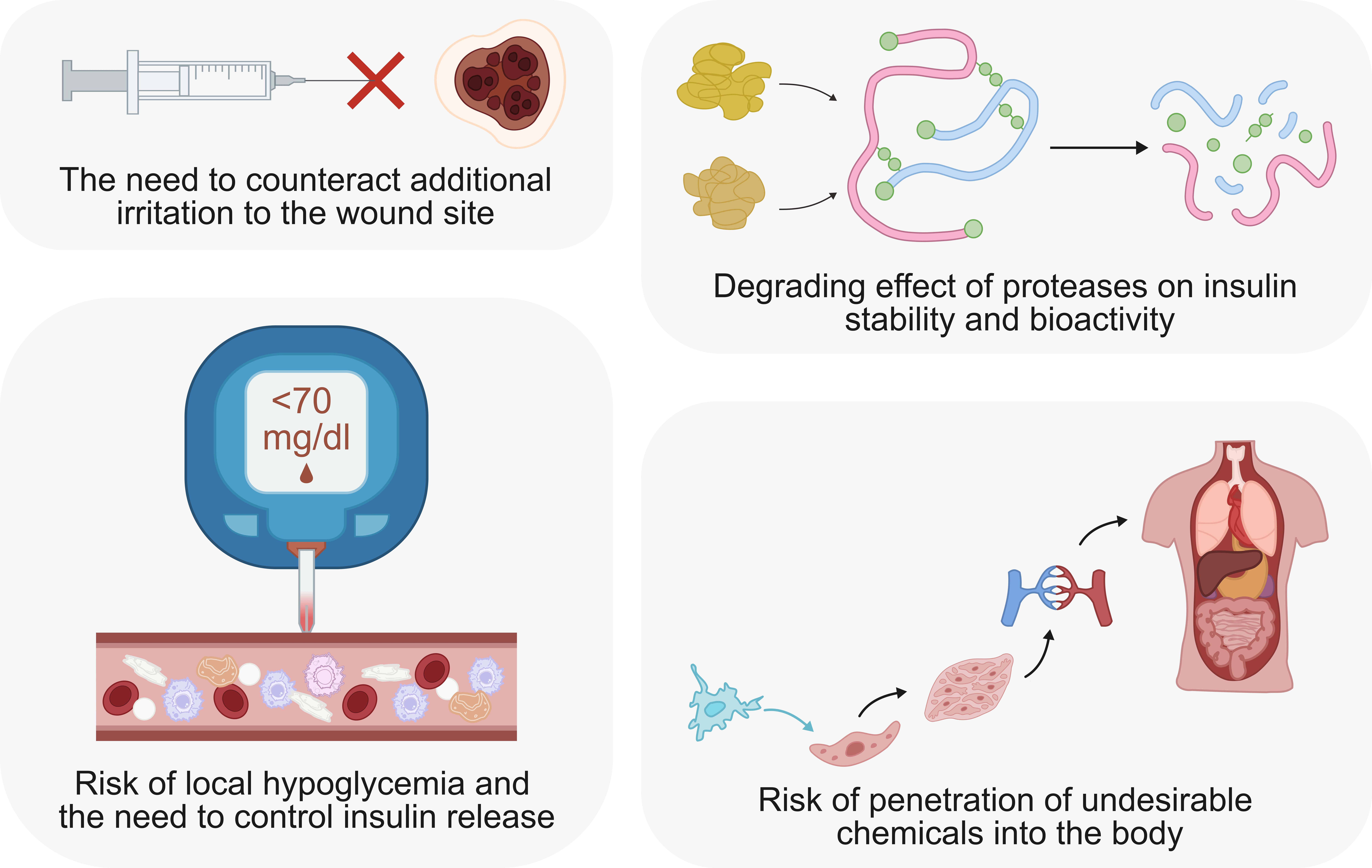 Fig. 4.
Fig. 4.
The most important requirements and difficulties in delivering insulin to diabetic wounds. Insulin delivery to the diabetic wound site should be realized as non-invasively as possible, keeping in mind that insulin levels and release rate should be tightly controlled, along with assurance of its stability and bioactivity. The image was created with Inkscape v1.4, retrieved from https://inkscape.org.
In chronic wounds, there is increased activity of proteolytic enzymes such as matrix metalloproteinases (MMPs) and serine proteases, which degrade the extracellular matrix and destroy growth factors and their receptors. This, in turn, contributes to a limited supply of growth factors in the wound area, resulting in impaired healing. In the context of diabetic wounds, the proteolytic enzyme that exhibits increased activity is the insulin-degrading enzyme (IDE), which leads to a local deficiency of normally occurring insulin in the tissues, thereby delaying tissue healing. Conversely, in wounds that are undergoing the healing process, IDE activity decreases as healing progresses, similar to the changes in the levels of proinflammatory cytokines. Nevertheless, the presence of insulin-degrading proteases is the primary reason for the necessity of protecting insulin from biodegradation during local delivery [38].
An equally important aspect related to the delivery of insulin to diabetic wounds is its controlled release. A too rapid release of insulin into the wounds may lead to the development of local hypoglycemia, and once it penetrates into the muscles and circulatory system, it can disrupt glucose homeostasis throughout the body. To counteract this, systems with prolonged insulin secretion and insulin release in response to stimuli are employed. To overcome the above limitations, several drug delivery systems have been developed to control the pharmacokinetic profiles of various analogs. Therapeutic efficacy depends on many factors related to pharmacokinetics, distribution, cellular uptake, metabolism, excretion, and toxicity, all of which are influenced by the method and route of administration. The main goals of developing these systems are to improve the stability of therapeutic substances in vivo, increase the control of their release in response to stimuli, and direct the action of drugs to a specific site [39, 40]. In a clinical study reported by Z. Zhang et al. [41], it was demonstrated that in most individuals with developing diabetic foot syndrome, the condition of the wound improved following insulin injection into the wound. However, among the 32 participants studied, characteristic symptoms of hypoglycemia were observed in two cases, which included palpitations, dizziness, pallor, and cold sweats. Additionally, the study indicate that local injection of insulin into the wound can both reduce systemic blood glucose levels and enhance wound closure, shorten healing time, and improve wound remodeling by modulating inflammation, accelerating epithelialization, and promoting neovascularization [41]. In other clinical study where insulin was formulated in solutions, sprays, creams, or dressings, no adverse systemic effects (such as hypoglycemia, hypokalemia, or hypoaminoacidemia) or local adverse effects (including infection, pain, or allergenicity) were noted. Considering the aforementioned factors, it is essential to develop a continuous delivery system for this hormone to minimize the risk of local hypoglycemia and enhance patient comfort, thereby eliminating the need for injections [42].
At the same time, taking biomechanical aspects into account, injectable systems are being developed to counteract additional irritation at the site and address the need to treat very complex and deep wounds. These systems utilize materials that consist mainly of biodegradable and biocompatible soft polymers, which are available in the form of hydrogels, microspheres, microgels, and gels cross-linking in situ [43]. The use of injectable materials in the form of dressings, which also enable self-regulating insulin delivery, allows for the treatment of very deep tissue defects. Injectable dressings perfectly conform to the edges of these defects, fill them, are minimally invasive, reduce the risk of irritation, and minimize the risk of hypoglycemia [44].
When administering insulin via injection, oral methods, or transdermal means, it is essential to protect this peptide from enzymatic degradation. Delivering insulin in its unchanged form is undesirable due to its low bioavailability, which results from rapid hormone degradation caused by enzymes. This necessitates the use of higher doses, consequently increasing the risk of local hypoglycemia. To mitigate this risk, micro- and nanocarriers are developed to safeguard insulin against degradation, facilitate the use of smaller doses, and ensure controlled, gradual release to the target site, thus eliminating the burst effect [45]. In comparison to traditional insulin delivery systems, encapsulating insulin in organic or inorganic nano- and micro-delivery vehicles can significantly enhance its pharmacological properties, such as solubility, blood half-life, and toxicity, leading to safer and more effective therapy [46].
Such carriers can be designed to increase therapeutic efficacy and minimize side effects, protect against premature degradation and denaturation upon contact with the physiological environment, enhance penetration through physiological barriers like the skin, and incorporate stimuli-responsive elements that enable controlled substance release on demand [46]. Additionally, nanoparticle carriers may offer further benefits, such as enhancing drug stability and reducing skin irritation that can occur with certain medications. Nanoparticles effectively shield peptides from the action of skin peptidases, directing their delivery to the skin or within it [47]. This capability is attributed to the unique properties of nanomaterials, including a high surface-to-volume ratio and specific shape factors resulting from their small size compared to bulk material [45].
Liposomal and polymeric micro- and nanocarriers made from biocompatible, bioavailable, and biodegradable components have demonstrated improved therapeutic outcomes compared to traditional methods. Furthermore, the process of both covalent and non-covalent attachment of polyethylene glycol polymer chains to molecule (PEGylation) of these carriers enhances drug solubility, reduces immunogenicity, decreases dosing frequency, and prolongs serum half-life. Therefore, PEGylation is considered one of the key strategies in local insulin delivery [45]. Currently, systems utilizing micro- and nanocarriers embedded in hydrogel matrices are being developed as dressings for diabetic wounds. Due to their unique microstructure and high water content, these carriers better mimic the surrounding soft tissues and support their regeneration compared to conventional dressings, such as hydrocolloid patches or semi-permeable polyurethane foam dressings [24, 25].
Such systems have been developed by numerous teams, including scientists from the group of H. Wang et al. [48], who created a microgel containing chitosan microspheres with insulin. The preparation process involved transferring a solution of chitosan and acetic acid along insulin through a glass membrane into an emulsion of paraffin and ether with the emulsifier. Cross-linking of the emulsion and the formation of the microgel was achieved by adding tripolyphosphate, while the hardening of the chitosan droplets was conducted using glutaraldehyde. In vitro study demonstrated that the solidification state of the microgel could be adjusted based on the encapsulation efficiency, the shape of the microspheres, the activity of the drug, and the insulin release profile.
Another example is the system of poly(lactide-co-glycolide) nanoparticles loaded with insulin and suspended in a structured hydrogel of poly(vinyl alcohol)-borate, obtained by the group of Abdelkader [49]. This material effectively contributed to the improvement of the wound healing process. Similar effects were demonstrated by the complex of chitosan nanoparticles with insulin.
In another study, J. Zhu et al. [50] developed gels based on oxidized hyaluronic acid and succinyl chitosan, integrating them with insulin-containing micelles. This system demonstrated the ability to stimulate inflammatory cell proliferation, angiogenesis, and wound maturation. Additionally, it was shown that the combination of both types of polymers using the applied procedure led to the formation of a hydrogel with improved mechanical properties. Scientists from Lee’s team [51] also obtained an injectable form of hydrogels, developing a material based on trehalose that ultimately protected the encapsulated insulin against thermal degradation. The polymer used in this study, containing trehalose side chains with poly(ethylene glycol), was functionalized with phenylboronic acid (PBA) [51]. This resulted in a hydrogel that cross-links after injection and responds to glucose concentration, releasing insulin in its presence. Moreover, thanks to trehalose, the hydrogel provided excellent protection against heat stress for insulin, which opens up the potential use of this material without the need for cooling.
In a recent study from 2024, F.C. Zanchetta and the team [52] recognized the potential of insulin-polysaccharide formulations in biohybrid hydrogel systems for regulating oxidative stress and inflammatory responses. They developed a hydrogel-based system containing insulin, chitosan, and hydroxypropylmethylcellulose (Chi/HPMC/Ins), which synergistically combined the bioactivity of the protein with the biocompatibility and hydrogel properties of polysaccharides. The resulting biomaterial exhibited no cytotoxicity, promoted faster gap closure in the scratch test, and in in vivo tests demonstrated that wounds treated with Chi/HPMC/Ins hydrogel led to faster wound closure, formation of more organized granulation tissue, and hair follicle regeneration.
In another study, C-H. Lee’s team [53] developed absorbable and biocompatible
PLGA-based core-shell nanofibrous membranes that sustainably released
insulin/vildagliptin for two weeks and at least four weeks, respectively. The
functional and sustained delivery of vildagliptin increased the migration rate of
endothelial progenitor cells (EPCs) and improved the healing of diabetic wounds.
The obtained nanofibrous scaffolds increased epidermal thickness, promoted wound
closure, and reduced the expression of
In a study conducted by X. Gao’s team [54], Michael addition was used to internally cross-link bioactive maleated chitosan/thiolated hyaluronan (mCH/tHA) multilayer coatings on poly(L-lactic acid) (PLLA) nanofibrous mats (referred to as P-mCH/tHA), aiming to achieve sustained insulin release (IN). Physicochemical studies showed that P-mCH/tHA demonstrated higher tensile strength, an accelerated degradation rate, greater antibacterial activity, and sustained insulin release compared to P-CH/HA and pure PLLA mats. Moreover, P-CH/HA displayed improved adhesion, spreading, and proliferation of mesenchymal stem cells in comparison to other PLLA mats. In vivo studies conducted in a mouse model of diabetes revealed that P-mCH/tHA_IN facilitated the fastest wound closure among all groups, promoting reepithelialization, angiogenesis, and increased collagen deposition in wounds. This suggests that the coating combined with IN is promising for the development of new bioactive wound dressings.
In the work of L. Fang et al. [55], a thermosensitive hydrogel,
poloxamer (Pox), was applied topically to the wound in combination with insulin
injection to investigate improvements in wound healing. Compared to the control
animals (healthy mice), those treated with poloxamer plus insulin (Poxin)
exhibited accelerated wound closure and healing rates; the expression of both
alpha-smooth muscle actin (
Glucose-responsive hydrogels are particularly beneficial in the treatment of chronic diabetic wounds, where the skin repair processes are impaired due to elevated blood glucose levels. Hyperglycemia induces chronic inflammation, alters the angiogenesis process, and increases the production of glycation end products, resulting in severe oxidative stress conditions. Hence, hydrogels that release insulin in response to high glucose concentration in the wound have significant potential for application in diabetic wound treatment [56]. Glucose-responsive hydrogels can be categorized into three types based on the responsive agent employed: glucose oxidase (GOx), concanavalin A (Con A), and phenylboronic acid (PBA) groups. These delivery systems release insulin via glucose-induced changes in binding capacity or structural alterations, such as matrix swelling or shrinkage, material dissolution, changes in pore size, or degradation [57, 58].
A summary of the mechanisms of action of glucose-sensitive hydrogels is depicted in Fig. 5. Glucose oxidase is a naturally derived enzyme comprised of glycoproteins that catalyzes the oxidation of glucose to gluconolactone, generating hydrogen peroxide (H2O2) as an intermediate. Gluconolactone is then hydrolyzed to gluconic acid in an aqueous environment, resulting in a local decrease in glucose levels and pH, which limits local hyperglycemia and the proliferation of pathogenic bacteria (Fig. 5A). However, the generation of H2O2 as a byproduct results leads to reduced oxygen levels and increased tissue hypoxia, an undesirable effect. Therefore, in most hydrogel systems that incorporate this enzyme, local physicochemical changes in the environment, such as pH, H2O2 concentration, or oxygen levels, are used for the controlled release of insulin. The use of hydrogels sensitive to pH or H2O2 changes loaded with GOx allows for a more controlled release of insulin while minimizing the side effects associated with elevated concentrations of H2O2 and gluconic acid, such as increased oxidative stress, tissue hypoxia, and reduced GOx activity [57].
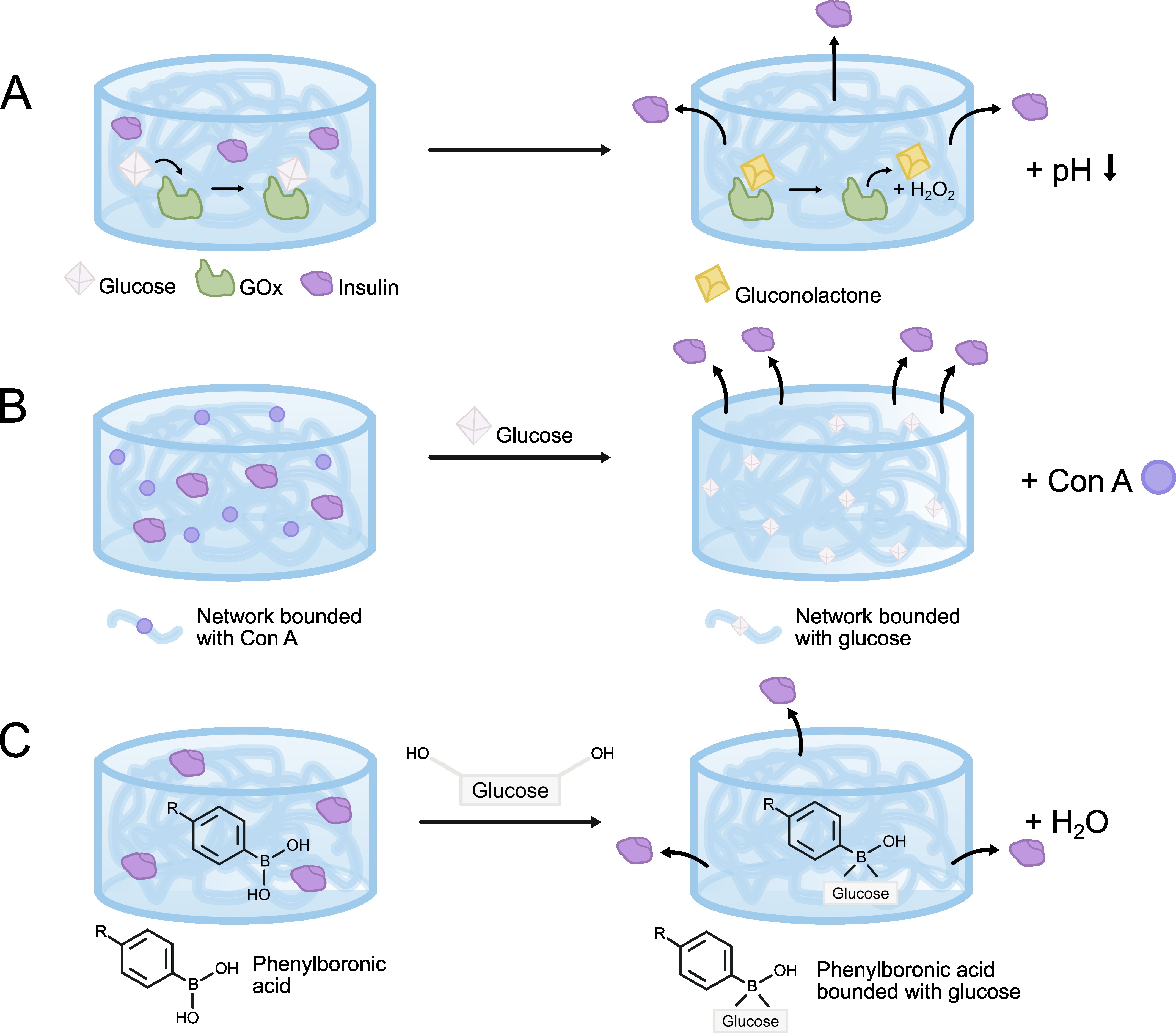 Fig. 5.
Fig. 5.
Release of insulin under the influence of glucose from a hydrogel loaded with different compounds. (A) glucose oxidase (GOx) in direct contact with glucose, oxidizing to gluconolactone, which is then hydrolyzed to gluconic acid, resulting in a local decrease in glucose and pH. (B) Concanavalin A (Con A) creates tight hydrogel network with entrapped insulin when glucose penetrates the polymer matrix, competitive binding of glucose with Con A occurs. (C) Phenylboronic acid (PBA) is a synthetic equivalent of the glucose-sensitive agent with an interesting ability to form reversible covalent complexes with diols. The image was created with Inkscape v1.4, retrieved from https://inkscape.org.
One example of such a system is an injectable microgel consisting of a network of dextran nanoparticles, developed by L.R. Volpatti’s team [59]. In the process of creating a porous network, alginate and chitosan were used to coat acid-sensitive dextran, resulting in both positively and negatively charged particles. The resulting nanosheet was then modified by degradation in an acidic environment to coat it with insulin, catalase, and GOx. The hydrogel functioned based on the disintegration of the nanosheet in the presence of hyperglycemia, leading to the simultaneous release of insulin. Another example is the biomaterial developed by J. Yang et al. [60], who designed a glucose-responsive, multifunctional, injectable, self-healing drug-loaded metal-organic hydrogel (DG@Gel) that responds to the presence of glucose via the loading of glucose oxidase. When injected into a diabetic wound, GOx in DG@Gel altered the hyperglycemic wound microenvironment by decomposing excess glucose into hydrogen peroxide and glucuronic acid, which lowered the wound pH. The reduced pH promoted the release of zinc ions and deferoxamine mesylate (DFO), displaying both antibacterial and angiogenic activity in diabetic wound healing. In vitro studies revealed the antibacterial activity of DG@Gel and its ability to promote cell proliferation, migration, and tube formation, while in vivo studies showed that DG@Gel could induce reepithelialization, collagen deposition, and angiogenesis during wound healing in diabetic mice, with good biocompatibility and biodegradability. The results suggest that this hydrogel is a promising innovative dressing for treating diabetic wounds.
Concanavalin A (Con A) belongs to the lectins, a class of carbohydrate-binding proteins that are used as natural receptors in the formation of glucose-responsive hydrogels. Systems for glucose-regulated insulin release based on Con A are based on physical cross-linking of Con A within a glycosylated backbone that contains insulin. Con A physically binds to the glycosylated functional groups of the hydrogel network, creating a tightly complex matrix with small pores that effectively traps insulin within the hydrogel. When glucose penetrates the polymer matrix, competitive binding occurse between glucose and Con A. Due to the higher affinity of Con A for glucose compared to glycosylated groups, glucose replaces the glycosylated polymer. This process leads to the degradation of the hydrogel network, which is manifested through its swelling and the release of insulin by diffusion or transition from gel to sol phase (Fig. 5B). Unfortunately, this mechanism is characterized by a relatively slow reaction time and a slow release of Con A from the hydrogel, thus limiting the therapeutic potential of the system. To address this, modifications are implemented to increase stability by conjugating Con A with poly(ethylene glycol) chains. This results in a more hydrophilic and stable Con A system, showing improved solubility, stability, and affinity for glucose, which improves the sensitivity of the hydrogel and reduces the lag time of the release reaction. A similar improvement is achieved through the covalent immobilization of Con A in the hydrogel matrix via carbodiimide cross-linking, which prevents the leaching of Con A from the polymer, thereby increasing the stability of the gel and allowing for repeatable swelling behavior [57, 61].
An example of such a solution is provided by the work of R. Yin et al. [62], who employed the reverse phase emulsion cross-linking technique to create glucose-sensitive microgels using Con A. The study explored the potential of using microgels cross-linked with genipin (ConA/GEA-Cs) as a glucose-sensitive drug delivery system [62]. In this research, the polymeric ligand for Con A was prepared as an acrylated glucosyloxyethyl derivative of chitosan (GEA-Cs). This strategy facilitated rapid cross-linking of the hydrogel bound to ConA via genipin, contributing to the increased stability of the system [62]. The study demonstrated that insulin released from this system retained its tertiary structure, thus preserving its bioactivity [62].
Despite their ubiquity and excellent glucose selectivity, GOx and Con A, as protein-based systems, are susceptible to environmental changes and are typically characterized by antigenicity, instability, and high costs. Consequently, they are not suitable for long-term storage or use. Hence, more stable hydrogels are being developed, using phenylboronic acid as a synthetic equivalent of the glucose-sensitive agents (Fig. 5C). One of the most significant chemical properties of boronic acids, which has expanded their application in medical devices, is their ability to form reversible covalent complexes with diols. When glucose, which contains a diol functional group, enters the hydrogel, phenylboronic acid residues form reversible complexes with it, shifting the equilibrium towards positively charged boron residues. This reaction alters the overall charge density of the gel, increasing the proportion of cationically charged residues. The increased charge enhances the hydrophilicity of the hydrogel, which, combined with ionic repulsion within the gel, leads to a pronounced swelling reaction. Conversely, the reaction of boronate anions with a diol leads to the formation of a complex that shifts the equilibrium towards the hydrophilic and negatively charged PBA. This glucose-dependent change in the ratio between uncharged and charged borates influences the solubility of the polymer, providing the basis for the release of diol-sensitive insulin.
Two forms of boronic acids create esters with diols through the loss of water: one form has the parent hydroxyl group replaced by carbon substituents while the other has two hydroxyl groups substituted by carbon. Unfortunately, the bond between neutral boronic acid and diols is also considered hydrolytically unstable due to their high susceptibility to hydrolysis. Additionally, PBA is less selective for glucose than GOx and Con A. Nevertheless, systems based on the use of phenylboronic acid in glucose-sensitive hydrogels, compared to those based on GOx and Con A proteins, are characterized significantly higher reactivity, long-term stability, and the possibility of long-term storage [61, 63]. Consequently, numerous studies are being conducted to develop glucose-sensitive hydrogels that employ phenylboronic acids. For example, Y. Dong et al. [64] developed an injectable stimuli-responsive hydrogel based on the complexation of glucose and boronic acid. The hydrogel showed shear-thinning and self-healing properties, rapidly transitioning from a gel to a fluid state in response to shear, and demonstrated controlled release in vitro in response to glucose concentration. In another study, Z. Guo et al. [65] developed a stimuli-sensitive microneedle hydrogel dressing with unique glucose-responsive phenylborate groups through the in situ copolymerization of gelatin methacrylate, the glucose-responsive monomer 4-(2-acrylamidoethylaminoformyl)-3-fluorobenzeneboronic acid (AFPBA), and gluconic insulin (G-insulin). The resulting material showed controlled glucose-dependent insulin release, and in in vivo studies conducted on mice with streptozocin-induced type I diabetes, insulin release was found to reduce inflammation, increase collagen deposition, and improve the hyperglycemic wound environment, thereby accelerating the wound healing process.
In another work, Z. Xu’s team [66] utilized gallic acid (GA), known for its
strong antioxidant properties, to modify chitosan (CS) chains by incorporating
them into a hydrogel based on poly(ethylene glycol) and diacrylate (PEG-DA),
creating a new hybrid antioxidant hydrogel (PEG-DA/CS-GA). Then,
polyethyleneimine (PEI) was modified with glucose-sensitive phenylboronic acid
(PBA) to load insulin (PEI-PBA/insulin NP). Insulin was immobilized in the
PEG-DA/CS-GA hydrogel via borate bonds between PBA and polyphenol groups on
CS-GA. Studies demonstrated that the PEG-DA/PEI-PBA/insulin/CS-GA (PPIC) hydrogel
exhibited excellent biocompatibility, antioxidant properties (DPPH removal rate
Diabetes, recognized as a civilization disease, is associated with numerous complications, among which diabetic wounds and Diabetic Foot Syndrome are some of the most challenging and costly to treat. Current therapies and dressings, although they bring positive results, fall short of meeting the needs of patients. Hence, the use of hydrogel dressings that enable controlled insulin delivery to diabetic wounds demonstrates clear therapeutic potential, as discussed in this paper. Innovative bioactive hydrogel systems leverage the synergistic effect of insulin as a growth factor alongside the favorable properties of hydrogel matrices that support tissue regeneration.
Insulin delivery systems for diabetic wounds that utilize micro- and nanoparticles embedded in hydrogel matrices are particularly interesting. However, the application of such technologies is accompanied by certain limitations. One primary contraindication for using nanotechnology solutions is the risk of exacerbating allergic and inflammatory reactions caused by certain drug carriers. Nanoparticles can induce oxidative stress, autophagy, and apoptosis in keratinocytes and fibroblasts. The cytotoxicity of nanomaterials is influenced by factors such as particle size, shape, surface charge, stability, and concentration. Therefore, when developing new nanomaterials for wound healing, it is crucial to appropriately tailor their physicochemical properties to minimize toxicity to skin cells. This can be achieved by incorporating stabilizers and surfactants and selecting materials with low sensitizing potential. Moreover, studies show that nanomaterials can cause DNA damage and reduce gene methylation, suggesting a potential carcinogenic effect. The contact of nanomaterials with blood in wounds, resulting from blood vessel disruption, can lead to hemolysis. To mitigate this risk, the physicochemical properties of nanomaterials can be modified, or they can be coated with biologically active substances, such as phospholipids and polysaccharides. Therefore, current research on insulin micro- and nanocarriers should focus not only on their fundamental parameters, such as size, shape, stability, and drug encapsulation efficiency, but primarily on the surface modification of these structures. This may involve, for instance, incorporating active groups through chemical modifications or attaching polymer conjugates, proteins, or antigens that would offer protection to the carrier against an aggressive immune response. This approach would minimize the risk of the aforementioned side effects resulting from undesirable reactions of the body to nanomaterials.
Conversely, a significant limitation of hydrogel matrices that reduces their effectiveness as dressings is their poor mechanical properties and limited ability to adhere to tissues. For a hydrogel to adequately support wound regeneration, its microstructure must closely mimic the structure of the tissue, providing appropriate porosity to enable cell migration and proliferation, as well as possessing sufficient strength and stiffness to support proper cell differentiation. In the case of biodegradable hydrogels, the rate of degradation must be synchronized with the rate of new tissue regeneration, ensuring that the polymer structure diminishes concurrently with the formation of new tissue. Another challenge is to enhance the adhesion of the hydrogel to the wound edges and ensure its ability to fill the entire wound surface, irrespective of its complexity. Consequently, the design of hydrogel matrices should focus on enhancing these properties, which can be achieved through the use of nanoadditives or the development of new in situ cross-linking techniques, as exemplified by injectable hydrogels [67].
In the case of hydrogels that respond to glucose levels, it is crucial to achieve an effective insulin release process while maintaining appropriate mechanical properties of the gel and minimizing the content of reaction by-products. Current research on the use of glucose oxidase (GOx), concanavalin A (Con A), and boric acid (PBA) indicates that, although these systems provide the most controlled insulin delivery among the technologies currently being developed, they possess limitations that hinder further advancement. Therefore, an important direction for research is to explore methods to enhance the effectiveness of the response to glucose stimuli—either by introducing new factors or by modifying the structure of the hydrogel network. However, hydrogels also hold great potential as dressings due to their ability to perform dual functions: protecting wounds and serving as scaffolds for regenerating tissue, while supporting the processes of cell multiplication and proliferation through the controlled release of growth factors. Future work should also prioritize addressing the most urgent challenges, including the difficulties of encapsulating insulin and preserving its bioactivity during the loading and release process from carriers, as well as enhancing the mechanical properties of the resulting hydrogel matrices.
Concept and design: AK and PDP; Formal analysis: AK and PDP; Writing—initial draft: AK; Writing—review and editing: AK and PDP; Project administration: PDP. Both authors read and approved the final manuscript. Both authors have participated sufficiently in the work and agreed to be accountable for all aspects of the work.
Not applicable.
All graphics were prepared with Inkscape v1.4, retrieved from https://inkscape.org.
This study was supported by the subsidy (No 16.16.160.557) for the AGH University of Krakow.
The authors declare no conflict of interest.
References
Publisher’s Note: IMR Press stays neutral with regard to jurisdictional claims in published maps and institutional affiliations.





