1 Department of Urology, The First Affiliated Hospital of Nanchang University, 330006 Nanchang, Jiangxi, China
2 Department of Breast Surgery, Jiangxi Cancer Hospital of Nanchang University, 330029 Nanchang, Jiangxi, China
3 Department of Nursing, Nanchang Medical College, 330052 Nanchang, Jiangxi, China
Abstract
Background: The population of older women (
Keywords
- SEER database
- chemotherapy
- breast cancer-specific death
- older patient
- TNBC
- competing risk
Breast cancer is the most prevalent malignancy in women worldwide. The incidence
and mortality of breast cancer increases with age [1]. Triple-negative breast
cancer (TNBC), makes up 12–18% of breast cancer patients [2], is a type of
breast cancer that lacks the expression of the estrogen receptor (ER),
progesterone receptor (PR), and human epidermal growth factor receptor-2 (HER2)
[3, 4, 5]. TNBC is more likely to recur and metastasize than type of luminal or HER2
positive, and it has relatively a lower survival rate [6]. Due to the lack of
definitive targets, novel therapeutic interventions were limited, and
chemotherapy remains the primary treatment [7]. With the aging of the population,
older women with TNBC will also be increasing. However, data on TNBC treatment,
including chemotherapy, in older patients (
Older breast cancer patients frequently had one or more concomitant illnesses at
the time of diagnosis because of the patient’s own factors (e.g., heart
disease, chronic obstructive pulmonary disease, diabetes, hypertension, and
arthritis) [8]. The mortality rate of breast cancer in older women was relatively
high due to numerous reasons such as inadequate treatment and the presence of
multiple comorbidities [9]. In daily clinical practice, the presence of
comorbidities often reduces available treatments and increases their likelihood
of dying from non-breast cancer causes [8]. Chemotherapy was recommended by many
authoritative guidelines for patients with TNBC [10, 11]. However, the guidelines
did not provide specific treatment recommendations for older patients with TNBC.
There haven’t been any significant randomized studies on the advantages of
chemotherapy for older patients (
In this study, we collected a large cohort of patients from the Surveillance,
Epidemiology, and End Results (SEER) database, and conducted a competing risk
analysis in the study for TNBC patients (
The SEER 18 registries’ research data from 1975 to 2019 were available in the
SEER database’s current version (https://seer.cancer.gov). For analysis,
we received authorization to use study data from November 2021 (Reference number:
11078-Nov2021). SEER*Stat software (Version 8.4.0.1, National Institutes of
Health, Bethesda, Rockville, MA, USA) was used to collect all data on TNBC
patients (
Patients who met the following criteria were included: (1) diagnosed with TNBC
between 2010 and 2019 (candidates in this study were included between 2010 and
2019 since HER2 status was only reported in SEER data after 2010); (2) with
primary cancer; (3) aged 70 years and over, and (4) diagnosed as M0 stage. Then,
patients who met the following requirements were disqualified: (1) unknown or no
surgery information; (2) survival time
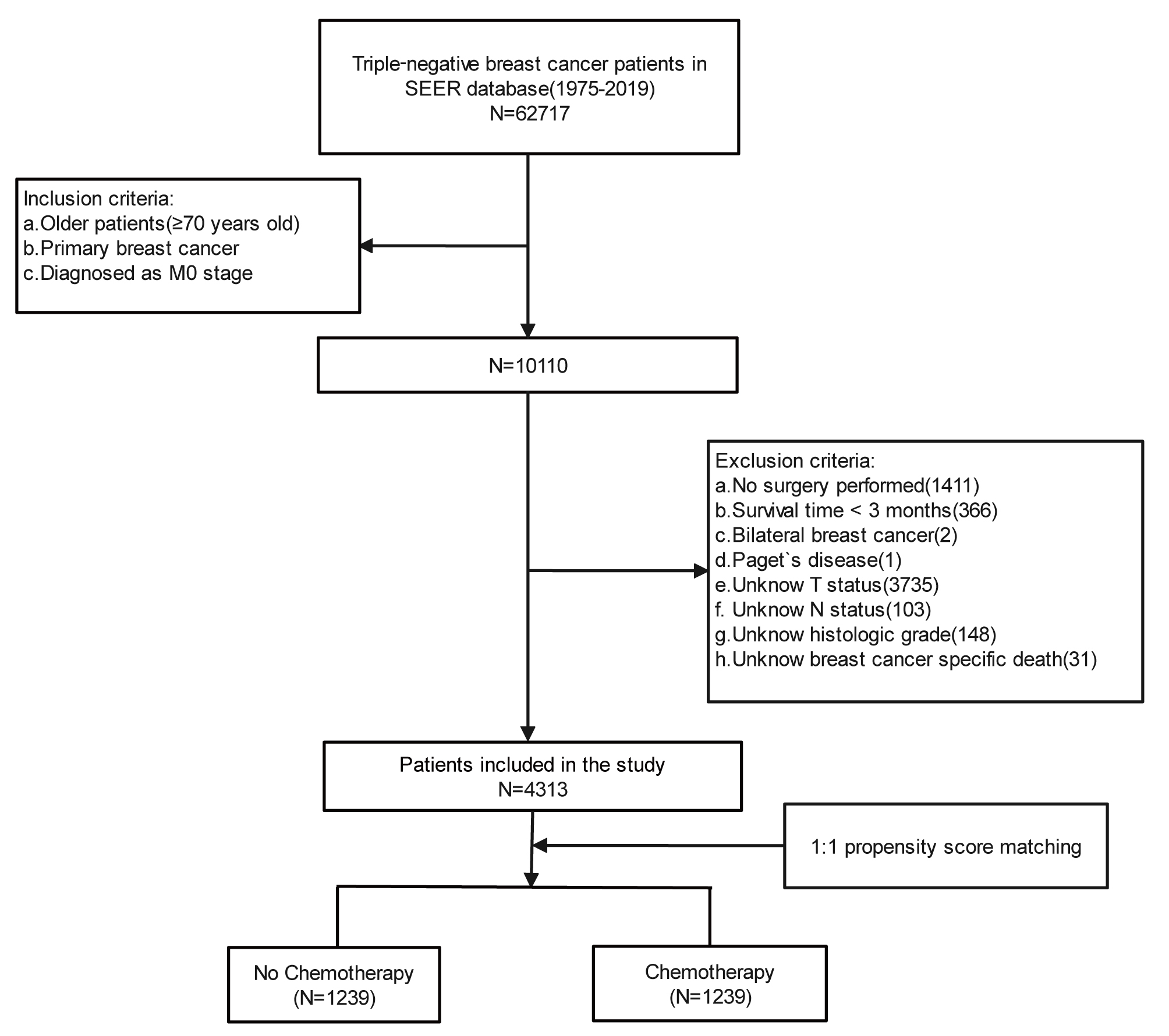 Fig. 1.
Fig. 1.The flowchart of the included population in this study.
In this investigation, the following information was gathered for each patient: patient id, age, sex, race recode (white, black, other), marital status at diagnosis, year of diagnosis, laterality, ICD-O-3 Hist/behave, surgery information, radiation recode, chemotherapy recode, AJCC (American Joint Committee on Cancer) T status, AJCC N status, AJCC M status, TNM (tumor node metastasis) status, grade, sequence number, SEER cause-specific death classification, SEER other cause of death classification and survival months. Age was classified as 70–79; 80–89, 90–99 and 100+ years. Race was classified as white, black and others. Marital status was classified as single and married. Tumor laterality was classified as left and right. Histologic grade was classified as grade I, II, III and IV. Histologic type was classified as infiltrating lobular carcinoma, infiltrating duct carcinoma and other type of carcinoma. AJCC T status was classified as T0, T1, T2, T3 and T4. AJCC N status was classified as N0, N1, N2 and N3. AJCC TNM stage was classified as stage I, II and III. Surgical treatment was classified as mastectomy and partial mastectomy. Radiotherapy and chemotherapy were classified as receiving or not. Causes of death were categorized as breast cancer-specific death (BCSD) or other cause-specific death (OCSD).
Causes of patient death included BCSD and OCSD. The OCSD was considered as a competing event. The survival time was from the date of diagnosis of breast cancer to the date of death or to the date of last follow-up.
Propensity score matching (PSM) was subsequently done with 1:1 nearest neighbor
method without replacement. Balance of propensity-matched groups was assessed and
confirmed with mean standardized differences, with absolute values greater than
0.1 being considered unacceptably imbalanced. Survival curves were produced by
the Kaplan-Meier method, and the log-rank test was used to compare the overall
survival rates between two groups. The “cmprsk” package in R statistical software
(Version 4.1.3, the Vienna University of Economics and Business, Vienna, Austria)
was used for statistical analysis [15]. The mortality rates between groups were
analyzed using the cumulative incidence function, and differences between groups
were analyzed using Gray’s test. The variables with p value less
than 0.1 in the univariate analysis were incorporated into the multivariate
analysis. The partial proportional risk regression model was performed using the
“crr” function. R statistics software 4.1.3 was used to perform all statistical
analyses. All statistical tests were two-sided, and the level of significance was
set at p
Patients were followed up until November 2019, and the median follow-up time was
61 months (ranging from 3 to 119 months). Fig. 1 depicted the process of
including participants from the SEER database. We initially acquired 10,110 TNBC
patients (
| Characteristics | Before PSM | After PSM | |||||
|---|---|---|---|---|---|---|---|
| No Chemotherapy | Chemotherapy | p value | No Chemotherapy | Chemotherapy | p value | ||
| Total | n = 2452 (56.9) | n = 1861 (43.1) | n = 1239 (50) | n = 1239 (50) | |||
| Age (years) | 0.751 | ||||||
| 70–79 | 1215 (49.6) | 1608 (86.4) | 982 (79.3) | 991 (80.0) | |||
| 80–89 | 1045 (42.6) | 245 (13.2) | 251 (20.3) | 240 (19.4) | |||
| 90–99 | 189 (7.7) | 8 (0.4) | 6 (0.5) | 8 (0.6) | |||
| 100+ | 3 (0.1) | 0 (0.0) | |||||
| Race | 0.689 | 0.180 | |||||
| Black | 336 (13.7) | 272 (14.6) | 189 (15.3) | 187 (15.1) | |||
| Other | 177 (7.2) | 131 (7.0) | 79 (6.4) | 103 (8.3) | |||
| White | 1939 (79.1) | 1458 (78.3) | 971 (78.4) | 949 (76.6) | |||
| Marital | 0.223 | ||||||
| Married | 858 (35.0) | 920 (49.4) | 546 (44.1) | 515 (41.6) | |||
| Single | 1594 (65.0) | 941 (50.6) | 693 (55.9) | 724 (58.4) | |||
| Histologic grade | 0.127 | ||||||
| I | 113 (4.6) | 27 (1.5) | 21 (1.7) | 27 (2.2) | |||
| II | 655 (26.7) | 355 (19.1) | 258 (20.8) | 301 (24.3) | |||
| III | 1666 (67.9) | 1463 (78.6) | 953 (76.9) | 902 (72.8) | |||
| IV | 18 (0.7) | 16 (0.9) | 7 (0.6) | 9 (0.7) | |||
| Laterality | 0.968 | 0.006 | |||||
| Left | 1286 (52.4) | 974 (52.3) | 634 (51.2) | 703 (56.7) | |||
| Right | 1166 (47.6) | 887 (47.7) | 605 (48.8) | 536 (43.3) | |||
| Histologic | 0.112 | 0.260 | |||||
| Infiltrating Lobular carcinoma | 45 (1.8) | 32 (1.7) | 16 (1.3) | 26 (2.1) | |||
| Infiltrating duct carcinoma | 1992 (81.2) | 1557 (83.7) | 1023 (82.6) | 1024 (82.6) | |||
| Other type of carcinoma | 415 (16.9) | 272 (14.6) | 200 (16.1) | 189 (15.3) | |||
| T status | 0.456 | ||||||
| T0 | 0 (0.0) | 3 (0.2) | |||||
| T1 | 1376 (56.1) | 798 (42.9) | 667 (53.8) | 649 (52.4) | |||
| T2 | 837 (34.1) | 824 (44.3) | 456 (36.8) | 450 (36.3) | |||
| T3 | 159 (6.5) | 125 (6.7) | 66 (5.3) | 82 (6.6) | |||
| T4 | 80 (3.3) | 111 (6.0) | 50 (4.0) | 58 (4.7) | |||
| N status | 0.226 | ||||||
| N0 | 1985 (81.0) | 1134 (60.9) | 948 (76.5) | 903 (72.9) | |||
| N1 | 302 (12.3) | 461 (24.8) | 187 (15.1) | 215 (17.4) | |||
| N2 | 92 (3.8) | 167 (9.0) | 60 (4.8) | 71 (5.7) | |||
| N3 | 73 (3.0) | 99 (5.3) | 44 (3.6) | 50 (4.0) | |||
| TNM status | 0.048 | ||||||
| I | 1264 (51.5) | 618 (33.2) | 599 (48.3) | 546 (44.1) | |||
| II | 936 (38.2) | 866 (46.5) | 487 (39.3) | 507 (40.9) | |||
| III | 252 (10.3) | 377 (20.3) | 153 (12.3) | 186 (15.0) | |||
| Surgery | 0.061 | 0.123 | |||||
| Mastectomy | 1132 (46.2) | 805 (43.3) | 514 (41.5) | 553 (44.6) | |||
| Partial mastectomy | 1320 (53.8) | 1056 (56.7) | 725 (58.5) | 686 (55.4) | |||
| Radiotherapy | 0.243 | ||||||
| No | 1499 (61.1) | 816 (43.8) | 649 (52.4) | 679 (54.8) | |||
| Yes | 953 (38.9) | 1045 (56.2) | 590 (47.6) | 560 (45.2) | |||
TNBC, triple-negative breast cancer; SEER, the Surveillance, Epidemiology, and End Results; TNM, tumor node metastasis; PSM, propensity score matching.
By propensity score matching, 1239 patients undergoing chemotherapy were matched
against 1239 patients who did not receive chemotherapy. The survival analysis
showed that patients who received chemotherapy had a better prognosis than those
who did not received chemotherapy (HR (hazard ratio) 0.72; 95% CI (confidence interval) 0.63–0.82;
p
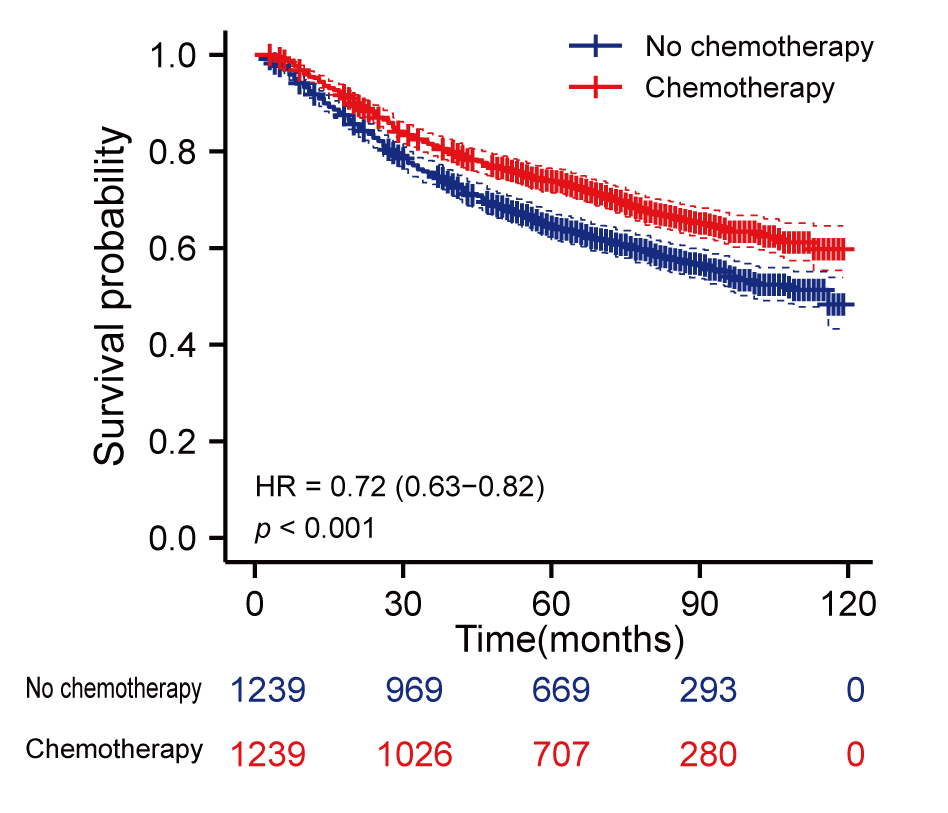 Fig. 2.
Fig. 2.Kaplan-Meier curves for overall survival in old patients
(
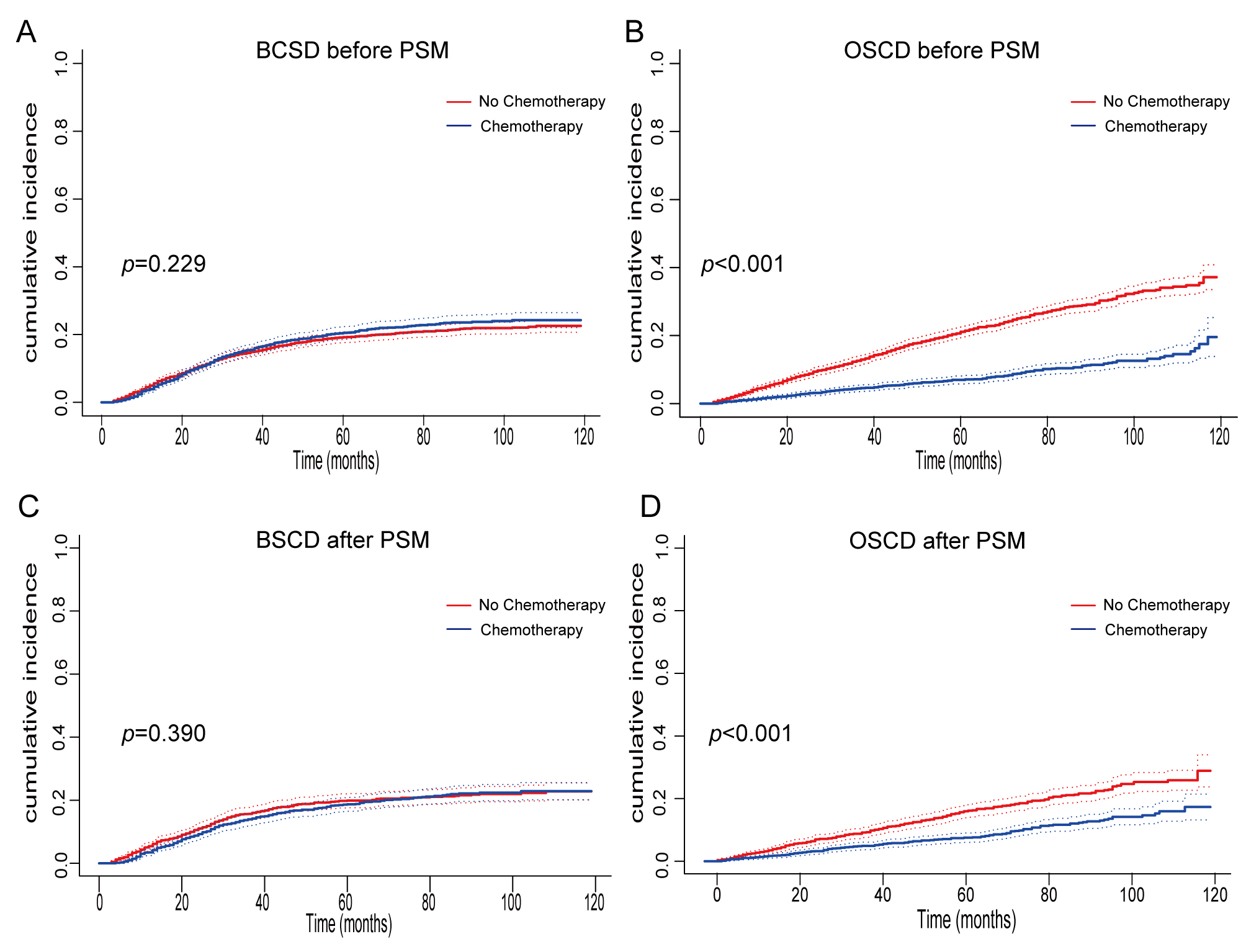 Fig. 3.
Fig. 3.Cumulative incidence function analysis of old patients
(
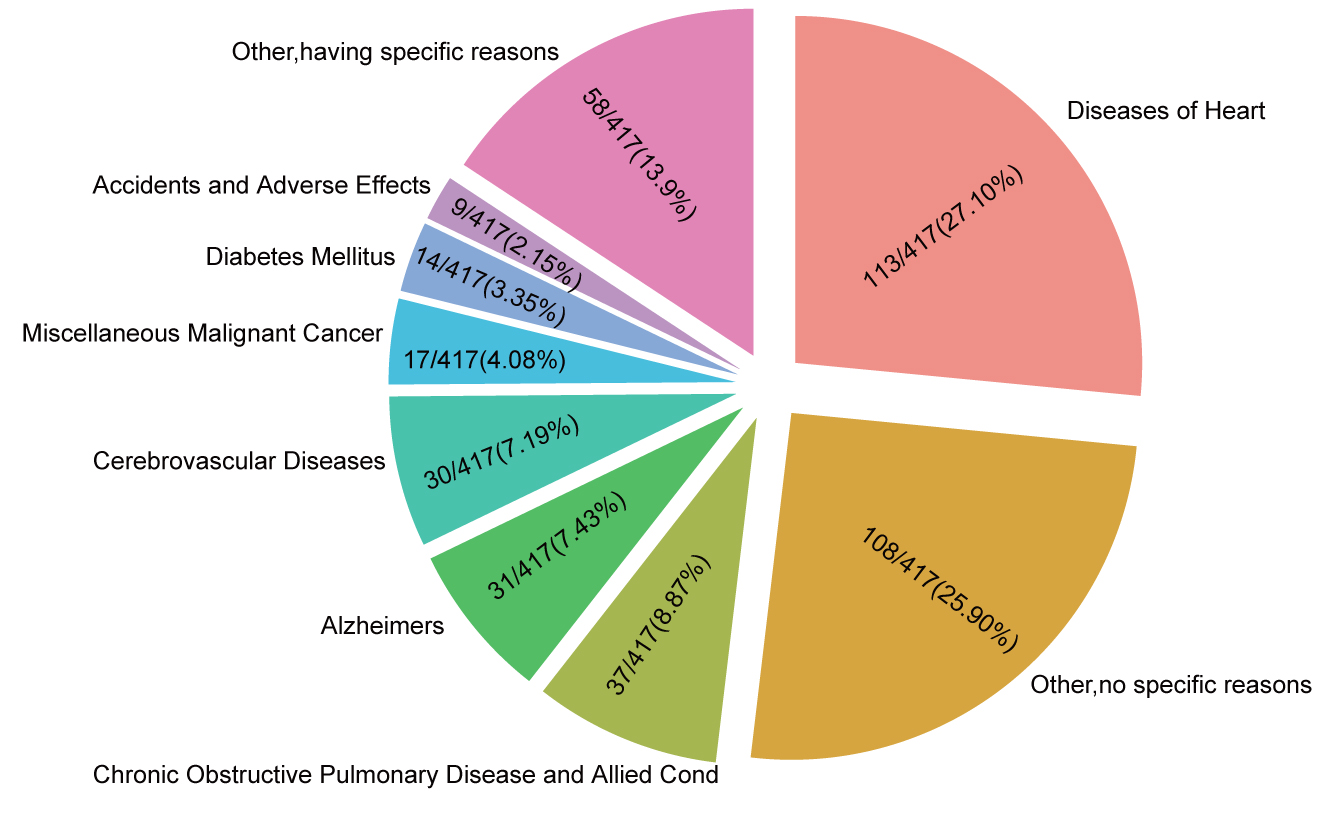 Fig. 4.
Fig. 4.The OCSD classification in older patients (
During the follow-up period, there were 512 patients died from breast cancer and 386 patients died from other causes. Accordingly, Table 2 showed the cumulative occurrences of BCSD and OCSD during 3-, 5-, and 8-year periods grouped by different clinical factors. Across the three, five, and eight-year periods, the overall mortality rate for breast-related causes was 15.34%, 20.30% and 23.73%, respectively. A higher cumulative incidence was observed in those patients who were 80–89 years of age, married, black, in grade IV, with advanced T and N statuses, underwent mastectomy, and did not receive radiotherapy. Statistics showed that tumor location, histologic type, and receiving chemotherapy had no impact on BCSD outcomes. Meanwhile, the 3-year, 5-year and 8-year other cause-specific mortalities were 7.36%, 13.20% and 23.02%. Patients with older ages (80–89), single status, advanced grades, advanced T status, advanced N status, mastectomy and patients did not receive radiotherapy and chemotherapy for OCSD were associated with higher cumulative incidences of OCSD. In the cumulative incidence function (CIF) of OCSD, no statistically significant differences were seen for race, laterality, or histologic type.
| Characteristics | BCSD | OCSD | |||||||||||
|---|---|---|---|---|---|---|---|---|---|---|---|---|---|
| Event | % | 3 years (%) | 5 years (%) | 8 years (%) | p value | Event | % | 3 years (%) | 5 years (%) | 8 years (%) | p value | ||
| Total | 512 | 100.00 | 15.34 | 20.30 | 23.73 | 386 | 100.00 | 7.36 | 13.20 | 23.02 | |||
| Age (years) | 0.00 | ||||||||||||
| 70–79 | 335 | 65.43 | 11.91 | 16.22 | 19.45 | 255 | 66.06 | 5.87 | 10.51 | 18.39 | |||
| 80–89 | 167 | 32.62 | 28.41 | 36.37 | 40.64 | 128 | 33.16 | 13.72 | 25.95 | 45.17 | |||
| 90–99 | 10 | 1.95 | 69.39 | 79.59 | NA | 3 | 0.78 | 20.00 | 20.00 | NA | |||
| Race | 0.034 | 0.055 | |||||||||||
| Black | 94 | 18.36 | 17.10 | 24.84 | 29.88 | 63 | 16.32 | 8.39 | 12.73 | 24.75 | |||
| White | 389 | 75.98 | 15.12 | 19.82 | 23.22 | 305 | 79.02 | 7.48 | 13.72 | 23.43 | |||
| Other | 29 | 5.66 | 14.08 | 16.08 | 16.97 | 18 | 4.66 | 3.96 | 8.43 | 15.31 | |||
| Marital | 0.001 | 0.003 | |||||||||||
| Married | 190 | 37.11 | 12.58 | 16.91 | 20.82 | 145 | 37.56 | 6.27 | 11.21 | 20.00 | |||
| Single | 322 | 62.89 | 17.42 | 22.87 | 25.91 | 241 | 62.44 | 8.21 | 14.78 | 25.44 | |||
| Grade | 0.002 | ||||||||||||
| I | 1 | 0.20 | 2.08 | 2.08 | 2.08 | 5 | 1.30 | 0.00 | 4.56 | 23.71 | |||
| II | 89 | 17.38 | 11.09 | 15.08 | 17.73 | 67 | 17.36 | 4.97 | 9.74 | 17.32 | |||
| III | 415 | 81.05 | 16.79 | 22.19 | 26.01 | 313 | 81.09 | 8.31 | 14.57 | 24.96 | |||
| IV | 7 | 1.37 | 40.74 | 48.15 | 48.15 | 1 | 0.26 | 10.00 | 10.00 | 10.00 | |||
| Laterality | 0.441 | 0.999 | |||||||||||
| Left | 268 | 52.34 | 15.02 | 19.90 | 22.99 | 209 | 54.15 | 7.69 | 13.44 | 23.27 | |||
| Right | 244 | 47.66 | 15.71 | 20.77 | 24.61 | 177 | 45.85 | 6.98 | 12.93 | 22.73 | |||
| Histologic | 0.183 | 0.148 | |||||||||||
| Infiltrating lobular carcinoma | 428 | 83.59 | 22.88 | 28.94 | 36.89 | 2 | 0.52 | 2.78 | 6.13 | 6.13 | |||
| Infiltrating duct carcinoma | 13 | 2.54 | 15.21 | 20.25 | 24.18 | 319 | 82.64 | 7.34 | 13.09 | 22.68 | |||
| Other type of carcinoma | 71 | 13.87 | 15.25 | 19.65 | 19.65 | 65 | 16.84 | 7.95 | 14.54 | 26.36 | |||
| T status | |||||||||||||
| T1 | 138 | 26.95 | 6.58 | 10.01 | 12.02 | 160 | 41.45 | 4.20 | 8.78 | 17.46 | |||
| T2 | 255 | 49.80 | 21.03 | 27.91 | 33.36 | 171 | 44.30 | 10.05 | 17.39 | 28.67 | |||
| T3 | 64 | 12.50 | 41.09 | 46.97 | 50.56 | 29 | 7.51 | 15.51 | 23.88 | 36.58 | |||
| T4 | 55 | 10.74 | 44.95 | 53.56 | 60.27 | 26 | 6.74 | 18.19 | 30.68 | 46.24 | |||
| N status | |||||||||||||
| N0 | 242 | 47.27 | 8.63 | 12.44 | 15.29 | 256 | 66.32 | 5.66 | 10.44 | 19.84 | |||
| N1 | 142 | 27.73 | 28.47 | 35.18 | 41.41 | 82 | 21.24 | 12.09 | 21.62 | 30.73 | |||
| N2 | 67 | 13.09 | 43.78 | 56.09 | 60.71 | 30 | 7.77 | 14.26 | 28.53 | 47.26 | |||
| N3 | 61 | 11.91 | 57.77 | 71.98 | 74.32 | 18 | 4.66 | 16.50 | 28.28 | 51.32 | |||
| Surgery | 0.001 | ||||||||||||
| Mastectomy | 304 | 59.38 | 21.63 | 28.58 | 32.97 | 186 | 48.19 | 9.54 | 16.15 | 26.96 | |||
| Partial mastectomy | 208 | 40.63 | 10.68 | 14.18 | 16.87 | 200 | 51.81 | 5.81 | 11.16 | 20.31 | |||
| Radiotherapy | 0.001 | ||||||||||||
| No | 309 | 60.35 | 17.50 | 23.12 | 27.03 | 230 | 59.59 | 8.84 | 15.33 | 26.35 | |||
| Yes | 203 | 39.65 | 12.88 | 17.13 | 20.02 | 156 | 40.41 | 5.70 | 10.85 | 19.40 | |||
| Chemotherapy | 0.390 | ||||||||||||
| No | 260 | 50.78 | 16.41 | 21.24 | 23.92 | 253 | 65.54 | 9.57 | 18.11 | 28.77 | |||
| Yes | 252 | 49.22 | 14.28 | 19.38 | 23.57 | 133 | 34.46 | 5.19 | 8.33 | 17.02 | |||
TNBC, triple-negative breast cancer; BCSD, breast cancer-specific death; OCSD, other cause-specific death.
After the univariate analysis of CIF, the Fine and Gray method was used to
perform multivariate analysis of BCSD and OCSD in older TNBC patients. BCSD had
been found to be associated with age at diagnosis, race, tumor grade, T status, N
status, and having received radiotherapy. The results of our study showed that,
for older TNBC patients, subjects of 80–89 years and 90–99 years had worse BCSD
(80–89 vs. 70–79: SHR (subdistribution hazard ratio) 1.240; 95% CI
1.004–1.532, p = 0.046; 90–99 vs. 70–79: SHR 2.462; 95% CI
1.290–4.697, p = 0.006). Moreover, race black, compared with patients
with other race (expect for race white) had worse BCSD (Black vs. other:
SHR 1.590; 95% CI 1.021–2.476, p = 0.040). Compared to patients with
grade I, those with higher grades had worse BCSD (IV vs. I :
SHR 14.832; 95% CI 1.700–129.381, p = 0.015). Furthermore, patients
with advanced T stages were more likely to develop BCSD compared to those with T1
stages (T2 vs. T1: SHR 2.066; 95% CI 1.648–2.589, p
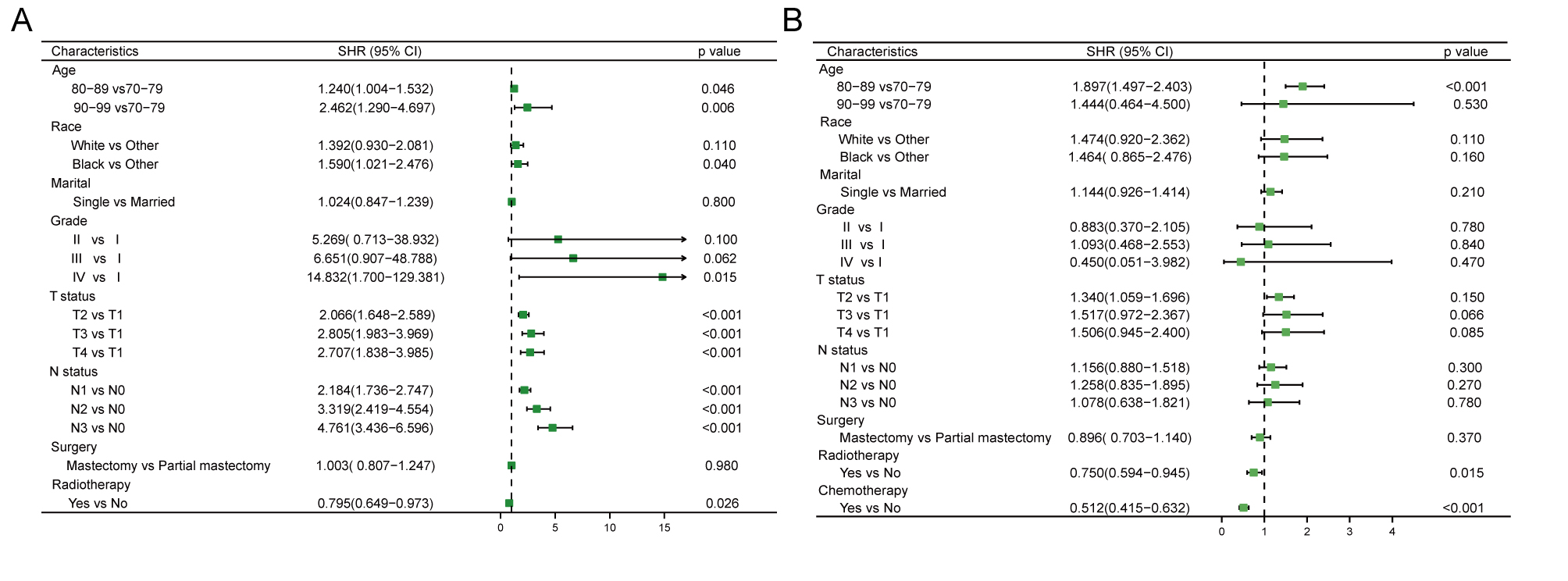 Fig. 5.
Fig. 5.Forest plot showed prognostic factors for BCSD (A) and OCSD (B) in older TNBC patients by the Fine and Gray model. BCSD, breast cancer-specific death; OCSD, other cause-specific death.
In this study, the main objective was to examine how chemotherapy affected BCSD
and OCSD in older TNBC women (
Because chemotherapy-induced toxicity was more severe and the advantages were less favorable than younger patients, the benefit-risk balance in clinical practice for elderly patients was difficult [17]. Therefore, the choice of chemotherapy for the elderly needs to be more cautious. Many randomized controlled trials had shown that adjuvant systemic chemotherapy improves overall patient survival in younger patients with TNBC [18, 19, 20]. Unfortunately, the number of patients older than 70 was small in these randomized controlled trials [21, 22, 23], so the results of these trials were not as convincing in guiding the value of chemotherapy in older women with TNBC. There had been some previous small retrospective analyses of the treatment of older breast cancers, most commonly assessing women aged 60–65 years and older. In a SEER database analysis with a small percentage of older patients, the use of chemotherapy was not linked to better survival in the elderly [24]. However, these studies had tended to examine the effect of chemotherapy on overall survival using ER-negative patients as a subgroup [25, 26]. Without exception, none of these studies made a specific distinction between the endpoint death events as BCSD or OCSD. Next, in Table 2 and Fig. 5, the univariate CIF and multivariate Fine and Gray competitive risk analysis method were used to select the independent prognostic factors of BCSD and OCSD in older TNBC patients. Firstly, patients of 80–89 years were found to have a higher risk of OCSD. Advanced age implied a significant decline in physical function [27]. Thus, advanced age was the most significant factor affecting OCSD. Our study, which was consistent with earlier studies [28], discovered that racial disparity played a significant effect in the survival prognosis of BCSD for older TNBC patients. It was an important reason that black people had greater rates of triple-negative breast cancer than white [29]. The result of competitive risk analysis suggested that grade, T status and N status were more correlated with BCSD, which was consistent with another research [30]. Surgery was still the primary treatment for breast cancer. Because the patients who participated in our study had surgery, it was not possible to assess BCSD and OCSD in patients who had surgery versus those who did not. However, our study found that the risk of BCSD or OCSD was not influenced by the type of surgery. In our study, radiotherapy and chemotherapy both had an impact on the OCSD, and radiotherapy also had an impact on the BCSD.
In this study, with a median follow-up time of 61 months follow-up, a total of 898 older breast cancer patients died. Of these, 386 patients (43.0%) died from other causes except breast cancer. Among them, diseases of heart, chronic obstructive pulmonary disease and Alzheimer were three common non-breast cancer causes of death in the elderly TNBC patients (Fig. 4). There was a risk of developing various chronic diseases for older patients, such as heart disease or lung disease, before and after the diagnosis of breast cancer. All of these diseases could be important causes of death in breast cancer patients. Actually, age was no longer the main factor determining the best treatment plan for breast cancer patients, and functional level and comorbidities must also be taken into account [31]. One study showed that 2% to 10% of breast cancer patients died from CVD (cardiovascular disease), especially if the patient had risk factors for CVD themselves, their risk of CVD death would be higher [32]. In addition, the death risk of CVD in breast cancer patients may also be increased by the cardiotoxic effects of treatment, such as receiving radiotherapy and chemotherapy. Therefore, it was very important to know the risk of CVD in breast cancer patients, especially if one treatment might be cardiotoxic.
Due to the special characteristics of elderly patients, another issue to consider was the impact of chemotherapy on quality of life. In clinical work, the choice of chemotherapy for an elderly patient with TNBC who has multiple chronic conditions might be a tricky situation for both the physician and the patient. Chemotherapy had the potential to aggravate pre-existing disease in patients. In older breast cancer patients, chemo-endocrine therapy resulted in net reductions in quality-adjusted life years (QALYs) for all 75 years and older. As treatment effectiveness improve, chemotherapy had greater benefits, but at the same time, the toxicity of chemotherapy reduces patients’ QALYs [33]. However, the difference between the two groups largely disappeared at about 12 months. The study also suggested that these transient changes in QoL (quality of life) were a modest contribution to improved survival [34]. Some specialists advised to add chemotherapy for some people with high-risk characteristics and anticipated life expectancies longer than five years [35]. Therefore, when choosing a chemotherapy protocol, in addition to the benefit of chemotherapy, the side effects of chemotherapy and the length of survival of the patient need to be considered.
In this study, chemotherapy induced reduction of OCSD, not BCSD, of patients with TNBC. This result was similar to the study of Schonberg et al. [36] that chemotherapy could significantly improve the non-breast cancer survival among all women (adjusted hazard ratio [aHR], 0.6; range, 0.4 to 0.8). We analyzed some reasons for this. Firstly, elderly patients had numerous underlying diseases, and death from underlying diseases often preceded death from breast cancer. The study of Ferrigni et al. [37] found the main cause of death was often due to other causes besides breast cancer (20% due to other causes, 14% due to unknown causes), with only 6 patients (5%) dying from causes related to their breast cancer. Studies by Colzani et al. [38] and Cyr A et al. [39] also showed that older breast cancer patients were unlikely to suffer breast cancer-related mortality. Hence, causes other than breast cancer become more important as causes of death in the oldest old patients [38, 39]. Therefore, OSCD was more likely to occur than BSCD. Secondly, due to limitations in access to the SEER database, we did not have access to the underlying disease and severity of the patient at the time of breast cancer diagnosis. This result would be more plausible if patients with underlying disease could be put through PSM between the chemotherapy and no-chemotherapy groups. Thirdly, chemotherapy was the recommended regimen for the adjuvant treatment of TNBC. Many elderly TNBC patients did not receive chemotherapy due to a variety of factors. Patients who received chemotherapy might have a higher awareness of diseases (including cancer and other underlying diseases) compared to those who did not receive chemotherapy. Although chemotherapy drugs (such as paclitaxel) commonly used for breast cancer had side effects in older patients, the common side effects had little impact on patient survival [40, 41, 42]. The difference in awareness may lead to older patients who receive chemotherapy being more receptive to treatment for other underlying diseases. This might be one of the reasons for reduction of OCSD of patients with TNBC who received chemotherapy.
There were still some areas for improvement in this study. Firstly, we used the PSM method to make the baseline information of the two cohorts as balanced as possible. However, in this process, some patients were excluded, which might lead to selection bias or inaccurate results. Secondly, there are various regimens of adjuvant chemotherapy for breast cancer, but due to the limitations of the SEER database, we were unable to obtain the relevant chemotherapy protocols, which prevented us from performing a stratified analysis of these elderly TNBC patients. Thirdly, the presence or absence of patient’s previous chronic disease was equally important for the OCSD. Because we were unable to obtain the prevalence of chronic disease in elderly patients prior to the diagnosis of breast cancer, we were unable to judge whether the prevalence of chronic disease was balanced between the chemotherapy and no-chemotherapy groups. Finally, as a retrospective study, the inevitable selection bias in patient selection might affect the conclusions, and we hoped that larger prospective randomized controlled trials with a higher level of evidence would be able to validate the conclusions in the future.
For older patients (
The datassets used and/or analyzed during the current study are available from the corresponding author on reasonable request.
CWH, BH, THY designed the research; THY acquired funds; CWH, JC, MJ, RC collected the data, and performed the analysis. CWH, JC wrote the manuscript. CWH, JLL, GXW, THY contributed to the statistical analysis and to the final version of the manuscript. GXW, THY supervised the project. All authors read and approved the final manuscript.
This study required no informed consent from patients because the SEER database was publicly accessible worldwide. Therefore, it was deemed exempt from review by the Ethics Committee of the Jiangxi Cancer Hospital of Nanchang University. The study was performed in accordance with the principles of the Declaration of Helsinki. The authors are accountable for all aspects of the work in ensuring that questions related to the accuracy or integrity of any part of the work are appropriately investigated and resolved.
The authors thank the Surveillance, Epidemiology, and End Results Program tumor registries for the creation and maintenance of the open database.
This study was supported by National Natural Science Foundation of China (Grant Number: 82160565), Jiangxi Provincial Natural Science Foundation of China (Grant Number: 20212BAB216063) and Science and Technology Program of Health Commission of Jiangxi Province (Grant Number: 202210055).
The authors declare no conflict of interest.
References
Publisher’s Note: IMR Press stays neutral with regard to jurisdictional claims in published maps and institutional affiliations.





