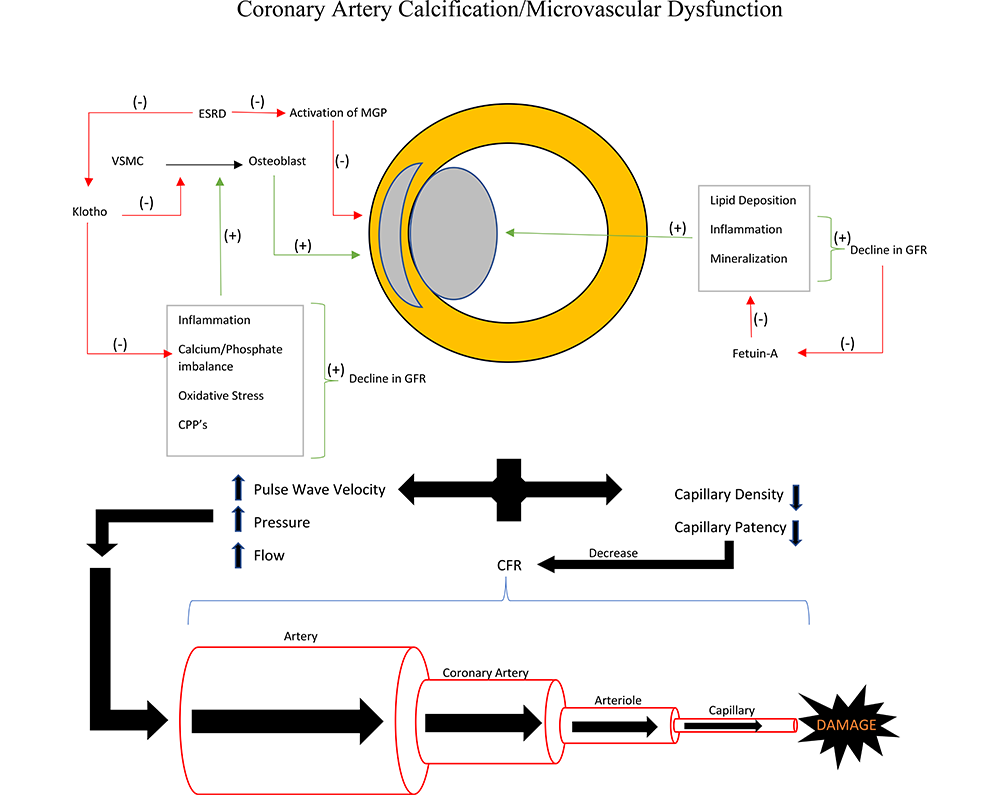
Cardiovascular disease, and in particular coronary artery disease (CAD), remains an important contributor of morbidity and mortality among patients with chronic kidney disease (CKD). Classic symptomatology of CAD and effectiveness of established therapeutic measures is less frequent in patients with CKD. This suggests unique characteristics of CAD among patients with CKD. Two important features of CAD in CKD include increased calcific density of atherosclerotic plaques and of the vessels themselves (coronary artery calcification -- CAC), as well as a decrease in microcirculatory function -- or coronary microcirculatory dysfunction. A multitude of pathophysiologic pathways have been identified that contribute to CAC in CKD; less is known about the pathophysiology of microcirculatory dysfunction. It is not well established if these two processes are directly related to each other, but the combination results in a greater severity of effect on overall myocardial function and may in part explain the greater preponderance of silent myocardial infarction. Further investigation is needed to better understand these unique aspects of CAD in CKD as well as the role they play in overall CVD in this group, and ultimately therapeutics that may lessen the burden of disease.