1 Department of Obstetrics and Gynecology, Faculty of Medicine, Akdeniz University, 07070 Antalya, Turkey
Abstract
Recurrent ipsilateral ovarian torsion is uncommon; extreme recurrence (≥7 episodes) is exceptionally rare. Herniation of the adnexa through a broad ligament fenestration may precipitate torsion but is seldom reported. Optimal prevention of recurrence remains debated.
A 27-year-old woman with two prior vaginal births presented with acute right-lower-quadrant pain. Ultrasound showed an enlarged right ovary with absent color Doppler flow. She had seven prior right-sided torsions (2020–2024) managed surgically. Laparoscopy revealed a broad ligament fenestration on the right; the ovary had passed through this fenestration twice and undergone two 360° rotations on its axis. The ovary was delivered back through the window (reduction), detorsed, and oophoropexy was performed to the posterolateral uterine serosa; the broad ligament defect was closed. Pain resolved. At the 1-week and 3-month follow-ups, color Doppler ultrasound demonstrated normal perfusion, with no recurrence by 3 months.
In recurrent torsion with a broad ligament fenestration, reduction + detorsion + closure of the defect with uterine oophoropexy may represent a pragmatic, fertility-sparing strategy, although longer follow-up is needed to confirm durability. To our knowledge—considering prior reports of up to seven ipsilateral recurrences—this represents the first report of 8 right-sided torsion episodes.
Keywords
- ovarian torsion
- recurrent torsion
- broad ligament fenestration
- oophoropexy
- uterine fixation
- laparoscopy
Adnexal torsion accounts for about 2%–5% cases of gynecological emergencies and mostly occurs in the childbearing age group [1]. Recurrences have also been recorded, although there have been fewer cases, mostly in those who do not have a stabilizing mass, those who appear to have hypermobile adnexae, and in those who have lax ligaments [2]. Different surgical modalities have also been discussed in different studies in a bid to counter recurrence, and these include fixation of the uterus, truncation of the utero-ovarian ligament (UOL), round ligament fixation, and pelvic side-wall fixation [3].
Broad ligament defects are unusual and may allow an internal herniation of bowel and/or adnexa, and the recognition and closing of such defects are advocated in the prevention of recurrence [4].
We report an adult patient with eight events of right-sided torsion, in whom the presentation included double passage of the ovary through a broad-ligament fenestration. The treatment was successful, including detorsion, defect closure, and posterior uterine oophoropexy. In order to provide proper context in relation to the treatment provided, the present paper initiated a mini-review concerning the high recurrence rate in ovarian torsion. The essential part thereof has been summarized in Table 1 (Ref. [3, 5, 6, 7]).
| Study (year; journal) | Laterality | Age | No. of episodes | Prior fixation(s) | Definitive/last procedure | Outcome/follow-up |
| Brady & Styer (2015; Fertility Research & Practice) [5] | Right | 28 | 7 | Round-ligament oophoropexy (absorbable, failed); USL oophoropexy (absorbable, failed) | UOL truncation → interval USL oophoropexy (non-absorbable) | No recurrence at 45 months; six of the seven ipsilateral torsion episodes occurred within an 18-month interval. |
| Obut & Değer (2019; Case Reports in Obstet Gynecol) [3] | Left | 21 | 7 | Oophoropexy at 5th and 6th surgeries (failed) | Folded UOL fixed to the round ligament (novel technique) | Presented with a seventh ipsilateral recurrence. Normal Doppler at 2 and 4 months; symptom-free early follow-up. |
| Simsek et al. (2013; Eur J Obstet Gynecol Reprod Biol) [6] | Right | Young adult | 6 | Two failed oophoropexies (3rd & 5th lap.) | Combined approach after repeated failures | Managed at the sixth ipsilateral recurrence in a young adult with PCOS; technique detailed in the paper. |
| Ellison et al. (2024; Case Reports in Women’s Health) [7] | Left (ovary/tube) | 31 | 5 | Bilateral oophoropexy at 4th presentation | Detorsions ×4; later left ovary auto-amputated (late presentation) | Five ipsilateral presentations, including isolated tubal and tubo-ovarian torsion events; detorsions ×4; later left ovary auto-amputated (late presentation). Highlights lack of consensus on prevention and timing of fixation. |
Abbreviations: UOL, utero-ovarian ligament; USL, uterosacral ligament; PCOS, polycystic ovary syndrome.
Note: “No. of episodes” denotes the total number of distinct ipsilateral
torsion episodes per case (e.g., Brady & Styer [5]: 7 episodes, 6 within 18
months; Ellison et al. [7]: 5 presentations including both isolated
tubal and tubo-ovarian torsion events), not the number of axial twists within a
single episode. Selection limited to reports with
The reported cases are in accordance with the CARE guidelines. The manuscript has obtained written patient consent for the use and publication of their medical information. As a single patient report, there was no need for formal institutional review, and the manuscript was in accordance with the Declaration of Helsinki. In order to introduce the rationale and scope of our critical mini-review, the search included the use of the PubMed and PubMed Central search engines, focusing on the literature from database inception until August 2025. A combination of search terms and Boolean logic was used, focusing on the terms “ovarian torsion” and “fixation procedures, such as (“ovarian torsion” OR “adnexal torsion”) AND (“recurrent” OR “recurrence”) AND (“oophoropexy” OR “uterine fixation” OR “utero-ovarian ligament” OR “round ligament” OR “uterosacral ligament” OR “pelvic sidewall”) AND (“broad ligament defect” OR “fenestration”). The search was limited to English-language cases and case reports. After eliminating the duplicates, there were 15 references, and 9 were eliminated based on the full text, as they focused on subjects who had single torsion episodes, or those where there was lack of direct attention on the management of recurrent torsion. The remaining 6 studies were screened in their entirety, and 4 cases fit the inclusion criteria through the presentation of at least five instances of the condition in the patient through sufficient detail. These cases are recorded in Table 1. In the high-recurrence patient cases, the side, age, number, fixation, and definitive, ultimate procedure, and patient outcomes are recorded. In a supporting table, Table 2 (Ref. [3, 7, 8, 9, 10]), all adult procedure reports (regardless of the number) are reported, given the protocol and patient outcome measures were provided. These outcome measures included the conditions and indication in the patient, the oophoropexy steps, the patient torsion episodes, and the patient outcomes. The patient episodes were determined when they were distinct events.
| Study (year; journal) | Clinical setting/indication | Oophoropexy technique (key steps) | Episodes reported | Outcome/notes |
| Hartley et al. (2018; Case Reports in Obstet Gynecol) [8] | Adult recurrent torsion after prior detorsions | UOL plication and uterine or uterosacral fixation; technique note and rationale | Not focused on |
Supports uterine based fixation or UOL modification to prevent further events |
| Obut & Değer (2019; Case Reports in Obstet Gynecol) [3] | Recurrent torsion after failed oophoropexies | Folded UOL fixed to the round ligament (novel technique) | 7th episode (left sided) | Early follow up with normal Doppler; symptom free |
| Smorgick et al. (2023; J Pediatr Adolesc Gynecol) [9], Smorgick et al. (2020; Clin Exp Obstet Gynecol) [10] | Technique note/small series | Combined UOL plication with round ligament fixation | Technique oriented | Describes combined approach where single site fixation may have failed |
| Ellison et al. (2024; Case Reports in Women’s Health) [7] | Adult with multiple presentations of adnexal torsion | Bilateral oophoropexy described; timing and prevention discussed | 5 presentations (left ovary/tube) | Highlights lack of consensus on prevention and timing |
Notes: This table summarizes technique-focused reports irrespective of episode count, to contextualize fixation choices in adults.
The patient was a 27-year-old woman who had undergone two vaginal deliveries.
The patient came in with severe pelvic pain on the right side, measuring 10/10 on
the numeric pain scale, accompanied by nausea and vomiting. The patient had
received oral and IV NSAIDs in the last 12 hours with only partial relief. The
patient had undergone seven right-sided torsion operations between the years 2020
and 2024. These included four laparoscopic detorsions in February 2020, November
2020, April 2021, and December 2021, and three subsequent laparotomies in
November 2022, June 2023, and November 2024. The operative notes from these seven
procedures are listed in Table 3, describing the timing, type, important
operative findings, and the procedure performed. None of the procedures precluded
recurrence. The eighth recurrence was managed through a laparoscopy performed in
May 2025. The patient was found on presentation to have lower right quadrant
tenderness without evidence of peritoneal irritation, and her vital signs
remained stable. Laboratory work was notable for a WBC of 6.18
| Episode | Timing (month/year) | Surgical approach | Procedure/key intraoperative information | Broad ligament abnormality mentioned? | Interval to next torsion episode |
| 1 | February 2020 | Laparoscopy | Detorsion of right adnexa ( |
Not specifically mentioned; no defect documented | 9 months (to episode 2, November 2020) |
| 2 | November 2020 | Laparoscopy | Detorsion of recurrent right adnexal torsion ( |
Not specifically mentioned; no defect documented | 5 months (to episode 3, April 2021) |
| 3 | April 2021 | Laparoscopy | Detorsion of right adnexa ( |
Not specifically mentioned; no defect documented | 8 months (to episode 4, December 2021) |
| 4 | December 2021 | Laparoscopy | Detorsion of right adnexa ( |
Not specifically mentioned; no defect documented | 11 months (to episode 5, November 2022) |
| 5 | November 2022 | Laparotomy | Detorsion of right adnexa ( |
Not specifically mentioned; no defect documented | 7 months (to episode 6, June 2023) |
| 6 | June 2023 | Laparotomy | Detorsion of right adnexa ( |
Not specifically mentioned; no defect documented | 17 months (to episode 7, November 2024) |
| 7 | November 2024 | Laparotomy | Detorsion of right adnexa ( |
Not specifically mentioned; no defect documented | 6 months (to current 8th episode, May 2025) |
Note: Based on the summaries of the operative reports, the common feature of the
first seven procedures was detorsion
The transvaginal ultrasonography showed an enlarged right ovary measuring approximately 4–5 cm in size and peripheral follicles, with either absent or decreased color flow, minimal free fluid, and normal uterus and left ovary. The diagnostic laparoscopy revealed an approximately 3–4 cm fenestration in the right broad ligament. The right broad ligament fenestration is shown in Fig. 1. The right ovary had herniated through the window twice and completed two full turns on the pelvis. Herniation of the right ovary through the defect before reduction is shown in Fig. 2. The Fallopian tube was viable with normal color, the ovary was congested but viable, and the surface was dark red-blue and edematous, rather than black and necrotic. Post-detorsion, the ovary quickly turned pink and restored normal turgor. The elongated uterovarian ligament was also appreciated. The elongated UOL and adnexal orientation are illustrated in Fig. 3.
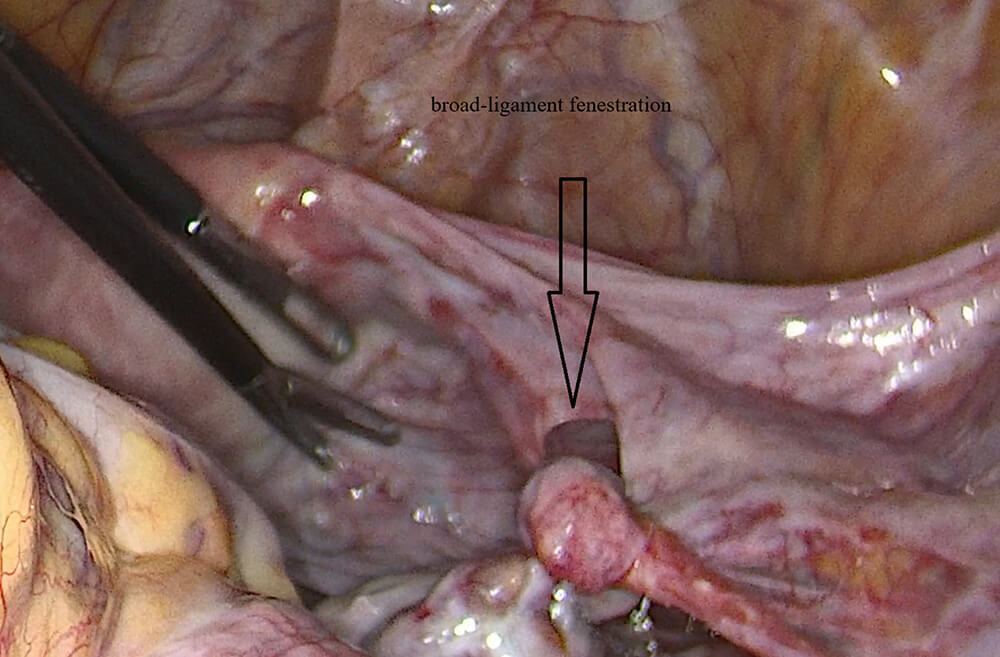 Fig. 1.
Fig. 1.
Broad ligament fenestration on the right.
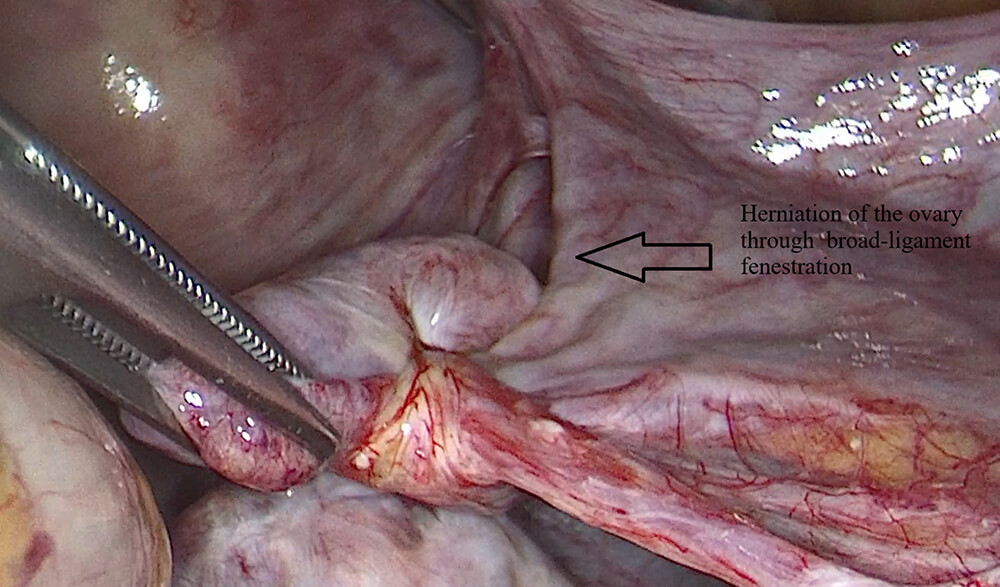 Fig. 2.
Fig. 2.
Herniation of the right ovary through the broad ligament fenestration before reduction.
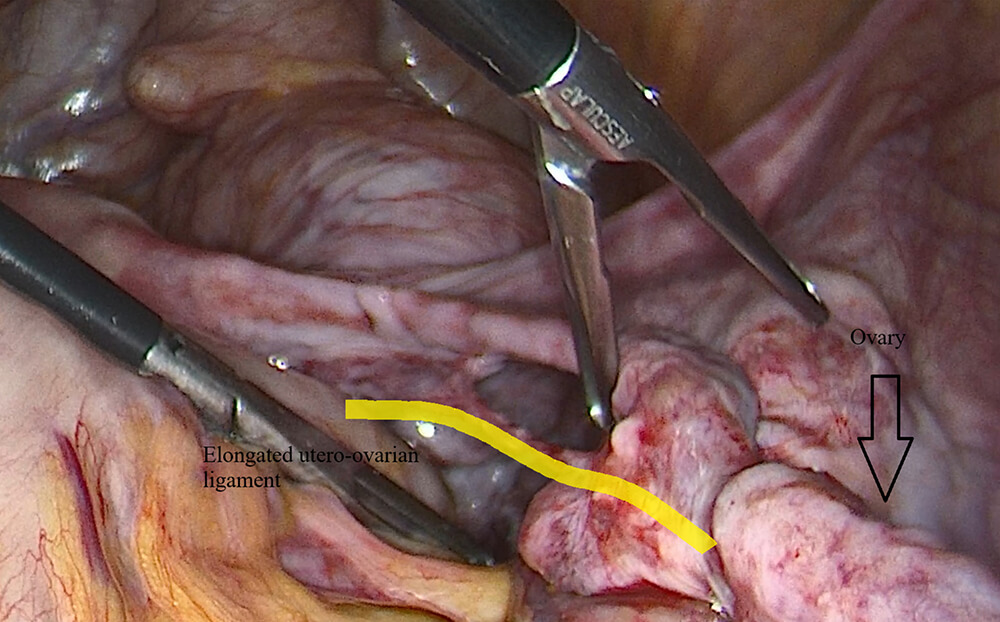 Fig. 3.
Fig. 3.
Elongated UOL and orientation of the adnexa. The thick yellow line highlights the elongated utero-ovarian ligament.
The ovary was then reinstated through the fenestration, reducing its size, and then detorsed using two counterclockwise turns, after which perfusion and turgor returned normally without the need for further intervention. Posterolateral oophoropexy of the uterus was carried out using United States Pharmacopeia (USP) 2-0 polyglactin 910 (Vicryl®) sutures, using superficial seromuscular sutures on the uterine serosa and matching mesovarian and ovarian sutures, keeping them away from the large vessels. The defects on the broad ligament were closed using USP 2-0 polyglactin 910 sutures, known as Vicryl. The ultimate placement can be seen in Fig. 4. The other side was examined and no defects on the broad ligament could be detected. There were no drains used, and the approximate blood loss was 250 mL. The patient was subsequently discharged on the second postoperative day. Approximately one week and three months later, the color Doppler scans revealed normal perfusion and venous flow, without recurrence at the end of three months. Written informed consent was obtained from the patient for publication of the clinical details and images.
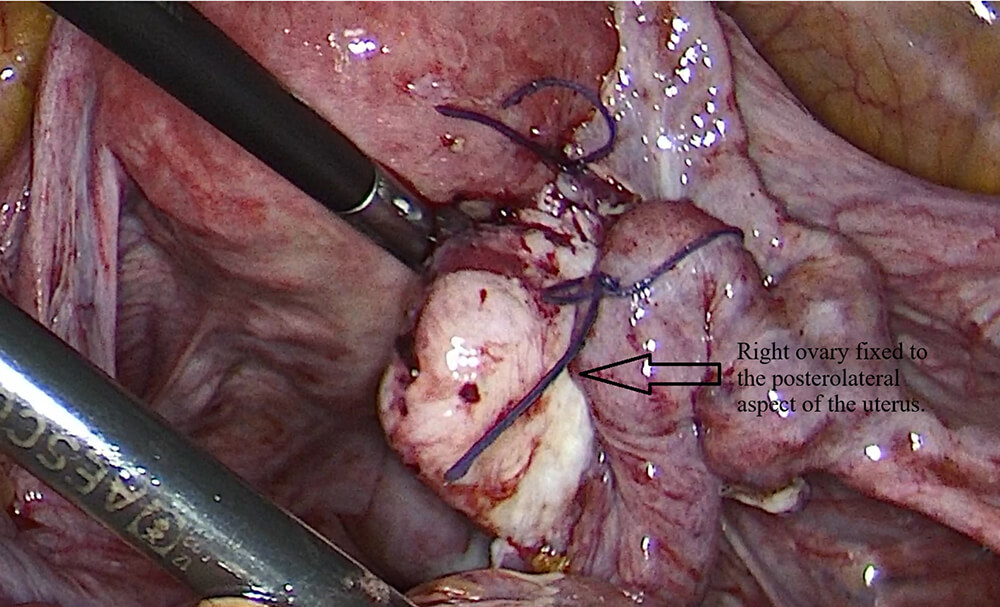 Fig. 4.
Fig. 4.
Right ovary fixed to the posterolateral aspect of the uterus after oophoropexy with the defect was closed.
The review of antecedent operative notes revealed that the preceding surgical procedures had included detorsion with cyst drainage, where present, and adnexal fixation without broad ligament defects. Beginning with the eighth procedure, the inspection of the broad ligament had become routine, the fenestration had been recognized and closed, and oophoropexy had been added.
As listed in Table 3, the first seven events involved detorsion with and without cyst drainage, right ovarian preservation, and the absence of adnexal fixation. In all seven previous surgical procedures, the absence and normal appearance of the broad ligament fenestration, with no defects, were documented. The changeover from laparoscopy to open laparotomy in the fifth, sixth, and seventh surgical procedures likely depends on the surgeons’ personal preference and their worries about the likely ischemia and/or necrosis in the setting of repeated severe bouts, although there was no direct contraindication in the operation notes. Thus, whether the absence of the eighth step broad ligament fenestration, revealed by laparoscopy, was indeed present in the past surgical procedures cannot be determined. The likely inconspicuousness, because of the smallness and depth in location, in conjunction with the acute need for detorsion, may occasionally have been occult in the vicinity of the adnexa and possibly increased over time through repeated bouts of torsion and pull.
Under general anesthesia and standard laparoscopy, the pelvis was inspected, and an approximately 3–4 cm fenestration in the right broad ligament and the courses of the utero-ovarian and infundibulopelvic ligaments were delineated. The right ovary was reduced from the fenestration without disturbing the infundibulopelvic pedicle, then detormented in two counter-rotations and re-oriented, where perfusion and turgor were normalized. In an attempt to prevent recurrence, the fenestration in the broad ligament was closed using interrupted USP 2-0 polyglactin 910 sutures, and posterior and lateral uterine oophoropexy using two interruptions with USP 2-0 polyglactin 910 sutures on the serosa was carried out. The opposite side’s broad ligament was inspected and intact without defects, hemostasis and irrigation affirmed, and no drains were placed.
Recurrent torsion in the adult adnexa is rare, and highly recurrent cases are even rarer. The largest number (on either side) reported in the literature is seven cases, and there are no reported cases of eight on the right side (Table 1), although there has been a reported right-sided predominance, presumed due to the sigmoid recess on the left protecting against torsion; our patient confirms this pattern, but far exceeds the numbers [11]. Literature related to surgical technique and fixation decision-making has been summarized in Table 2.
In this patient, the fenestration in the broad ligament created an entrance site for an internal hernia, leading to the entrance and twist of the adnexa on itself, resulting in a fixed fulcrum. The fixed fulcrum can be congenital, acquired from previous surgery, pregnancy-induced stretching, or endometriosis. The surgical observation that there was a double entrance through the window with double rotation on the axis, explaining the severity of pain and recurrence. Closure of the defect would eliminate the causative factor and the risk for recurrence, and detorsion would resolve the acute condition. The absence of closing the defects and fixing the uterus in the other seven operations could explain the recurrence, since the defects and the elongated UOL were left untreated.
The management was intended to deal with both factors responsible for recurrence, namely hypermobility and the defective herniation process. Closure of the broad ligament fenestration, together with fixation of the uterus to the ovary, was performed. The posterolateral uterine oophoropexy fixation was performed because it provides a direct and fixed length, reducing the scope for torsion and fixing the tubes in their correct positions. The fixation was performed using two interrupted USP 2-0 polyglactin 910 Vicryl sutures on the uterine serosa and corresponding mesovarian/ovarian inclusions, placed far away from the major vessels, ensuring adequate fixation and reducing myometrial invasion and the risk of hematomas. The management offered the advantage of preserving fertility and was in line with modern treatment. Preoperative color-flow Duplex studies suggested absent or markedly reduced flow in the ovarian vessels.
Although preoperative color Doppler suggested absent or markedly reduced flow, this did not translate into irreversible necrosis. As described in prior imaging studies of torsion, Doppler findings have limited sensitivity and specificity for viability, and salvageable ovaries may show no detectable flow. In our patient, macroscopic appearance and rapid color change after detorsion confirmed that the ovary remained viable.
The takeaway from the experience in the field is that in the setting of recurrent torsion in adult patients with normal and mobile pelvic structures, there appears to be an important role in the systematic assessment of the broad ligament, and the exclusion and repair of any fenestrations. The approach used here, including the defects and the oophoropexy, provides an excellent means of reducing the risk of recurrence in an environment in which there was an unusually high risk, and in conjunction with the brief review on the related defects, provides a direct means of translating the experience and knowledge that has been accumulated.
Published experience in the last decade indicates that recurrent torsion is more likely when the adnexa are otherwise normal and mobile, and when a correctable anatomical factor is present. In such a scenario, oophoropexy has been encouraged in the setting of more than one recurrence, although there exists a lack of comparative studies among the methods, and this has been discussed in Table 1 [3, 5, 6, 7]. There exists no left-sided recurrence in the setting of eight episodes in the adult in the present mini-review, and this is shown in Table 1.
In terms of preventive measures, four regular strategies emerge in modern literature. These are uterine fixation, UOL truncation/plication, round ligament fixation, and pelvic sidewall fixation [12]. In smaller series and tips since 2018, there appears to be some efficacy with uterine fixation and/or UOL truncation in reducing the issue of retorsion in the adult patient who has an idiopathic and hypermobile pelvis [9]. In the high recurrence scenario with the right side, the truncation and fixation procedure to the uterosacral area was successful in eliminating events in the long term [5, 8].
Uterine fixation was chosen in the current situation because of the following three reasons, all justified by the preceding literature. First, the short and direct fixation to the uterus secures the normal tubal axis and prevents the pull on the infundibulopelvic pedicle laterally, which would be particularly risky in the presence of the long UOL. Second, the anatomical trigger was the fenestration of the broad ligament. The closing of the hernia route and the fixation of the ovary on the posterior and lateral uterine serosa would solve the problem in one step and deal with both. Third, the available reports from 2018 through 2024 testify that there are satisfactory functional results in the adult cases with uterine fixation, in contrast to the failed cases treated with the use of side-wall and round-ligament sutures with the mentioned and undesirable long UOL [3, 5, 7].
Reproducibility advice includes the following. Use two interrupted resorbable sutures with superficial seromuscular sutures on the uterus and similar sutures on the mesovarium/ovarian cortex, securely away from the major vessels. Keep the short tether non-distorted. Always check the opposite side defects. Reperfusion must be recorded in the follow-up by Doppler when available [3, 8].
There are some limitations in the present study. Firstly, the present observation in relation to one adult patient means that there cannot be any recurrence risk probabilities and relative fixative efficacy analyses among the fixation methods. Secondly, the patient has only been followed up for 3 months, and although there has been no recurrence, long-term follow-ups in the present patient and other subjects would be important in assessing the long-term efficacy of the combined strategy. Thirdly, the mini-review, like all other mini-reviews, faces the problem of publication and reporting bias, in that there has been some lack of detail in the operative aspects in relation to the earlier surgery performed on the patient.
• In adults with recurrent torsion, actively inspect for broad ligament defects and close any fenestrations to eliminate the herniation pathway.
• Manage acutely with reduction and detorsion, then choose oophoropexy tailored to the anatomy; uterine fixation or modification of the UOL are reasonable options.
• A short, direct uterine tether helps limit rotational freedom while preserving tubal orientation and avoiding lateral pedicle tension; this is pragmatic and fertility sparing.
The patient reported rapid pain relief after surgery. The follow-up ultrasound was normal, and she felt reassured about fertility preservation.
This presentation describes an unusual etiopathogenesis in an adult patient who has had eight incidents of torsion on the right side, involving a double passage of the ovaries through a fenestration in the broad ligament with two complete rotational turns. A single-stage management approach, including reduction, detorsion, and both fixation and coverage of the defect, augmented by posterolateral uterine oophoropexy, led to the re-establishment of ovarian flow and the absence of recurrence during the first 3 postoperative months. Given our patient’s clinical course and the cumulative experience reported in the literature, we believe that in women who have had two or more ipsilateral ovarian torsion episodes, oophoropexy should be actively discussed and, whenever technically feasible, offered as a fertility-sparing option to lower the likelihood of further recurrence. In the setting of antecedent studies describing up to seven incidents of torsion on the same side, the current presentation offers hypothesis-generating, descriptive-level evidence that the management in a single surgical setting of the broad ligament fenestration and the hypermobile pelvis may represent a viable fertility-sparing approach when anatomical risk factors for recurrence are present. However, the absence of long-term follow-through in the present scenario, and the fact that the present manuscript represents the experience of a single patient, would appear to preclude the definitive assessment of the long-term effectiveness in this manner.
The datasets generated and analyzed during the current study are available from the corresponding author upon reasonable request.
ÖFÖ: literature review, data collection; CD: surgery/conception, drafting literature review; both authors approved the final version. Both authors contributed to editorial changes in the manuscript. Both authors participated sufficiently in the work and agreed to be accountable for all aspects of the work.
According to the Akdeniz University Medical Scientific Research Ethics Committee policy, single-patient case reports do not require formal institutional review board approval; therefore, separate ethical approval was not sought for this case. The report complies with institutional policy and the Declaration of Helsinki. The patient provided written informed consent to participate in this case report and for publication of anonymized clinical data and images.
Not applicable.
This research received no external funding.
The authors declare no conflict of interest.
During the preparation of this work, the authors used ChatGPT (OpenAI) to improve language and check spelling and grammar. After using this tool, the authors reviewed and edited the content as needed and take full responsibility for the content of the publication.
Supplementary material associated with this article can be found, in the online version, at https://doi.org/10.31083/CEOG47384.
References
Publisher’s Note: IMR Press stays neutral with regard to jurisdictional claims in published maps and institutional affiliations.




