1 Department of Obstetrics and Gynecology, Peking University People’s Hospital, 100044 Beijing, China
†These authors contributed equally.
Abstract
To evaluate the effects of holistic postural rehabilitation exercise in combination with electrical stimulation and biofeedback on urinary incontinence (UI) symptoms and pelvic floor muscle strength in patients suffering postpartum pelvic floor dysfunction.
A single-anonymized, randomized controlled trial was conducted from January 2021 to December 2022. A total of 120 patients, 42 days postpartum and diagnosed with pelvic floor dysfunction at three medical institutions in a certain city (Beijing, China), were enrolled and randomly assigned into the experimental group (n = 41) or control group (n = 46) using a random number table; thus, 87 medical records were included in the analysis. The experimental group received holistic postural rehabilitation exercises and electrical stimulation biofeedback therapy, while the control group received conventional Kegel exercises and electrical stimulation biofeedback therapy. Pelvic floor muscle strength and pelvic floor function were assessed at 42 days postpartum (baseline), 1 month, and 3 months post-intervention using the Pelvic Floor Distress Inventory-20 (PFDI-20) questionnaire, to evaluate bladder symptoms, bowel symptoms, and UI. The scores of the two groups were compared.
The experimental group exhibited significantly improved Class I pelvic floor muscle strength compared to the control group at a statistical level (p = 0.00). For UI symptoms, the frequency of urine leakage differed significantly at 3 months post-intervention (p = 0.03). The results of the comparison between the analysis groups: At all three time points (baseline, 1 month, and 3 months), comparisons of each index yielded p > 0.05. The analysis concludes that total PFDI-20 scores or any subscale scores did not differ significantly instatistical level between the groups at any time point. According to the analysis results of pelvic floor physiological indicators After the 3-month intervention, both groups exhibited improvements in postpartum pelvic floor muscle recovery. However, when comparing Type I muscle strength, the experimental group out performed the control group statistically (p < 0.05). At baseline, the severity of UI symptoms did not present an obvious difference in statistical level between the two groups, indicating good baseline consistency. After 3 months of intervention, the frequency of urinary leakage differed a lot. The intergroup comparison showed that t = 4.83 and p = 0.03 (< 0.05), suggesting that the experimental group achieved remarkably larger improvement in reducing urinary leakage frequency versus the control group.
Holistic postural rehabilitation exercise combined with electrical stimulation biofeedback can reduce the frequency and volume of postpartum UI, improve Class I fibromuscular muscle strength, and enhance pelvic floor stability and function. However, the effects on pelvic organ prolapse (POP), colorectal and anal dysfunction, and lower urinary tract symptoms were not significant and warrant further clinical investigation.
The study has been registered on https://clinicaltrials.gov/ (registration number: ChiCTR2000029618, registration link: https://www.chictr.org.cn/showprojEN.html?proj=48903).
Keywords
- holistic postural rehabilitation exercise
- electrical stimulation biofeedback
- pelvic floor muscle strength
- urinary incontinence
In recent years, postpartum pelvic floor dysfunction has increasingly received attention. It is a common condition with high morbidity among postpartum women, and is manifested as urinary incontinence (UI), pelvic organ prolapse (POP), and sexual dysfunction (SD). UI is further classified into stress urinary incontinence (SUI), urge urinary incontinence (UUI), and mixed urinary incontinence (MUI) [1]. An epidemiological study indicates that pregnancy and childbirth are two independent factors predicting the risk of pelvic floor dysfunction [2]. In the early postpartum period, approximately half of the primiparous women experience varying degrees of pelvic floor muscle weakness [3]. Without timely intervention postpartum, pelvic floor dysfunction may worsen with age and declining hormone levels. Current clinical treatments primarily include physical therapy and surgical interventions [4]. Both approaches are effective to varying degrees but have inherent limitations. For example, electrical stimulation biofeedback and pessary use require professional guidance and resources, involving additional cost and labor. Surgical interventions, in addition to high cost, may disrupt normal anatomical structures and carry risks of postoperative complications of urinary retention and mesh exposure. Pelvic floor rehabilitation can be a preferred treatment method specific to young patients with mild symptoms. It is cost-effective, non-invasive, and free of side effects. With correct guidance, exercise or use of devices and electrostimulation, long-term adherence may help prevent disease progression [5]. Therefore, to further optimize pelvic floor rehabilitation strategies, this study developed a comprehensive rehabilitation program combining exercise with electrical stimulation biofeedback based on an evidence-based approach. The study was conducted on 87 postpartum women with pelvic floor dysfunction, and the following results were obtained.
General Information: Patients with postpartum pelvic floor dysfunction visiting three hospitals in Beijing from January 2021 to December 2022 were recruited. Two hospitals were district-level maternal and child health care centers, and one was a tertiary general hospital. Each hospital recruited 40 patients, evenly falling into the control and experimental groups (n = 20). In total, 60 patients were assigned to the experimental group and 60 to the control group. A single-blind intervention was applied to both groups. A total of 87 medical records were included in the final analysis. Inclusion criteria: (1) provision of informed consent; (2) diagnosis of Pelvic Floor Distress (PFD) according to the textbook Obstetrics and Gynecology, with pelvic floor muscle strength graded 0 to 3; (3) age between 22 and 35 years; and (4) full-term singleton vaginal delivery. Exclusion criteria: (1) history of pelvic floor surgery; (2) reproductive system infections; (3) presence of cardiac pacemakers; (4) neurological diseases; (5) endocrine or hematological disorders; and (6) cognitive, communication, auditory, visual, or motor impairments. All participants were informed of the study procedures and their required cooperation prior to participation. The study protocol obtained the approval of the hospital ethics committee and participants had provided their written informed consent.
The Questionnaire comprised two sections: demographic characteristics (age, gender, marital status) and information related to pregnancy, childbirth, and neonatal conditions.
Assessment of pelvic floor muscle strength was conducted by a single experienced rehabilitation therapist using a bioelectric feedback stimulator (Leborui, UROSTYM, URS 12081936, Laborie Medical Technologies Canada ULC, Portsmouth, New Hampshire, Canada). The system provided real-time feedback of electromyographic or pressure signals to participants through a computer screen, displayed as intuitive graphics (e.g., bar charts, line graphs, animation games) or auditory signals. Resting state assessment: Participants were instructed to remain fully relaxed without contracting any muscles, including the abdomen and gluteal muscles. Baseline electromyographic activity or pressure was recorded to assess resting muscle tone. Maximum voluntary contraction assessment: Instruction: Participants were instructed to contract the pelvic floor muscles maximally, as if preventing urine leakage or lifting the anus, without simultaneous contraction of the abdomen, gluteal or thigh muscles, and without holding their breath. Operation: Each contraction was maintained for 3 to 5 seconds, repeated 3 times with sufficient rest between trials. The system recorded the maximum contraction amplitude (muscle strength) and contraction pattern. Rapid contraction assessment: Participants were required to contract and relax the pelvic floor muscles as quickly and forcefully as possible, repeating several times. This evaluation assessed rapid contraction ability and muscle coordination. Higher system values indicated greater muscle strength.
The Pelvic Floor Distress Inventory-20 (PFDI-20) served for assessing pelvic
floor dysfunction-related symptoms. The PFDI-20 comprises 20 items grouped into
three subscales: urinary symptoms (Urinary Distress Inventory-6, UDI-6), bowel
symptoms (Colorectal-Anal Distress Inventory-8, CRADI-8), and POP symptoms
(Pelvic Organ Prolapse Distress Inventory-6, POPDI-6) [6], scored on a 0–4
scale, where higher scores indicate larger symptom severity. The PFDI-20
exhibited a good internal consistency, with Cronbach’s
Postpartum SUI assessment was conducted using the International Consultation on Incontinence Questionnaire-Short Form (ICI-Q-SF) according to established guidelines. The ICI-Q-SF is strongly recommended (Grade A) by the International Continence Society (ICS) for evaluating SUI [7]. The ICI-Q-SF questionnaire comprises 3 items addressing the UI frequency, the volume of urine leakage, and its influence on daily life.
The intervention team consisted of a research nurse, a pelvic floor specialist nurse, a rehabilitation therapist, an obstetrician/gynecologist, and a chief nurse. The lead instructor oversaw project quality control. The researcher was responsible for constructing, implementing, and analyzing the intervention program. The rehabilitation therapist, obstetrician/gynecologist, and chief nurse developed the comprehensive posture rehabilitation exercise program and ensured training safety. The research nurse and pelvic floor specialist nurse managed patient recruitment, data collection, and program execution.
Development of the Postpartum Comprehensive Posture Exercise Program: An
extensive literature review was conducted across Embase, PubMed, Cochrane, OVID,
Web of Science, China National Knowledge Infrastructure (CNKI), Wanfang Data, VIP
Full-text Electronic Journals, and other Chinese biomedical literature databases
to collect relevant publications on postpartum pelvic floor rehabilitation
exercises. Following initial discussions among the research team, a preliminary
framework for the postpartum pelvic floor rehabilitation program was established.
After three rounds of discussions, a draft exercise program, suitable for
initiation at 42 days postpartum, was developed. Subsequently, the Delphi expert
consultation method was employed, involving two rounds of consultations with 18
experts in postpartum pelvic floor disease management, nursing, and education,
with a 2–3 week interval between rounds. After the first round, items were
screened, modified, and supplemented based on expert feedback and statistical
analysis to generate the second-round questionnaire, which was subsequently sent
to the same experts. Item selection criteria included a mean score
| Models | Specific movement steps | ||
| Posture preparation | Exercise method | Exercise time | |
| 1. Abdominal Breathing | Lie on your back on a yoga mat or WAFF mat. (Instrument name: Sports air cushion; the manufacturer: WAFF SAS; batch number: LO23; location: France) | • Firstly, breathe naturally. Then, inhale through your nose slowly, as if you were smelling a flower; exhale through your mouth slowly. Feel the gas filling your belly as you inhale and gradually tighten your transverse abdominal muscles as you exhale. Repeat the same nasal inhale and mouth exhale. | Spend 2~5 minutes, keeping your breathing rhythm as slow as possible. |
| 2. Pelvic Exercise | Sit on a yoga mat or WAFF mat with knees bent, sitting bones on either side of the spine, feet shoulder-width apart, hands hooked on the back of the thighs. | • Use abdominal breathing to activate the core muscles and keep the “smaller jeans zipper” closed. | Perform 2~4 sets of 6~8 repetitions, and finish the exercise in about 3~5 minutes. |
| • Inhale slowly to extend the spine. Exhale and tilt the pelvis back, curving the spine into a capital “C”, then inhale and tilt the pelvis forward, arching the spine upwards. Repeat. | |||
| 3. Bridge Exercise | Lie on your back with knees bent, feet on yoga mat or WAFF mat, pelvis in neutral position, shoulders away from ears, chin slightly tucked. | • Use abdominal breathing to activate the core muscles. | Perform 2~4 sets of 6~8 repetitions, and finish the exercise in about 8 minutes. |
| • Posterior pelvic tilt on exhalation | |||
| 4. Kneeling Balance | Kneel on your yoga mat or WAFF mat, keeping your body upright. | • Use abdominal breathing to activate the core muscles. | Perform 4~6 sets of 30 seconds repetitions, and finish the exercise in about 2~3 minutes. |
| • Lift your feet off the floor slowly, keeping your body stable, gradually transitioning to holding for 30 seconds, with your core muscles tightened at all times. | |||
| 5. Quadrupedal Stretching | Kneel, keeping both knees under the hip joints, adjust the pelvis to a neutral position where the occiput, the highest point of the thoracic spine and the sacrum should be in a straight line. | • Use abdominal breathing to activate the core muscles. | Perform 3~4 sets of 6~8 repetitions on each side of the limb, and finish the exercise in about 8 minutes. |
| • Inhale to extend the spine and keep the spinal pelvis stable | |||
| 6. Supine Hand-And-Knee Confrontation | Lie on your back on a yoga mat or WAFF mat with your hands pointing vertically to the ceiling, keeping your knees above your hips in a tabletop position, adjusting your pelvis to a neutral position with your shoulders away from your ears and your chin slightly tucked in. | • Use abdominal breathing to activate the core muscles. | Perform 4~6 sets of 30 seconds repetitions, and finish the exercise in about 2~3 minutes. |
| • Place your hands on your knees, inhale in preparation, exhale as your hands and your knees resisting each other and holding the counter force for 20~30 seconds, keeping your breath even and your core muscles tightened at all times. | |||
WAFF, Whole-body Advanced Functional Foam.
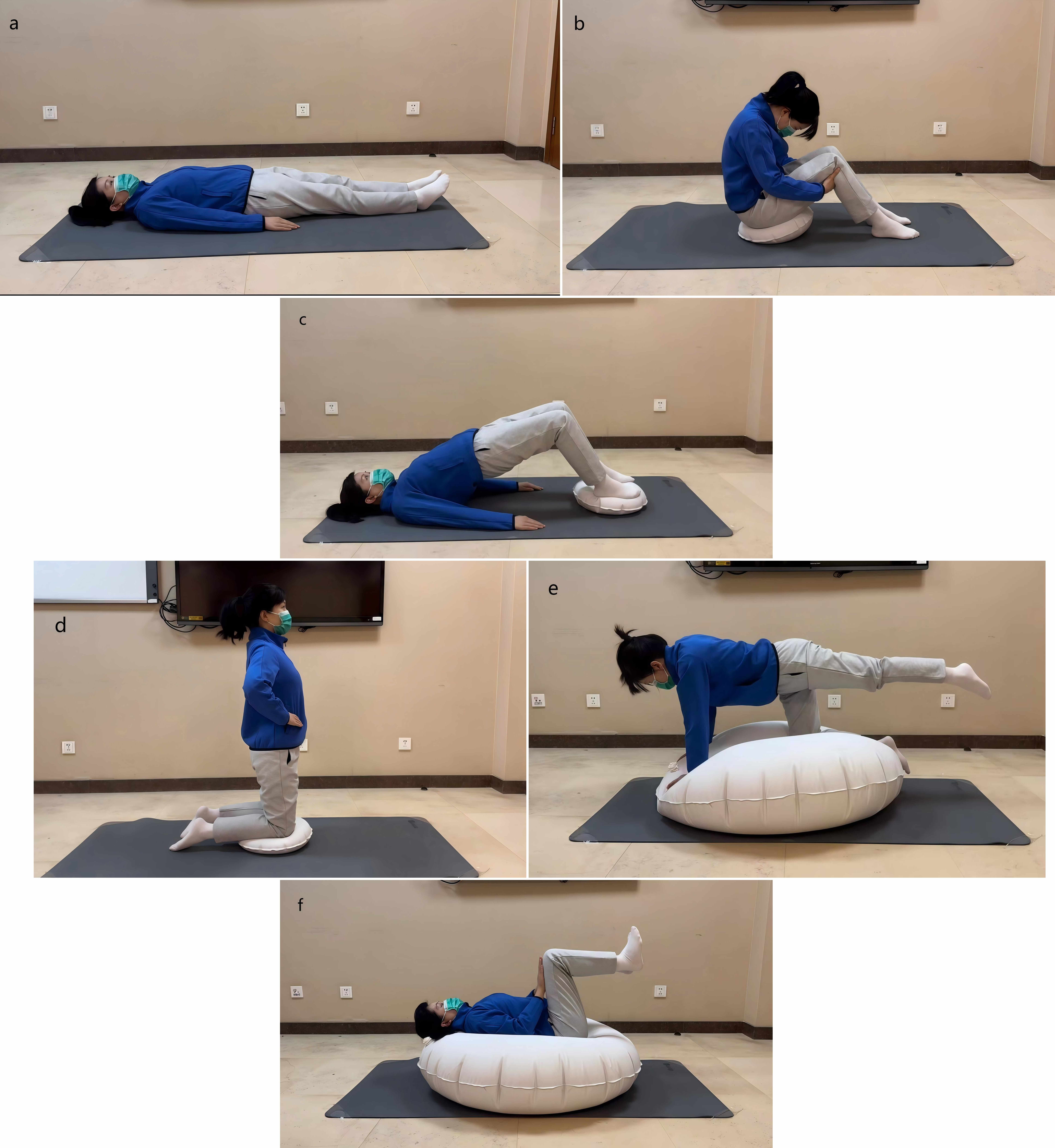
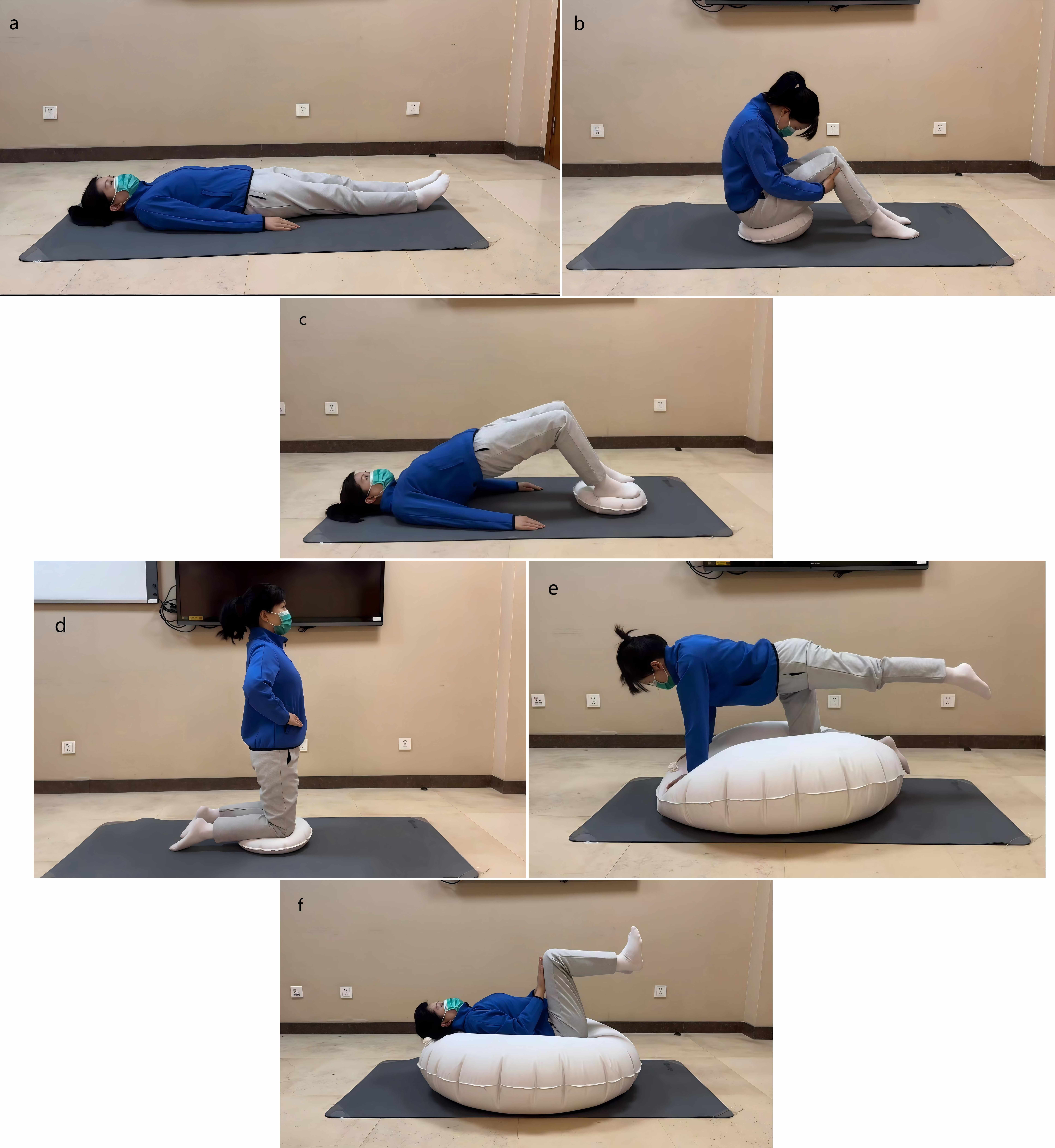 Fig. 1.
Fig. 1.
Visualization of postpartum holistic postural exercise program. (a) Abdominal Breathing. (b) Pelvic Exercise. (c) Bridge Exercise. (d) Kneeling Balance. (e) Quadrupedal Stretching. (f) Supine Hand-and-Knee Confrontation.
In the experimental group, participants received individualized one-on-one guidance from trained pelvic floor specialist nurses. Relevant instructional video materials were provided, and WeChat-based check-ins were conducted. The patients were guided to practice at home for 20–30 minutes once daily, with exercise logs maintained. Research nurses conducted face-to-face follow-ups twice weekly for four weeks, providing supervision and guidance during exercises. Electrical stimulation combined with biofeedback was administered for 30 minutes per session, twice weekly, with 10 sessions constituting one treatment course. The intervention period commenced 6 weeks postpartum and continued for 3 months.
Participants received regular health education, including lifestyle modifications such as avoiding prolonged squatting, refraining from lifting heavy objects, and performing regular pelvic floor muscle training (PFMT). A clinical physician developed an individualized treatment plan based on each patient’s condition, including Kegel training, electrical stimulation and biofeedback therapy. Each session lasted 30 minutes, administered twice weekly, with 10 sessions constituting one treatment course. The intervention period commenced 6 weeks postpartum and continued for 3 months.
Data were entered via Microsoft Excel, and statistical analyses relied on SPSS
version 17.0 (IBM Corp., Chicago, IL, USA).
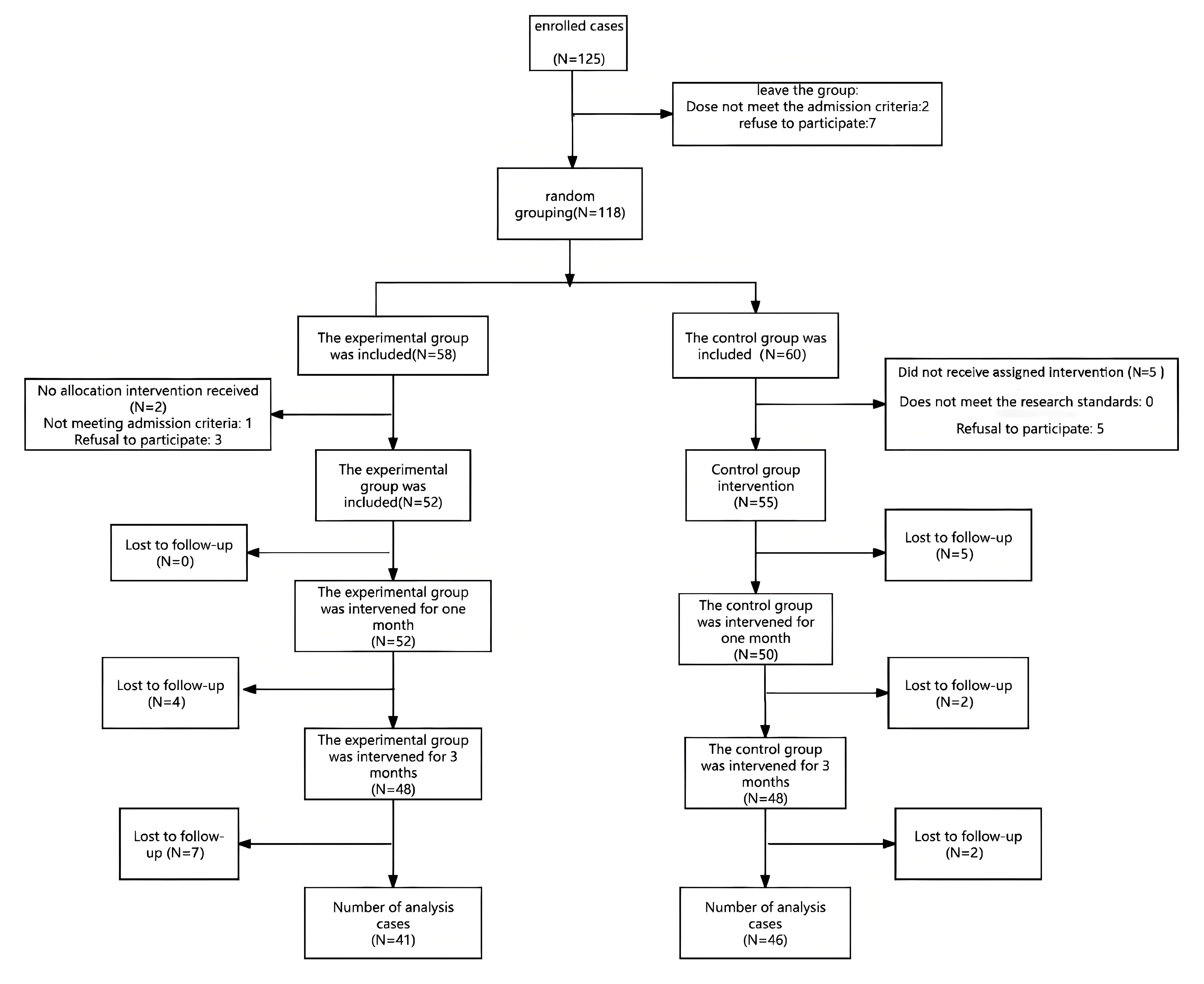
A total of 125 individuals were screened for eligibility covering the period of January 2021–December 2022. Ultimately, a total of 87 participants satisfying the inclusion criteria were enrolled in the study, with 41 and 46 assigned to the experimental group and the control group, respectively. All participants completed three follow-up assessments (The detailed study flow is presented in Fig. 2).
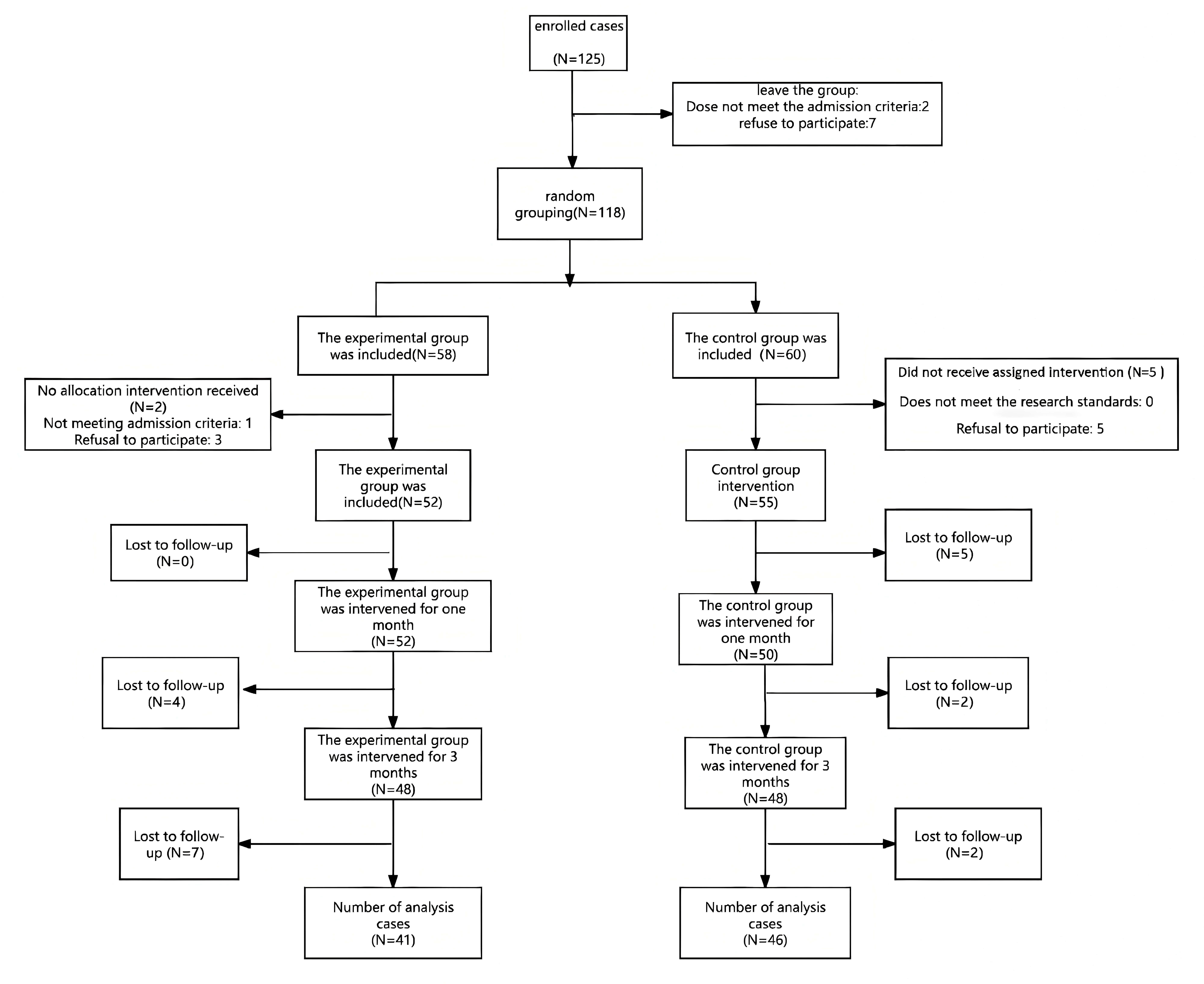 Fig. 2.
Fig. 2.
Flowchart.
The two groups were comparable, as evidenced by no significant difference in
their baseline characteristics (p
| Control group (N = 46) | Experimental group (N = 41) | t/ |
p | ||
| Age (years, |
31.00 |
32.80 |
1.39 | 0.22 | |
| Height (cm, |
165.20 |
160.70 |
–1.11 | 0.27 | |
| Weight (kg, |
62.40 |
61.90 |
–0.25 | 0.80 | |
| Waist circumference (cm, |
79.40 |
82.70 |
1.26 | 0.21 | |
| Educational background | |||||
| Master’s degree or above | 24 (52.17) | 23 (56.10) | 1.15 | 0.77 | |
| Undergraduate or junior college | 22 (47.83) | 16 (39.02) | |||
| High school or technical secondary school | 0 | 1 (2.44) | |||
| Junior high school below | 0 | 1 (2.44) | |||
| Newborn body weight (kg) | |||||
| 26 (81.25) | 44 (77.19) | 0.20 | 0.65 | ||
| 6 (18.75) | 13 (22.81) | ||||
| Complications of pregnancy | |||||
| Glycuresis | 3 (9.38) | 6 (10.53) | 0.93 | 0.82 | |
| Hypertension | 1 (3.13) | 3 (5.26) | |||
| Else | 4 (12.50) | 4 (7.02) | |||
| Absence | 24 (75.00) | 44 (77.19) | |||
| Total score of PFDI-20 | 24.77 |
19.44 |
–0.89 | 0.37 | |
| Bladder symptoms | 0.20 |
0.20 |
–0.02 | 0.99 | |
| Intestinal symptoms | 0.43 |
0.32 |
–1.15 | 0.26 | |
| Desperation symptoms | 0.35 |
0.25 |
–0.97 | 0.34 | |
| Class I fibromuscular muscle | 10.59 |
10.42 |
–0.06 | 0.96 | |
| Adventitia muscle strength | 22.56 |
18.07 |
–1.31 | 0.20 | |
| Fatigue % | 2.03 |
2.30 |
0.15 | 0.89 | |
PFDI-20, Pelvic Floor Distress Inventory-20; N, number of samples.
The results of the comparison between the analysis groups (Tables 3,4,5 and Fig. 3): At all three time points (baseline, 1 month, and 3 months), comparisons of
each index yielded p-values
| Experimental group (N = 41) | Control group (N = 46) | t | p | ||
| Evaluation of the pelvic floor dysfunction | |||||
| Enter the group | |||||
| Total score of PFDI-20 | 21.23 |
24.39 |
–0.89 | 0.37 | |
| UDI-6 | 0.21 |
0.21 |
–0.02 | 0.99 | |
| CRADI-8 | 0.32 |
0.40 |
–1.15 | 0.26 | |
| POPDI-6 | 0.31 |
0.36 |
–0.97 | 0.34 | |
| Enrollment for 1 month | |||||
| Total score of PFDI-20 | 11.26 |
15.62 |
–0.81 | 0.42 | |
| UDI-6 | 0.09 |
0.17 |
–1.11 | 0.27 | |
| CRADI-8 | 0.22 |
0.26 |
–0.47 | 0.64 | |
| POPDI-6 | 0.14 |
0.19 |
–0.59 | 0.56 | |
| Enrollment for 3 months | |||||
| Total score of PFDI-20 | 11.34 |
24.38 |
–0.89 | 0.38 | |
| UDI-6 | 0.15 |
0.37 |
–0.99 | 0.33 | |
| CRADI-8 | 0.15 |
0.17 |
–0.12 | 0.91 | |
| POPDI-6 | 0.15 |
0.43 |
–1.39 | 0.17 | |
UDI-6, Urinary Distress Inventory-6; CRADI-8, Colorectal-Anal Distress Inventory-8; POPDI-6, Pelvic Organ Prolapse Distress Inventory-6.
| Name | Name | Average value | Average value | Difference | Standard error | p | |
| POPDI-6 | 0 months | 1 month | 0.21 | 0.17 | 0.05 | 0.07 | 0.52 |
| 0 months | 3 months | 0.21 | 0.37 | –0.16 | 0.12 | 0.18 | |
| 1 month | 3 months | 0.17 | 0.37 | –0.20 | 0.12 | 0.11 | |
| CRADI-8 | 0 months | 0 months | 0.40 | 0.26 | 0.14 | 0.08 | 0.09 |
| 0 months | 3 months | 0.40 | 0.18 | 0.23 | 0.13 | 0.09 | |
| 1 month | 3 months | 0.26 | 0.18 | 0.09 | 0.14 | 0.54 | |
| UDI-6 | 0 months | 1 month | 0.36 | 0.19 | 0.17 | 0.07 | 0.02* |
| 0 months | 3 months | 0.36 | 0.43 | –0.07 | 0.12 | 0.54 | |
| 1 month | 3 months | 0.19 | 0.43 | –0.24 | 0.12 | 0.06 | |
| Total score of PFDI-20 | 0 months | 1 month | 24.39 | 15.62 | 8.77 | 4.43 | 0.05* |
| 0 months | 3 months | 24.39 | 24.37 | 0.02 | 7.42 | 0.99 | |
| 0 months | 3 months | 15.63 | 24.37 | –8.75 | 7.91 | 0.27 |
* p
| Name | Name | Average value | Average value | Difference | Standard error | p | |
| POPDI-6 | 0 months | 1 month | 0.21 | 0.09 | 0.12 | 0.05 | 0.02* |
| 0 months | 3 months | 0.21 | 0.15 | 0.06 | 0.06 | 0.24 | |
| 1 month | 3 months | 0.09 | 0.15 | –0.06 | 0.06 | 0.36 | |
| CRADI-8 | 0 months | 1 month | 0.32 | 0.22 | 0.11 | 0.05 | 0.05 |
| 0 months | 3 months | 0.32 | 0.15 | 0.17 | 0.06 | 0.00** | |
| 1 month | 3 months | 0.22 | 0.15 | 0.06 | 0.06 | 0.34 | |
| UDI-6 | 0 months | 1 month | 0.32 | 0.14 | 0.17 | 0.07 | 0.01* |
| 0 months | 3 months | 0.31 | 0.15 | 0.16 | 0.07 | 0.02* | |
| 1 month | 3 months | 0.14 | 0.15 | –0.01 | 0.08 | 0.92 | |
| Total score of PFDI-20 | 0 months | 1 month | 21.23 | 11.26 | 9.97 | 3.80 | 0.01** |
| 0 months | 3 months | 21.23 | 11.34 | 9.89 | 3.87 | 0.01* | |
| 1 month | 3 months | 11.26 | 11.34 | –0.08 | 4.47 | 0.99 |
* p
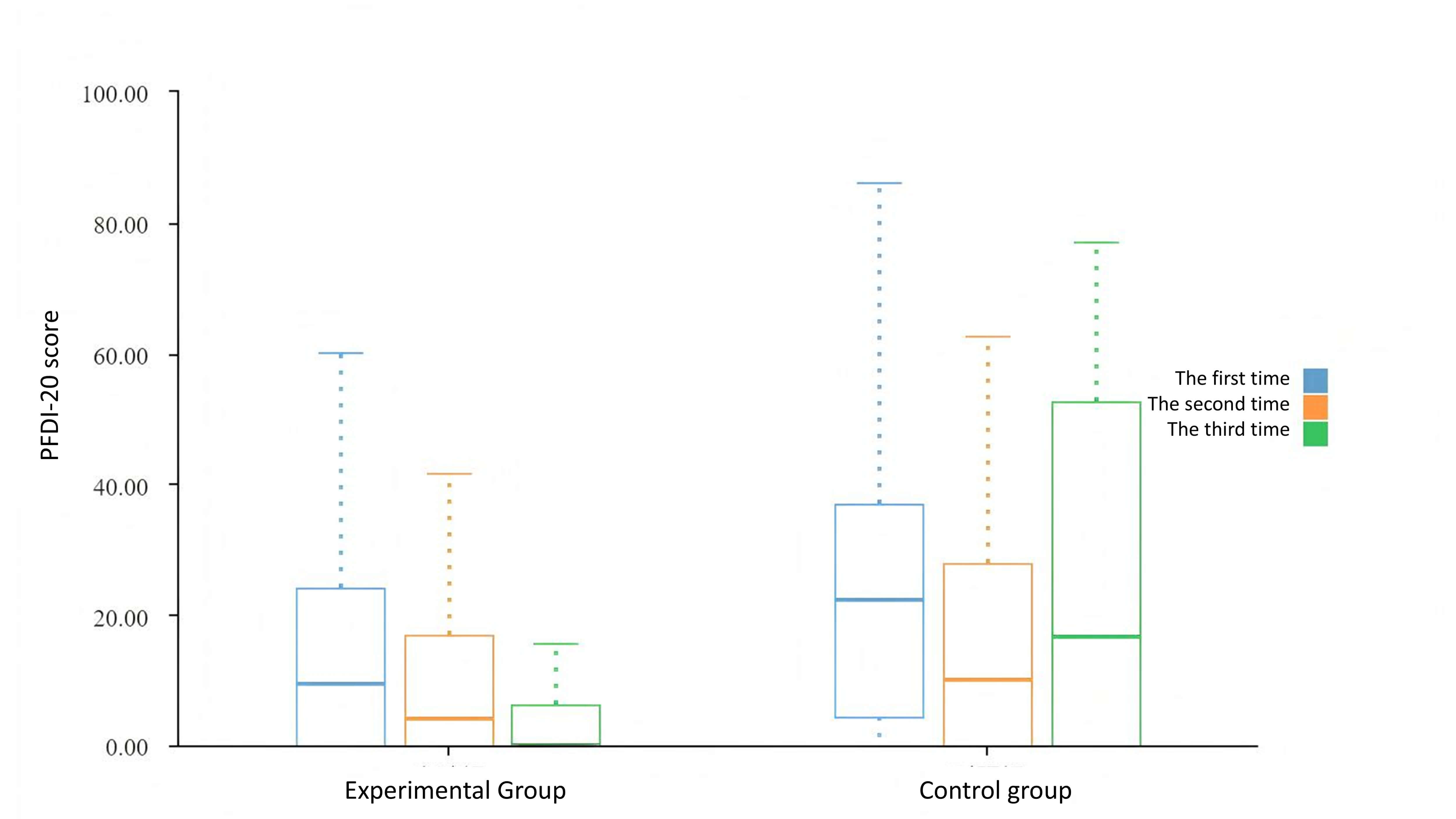
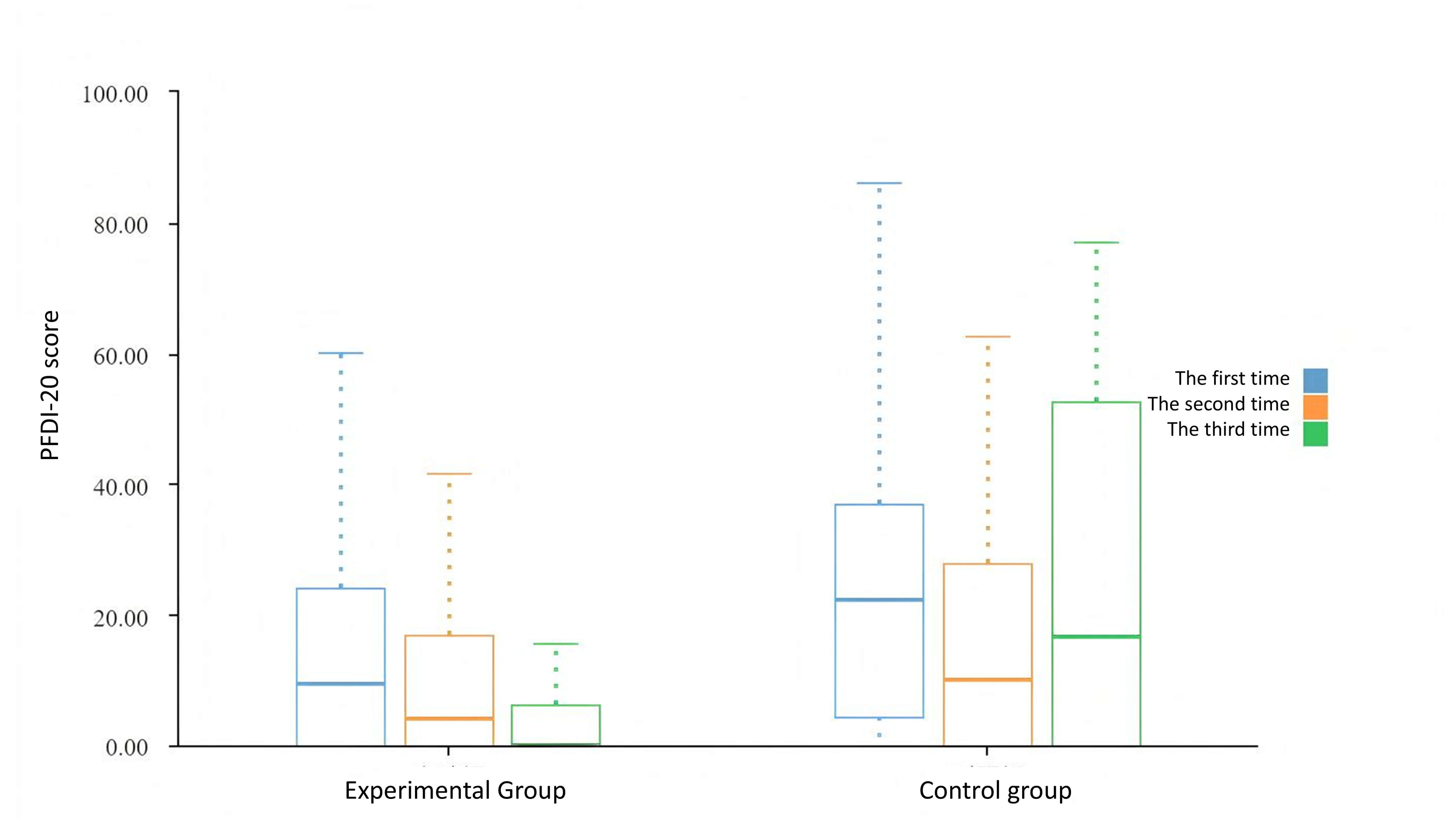 Fig. 3.
Fig. 3.
Evaluation of pelvic floor dysfunction in both groups.
Within the control group: UDI-6 (urinary distress): Scores significantly decreased from baseline to 1 month (p = 0.02), and the mean was higher at 0 months (Before intervention, 0.362 vs. 0.194), indicating symptom improvement. Total score of PFDI-20: A significant reduction was observed from baseline to 1 month (p = 0.05). The total score was higher at 0 months (24.39 vs. 15.625), indicating overall symptom improvement. All other comparisons were not statistically significant.
Within the experimental group: POPDI-6 (POP distress): Scores significantly
decreased from baseline to 1 month (p = 0.02), and the mean was higher
at 0 months (0.21 vs. 0.09), indicating symptom improvement. CRADI-8 (colorectal
and anal distress): Significant reductions were observed between baseline and 1
month (p = 0.05) and between baseline and 3 months (p
According to the analysis results of pelvic floor physiological indicators at 6
weeks postpartum, no significant difference was found between the two groups in
terms of Type I muscle strength, Type II muscle strength, and fatigue level in
statistical level (p
| Control group (N = 46) | Experimental group (N = 41) | t | p | ||
| Muscle strength evaluation | |||||
| Enter the group | |||||
| Class I fibromuscular muscle | 10.42 |
10.59 |
–0.06 | 0.96 | |
| Class II fibromuscular muscle | 18.07 |
22.56 |
–1.31 | 0.20 | |
| Fatigue % | 2.30 |
2.03 |
0.15 | 0.89 | |
| Enrollment for 1 month | |||||
| Class I fibromuscular muscle | 11.11 |
15.17 |
–1.56 | 0.12 | |
| Class II fibromuscular muscle | 20.33 |
26.50 |
–1.49 | 0.14 | |
| Fatigue % | 1.62 |
1.06 |
0.23 | 0.82 | |
| Enrollment for 3 months | |||||
| Class I fibromuscular muscle | 7.77 |
20.40 |
–3.04 | 0.00** | |
| Class II fibromuscular muscle | 22.09 |
25.80 |
–0.55 | 0.58 | |
| Fatigue % | 2.83 |
3.40 |
–0.51 | 0.62 | |
** p
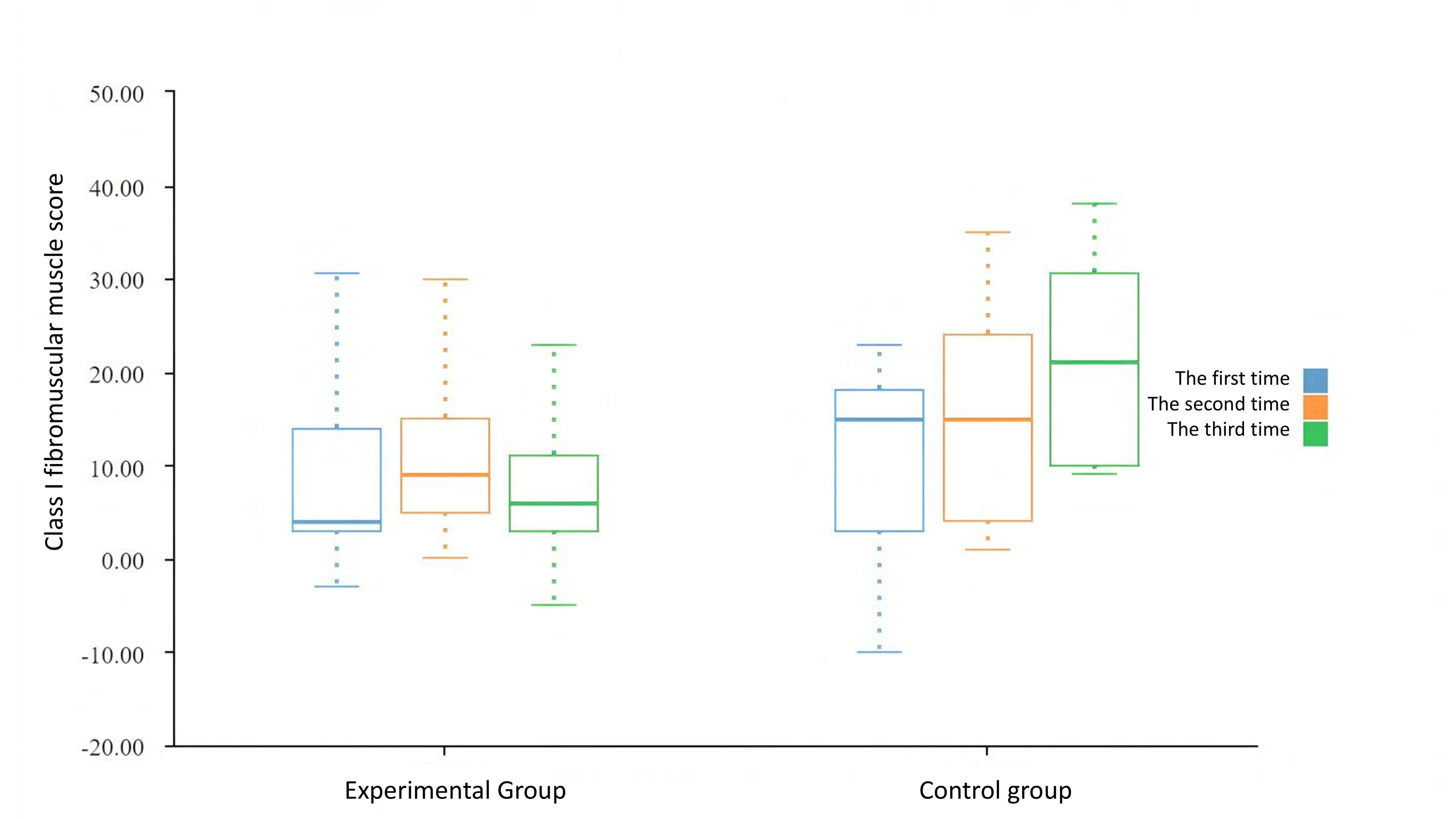
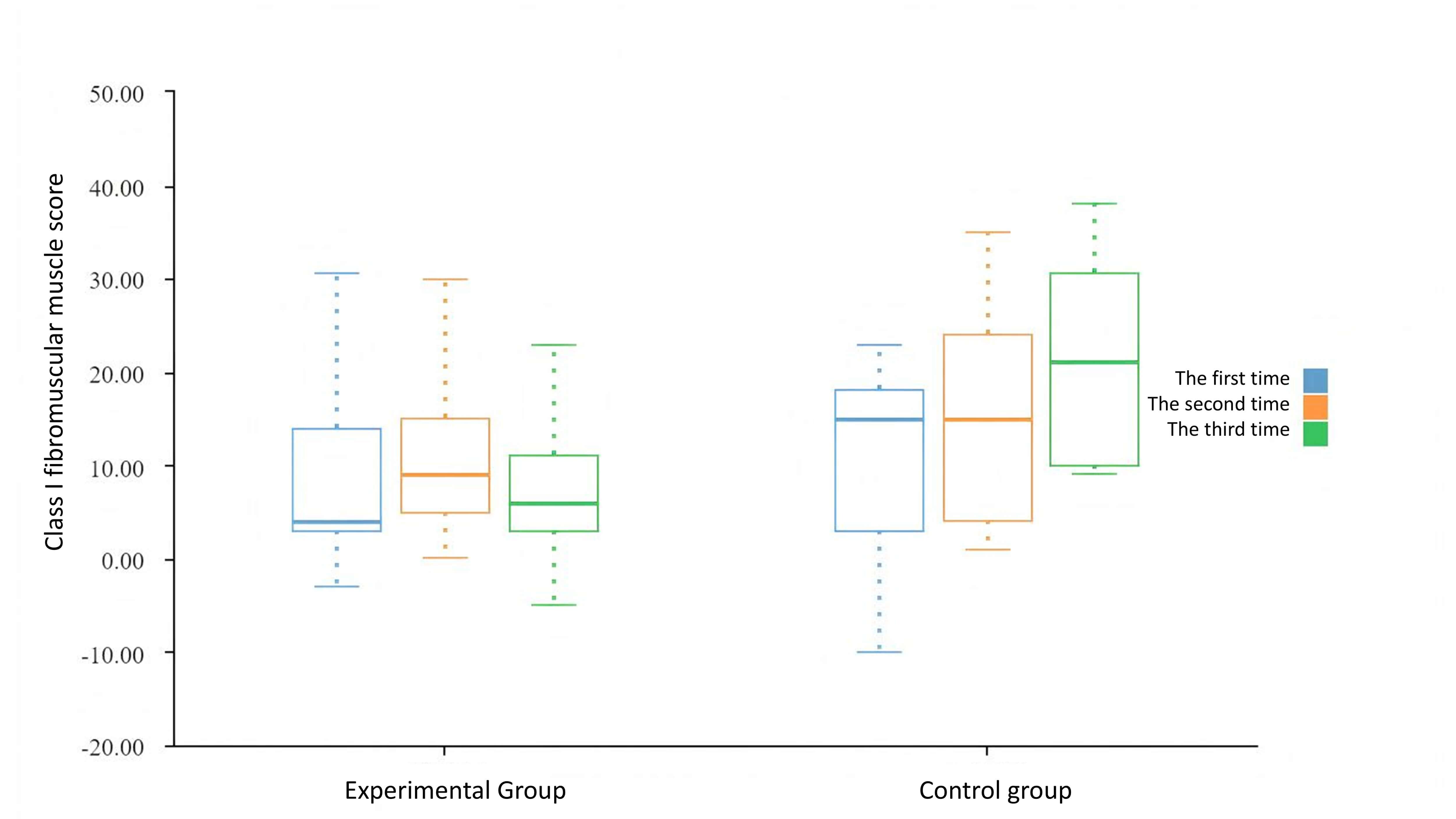 Fig. 4.
Fig. 4.
Evaluation of Class I fibromuscular muscle in the two groups.
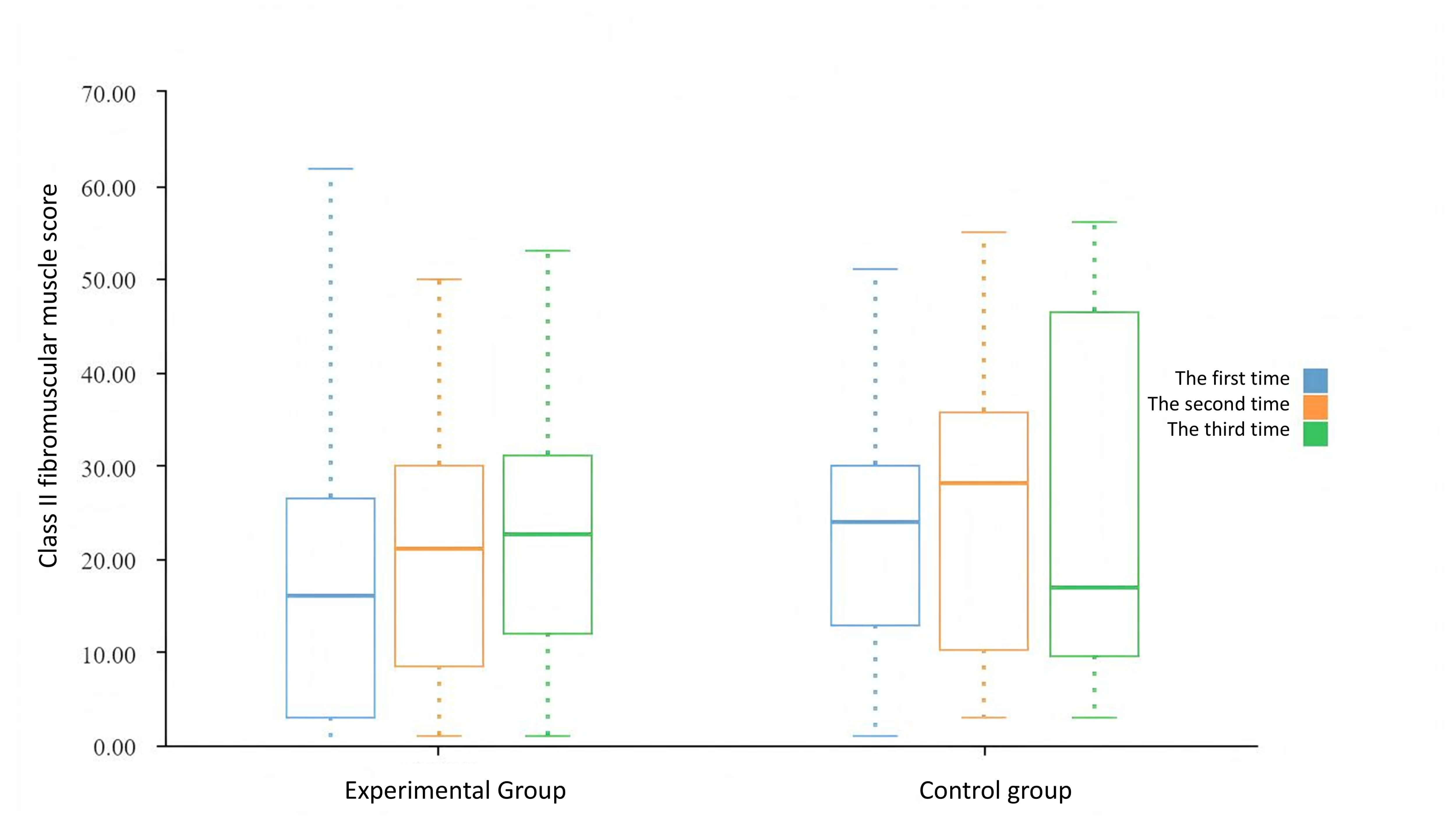 Fig. 5.
Fig. 5.
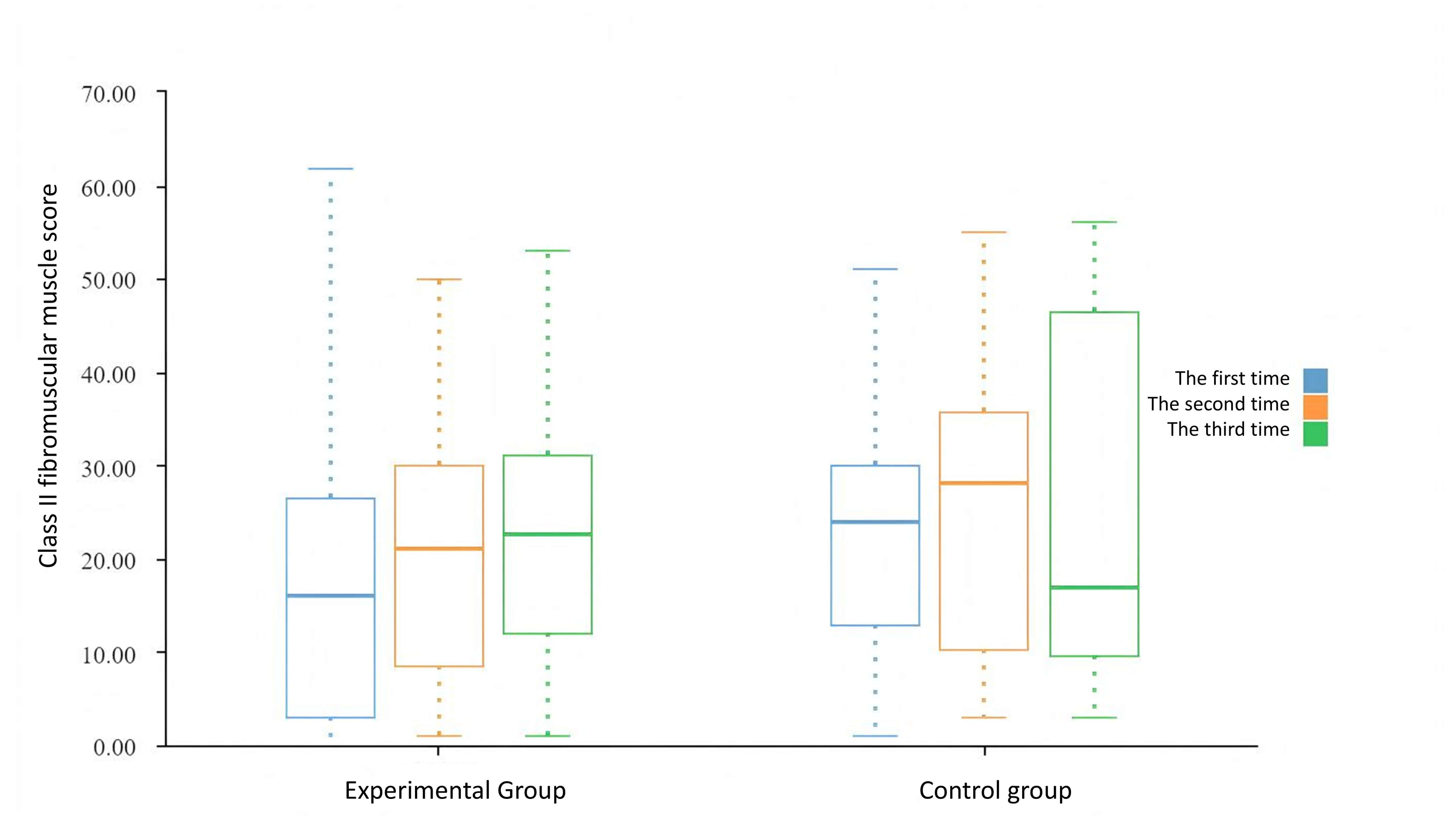
Evaluation of Class II fibromuscular muscle in the two groups.
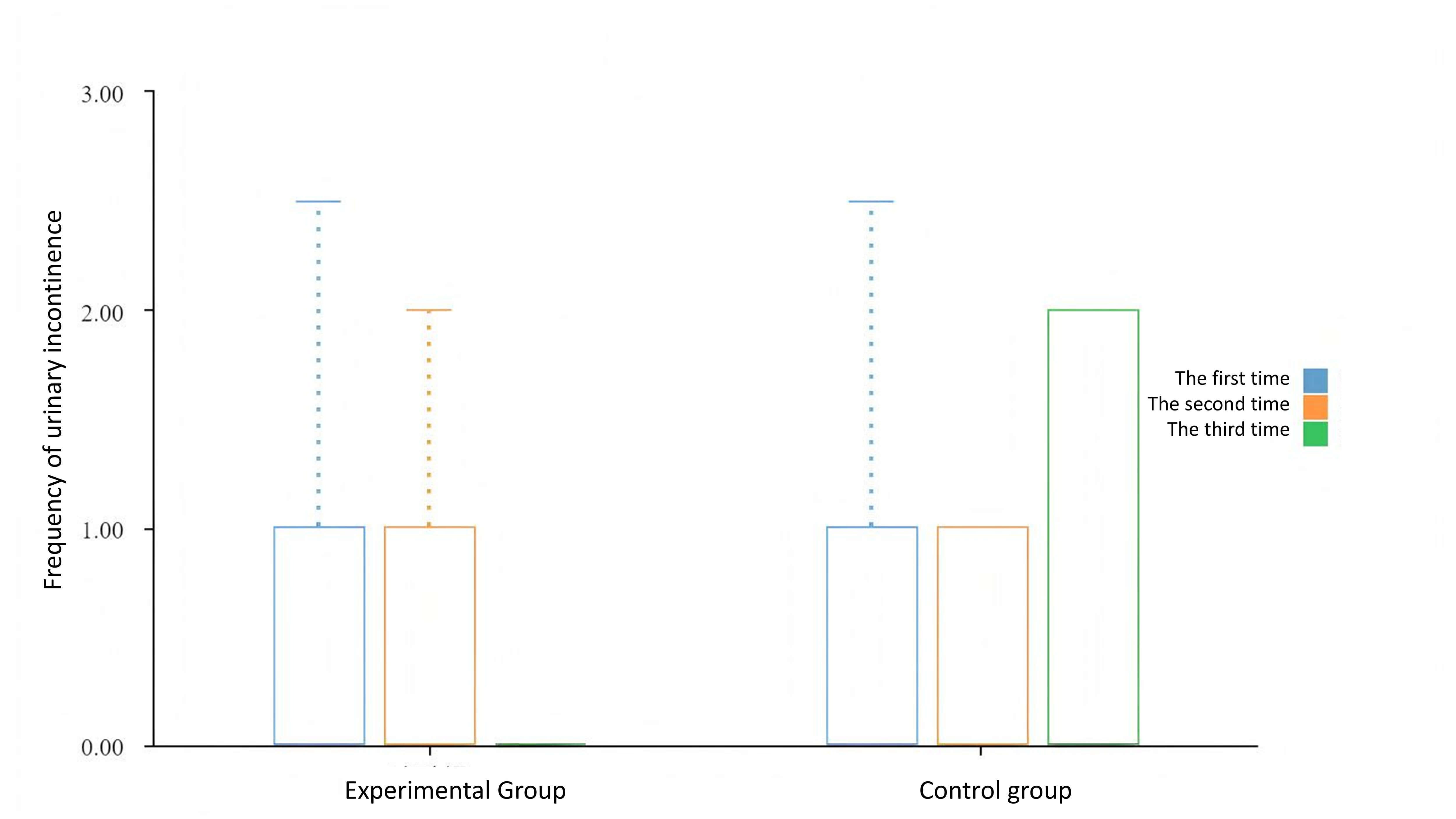
At baseline, the severity of UI symptoms did not present an obvious difference in statistical level between the two groups, indicating good baseline consistency. After 3 months of intervention, the frequency of urinary leakage differed a lot (Table 7 and Fig. 6).
| Control group (N = 46) | Experimental group (N = 41) | t | p | ||
| Urinary incontinence symptoms (ICI-Q-SF) | |||||
| Enter the group | |||||
| Urinary leakage frequency | 0.56 |
0.53 |
0.04 | 0.84 | |
| Missing urine volume | 0.53 |
0.50 |
0.02 | 0.89 | |
| Impact of urine on life | 0.62 |
0.34 |
0.91 | 0.34 | |
| Enrollment for 1 month | |||||
| Urinary leakage frequency | 0.33 |
0.41 |
0.20 | 0.66 | |
| Missing urine volume | 0.11 |
0.4 |
2.30 | 0.14 | |
| Impact of urine on life | 0.00 |
0.30 |
2.39 | 0.13 | |
| Enrollment for 3 months | |||||
| Urinary leakage frequency | 0.80 |
0.20 |
4.83 | 0.03* | |
| Missing urine volume | 0.80 |
0.34 |
1.41 | 0.24 | |
| Impact of urine on life | 0.60 |
0.20 |
1.58 | 0.22 | |
* p
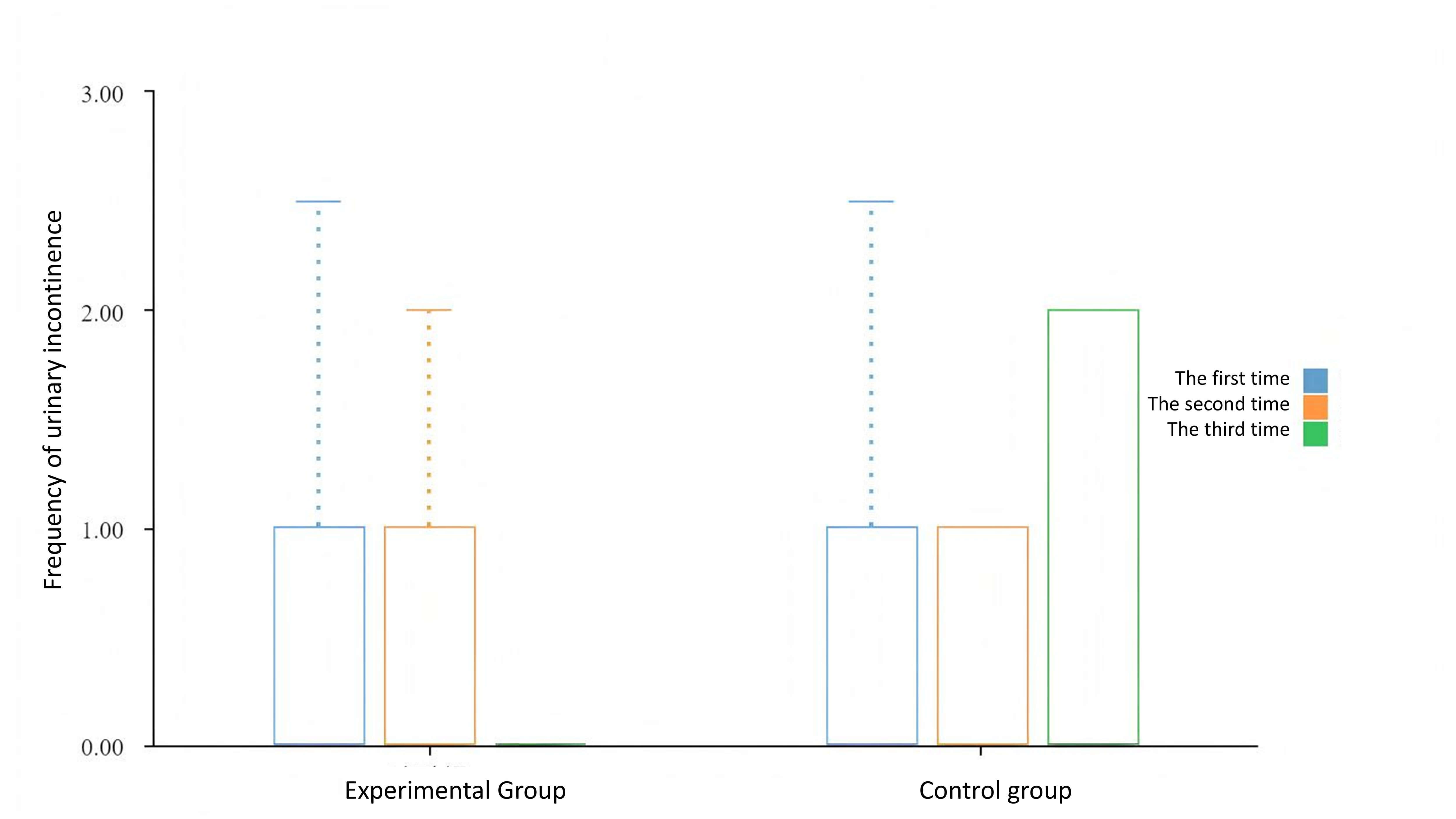 Fig. 6.
Fig. 6.
Evaluation of UI in both groups.
The intergroup comparison showed that t = 4.83 and p = 0.03
(
Holistic postural rehabilitation exercises in combination with electrical
stimulation and biofeedback improved the pelvic floor muscle strength in
postpartum patients. Baseline comparisons between the two groups demonstrated no
significant differences (p
Holistic postural rehabilitation exercises combined with electrostimulation and biofeedback reduced the frequency of postpartum urinary leakage. At enrollment, UI-related indicators showed no obvious difference between groups, ensuring reliable comparisons of subsequent intervention effects. After one month, the experimental group showed no significant advantage over the control group. At three months, however, the experimental group significantly outperformed the control group in “urinary leakage frequency”, suggesting that this intervention may require continuous implementation for at least three months to achieve measurable effects. Significant between-group differences were observed only in urinary leakage frequency at 3 months. Improvements in missing urine volume and its impact on daily life did not reach statistical significance. Possible explanations include the intervention being more specifically targeted at leakage frequency, while improvements in leakage volume and quality-of-life impact may require a longer intervention period, or the relatively small sample size (46 and 41 in the control group and experimental group, respectively) may have limited statistical power to detect differences. Globally, the prevalence of SUI in women ranges from 10% to 50% [10, 11], with rates among adult women in China reaching 18.9% [12]. Although variations exist in study populations, survey instruments, and diagnostic criteria, and prevalence differs by country and region, a study indicates a global upward trend in SUI prevalence. Many women with SUI delay seeking medical care due to limited knowledge of the condition or the stigma associated with leakage symptoms, resulting in underestimation of its true incidence in epidemiological surveys [13]. Early identification and effective intervention are of great significance for the recovery of pelvic floor dysfunction.
In 1981, Philippe Souchard empirically developed Global Postural Reeducation (GPR), which is currently used in countries including Brazil, Spain, France, and Portugal [14, 15]. In a randomized controlled trial conducted by Fozzatti et al. [16], both groups showed significant reductions in urinary leakage episodes, with a greater decrease observed in the GPR group. Both groups also showed significant decreases in daily pad use and significant improvements in pelvic floor function, with no significant difference between groups (p = 0.628). The holistic postural rehabilitation program is scientifically robust and has the potential to further improve clinical outcomes, reflecting the principles of contemporary holistic nursing.
Cross-sectional comparisons between the experimental and control groups (0 months, 1 month, and 3 months) and longitudinal analyses within each group show no baseline differences, thereby eliminating potential bias from the initial state and ensuring comparability. Despite the absence of significant differences between groups in statistical level, intra-group trends suggested potential benefits of the intervention. The lack of significant intergroup differences may be attributed to the limited sample size, which resulted in insufficient statistical power to detect potential true differences.
The follow-up duration of 3 months may have been insufficient. If the long-term effects of the intervention measures had not fully manifested, an extended follow-up would be required. Control group: Only short-term improvements in bladder symptoms and overall function were observed at 1 month, followed by complete rebound after 3 months, with no improvement in prolapse or intestinal symptoms. This pattern suggests that the observed changes may reflect natural recovery or a placebo effect, both of which are unsustainable. Experimental group: Prolapse, bladder, intestinal symptoms and overall function improved significantly and were maintained for 3 months without rebound. Notably, intestinal symptoms improved markedly from baseline to 3 months, and overall function showed significant gains from baseline to both 1 and 3 months, demonstrating the characteristics of “effective intervention”. Although no statistical differences were detected between groups, the comparison between the “comprehensive and sustained improvements” in the experimental group and the transient improvements with rebound in the control group suggests that the interventions administered to the experimental group (e.g., pelvic floor rehabilitation training and targeted therapy, though not explicitly detailed) may be superior to conventional treatment. The core principle of holistic postural rehabilitation exercises lies in combining abdominal breathing with activation and training of core muscle groups. By engaging and controlling the core, energy is transmitted from the center to the limbs and peripheral muscles, thereby maintaining stability, enhancing sensitivity, and improving muscle coordination. This process contributes to the alleviation of postpartum pelvic floor symptoms and promotes postpartum pelvic floor recovery.
Holistic postural rehabilitation exercises combined with electrical stimulation biofeedback can reduce the frequency and volume of postpartum UI, strengthen Class I fibromuscular muscles, and enhance pelvic floor stability and function, accordingly improving patients’ quality of life. Nevertheless, their effects on POP, colorectal and anal dysfunction, and lower urinary tract symptoms remain inconclusive possibly resulting from the relatively small sample size alongside short intervention duration in this study. The intervention lasted only three months, while holistic postural rehabilitation exercises typically require long-term adherence for optimal effectiveness. Future research should therefore extend the intervention period, expand the study population, and employ longitudinal designs to better elucidate the intervention’s effects.
Looking ahead, broader application of holistic postural rehabilitation exercises may deliver high-quality care, enhance postpartum women’s well-being, and provide lasting benefits throughout their lives.
The datasets used and analyzed during the current study are available from the corresponding author on reasonable request.
Study design: XW, LB; acquisition of data: YY, YZ; analysis: XW, LB, XL; drafting of the article: XW, LB, XL. All authors contributed to editorial changes in the manuscript. All authors read and approved the final manuscript. All authors have participated sufficiently in the work and agreed to be accountable for all aspects of the work.
All subjects gave their informed consent for inclusion before they participated in the study. The study was conducted in accordance with the Declaration of Helsinki, and the protocol was approved by the Ethics Committee of Peking University People’s Hospital (approval number: 2020PHB132-0).
Not applicable.
Research reported in this publication was supported by the Chinese Association of Plastics and Aesthetics under Award Number FRPR2020-nxxt-09.
The authors declare no conflict of interest.
References
Publisher’s Note: IMR Press stays neutral with regard to jurisdictional claims in published maps and institutional affiliations.