1 Department of Dermatology, Basildon University Hospital, SS16 5NL Basildon, UK
2 Department of Dermatology, Homerton Healthcare NHS Foundation Trust, E9 6SR London, UK
Skin of colour (SOC) can mask erythema due to higher eumelanin, altering emergency presentations and risking delayed care [1]. SOC is a broad term referring to people with non-white European skin, encompassing diverse groups including African, Asian, Indigenous and Pacific Islander people [2]. No widely adopted scale exists to classify the skin’s response to inflammation caused by disease. The Fitzpatrick scale predicts sensitivity to ultraviolet radiation (UVR) [3] but not inflammation [4], leading to calls for a scale describing skin in relation to the eumelanin concentration scale to predict inflammatory response. To this end, the Eumelanin Human Skin Colour Scale has been designed but is yet to be routinely used [5].
Everyone, regardless of skin colour, has the same number of melanocytes; differences in eumelanin amount, melanosome size, and maturity determine skin colour, ultraviolet (UV) protection levels and response to inflammation [6].
Erythema (from the Ancient Greek meaning, “a redness or flush on the skin”) has been used as the key sign of inflammation. However, in SOC, erythema may be masked by the brown pigment of eumelanin, leading to an underestimation in the severity of the presentation, leading to inequitable dermatological care as a consequence [7]. In addition to this, images of SOC are underrepresented in medical literature and education [8, 9].
In this editorial, we address common dermatological emergencies and key principles in examining and providing initial management.
Erythroderma is described as fine scaling of 90% of the skin surface in association with erythema and significant pain and high risk of mortality due to skin barrier failure leading to fluid loss and heart failure [7]. Full medical assessment, including history, head-to-toe examination of skin and mucosal surfaces, photos of original skin, and pain inquiry, is crucial to avoid misdiagnosis. The commonest causes of Erythroderma are pre-existing dermatoses, severe drug reactions, malignancy and idiopathic reactions [10, 11] (Tables 1,2).
| Cause | Percentage |
| Pre-existing dermatoses | 70.77% |
| Idiopathic | 14.23% |
| Drug induced | 12.69% |
| Malignancy | 2.31% |
| Summary of clinical features |
| Generalised violaceous or hyperpigmented skin affecting |
| Exfoliation of the skin |
| Lichenification |
| Palmoplantar keratoderma |
| Ectropion |
| Peripheral lymphadenopathy |
| Nail changes (dull, brittle, shiny) |
| Non-scarring alopecia |
In SOC, dry skin may appear ashen, while exfoliation presents as darkened patches with white or yellow scales [12] (Fig. 1). On the feet, there may also be palmoplantar keratoderma presenting as thick, dry palmoplantar skin [13]. Reported nail changes include a ‘shiny’ appearance, discolouration, brittleness and in some instances the nail may totally shed [10] (Figs. 1,2). Commonly associated symptoms are pruritus and pain [14].
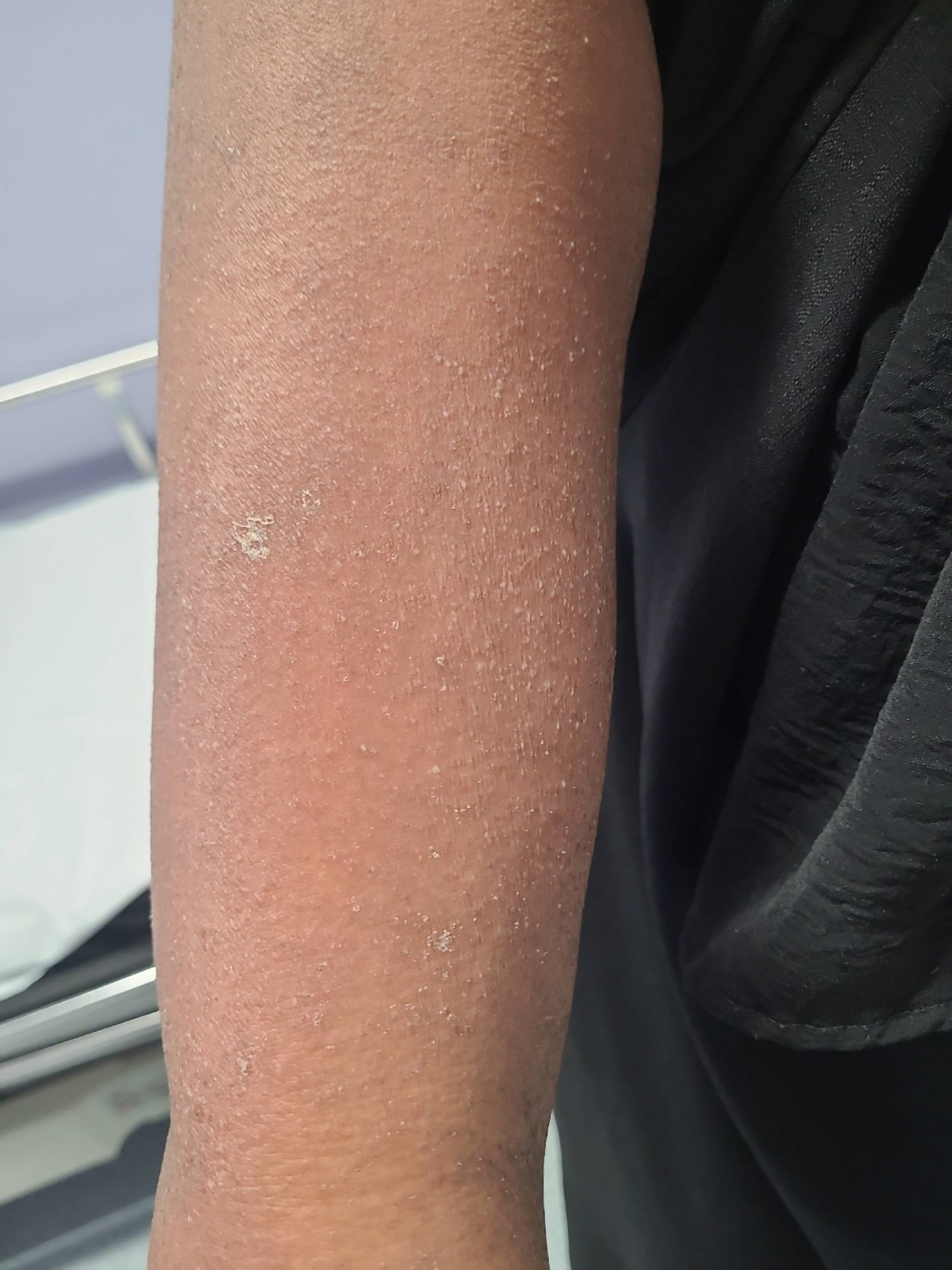 Fig. 1.
Fig. 1.
Erythroderma in a patient of South Asian heritage. Hyperpigmentation and fine scale are present; erythema is absent.
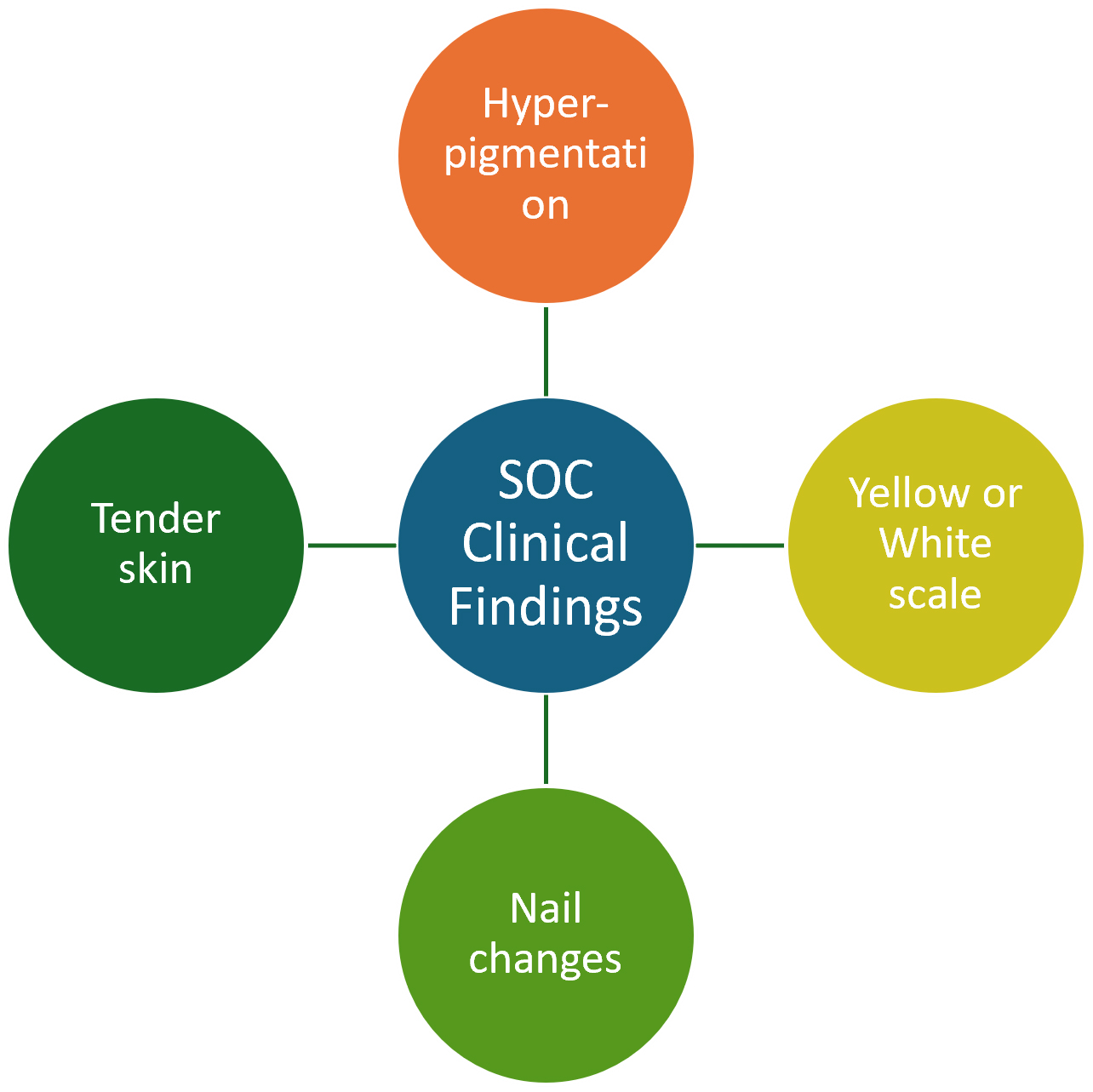 Fig. 2.
Fig. 2.
Clinical findings of Erythroderma in SOC.
Erythroderma requires urgent hospitalisation and immediate medical assessment. In SOC patients, document symptoms including pain, skin colour changes, drug history going back 8 weeks, and perform a full body exam, including mucosal surfaces (oral, genital and ophthalmic) and nails, to aid diagnosis.
Initial management includes fluid and electrolyte correction, thermoregulation support, and septic screen (Fig. 3). Contact Dermatology for further guidance. Initial skincare includes a bland petrolatum-based ointment to replace the damaged skin barrier and strict bedrest to stabilise thermos dysregulation and haemodynamic instability. Discontinue any potential culprit drugs.
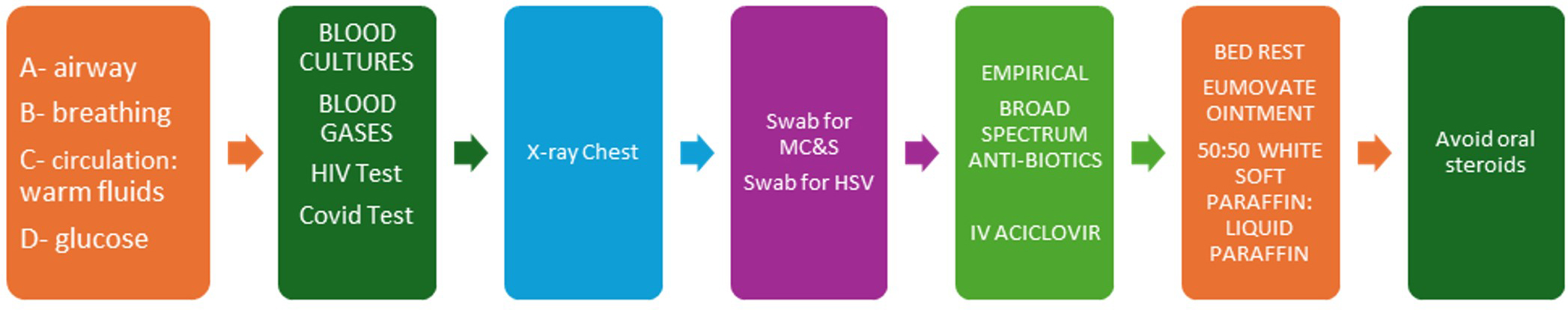 Fig. 3.
Fig. 3.
Clinical management. HIV, Human Immunodeficiency Virus; MC&S, Microbiology Culture and Sensitivity; HSV, Herpes Simplex Virus; IV, Intravenous.
Stevens-Johnson Syndrome /Toxic Epidermal Necrolysis (SJS/TEN) is a severe
cutaneous adverse reaction that involves sloughing and detachment of the
epidermis. SJS involves
In SOC, early SJS/TEN lesions are darker and less distinct, risking delayed recognition [19] (Fig. 4). Clinical suspicion for SJS/TEN should be high in a person with SOC presenting with widespread, acutely tender skin and mucosal involvement. Mucosal involvement may be the first appreciable clinical sign in those with SOC [15]. Ocular involvement can occur in up to 75% of patients, and can lead to long-term dryness, photophobia and visual loss. Evidence suggests that those with SOC are at risk of more severe ocular complications [20]. Survivors of SJS/TEN may face anxiety and distress from scarring, with those with SOC more prone to hyperpigmentation, hypertrophic, and keloid scarring; these sequelae can negatively impact psychosocial well-being [21].
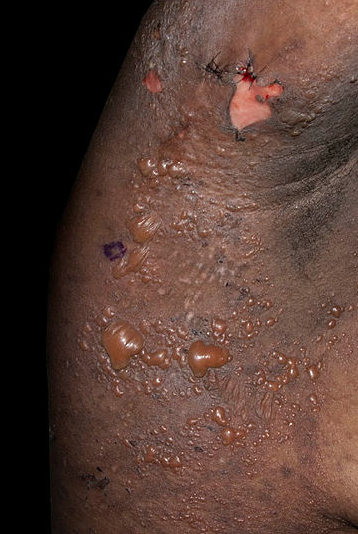 Fig. 4.
Fig. 4.
Toxic Epidermal Necrolysis (TEN) in a patient of black African heritage with bullae and hyperpigmentation; erythema is masked.
SJS/TEN is most commonly triggered by hypersensitivity to a drug, typically within 4 weeks of exposure. Drugs that are high risk for SJS/TEN are allopurinol, carbamazepine, lamotrigine, nevirapine, oxicam non-steroidal anti-inflammatory drugs, phenobarbital, sulfamethoxazole and other sulfur antibiotics and sulfasalazine [19, 22]. Infective triggers include Mycoplasma pneumonia, dengue virus and cytomegalovirus; while contrast medium administered for radiological assessments can be an iatrogenic cause [23].
SJS/TEN is rare; however, those with SOC have been found to be at increased risk of SJS/TEN compared to their white counterparts when exposed to the same drug [24]. Overall, there is thought to be a 2-fold increased risk compared to white patients [25]. The differences could be due to a variety of reasons, including genetic susceptibility based on Human Leukocyte Antigen (HLA) types, such as the HLA-B*15:02, which has been linked to an increased risk of hypersensitivity in Asian patients to carbamazepine [26].
For suspected SJS/TEN, take a detailed history, check for recent medication changes, and perform a full skin and mucosal exam. Assess the severity using the Score of Toxic Epidermal Necrolysis (SCORTEN), which can accurately predict mortality [27]. Discontinue the causative agent, transfer to intensive care or burns unit, and involve the multidisciplinary team for early supportive care.
Drug Reaction with Eosinophilia and Systemic Symptoms (DRESS) develops 2 to 6 weeks after initiation of a drug, and is characterised by a morbilliform eruption, fever, systemic involvement, lymphadenopathy, eosinophilia, and there can be multi organ involvement [28]. Common triggers include anticonvulsants, antibiotics, sulphonamides and allopurinol. The incidence of DRESS is estimated to be between 1 in 1000 and 1 in 10,000, depending on the causative agent. There is a mortality of up to 10%, often from hepatic necrosis, and after recovery, there can be significant long-term complications [29].
DRESS presents as a morbilliform rash, appearing violaceous or hyperpigmented in SOC, leading to delayed diagnosis and reliance on skin biopsy, risking poorer outcomes [30]. Lymphadenopathy, facial and ear oedema, mucosal involvement, and polymorphic skin lesions may develop (Fig. 5). Systemic involvement includes the liver, kidneys, lungs, and more, requiring a comprehensive clinical evaluation [28].
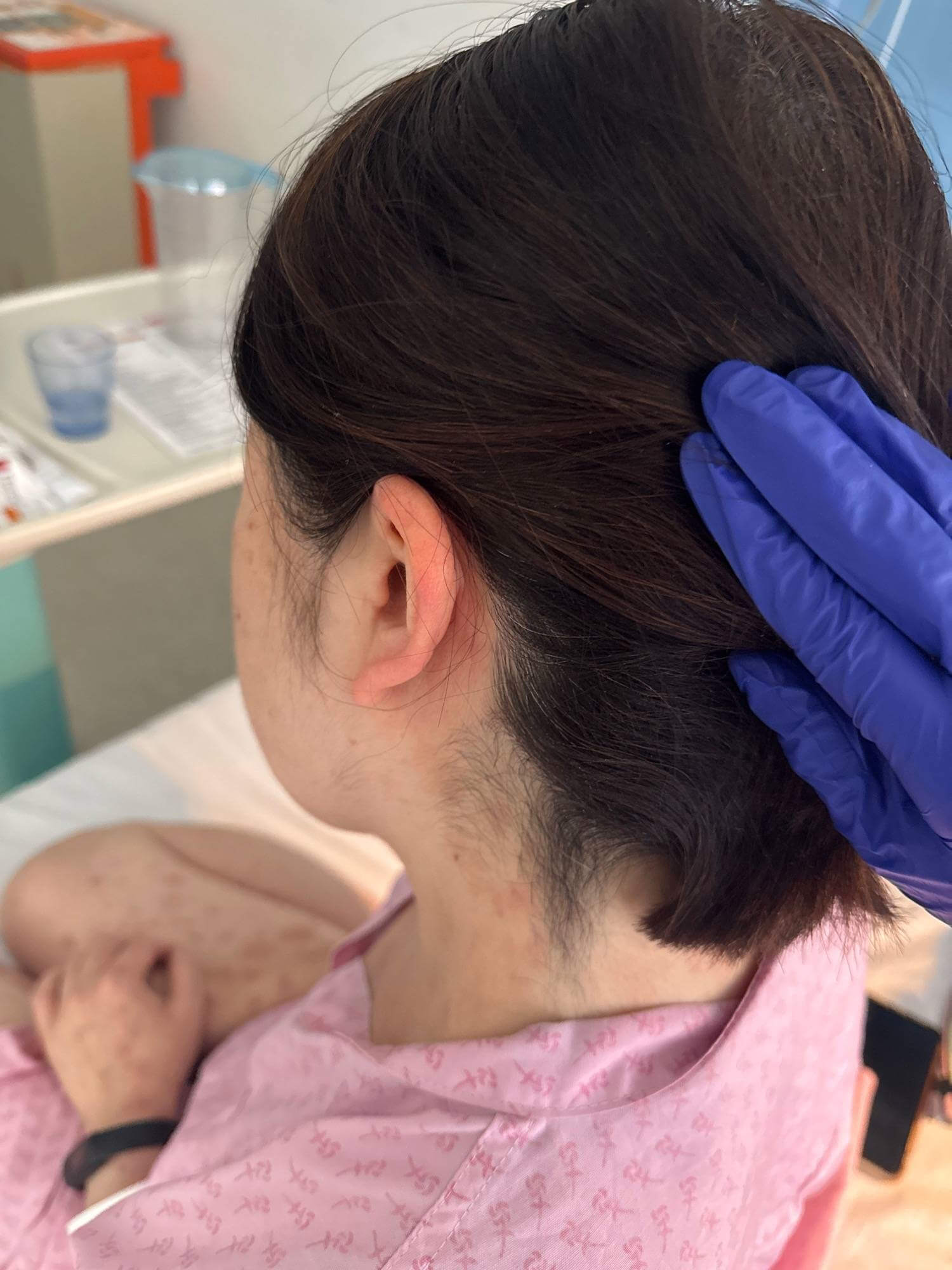 Fig. 5.
Fig. 5.
Swollen ear in the context of DRESS in a patient of East Asian heritage. DRESS, Drug Reaction with Eosinophilia and Systemic Symptoms.
The pathogenesis of DRESS is due to a complex interaction between drugs, viruses, and the T-cell-mediated immune system. The commonest triggers of DRESS include allopurinol, vancomycin, lamotrigine, carbamazepine, and trimethoprim-sulfamethoxazole [31]. Non-drug causes include vaccines and contrast media [32, 33]. Factors increasing the risk of DRESS include Human Herpesvirus 6 (HHV-6) reactivation, specific HLA alleles, comorbidities, and allopurinol use. A detailed drug history, including medications from the past 6 weeks, is essential [28].
DRESS diagnosis is clinical, with biopsy showing lymphocytic infiltrates and eosinophilia. Scoring systems such as Registry of Severe Cutaneous Adverse Reactions (RegiSCAR) aid diagnosis, given the constellation of symptoms and signs [34] (Table 3). Stopping the causative drug is crucial once DRESS is suspected. Investigations include blood tests, chest X-ray, electrocardiogram, and urinalysis. Treatment involves topical and systemic immunosuppression, supportive care, and specialist involvement for organ involvement, such as liver injury [34].
| Yes | No | Unknown | |
| Fever |
+1 | 0 | 0 |
| Enlarged lymph nodes |
+1 | 0 | 0 |
| Eosinophilia: |
+1 | 0 | 0 |
| Atypical lymphocytes | +1 | 0 | 0 |
| Skin rash |
+1 | 0 | 0 |
| Skin rash suggestive of DRESS (e.g., oedema, purpura) | +1 | 0 | 0 |
| Organ involvement (liver, kidney, lung, heart, thyroid) | +1 per organ affected | 0 | 0 |
| Resolution |
+1 | 0 | 0 |
| Previous exposure to the suspected drug | +1 | 0 | 0 |
| Absence of other causes (infection, autoimmune, etc.) | +1 | 0 | 0 |
RegisSCAR, Registry of Severe Cutaneous Adverse Reactions; WBC, whole blood count.
Scoring Interpretation:
•
• 2–3 points: Possible DRESS;
• 4–5 points: Probable DRESS;
•
Systemic involvement can cause long-lasting issues like hepatitis and myocarditis with a mortality of 10%, typically from hepatic necrosis [28].
Recognising dermatological emergencies in skin of colour (SOC) is vital to promoting health equity. Conditions like SJS/TEN and DRESS may present with subtle hyperpigmentation instead of classic erythema. Early recognition, thorough history-taking, prompt drug withdrawal, and supportive care are key to improving outcomes and reducing morbidity and mortality.
• Skin changed in dermatological emergencies such as Erythroderma, SJS/TEN, and DRESS may appear as hyperpigmented rather than erythematous, complicating and delaying early recognition.
• Consider and screen for drug reactions causing severe cutaneous adverse events in those with SOC given as genetic susceptibility may be increased.
• Those with SOC are more likely to develop keloidal scarring and dyspigmentation; therefore, early diagnosis is crucial to prevent long-term sequelae.
Not applicable.
RA, CU and MS designed and conducted the work. RA and CU wrote the manuscript. MS reviewed and edited the draft manuscript. CU and MS generated the diagrams and tables. All authors contributed to critical revision of the manuscript. All authors read and approved the final manuscript. All authors participated sufficiently in the work and agreed to be accountable for all aspects of the work.
The research was conducted in strict accordance with the ethical principles outlined in the Declaration of Helsinki. All patients provided written informed consent.
We are thankful to patients who gave permission to share their anonymous images in this publication.
This research received no external funding.
Dr. Sommerlad has received honoraria for speaking engagements from Johnson & Johnson, AbbVie, UCB, L’Oréal, and Avène. The authors declare no conflict of interest.
References
Publisher’s Note: IMR Press stays neutral with regard to jurisdictional claims in published maps and institutional affiliations.





