1 Research Division, Medhub Academy, 11440 Jakarta, Indonesia
Coronary Heart Disease (CHD) remains the leading cause of global mortality, including in Indonesia. Recent data revealed that approximately two million working-age Indonesians. By retirement age, CHD is estimated to result in 32,492 (36.6%) excess deaths and 128,132 (0.5%) years of life lost [1]. This crisis is compounded by systemic challenges within the screening process in Indonesia, including issues with accessibility, financing, logistics, the availability of medical instrumentation, and human resources; as well as disjointed reporting systems [2].
This situation demands a new paradigm. Emerging evidence suggests that facial phenotypes, analysed by artificial intelligence (AI), can detect underlying cardiovascular conditions. AI examines external physical traits as non-invasive biomarkers for risk determination [3, 4]. This approach, known as digital phenotyping, is grounded in decades of clinical observation and cutting-edge machine learning. This methodology can potentially be integrated with the existing system developed by the Badan Penyelenggara Jaminan Sosial (BPJS Kesehatan), named Face Recognition Integrated System Hospital (FRISTA), which is primarily intended to assist in patient administration and claims [5]. The current article describes the potential of utilising facial and lingual data through FRISTA system to assist in CHD screening among the Indonesian population.
Clinically proven facial hallmarks, including a diagonal earlobe crease and xanthelasma, have been associated with an increased risk of CHD. Contemporary AI advances this concept by employing deep learning (DL) to analyse more nuanced details. Early studies utilised facial pattern data (derived from nose bridge, canthus, crow’s feet, ear, and forehead) of more than one thousand CHD patients. The model demonstrated high sensitivity (80%) and modest specificity (61%), with a detection accuracy of 75% and a high positive predictive value (PPV) (87%) [3].
Certain systems assess the density of micro-wrinkles and skin pigmentation to determine an individual’s biological age in relation to their chronological age, thereby assisting in cardiovascular disease (CVD) risk assessment [6]. In the Indonesian context, diverse skin pigmentation may pose a challenge. Previous AI models were mostly trained on “Asian” data (particularly Chinese) which may perform well on lighter-skinned Indonesians but fail in darker-skinned communities. This necessitates a thorough validation investigation involving participants from various regions of Indonesian to ensure the algorithm’s accuracy.
Furthermore, non-contact facial thermal imaging can detect patterns of inflammation and irregular blood flow while predicting CHD with a good level of accuracy (area under the curve [AUC] of 0.804) [7]. An Indonesian study involving 26 CHD patients also demonstrated that facial texture could be a good indicator for CHD screening, as used in face recognition technology. The model produced a moderate accuracy (76.9%) and an outstanding discriminatory ability (AUC: 0.928), demonstrating its outstanding discriminatory ability. Moreover, the study showed that the forehead area has the highest prediction accuracy (90%) [8].
In addition to facial features, lingual diagnostics are also beneficial for the CHD screening process. A study demonstrated the utility of DL technology combined with an eXtreme Gradient Boosting (XGBoost) classifier to determine CHD status with a 76% accuracy [9]. The true efficacy of AI technology lies in its capacity to fuse data from diverse sources, yielding a more precise and comprehensive evaluation than any singular source achieved independently. The combination of facial and lingual data produces a comprehensive clinical portrait that is both scientifically sophisticated and culturally pertinent in Indonesia.
It is vital to understand the potential screening difficulties given Indonesia’s status as the nation with the largest Muslim population, especially for women who wear hijabs, niqabs, or chadors. The hijab covers the ears, making it difficult to identify diagonal earlobe creases, while wearing a niqab or chador makes it more challenging to complete typical facial recognition and thermal scans. Some suggested alternatives include setting up private, women-only registration booths for medical scans and collaboration with the Majelis Ulama Indonesia (MUI) to evaluate the technology within the country’s cultural context. Furthermore, AI should prioritise “central face” elements, including the eyes (specifically the iris), nose, and mouth, to overcome instances where the ears are obscured.
Indonesia has a unique resource for implementing face recognition technology nationwide: the FRISTA, launched in 2024 by BPJS Kesehatan. Hospitals have already implemented this biometric verification technology, which uses facial and fingerprint recognition to authenticate patients for medical services. Its primary functions are to expedite enrolment and prevent insurance fraud [5]. This technology integrates seamlessly with the Indonesian Hospital Management Information (IHMI) system, enabling access to medical records to assess health status [10].
FRISTA, with its extensive database of patient records, has the potential to evolve from a basic administrative instrument into a robust clinical tool. The technology now captures photos or videos of patients in real time during registration. It utilises facial identification to transmit information confidentially to a central AI engine for evaluation [5, 10]. Proposed development using multimodal data will provide a CHD risk score almost instantaneously, which can be incorporated into the patient’s digital record. The screening result would be non-intrusive and advantageous, providing support for the attending physician while maintaining the clinical workflow [3, 4].
However, the inherent limitations of this equipment must be carefully considered. FRISTA is intended as an administrative system rather than a clinical one. Field research reveals significant operational issues, including recurrent verification failures attributed to insufficient illumination, masks, and variations in facial appearance, particularly among elderly or emergency patients. The stringent BPJS policy permitting human verification overrides for only 2% of patients monthly exacerbates these issues by generating a bottleneck that might impede care delivery [5]. This project requires more than a mere software update; it necessitates a comprehensive redesign of the FRISTA ecosystem, encompassing hardware upgrades and a transformation from rigid administrative oversight to adaptable, risk-based clinical facilitation. The strengths, weaknesses, opportunities, and threats (SWOT) analysis regarding FRISTA and multimodal face recognition for CHD screening is available in Fig. 1.
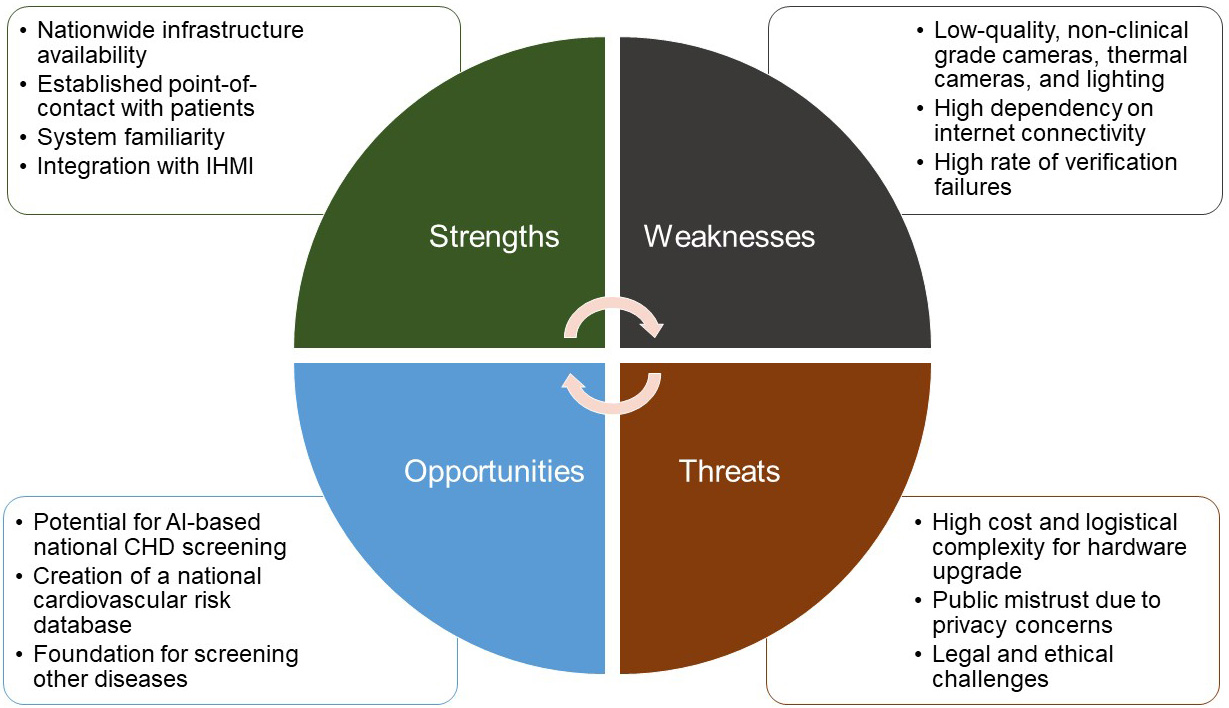 Fig. 1.
Fig. 1.
Strengths, weaknesses, opportunities, and threats (SWOT) analysis. CHD, Coronary Heart Disease; AI, artificial intelligence; IHMI, Indonesian Hospital Management Information. Source: Author’s creation (TPU). Created using Microsoft PowerPoint 2108 (Microsoft Corporation, Redmond, WA, USA).
Implementing a revolutionary system necessitates a robust foundation of governance and ethics. Indonesia possesses a comprehensive legal framework that facilitates this; the Personal Data Protection (PDP) Law (Law No. 27 of 2022) serves as a regulation equivalent to the European General Data Protection Regulation (GDPR). It categorises health and biometric information as “sensitive personal data” and mandates stringent management methods, including a Data Protection Impact Assessment (DPIA) [11].
Because Facial Recognition Technology (FRT) collects unique and sensitive biometric data, it remains vulnerable to misuse unless handled with robust transparency and security protocols [12]. Unlike conventional authentication data, such as passwords, facial data are permanent and immutable, inherently linked to an individual’s identity. Potential misuse includes, but is not limited to, the leakage of personal or financial data, misidentification, and concerns during mass surveillance, all of which can erode individual privacy.
The formulation of clear regulations governing this technology’s use, transparency in system operations, and data security guarantees are critical to the responsible and ethical functionality of AI systems while mitigating potential risks. Such regulations must balance the prevention of data misuse with the technology’s use for beneficial applications, such as enhancing disease detection accuracy. The AI model qualifies as Software as a Medical Device (SaMD) and must undergo extensive clinical testing before approval by the Ministry of Health. Thus, the implementation process will be extensive, consisting of a pilot study, scaled rollout, and national screening programme implementation [13].
The cost-effectiveness of introducing facial recognition for CHD screening rests on the principle of high initial fixed costs counterbalanced by negligible variable costs (per-screening) and significant downstream savings from avoided cardiovascular events. The implementation of face recognition for CHD detection may be beneficial to support the readily available screening program in Indonesia (a universal health screening programme for every resident on their birthday).
The financing model can be divided into two distinct phases: (1) development &
calibration (investment phase) and (2) deployment (operational phase). The first
phase contributed as the primary expenditure of developing and calibrating the AI
algorithm to ensure diagnostic accuracy. Market estimates for developing a
custom, regulatory-grade computer vision application for healthcare diagnostics
range from US
The proposed workflow starts with notification to the patients and a positive screening result based on the AI facial recognition system through the BPJS Kesehatan app. Subsequently, physicians will conduct targeted consultations and physical examinations for CHD signs. Subjects with a perturbing screening result with relevant symptoms will be instructed to undertake biochemical laboratory tests and cardiovascular exams, including lipid profiles, blood glucose levels, and electrocardiograms. Patients without severe clinical manifestations will be directed into early intervention programmes—nutrition education, community exercise, and regular monitoring. Meanwhile, individuals with substantial abnormalities will be referred to a cardiologist for further examinations involving echocardiography, treadmill stress tests, and computed tomography calcium score/angiogram assessments.
Multimodal face recognition is feasible to implement within the FRISTA system as an extension of the existing instrument. By transforming the existing administrative network into a cutting-edge clinical screening platform, Indonesia has an unprecedented opportunity to combat its leading cause of death, reduce healthcare inequities, and establish itself as a global pioneer in digital health innovation. However, implementation requires a significant time and costs, especially for enhancing infrastructure. Large-scale testing remains necessary before a nationwide screening process can be initiated.
• CHD represents a critical health issue in Indonesia, contributing significantly to national morbidity and mortality.
• Current CHD screening methods are often ineffective, causing late diagnosis and direct complication.
• AI-based facial recognition technology has a significant potential to enhance non-invasive CHD screening.
• Implementing facial recognition-based CHD screening needs robust interprofessional collaboration to determine suitable management following positive findings.
• Facial recognition-based CHD screening implementation needs a very long process, from a pilot study to external validation and a final national programme initiative.
Not applicable.
Conceptualization: TPU; data collection and synthesis: TPU, MMS, and AMS; visualization: TPU; resources: TPU; writing—original draft preparation: TPU; writing—review and editing: TPU, MMS, and AMS. All authors contributed to the important editorial changes in the manuscript. All authors read and approved the final manuscript. All authors have participated sufficiently in the work and agreed to be accountable for all aspects of the work.
Not applicable.
Not applicable.
This research received no external funding.
The authors declare no conflict of interest.
References
Publisher’s Note: IMR Press stays neutral with regard to jurisdictional claims in published maps and institutional affiliations.

