1 Department of Clinical and Experimental Sciences, University of Brescia, 25121 Brescia, Italy
2 Department of Obstetrics and Gynecology, AOUI-University of Verona, 37129 Verona, Italy
3 Department of Phatology, Spedali Civili di Brescia, 25123 Brescia, Italy
†These authors contributed equally.
Academic Editor: Shigeki Matsubara
Abstract
Background: High grade serous cancers (HGSC) of gynecological
origin can be treated with neoadjuvant chemotherapy (NACT) and subsequent
interval debulking surgery (IDS) when upfront surgery is not feasible.
Chemotherapy response score (CRS) was proposed to evaluate on pathological
specimens at IDS the response to NACT. Objective: We aim to
assess survival outcomes stratified by CRS in HGSC patients and to explore
interaction with residual disease (RD) after surgery. Methods: We identified all consecutive patients with HGSC at advanced stage (FIGO
III–IV) that underwent NACT and IDS. We collected baseline data as well as
survival data such as disease-free survival (DFS) and overall survival (OS). CRS
was assessed on adnexal and omental specimens based on a three-tier
classification. We conducted multivariate cox regression analyses of CRS
classifications (CRS 1 vs 2 vs 3, CRS 1+2 vs 3 and CRS 1 vs 2+3) using RD as
covariate. Results: We enrolled 47 patients with a median
follow-up of 25 months (IQR: 11–78). RD after IDS failed to correlate with DFS
(p = 0.73) and OS (p = 0.93). Adnexal CRS 2 (HR 0.4; 95% CI
0.2–1.0; p = 0.05) and CRS 3 (HR 0.30; 95% CI 0.11–0.65; p =
0.04) correlated with longer DFS. Moreover, CRS 2 (HR 0.12; 95% CI 0.04–0.33;
p
Keywords
- ovarian cancer
- chemotherapy response score
- debulking surgery
Ovarian cancer is a lethal malignancy and the majority of the patients are diagnosed with advanced stage [1, 2, 3] disease. The standard of care is primary debulking surgery (PDS) followed by platinum-based chemotherapy [1, 2, 4]. Neoadjuvant chemotherapy (NACT) and subsequent interval debulking surgery (IDS) is an alternative option when PDS is not feasible [5], demonstrating similar survival outcomes and rates of lower surgical morbidity in selected patients [6, 7].
Böhm et al. [8] proposed a three-tier standardized histological scoring system to evaluate NACT response in high grade serous cancers (HGSC) of gynecological origin. Subsequent studies supported the prognostic role of this scoring system for progression free survival (DFS), even though findings on overall survival (OS) are unclear [9, 10]. More recently the International Collaboration on Cancer Reporting (ICCR) recommend the use of chemotherapy response score (CRS) to evaluate HGSC after NACT, but routine clinical use has not yet been validated [11]. The aim of the current study is to assess the survival outcomes based on CRS classification and to explore the prognostic interaction with residual disease (RD) at IDS.
We considered all the consecutive cases of advanced FIGO Stage III–IV, classified as HGSC underwent NACT and subsequent IDS treated in a selected period to ensure adequate follow-up at 5 years (2011–2016). We further selected the patients according to the availability of adnexal and omental specimens for pathological evaluation. NACT was defined with at least two cycles of platinum-based treatment. IDS was performed by a dedicated gynecologic oncology team that provided surgical management as follow: midline laparotomy, total hysterectomy, bilateral salpingo-ophorectomy and inframesocolic or radical omentectomy. Additional surgical procedures were performed if required to achieve complete macroscopic cytoreduction including multiple visceral resections and peritonectomies. Subsequent adjuvant chemotherapy was administered with at least three cycles of platinum-based treatment. Clinical response to treatment was confirmed by radiological imaging at the end of the treatment. For each patient we collected age at diagnosis, FIGO stage, NACT regimen, RD after IDS, adjuvant chemotherapy regimen and survival outcomes (DFS and OS).
CRS was determined on hematoxylin and eosin staining (see Fig. 1) of adnexal and omental specimens according to Böhm et al. [8] criteria.
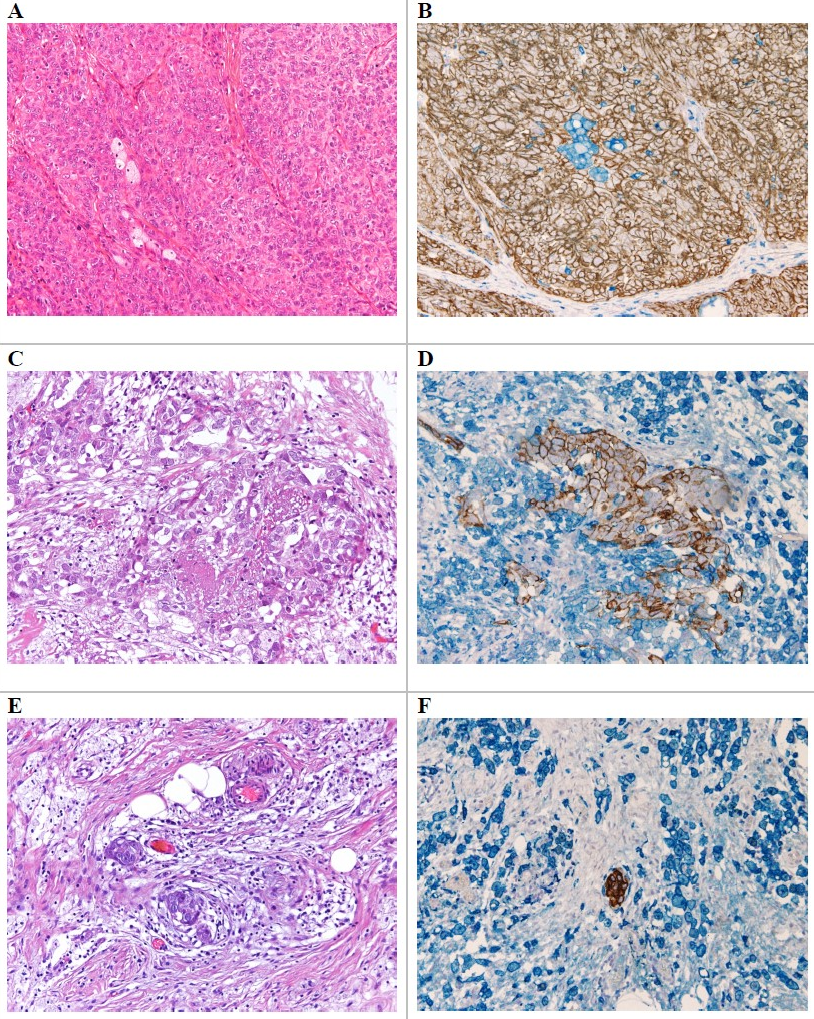 Fig. 1.
Fig. 1.Comparison of different CRS on omental specimen. (A) Hematoxylin and eosin staining of omental CRS 1. (B) Pan-cytokeratin (brown) and CD-163 (blue) staining of omental CRS 1. (C) Hematoxylin and eosin staining of omental CRS 2. (D) Pan-cytokeratin (brown) and CD-163 (blue) staining of omental CRS 2. (E) Hematoxylin and eosin staining of omental CRS 3. (F) Pan-cytokeratin (brown) and CD-163 (blue) staining of omental CRS 3.
The histological evaluation of specimens was independently performed by two gyne-pathologists who undertook the online training to acquire the skills for the application of the CRS, as provided by the aforementioned publication [8]. In case of disagreement a discussion on the specific case was held and CRS was accordingly applied. As originally described by Böhm et al. [8] both omental and adnexal samples obtained from IDS were scored given a CRS score ranging from 1 to 3. Specific description of CRS score system is summarized in Table 1.
| Score | Description |
| CRS 1 | None or minimal tumor response. Mainly viable tumor with no or minimal regression associated fibroinflammatory changes, limited to a few foci; cases in which it is difficult to decide between regression and tumor-associated desmoplasia or inflammatory cell infiltration. |
| CRS 2 | Appreciable tumor response amid viable tumor that is readily identifiable. Tumor is regularly distributed, ranging from multifocal or diffuse regression-associated fibro inflammatory changes with viable tumor in sheets, streaks, or nodules to extensive regression-associated fibro inflammatory changes with multifocal residual tumor, which is easily identifiable. |
| CRS 3 | Complete or near-complete response with no residual tumor or minimal, irregularly scattered tumor foci seen as individual cells. cell groups or nodules up to 2 mm maximum size. Mainly regression-associated fibro inflammatory changes or very little residual tumor in the complete absence of any inflammatory response. |
| CRS, Chemotherapy response score. | |
The univariate statistical analyses were conducted with log rank test and Kaplan
Meier curves. We conducted multivariable cox regression analyses either for DFS
and OS taking in account RD, three-tiered and two tiered adnexal and omental CRS
classifications as covariates. The statistical significance was defined with
p
We identified 47 patients fulfilling the criteria. Characteristics of the population are summarized in Table 2. At the end of the follow-up 37 (78.7%) patients died of disease.
| Characteristics | n | |
| Median age, years (range) | 69 (63–74) | |
| Median follow-up, months (IQR) | 25 (11–78) | |
| FIGO stage, n (%) | ||
| III | 22 (46.8%) | |
| IV | 25 (53.2%) | |
| Residual tumor, n (%) | ||
| Optimal (0 cm) | 25 (53%) | |
| Suboptimal ( |
22 (47%) | |
| Cycles of NACT, n (%) | ||
| 10 (20.9%) | ||
| 37 (79.1%) | ||
| Regiment of NACT, n (%) | ||
| Carboplatin | 10 (20.8%) | |
| Carboplatin/Paclitaxel | 35 (75%) | |
| Carboplatin/Paclitaxel/Bevacizumab | 2 (4.2%) | |
| Regiment of ACT, n (%) | ||
| Carboplatin | 11 (23.5%) | |
| Carboplatin/Paclitaxel | 34 (72.3%) | |
| Carboplatin/Paclitaxel/Bevacizumab | 2 (4.2%) | |
| IQR, inter quartile range; FIGO, International Federation of Gynecology and Obstetrics; CRS, chemotherapy response score; NACT, neoadjuvant chemotherapy. | ||
NACT was administered as follows: Carboplatin and Paclitaxel in 35 patients (75%), single agent Carboplatin (20.8%) in 10 patients and Carboplatin, Paclitaxel and Bevacizumab in 2 patients (4.2%). Twenty-one women received 4 cycles (45.8%), ten patients 3 cycles (20.9%), twelve patients 6 cycles (25%) and 4 patients 7 cycles of NACT (8.3%). Optimal cytoreduction was achieved in 34 patients (72.3%) at the time of IDS. Optimal RD did not correlate with DFS (Median 17 vs 20 months; p = 0.73) and OS (Median 28 vs 22; p = 0.93) as can be seen in Fig. 2. Adjuvant chemotherapy was administered in all the included patients with the same regimen of NAC, except for one patient who discontinued Paclitaxel.
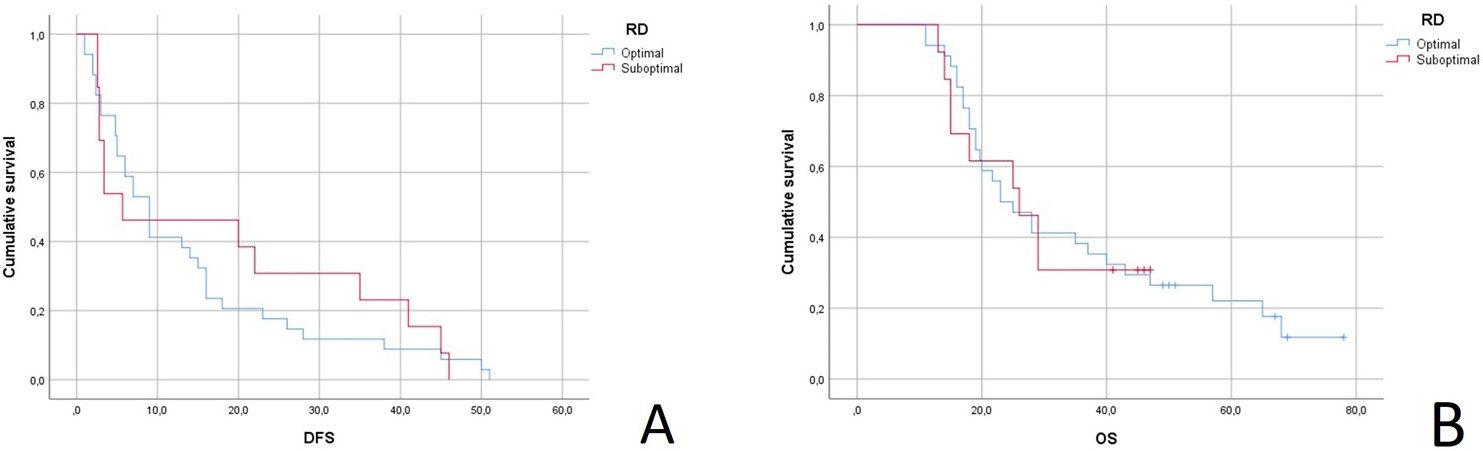 Fig. 2.
Fig. 2.Survival outcomes based on residual disease (RD). (A) DFS (Disease free survival) stratified according to RD. DFS, disease-free survival. (B) DFS (Overall survival) stratified according to RD. OS, overall survival.
At histological evaluation of the adnexa 17 patients were categorized as CRS 1 (36.2%), 17 patients as CRS 2 (36.2%) and 13 patients as CRS 3 (27.6%). CRS for corresponding omental specimen found discordance with adnexal results in 22% of the cases: 17 patients categorized as CRS 1 (36.2%), 13 patients as CRS 2 (27.6%) and 17 patients as CRS 3 (36.2%) as can be seen in Table 3.
| Omental CRS | Total | ||||
| 1 | 2 | 3 | |||
| Adnexal CRS | 1 | 10 | 4 | 3 | 17 (36.2%) |
| 2 | 1 | 8 | 8 | 17 (36.2%) | |
| 3 | 6 | 1 | 6 | 13 (27.6%) | |
| Total | 17 (36.2%) | 13 (27.6%) | 17 (36.2%) | 47 (100%) | |
Using adnexal and omental CRS 1 as reference, we respectively found that adnexal CRS 2 (HR 0.4; 95% CI 0.2–1.0; p = 0.05) and adnexal CRS 3 (HR 0.30; 95% CI 0.11–0.65; p = 0.04) were both good prognostic factors for DFS, while omental CRS 2 and CRS 3 were not significant (respectively with a p value of 0.72 and 0.96).
Adnexal CRS 2 (HR 0.12; 95% CI 0.04–0.33; p
We avoided the analysis of a two-tier classification of adnexal CRS given the significant results obtained by the three-tiered one. On the counter side, using omental CRS 1 as reference, we failed to found a significant role for CRS 1+2 for DFS (p = 0.7) and OS (p = 0.38). Again, exploring the two-tier omental system by combining CRS 2+3, we failed to found a significant correlation with DFS (p = 0.7) and OS (p = 0.4).
To investigate if the number of cycles would impact the prognostic performance
of CRS we further performed a multivariable analysis incorporating this variable
as covariate. Using adnexal CRS 1 as reference, we found that CRS 2 (HR 0.43; 95%
CI 0.18–1.00; p = 0.5) and adnexal CRS 3 (HR 0.29; 95% CI 0.11–0.65;
p
Our results confirmed that, regardless the number of cycles administered as NACT and the RD at IDS, adnexal CRS three-tied system can be a useful prognosticator for DFS and OS, while omental CRS was not able to provide clinical insights regarding survival trends. Histopathological tumor response to NACT is routinely assessed in breast, esophageal, and rectal cancers [12, 13, 14]. In 2015 Böhm et al. [8] proposed the three-tier CRS system to evaluate NACT response in HGSC. Subsequently different studies investigated this system and its correlation with DFS and OS [9, 10, 15, 16, 17, 18, 19, 20, 21, 22, 23, 24, 25]. Heterogeneous results were reported and its prognostic value remained unclear. Our findings support that the three-tier CRS system is reproducible scoring system, even though with limitations.
In fact, our study demonstrated a correlation of adnexal CRS three-tier system with DFS, consistently with the majority of the published studies [9, 10, 15, 19]. The three-tier system had significant association with OS in adnexal specimens, in line with Ditzel et al. [9], but in contrast with other authors and the original paper of Böhm et al. [8, 10, 19, 23]. Moreover, as original results, we further demonstrated the validity of the aforementioned correlations regardless the RD after IDS and regardless the number of cycles of NACT and in our mind, this is the “real world” results of CRS application.
In our study the omental CRS three-tier system did not correlate with DFS and OS, confirming the main findings of the previous studies [9, 10, 26]. To increase the prognostic value, we applied a two-tier score, as previously proposed in literature, combining omental CRS 1 and CRS 2 but statistical analysis failed to demonstrated correlation with OS, supporting other authors findings [9, 10, 15, 18]. In our study neither the three-tier system or the two-tier system on omental specimens demonstrated to correlate with a longer DFS in contrast with the majority of the previous reported results [8, 9, 23]. To our knowledge, for the first time we proposed an analysis of an omental two-tier system, even though our findings did not support its use as prognosticator.
The discordant results on adnexal and omental specimens may reflect the different susceptibility to chemotherapy in different cell clones with heterogeneity of genomic profiles in metastatic localization [27]. Cancer cell which migrated to other sites may develop less sensitivity to chemotherapy compared to the primary adnexal localization and different tissue blood supply influences the response to medical treatment [27]. Moreover, host immunity response demonstrated to correlate with survival [28] and other authors proposed to include additional histopathologic features into CRS system to increase the prognostic accuracy, investigating tumor-specific infiltrating inflammatory cells [24].
In our cohort of patients, the statistical analyses failed to demonstrated a correlation between RD and OS (p = 0.93) probably due to the small simple size and the retrospective design of the study. Moreover, older patients may be less frequently candidate to PDS and our results could be influenced by age or performance status at baseline, reducing the CRS role in every day practice, even though NACT is used mostly for patients with not resectable disease [29]. Nowadays, the clinical role of CRS is unclear, since it is a post-surgical data and so far, is unable to predict RD, feasibility of IDS should be evaluated with clinical and radiological findings [21]. On the other side, Zorzato et al. [25] selected a cohort of patients with complete clinical response presenting different rates of CRS and authors found out the inadequacy of preoperative radiological and serologic evaluation to identify the magnitude of response and suggested histological assessment to improve the accuracy.
CRS was applied to a uniform population with updated and documented follow-up of which adnexal and omental specimens were both available. Moreover, the statistical analysis investigated the impact of RD on CRS prognostic performance.
Our study has few limitations such as its retrospective single center design and the small sample size. Again, BRCA status was not available at the moment of analysis and this could impact analysis.
Our results demonstrated that adnexal CRS three-tier system may represent a useful tool to predict DFS and OS regardless RD at IDS. On the contrary, omental CRS failed to correlate with survival both in three and two-tier system. Future trials are needed to clarify the correlation of CRS with DFS and OS and to understand the possibility of a tailored treatment based on histological response to NACT. Research efforts are required to detect potential molecular factors correlated with a better CRS score to predict the sensibility to chemotherapy in HGSC.
FF, FC, AG contributed to the intellectual content of the study and approved the final version of the article. FF, FC, AG, LA, ES and FO were responsible for the study design. FF and FAF performed data analysis. FF, FC, FAF wrote the manuscript. FF, SF edited the manuscript for intellectual content and supervised the study development. FF, FC, AG, FAF, LA, SF, ES and FO gave approval for the final version of the manuscript.
The institutional review board and the ethical committee of the Spedali Civili di Brescia and University of Brescia considered this study exempt since it was conducted as an internal audit. The study complied with the Ethical Principles for Medical Research Involving Human Subjects according to the World Medical Association Declaration of Helsinki and was conducted as an internal audit.
Not applicable.
This research received no external funding.
The authors declare no conflict of interest. FF is serving as the guest editor of this journal. We declare that FF had no involvement in the peer review of this article and has no access to information regarding its peer review. Full responsibility for the editorial process for this article was delegated to SM.
References
Publisher’s Note: IMR Press stays neutral with regard to jurisdictional claims in published maps and institutional affiliations.


