1 School of Physical Therapy, Western University, London, ON N6A 3K7, Canada
2 The WOMB Milton, Milton, ON L9T 1P8, Canada
3 Knew Life Physiotherapy, Ancaster, ON L9K 0C4, Canada
4 Compass Rose Wellness, Middlesex Centre, ON N0L 1R0, Canada
5 Faculty of Health Sciences, University of Ottawa, Ottawa, ON KIN 6N5, Canada
6 Faculty of Heath Science, McMaster University, Hamilton, ON L8S 4L8, Canada
Abstract
Electrical muscle stimulation (EMS) is a conservative management tool for the treatment of pelvic floor dysfunctions (PFDs). The aim of this review was to scope, summarize and critically evaluate available research investigating the impact of various modes of EMS on PFDs in females.
Joanna Briggs Institute methodology for scoping reviews was used with The Preferred Reporting Items for Systematic Reviews and Meta-Analyses Extension for Scoping Reviews. Three databases were searched. Articles published in English that included female participants living with pelvic floor muscle dysfunction where EMS was used as a conservation care intervention were included in the review. Included studies were analyzed following Arksey and O’Malley’s framework. The Cochrane Risk of Bias Tool for randomized trials was used to assess risk of bias for the randomized controlled trials (RCTs), and Hawker and Payne’s quality appraisal criteria was used to appraise the data from the other included papers systematically.
A total of 37 studies, including 20 RCTs were included. A favorable impact, across various outcomes, was found across trials which investigated different types of EMS with varying protocols. The heterogenous nature of intervention protocols limited the ability to apply any statistical or meta-analyses. EMS demonstrates a positive effect for improving outcomes related to PFDs in adult women. Included studies support the use of EMS for stress, urgency and mixed urinary incontinence. All versions of EMS studied were found to provide significant improvements, which included them being used as a sole intervention or as an adjunct intervention. High intensity forms of EMS were consistently found to require shorter intervention times.
EMS demonstrates improvement across outcomes for PFDs among adult women. In particular, the results of this review suggest that EMS may be particularly useful in women living with stress urinary incontinence (SUI) or who those are unable to perform voluntary muscle contractions when pelvic floor muscle training is attempted. Further research related to more novel versions of high intensity EMS approaches is needed.
Keywords
- review
- pelvic floor disorders
- female
- electric stimulation therapy
- conservative treatment
Electrical muscle stimulation (EMS) is a conservative management tool for the treatment of pelvic floor dysfunctions (PFDs; e.g., bladder and bowel incontinence, pelvic pain, dyspareunia, sexual dysfunction, and pelvic organ prolapse [POP]) that is supported by the 7th International Consultation on Incontinence (ICI) from the International Continence Society (ICS) and the International Consultation on Urological Diseases (ICUD) [1]. The 2023 Incontinence recommendations indicate that EMS can be considered for treatment to improve symptoms of urgency urinary incontinence (UUI), and that it can improve quality of life in women living with stress urinary incontinence (SUI; grade of recommendations: B). According to the 2023 Incontinence recommendations, medical treatments (e.g., vaginal oestrogens, propantheline bromide, and oxybutynin) appear to be less effective than EMS, or a combination of pelvic floor muscle training (PFMT) and EMS, for SUI (grade: B) [1]. Further, evidence suggests that magnetic EMS (i.e., EMS in conjunction with a magnetic field that depolarizes membranes of peripheral motor neurons and initiates muscle contraction at what are considered greater intensities than non-magnetic EMS and has been referred to as causing “supramaximal” muscle contraction) [2] should be considered for improving symptoms in women living with mixed urinary incontinence (MUI) and SUI (grade: B-new when compared to no active treatment) [1].
Pelvic floor dysfunction (PFD) is a term used to describe a series of clinical diagnoses that include challenges with control of bladder and bowel function such as incontinence, pelvic pain, dyspareunia, sexual dysfunction, and POP [3, 4]. Pelvic health physical therapy (PHPT) and PFMT are conservative, first-line treatments for many pelvic floor disorders (level of evidence: 1) [1, 5, 6]. PFMT is a general term for the instruction of pelvic muscle strengthening, relaxation, and coordination exercises led by a trained physical therapist [7]. PHPT, denotes the conglomerate of care provided by pelvic health physiotherapists which includes; education, lifestyle and behavioural counseling, manual therapy, exercise prescription, including PFMT and the use of adjuncts to support the delivery of PFMT [8, 9, 10]. Robust evidence supports the role of PHPT as a first line, minimally invasive option to treat PFDs [1, 11, 12, 13].
In the treatment of PFDs, EMS modalities can be used to promote muscle
contractions through depolarization of the motor units in muscle tissue. EMS
modalities have been used in the management of PFD, specifically urinary
incontinence, for decades [14]. A wide variety of EMS tools that vary in design,
application, invasiveness, and treatment parameters currently exist. Some EMS
tools are designed to be used intra-vaginally, which have been reported to
sometimes cause adverse events such as discomfort [5], while others apply the
energy externally to the perineal region [15, 16]. Studies have shown that a
significant percentage of women with diagnosed PFDs struggle with voluntary
pelvic floor muscle contractions [17, 18]. In one study of 325 women presenting
for evaluation of a diagnosed PFD, only 23% were able to perform a contraction
with Oxford Scale strength
A recent systematic review [20] examining perspectives on the therapeutic effects of pelvic floor EMS highlights the positive effects of EMS on urinary control and sexual quality but acknowledges clear gaps in the literature regarding EMS intensity, frequency, and duration. The results highlight a lack of standardization for EMS treatment. Current research does not provide evidence about outcomes based on the use of specific EMS tools, procedures, and protocols. In addition, newer EMS tools have been developed in recent years, many of which can only be accessed in a clinic environment. These innovations of EMS claim to be more advantageous than traditional tools, but the currently such comparisons have yet to be found in the existing literature. Therefore, the aim of this review is to scope, summarize and critically evaluate available research investigating the impact of all current forms of EMS on PFDs in females.
A scoping review allows the mapping of key concepts underpinning a research area and is useful when a topic has yet to be comprehensively reviewed. A five-stage methodological framework was used to guide the review according to the following steps: (1) identify the research question; (2) identify relevant studies; (3) select studies for more-detailed analysis; (4) chart the data; and (5) collate, summarize and report the results [21, 22]. Joanna Briggs Institute methodology was also applied to supplement the scoping review methodology [23, 24]. The review protocol was registered on the Open Science Framework on November 28, 2022 (https://osf.io/nt58u) and followed Preferred Reporting Items for Systematic Reviews and Meta-Analyses (PRISMA) guidelines. As a scoping review, ethical approval was not required in order to research.
The inclusion and exclusion criteria are presented in the methods summary (Table 1).
| Key search teams | Pelvis, pelvic floor, electrical stimulation, electrical stimulation therapy, high frequency electrical simulation, electromagnetic simulation. |
|---|---|
| Sampling strategy | Selective databases: from medicine, nursing, allied health, and science fields within specified limits. Journal hand searching from reference lists. |
| Type of article | All original, peer reviewed quantitative studies (randomized controlled trials, quasi experimental, cross sectional and cohort studies)*. |
| Approaches | Citation searches, cross referenced with google scholar and contact with authors – 38 searches including combination of search terms completed. |
| Language | English. |
| Range of years | January 2017–December 2023. |
| Inclusion and exclusion | Inclusion: studies with female subjects (18 years and older) with the diagnosis or self-reported clinical presentation of PFDs (e.g., FI, POP, and/or impaired sexual function), studies that evaluated EMS as the intervention, studies that included conservative care interventions as the comparison or control group, studies that had at least one clear measurable outcomes measure that was physical assessment or self-report. |
| Excluded: studies on populations other than the above, studies that used energy based modalities that did not incorporate an EMS component, studies that did not report clearly enough on intervention parameters or outcome measures, studies that used pharmacological or surgical interventions as the comparison, studies that used EMS for assessment not an intervention, and studies published prior to January 2017 and in a language other than English. | |
| Electronic sources | Medical Literature Analysis and Retrieval System Online (MEDLINE), Excerpta Medica Database (EMBASE), and Cumulative Index of Nursing and Allied Health Literature (CINAHL). Hand searching and reference list searching were also employed to locate peer-reviewed literature. |
PFD, pelvic floor dysfunction; FI, fecal incontinence; POP, pelvic organ prolapse; EMS, electrical muscle stimulation. All types of study designs were considered for inclusion.
*Published abstracts of studies meeting the inclusion criteria were included. Articles not available in English or that were strictly theoretical, conceptual, or grey literature were excluded.
Computer-aided searches of MEDLINE (Ovid), EMBASE (Ovid), and CINAHL were conducted in collaboration with a Health Sciences Librarian at McMaster University, who suggested the above three databases to ensure literature saturation. The final search was conducted in September 2022 (Table 1). All search terms were searched as keywords in addition to each database’s specific subject headings (e.g., MEDLINE). Within each database, search terms for electrical stimulation, electromagnetic, pelvic, pelvic floor, and women were included (see Supplementary File 1). No restrictions on language of publication were included in the search (i.e., language was used as an inclusion criterion that was manually confirmed by study authors), but databases were filtered to display results from the year 2017 and onwards only.
Covidence review management software was used for study screening and selection (https://www.covidence.org/). Citations identified through our database search were uploaded into Covidence, where duplicates were removed. Two authors [PA, NG] screened the identified papers against our inclusion criteria. Additional insight from other study authors was obtained when necessary to resolve concerns about literature eligibility. A priori it was determined that disagreements would be resolved through discussion; however, no disagreements about study inclusion occurred.
All authors performed full text data extraction to identify information from each paper (see Supplementary File 2). Arksey and O’Malley (2005) [21] framework was followed for the analysis of extracted data.
One author [PA] individually assessed the quality of the non-randomized trials using Hawker et al. (2002) [25] quality appraisal criteria. The Hawker et al. (2002) [25] tool consists of nine subscales (i.e., abstract and title, introduction and aims, method and data, sampling, data analysis, ethics and biases, results, transferability and generalizability, and implications and usefulness of the study). The items in each subscale are rated on a 4-point ordinal scale described as good (4), fair (3), poor (2), and very poor (1). Each article received a summary score within a range of 9–36 [25]. A score of 28–36 was associated with good quality articles, 20–27 for fair articles, 10–20 for poor quality articles, and less than 10 for very poor-quality articles.
A different author [HA] independently assessed the risk of bias for the included randomized trials using the Cochrane Risk of Bias Tool for randomized trials (RoB 2) [26]. The risk of bias (RoB) 2 assesses seven domains: random sequence generation, allocation concealment, blinding of participants and personnel, blinding of outcome assessment, incomplete outcome data (attrition bias), selective reporting (reporting bias), and other biases [26]. Risk was categorized as: low, high or unclear with some concerns.
A total of 37 articles from 15 different countries published between 2017–2022 were included in this review (Fig. 1). All studies demonstrated improvements on outcomes following the studied EMS intervention (Table 2, Ref. [8, 14, 15, 16, 27, 28, 29, 30, 31, 32, 33, 34, 35, 36, 37, 38, 39, 40, 41, 42, 43, 44, 45, 46, 47, 48, 49, 50, 51, 52, 53, 54, 55, 56, 57, 58]).
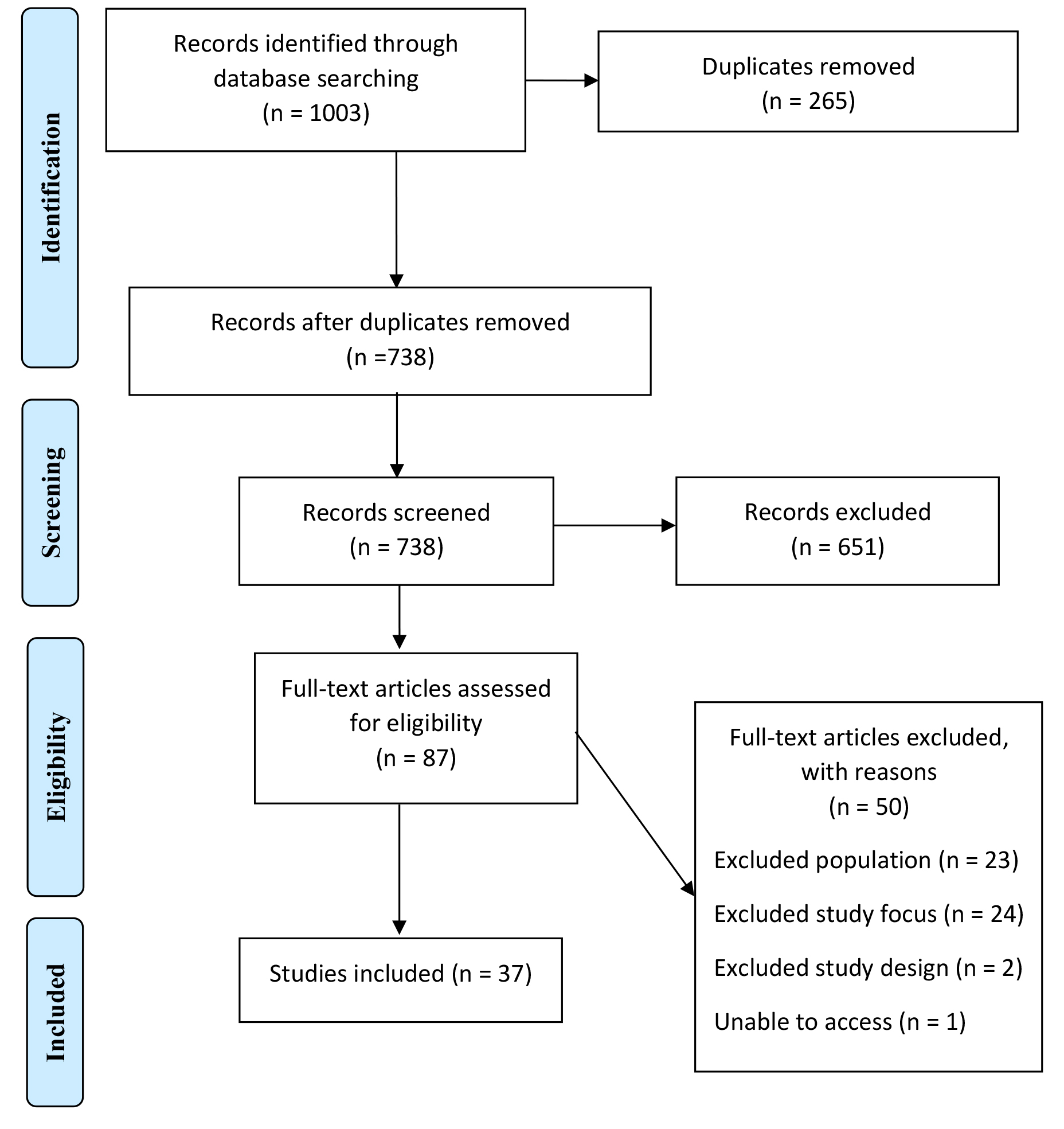 Fig. 1.
Fig. 1.
Flow-chart of the process of the scoping review article identification, screening, and eligibility.
| Author/country | Study design | Sample size | Participants (median age, years) | EMS type; mode; Tool used | Intervention parameters | Outcome measures | Relevant findings | Risk of bias/quality assessment |
|---|---|---|---|---|---|---|---|---|
| Aalaie et al., 2021 Iran [30] | RCT | 22 | Women (50.1) | Low frequency (10 Hz); intervaginal; Enraf Nonius Myomed | 2 sessions/w | FSFI | Significant improvement on FSFI score (p |
Low risk of bias |
| 6 w | ||||||||
| 100 min/session | ||||||||
| Total = 1200 min | ||||||||
| Brusciano et al., 2020 Italty [31] | Prospective cohort | 30 | Women, n = 26 | High frequency (60 Hz); HIFEM external application; Tesla Care®Armchair | 1 session/w | CCFIS | Significant improvement of the CCFIS and FIQL (p |
Score = 30 |
| Men, n = 4 (65) | 8 w | FIQL | Good quality | |||||
| 15 min/session | ||||||||
| Total = 120 min | ||||||||
| Chiu et al., 2018 USA [32] | Retrospective case series | 27 | Women (49.7) | Low frequency (20 Hz); intravaginal; Urostym® | Ranged across participants | Number of urinary incontinence accidents | Significant decrease in the number of urinary incontinence accidents post EMS intervention (p |
Score = 25 |
| Minimum of 4 sessions to fulfil the intervention criteria = 21/27 | Fair quality | |||||||
| Firinci et al., 2020 Turkey [33] | RCT | 69 | Women (55) | Low frequency (10 Hz); intervaginal; Enraf Nonius Myomed | 3 sessions/w | Pad test (24 h) | Adding EMS to behavioral therapy increased treatment effectiveness on all outcomes | Low risk of bias |
| 8 w | PFM strength | |||||||
| 20 min/session | IIQ-7 | |||||||
| Total = 480 min | ||||||||
| Guerette 2022 USA [15] | RCT | 47 | Women (43) | High frequency ( |
2 sessions/w | Pad use (over 6 months) | Significant improvements in ICIQ-LUTS in the HIFEM group (p |
Some risk of bias concerns |
| 3 w | UDI-6 | |||||||
| 28 min/session | ICIQ-LUTS | |||||||
| Total = 168 min | Other outcomes improved in both groups | |||||||
| Gumussoy et al., 2021 Turkey [34] | RCT | 51 | Women (51) | High frequency (50 Hz); HIFEM external application; Magther E-6000 system | 2 sessions/w | Pad test (1 h) | The mean scores on the I-QOL improved significantly in both groups (p |
Some risk of bias concerns |
| 8 w | I-QOL | |||||||
| 20 min/session | FSFI | |||||||
| Total = 320 min | PFMS (perineometry and oxford scale) | There was no statistically significant difference between the groups in terms of cure and improvement (p = 0.895) | ||||||
| Hiemstra et al., 2020 Netherlands [35] | Pilot study abstract only | 31 | Women | High frequency (50 Hz); HIFEM external application; Pelvipower | 1 session/w | PGI-S PGI-I | 33% of participants (n = 5) went from mild/moderate SUI complaints to light/no complaints on the PGI-S and PGII. The number of participants with moderate to severe SUI decreased from 62% to 40% | Score = 16 |
| 6 w | Poor quality | |||||||
| 30 min/session | ||||||||
| Total = 180 min | ||||||||
| Hwang et al., 2020 Korea [36] | RCT | 34 | Women (42) | Low frequency (25 Hz); external application; EasyK7 | 5 sessions/w | PFMS (perineometry) | Significant differences were observed in the EMS group for muscle strength, power and endurance (p |
Low risk of bias |
| 8 w | UDI-6 | |||||||
| 15 min/session | Pad test (ultra short) | |||||||
| Total = 600 min | ||||||||
| Hwang et al., 2020 Korea [37] | RCT | 33 | Women (42) | Low frequency (25 Hz); external application; EasyK7 | 5 sessions/w | PFMS (perineometry) | The p-values for the differences in PFM measurements between the groups, and between the pre and post-intervention measurements within the EMS group, were 0.001 and 0.004 for power, 0.015 and 0.011 for strength. In addition, in the PISQ increased to a greater extent in the EMS group | Low risk of bias |
| 8 w | PSIQ | |||||||
| 15 min/session | ||||||||
| Total = 600 min | ||||||||
| Hwang and Lee 2021 Korea [16] | RCT | 33 | Women (42) | Low frequency (25 Hz); external application; EasyK7 | 5 sessions/w | PFMS (perineometry) | There were significant differences for a main effect between pre- and post-training and between groups in PFM strength in favour of the EMS group. PFM strength (p |
Low risk of bias |
| 8 w | Diaphragm excursion (ultrasound) | |||||||
| 15 min/session | ||||||||
| Total = 600 min | ||||||||
| Hwang et al., 2023 Korea [38] | RCT | 34 | Women (42) | Low frequency (25 Hz); external application; EasyK7 | 5 sessions/w | IIQ-7 | The EMS group showed significantly improved IIQ-7 scores and PFM performance, and had significantly higher values in both one and double-leg lowering tests (p |
Low risk of bias |
| 8 w | PISQ | |||||||
| 15 min/session | PFMS (perineometry) | |||||||
| Total 600 min | ||||||||
| Ignácio Antônio et al., 2022 Brazil [8] | RCT | 61 | Women (53) | High frequency (50 Hz); intravaginal; device not specified | 1 session/w | PFMS (oxford scale) | PFMS was acquired by 36% of the experimental group and 12% of the control group (absolute risk difference 0.24, 95% CI: 0.02 to 0.43). The experimental group improved by a mean of 2 points more than control group on the ICIQ-UI-SF (95% CI: 0.02 to 3.97) | Low risk of bias |
| 8 w | ICIQ-UI-SF | |||||||
| 20 min/session | ||||||||
| Jha et al., 2018 England [39] | RCT | 144 | Women (46) | Low frequency (40 Hz); intervaginal; device not specified | EMS protocol not reported | PISQ | No significant differences in outcomes between groups. Both groups demonstrated clinical significant improvement | Some risk of bias concerns |
| SF-36 | ||||||||
| Kołodyńska et al., 2022 Poland [40] | Prospective cohort | 60 | Women (57) | Low frequency (20 Hz); intervaginal; MyoPlus4 | 5 sessions/w | Pad test 1 h | Significant reduction in pad weight for the EMS group (p |
Score = 30 |
| 2 w | Good quality | |||||||
| 30 min/session | ||||||||
| Total = 300 min | ||||||||
| Li et al., 2020 China [41] | RCT | 67 | Women (31) | High frequency (50 Hz); intravaginal; device not specified | 5 sessions | PFMS | No significant difference of muscle strength (oxford scale) between the two groups; in the EMS group the mean value of EMG in endurance was significantly improved (p |
Low risk of bias |
| (perineometer & oxford scale) | ||||||||
| 30 min/session | PFIQ-7 | |||||||
| Total = 300 min | IIQ-7 | |||||||
| Lim et al., 2021 South Korea [42] | Prospective cohort | 54 | Women (51) | Low frequency (27 Hz); external application; Kegel Smart | 2 sessions/d | PFMS (perineometer) | The EMS group achieved significantly greater reductions in LUTS (p |
Score = 35 |
| 8 w | Good quality | |||||||
| 15 min/session | BFLUTS | |||||||
| Total = 1800 min | KHQ | |||||||
| Liu et al., 2018 China [43] | Prospective cohort | 72 | Women (56) | High frequency (80 Hz); intravaginal; PHENIX | 2 sessions/w | PFMS (perineometer) | Both groups saw significant improvement in the frequency of UI episodes after 8-weeks (p |
Score = 31 |
| 8 w | CIQ-UI SF | Good quality | ||||||
| 30 min/session | ||||||||
| Total = 480 min | ||||||||
| Lu et al., 2020 China [44] | Prospective cohort | 180 | Women (30) | High frequency (80 Hz); intravaginal; PHENIX | 2 sessions/w | PFMS (perineometer) | Maximal urethral closure pressure, maximal urethral pressure, maximum urinary flow rate and electromyogram values in the EMS and control groups were significantly increased after treatment, and the values in the EMS group were greater than those in the control group (all p |
Score = 26 |
| 12 w | Fair quality | |||||||
| 15 min/session | ||||||||
| Total = 450 min | ||||||||
| Martín Prieto et al., 2023 Spain [45] | Prospective cohort | 27 | Women (58) | Low frequency (35 Hz); intrarectal; MAPLe probe | 1–2 sessions/w | PFMS (perineometer) | Maximum voluntary manometric contraction, the average and peak resistance, the average general voluntary contraction, and average and peak voluntary contraction for both the external anal sphincter and the puborectalis significantly improved from baseline (p |
Score = 28 |
| 10 sessions | Good quality | |||||||
| 30 min/session | ||||||||
| Total = 300 min | ||||||||
| Mundet et al., 2021 Spain [46] | RCT | 180 | Women (61) | Low frequency (35 Hz); intervaginal; Elpha 3000 EMS unit +Periform+ vaginal probe vs. Low frequency (35 Hz); extravaginal; Elpha 3000 EMS unit with surface electrodes | 5 sessions/w | PFMS (perineometer) | Improvement was across all 4 groups with the intervaginal EMS group demonstrating the most notable improvement across PFM characteristics. There was a statistically significant decrease in the ICIQ score at 3 months post-treatment in both EMS groups (intravaginal and extravaginal) | Some risk of bias concerns |
| 12 w | ICIQ | |||||||
| 30 min/session | ||||||||
| Total = 360 | ||||||||
| Nicoletti et al., 2020 USA [47] | Prospective cohort | 39 | Women (63) | Low frequency (20 Hz); intervaginal; Urostym | 2–3 sessions/w | OAB-q | HRQL significantly improved post EMS (p |
Score = 30 |
| 8 w | HRQL | Good quality | ||||||
| 15 min/session | ||||||||
| Total = 320 min | ||||||||
| Oldham et al., 2021 UK [48] | RCT | 86 | Women (46) | High frequency (125 Hz); intravaginal; Pelviva | 3–4 sessions/w | Pad test (1 h) | Significant improvement scores on ICIQ-UI (p |
Low risk of bias |
| 12 w | ICIQ-U | |||||||
| 30 min/session | PGI-I | |||||||
| Total = 180 | PISQ-IRI | |||||||
| Ptaszkowski et al., 2020 Poland [49] | RCT | 41 | Women (64) | High frequency (50 Hz); HIFEM external application; Solus Talen | 1 single session | PFMS (electromyograpy) | In the EMS group, there was a significant improvement in the surface electromyography measurements of PFM activity (p |
Some risk of bias concerns |
| 20 min/session | ICIQ-SF | |||||||
| Total = 20 min | ||||||||
| Rodrigues et al., 2019 Brazil [50] | RCT | 35 | Women (58) | High frequency (50 Hz); intravaginal; device not specified | 1 session/w | PFMS | PFMS in the vibratory group improved significantly in relation to the EMS group (p = 0.026); ICIQ-UI improved significantly for both groups (p |
Low risk of bias |
| 6 sessions | (oxford scale) | |||||||
| 6 w | ICIQ-UI | |||||||
| 20 min/session | ||||||||
| Total = 120 min | ||||||||
| Samuels et al., 2019 USA [14] | Prospective cohort | 75 | Women (55) | High frequency ( |
2 sessions/w | Pad test | An average improvement of 64.42% in ICIQ‐SF score was observed after the 6-week follow‐up (p |
Score = 28 |
| 3 w | (# of pads used) | Good quality | ||||||
| 6 sessions | ICIQ-SF | |||||||
| 28 min/session | ||||||||
| Total = 168 min | ||||||||
| Samuels et al., 2020 USA [27] | Prospective cohort | 31 | Women | High frequency ( |
2 sessions/w | ICIQ-UI | Initial ICIQ-UI scores were significantly improved at 1, 3 and 6 months respectively (p |
Score = 11 |
| 6 sessions | FSFI | Very poor quality | ||||||
| Total = 168 | PISQ | |||||||
| Scaldazza et al., 2017 Italy [51] | RCT | 60 | Women (59) | Low frequency (20 Hz); intravaginal; device not specified | 3 sessions/w | OAB-q SF | A reduction in daily voiding episodes was found both with EMS+PFMT and with percutaneous tibial nerve stimulation (PTNS) with a significant difference in the group of participants undergoing percutaneous tibial nerve stimulation (p |
Some risk of bias concerns |
| 10 sessions | PGI-I | |||||||
| 6 w | ||||||||
| 60 min/session | ||||||||
| Total = 1800 min | The PGI-I showed improvements in both groups, favouring the PTNS group. This study demonstrates the effectiveness of PTNS and EMS with PFMT in women with OAB, but greater improvements for PTNS | |||||||
| Silantyeva et al., 2021 Russia [28] | Prospective cohort | 95 | Women (31) | High frequency ( |
2–3 sessions/w | PFMS – (perineometrey) | PFIQ-7 scores significantly improved for participants in the HIFEM group (p |
Score = 33 |
| 4–5 w | PFIQ-7 | This study documented that the HIFEM procedure was significantly more effective than low frequency EMS in treatment of PFDS in postpartum women. Both the objective and subjective evaluation indicates more profound effects of HIFEM | Good quality | |||||
| 10 sessions | ||||||||
| Total = 224 min | ||||||||
| Silantyeva et al., 2021 Russia [28] * | Prospective cohort | 95 | Women (31) | High frequency ( |
2–3 sessions/w | Transperineal-US | Significant improvement in PFDI-20 score (p |
Score = 30 |
| 4–5 w | PFDI-20 | Good quality | ||||||
| 10 sessions | ||||||||
| Total = 224 min | ||||||||
| *both interventions administered matched parameters | ||||||||
| Singhal et al., 2022 USA [29] | Prospective cohort | 49 | Women (59) | High frequency ( |
2 sessions/w | BFLUTS-SF | Significant improvement BFLUTS-SF scores including Filling (p |
Score = 27 |
| 6 sessions | POP-Q score | Fair quality | ||||||
| 28 min/session | ||||||||
| Total = 168 | ||||||||
| Wang et al., 2022 China [52] | Retrospective study | 78 | Women (48) | Low frequency (33 Hz); intravaginal; PHENIX | Protocol 1 | I-QOL | The longer EMS protocol (15 min EMS group) had improved PFM parameters than the 10 min EMS group. There were no other between group differences | Score = 30 |
| 10 min EMS sessions | PISQ-12 | Good quality | ||||||
| vs. Protocol 2: | PFMS (OS) | |||||||
| 15 min EMS sessions | ||||||||
| *Number of sessions not reported | ||||||||
| Weber-Rajek et al., 2020 Poland [53] | RCT | 111 | Women (68) | High frequency (50 Hz); HIFEM external application; NeoControl chair | 3 sessions/w | RUSI | A statistically significant decline in depressive symptoms (BDI-II) and an improvement in urinary in- continence severity (RUIS) and quality of life (KHQ) were found in both EMS and PFMT groups (p |
Low risk of bias |
| 4 w | GSES | |||||||
| 15 min/session | BDI | |||||||
| Total = 180 min | KHQ | |||||||
| Yang et al., 2021 Taiwan [54] | Retrospective cohort | 73 | Women (59) | Low frequency (20 Hz); intervaginal; Urostym | 2 sessions/w | PFMS (perineometry) | Vaginal pressure in the total study population, SUI, and MUI groups increased significantly at week 6 (p = 0.000, 0.000, & 0.015, respectively) and week 12 (p = 0.000, 0.000, & 0.002, respectively). UDI-7 and IIQ-7 scores improved significantly. The intervention was particularly effective for subjects with SUI | Score = 29 |
| 12 w | UDI-6 | Good quality | ||||||
| 15 min/session | IIQ-7 | |||||||
| Total = 480 | ||||||||
| Yildiz et al., 2021 Turkey [55] | RCT | 62 | Women (55) | Low frequency (10 Hz); intervaginal; Enraf Nonius Myomed | 2 sessions/w | PFMS (perineometey) | The severity of incontinence, frequency of voiding, frequency of incontinence episodes, nocturia, number of pads used, symptom severity, and quality of life parameters were all significantly improved in the EMS group (p |
Low risk of bias |
| 8 w | OAB-V8 | |||||||
| 25 min/session | IIQ-7 | |||||||
| Total = 400 min | ||||||||
| Yildiz et al., 2022 Turkey [56] | RCT | 52 | Women (57) | Low frequency (10 Hz); intervaginal; Enraf Nonius Myomed | 5 sessions/w | PFMS – (perineometey) | All outcomes were significantly improved in both the EMS groups (treatments 2x and 5x per week; p |
NA |
| 8 w | OAB-V8 | |||||||
| 20 min/session | IIQ-7 | |||||||
| Total = 800 min | ||||||||
| vs. | ||||||||
| 2 sessions/w | ||||||||
| 8 w | ||||||||
| 20 min/session | ||||||||
| Total = 400 min | ||||||||
| Zhou et al., 2020 China [57] | RCT | 720 | Women (27) | High frequency (80 Hz); intervaginal; PHENIX | 2 sessions/w | PFMS – (perineometry) | The EMS group showed significantly improved POP-Q scores compared with the control group (p |
Low risk of bias |
| 8 w | ICI-Q-SF | PFDS respond favorably to intense EMS when combined with PFMT | ||||||
| 15 min/session | PFIQ-7 | |||||||
| Total = 240 | ||||||||
| Zhu et al., 2022 China [58] | Prospective cohort | 110 | Women (28) | High frequency (80 Hz); intervaginal; device not specified | 2 sessions/w | ICIQ-SF | ICIQ-SF and I-QOL scores in the study group (EMS intervention) were significantly better (p |
Score = 29 |
| 5 w | I-QOL | Good quality | ||||||
| 20 min/session | PFDI-20 | |||||||
| Total = 4050 min |
Summary of the relevant findings from the peer-reviewed literature.
EMS, electrical muscle stimulation; HIFEM, high intensity focused electromagnetic stimulation (frequency of 50 Hz, magnetic stimulation); RCT, randomized controlled trial; UI, urinary incontinence; POP, pelvic organ prolapse; PFMT, pelvic floor muscle training; PFMS, pelvic floor muscle strength; FI, fecal incontinence; SUI, stress urinary incontinence; OAB, overactive bladder; MUI, mixed urinary incontinence; UUI, urge urinary incontinence; w, week; UDI-6, urinary distress inventory-6.
Outcome Measures: PFDI-20, pelvic floor disability index; PGI-S, patient global impression of severity; PGI-I, patient global impression of improvement; I-QOL incontinence quality of life; ICIQ-UI, international consultation on incontinence questionnaire urinary incontinence short form; PISQ-IR, pelvic organ prolapse/urinary incontinence sexual questionnaire; IIQ-7, incontinence impact questionnaire; BFLUTS-SF, Bristol’s female lower urinary tract symptoms questionnaire; FISI, fecal incontinence severity index; FISS, fecal incontinence severity score; FSFI, female sexual function index; CCFIS, cleveland clinic fecal incontinence score; FIQL, fecal incontinence QOL scale; PFIQ-7, pelvic floor impact questionnaire; PISQ-IRI, pelvic organ prolapse/urinary incontinence sexual questionnaire; ICIQ-LUTS, international consultation on incontinence questionnaire lower urinary tract symptoms; BDI-II, Beck depression inventory-II; KHQ, King’s health questionnaire; RUIS, the revised urinary incontinence scale; OAB-Q, overactive bladder questionnaire; * indicates a published abstract.
Of the 37 studies, the majority were randomized controlled trials (RCTs) (n = 20), followed by prospective cohort studies (n = 13), with the remaining 4 studies constituting low level designs; retrospective (n = 3) and pilot (n = 1). Refer to Table 2 for a summary of results.
The 20 RCTs were rated using the Cochrane RoB 2. Fourteen of the studies were found to have low risk of bias, and six of the studies were found to have some concerns regarding risk of bias (Fig. 2 and Table 2). The other 17 studies were assessed for quality using the Hawker & Payne scale. Twelve of the studies were rated as “good” quality, three were rated as “fair”, one was rated “poor,” and one was rated “very-poor” (Table 2). Overall, the majority of the risk of bias assessments for the included RCTs was low, and the quality assessments for the prospective and retrospective studies (including the one pilot study) was high, indicating we can have reasonable trust in the results of this review; however, we suggest interpreting each included study with caution as appropriate based off their individual assessments (Table 2).
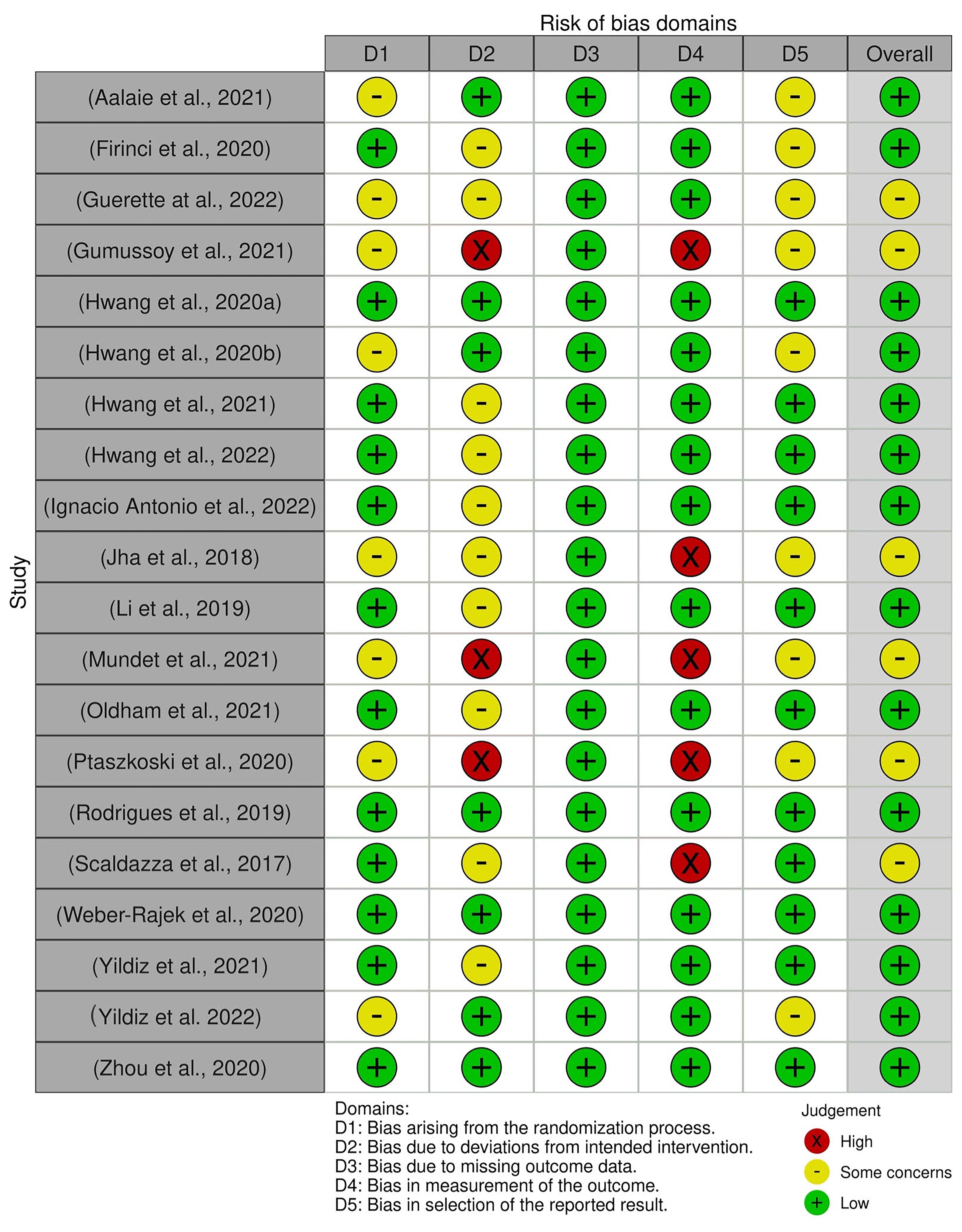 Fig. 2.
Fig. 2.
Risk of Bias Assessment for included randomized controlled trials (RCTs) in the review.
All but one study included only female participants (n = 36; see Table 2). Additionally, the majority of studies included participants in perimenopause or menopause (n = 34). Only four studies used EMS interventions for women in the postpartum period. Eleven studies specifically focused on females with SUI (Table 2). Six other studies included females with any type of UI. Two studies included people living with POP. People living with fecal incontinence (FI) were included in five studies. Five studies focused on overactive bladder (OAB) patients while the remaining seven studies included participants living with any lower urinary tract symptoms (LUTS), FI and/or sexual dysfunction (e.g., dyspareunia). Most studies used outcomes measures that captured PFDs outside of the condition that was used for study recruitment. As such PFDs was determined to encompass a variety of systems and conditions across studies beyond that of the diagnosis used as part of the primary inclusion, highlighting the multifaceted nature of PFD.
The majority of studies used traditional intra-vaginal or intra-rectal probes as
the mode of EMS induction (n = 20; see Table 2). As for as more novel versions of
EMS, N = 15 studies used tools that applied EMS externally. Of these, N = 11 used
high frequency electromagnetic stimulation (HIFEM), with N = 6 via the Emsella
(
For the twenty included studies that used intra-vaginal/ rectal stimulation, three used the PHENIX (20–80 Hz), Enraf Nonius (10 Hz), and UroStym (20 Hz) devices. The MyoPlus4 (20 Hz), Pelviva (2–125 Hz), MAPle Probe (35 Hz), Elpha 3000 (35 Hz), BrioBravo (10 Hz) and MyoMed (40 Hz) were also used. Several studies did not specify the devices used (Table 2).
A total of 19 studies used high-frequency stimulation (
Although the existing literature base has been clear with respect to the benefit
of using traditional low-intensity intervaginal EMS to improve outcomes among
women with PFD, insight related to more novel forms of EMS, particularly those
that are higher intensity and are applied externally is limited. Therefore, in
this review we scoped, summarized and critically evaluated the available research
investigating the impact of all current forms of EMS on PFDs in females. A large
proportion of the reviewed studies pertained to the use of traditional low
intensity (
The next most common form of EMS studied, used high frequency (
In considering what might improve the efficacy of Emsella, over other forms of EMS, we note that Emsella uses a frequency of energy significantly higher than other HIFEM tools [59]. Further, when considering the potential benefit of all HIFEM tools, given the shorter intervention times, what needs to be considered is the pulsed electromagnetic component of energy that is incorporated into these therapies. Interestingly, all studies using HIFEM referred to the mechanism of action being related to strengthening of the pelvic floor. It is established the EMS is an effective rehabilitation strategy for muscle hypertrophy development and that positive muscle adaptions occur even with low intensity and low frequency applications [60]. However, a cited difference with respect HIFEM is that it induces electrical currents selectively in the PFM by mechanism of electromagnetic induction [61]. As magnetic field passes any medium without attenuation of the energy, the induced contractions may be achieved at greater depths and intensities [62] to possibly provide better outcomes. In addition, beneficial immune system mechanisms have been established with the use of pulsed electromagnetic frequency and such mechanisms should be further explored with respect HIFEM as a tool to assist with PFDs [63]. The mechanism of Pulsed Electromagnetic Fields (PEMFs), for example, is known to regulate cell proliferation, immune modulation, and inflammation responses through a variety of underlying molecular mechanisms with strong anti-inflammatory effects [64].
In the present review, only research examining EMS tools were examined; therefore, interventions examining magnetic stimulation in isolation were excluded. However, evidence from a systematic review and meta-analysis of 17 RCTs indicates that magnetic stimulation is effective in the treatment of urinary incontinence and improves quality of life in people living with SUI (i.e., extracorporeal magnetic stimulation) [65, 66]. In the meta-analysis, significant improvements were noted on assessment measures of quality of life, number of daily pads used, and number of incontinence events [65]. Research suggests that the pulsed electromagnetic fields can penetrate pelvic floor muscles and strengthen them by stimulating pelvic floor nerves to contract [66, 67]. The mechanism of action warrants further investigation, comparing extra- and intra-vaginal, low and high-intensity and magnetic and non-magnetic EMS modalities. A recent scoping review examining the mechanism of action of EMS suggests that an anti-inflammatory response is at least partially responsible for the positive outcomes observed after EMS [68] which may contradict previously held beliefs about the impact of EMS on pelvic floor muscle tone.
Four studies, all of which were RCTs and determined to be low risk of bias, studied a novel tool called EasyK7. Like the HIFEM tools, the EasyK7 administers energy externally vs. intravaginally. However, unlike HIFEM, this tool uses low frequency EMS (25 Hz) and does not have an additional magnetic stimulation component; despite this, all four studies demonstrated significant improvement across all outcomes with the use of EasyK7. It should be noted that the same participant group is used for all studies and thus further study of such a form of EMS is needed.
Due to the heterogeneity of the types of EMS used, protocols and outcomes measures used, which included a range of physical and self-report measures, it was not possible pool the data. It is not known, based on the information available from the included studies, why certain treatment protocols were used in the included studies. It is suspected that manufacturer recommendations were used in the included studies, rather than observing treatment effects throughout the duration of exposure to EMS. Moreover, it is not known how any benefit of EMS is maintained over time or how the benefit of EMS interacts with other aspects of clinical care beyond the scope of the trials included, which did often include EMS within the context of other PFM rehabilitation strategies.
The findings of the present review are also positive for individuals whose care preference does not include intravaginal or intrarectal care. The lack of acceptance of intervaginal care spans the landscape of PFDs and lumbopelvic pain [69]. Further, EMS may be particularly useful in women living with SUI or who are unable to perform voluntary muscle contractions: some research suggest this exceeds 50% of females [17, 18]. Extra-vaginal EMS devices tend to be more costly when compared to intra-vaginal devices intended for a person’s use at home and, as such, a variety of feasibility and acceptability factors beyond the scope of this review are likely important to consider when providing individualized care. It is also unclear if participants in the included research studies were paying for the EMS treatments they received. It must be considered that the duration of treatments may have been dependent on what was determined as a feasible cost, rather than an established protocol. However, high intensity, extra-vaginal EMS modalities, especially those like HIFEM with a magnetic component, do have higher costs and therefore may not present as a feasible treatment option for all people living with PFDs.
Future large-scale high-quality research interventions are required in order to determine the clinical utility of different EMS protocols, particularly novel HIFEM protocols. Ongoing research should be conducted to standardize protocols for better clinical implementation of EMS modalities for the treatment of PFDs in both females and males.
Although this scoping review provides valuable insight related to the current landscape of EMS tools to support PFD, the current state of the science did not allow for the needed analysis to optimally guide clinical reasoning. The included studies did not address the magnitude of benefits to included participants, patients’ preferences when it comes to the use of EMS, or tolerability of the modalities. In fact, a wide variety of assessment and outcome measures were used in the studies included in this review, making it difficult to determine the clinical significance of EMS on these outcomes. Given rise in popularity of HIFEM technologies, and the associated large claims made by manufactures, further clarity on the use of these tools and the validity of these claims is needed. Currently six trails investigating HIFM forms of EMS are registered on https://ClinicalTrials.gov. Thus, conducting a systematic review and associated meta-analysis specifically on HIFEM when more studies are pushed is an important next step to guide practice. We note several of the studies included have low quality of evidence and high risk of bias. Such limitations are all recorded within Table 2.
EMS demonstrates improvement across outcomes for PFDs among adult women. In particular, the results of this review suggest that EMS may be particularly useful in women living with SUI or who those are unable to perform voluntary muscle contractions when pelvic floor muscle training is attempted. Novel forms of EMS that used HIFEM appear to require less time to achieve therapeutic effects when compared to low-intensity modalities and furthermore might be preferable due to the external application of EMS. However, more RCTs and associated heterogeneity across studies is needed to generalizes the findings of the studies included in this review.
The data that support the findings of this study are openly available and are identified in the reference list of this review paper. The authors confirm that the data supporting the findings of this study are available within the articles referenced in this work and/or their supplementary materials.
NG and SD co-led this work and established the aim and methods. PA performed the initial literature search together with a medical librarian (McMaster University). PA, CD, HA and KK carried out abstract and full article screening as well as data extraction. NG carried out the analysis, quality assessments, and drafted the manuscript. HA conducted the risk of bias assessments. SD, PA, CD and KK all assisted with manuscript revisions with SD taking a lead role. All authors contributed to editorial changes in the manuscript. All authors read and approved the final manuscript. All authors have participated sufficiently in the work and agreed to be accountable for all aspects of the work.
Not applicable.
We would like to thank Dr. Luciana Macedo (McMaster University) for consulting with our team and assisting us with aspects of the methods and registering our protocol.
This research received no external funding.
The authors declare no conflict of interest. The WOMB Milton, Knew Life Physiotherapy, and Oakville Pelvic Health were not involved in the preparation and publication of the manuscript.
Supplementary material associated with this article can be found, in the online version, at https://doi.org/10.31083/j.ceog5111257.
References
Publisher’s Note: IMR Press stays neutral with regard to jurisdictional claims in published maps and institutional affiliations.


