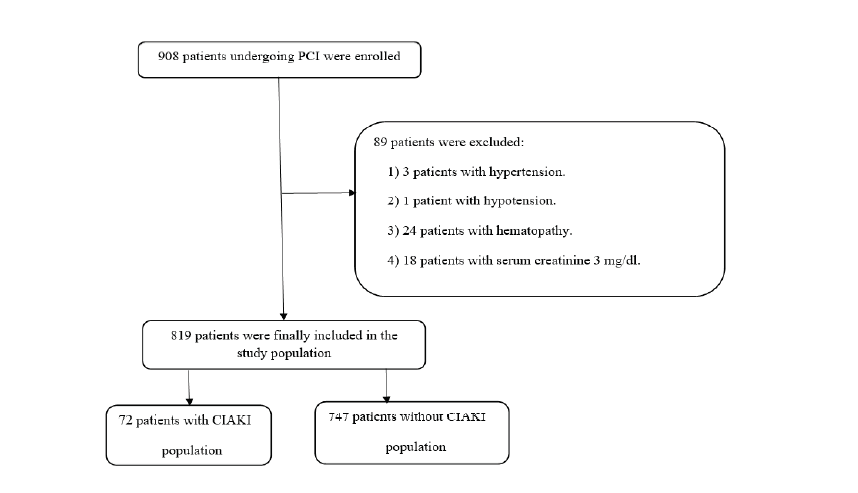
Serum creatinine and serum albumin levels were measured prior to surgery, and serum creatinine level was also measured at 72 hours following percutaneous coronary intervention in 819 (January 1st, 2015 and December 31th, 2018). According to whether patients developed contrast-induced acute kidney injury or not, they were assigned to either a contrast-induced acute kidney injury group (72 cases, 8.8%) or a non-contrast-induced acute kidney injury group (747 cases; control). Serum albumin was significantly lower in the contrast-induced acute kidney injury group than control (39.33 ± 5.09 g/l and 42.69 ± 5.19 g/l, respectively, P < 0.001). The results of a receiver-operating curve analysis indicated a serum albumin level of 40.5 g/L was the optimal cut-off value for prediction of contrast-induced acute kidney injury and according to a multivariate logistic regression analysis, serum albumin was an independent biomarker for prediction of (95% confidence interval: 0.836-0.935, odds ratio: 0.884, P < 0.001). Serum albumin, a low-cost and easily assessable laboratory protein, was independently related to a greater risk of contrast-induced acute kidney injury among patients that received percutaneous coronary intervention. It is proposed that under these circumstances SA is a potential biomarker for contrast-induced acute kidney injury.