1 Department of Ambulatory Surgery, Women’s Hospital, Zhejiang University School of Medicine, 310006 Hangzhou, Zhejiang, China
2 Zhejiang Provincial Clinical Research Center for Obstetrics and Gynecology, Women’s Hospital, Zhejiang University School of Medicine, 310006 Hangzhou, Zhejiang, China
Abstract
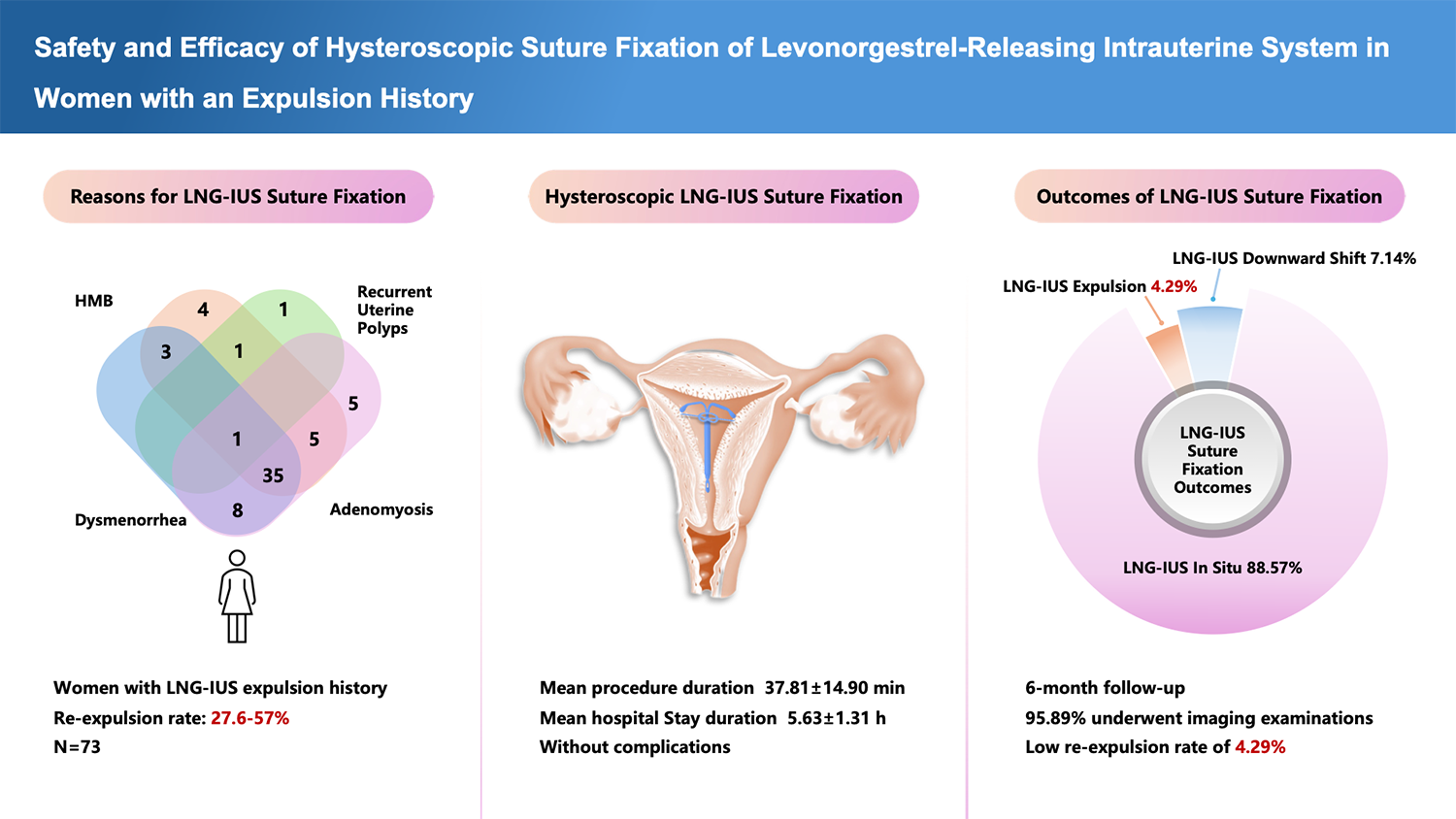
The levonorgestrel-releasing intrauterine system (LNG-IUS) is an effective contraceptive and non-surgical treatment for various gynecological conditions. However, its high expulsion rate remains a concern, particularly in women with a history of prior expulsion. This study aimed to evaluate the effectiveness of non-absorbable suture fixation under hysteroscopic guidance to reduce expulsion rates.
A total of 73 women with a history of LNG-IUS expulsion were enrolled between August 2022 and August 2023 at the Women's Hospital, Zhejiang University School of Medicine. All participants underwent hysteroscopic suture fixation of the LNG-IUS. Postoperative assessments were conducted on days 1, 3, and 7 using electronic questionnaires, along with outpatient follow-up and ultrasonography at 1, 3, and 6 months.
All 73 procedures were successfully performed as outpatient (day) surgeries, with a mean duration 37.81 ± 14.90 min, without encountering any complications. Follow-up was conducted for all 73 patients at 6 months, with 70 patients undergoing postoperative imaging, primarily using ultrasonography. Low rates of expulsion (4.29%) and downward-shift (7.14%) were observed. Decreased menstrual bleeding or amenorrhea was reported by 68 patients (93.15%). Among the 47 patients with preoperative dysmenorrhea, complete symptom relief was achieved in 39 cases (82.97%).
In patients with a history of LNG-IUS expulsion, hysteroscopic suture fixation of the LNG-IUS not only lowers the rate of re-expulsion but also alleviates associated symptoms.
Graphical Abstract
Keywords
- progesterone-releasing intrauterine devices
- hysteroscopic surgery
- intrauterine device expulsion
The levonorgestrel-releasing intrauterine system (LNG-IUS) is a long-acting, reversible contraceptive (LARC) that is inserted into the uterine cavity. It has been used in clinical practice for over 30 years and functions by locally and gradually releasing levonorgestrel (LNG) within the uterus, thereby exerting sustained progestogenic effects for 5 to 8 years. These effects include thickening of the cervical mucus and inhibition of endometrial maturation [1]. In addition to its high contraceptive efficacy, the LNG-IUS is also a first-line, non-surgical treatment for several benign gynecological conditions due to its prolonged progestogenic action on the endometrium. These conditions include adenomyosis [2], endometriosis [3], and endometrial hyperplasia (EH) [4]. It is also effective in treating menorrhagia, and prevents the recurrence of endometrial polyps (EPs) [5, 6].
However, the high rate of LNG-IUS expulsion is a concern. Women presenting with dysmenorrhea, menorrhagia, or adenomyosis experience a higher rate of LNG-IUS expulsion, ranging from 8.10% to 31.10%, compared to those using the LNG-IUS for contraception alone [7]. Patients with a history of LNG-IUS expulsion have a markedly higher risk of re-expulsion, ranging from 27.60% to 57.00% [8, 9]. Consequently, a substantial majority (58.60%–84.50%) of these women discontinue its use after expulsion [7, 8, 10].
Currently, there is no effective strategy to significantly reduce the recurrence of LNG-IUS expulsion in women with high-risk factors. Although pre-treatment with gonadotropin-releasing hormone analogs (GnRHa) can shrink the uterine volume, this does not substantially reduce the expulsion rate, which remains at 13.30%–14.00% [7, 11]. Some combination therapies have shown additional benefits for adenomyosis, including the relief of symptoms such as dysmenorrhea and menorrhagia, while also reducing the expulsion risk. For instance, LNG-IUS placement after GnRHa and high-intensity focused ultrasound (HIFU) reduced the 2-year expulsion rate to 6.38% [12], concurrent endometrial ablation reduced it to 1.90% [13], and laparoscopic adenomyomectomy combined with LNG-IUS showed an expulsion rate of 3.80% [14]. However, these approaches may not be suitable for women requiring LNG-IUS monotherapy.
Zhu et al. [15] first introduced hysteroscopic suturing of the LNG-IUS in a patient with adenomyosis in 2021, effectively preventing expulsion. Subsequent small-scale studies reported lower expulsion rates, ranging from 0.00% to 8.33% [15, 16, 17, 18, 19]. However, not all patients in these studies had a history of LNG-IUS expulsion.
The present study enrolled women with at least one prior LNG-IUS expulsion who wished to continue its treatment. The LNG-IUS was sutured to the uterine cavity under hysteroscopic guidance and using non-absorbable sutures to preserve therapeutic efficacy and reduce the risk of re-expulsion. The aim of this prospective observational study was to evaluate the feasibility, expulsion rate, and adverse effects of this fixation procedure.
This prospective, single-arm study enrolled patients who underwent hysteroscopic LNG-IUS suture fixation at the Women’s Hospital, Zhejiang University School of Medicine, from August 2022 to August 2023. The study protocol was approved by the ethics committee of the hospital (IRB-20220332-T), and all participants provided written informed consent. Surgical procedures were performed by experienced senior physicians in the ambulatory surgery department.
The inclusion criteria were: (a) a history of LNG-IUS expulsion; and (b) a desire to have the LNG-IUS inserted for the treatment of conditions such as menorrhagia, dysmenorrhea, adenomyosis, EH, and recurrent EPs.
The exclusion criteria were: (a) pregnant or uncertain pregnancy status; (b) acute infection of the female reproductive tract; (c) recent uterine injury or perforation; (d) cervical or uterine malignancies; (e) progesterone-dependent tumors; (f) acute liver disease or liver tumors; (g) allergy to LNG-IUS components; and (h) inability to undergo postoperative follow-up.
All participants underwent preoperative laboratory tests, including complete
blood count, coagulation profile, screening of sexually transmitted diseases
(STDs), liver and kidney function tests, and electrolyte analysis. They also
underwent cervical cancer screening, electrocardiography, breast ultrasound, and
transvaginal ultrasound to exclude contraindications for hysteroscopic surgery
and LNG-IUS placement. In addition, all participants underwent preoperative
assessment of female reproductive hormones to exclude perimenopausal women. The
uterine volume was calculated using the formula: 0.52
The procedure involved the use of a LNG-IUS (Mirena®, 52 mg; Bayer Inc., Turku, Finland); a 3-0, 17 mm non-absorbable polyester needle suture (ETHIBOND EXCEL® MX552; Ethicon Inc., Raritan, NJ, USA); a 6.25 mm, 0° operative hysteroscope with a 3 mm instrumental working channel (MyoSure®, REF 40-250; Hologic Inc., Marlborough, MA, USA); a 3 mm endoscopic needle holder (KANGJI®; Kangji Inc., Hangzhou, Zhejiang, China); a 3 mm knot pusher without suture opening (KANGJI®; Kangji Inc., Hangzhou, Zhejiang, China); and 3 mm endoscopic scissors (KANGJI®; Kangji Inc., Hangzhou, Zhejiang, China).
Based on existing reports, hysteroscopic suturing can be performed through the operative channel of the hysteroscope, or via a paracervical route adjacent to the hysteroscope [15, 16]. Drawing from the technique reported by Zhu et al. [15], we modified the procedure by introducing a hysteroscopic view-assisted knot-push technique, leading to improved surgical efficiency.
Hysteroscopy was initially conducted to identify intrauterine masses such as EPs or submucosal fibroids. Any necessary surgical interventions were subsequently performed. In cases with insufficient uterine septum and adenomyosis with distortion of the uterine cavities, a portion of the fundal myometrium was incised during hysteroscopy to ensure an adequately sized uterine cavity. Subsequently, hysteroscopic suture fixation of the LNG-IUS was performed after satisfactory observation of the uterine cavity. The LNG-IUS was securely positioned at the base of the uterine cavity by using a knot pusher under hysteroscopic guidance, with normal wing expansion and the absence of active bleeding. After successfully placing 6 knots under hysteroscopic guidance, the LNG-IUS string and suture were severed, and the surgical instruments withdrawn.
Oral antibiotics were administered within 48 h postoperatively, and all patients who underwent hysteroscopy were discharged on the same day.
Electronic questionnaires were sent to patients on postoperative days 1, 3, and 7, and an intelligent information platform was used to facilitate assessment of their postoperative condition. Outpatient follow-up and ultrasound assessments were also conducted at 1, 3, and 6 months after the procedure. These follow-up sessions were designed to evaluate parameters including menstrual flow, severity of dysmenorrhea, abnormal bleeding, non-menstrual lower abdominal pain, and other potential adverse effects. Additionally, the results of postoperative ultrasound or other imaging examinations were documented during follow-up assessments.
Upon completion of the 5-year therapeutic duration, the LNG-IUS requires hysteroscopic suture division for removal, or replacement with renewed fixation. If the patient requests premature removal of the suture-fixed LNG-IUS during follow-up, the same hysteroscopic suture transection procedure must be performed prior to extraction.
Statistical analysis was performed using SPSS 20 software (IBM Corporation,
Armonk, NY, USA). The results are presented as the mean
The required sample size was calculated using the formula for a single-arm study with a binary outcome based on a target value approach:
where n is the required sample size, p₀ is the target (null)
proportion, p is the anticipated response rate under the alternative
hypothesis, Z₁₋α/2 is the critical value for a two-sided
significance level (e.g., 1.96 for
A total of 74 women with at least one prior LNG-IUS expulsion (range: 1–5) were
enrolled in the study. One patient was excluded due to a confirmed diagnosis of
uterine carcinoma, resulting in a final cohort of 73 patients who underwent
successful LNG-IUS suture fixation. As shown in Table 1, the age of participants
ranged from 25 to 52 years, with an average of 41.34 years. The average body mass
index (BMI) for 65 patients was calculated to be 24.43 kg/m2, with 38.46% (25/65)
classified as overweight (BMI
| Variable | Value | |
| Age (years) [mean |
41.34 | |
| BMI (kg/m2) [mean |
24.43 | |
| Parity [n (%)] | ||
| Parous | 70/73 (95.89) | |
| Non-parous | 3/73 (4.11) | |
| Number of prior LNG-IUS expulsions [median] | 1.00 | |
| 1 [n (%)] | 55/73 (75.34) | |
| 2 [n (%)] | 15/73 (20.55) | |
| 3 [n (%)] | 2/73 (2.74) | |
| 4 [n (%)] | 0/73 (0.00) | |
| 5 [n (%)] | 1/73 (1.37) | |
| Ultrasonic uterine size (cm3) [mean |
168.28 | |
| Cases with ultrasonic uterine size |
35/67 (52.24) | |
| Depth of uterine cavity exploration (cm) [mean |
8.95 | |
| Depth of uterine cavity exploration |
47/70 (67.14) | |
| Anemia [n (%)] | 21/73 (28.77) | |
| HGB level with anemia (g/L) [mean |
97.90 | |
| HGB level without anemia (g/L) [mean |
126.30 | |
LNG-IUS, levonorgestrel-releasing intrauterine system; HGB, hemoglobin; BMI, body mass index.
The decision to perform suture fixation of the LNG-IUS in 73 patients was based primarily on specific clinical indications: 67.12% (49/73) had heavy menstrual bleeding, 64.38% (47/73) experienced dysmenorrhea, 73.97% (54/73) were diagnosed with adenomyosis, 9.59% (7/73) had concomitant EH, and 4.11% (3/73) had a history of recurrent EPs.
All surgeries were successfully completed, without complications such as fluid
overload, significant bleeding, or uterine perforation. The mean duration of the
entire procedure, including corresponding hysteroscopic steps, was 37.81
 Fig. 1.
Fig. 1.
Additional hysteroscopic procedures and surgical outcomes in LNG-IUS suture fixation. (A) Number of patients undergoing additional hysteroscopic procedures. (B) Operation time and hospital stay for LNG-IUS suture fixation, with or without additional hysteroscopic procedures. LNG-IUS, levonorgestrel-releasing intrauterine system.
The follow-up electronic questionnaire conducted on postoperative days 1, 3, and 7 revealed that none of the patients experienced lower abdominal pain, significant vaginal bleeding, fever, nausea, vomiting, or the need for readmission.
As of February 2024, all 73 patients (100.00%) had undergone a 6-month follow-up assessment, either through telephone consultation or an in-person visit to the clinic.
Of these, 70 (95.89%) underwent postoperative imaging examinations, primarily ultrasound. Three cases (4.29%) exhibited LNG-IUS expulsion or partial expulsion, and 5 cases (7.14%) exhibited a downward shift of the LNG-IUS, with an average distance of 1.46 cm on ultrasound. The LNG-IUS remained in situ in 62 patients (88.57%).
Hysteroscopic re-suturing with “two-point” fixation was performed in the three patients who experienced expulsion (Fig. 2A). During re-suturing, the LNG-IUS was expelled into the cervical canal, with intact thread loops and knots still in place (Fig. 2B). Transvaginal ultrasound examinations conducted at 4, 6, and 8 months post-operatively in these cases, respectively, indicated the LNG-IUS was still in situ.
 Fig. 2.
Fig. 2.
Hysteroscopic re-suture fixation and expulsed LNG-IUS. (A) ‘Two point’ fixation of LNG-IUS. Void arrow: First stitcher. Black arrow: Second stitcher. (B) Expulsed LNG-IUS with intact thread loop and knots. Black arrow: Intact thread loop and knots.
At the 6-month follow-up, 11/73 (15.07%) patients reported amenorrhea, and 57/73 (78.08%) reported a significant reduction in menstrual flow. Of the 47 patients who had preoperative dysmenorrhea symptoms, 82.97% (39/47) experienced complete relief, and 14.89% (7/47) had partial relief. Of the 7 patients diagnosed with EH, four underwent repeat hysteroscopic evaluation after surgery, with histopathology confirming complete reversal (CR). Additionally, none of the three patients with EPs experienced a recurrence during the follow-up period (Fig. 3A).
 Fig. 3.
Fig. 3.
Clinical outcomes of LNG-IUS suture fixation: efficacy and adverse effects. (A) Efficacy of LNG-IUS suture fixation. (B) Adverse effects of LNG-IUS suture fixation.
One patient (1.37%) was diagnosed with adenomyosis in a unicornuate uterus with a rudimentary horn (type IIC), and continued to experience unrelieved dysmenorrhea for 5 months postoperatively. Despite the LNG-IUS remaining in situ, the patient ultimately opted to undergo uterine resection. Two patients (2.74%) reported an increase in menstrual flow during their most recent follow-up, despite the LNG-IUS being in place. One of these patients required hospitalization and conservative treatment, while the other received additional treatment with dienogest.
The common adverse effects were similar to those observed with normal LNG-IUS placement. Irregular uterine bleeding (spotting) is defined as spotting or bleeding lasting more than 8 days per menstrual cycle, or more than 24 days within a 90-day period [20]. Irregular uterine bleeding in the form of spotting was reported by 52 of the 73 patients (71.23%). Additionally, 6 patients (8.22%) reported increased vaginal discharge, 5 patients (6.85%) experienced non-menstrual lower abdominal pain, and 2 patients (2.74%) complained of breast swelling. Weight gain was also observed in 2 patients (2.74%) (Fig. 3B).
This study included 73 women who had previously benefited from LNG-IUS treatment
but had experienced at least one episode of LNG-IUS expulsion. A documented
history of LNG-IUS expulsion may be a more appropriate indication for
hysteroscopic LNG-IUS suture fixation than other reported high-risk factors, such
as adenomyosis, uterine fibroids, dysmenorrhea, an enlarged uterine cavity
(uterine volume
All patients successfully underwent hysteroscopic LNG-IUS suture fixation, with
a mean operative time of 37.81
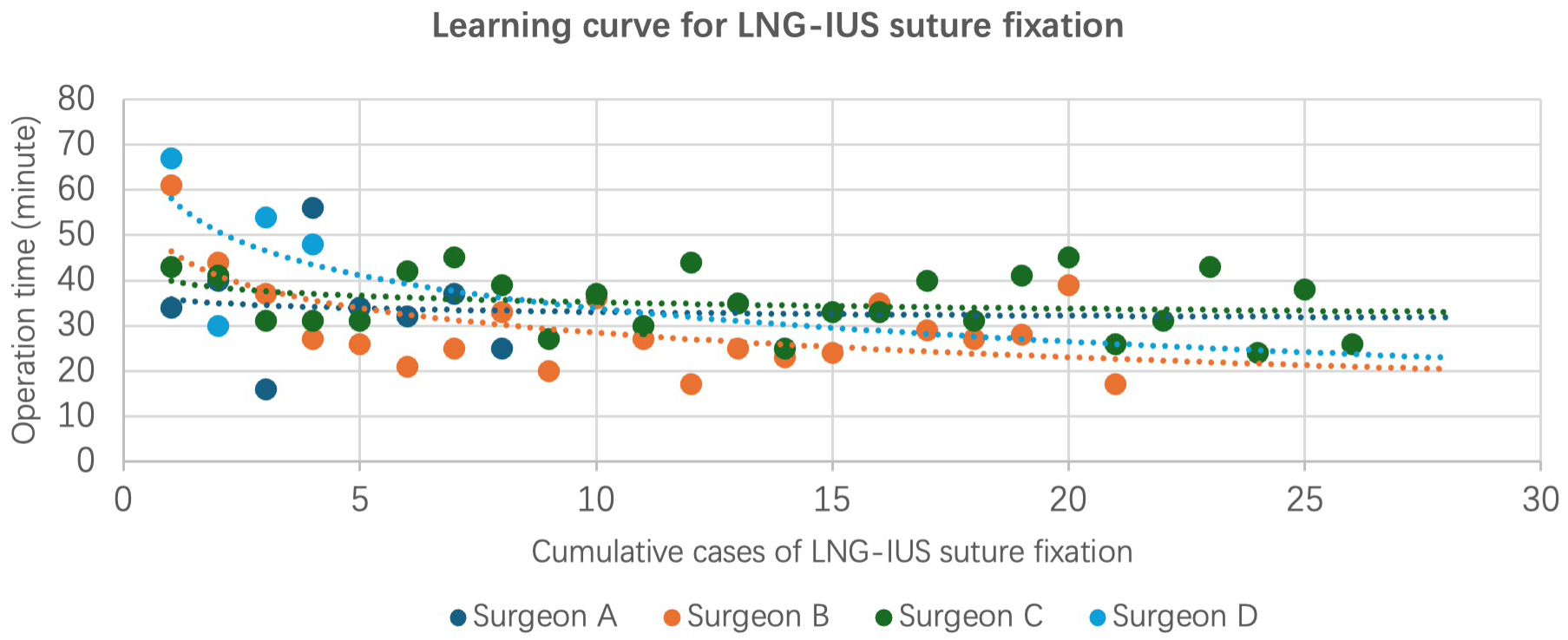 Fig. 4.
Fig. 4.
Learning curve for LNG-IUS suture fixation.
Patients with a history of LNG-IUS expulsion have a high rate of re-expulsion, ranging from approximately 27.60% to 57.00% [8, 9]. In our study, the expulsion rate was successfully reduced to 4.29% through hysteroscopic suture fixation. Similar studies have also reported low expulsion rates following hysteroscopic LNG-IUS suture fixation, ranging from 0.00% to 8.33% (Table 2) [15, 16, 17, 18, 19]. However, in the limited number of published clinical studies, not all patients who underwent the procedure had a prior history of LNG-IUS expulsion. In the study by Zhang et al. [17], only 25.00% (3/12) of patients had a history of expulsion, and a re-expulsion rate of 8.33% was observed 6 months postoperatively. In the study by Lv et al. [19], 49.40% (39/79) of patients had a history of expulsion, with a re-expulsion rate of 2.60%.
| Author | Publication year/month | Inclusion criteria | N | Follow-up (months) | Symptom improvement | Main adverse reactions | Expulsion/Downward shift |
| Zhu et al. [15] | 2021/5 | Adenomyosis | 1 | 12 | Obvious dysmenorrhea relief | NA | 0 |
| Obvious menorrhagia relief | |||||||
| Huang et al. [16] | 2023/8 | Previous LNG-IUS expulsion history | 2 | 3 | Decreased menstrual volume | NA | 0 |
| Zhang et al. [17] | 2022/11 | Adenomyosis | 12 | 6 | Decreased menstrual volume | prolonged vaginal spotting (33.00%) | 8.30%/16.67% |
| Significant dysmenorrhea relief | abnormal vaginal discharge (25.00%) | ||||||
| Cui et al. [18] | 2023/9 | Adenomyosis | 1 | 6 | Dysmenorrhea relief | NA | 0 |
| Decreased menstrual flow | |||||||
| Lv et al. [19] | 2024/1 | Adenomyosis | 79 | 12 | Improvement of pain and bleeding (97.40%) | irregular bleeding (44.30%) | 2.60%/NA |
| weight gain (29.20%) |
NA, not applicable.
In the present study, three patients experienced a recurrence of LNG-IUS expulsion at 4–5 months postoperatively, corresponding with the high-risk expulsion period reported in a previous study [19]. In our three patients with recurrence of expulsion, the initial suture fixation procedure was performed by three different surgeons. Moreover, the suture thread loops and knots were intact, suggesting the expulsion may have been caused by tearing of the muscular layer. Upon reviewing the operation videos for these cases, we identified that the first two knots were over-pushed, therefore creating excessively tight sutures. Zhang et al. [17] have suggested that expulsion could be related to the absorption of absorbable sutures. In a subsequent study, these authors improved fixation by using non-absorbable sutures, resulting in a significantly reduced expulsion rate of 2.60%. However, the specific reasons behind this reduction were not explored in detail [15, 19].
Five patients in the present study experienced a downward shift of the LNG-IUS, all of whom had a diagnosis of adenomyosis. One patient had a distorted uterine cavity, with the uterine fundus protruding into the cavity as a pseudo-septate uterus (Fig. 5A). In this case, the LNG-IUS was fixed at a low position, as the tail reached the internal cervical orifice (Fig. 5B). During follow-up of this patient, transvaginal ultrasound consistently demonstrated that the LNG-IUS remained positioned at least 1 cm from the uterine fundus (Fig. 5C,D). The other cases of downward shift may have been caused by loose formation of the thread loop (Fig. 5E). We also noted the occurrence of an “LNG-IUS swing” phenomenon in two cases with loose thread loops, which has not been reported previously. Both cases exhibited a downward shift in the LNG-IUS during the 1-month follow-up period, although it remained in situ at the 2- and 3-month follow-up times (Fig. 5F,G). The loose thread loop could potentially cause the LNG-IUS to swing within the uterine cavity. It is important to note that even when the LNG-IUS shifts downward, it still provides contraceptive and therapeutic benefits [7]. Therefore, we closely monitored the five patients with a downward shift, in light of the continued benefits they were likely to receive from the device.
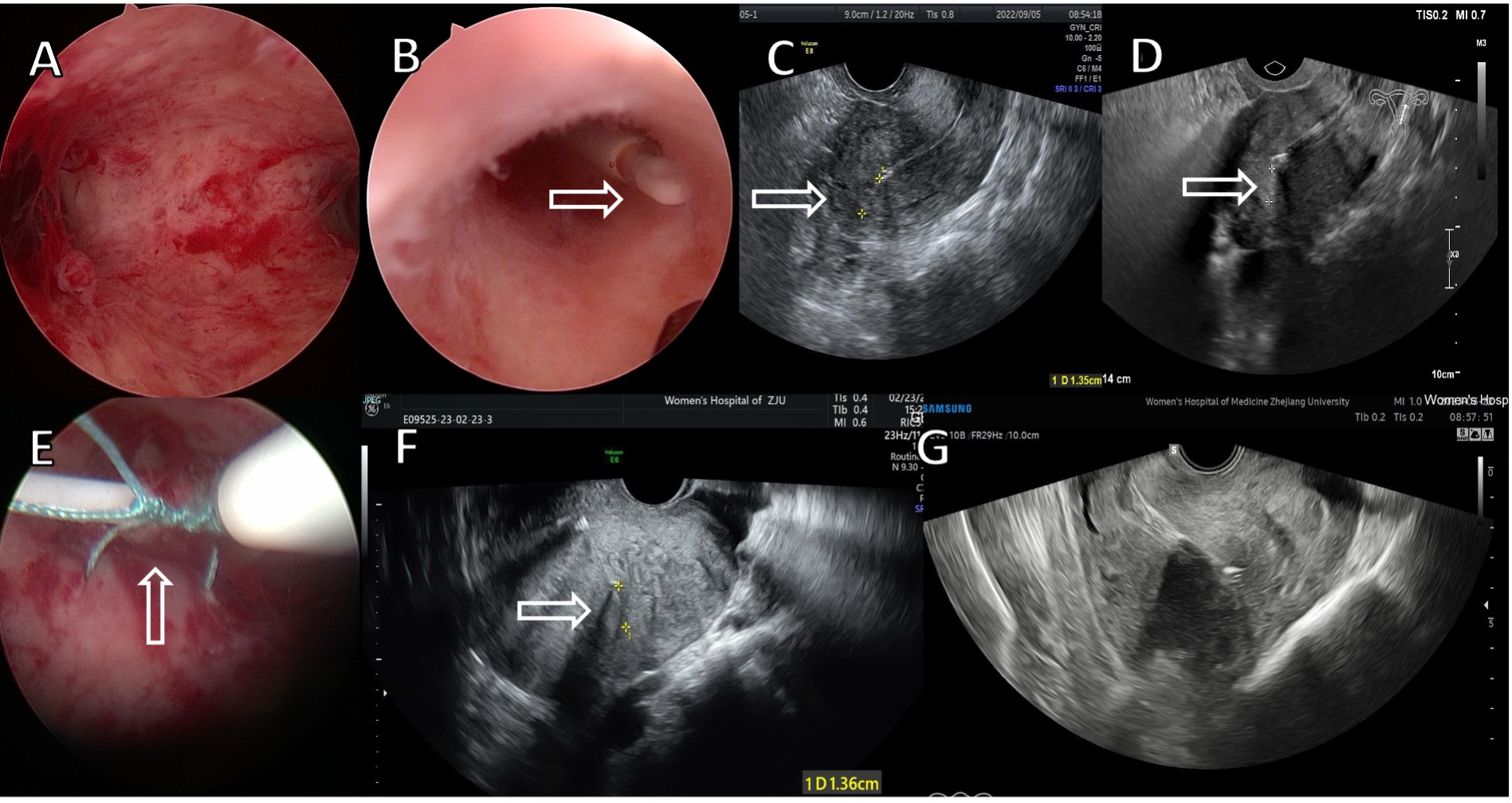 Fig. 5.
Fig. 5.
LNG-IUS downward shift and ‘swing’ phenomenon. (A) Distorted uterine cavity with adenomyosis. Protrusion of the uterine fundus, mimicking a ‘pseudo-septate uterus’ (5 August 2022). (B) Void arrow: Distal tip of the LNG-IUS reaching the internal cervical orifice (5 August 2022). (C) 1.35 cm downward shift of the LNG-IUS at 1-month follow-up (5 September 2022) (void arrows indicate position change). (D) 1.14 cm downward shift of the LNG-IUS at 8-month follow-up (7 April 2023) (void arrows indicate position change). (E) Void arrow: Single case exhibiting a loose thread loop (30 January 2023). (F) Void arrow: 1.36 cm downward shift observed at the 1-month follow-up (23 February 2023). (G) In situ position confirmed at the 2-month follow-up time in the same patient (22 March 2023).
Consistent with previous findings, our study demonstrated that LNG-IUS suture fixation can reduce the menstrual volume and alleviate dysmenorrhea symptoms (Table 2). A large majority of our patients (68/73, 93.15%) experienced either reduced menstrual bleeding or amenorrhea. Among the 47 patients with preoperative dysmenorrhea, 97.87% (46/47) achieved complete or partial symptom relief, comparable to the relief rate of 97.40% reported by Lv et al. [19] in 2024.
In addition to cases of adenomyosis, our study is the first to include patients with EH. Of the 7 patients with this condition, four required postoperative hysteroscopic evaluation. Follow-up multi-point endometrial biopsies revealed complete histopathological regression in two patients with complex hyperplasia, and in two with atypical hyperplasia. The LNG-IUS remained in place in all four cases. These findings suggest that LNG-IUS fixation may also be a viable treatment option for EH. Moreover, in three patients with recurrent EPs, no recurrence was observed after LNG-IUS fixation, indicating a potential preventive effect. However, due to the absence of a control group, the efficacy of LNG-IUS suture fixation for treating EH and recurrent polyps requires further confirmation through prospective, controlled clinical trials.
Nonetheless, suboptimal treatment outcomes were observed in three patients with adenomyosis. One case involved a unicornuate uterus with a rudimentary horn (type IIC). Despite successful LNG-IUS fixation and no postoperative expulsion, the patient experienced persistent dysmenorrhea and ultimately underwent hysterectomy 5 months later. The other two cases, with uterine volumes of 215.78 mL and 619.11 mL, experienced worsening menstrual bleeding despite proper LNG-IUS placement, requiring additional interventions. Similarly, Lv et al. [19] reported two cases in which patients opted for hysterectomy due to unsatisfactory symptom control following LNG-IUS fixation for adenomyosis. The fixed 52 mg dose of the LNG-IUS could limit its effectiveness in patients with a high adenomyosis burden. Therefore, careful patient selection and thorough preoperative evaluation are essential when considering LNG-IUS fixation for such cases.
In our study, irregular uterine bleeding was defined as spotting lasting more than 8 days within one month, or more than 24 days within 90 days. During the 6-month follow-up period, we observed a relatively high incidence (71.23%) of irregular uterine bleeding. A previous study on LNG-IUS suture fixation reported an irregular uterine bleeding rate of 44.30% at 12 months post-procedure [19]. This exceeds the 24.00% incidence of irregular bleeding observed at 12 months following standard LNG-IUS placement in patients with adenomyosis [10]. However, neither the earlier clinical studies on LNG-IUS suture fixation, nor those on standard placement, have clearly defined what constitutes LNG-IUS—related irregular bleeding. Therefore, the relatively high rate of irregular spotting observed in our study may partly reflect differences in the definition of irregular uterine bleeding. As one of the most common adverse effects associated with standard LNG-IUS placement, irregular uterine bleeding typically decreases over time and is negatively correlated with duration of use [24, 25]. The follow-up period in the present study was relatively short compared with the study by Lv et al. [19], which may partly explain the higher incidence of irregular uterine bleeding. Although suture fixation of the LNG-IUS may increase the risk of irregular bleeding, confirmation of such an association requires a control group undergoing standard LNG-IUS placement, a longer follow-up period, systematic data collection at predefined intervals, and quantitative evaluation using bleeding diaries. Despite the relatively high incidence of vaginal spotting in our study, no cases of pelvic inflammatory disease were identified during the 6-month follow-up. All patients tolerated the device well, and none required early removal of the levonorgestrel-releasing intrauterine system due to bleeding.
This study represents the largest clinical investigation to date on hysteroscopic suture fixation of the LNG-IUS in patients with a documented history of expulsion. At 6-month follow-up, the rates of expulsion (4.29%) and downward displacement (7.14%) were both relatively low. LNG-IUS suture fixation also improved dysmenorrhea (97.87%, 46/47) and reduced menstrual volume or the onset of amenorrhea (93.15%, 68/73) in the large majority of patients, while proving effective in the treatment of EH and recurrent EPs.
However, several limitations should be acknowledged. First, the absence of a control group prevents direct comparison with alternative treatment approaches, thereby weakening the strength of our conclusions. Unlike previous clinical studies on LNG-IUS suture fixation, all participants in our study had experienced at least one prior LNG-IUS expulsion. These patients opted either for suture fixation in the hope of continued therapeutic benefit, or abandoned LNG-IUS treatment for alternative therapies. Additionally, LNG-IUS is not covered by medical insurance in China, and hence the recruitment of a control group willing to undergo standard re-insertion posed significant challenges. Second, the study population was heterogeneous, with 73.97% (54/73) of patients diagnosed with adenomyosis. As a result, quantitative assessments such as the Pictorial Blood Loss Assessment Chart (PBAC) and Visual Analog Scale (VAS) for dysmenorrhea were not included. This weakened the reliability of our evaluation of symptom improvement. Third, due to the novelty of the surgical technique at the time this study was initiated, the increased incidence of irregular bleeding was not anticipated. Moreover, previous studies lacked clear definitions or evaluation criteria for irregular bleeding [17, 19]. Objective tools such as bleeding diaries were not employed to assess spotting frequency or volume, thus limiting the robustness of the safety analysis related to irregular bleeding.
Future studies should adopt more refined subgroup designs based on underlying conditions, and incorporate standardized quantitative measures to better assess the efficacy and safety of this technique.
Among patients with a history of LNG-IUS expulsion, hysteroscopic suture fixation demonstrates dual benefits: it reduces the re-expulsion rate to 4.90% while simultaneously alleviating symptoms of dysmenorrhea and menorrhagia.
The datasets used and analyzed during the current study are available from the corresponding author on reasonable request.
YG and YW designed the research study. BL and YG conducted follow-up visits and collected the data. YG and GX analyzed the data and drafted the manuscript. GX and YW critically revised the manuscript. All authors contributed to editorial changes in the manuscript. All authors read and approved the final manuscript. All authors have participated sufficiently in the work and agreed to be accountable for all aspects of the work.
This study was conducted in accordance with the guidelines of the Declaration of Helsinki. The study was approved by the Women’s Hospital of Zhejiang University School of Medicine ethics committee (IRB-20220332-T), and all participants provided written informed consent.
The uterine image featured in the graphical abstract was sourced from http://www.album-online.com (alb11341740) and has been properly licensed.
This research received no external funding.
The authors declare no conflict of interest.
References
Publisher’s Note: IMR Press stays neutral with regard to jurisdictional claims in published maps and institutional affiliations.





