1 Department of Aristogenesis Clinic (Birth Control), Women and Children’s Hospital, School of Medicine, Xiamen University, 361000 Xiamen, Fujian, China
2 Department of Gynecology, Women and Children’s Hospital, School of Medicine, Xiamen University, 361000 Xiamen, Fujian, China
Abstract
Background: Many studies have reported irregular menstruation in women of childbearing age after vaccination or infection with severe acute respiratory syndrome coronavirus 2 (SARS-CoV-2). However, no studies have discussed the changes in menstrual patterns after reinfection with SARS-CoV-2 after vaccination. This study aimed to evaluate the effect of SARS-CoV-2 infection on menstruation in vaccinated and unvaccinated women of reproductive age. Methods: This retrospective study analysed the menstrual data of 241 women of childbearing age. Between December 8th, 2022 and February 11th, 2023, 201 participants were diagnosed with SARS-CoV-2 infection (observation group), while 40 remained uninfected (control group). The Chi-square test and Fisher’s exact test were used to assess menstrual irregularities among the participants. Logistic regression analysis was performed to determine the factors influencing menstrual patterns. Results: Among the 241 women who completed the survey, approximately one-third experienced changes in their menstrual patterns, including a shortened cycle (30.3%), a prolonged duration (13%), a decreased volume (24.9%), and increased dysmenorrhea (9.9%). Over half of the infected women did not experience any changes in their menstrual pattern. Only changes in the menstrual volume were statistically significant (p = 0.003). Logistic regression revealed that vaccination may be a protective factor against changes in the menstrual cycle (p = 0.036, odds ratio (OR) = 0.703, 95% confidence interval (95% CI): 0.506–0.977) and volume (p = 0.032, OR = 0.700, 95% CI: 0.505–0.969) after SARS-CoV-2 infection. Conclusions: SARS-CoV-2 infection did not appear to affect menstruation in vaccinated women. There were no significant changes in menstrual patterns except for menstrual cycle in women infected with SARS-CoV-2 after coronavirus disease 2019 (COVID-19) vaccination. In addition, vaccination seems to be a protective factor against changes in the menstrual cycle and volume after SARS-CoV-2 infection.
Keywords
- COVID-19
- SARS-CoV-2
- menstruation
- vaccines
Towards the end of 2019, severe acute respiratory syndrome
coronavirus 2 (SARS-CoV-2) caused an unprecedented global pandemic, leading to a
public health crisis. The pandemic caused
This monocentric retrospective study was conducted on women of childbearing age (aged 18–50 years) who were hospitalized at the Family Planning Clinic of Xiamen Maternity and Child Care Hospital (Xiamen, China) between December 8th, 2022, and February 11th, 2023. The exclusion criteria were pregnancy or lactation (in the last 6 months), early menopause or premature ovarian failure, previous hysterectomy or oophorectomy, use of hormonal contraception (oral contraceptive, hormonal intrauterine device, or etonogestrel implants), and hypothyroidism. Ultimately, 241 patients vaccinated with the Sinopharm COVID-19 vaccine (Beijing Institute of Biological Products Co., Ltd., Beijing, China) were enrolled, of whom 201 were infected (observation group) and 40 were not (control group). In this survey, we asked women of childbearing age who had received COVID-19 vaccination for information on the characteristics of their menstrual cycles before and after SARS-CoV-2 infection between January and March 2023. All women voluntarily completed the survey and provided written informed consent to participate in the study. The confidentiality of sensitive data was assured.
The primary objective was to evaluate menstrual changes after SARS-CoV-2 infection in vaccinated and unvaccinated women of childbearing age. We also evaluated alterations in sleep duration after SARS-CoV-2 infection. The participants were asked about their age, weight, height, reproductive history, vaccination status, and vaccination date (received the vaccine, completed one to four doses). All the data were collected during the clinic visit. Characteristics of the menstrual cycle, including the frequency, regularity, duration, and volume, were collected. Menstrual abnormalities were defined based on previous literature [18] and compared to the average of the last 6 cycles in the same patient before infection, which was defined as either a prolonged or a shortened menstrual cycle or period.
All the statistical analyses were performed using SPSS Statistics for Windows
(version 26.0; IBM Corp., Armonk, NY, USA). Descriptive statistics are presented
as frequencies (percentages) for categorical and continuous variables, and the
collected data were analysed using the Fisher’s exact test, and binary logistic
regression using the SPSS program. Pearson’s Chi-square test was used to compare
menstrual frequency between infected women (observation group) and uninfected
women (control group) after December 8th, 2022. Binary logistic regression models
were used to analyse the risk factors. Statistical significance was set at
p
In total, 201 women of childbearing age with confirmed SARS-CoV-2 infection and
40 women of childbearing age without SARS-CoV-2 infection were
included. The study was conducted on patients aged 18–50 years, and their
clinical characteristics are shown in Table 1. There were no significant
differences between the groups regarding sociodemographic or clinical variables,
including age, body mass index, sleep duration, profession, or age at first
menarche (p
| Parameter | Infected, N = 201 | Uninfected, N = 40 | p-value | |
| Age, years | 0.646 | |||
| 2 (1.0%) | 0 (0.0%) | |||
| 20–25 | 14 (7.0%) | 4 (10.0%) | ||
| 26–30 | 36 (17.9%) | 11 (27.5%) | ||
| 31–35 | 48 (23.9%) | 5 (12.5%) | ||
| 36–40 | 45 (22.4%) | 7 (17.5%) | ||
| 41–45 | 34 (16.9%) | 10 (25%) | ||
| 22 (10.9%) | 3 (7.5%) | |||
| Age at menarche, years | 0.207 | |||
| 11 | 5 | 1 | ||
| 12 | 37 | 6 | ||
| 13 | 49 | 20 | ||
| 14 | 57 | 5 | ||
| 15 | 26 | 3 | ||
| 16 | 22 | 2 | ||
| 17 | 5 | 1 | ||
| 18 | 0 | 8 | ||
| BMI category, kg/m |
0.078 | |||
| Low weight (BMI |
9 (4.5%) | 2 (5.0%) | ||
| Normal (18 |
170 (84.6%) | 26 (65.0%) | ||
| Overweight (25 |
7 (3.5%) | 5 (17.5%) | ||
| Obesity (BMI |
15 (7.5%) | 7 (12.5%) | ||
| Sleep duration | 0.802 | |||
| 3 (1.5%) | 1 (2.5%) | |||
| 5.1 |
18 (9.0%) | 4 (10.0%) | ||
| 6.1 |
85 (42.3%) | 15 (37.5%) | ||
| 7.1 |
71 (35.3%) | 14 (35.0%) | ||
| 24 (11.9%) | 6 (15.0%) | |||
| Occupation | 0.644 | |||
| Unemployment | 4 (2.0%) | 2 (5.0%) | ||
| Service | 8 (4.0%) | 1 (2.5%) | ||
| Self-employed | 4 (2.0%) | 1 (2.5%) | ||
| Civil servant | 12 (6.0%) | 2 (5.0%) | ||
| Internet professional | 3 (1.5%) | 0 (0.0%) | ||
| Teacher | 19 (9.5%) | 3 (7.5%) | ||
| Financier | 6 (3.0%) | 0 (0.0%) | ||
| Peasant | 1 (0.5%) | 3 (7.5%) | ||
| Salesperson | 16 (8.0%) | 3 (7.5%) | ||
| Student | 12 (6.0%) | 3 (7.5%) | ||
| Staff | 11 (5.5%) | 3 (7.5%) | ||
| Manual worker | 3 (1.5%) | 0 (0.0%) | ||
| Researcher | 57 (28.4) | 8 (20%) | ||
| Cultural worker | 3 (1.5%) | 0 (0.0%) | ||
| Others | 42 (20.9) | 12 (30%) | ||
| Pre-SARS-CoV-2 infection menstruation cycle | 0.311 | |||
| 3 (1.5%) | 2 (5.0%) | |||
| 21–27 | 52 (25.9%) | 14 (35%) | ||
| 28–35 | 132 (65.7%) | 23 (57.5%) | ||
| 36–60 | 8 (4.0%) | 1 (2.5%) | ||
| 61–90 | 6 (3.0%) | 0 (0.0%) | ||
| Pre-SARS-CoV-2 infection menstruation duration | 0.389 | |||
| 2–4 | 38 (18.9%) | 9 (22.5%) | ||
| 5–7 | 141 (70.1%) | 26 (65.0%) | ||
| 8–10 | 22 (10.9%) | 5 (17.5%) | ||
| Pre-SARS-CoV-2 infection menstrual volume | 0.604 | |||
| Normal | 125 (62.2%) | 24 (60.0%) | ||
| Light volume | 44 (21.9%) | 10 (25.0%) | ||
| Heavy volume | 32 (15.9%) | 6 (15.0%) | ||
| Pre-SARS-CoV-2 infection dysmenorrhea | 0.763 | |||
| No | 131 (65.2%) | 31 (87.0%) | ||
| Yes | 70 (34.8%) | 9 (22.5%) | ||
| Vaccination | 0.963 | |||
| Zero-shot | 7 (3.5%) | 2 (5.0%) | ||
| One-shot | 7 (3.5%) | 1 (2.5%) | ||
| Two-shot | 30 (14.9%) | 6 (15.0%) | ||
| Three-shot | 132 (65.7%) | 27 (67.5%) | ||
| Four-shot | 25 (12.4%) | 4 (10.0%) | ||
| Post-SARS-CoV-2 infection menstrual cycle | 0.003 | |||
| Unchanged | 126 (62.7%) | 29 (72.5%) | ||
| Menelipsis | 14 (7.0%) | 3 (7.5%) | ||
| Shorten | 61 (30.3%) | 8 (20.0%) | ||
| Post-SARS-CoV-2 infection menstrual frequency | 0.237 | |||
| Unchanged | 126 (62.7%) | 29 (72.5%) | ||
| Changed | 75 (37.3%) | 11 (27.5%) | ||
| Post-SARS-CoV-2 infection menstrual duration | 0.682 | |||
| Unchanged | 154 (76.6%) | 33 (82.5%) | ||
| Shortened | 21 (10.4%) | 4 (10.0%) | ||
| Prolonged | 26 (13.0%) | 3 (7.5%) | ||
| Post-SARS-CoV-2 infection menstrual volume | 0.192 | |||
| Normal | 131 (65.2%) | 29 (72.5%) | ||
| Light volume | 50 (24.9%) | 5 (12.5%) | ||
| Heavy volume | 20 (9.9%) | 6 (15.0%) | ||
| Post-SARS-CoV-2 infection dysmenorrhea | 0.718 | |||
| Unchanged | 169 (84.1%) | 35 (87.5%) | ||
| Increased | 17 (9.9%) | 2 (5.0%) | ||
| Decreased | 12 (6.0%) | 3 (7.5%) | ||
N, number; BMI, body mass index; SARS-CoV-2, severe acute respiratory syndrome coronavirus 2.
The menstrual cycle distribution of the 241 patients is shown in Table 1. There were 3 (1.5%) patients in the observation group and 2 (5%) patients in the control group with cycles shorter than 21 days. A total of 52 (25.9%) and 14 patients (35%) in the observation and control groups, respectively, had cycles lasting between 21 and 27 days. A total of 132 (65.7%) and 23 (57.5%) patients in the observation and control groups, respectively, had cycles lasting between 28 and 35 days. Fourteen (7%) participants in the observation group had cycles longer than 36 days, while one (2.5%) participant in the control group had cycles longer than 36 days. Further statistical analysis revealed no significant difference between the groups (p = 0.311).
Among the participants who reported a menstrual period in the baseline survey, in the observation group, 38 participants (18.9%) had a menstrual period lasting 2–4 days, 141 (70.1%) had a period lasting 5–7 days, and 22 (10.9%) had a period lasting 8–10 days; in the control group, 9 (22.5%) participants had a menstrual period lasting 2–4 days, 26 (65%) had a period lasting 5–7 days, and 5 (17.5%) had a period lasting 8–10 days (p = 0.389).
Among the participants in the observation group, 125 (62.2%) had a normal menstrual volume, 44 (21.9%) had a light menstrual volume, and 32 (15.9%) had a heavy menstrual volume. However, 24 (60%) patients in the control group had a normal menstrual volume, 10 (25%) had a light menstrual volume, and 6 (15%) had a heavy menstrual volume.
Dysmenorrhea typically significantly reduces women’s quality of life and was included in this study as an observational indicator. In total, 131 (65.2%) patients in the observation group did not experience dysmenorrhea, whereas 70 (34.8%) did. Moreover, 31 (77.5%) participants in the control group did not experience dysmenorrhea, whereas 9 (22.5%) did.
The menstrual cycle distribution of the 40 uninfected participants (control group) is shown in Table 1. There were 29 (72.5%) participants with unchanged menstrual cycles, 8 (20%) with a shorter menstrual cycle than before SARS-CoV-2 Infection infection, and 3 (7.5%) experienced amenorrhoea.
We found that 126 (62.7%) infected patients (observation group) had no change in their menstrual cycles, 14 (7%) experienced amenorrhoea, and 61 (20.3%) had shortened cycles (Table 1). Further statistical analysis revealed a significant difference between the groups (p = 0.003).
A total of 241 patients were included in the menstrual analysis because they had complete data on their menstrual histories available in the database. Among the control group, 29 (72.5%) patients had no change in menstrual volume, 5 (12.5%) had a decrease in menstrual volume, and only 6 (15%) had an increase in menstrual volume.
The distribution of the menstrual volume of infected patients (observation group) is shown in Table 1. A total of 131 (65.2%) patients had no change in menstrual volume, 50 (24.9%) had a decreased menstrual volume, and 20 (9.9%) had an increased menstrual volume, which was consistent with the findings in the uninfected population. Further statistical analysis revealed no significant differences between the observation and control groups in terms of menstrual volume changes (p = 0.192).
The distribution of dysmenorrhea among infected patients (observation group) is shown in Table 1. The degree of pain was unchanged in 169 patients (84.1%), alleviated in 12 patients (6%), and aggravated in 17 patients (9.9%). There was no significant difference in the degree of dysmenorrhea between the observation and control groups (p = 0.718).
Multivariate logistic regression analysis was performed to assess the effects of age, daily sleep duration, vaccination status, age at first menarche, and SARS-CoV-2 infection on menstrual patterns (Fig. 1). Vaccination (p = 0.036, odds ratio [OR] = 0.703, 95% confidence interval [95% CI]: 0.506–0.977) was found to be a significant predictor of menstrual cycle alterations after SARS-CoV-2 infection (Fig. 1A). Vaccination (p = 0.032, OR = 0.700, 95% CI: 0.505–0.969) was also a significant predictor of menstrual volume after SARS-CoV-2 infection (Fig. 1B). No predictors were found regarding menstrual duration or dysmenorrhea changes (Fig. 1C,D). In addition, age (p = 0.012, OR = 0.714, 95% CI: 0.550–0.926) was a significant predictor of changes in menstrual dysmenorrhea after SARS-CoV-2 infection (Fig. 1D).
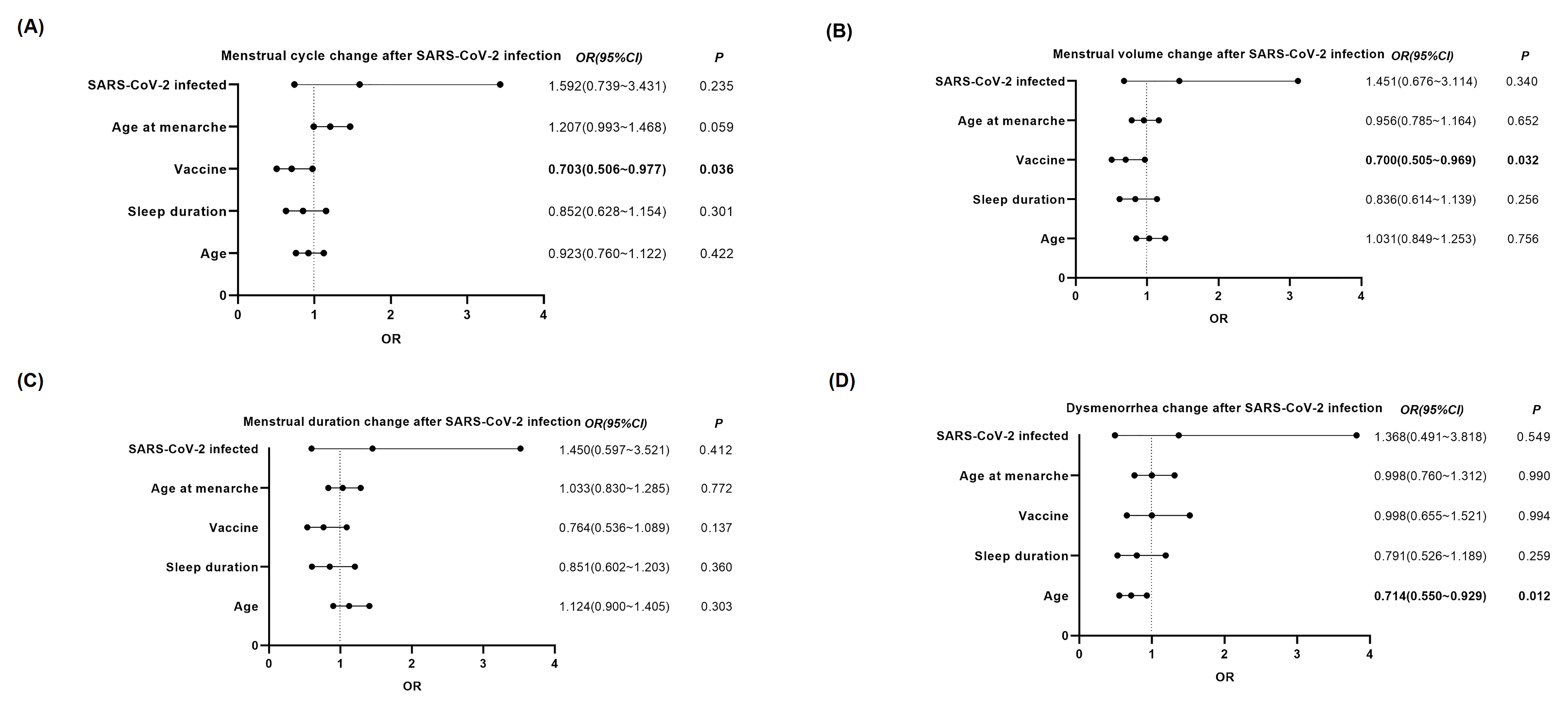 Fig. 1.
Fig. 1.Logistic regression analysis of the factors influencing menstrual patterns. (A) Menstrual cycle. (B) Menstrual volume. (C) Menstrual duration. (D) Dysmenorrhea. OR, odds ratio; 95% CI, 95% confidence interval.
In the present study, approximately two-thirds of the participants did not experience changes in their menstrual status. However, at least one of the four parameters indicated an abnormal menstrual status after December 8th, 2022, confirming the presence of changes. The female reproductive system is susceptible to known viruses, such as herpes simplex virus (HSV-2), human immunodeficiency virus (HIV), hepatitis B (HBV) and C (HCV) viruses, and Zika virus [19, 20, 21]. Studies have revealed that SARS-CoV-2 uses angiotensin-converting enzyme (ACE)-2 cell receptors to enter target cells, similar to HSV-2, HIV, HBV, HCV, and Zika virus, since ACE-2 is present in the respiratory tract and different organs, including the ovaries, uterus, and vagina [22, 23, 24]. Many studies have linked COVID-19 infection and vaccination to changes in the menstrual cycle [25, 26, 27, 28, 29]. Furthermore, COVID-19 infection has been reported to alter the menstrual cycle regardless of vaccination status [30]. However, no previous study has specifically examined menstrual pattern changes in women infected with SARS-CoV-2 after vaccination.
In our study, approximately 37.3% of the childbearing women infected with SARS-CoV-2 after vaccination experienced irregular menstrual cycles. Analysis of menstrual changes in infected patients revealed varying degrees of transient changes, including shortened cycles and decreased volume. Irregular cycles and increased volume were also observed in a few participants in the control group. When studying the effect of COVID-19 infection on menstrual patterns, several factors related to the pandemic, such as stress, vaccinations, and COVID-19 infection, must be considered. A high stress level is associated with menstrual irregularities. Since the COVID-19 pandemic changed people’s lives in many ways (e.g., by changing occupation status or affecting sleep duration), it has become a stressor that many researchers believe can affect the menstrual cycle. After vaccination, the greatest percentage of alterations were observed in menstrual volume and amenorrhea [18]. The body produces an immune response after COVID-19 vaccination, which results in the emergence of immunological memory. When first exposed to SARS-CoV-2, the body’s immune response is muted or nonexistent. The immune response following SARS-CoV-2 infection, such as that resulting from COVID-19 vaccination, could affect the hypothalamic–pituitary–ovarian axis. During the pandemic, while the menstrual cycles of most women infected with SARS-CoV-2 after COVID-19 vaccination remained unaffected, those of women who experienced anxiety, stress, and depression showed changes. In addition, our data showed that the proportion of individuals with no change in dysmenorrhea among women infected with SARS-CoV-2 after vaccination (84.1%) was approximately the same as that among women who were not infected with SARS-CoV-2 after vaccination (87.5%). There were no significant changes in menstrual patterns except for the menstrual cycle in women infected with SARS-CoV-2 after COVID-19 vaccination. Logistic regression revealed that vaccination may be a protective factor against changes in the menstrual cycle and volume after COVID-19 infection.
The COVID-19 pandemic has been the subject of research and articles over the past 3 years [31]. Women’s health issues during the COVID-19 pandemic deserve public attention. In particular, alterations in women’s menstrual patterns affect their quality of life; thus, it is important to study this topic in depth. It is essential to understand and explain the impact of SARS-CoV-2 infection on women’s health after vaccination to guide postpandemic menstrual health recovery among women.
Although the study had the limitation of having a small sample size, it had several strengths. To date, no study has investigated menstrual pattern issues related to women infected with SARS-CoV-2 after COVID-19 vaccination. This study suggested that COVID-19 infection does not affect short-term menstrual patterns among women of childbearing age who have received the COVID-19 vaccine. Since only the cycles before and after COVID-19 infection were investigated, whether the lack of change in the cycles is long-term cannot be determined based on this study. This study has certain limitations. First, it is impossible to infer causality from the results because of its cross-sectional design. Second, the number of participants involved in the data collection was limited, which limits the generalizability of the results.
SARS-CoV-2 infection does not appear to affect menstruation in vaccinated women. There were no significant changes in menstrual patterns except for the menstrual cycle in women infected with SARS-CoV-2 after COVID-19 vaccination. Vaccination seems to be a protective factor against changes in the menstrual cycle and volume after SARS-CoV-2 infection.
The datasets used and/or analysed during the current study are available from the corresponding author upon reasonable request.
RS, WW, and JA designed the study, analysed the data, and wrote the paper. JL and HD collected all the raw data. JA and WW read and approved the final manuscript. All authors contributed to editorial changes in the manuscript. All authors read and approved the final manuscript. All authors have participated sufficiently in the work and agreed to be accountable for all aspects of the work.
The study was conducted according to the guidelines of the Declaration of Helsinki and this study was reviewed and approved by the Research Ethics Committee of Women and Children’s Hospital, School of Medicine, Xiamen University (KY-2023-144-K01; Nov. 28th, 2023). Before we distributed the questionnaires, we assured the participants that the questionnaire would be used for academic research, that their personal information would be kept confidential, and that they could withdraw from the study at any stage. Moreover, the participants signed informed consent forms.
The authors would like to acknowledge the cooperation of the women of childbearing age after reinfection with SARS-CoV-2 after vaccination who participated in this study and express their gratitude for the valuable contributions of the research assistants.
This research received no external funding.
The authors declare no conflict of interest.
References
Publisher’s Note: IMR Press stays neutral with regard to jurisdictional claims in published maps and institutional affiliations.

