1 Department of Caring Sciences, University of Gävle, 80176 Gävle, Sweden
2 National Board of Health and Welfare, 11259 Stockholm, Sweden
3 Department of Women’s and Children’s Health, Uppsala University, 75185 Uppsala, Sweden
Academic Editor: Michael H. Dahan
Abstract
Background: Female genital mutilation/cutting (FGM/C) is a global public health problem associated with an increased risk of physical, sexual, and mental health consequences. Surgical healthcare intervention may alleviate negative health consequences related to FGM/C. In this review, we aim to offer an overview of documented effects of surgical healthcare interventions after FGM/C, from the perspectives of both healthcare providers (HCPs) performing such interventions and the women receiving them. Methods: We searched four databases (PUBMED/MEDLINE, CINAHL, PsychInfo, Cochrane Library) for peer-reviewed articles published between 2000 and 2021, and retrieved a total of 1978 citations (1203 + 775). After scrutinizing the citations with the inclusion criteria (1) observable outcomes of surgical healthcare interventions after FGM/C, (2) HCPs’ perceptions of FGM/C-related surgical healthcare and experiences of providing surgical care for FGM/C-affected women, and (3) FGM/C-affected women’s perceptions and experiences of the effects of FGM/C-related surgical healthcare, we selected 38 articles to include in this review. Results: HCPs and FGM/C-affected women differed in their views on surgical interventions. While providers seemed to suggest premarital defibulation regardless of a woman’s age and marital status, affected women voiced social and marital concerns related to defibulation, which sometimes overrode the physical consequences. On the other hand, some providers were reluctant to perform intrapartum defibulation due to uncertainty or misinformation about infibulated women’s wishes, while women often expected and desired defibulation prenatally. And while gynecologists demonstrated skepticism towards clitoral reconstruction, most women who had undergone the procedure were satisfied, particularly regarding the psychosocial and sexual aspects. Conclusions: Providers and recipients of surgical interventions after FGM/C seem to display contrasting views on surgical intervention after FGM/C, which may have implications for healthcare recommendations as well as satisfaction. This apparent ambiguity between providers’ and recipients’ perceptions of surgical interventions needs further investigation.
Keywords
- clitoral reconstruction
- defibulation
- female genital mutilation/cutting
- gynecology
- healthcare
- interventions
- midwifery
- obstetrics
- providers
- surgery
Female genital mutilation/cutting (FGM/C), an acknowledged public health problem, entails altering the female genitalia for non-medical reasons [1]. It may involve cutting the clitoris (clitorectomy) or the labia minora/majora (excision), and/or closing the vaginal orifice (infibulation). It may also involve pricking or burning the clitoris. While the World Health Organization has classified FGM/C into four types [1], cutting communities may use different terminology, including “pharaonic circumcision” (which often refers to infibulation) or “sunna circumcision” (which may refer to pricking, clitorectomy, or even excision) [2].
Worldwide, around 200 million women and girls are thought to have undergone some form of FGM/C [3]. While it is carried out mainly in parts of Africa, Asia, and the Middle East, due to migration it is increasingly becoming a healthcare concern in non-practicing countries: An estimated half a million women and girls with FGM/C live in Europe [4]. Most of them are likely to have been cut before migration, as there is reason to believe that positive attitudes towards FGM/C, particularly infibulation or “pharaonic circumcision”, diminish after migration [5, 6, 7].
FGM/C is associated with an increased risk of health consequences [8]. Long-term health consequences can include urinary tract infections, bacterial vaginosis, increased risks of obstetric consequences, obstruction of urine and menstrual blood, and sexual dysfunction [8, 9]. While such medical consequences are widely documented [1], a distinction between types of FGM/C in relation to consequences is rarely mentioned in the literature. Yet, many of the documented health consequences are more related to the more invasive forms of FGM/C, including infibulation, than to less invasive forms such as “sunna” or pricking, even if these distinctions are often blurred [2]. Studies show that access to surgical interventions can alleviate negative health consequences, particularly in relation to certain types of FGM/C, including infibulation and clitorectomy [10].
The reasons for carrying out FGM/C are multilayered and complex, and involve (but are not limited to) rite of passage and initiation into adulthood, long-held traditions meaningful for the formation of gender and ethnicity, and ensuring sexual and moral dignity [7, 11]. Meanwhile, research concerning FGM/C from a global health perspective often focuses solely on the medical consequences, which has caused some scholars to criticize this literature for being oversimplistic in its failure to consider the cultural, historical, and relational meaning-making of FGM/C [12, 13]. To deepen the understanding of whether and how surgical interventions may alleviate FGM/C-related health consequences, taking into consideration medical, social, and interpersonal aspects, this review offers an overview and analysis of studies from multiple perspectives, including those of healthcare providers (HCPs) and FGM/C-affected women.
In this review we aim to provide an overview of the existing research concerning surgical healthcare interventions for FGM/C-related health consequences. To do this, our specific objectives are to investigate the published literature on (1) observable outcomes of surgical healthcare interventions after FGM/C, (2) HCPs’ perceptions of FGM/C-related surgical healthcare and experiences of providing surgical healthcare interventions for FGM/C-affected women, and (3) FGM/C-affected women’s perceptions and experiences of the effects of FGM/C-related surgical healthcare interventions.
Our inclusion criteria were peer-reviewed, original qualitative and quantitative research articles and literature reviews relevant to the study objectives, published in English after the year 2000. We included studies investigating surgical healthcare interventions for all types of FGM/C-related complications and the outcome of such interventions in the form of measurable outcomes as well as perceptions of providers and recipients. We excluded studies reporting on HCPs’ knowledge and attitudes about FGM/C, or on HCPs’ general perceptions of FGM/C-related care (i.e., that did not explicitly relate to surgical care). Likewise, we also excluded studies concerning FGM/C-affected women’s general perceptions of HCPs and care. We did this because such general aspects of FGM/C-related care are already well documented elsewhere. Further, we excluded studies related to the medicalization or reinfibulation of FGM/C (when FGM/C is performed in hospitals or at healthcare clinics) since this is illegal in most countries of the Global North and is thus not considered “surgical healthcare”. We also excluded conference proceedings, posters, commentaries, discussion papers, and case studies. Finally, we excluded reviews with “no included studies”. We did not exclude studies based on their methodological quality, but instead assessed the quality (see Supplementary Material 1) to judge the studies’ relative contribution to the evidence.
A database search specialist performed electronic database searches in PUBMED/MEDLINE, CINAHL, PsychInfo, and the Cochrane Library in consultation with the authors. The databases were searched for articles published between 2000 and May 2019 covering the existing published research on healthcare related to FGM/C, and a second search with slightly modified search terms was done in March 2021. For a detailed overview of the first and second search strategies and search terms for each database (see Supplementary Materials 2 and 3).
In the first search we identified 1203 unique citations, which we considered for eligibility (after duplications were removed), including six citations identified through other sources. The first and last authors scrutinized all citations based on title, keywords, and abstract according to the study objective. At this point, citations were excluded when the eligibility criteria were not fulfilled, resulting in the exclusion of a total of 1078 citations Full-text articles were retrieved for the remaining 125 citations. These articles were read by the first author who, if uncertain about whether an article should be included in the review, discussed this with the last author. They then compared their judgements and came to a consensus decision regarding which articles to include in the review. On further scrutiny, and with the aim of this article in mind, 90 articles were removed as they did not meet the inclusion criteria. Ultimately, 35 articles were selected from this search. In the second search 775 additional citations were identified, and were scrutinized in the same manner as those identified through the first search. In the second search, three additional articles fulfilled the eligibility criteria. A total of 38 articles were included in this review (see Fig. 1).
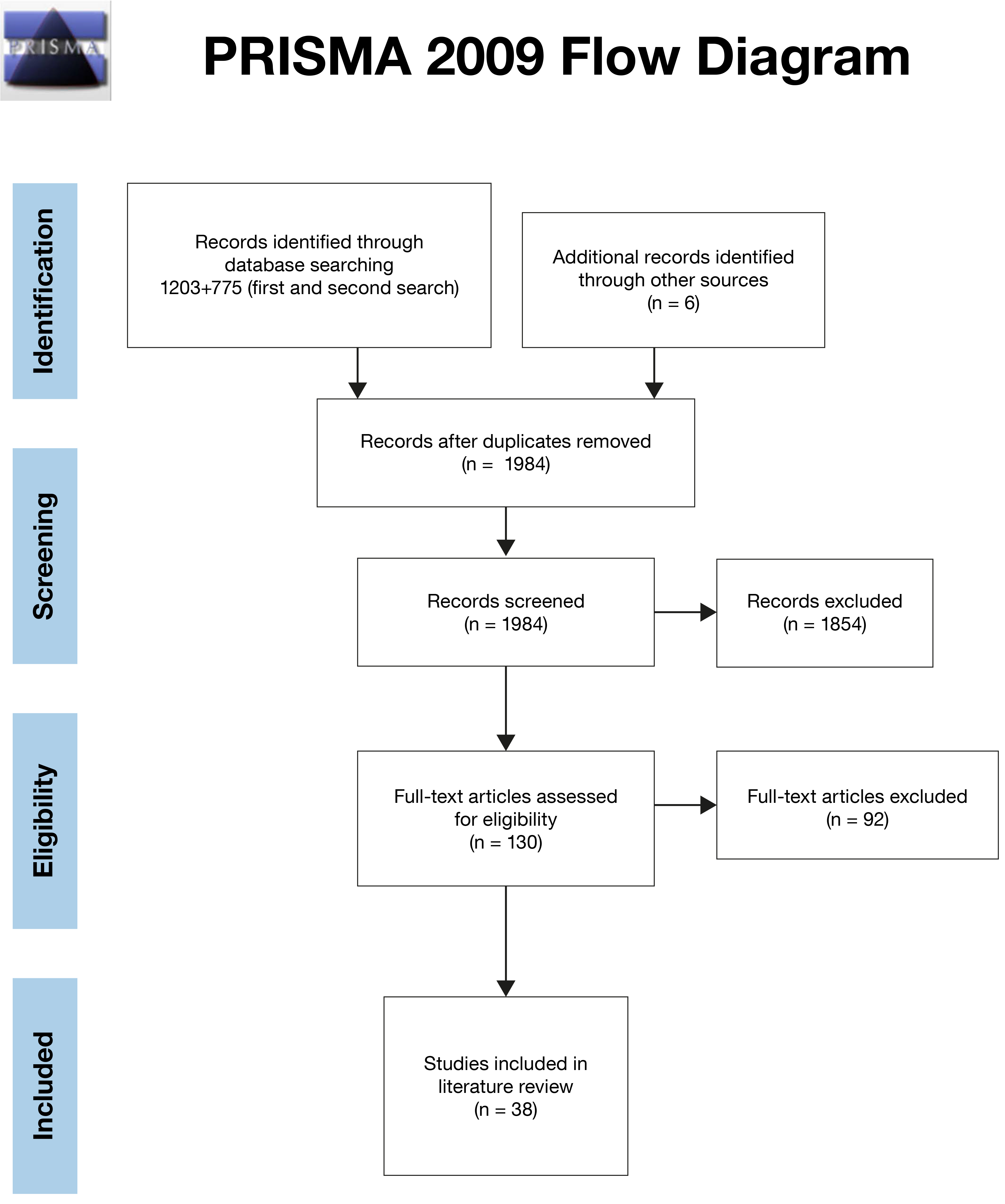 Fig. 1.
Fig. 1.Prisma 2009 flow diagram. From: Moher D, Liberati A, Tetzlaff J, Altman DG, The PRISMA Group (2009). Preferred Reporting Items for Systematic Reviews and Meta-Analyses: The PRISMA Statement. PLoS Med 6(7): e1000097. doi:10.1371/journal.pmed1000097. For more information, visit http://www.prisma-statement.org.
The quality of all the included articles was assessed using the Johns Hopkins Evidence-Based Practice for Nurses and Healthcare Professionals Model (see Supplementary Materials 1 and 4). By scrutinizing the content and looking for patterns in the included articles’ result sections (rather than merely the predefined themes and/or headings identified by the authors) we created themes and subthemes, presented below.
The identified studies reporting on surgical interventions concerned mainly defibulation, clitoral reconstruction, and to a smaller extent, cyst removal. Most of the included studies were from a Western healthcare setting. A prominent finding was that providers and recipients seemed to hold different views: While providers seemed not to question the benefit of premarital defibulation, this was not unproblematic for infibulated women. On the other hand, at times some providers seemed reluctant to perform intrapartum defibulation due to misconceptions regarding infibulated women’s wishes, while the women in question often expected and desired it. Regarding clitoral reconstruction, providers demonstrated skepticism while most women who had undergone this surgery seemed to appreciate it.
Defibulation — reconstructive surgery of the infibulated scar, surgically opening the fused labia caused by infibulation — was (at least partly) the phenomenon of concern in 28 articles.
Most articles concerning defibulation investigated perceptions and outcomes of the surgery in the context of pregnancy and childbirth. Studies involving the opinion of infibulated women demonstrated that defibulation surgery was deemed necessary during childbirth to avoid tears and prolonged labor [14, 15, 16, 17, 18]. Yet, in some included studies the women reported dissatisfaction with, and communication problems regarding, how and when defibulation should be done. When attempting to communicate how they wanted the defibulation to be done, infibulated women were often met with an unwillingness by doctors and midwives to listen to their advice [19]. Consequently, they did not feel involved in the healthcare process, which led to a sense of loss of autonomy related to the clinical decision-making [20]. Further, when infibulated women were asked about their preferences regarding the timing of defibulation, the authors of several studies found that the women preferred intrapartum defibulation as they wanted to avoid being cut twice (first during the intrapartum defibulation and again during childbirth if episiotomy was necessary) [21, 22, 23]. In other studies, the authors demonstrated that infibulated women preferred being defibulated prior to childbirth, particularly if there were medical benefits, as it can then be done in a calmer setting than during childbirth [14, 24].
HCPs, on the other hand — often including midwives, gynecologists, and obstetricians working in maternity wards — reported insecurity concerning how to care for infibulated women. This could include judging the inelasticity of the perineum when infibulated women presented for childbirth, how to open the infibulation scar during childbirth without damaging nearby tissue, how to give local anesthesia, how much to cut open, and how to sew afterwards [16, 25, 26, 27]. The lack of a system for reporting FGM/C in the medical records further resulted in a sense of unpreparedness in dealing with FGM/C, which created chaotic delivery situations and stress for both midwives and infibulated birthing women [15, 16, 19, 25, 28, 29]. HCPs were also of divergent opinions regarding whether and when to defibulate; some midwives in Australia thought that infibulated women wanted to wait with defibulation until the delivery, when they were most likely to have an episiotomy anyway, or that the woman’s family members would discourage this, while others thought it should be done prenatally [30]. Some midwives in Norway said they refrained from performing defibulation surgery as they thought it was “difficult” or dangerous, or because they believed that infibulated women wanted to keep their infibulation intact [15, 16]. And some doctors working in delivery wards in Sweden advocated for defibulation while taking care not to damage underlying tissue, while others suggested mediolateral episiotomy only, a procedure similar to that performed on non-cut women [28]. Thus, HCPs sometimes performed a caesarean section or multiple episiotomies instead of defibulation, despite the former being physiologically more invasive [15, 31].
Several articles measured observable medical outcomes of prenatal versus intrapartum defibulation, such as blood loss, vaginal tears, and the likelihood of having an episiotomy [10, 16, 21, 32, 33, 34, 35]. In one study, the authors found a slight medical advantage of prenatal defibulation compared to intrapartum [33]. In another, women with intrapartum defibulation had higher blood loss on average, but lower levels of vaginal tears during childbirth [36]. Here, the authors also found that women with prenatal defibulation were more likely to have an episiotomy during childbirth than women who did not. In a meta-analysis of four studies investigating prenatal versus intrapartum defibulation [10], no statistically significant difference in obstetric outcomes was found. Thus, the available evidence regarding obstetric outcomes related to the optimal timing of defibulation during pregnancy points in different directions.
While infibulated women perceived defibulation during pregnancy or childbirth necessary, this was not necessarily the case for defibulation outside this context. Because infibulation was considered a sign of virtue and sexual morality, several authors demonstrated that defibulation prior to marriage was not accepted among women as they feared it would impact their marital and sexual relationships negatively [15, 21, 24, 37]. Consequently, some infibulated women were resistant to undergoing premarital defibulation even if they were experiencing physical pain and discomfort. Women who nonetheless opted for premarital defibulation, mainly due to medical issues and physical discomfort, often kept this a secret due to a fear of being regarded as promiscuous or of humiliating their husband, as defloration of the scar is a demonstration of virility [21, 32, 37, 38].
In a handful of studies, women’s satisfaction with their genital appearance after defibulation was considered; whereas some said they were satisfied with how their genitals looked post-surgery [21], others disliked the post-defibulation appearance, which created distress [32, 37, 39].
Some studies concerned women’s satisfaction with defibulation in relation to sexual function [10, 21, 38, 40, 41]. In one systematic review, the authors demonstrated that sexual function mostly improved after defibulation, mainly as penetrative intercourse became less painful but also because in some instances the women experienced an increased ability to reach orgasm [10]. In two studies, the authors had used the Female Sexual Function Index (FSFI) questionnaire to measure the effect of defibulation on sexual function [38, 41]. In their before-and-after study, Krause et al. [41] found that defibulation led to improvements in desire, arousal, satisfaction, and pain, while lubrication and orgasm remained unchanged; and Nour et al. [38] found that 94% of the 32 women involved in the study would recommend defibulation to other women, based on the sexual outcomes. However, only a limited number of the studies on defibulation focused on sexual outcomes.
Clitoral reconstruction (CR) was (at least partially) the focus of concern in 13 of the included articles. CR is a surgical technique aimed at reducing pain and restoring the anatomy and function related to sexual capacity in women with clitorectomy [42]. While outcomes regarding sexual function were the primary focus of most of the studies, some also examined satisfaction with one’s genital appearance. In the majority of the studies investigating sexual function before and after CR, the authors used non-validated scales for measuring outcomes like pain, clitoral pleasure, and sexual function; some, however, used validated scales such as the FSFI questionnaire [43, 44, 45].
Most of the women undergoing CR, although not all, expressed satisfaction regarding both genital appearance and sexual function. In a large cohort study comprising a follow-up of 866 women one year post-surgery, the authors found that almost all included women had experienced improvements, or at least no worsening, in pain and clitoral pleasure [42]. In one systematic review concerning women’s experiences of undergoing CR, the authors found that 64–86% of the women were very satisfied with the surgery, particularly regarding aesthetics and gender identity [21]. In another systematic review investigating the effectiveness of CR, in which sexual function was measured in eight studies [10], the authors concluded that 43% of the women experienced improvements in pain, 63% in clitoral pleasure and function, and 50.8% in desire. In other studies as well, the authors reported overall improvement in women’s sexual function after the surgery [43, 44, 46, 47]. Improvements in body image, aesthetic appearance, relationships with others, and psychological well-being, ranging from 88% to 96%, were also reported [10, 46, 48]. Improvement in sexual distress, psychopathology, was reported in a study with 27 patients, using validated scales such as Beck’s Depression Inventory and Female Sexual Distress Scale-Revised [43].
Negative effects of CR were reported in some studies, including the cohort study by Foldès et al. [42]; here, the authors reported that 2.3% of the women experienced a worsening of clitoral pleasure, 8.2% decreased desire, and 22.6% a diminished ability to reach orgasm after the surgery in women who had experienced regular orgasms prior to surgery [10]. However, outcomes of CR on orgasmic function are ambiguous, as authors of other studies on CR have reported improved orgasmic function [44]. Only one study investigated obstetric outcomes after CR [49]. Here, conducting a case-control study with 84 women (28 in the CR group and 56 in the control group), the authors found that CR reduced the risk of episiotomy during childbirth (29.54%) compared to the control group (63.6%) [49].
Only one study investigated HCPs’ perspectives on CR: In a qualitative study investigating gynecologists’ attitudes towards CR, a negative attitude towards CR and consequently a reluctance to refer women to such surgery was demonstrated [50]. The gynecologists justified their reluctance by explaining that they did not regard the surgery as having functional benefits, and that potential symbolic, aesthetic, and mental justifications for seeking surgery were not considered sufficient for referral [50].
A third type of reported surgical intervention for improving FGM/C complications was the removal of cysts and keloids. Most of the published studies on cyst removal were clinical case studies, which were excluded in this review. However, one systematic review by Berg et al. [10] including 21 published case studies on cyst removal was included. Here, the authors found no intraoperative complications, good recovery, and no reoccurrence of cysts one to six years post-surgery. Improvement of women’s sexual function was another documented outcome related to cyst removal surgery in this review [10]. Yet, in an original study from Egypt, the authors reported a worsened sexual score after cyst removal [51]. The lack of conclusiveness on sexual function after the removal of cysts is inconclusive, likely highly related to the scarcity of studies on this topic.
In this review we found that defibulation and CR are the two most reported surgeries for treating FGM/C-related health complications. Scrutinizing the literature on these surgeries, we found that HCPs and FGM/C-affected women largely viewed the surgeries differently, in regard to both approving of the surgery as well as when, how, and why to perform it.
For several decades, health policy organizations such as the World Health Organization and the Royal College of Obstetricians and Gynaecologists have recommended defibulation for all infibulated girls and women, preferably prior to marriage and the initiation of sexual activity [52, 53]. The rationale behind this is to reduce physical complications related to micturition and menstrual blood flow, sexual intercourse, and childbirth, and the notion that improving such functions will improve cut women’s health and well-being. We found, however, that infibulated women reported negative attitudes towards premarital defibulation or defibulation prior to childbirth, even if they were experiencing such physical problems, and that women undergoing premarital defibulation reported genital anxiety and a fear of being discovered. While this may seem irrational in a Western context and from an HCP perspective, refuting premarital defibulation may be logical from the women’s perspective as it removes the purpose and thus the meaning of the infibulation (to ensure sexual chastity and virginity) [15], as well as jeopardizing their own and their families’ social status and well-being. Even so, most of the studies on defibulation we reviewed focused not on social risks but on physical outcomes in the context of pregnancy and childbirth.
It might be the case that infibulated women experiencing physical concerns related to infibulation may be positive to “partial defibulation”; that is, opening the defibulation enough to allow urine and menstrual blood to flow, but without radically altering the aesthetic. While defibulation is often portrayed as “easy to perform” and as not requiring particular surgical skills in plastic and reconstructive surgery [54], HCPs report uncertainty regarding how to defibulate. Furthermore, defibulated women reported distress and stigma for having “ugly” (post-defibulation) genitals, with the “flesh…hanging” [55]. Without proper communication about the physical and social issues of defibulation, as well as a requirement that operating HCPs have sufficient reconstructive surgical skills, women may be reluctant to opt for defibulation. Instead, the enabling of a forum in which different care possibilities can be discussed could enhance safe and professional care.
CR surgery was mainly developed to reduce pain and improve sexual function [42, 51]; however, women also seek CR for symbolic, aesthetic, and emotional reasons [56]. While the large health organizations widely endorse defibulation, they do not recommend CR due to a lack of evidence on its risks and benefits [1, 53]. Another possible reason for this reluctance may be that the primary outcome of CR is the improvement of sexual health and aesthetic rather than physical health, which is the case for defibulation. Yet, as the surgical risk entailed by CR seems low [10, 57], and as studies suggest satisfaction among women undergoing it [21, 42], the recommendation scheme is somewhat puzzling and needs to be explored further.
Interviews with women opting for CR demonstrate that the women themselves perceive it as less controversial than caregivers and policy guidelines do, and many claim CR as a basic human right and redress for the injustice done to them [56]. Still, HCPs and researchers seem concerned about the surgical risks related to CR as well as women’s rationales for wanting surgery [58]. Instead, non-surgical interventions such as sexual education and counseling are often suggested for improving cut women’s sexual health [59, 60]. This could be seen as a valid point, as surgery is always risky. However, suggesting therapy for something that is perceived as a physical violation has been strongly criticized by women seeking and undergoing CR [61]. While sexual education and counseling might well be a solution to FGM/C-affected women’s sexual problems and should indeed be available, this may not be everyone’s preference. Instead, women wanting CR should be listened to and respected regarding their perceptions and needs, while simultaneously being given adequate information on the inconclusive, yet growing, evidence of the benefits and risks of CR.
In this review we identified that most research on FGM/C-related healthcare is carried out in the context of pregnancy and delivery. This could indicate that most cut women do not experience FGM/C-related problems, or that it is the medical outcomes of FGM/C and potential healthcare interventions that are in focus rather than the psychosexual aspect, even if there seems to be a shift underway here. It could also relate to women who are experiencing FGM/C-related health problems related to things like menstruation, micturition, and penetrative sex (if infibulated) refraining from seeking care due to various obstacles. One such obstacle could involve the woman’s conceptualization of FGM/C. Norwegian anthropologist Elise Johansen [7] suggests that infibulated women’s lack of acceptance of premarital defibulation is linked to infibulation being seen as a sign of virtue and virginity, and thus important to maintain due to social status and relations. Another obstacle to seeking care could lie in the woman’s lack of knowledge regarding the existence of services [24] that provide FGM/C-related care such as surgical and psychological care, which are nevertheless scarce in most settings. Yet another obstacle could be related to cut women’s previous negative experiences of healthcare services in diaspora. The first obstacle, how FGM/C is perceived, could change with time as migrants’ values concerning it are likely to change with exposure to the dominant values in the host country [5, 62]. As discussed above, negotiating partial defibulation may reduce some of the anxiety related to defibulation while at the same time alleviating physical problems such as the obstruction of urine or menstrual flow. The second, a lack of knowledge of FGM/C care services, could be diminished through improved information about such specialized services, as well as integrating specialized care and competence in the public healthcare setting and thereby ensuring that it is available to all women regardless of where they live. The third obstacle, involving how women are met in healthcare contexts, could be improved by providing HCPs with skills and confidence in how to provide good care for FGM/C-affected women through educational programs, continuous training in the technical and social aspects of surgical interventions, and policy guidelines.
This article is based on a report providing an overview of the existing healthcare for FGM/C-related problems, carried out for the National Board of Health and Welfare in Sweden. While the scope of the original report included all types of healthcare interventions, we decided to narrow this review to FGM/C-related surgical healthcare interventions, yet from multiple perspectives including those of HCPs and FGM/C-affected women. Thorough discussions between the authors and a professional database search specialist led to a broad body of citations, which were scrutinized carefully so as not to miss any important articles. Our awareness of existing systematic reviews on surgical healthcare prompted the decision to include reviews. Although this is unusual in reviews, we believe that this decision provided a broader picture of the phenomenon, as these reviews may have included studies we would otherwise have missed, such as single case studies. One limitation was the lack of identification of randomized control trials and experimental studies. This may be related to the difficulty (not least ethically) of carrying out such studies related to surgical care for FGM/C-affected women. Further limitations were that most of the included studies were qualitative and based on a small sample size, that the quantitative studies often used non-validated questionnaires, and that differentiation between different types of FGM/C was seldom reported. Further, our decision to include studies regardless of quality level (see Supplementary Material 1) indicates a need for caution regarding the strength of the evidence. These limitations reflect the still marginalized research within the field of FGM/C.
Most of the included studies dealt with FGM/C Type III (infibulation) in relation to pregnancy and childbirth. This reflects where the attention lies in terms of FGM/C-related problems, and may provide a distorted picture of the need for FGM/C-related care. Our review signifies the dearth of research within the area of FGM/C, and the predisposition to focus on certain types of FGM/C (such as Type III) and treatments (such as defibulation surgery).
Also, many of the included studies were published more than ten years ago, which may also partly be the reason for the unequal focus on defibulation surgery; while there are several studies on defibulation throughout the time span researched (2000–2021), those on CR are fewer and more recent, as CR surgery has mostly been available in the last decade. This is also reflected in the virtual absence of studies on HCPs’ perceptions of CR. This unequal bias towards defibulation research is (hopefully) likely to change with time.
This review has demonstrated that defibulation surgery and clitoral reconstruction are the two main surgical interventions available to women with FGM/C. HCPs and FGM/C-affected women largely consider these two types of surgeries differently, particularly when it comes to sexual, aesthetic, and social benefits and risks. While HCPs are more concerned with medical outcomes and surgical risks, the psychosocial aspects of these surgeries are important to FGM/C-affected women. To provide FGM/C-affected women with quality care, HCPs need to understand surgical healthcare interventions after FGM/C beyond the purely medical/surgical risks and benefits.
The first and the last author (MJ and AW) were responsible for reviewing the selected articles, drafting and writing up the final article. The second author (SA) were responsible for the design of the study as well as reading and commenting on the final draft. All three author have read and approved the final version.
Not applicable.
We want to acknowledge the search specialist Kazuko Gustafsson who carried out the literature search.
The study was funded by the Swedish National Board of Health and Welfare.
This study was undertaken on behalf of the Swedish National Board of Health and Welfare and has previously been published as part of a report in Swedish. The study has been rewritten. Permission to publish the study has been granted by the Swedish National Board of Health and Welfare. We declare no competing interests.
Supplementary material associated with this article can be found, in the online version, at https://doi.org/10.31083/j.ceog4906136.

